Abstract
Ginkgo biloba has long been used in traditional Chinese medicine. In this study, ginkgoneolic acid, a kind of compound extracted from G. biloba, was investigated for its effects on growth, acid production, adherence, biofilm formation, and biofilm morphology of Streptococcus mutans. The results showed that ginkgoneolic acid inhibited not only the growth of S. mutans planktonic cells at minimum inhibitory concentration (MIC) of 4 μg/mL and minimum bactericidal concentration (MBC) of 8 μg/mL but also the acid production and adherence to saliva-coated hydroxyapatite of S. mutans at sub-MIC concentration. In addition, this agent was effective in inhibiting the biofilm formation of S. mutans (MBIC50 = 4 μg/mL), and it reduced 1-day-developed biofilm of S. mutans by 50 % or more at low concentration (MBRC50 = 32 μg/mL). Furthermore, the present study demonstrated that ginkgoneolic acid disrupted biofilm integrity effectively. These findings suggest that ginkgoneolic acid is a natural anticariogenic agent in that it exhibits antimicrobial activity against S. mutans and suppresses the specific virulence factors associated with its cariogenicity.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Dental caries is a chronic, progressive, destructive, and transmissible infectious disease on the tooth hard tissue (Selwitz et al. 2007). As it progresses, extensive destruction of the enamel and dentin occurs, followed by cavitation, inflammation of pulp, and periapical tissue, even tooth loss. Streptococcus mutans has long been considered as the principal etiological agent of dental caries (Beighton 2005). Virulence factors associated with cariogenicity of S. mutans include adherence to tooth surface (Stenudd et al. 2001), acid production through sugar fermentation (Hamada et al. 1984), polysaccharide synthesis (Rölla 1989), and tenacious biofilm formation (Marsh 2010).
Fluoride is an effective cariostatic agent (Featherstone 2009). The caries-preventive effect of fluoride is mainly attributed to the effect of demineralization/remineralization activities of dental enamel following the acid challenge (ten Cate 2004). Besides, it directly reduces bacterial enzyme enolase, leading to glucose uptake decrease and, finally, less glycosis and polysaccharide synthesis (Featherstone 2000). Application of fluoride in oral hygiene product is believed to be the main reason for the substantial decline of dental caries incidence in many industrial countries (Marthaler 2004). However, excessive fluoride may cause side effects such as fluorosis, leading to its limited use for public health (Featherstone 1999). Other caries prevention methods include replacement of sucrose with artificial sweeteners (Hayes 2001), anti-plaque, or antibacterial agents (Slot et al. 2011), and vaccine (Michalek et al. 2001). These methods have all achieved success to various extents, but each possesses innate limitations. Therefore, the development of alternative agents with cariostatic property and minimal adverse effects is promising.
Chemotherapeutic agents from natural products, which may be potentially active against cariogenic organisms, have been of great interest to researchers over the past years. At present, many natural products with cariostatic potential have been identified, such as Nidus Vespae (Xiao et al. 2007), Psoralea corylifoli (Katsura et al. 2001), cranberry (Duarte et al. 2006), and Oolong tea (Nakahara et al. 1993). However, most of those studies were carried out on crude extracts, so determination of active ingredients is regarded as a bottleneck of further research (Jeon et al. 2011). Instead of investigating the inhibitory effect of crude extracts from natural products, our group has been focused on the anticariogenic properties of purified natural compounds (Xu et al. 2011a, b; Guan et al. 2012).
