Abstract
The poor prognosis of adults with B cell precursor acute lymphoblastic leukemia (BCP-ALL) is attributed to leukemia cells that are protected by the bone marrow (BM) microenvironment. In the present study, we explored the pharmacological targeting of mesenchymal stromal/stem cells in BM (BM-MSCs) to eliminate chemoresistant BCP-ALL cells. Human BCP-ALL cells (NALM-6 cells) that adhered to human BM-MSCs (NALM-6/Ad) were highly resistant to multiple anti-cancer drugs, and exhibited pro-survival characteristics, such as an enhanced Akt/Bcl-2 pathway and increased populations in the G0 and G2/S/M cell cycle stages. Bortezomib, a proteasome inhibitor, interfered with adhesion between BM-MSCs and NALM-6 cells and up-regulated the matricellular protein SPARC (secreted protein acidic and rich in cysteine) in BM-MSCs, thereby reducing the NALM-6/Ad population. Inhibition of SPARC expression in BM-MSCs using a small interfering RNA enhanced adhesion of NALM-6 cells. Conversely, recombinant SPARC protein interfered with adhesion of NALM-6 cells. These results suggest that SPARC disrupts adhesion between BM-MSCs and NALM-6 cells. Co-treatment with bortezomib and doxorubicin prolonged the survival of BCP-ALL xenograft mice, with a significant reduction of leukemia cells in BM. Our findings demonstrate that bortezomib contributes to the elimination of BCP-ALL cells through disruption of their adhesion to BM-MSCs, and offer a novel therapeutic strategy for BCP-ALL through targeting of BM-MSCs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adult B cell precursor acute lymphoblastic leukemia (BCP-ALL) belongs to an entity of intractable hematological diseases. Although remission rates for newly diagnosed adult patients with BCP-ALL are >80% with standard induction regimens, approximately half of them eventually experience relapse with 5-year overall survival of about 50% [1]. Dose-intensified chemotherapies that follow pediatric treatment protocols improve outcomes in young adult patients [2]. However, the prognosis is still poor and therapy-related death is an important problem in aged patients [3]. In addition, the benefits of hematopoietic stem cell transplantation are limited to a subset of patients [4]. Therefore, a novel therapeutic strategy needs to be sought to overcome the current clinical situation in the treatment of adult patients with BCP-ALL.
The poor outcomes of patients with BCP-ALL are related to the existence of chemoresistant leukemia cells in bone marrow (BM) [5]. Several lines of evidence suggest that this is largely due to the protection of leukemia cells through soluble mediators or cell adhesion provided by various components of the BM microenvironment, particularly BM mesenchymal stromal/stem cells (BM-MSCs) [6,7,8]. Multiple factors are involved in the protection of BCP-ALL cells by BM-MSCs. For example, CXCL12 that is secreted by BM-MSCs promotes the proliferation of BCP-ALL cells [9, 10]. The activated Wnt signaling pathway in BCP-ALL cells is involved in BM-MSC-mediated drug resistance [11]. However, the contribution of cell adhesion in the cross-talk between BCP-ALL cells and BM-MSCs to drug resistance is not well known.
In this study, we determined the effects of adhesion to BM-MSCs on the drug resistance of BCP-ALL cells and the rationale of disrupting adhesion of BCP-ALL cells to BM-MSCs. Our results indicated that pharmacological treatment of BM-MSCs with a proteasome inhibitor, bortezomib (Bor), interfered with the adhesion of BCP-ALL cells to BM-MSCs. Combination therapy with Bor and doxorubicin consequently contributed to a reduction of leukemia cells in BM of xenograft model mice. An important finding was that the anti-adhesive matricellular protein secreted protein acidic and rich in cysteine (SPARC) was up-regulated in BM-MSCs by Bor and was functionally involved in the interference of adhesion of BCP-ALL cells to BM-MSCs.
Materials and methods
Reagents, antibodies, and cells
Recombinant human SPARC (rhSPARC) and doxorubicin hydrochloride (DXR) were purchased from Wako Pure Chemical Industries (Osaka, Japan). Methotrexate hydrate (MTX) and cytosine β-d-arabinofuranoside (AraC) were purchased from Sigma-Aldrich (St. Louis, MO, USA). Bor was a product of Millennium (Cambridge, MA, USA). Carfilzomib (Car) and oprozomib (Opr) were purchased from Active Biochemicals (Hong Kong, China). NALM-6 cells were purchased from ATCC (Manassas, VA, USA). Human BM samples from individuals with BCP-ALL were purchased from Lonza (Basel, Switzerland) or were obtained with informed consent and the approval of the ethical committee of Kyoto University Hospital. The antibodies used are listed in Supplementary Table 1.
