Abstract
Intratumoral heterogeneity (ITH) may produce regional biases in genotype and phenotype evaluation in a single tumor and may impede proper cancer diagnosis. To evaluate the extent of ITH in colorectal cancer (CRC) with microsatellite instability (MSI), we obtained 4–7 biopsies from 39 CRCs followed by MSI analysis either using the Bethesda MSI evaluation system or Promega system with 5 mononucleotide markers. We found decreased prevalence of MSI (+) by the Promega system compared to the Bethesda system. The overall discordance between the two systems was 54 %. In contrast to the previous studies that had shown discordance only in low MSI (MSI-L), our results showed the discordance not only in MSI-L, but also in high MSI (MSI-H) cases. Among the MSI (+) CRCs, ITH of MSI status was identified in 41.7 % of CRC by the Bethesda system and 22.2 % by the Promega system. In terms of MSI markers, the ITH originated from dinucleotide markers in most cases (69 %), but it originated from mononucleotide markers (31 %) as well. Pooling of DNA from a regional biopsy with MSI (+) with additional biopsies from stable MSI (MSS) showed that this approach was beneficial to increase the sensitivity of MSI detection. Our results indicate that ITH of MSI phenotype by the Bethesda system is more overestimated than previously identified. However, because there was considerable ITH of MSI subtypes and markers even by the Promega system, our data suggest that analysis of MSI status in multiple regional biopsies is needed for a better evaluation of MSI status in CRC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
It is now well believed that a cancer is formed by clonal expansion of a single cell from which new subclones emerge by multiple mutations [1]. As a cancer progresses with enriched subclones, it becomes heterogenous at genetic and phenotypic levels. Generation of such intratumoral heterogeneity (ITH) is important in acquiring aggressiveness in a cancer and possibly impedes accurate clinical diagnosis as well as proper selection of cancer therapies [2]. These days, many clinics use somatic mutations as diagnostic and therapeutic biomarkers in cancer patients, including EGFR mutations in lung cancers and BRAF mutations in melanomas [3]. However, a recent study reported that EGFR mutation ITH was present in 9–24 % of lung cancer patients, indicating that multiple biopsies would be required for accurate assessment of the mutation status [4].
Microsatellite instability (MSI), a type of genomic instability, is characterized by length alterations in repeated mononucleotide or dinucleotide DNA sequences and comprises 10–30 % of colorectal cancer (CRC) [5, 6]. Many genes harbor frameshift mutations within the nucleotide repeats in the cancers with MSI, including TGFBR2, BAX, IGFR2 and TCF4 [7–9]. There are several reports that identified genetic ITH of microsatellite markers used for MSI status evaluation as well as ITH of nucleotide lengths in the coding genes [10, 11]. However, most of the studies did not exactly specify strategies for regional tumor sampling for the evaluation of ITH [12]. Moreover, most of them used Bethesda MSI classification system using two mononucleotide repeats and three dinucleotide repeats, while Promega system, the more recent technique with quasi-mononucleotide repeats has been established [13, 14]. For a better understanding of ITH in CRCs with MSI, we investigated the ITH using both Bethesda and Promega systems with a well measured sampling strategy. The data indicated that ITH of MSI was evident not only by the Bethesda system, but also by the Promega system, and suggest that ITH should be considered in evaluating MSI.
Materials and Methods
Colorectal Cancer Tissues
Colectomy tissues from 39 CRC patients used for this study came from a university-affiliated hospital (Eujeongbu St. Mary Hospital, Korea). All of the patients with the cancers were Koreans without any positive family history of CRC. Approval for this study was obtained from the Catholic University of Korea, College of Medicine’s institutional review board. After the surgery, a surgeon picked four to seven different tumor areas and one normal mucosal area from each fresh colectomy specimen. The tumor areas were 0.027–1 cm3 and at least 1.0 cm apart from each other. Normal mucosae were collected at least 5 cm apart from tumor margins. All of the picked fragments from tumor and normal areas were frozen, cut, and stained with hematoxylin & eosin (H&E). Two pathologists selected areas with rich tumor cell population (at least 80 %), which were subsequently used as tumor areas 1–7 in this study. Also, the pathologists confirmed that none of the colectomy samples used in this study was multifocal tumors. In each patient’s sample, histologic grades of the selected areas were not different from each other, indicating that the selected areas represented the most common histologic patterns with minimal histologic differences in each sample. Each tumor area was further sliced into a fragment, which was subsequently used for genomic DNA extraction. For genomic DNA extraction, we used the DNeasy Blood & Tissue Kit (Qiagen, Hilden, Germany) according to the manufacturer’s recommendation.