Ginkgo biloba has been extensively used in traditional Chinese medicine, and currently, it is one of the most sold and most studied medicinal plants. Ginkgolic acids represent a major group of components found in extracts of Ginkgo leaves or seed coats, and they are a mixture of structurally related n-alkylphenolic acid, whose structural formula has been identified (Fig. 1). Ginkgolic acids are known to have a number of pharmacological effects, including antitumor (Zhou et al. 2010), antidepressant (Kalkunte et al. 2007), and antimicrobial properties (Wu et al. 2003). Ginkgolic acids are considered to be the main antimicrobial ingredients in G. biloba (Choi and Jeong 2009). Four main components of ginkgolic acids (ginkgoneolic acid, ginkgoic acid, hydroginkgoic acid, and hydroginkgolinic acid), particularly ginkgoneolic acid (C13:0), are proven to be effective antibacterial substances (Wu et al. 2003). Considering the bacterial etiology of dental caries, we hypothesized that ginkgoneolic acid might be useful as a potential preventive and therapeutic agent for this disease. Specifically, we aimed to investigate the effects of ginkgoneolic acid against the virulence factors of S. mutans, including acid production, adherence, biofilm formation, and biofilm morphology.
Materials and methods
Chemicals, test bacterium, and growth conditions
Test agent ginkgoneolic acid was commercially obtained from the National Institute for the Control of Pharmaceutical and Biological Products, Beijing, China. Other chemicals, unless otherwise stated, were purchased from Sigma-Aldrich Corp. (Saint Louis, MO, USA). To prepare stock solution, 2,560 μg of ginkgoneolic acid was dissolved in 0.3 mL dimethyl sulfoxide (DMSO), and 0.98 mL phosphate-buffered saline (PBS; pH 7.2) was added to get the final concentration of 2,000 μg/mL. The stock solution was sterilized by filtration through a 0.22-μm filter and protected from light at −4 °C.
Test bacterium S. mutans ATCC 25175 was grown in brain–heart infusion (BHI) broth at 37 °C under anaerobic conditions (20 % CO2 and 80 % N2). The number of colony-forming units (CFUs) was adjusted to obtain a final concentration of approximately 1 × 108 CFU/mL according to nephelometric measurements (Crystal SpecTM, Becton Dickinson and Company, USA).
MIC and MBC
Minimum inhibitory concentration (MIC) and minimum bactericidal concentration (MBC) of ginkgoneolic acid against S. mutans were determined by liquid medium twofold dilution method, as described previously (Xu et al. 2011b). BHI broth containing DMSO (0.1875 %, v/v) was used as a solvent control and run simultaneously to control for the possible growth inhibition caused by the added DMSO. Chlorhexidine (0.05 %, w/v) was used as a positive control, and BHI broth was used as a blank control.
Time–kill assay
The kinetics of the bacterial-killing effect of ginkgoneolic acid against S. mutans was investigated with the modified method from that of Koo et al. (2002). Tubes containing S. mutans suspension (5 × 107 CFU/mL, final concentration) and ginkgoneolic acid (2 and 4 μg/mL, final concentration) were incubated. Samples were removed for counting colonies at 0, 5, 10, 15, 30, and 60 min, serially diluted with PBS, and aliquots (5 μL) were incubated into BHI agar. The plates were incubated, and CFUs were counted. A bactericidal effect was defined as a more than 3-log CFU/mL decrease from the original inoculum.
Effect on acid production
The effect of ginkgoneolic acid on acidogenicity of S. mutans was examined by a standard pH drop. Bacteria were grown in BHI broth (with 1 % glucose) containing test agent at concentrations of 1/8 MIC, 1/4 MIC, and 1/2 MIC. The starting concentration of bacterial suspension was 5.0 × 107 CFU/mL, and the starting pH of the mixtures was adjusted to 7.4 with 0.1 mol/L KOH solution. The decrease in pH was monitored at intervals over a period of 60 min by means of the pH meter (model 710 A, Orion).