Culture of human BM-MSCs
Human BM-MSCs were isolated from BM samples of healthy adults purchased from AllCells (Emeryville, CA, USA) based on our previously published method. A single-cell suspension of 1 × 106 BM mononuclear cells was seeded into 15 cm culture dishes, and adherent cells were cultured in advanced-minimal essential medium (Invitrogen, Carlsbad, CA, USA) supplemented with 5% fetal bovine serum (FBS, Gibco, Carlsbad, CA, USA), 100 µM ascorbic acid (Wako Pure Chemicals Industries), 2 mM l-glutamine, 100 U/mL penicillin, and 100 µg/mL streptomycin (all from Gibco) (aMEM-based complete medium). The medium was changed on day 7 and day 14. Primary cultures were passaged to disperse the colony-forming cells (passage 1). Cells at passage 3 were used as BM-MSCs in this study. Prior to experiments, flow cytometric analysis was performed to confirm that these cells were positive for the mesenchymal stromal/stem cell-associated markers CD105, CD73, CD90, CD146, CD44, CD166 and were negative for the hematopoietic/endothelial cell-associated markers CD45, CD34, CD14, CD19, CD31, HLA-DR (Supplementary Fig. 1A). In addition, in vitro osteogenic, adipogenic, and chondrogenic differentiation assays and in vivo bone formation and hematopoietic induction assays were performed to confirm that these cells have multilineage differentiation capability and hematopoiesis-supportive capability (Supplementary Fig. 1B–E).
Co-culture of NALM-6 cells with BM-MSCs
Human BM-MSCs were prepared in a 10 cm culture dish or a 6-well culture plate. Twenty-four hours later, NALM-6 cells were added onto these BM-MSCs and co-cultured in RPMI 1640 (Wako Pure Chemical Industries) supplemented with 10% heat-inactivated fetal bovine serum (FBS, HyClone, Logan, UT), 2 mM l-glutamine, 100 U/mL penicillin, and 100 µg/mL streptomycin (all from Gibco) (RPMI-based complete medium). In some experiments, BM-MSCs were pretreated with Bor or other reagents before adding NALM-6 cells. Suspension cells were transferred to a tube and the remaining suspension cells in the culture dish/plate were carefully transferred to the same tube by gently pipetting with phosphate-buffered saline (PBS) twice. For flow cytometric analysis, these suspension cell fractions were washed twice with FACS buffer (2% FBS prepared in PBS), incubated with a phycoerythrin-conjugated mouse antibody against human CD19 and a fluorescein isothiocyanate-conjugated mouse antibody against human CD90 at 4 °C for 30 min, and analyzed with FACSCantoII (Becton–Dickinson, Franklin Lakes, NJ, USA) to determine the proportions of NALM-6 cells (CD19+) and BM-MSCs (CD90+) separately. Adherent cells on a dish/plate were treated with 0.05% trypsin–EDTA (Gibco) to disperse them and subjected to flow cytometric analysis in a similar manner as described for suspension cells. The suspension cells and adherent cells were applied to anti-human CD19 immunomagnetic microbeads (Miltenyi Biotec, Bergisch Gladbach, Germany) to purify NALM-6 cells in order to investigate their protein expression by immunoblot analysis or their cell cycle status by flow cytometric analysis.
Pretreatment of BM-MSCs with Bor, Car, Opr, and rhSPARC
BM-MSCs (2 × 105 cells) were prepared in aMEM-based complete medium in a 10 cm culture dish. Twenty-four hours later, the media were replaced with aMEM-based complete medium containing Bor or other proteasome inhibitors, and BM-MSCs were pretreated with these drugs for 1 or 4 h (transient exposure) or 24 h (continuous exposure) at the following concentrations: 10 nM Bor, 3 nM Car, or 10 nM Opr for 24 h; 100 nM Bor or 100 nM Car for 1 h; and 300 nM Opr for 4 h. After the pretreatment, the media were removed and the dish was washed with PBS twice. NALM-6 cells (5 × 105 cells) were added onto the pretreated BM-MSCs and co-cultured in RPMI-based complete medium. For pretreatment with rhSPARC, BM-MSCs were prepared at a density of 0.8 × 105 cells/well in a 6-well culture plate, pretreated with 200 ng/mL rhSPARC for 24 h, and co-cultured with NALM-6 cells at a density of 3 × 105 cells/well. Twelve hours later, suspension cells and adherent cells were collected as described above for further analysis.