Microsatellite Evaluation
MSI status of each area of each CRC was evaluated by two systems (Bethesda and Promega systems). The Bethesda system adopted two mononucleotide repeats (polyadenine repeats BAT-25 and BAT-26) and three dinucleotide CA repeats (D2S123, D5S346 and D17S250) based on the recommendations from National Cancer Institute in 2002 [13], tumoral MSI status of which was characterized as: high MSI (MSI-H), if two or more of these markers show instability, low MSI (MSI-L), if one of the markers shows instability, and stable MSI (MSS), if none of the markers shows instability. The Promega system used five mononucleotide repeats (BAT-25, BAT-26, NR-21, NR-24 and MONO-27), tumoral MSI status of which was characterized as: MSI-H, if two or more of these markers show instability, MSI-L, if one of the markers shows instability and MSS, if none of the markers shows instability [14] . When evaluating MSI status among multiple tumor areas of a single CRC tissue, we considered the CRC as MSI (+) when one or more tumor area (s) out of multiple regional biopsies was (were) identified either MSI-H or MSI-L. For the MSI status evaluation, we used conventional denaturing gel electrophoresis instead of fluorescent-labeled polymerase chain reaction (PCR) and capillary electrophoresis, because we would like to compare the two systems with the same method and because most of the studies on MSI heterogeneity had been performed with denaturing gel electrophoresis. Genomic DNA from tumor areas and matched normal tissues from the cases were amplified by PCR using specific primers that encompassed the repeat sequences. Radioisotope ([32P] dCTP) was incorporated into the PCR products for detection by autoradiogram. PCR products were then displayed on 6 % polyacrylamide gel containing 7 mol/L urea.
MSI Analysis Using Pooled DNA
For the cancers showing ITH among the regional biopsies, DNA from each fragment with ITH was pooled with DNA from one or more fragments without ITH to test whether multiple biopsies and pooling of multiple DNA samples would be sensitive enough to detect MSI. We considered the pooled DNA as MSI marker (+) when the corresponding MSI marker showed instability. We evaluated the MSI status of the pooled samples with the two MSI evaluation systems.
Statistical Analysis
Statistical analysis was performed using a commercially available statistical software package (SPSS statistical software version 18.0 (SPSS Inc, Chicago, IL)). Fisher’s exact test was used to analyze the ITH of Bethesda and Promega systems. The Cohen’s Kappa coefficient was calculated to determine inter-rater agreement between the two MSI evaluation systems. The level of significance was set at p < 0.05.
Results
MSI Analysis by the Bethesda and Promega Systems
From 39 CRC patients, 227 regional fragments of cancer tissues were collected and analyzed by two MSI evaluation systems. When the Bethesda system was adopted, 41 out of 227 cancer fragments from 39 CRCs were considered MSI-H (18.1 %), 28 were MSI-L (12.3 %), and 158 were MSS (69.6 %). Collectively, 12 of the 39 CRCs (30.1 %) showed MSI (+) (MSI-H or MSI-L) in at least one of the regional CRC tissue fragments from a single mass (Table 1). Of note, one of the 41 MSI-H fragments (2.4 %) and 19 of the 28 MSI-L fragments (67.9 %) were unstable at dinucleotide repeats, but not at monocleotide repeats. When the Promega system using the five mononucleotide repeats was adopted, 35 out of 227 cancer tissue fragments were MSI-H (15.4 %), 21 were MSI-L (9.3 %) and 171 were MSS (75.3 %). Nine out of 39 CRCs (23.1 %) were identified as MSI (+) in this system (Table 1).
Twenty MSI-L (n = 19) and MSI-H (n = 1) tissue fragments identified by the Bethesda system were reinterpreted as MSS by the Promega system. Interestingly, the above-mentioned 19 MSI-L and one MSI-H tissue fragments with MSI (+) only in dinucleotide repeats (D2S123 and D17S250) by the Bethesda system were all reclassified MSS by the Promega system.
The number of MSI (+) CRCs identified by the Bethesda system (12/39, 30.1 %) was reduced when adopted by the Promega system (9/39, 23.1 %). In order to evaluate the inter-rater reliability of the two systems, Cohen’s Kappa coefficient was analyzed. The overall average Kappa value between the two was 0.637; it indicates substantial agreement, not a perfect match.