Effect on adherence
A volunteer was recruited among the students in West China School of Stomatology, Sichuan University, and signed a consent for stimulated saliva collection. Saliva was collected and processed as described by Xiao et al. (2007). Hydroxyapatite beads (4 mg; BDH Chemical Ltd., Poole, England) were delivered into 0.5-mL polypropylene centrifuge tubes and equilibrated overnight at 4 °C with 120 μL of buffered KCl (0.05 mol/L KCl, 1 mmol/L KH2PO4, 1 mmol/L CaCl2, 0.1 mmol/L MgCl2, pH 6.0). The buffer was aspirated, and hydroxyapatite beads were coated with 120 μL of saliva for 1 h at room temperature, with continuous inversion. Saliva was aspirated, and the saliva-treated hydroxyapatite (S-HA) beads were washed three times with buffer. S-HA was further treated with buffered KCl (120 μL) containing 5 mg/mL bovine serum albumin for 30 min and then rewashed three times. The inhibitory effect of ginkgoneolic acid on the adherence of S. mutans to S-HA was investigated by means of modifying the method described by Clark et al. (1978). Tubes containing radiolabeled bacterial suspension (3 H-TdR, Chinese Academy of Science, Shanghai Institute of Atomic Nucleus; 5 × 107 CFU/mL, final concentration), ginkgoneolic acid (1/8 MIC, 1/4 MIC, and 1/2 MIC, final concentration), and S-HA were continuously inverted at room temperature for 60 min, and then, the beads were washed three times with buffered KCl. The bacteria-associated radioactivity of the beads was counted by direct scintillation counting. Buffered KCl was used as the blank control, DMSO (0.024 %, v/v) as solvent control, and chlorhexidine (0.05 %) as positive control.
Effect on biofilm formation
Minimum biofilm inhibition concentration (MBIC50) was used to describe effects of ginkgoneolic acid on S. mutans biofilm formation. A twofold serial dilution of ginkgoneolic acid (110 μL/well) was prepared in 96-well polystyrene tissue culture plates with concentrations ranging from 0.25 to 64 μg/mL. Aliquots of the bacteria cell suspension (5 × 105 CFU/mL, final concentration) were inoculated into the wells. Except for solvent control, blank control, and positive control, BHI broth without bacteria incubation taken as media control was run simultaneously. After incubation at 37 °C for 24 h, absorbance at 595 nm was recorded to assess the culture growth. The supernatants from the wells were decanted, and planktonic cells were removed by washing with PBS (pH 7.2) three times. Biofilm was fixed with methanol (15 min), air dried at room temperature, stained with 0.1 % (w/v) crystal violet for 5 min, and rinsed thoroughly with PBS until medium control wells were colorless. Two hundred microliters of 95 % ethanol was added to each crystal violet-stained well. The plate was rocked at room temperature for 30 min, and the absorbance at 595 nm (A595) was determined. The percentage of inhibition was calculated using the equation: (A595 of blank control − A595 of the test group) / A595 of blank control × 100 %. MBIC50 was defined as the lowest agent concentration that showed 50 % or more inhibition of biofilm formation.
Developed biofilm reduction assay
To examine the reduction effects of ginkgoneolic acid on the 1-day-developed biofilm, bacterial suspensions (220 μL aliquots, 5 × 105 CFU/mL, final concentration) were inoculated into the wells of a 96-well polystyrene tissue culture plate and incubated for 24 h. The supernatant from each well was decanted, and planktonic cells were removed by washing with PBS. Fresh BHI broth containing ginkgoneolic acid (0.125 to 32 μg/mL) was transferred into the 24-h biofilm plate (220 μL/well), and then, the plate was incubated. Cell growth was assessed by measurement of absorbance at 595 nm. Similarly, the biofilm was fixed, air dried, stained, washed, and quantified as described above. The lowest concentration that showed reduction of the biofilm by 50 % or more was defined as MBRC50.