Small interfering RNA (siRNA)-mediated knockdown of SPARC in BM-MSCs
Lipofectamine RNAiMax (Invitrogen) was used to transfect BM-MSCs with SPARC-targeting siRNA according to the manufacturer’s instructions. Lipofectamine RNAiMax (5 µL) was combined with 30 pmol of siRNA in 500 µL of Opti-MEM media (Gibco) and incubated for 20 min at room temperature. The mixture was then added directly to BM-MSCs in culture, and cells were incubated for 36 h. siRNAs targeting SPARC were purchased from Invitrogen (Stealth RNAi). The siRNA sequences (5′–3′) were as follows: GGAAGAAACUGUGGCAGAGGUGACU and AGUCACCUCUGCCACAGUUUCUUCC. The Stealth RNAi Negative Control Low GC Duplex (Invitrogen) was used as a negative control. These siRNA-treated BM-MSCs were co-cultured with NALM-6 cells.
Culture of NALM-6 cells on rhSPARC-treated fibronectin-coated dishes
Human Fibronectin Cellware Multiwell and Assay Plates (24 well) (Corning, Corning, NY, USA) were treated with rhSPARC diluted in PBS at a concentration of 500 ng/mL for 24 h at 37 °C. Then, the plates were carefully washed twice with PBS and used to culture NALM-6 cells. After 12 h of culture, the plates were carefully washed twice with PBS to remove suspension cells, and the number of NALM-6 cells that adhered to the bottom of the plates was counted under phase-contrast microscopy.
Co-treatment of NALM-6 cells and BM-MSCs in co-culture with anti-cancer drugs
BM-MSCs (2 × 105 cells) were prepared in aMEM-based complete medium in a 10 cm culture dish. Twenty-four hours later, the media were removed and the dish was washed with PBS twice. NALM-6 cells (5 × 105) were added onto these BM-MSCs and co-cultured in RPMI-based complete medium. Twenty-four hours later, DXR, AraC, or MTX was added to the co-cultures at a final concentration of 200, 500, or 50 nM, respectively. After exposure to these anti-cancer drugs for 12 h, the numbers of NALM-6 cells in suspension cell fractions and adherent cell fractions were counted by flow cytometric analysis as described above.
Growth assay of BM-MSCs treated with proteasome inhibitors
Cell Counting Kit-8 (Dojindo laboratories, Tokyo, Japan) was used according to the manufacturer’s protocol. BM-MSCs were prepared at a density of 1 × 105 cells/mL in a 96-well plate and treated with Bor (0–100 nM), Car (0–100 nM), or Opr (0–300 nM) transiently (1 or 4 h) or continuously (24 h). After exposure to these proteasome inhibitors, the media were removed and the cells were washed twice with PBS and cultured in RPMI-based complete medium. On day 1 or day 2 after cultivation, the relative cell growth was calculated as the ratio of the absorbance of treated cells to the absorbance of non-treated cells. Absorbance was measured at 450 nm using a microplate reader (Molecular Devices, Sunnyvale, CA, USA).
BCP-ALL xenograft model mice
Specific pathogen-free 6–7-week-old male SCID mice (Clea Japan, Tokyo, Japan) received 2 Gy of total body irradiation. Then, NALM-6 cells (1 × 107 cells/mouse) were injected via the tail vein into these mice on the same day. DXR (6 µg/g dissolved in PBS), Bor (0.1 µg/g dissolved in PBS), or PBS (control) was administered to the xenograft model mice via the tail vein on day 28 after NALM-6 cell injection, and the survival of mice was observed every day until day 91. In some experiments, the mice were sacrificed on day 35 and the proportion of NALM-6 cells in the BM was analyzed by flow cytometry. The survival of mice was analyzed using the log-rank test. These studies were approved by the committee for animal research of the Kyoto University Graduate School of Medicine. All methods relating to animals were performed in accordance with the relevant guidelines and regulations.
Statistical analysis
The unpaired Student’s t test was used for analysis, unless otherwise indicated. Data in bar graphs indicate the mean ± standard deviation (SD). Statistical significance is expressed as follows: *, P < 0.05; **, P < 0.01; n.s., not significant.