Intratumoral Heterogeneity
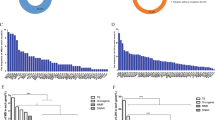
Next, we evaluated ITH of MSI status (MSI-H or MSI-L or MSS) among intratumoral fragments in each CRC (Figure 1). Among the MSI (+) CRCs (MSI-H or MSI-L), ITH of MSI status (any discordance among the fragments in a given CRC) by the Bethesda system was identified in five (cases 2, 15, 29, 35 and 40) of 12 CRCs (41.7 %), while the ITH by the Promega sysem was identified in two (cases 15 and 35) of nine CRCs (22.2 %) (Table 1). We also evaluated the ITH of individual MSI markers among the 39 CRCs and found that nine (23.1 %) had ITH by the Bethesda system and three of 39 (7.7 %) had ITH by the Promega system (Table 2). It was significantly different between the two systems (Fisher’s exact test, p = 0.009). Of the total number with MSI marker ITH (n = 26), 18 came from the dinucleotide markers (D2S123, D5S346 and D17S250) and eight came from mononucleotide markers (BAT-25, BAT-26, NR-21, NR-24 and MONO-27).
Of the 13 CRCs with MSI (+) by either Bethesda or Promega system, regional MSI status among the fragments of seven CRCs (cases 2, 17, 22, 27, 29, 35, and 40) showed discordance between the two systems (53.8 %). Of note, four CRCs (cases 2, 17, 29, and 40) were MSI (+) by the Bethesda system, but were reclassified MSS by the Promega system. By contrast, case 22 was classified MSS by the Bethesda system, but reclassified MSI (+) by the Promega system. Although case 35 was classified as MSI (+) by both systems, two of four fragments were differently evaluated (MSI-L by the Bethesda and MSI-H by the Promega system) (Table 1).
Pooled DNA Analysis
To test whether multiple regional biopsies and pooling of DNA would be sensitive enough to detect MSI in a single cancer tissue with ITH, we pooled genomic DNA of an MSI (+) tissue fragment together with DNA of one to six MSS fragments of each patient. Figure 2 depicts the regional biopsies with pooled DNA analysis. When a fragment with MSI (+) was pooled with either one or two or three or four or five or six fragments with MSS, 70.8 %, 66.6 %, 60 %, 33.3 %, 33.3 % and 0 % of the pooled DNA still showed MSI (+), respectively (Table 3).
Discussion
The purpose of this study was twofold. It was to define the extent of MSI ITH with the background of multiple regional biopsies in CRCs and to find whether pooled DNA analysis would be beneficial to overcome ITH in evaluating MSI status. First, we attempted to find whether there was any difference in MSI status between the Bethesda and Promega systems for CRCs in a condition with multiple regional biopsies, because earlier studies had compared the two systems only in condition with a single biopsy per CRC [15]. MSI (+) (MSI-H or MSI-L) was identified in 30.5 % of the fragments and 30.1 % of CRCs by the Bethesda system, while it was identified in 24.8 % of the fragments and 23.1 % of CRCs by the Promega system. Such decreased prevalence of MSI (+) by the Promega system compared to the Bethesda system had also been identified in earlier studies [16, 17], indicating that MSI (+) might be overestimated by the Bethesda system irrespective of the number of tissues.
Murphy et al. [15] identified that with a single biopsy, overall concordance between the Bethesda and Promega systems was 85 % that is much higher than our concordance data (46 %) with regional biopsies. Murphy et al. [15] also identified that there was complete concordance between the two systems for MSI-H and MSS cases. Also, all of the CRCs interpreted as MSI-L by the Bethesda system were interpreted as MSS by the Promega system [14]. By contrast, our data demonstrated that in the regional biopsies there was discordance between the two systems even for the MSI-H and MSS cases (Table 1). ITH of MSI phenotype was detected less in the Promega classification system than in the Bethesda system, which might hamper proper evaluation of MSI status in CRC.
The Bethesda MSI panel is known to have some limitations that are results of including dinucleotide repeats, because they are less sensitive and specific for detection of tumors with MSI than mononucleotide repeats and may result in misclassification of MSI-L as MSI-H [18, 19]. Our data generally agreed with this, as 69 % (18/26) of the MSI marker ITH (Table 2) originated from the dinucleotide markers. However, it is important to note that even the mononucleotide markers (BAT-25, BAT-26, NR-21, NR-24 and MONO-27) had ITH in the regional biopsies (31 %, 8/26). Inclusion of the dinucleotide markers may also explain the substantial agreement, not a perfect match by the Cohen’s Kappa analysis in our study. It remains unclear whether the disagreement came from the difference in regional biopsy numbers (3 vs. 4–7) or composition of the markers used or the other unidentified factors.