Effect on biofilm morphology
Hydroxyapatite discs obtained from the Engineering Research Center in Biomaterials, Sichuan University, (5 mm in diameter and 2 mm in thickness) were prefixed in 24-well polystyrene tissue culture plates vertically and coated with 2.3 mL of human saliva sterilized by filtration through a 0.22-μm filter for 1 h at room temperature. The saliva was aspirated, and hydroxyapatite discs were washed three times with saline. Aliquots (2.3 mL) of S. mutans suspension were inoculated into each well (5 × 105 CFU/mL) and incubated at 37 °C. At 24, 36, 48, 60, 72, 86, 96, and 108 h, supernatant from each well was aspirated, and hydroxyapatite discs were immersed first in saline for 1 min, then in ginkgoneolic acid solution (4, 8, and 16 μg/mL) for 5 min, and in saline again for 1 min. The procedure described above was repeated three times at each time point. Fresh broth was added into to each well. At 120 h, hydroxyapatite discs were washed with saline three times, fixed with 2.5 % glutaraldehyde for 2 h at room temperature, dehydrated using ascending-graded ethanol (30, 50, 70, 80, 90, and 100 %), and coated with gold. The samples were observed by means of SEM (KYKY 2800B; China Technical Instruments Inc., Beijing, China).
Statistical analysis
Intergroup differences were estimated by statistical one-way analysis of variance. The chosen level of significance for all statistical tests in the present study was p < 0.05, and statistical computation was performed using the SPSS 17.0 software (SPSS Incorporated, Chicago, IL, USA).
Results
Ginkgoneolic acid exhibits bactericidal effect against S. mutans
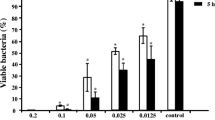
To evaluate its antimicrobial activity, the MIC and MBC of ginkgoneolic acid against S. mutans were determined. Ginkgoneolic acid inhibited growth of planktonic S. mutans at a MIC of 4 μg/mL and MBC of 8 μg/mL. The kinetics of the antimicrobial effect of ginkgoneolic acid against S. mutans is demonstrated in Fig. 2. Ginkgoneolic acid killed S. mutans in a time- and dosage-dependent manner. Ginkgoneolic acid at 4 μg/mL showed bactericidal activity against S. mutans, with a more than 6-log CFU/mL decrease after 10 min of incubation. However, the addition of 2 μg/mL (1/2 MIC) of ginkgoneolic acid to the S. mutans cell cultures had no effect on the viable counts over a 60-min incubation period. Bactericidal capacity of ginkgoneolic acid at a concentration of 4 μg/mL was comparable to that of 0.05 % chlorhexidine.
Kinetic killing effect of ginkgoneolic acid on S. mutans planktonic cell cultures. The bactericidal activity of ginkgoneolic acid at concentrations of 4 μg/mL (MIC) and 2 μg/mL (1/2 MIC) was tested. BHI broth, chlorhexidine (0.05 %, w/v) and DMSO (0.05 %, v/v) were used as blank control, positive control, and solvent control, respectively
Ginkgoneolic acid reduces acid production of S. mutans in planktonic culture
The effect of ginkgoneolic acid on the acid production of S. mutans was determined by monitoring the glycolytic pH drop of cultures. As shown in Fig. 3, incubation of S. mutans in sub-inhibitory concentrations of ginkgoneolic acid (1/2 MIC, 2 μg/mL) exhibited an attenuation in acid production. Also, this inhibitory effect was time and dosage dependent. Ginkgoneolic acid had effect on acid production up to 30 min and only at the highest concentration tested.
Effect of ginkgoneolic acid on the acid production of S. mutans. The inhibitory effect of ginkgoneolic acid at concentrations of 2 μg/mL (1/2 MIC), 1 μg/mL (1/4 MIC), and 0.25 μg/mL (1/8 MIC) on the acid production of S. mutans was investigated. BHI broth was used as blank control, chlorhexidine (0.05 %, w/v) as positive control, and DMSO (0.024 %, v/v) as solvent control. An asterisk indicates statistically significant difference between 1/2 MIC (2 μg/mL) of ginkgoneolic acid-treated group and solvent control at different time points (p < 0.05)
Ginkgoneolic acid disrupts cellular adherence
Ginkgoneolic acid suppressed the adherence of S. mutans to S-HA (Table 1). When radiolabeled S. mutans were treated with ginkgoneolic acid at a concentration of 2 μg/mL for 1 h, a significant inhibition in bacterial adherence to the S-HA was observed (p < 0.05), and ginkgoneolic acid (2 μg/mL) showed similar inhibitory effect as 0.05 % chlorhexidine (p > 0.05). Ginkgoneolic acid at a concentrations less than 2 μg/mL did not exhibit inhibitory effect on bacterial adherence (p > 0.05).