Results
NALM-6 cells that adhere to BM-MSCs show resistance to anti-cancer drugs
We first determined that BCP-ALL cells exhibited their drug-resistant phenotype through adhesion to human BM-MSCs. When co-cultured with BM-MSCs, human BCP-ALL cells (NALM-6 cells) were prone to adhere to BM-MSCs (Fig. 1a). In this co-culture system (Fig. 1b), the number of NALM-6 cells that were in suspension (NALM-6/Su) and the number of NALM-6 cells that adhered to BM-MSCs (NALM-6/Ad) were evaluated by flow cytometric analysis, in which NALM-6 cells (CD19+) were immunophenotypically distinguished from BM-MSCs (CD90+) (Fig. 1c). To examine the difference in sensitivity to anti-cancer drugs between NALM-6/Su and NALM-6/Ad, DXR, AraC, or MTX was added to this co-culture at a final concentration of 200, 500, or 50 nM, respectively. The number of NALM-6/Su was significantly reduced after 12-h exposure to these anti-cancer drugs compared with the number in non-drug-treated samples (Fig. 2a–c). On the other hand, the number of NALM-6/Ad was not reduced and was not different from the number in non-drug-treated samples (Fig. 2d–f).
Co-culture of NALM-6 cells with BM-MSCs. a A phase-contrast microscopy image of a co-culture of NALM-6 cells with BM-MSCs. NALM-6 cells (red arrows) were prone to adhere to BM-MSCs (blue line). A representative image is shown. Bar 50 μm. b Schema of the co-culture experiment system. NALM-6/Su: NALM-6 cells that are in suspension, NALM-6/Ad: NALM-6 cells that adhere to BM-MSCs, BM-MSCs: bone marrow mesenchymal stromal/stem cells. c Flow cytometric analysis of suspension cells and adherent cells in co-culture. Cells in each fraction were stained with an anti-CD19 antibody and an anti-CD90 antibody to distinguish NALM-6 cells (CD19+CD90−, red square) and BM-MSCs (CD19−CD90+, blue square) from each other
NALM-6 cells that adhere to BM-MSCs show resistance to multiple anti-cancer drugs. a–f The numbers of NALM-6/Su and NALM-6/Ad in co-cultures with BM-MSCs after treatment with DXR (a, d), MTX (b, e), and AraC (c, f). Open bars indicate the numbers of NALM-6 cells that were treated with anti-cancer drugs and closed bars indicate the numbers of NALM-6 cells that were not treated with anti-cancer drugs. g, h Flow cytometric analysis of adherent cells after processing with anti-human CD19 immunomagnetic microbeads. Open histograms indicate the expression levels of CD10 in the positive fraction (g) and CD90 in the negative fraction (h). Filled histograms indicate control staining (g, h). Positive and negative fractions represent ≥99% purity of NALM-6 cells (g, CD10+) and BM-MSCs (h, CD90+), respectively. Representative histograms are shown. i, j Immunoblot analysis showing the expression of Bcl-2 in NALM-6/Su and NALM-6/Ad before DXR treatment. Glyceraldehyde-3-phosphate dehydrogenase (GAPDH) was used as a loading control. Expression level of Bcl-2 was measured using densitometry and normalized against the expression level of GAPDH (j). k, l Immunoblot analysis showing the phosphorylation of Akt in NALM-6/Su and NALM-6/Ad after DXR treatment. Total Akt was used as a loading control. Expression level of phosphorylated Akt (pAkt) was measured using densitometry and normalized against the expression level of total Akt (l). m, n Cell cycle analysis of NALM-6/Su and NALM-6/Ad by flow cytometry using Ki-67/7-amino-actinomycin D (7-AAD). Representative dot plots are shown in n. a–f n = 4 per group. m n = 11 per group. Data are mean values ± SD in (a–f, m). *, P < 0.05; **, P < 0.01; n.s., not significant
NALM-6 cells were purified from the suspension cells or adherent cells in the co-culture using anti-CD19 immunomagnetic microbeads (Fig. 2g, h) and then applied to immunoblot and cell cycle analyses. The expression level of the anti-apoptotic protein Bcl-2 was higher in NALM-6/Ad than in NALM-6/Su in a steady state (Fig. 2i, j). In addition, the phosphorylation level of the pro-survival protein Akt was higher in NALM-6/Ad than in NALM-6/Su after treatment with DXR (Fig. 2k, l). Thus, NALM-6 cells that adhere to BM-MSCs are resistant to anti-cancer drugs through the pro-survival Akt/Bcl-2 signaling pathway, at least in part. In cell cycle analysis, the percentages of cells in the G0 and S/G2/M stages were higher among NALM-6/Ad than among NALM-6/Su (Fig. 2m, n), which indicated that the adhesive population of leukemia cells had increased chemoresistant and proliferative characteristics. Therefore, interfering with adhesion of BCP-ALL cells to BM-MSCs is effective to eliminate such leukemia cells.