An earlier study analyzed ITH of MSI phenotype in three regions of each CRC using two mononucleotide and another three dinucleotide repeats [20]. They found that within a same tumor the MSI phenotype was observed regardless of the regions analyzed, showing the reproducibility of MSI phenotype throughout a tumor. Moreover, they found that only dinucleotide marker-only cases showed MSI marker ITH. These data were quite contrast to ours that showed both MSI phenotype ITH and MSI marker ITH (mononucleotides as well as dinucleoides) in CRC.
Next, because we had identified evidence for ITH of MSI phenotype, we attempted to find a way to overcome the ITH by pooling DNA from regional biopsies of each CRC. Pooling DNA from a fragment with MSI (+) with additional one (1/2 dilution) or two (1/3 dilution) or three (1/4 dilution) or four (1/5 dilution) or five (1/6 dilution) or six (1/7 dilution) fragments with MSS were able to detect MSI at the levels of 70.8 %, 66.6 %, 60 %, 33.3 %, 33.3 % and 0 %, respectively. Provided that even one of four regions in a CRC has MSI (+), our data suggest that pooling of the DNA can detect MSI in more than 60 % cases. Table 3 shows a trend that the more additional fragments with MSI (−) are added to one fragment with MSI (+), the less the detection rate of MSI (+) cases is achieved, indicating that multiple biopsies from a CRC would help identify MSI status than a single biopsy.
In summary, the present study identified disagreement in the MSI phenotype by the Bethesda and Promega systems in multiple regional biopsies of CRC. Also, we newly identified that in some cases MSI-H phenotype could be misinterpreted as MSI-L or MSS because of the ITH. It is considered that different MSI status presents contrasting outcome of the CRC patients; meta-analyses suggest that MSI-H CRCs are less aggressive, yielding longer disease-free survival [21]. Moreover, treatment modality would be changed according to the MSI status; some reported that MSI-H CRC were sensitive to the majority of chemotherapeutic agents, but resistant to 5-fluorouracil [22, 23]. ITH of MSI may complicate not only diagnostic, but also therapeutic decisions. Empirical and mathematical approaches have been made in order to overcome the obstacle, yet it has not been successful. We believe that our data on analysis of MSI status in multiple regional biopsies from a cancer tissue and pooling of DNA from the regions indicated that multiple biopsies should be performed for a better understanding of MSI status that would further aid for diagnosis and treatment of CRC patients.
References
Wainscoat JS, Fey MF (1990) Assessment of clonality in human tumors: a review. Cancer Res 50:1355–60
Marusyk A, Almendro V, Polyak K (2012) Intra-tumour heterogeneity: a looking glass for cancer? Nat Rev Cancer 12:323–34
Duffy M, Crown J (2013) Companion biomarkers: paving the pathway to personalized treatment for cancer. Clin Chem 59:1447–56
Chen ZY, Zhong WZ, Zhang XC, Su J, Yang XN, Chen ZH, Yang JJ, Zhou Q, Yan HH, An SJ, Chen HJ, Jiang BY, Mok TS, Wu YL (2012) EGFR mutation heterogeneity and the mixed response to EGFR tyrosine kinase inhibitors of lung adenocarcinomas. Oncologist 17:978–85
Loukola A, Eklin K, Laiho P, Salovaara R, Kristo P, Järvinen H, Mecklin JP, Launonen V, Aaltonen LA (2001) Microsatellite marker analysis in screening for hereditary nonpolyposis colorectal cancer (HNPCC). Cancer Res 61:4545–9
Goel A, Arnold CN, Niedzwiecki D, Chang DK, Ricciardiello L, Carethers JM, Dowell JM, Wasserman L, Compton C, Mayer RJ, Bertagnolli MM, Boland CR (2003) Characterization of sporadic colon cancer by patterns of genomic instability. Cancer Res 63:1608–14
Markowitz S, Wang J, Myeroff L, Parsons R, Sun L, Lutterbaugh J, Fan RS, Zborowska E, Kinzler KW, Vogelstein B, Brattain M, Wilson JKV (1995) Inactivation of the type II TGF-beta receptor in colon cancer cells with microsatellite instability. Science 268:1336–8
Calin GA, Gaf R, Tibiletti MG, Herlea V, Becheanu G, Cavazzini L, Barbanti-Brodano G, Nenci I, Negrini M, Lanza G (2000) Genetic progression in microsatellite instability high (MSI-H) colon cancers correlates with clinico-pathological parameters: a study of the TGRbetaRII, BAX, hMSH3, hMSH6, IGFIIR and BLM genes. Int J Cancer 89:230–5