S. mutans biofilm is susceptible to ginkgoneolic acid
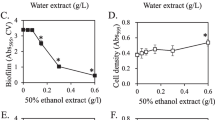
Ginkgoneolic acid inhibited 50 % or more (95.5 ± 4.2 %) of S. mutans biofilm formation at a concentration of 4 μg/mL (MBIC50 = 4 μg/mL). Meanwhile, 32 μg/mL of ginkgoneolic acid reduced 50 % or more (80.5 ± 5.7 %) of 1-day-developed S. mutans biofilm (MBRC50 = 32 μg/mL). The test agent at concentrations lower than the MBRC50 also disrupted the integrity of the S. mutans biofilm effectively, according to morphology alteration of S. mutans biofilm treated with ginkgoneolic acid observed under SEM (Fig. 4). Thick and relatively homogeneous biofilm was formed on S-HA in blank control and solvent control, suggesting that a small amount of DMSO had no significant effect on biofilm morphology. Compared to these untreated groups, biofilm integrity was disrupted when treated with 8 and 16 μg/mL of ginkgoneolic acid. Particularly, only a few scattered bacteria could be seen, and the chain of S. mutans was shorter when treated with 16 μg/mL of the test agent.
Discussion
Oral microorganisms cause caries through their carbohydrate metabolites, which destroy dental hard tissue and dissemble organic substance, thus resulting in tooth damage. Mutans streptococci, Lactobacillus, and Actinomyces have long been proven to be pathogens of dental decay. Among them, much research has suggested that S. mutans is the major pathogen of human dental caries (Beighton 2005). Reasons include the following: first, this organism is highly acidogenic and aciduric; second, S. mutans has a high affinity to enamel; and third, it produces water-insoluble glucan promoting bacterial adherence to the tooth surface and dental plaque formation. So, S. mutans and single-species biofilm model of this bacterium have been used widely to investigate the cariostatic potential of natural products (Yoo et al. 2011; Brighenti et al. 2008; Limsong et al. 2004).
After colonization, growth capacity became a key pathogenic determinant in causing tooth infection because small amounts of bacteria are easily cleared by the body’s defense system. We evaluated in vitro the antimicrobial activities of ginkgoneolic acid against S. mutans, and it showed bactericidal effects at a relatively low concentration (4 μg/mL). Normally, gram-negative bacteria are more susceptible to antimicrobial agents than gram-positive bacteria; however, MICs and MBCs of ginkgoneolic acid against some gram-negative bacteria associated with periodontal diseases were higher than that of cariogenic bacteria (data not shown). Some researchers postulated that the difference in the cell wall between gram-positive and gram-negative bacteria may be responsible for this phenomenon (Yang et al. 2004).
The production of acid by cariogenic bacteria and the subsequent environmental pH decrease contribute to the demineralization of the tooth surface and formation of dental caries (Leme et al. 2006). Therefore, reduction of bacterial acid production is a logical approach to the prevention of dental caries. We found in this study that 0.05 % chlorhexidine reduced the acid production of S. mutans by nearly 100 % after 10 min of incubation. This inhibitory effect on acid production is attributed to the bactericidal activity of chlorhexidine at this applied concentration (Fig. 2). However, our findings that ginkgoneolic acid significantly inhibited acid production without reducing the number of S. mutans suggest that this agent may suppress the acidogenicity of bacteria by a mechanism distinct from that of chlorhexidine.
Adherence is the initial step for biofilm formation. The interference of bacterial adherence on tooth surface is a promising approach to control oral biofilm (Gibbons 1989). In the present study, ginkgoneolic acid showed inhibitory activity on the adherence of S. mutans at a concentration of 2 μg/mL. Two mechanisms may be involved: reducing the number of viable bacteria and interfering with bacterial adherence process. It was verified that the viable cell counts of the culture incubated with ginkgoneolic acid within 1 h were not less than that of the untreated groups. Therefore, ginkgoneolic acid may interfere with bacterial adherence process. The adherence process of bacteria to solid surface is complicated, involving interactions between surface components of microorganisms and the solid surface, so further experimental studies are required for elucidation on the exact mechanism.
Bacteria in most environments form organized communities called biofilm, in which aggregated cells are embedded in a hydrated matrix of extracellular polymeric substances (Costerton et al. 1999; Donlan and Costerton 2002; Hoiby et al. 2011). Caries is a chronic disease linked to biofilm formation. Because of slow growth (Desai et al. 1998), activation of stress response (Cochran et al. 2000), induction of biofilm phenotype (Kuchma and O’Toole 2000), or other aspects of biofilm architecture, when cells exist in a biofilm, they can become 10–1,000 times more tolerant to the effects of antimicrobial agents (Prosser et al. 1987; Nickel et al. 1985). Consequently, using MIC and MBC alone, it is difficult to estimate the effects of drugs on bacteria. The authors also found that the test agent at a concentration of 8 μg/mL killed all the planktonic cells but did not exhibit more than 50 % reduction of S. mutans biofilm. MBIC50 and MBRC50 are used to evaluate the effects of drugs on biofilm in recent years. In present the study, ginkgoneolic acid inhibited biofilm formation and reduced developed biofilm effectively at a low concentration. The biofilm-forming potential of a strain depends on its growth and adherence capacity, that is, the more a strain grows and adheres to solid surfaces, the better it forms a biofilm. These data, in conjunction with data on adherence and antimicrobial activity, suggest that the inhibition or reduction of the biofilm might result from anti-adherence and antimicrobial activities.
In conclusion, our data demonstrated that ginkgoneolic acid showed inhibitory effect on growth, adherence, acid production, and biofilm formation of S. mutans, reduced early biofilm, and disrupted biofilm integrity. These data suggest that ginkgoneolic acid might be a potential preventive and therapeutic agent in dental caries. However, it should be more realistic in places in terms of the potential value of ginkgoneolic acid in oral care products. First, the present study has only been performed on a single strain of S. mutans and single-species biofilm, and the effects of ginkgoneolic acid on other putative pathogens (even some of the beneficial bacteria) and multiple-species biofilm should be investigated. Second, when delivered to the mouth, a key property of antimicrobial agents is their “substantivity” (the prolonged association between a material and a substrate) (Carrilho et al. 2010); otherwise, they are rapidly swallowed and lost. Natural products displayed some potentially beneficial properties when tested under ideal conditions (fixed concentration, long contact times) but often rapidly lost activity when tested at a reduced concentration. So, experiments investigating the substantivity of ginkgoneolic acid are important to evaluate the potential of ginkgoneolic acid in caries prevention.