Duval A, Gayet J, Zhou XP, Iacopetta B, Thomas G, Hamelin R (1999) Frequent frameshift mutations of the TCF-4 gene in colorectal cancers with microsatellite instability. Cancer Res 59:4213–5
Barnetson R, Jass J, Tse R, Eckstein R, Robinson B, Schnitzler M (2000) Mutations associated with microsatellite unstable colorectal carcinomas exhibit widespread intratumoral heterogeneity. Gene Chromosome Cancer 29:130–6
Duval A, Hamelin R (2002) Mutations at coding repeat sequences in mismatch repair-deficient human cancers: toward a new concept of target genes for instability. Cancer Res 62:2447–54
Chung YJ, Kim KM, Choi JR, Choi SW, Rhyu MG (1998) Relationship between intratumor histological heterogeneity and genetic abnormalities in gastric carcinoma with microsatellite instability. Int J Cancer 82:782–8
Boland CR, Thibodeau SN, Hamilton SR, Sidransky D, Eshleman JR, Burt RW, Meltzer SJ, Rodriguez-Bigas MA, Fodde R, Ranzani GN, Srivastava S (1998) A National Cancer Institute Workshop on microsatellite instability for cancer detection and familial predisposition: development of international criteria for the determination of microsatellite instability in colorectal cancer. Cancer Res 58:5248–57
Patil DT, Bronner MP, Portier BP, Fraser CR, Plesec TP, Liu X (2012) A five-marker panel in a multiplex PCR accurately detects microsatellite instability-high colorectal tumors without control DNA. Diagn Mol Pathol 21:127–33
Murphy K, Zhang S, Geiger T, Hafez MJ, Bacher J, Berg KD, Eshleman JR (2006) Comparison of the microsatellite instability analysis system and the Bethesda panel for the determination of microsatellite instability in colorectal cancers. J Mol Diagn 8:305–11
Tomlinson I, Halford S, Aaltonen L, Hawkins N, Ward R (2002) Does MSI-low exist? J Pathol 197:6–13
Xicola RM, Llor X, Pons E, Castells A, Alenda C, Piñol V, Andreu M, Castellví-Bel S, Payá A, Jover R, Bessa X, Girós A, Duque JM, Nicolás-Pérez D, Garcia AM, Rigau J, Gassull MA; Gastrointestinal Oncology Group of the Spanish Gastroenterological Association (2007) Performance of different microsatellite marker panels for detection of mismatch repair-deficient colorectal tumors. J Natl Cancer Inst 99:244–52
Buhard O, Suraweera N, Lectard A, Duval A, Hamelin R (2004) Quasimonomorphic mononucleotide repeats for high-level microsatellite instability analysis. Dis Markers 20:251–7
Suraweera N, Duval A, Reperant M, Vaury C, Furlan D, Leroy K, Seruca R, Iacopetta B, Hamelin R (2002) Evaluation of tumor microsatellite instability using five quasimonomorphic mononucleotide repeats and pentaplex PCR. Gastroenterology 123:1804–11
Danjoux M, Guimbaud R, Al Saati T, Meggetto F, Carrère N, Portier G, Delsol G, Selves J (2006) Contribution of microdissection for the detection of microsatellite instability in colorectal cancer. Hum Pathol 37:361–8
Popat S, Houlston RS (2005) A systematic review and meta-analysis of the relationship between chromosome 18q genotype, DCC status and colorectal cancer prognosis. Eur J Cancer 41:2060–70
Carethers JM, Smith EJ, Behling CA, Nguyen L, Tajima A, Doctolero RT, Cabrera BL, Goel A, Arnold CA, Miyai K, Boland CR (2004) Use of 5-fluorouracil and survival in patients with microsatellite-unstable colorectal cancer. Gastroenterology 126:394–401
Fallik D, Borrini F, Boige V, Viguier J, Jacob S, Miquel C, Sabourin JC, Ducreux M, Praz F (2003) Microsatellite instability is a predictive factor of the tumor response to irinotecan in patients with advanced colorectal cancer. Cancer Res 63:5738–44
Acknowledgments
This study was supported by a grant from National Research Foundation of Korea (2012R1A5A2047939).
Conflict of Interests
The authors declare no competing interests.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Choi, Y.J., Kim, M.S., An, C.H. et al. Regional Bias of Intratumoral Genetic Heterogeneity of Nucleotide Repeats in Colon Cancers with Microsatellite Instability. Pathol. Oncol. Res. 20, 965–971 (2014). https://doi.org/10.1007/s12253-014-9781-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12253-014-9781-y