References
Beighton D (2005) The complex oral microflora of high-risk individuals and groups and its role in the caries process. Community Dent Oral Epidemiol 33:248–255
Brighenti FL, Luppens SBI, Delbem ACB, Deng DM, Hoogenkamp MA, Gaetti-Jardim E Jr, Dekker HL, Crielaard W, ten Cate JM (2008) Effect of Psidium cattleianum leaf extract on Streptococcus mutans viability, protein expression and acid Production. Caries Res 42:148–154
Carrilho MR, Carvalho RM, Sousa EN, Nicolau J, Breschi L, Mazzoni A, Tjäderhane L, Tay FR, Agee K, Pashley DH (2010) Substantivity of chlorhexidine to human dentin. Dent Mater 26:779–785
Choi JG, Jeong SI (2009) Antibacterial activity of hydroxyl alkenyl salicylic acids from sarcotesta of Ginkgo biloba against vancomycin-resistant Enterococcus. Fitoterapia 80:1820–1883
Clark WB, Bammann LL, Gibbons RJ (1978) Comparative estimates of bacterial affinities and adsorption sites on hydroxyapatite surfaces. Infect Immun 19:846–853
Cochran WL, Suh SJ, McFeters GA, Stewart PS (2000) Role of RpoS and AlgT in Pseudomonas aeruginosa biofilm resistance to hydrogen peroxide and monochloramine. J Appl Microbiol 88:546–553
Costerton JW, Stewart PS, Greenberg EP (1999) Bacterial biofilms: a common cause of persistent infections. Science 284:1318–1322
Desai M, Bühler T, Weller PH, Brown MR (1998) Increasing resistance of planktonic and biofilm cultures of Burkholderia cepacia to ciprofloxacin and ceftazidime during exponential growth. J Antimicrob Chemother 42:153–160
Donlan RM, Costerton JW (2002) Biofilms: survival mechanisms of clinically relevant microorganisms. Clin Microbiol Rev 15:167–193
Duarte S, Gregoire S, Singh AP, Vorsa N, Schaich K, Bowen WH, Koo H (2006) Inhibitory effects of cranberry polyphenols on formation and acidogenicity of Streptococcus mutans biofilms. FEMS Microbiol Lett 257:50–56
Featherstone JDB (1999) Prevention and reversal of dental caries: role of low level fluoride. Community Dent Oral Epidemiol 27:31–40
Featherstone JDB (2000) The science and practice of caries prevention. J Am Dent Assoc 131:887–899
Featherstone JDB (2009) Remineralization, the natural caries repair process—the need for new approaches. Adv Dent Res 21:4–7
Gibbons RJ (1989) Bacterial adhesion to oral tissues: a model for infectious diseases. J Dent Res 68:750–760
Guan X, Zhou Y, Liang X, Xiao J, He L, Li J (2012) Effects of compounds found in Nidus Vespae on the growth and cariogenic virulence factors of Streptococcus mutans. Microbiol Res 167:61–68
Hamada S, Koga T, Ooshima T (1984) Virulence factors of Streptococcus mutans and dental caries prevention. J Dent Res 63:407–411
Hayes C (2001) The effect of non-cariogenic sweeteners on the prevention of dental caries: a review of the evidence. J Dent Educ 65:1106–1109
Hoiby N, Ciofu O, Johansen HK, Song ZJ, Moser C, Jensen PO, Molin S, Givskov M, Tolker-Nielsen T, Bjarnsholt T (2011) The clinical impact of bacterial biofilms. Int J Oral Sci 3:55–65
Jeon JG, Rosalen PL, Falsetta ML, Koo H (2011) Natural products in caries research: current (limited) knowledge, challenges and future perspective. Caries Res 45:243–263
Kalkunte SS, Singh AP, Chaves FC, Gianfagna TJ, Pundir VS, Jaiswal AK, Vorsa N, Sharma S (2007) Antidepressant and antistress activity of GC-MS characterized lipophilic extracts of Ginkgo biloba leaves. Phytother Res 21:1061–1065
Katsura H, Tsukiyama R-I, Suzuki A, Kobayashi M (2001) In vitro antimicrobial activities of bakuchiol against oral microorganisms. Antimicrob Agents Chemother 45:3009–3013
Koo H, Rosalen PL, Cury JA, Park YK, Bowen WH (2002) Effects of compounds found in propolis on Streptococcus mutans growth and on glucosyltransferase activity. Antimicrob Agents Chemother 46:1302–1309
Kuchma SL, O’Toole GA (2000) Surface-induced and biofilm-induced changes in gene expression. Curr Opin Biotechnol 1:429–433
Leme AFP, Koo H, Bellato CM, Bedi G, Cury JA (2006) The role of sucrose in cariogenic dental biofilm formation—new insight. J Dent Res 85:878–887
Limsong J, Benjavongkulchai E, Kuvatanasuchati J (2004) Inhibitory effect of some herbal extracts on adherence of Streptococcus mutans. J Ethnopharmacol 92:281–289
Marsh PD (2010) Microbiology of dental plaque biofilms and their role in oral health and caries. Dent Clin N Am 54:441–454
Marthaler TM (2004) Changes in dental caries 1953–2003. Caries Res 38:173–181
Michalek SM, Katz J, Childers NK (2001) A vaccine against dental caries: an overview. BioDrugs 15:501–508
Nakahara K, Kawabata S, Ono H, Ogura K, Tanaka T, Ooshima T, Hamada S (1993) Inhibitory effect of oolong tea polyphenols on glycosyltransferases of mutans Streptococci. Appl Environ Microbiol 59:968–973
Nickel JC, Ruseska I, Wright JB, Costerton JW (1985) Tobramycin resistance of Pseudomonas aeruginosa cells growing as a biofilm on urinary catheter material. Antimicrob Agents Chemother 27:619–624
Prosser BL, Taylor D, Dix BA, Cleeland R (1987) Method of evaluating effects of antibiotics on bacterial biofilm. Antimicrob Agents Chemother 31:1502–1506
Rölla G (1989) Why is sucrose so cariogenic? The role of glucosyltransferase and polysaccharides. Eur J Oral Sci 97:115–119
Selwitz RH, Ismail AI, Pitts NB (2007) Dental caries. Lancet 369:51–59
Slot DE, Vaandrager NC, Van Loveren C, Van Palenstein Helderman WH, Van der Weijden GA (2011) The effect of chlorhexidine varnish on root caries: a systematic review. Caries Res 45:162–173
Stenudd C, Nordlund A, Ryberg M, Johansson I, KallestÅl C, Strömberg N (2001) The association of bacterial adhesion with dental caries. J Dent Res 80:2005–2010
ten Cate JM (2004) Fluorides in caries prevention and control: empiricism or science. Caries Res 38:254–257
Wu X, Yang L, Chen J, Yuan X, Xia G (2003) Preparation of ginkgolic acid monomers and their antifungal activity. Chem Ind For Prod 23:17–21
Xiao J, Zuo Y, Liu Y, Li J, Hao Y, Zhou X (2007) Effects of Nidus Vespae extract and chemical fractions on glucosyltransferases, adherence and biofilm formation of Streptococcus mutans. Arch Oral Biol 52:869–875
Xu X, Zhou XD, Wu CD (2011a) Tea catechin epigallocatechin gallate inhibits Streptococcus mutans biofilm formation by suppressing gtf genes. Arch Oral Biol. doi:10.1016/j.archoralbio.2011.10.021
Xu X, Zhou XD, Wu CD (2011b) The tea catechin epigallocatechin gallate suppresses cariogenic virulence factors of Streptococcus mutans. Antimicrob Agents Chemother 55:1229–1236
Yang XM, Zhu W, Chen J, Qian ZY, Xie JM (2004) Study on anti-bacterium activity of ginkgolic acids and their momomers. Zhong Yao Cai 27:661–663
Yoo S, Murata RM, Duarte S (2011) Antimicrobial traits of tea- and cranberry-derived polyphenols against Streptococcus mutans. Caries Res 45:327–335
Zhou C, Li X, Du W, Feng Y, Kong X, Li Y, Xiao L, Zhang P (2010) Antitumor effects of ginkgolic acid in human cancer cell occur via cell cycle arrest and decrease the Bcl-2/Bax ratio to induce apoptosis. Chemotherapy 56:393–402
Acknowledgments
The authors are grateful to the State Key Laboratory of Oral Diseases of Sichuan University for kindly providing the microorganisms and technical assistance, to Dr. Jing Xue for the critical assessment, and to the anonymous reviewers for their comments on the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
He, J., Wang, S., Wu, T. et al. Effects of ginkgoneolic acid on the growth, acidogenicity, adherence, and biofilm of Streptococcus mutans in vitro. Folia Microbiol 58, 147–153 (2013). https://doi.org/10.1007/s12223-012-0191-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12223-012-0191-9