Bor and other proteasome inhibitors interfere with adhesion of NALM-6 cells to BM-MSCs
A proteasome inhibitor, Bor, has therapeutic effects on multiple myeloma (MM) [12]. It is mediated not only by directly killing of MM cells but also by acting on stromal cells to affect interaction between MM cells and stromal cells in BM [13]. Therefore, it is conceivable to speculate that Bor has influence on the interaction between BCP-ALL cells and BM-MSCs. We examined whether Bor acted on BM-MSCs and changed their property of inducing adherence of NALM-6 cells (Fig. 3a). When BM-MSCs were treated with Bor at various concentrations from 0 nM to 100 nM transiently for 1 h (transient treatment), the growth of BM-MSCs was not affected (Fig. 3b). When BM-MSCs were treated with Bor continuously for 24 h (continuous treatment), the growth of BM-MSCs was not affected at concentrations less than or equal to 10 nM, but it was delayed at concentrations of 30 and 100 nM (Fig. 3c).
Treatment of BM-MSCs with Bor. (a) Schema of the co-culture experiment of NALM-6 cells and proteasome inhibitor (PI)-treated BM-MSCs. (b, c) Relative growth of BM-MSCs on day 1 and day 2 after treatment with Bor at various concentrations from 0 to 100 nM transiently for 1 h (b) or continuously for 24 h (c). b, c n = 12 per group
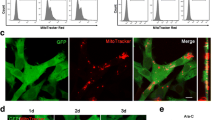
The number of NALM-6/Ad in co-cultures with BM-MSCs that had been pretreated with 100 nM Bor transiently (Fig. 4a) or 10 nM Bor continuously (Fig. 4e) was lower than the number of NALM-6/Ad in co-cultures with untreated control BM-MSCs, as assessed by flow cytometric analysis. Therefore, treatment of BM-MSCs with Bor interferes with the adhesion of NALM-6 cells to BM-MSCs without affecting their growth. These results were confirmed by microscopic observation, in which the number of NALM-6/Ad per BM-MSC was lower in co-cultures with BM-MSCs that had been pretreated with Bor either transiently (Fig. 4b–d) or continuously (Fig. 4f–h) than in co-cultures with untreated control BM-MSCs.
Proteasome inhibitors interfere with adhesion of NALM-6 cells to BM-MSCs. a–h The number of NALM-6/Ad in co-cultures with BM-MSCs that were pretreated with or without Bor transiently (a–d) or continuously (e–h). Cell counting was performed by flow cytometric analysis (a, e) or microscopic observation (b–d, f–h) and is indicated by the ratio of the number of NALM-6/Ad to the number of BM-MSCs (b, f). Representative images are shown in (c, d, g, h). Red arrows indicate NALM-6 cells that adhere to BM-MSCs (NALM-6/Ad). Bars 150 μm. i, j The number of NALM-6/Ad in co-cultures with BM-MSCs that were pretreated with or without Car transiently (i) or continuously (j). k, l The number of NALM-6/Ad in co-cultures with BM-MSCs that were pretreated with or without Opr transiently (k) or continuously (l). Cell counting was performed by flow cytometric analysis (i–l). In a, e, i–l, open bars indicate the number of NALM-6/Ad that were treated with proteasome inhibitors of Bor, Car, or Opr and closed bars indicate the number of NALM-6/Ad that were not treated with proteasome inhibitors. a, e n = 20 per group, b n = 12 per group, f n = 10 per group, i–l n = 12 per group. Data are shown as mean values ± SD in a, e, i–l). *, P < 0.05; **, P < 0.01
We further examined whether other proteasome inhibitors interfered with the adhesion of NALM-6 cells to BM-MSCs. Treatment with 100 nM Car transiently for 1 h (Supplementary Fig. 2A) and 3 nM Car continuously for 24 h (Supplementary Fig. 2B) did not affect the growth of BM-MSCs. Similarly, treatment with 300 nM Opr transiently for 4 h (Supplementary Fig. 2C) and 10 nM Opr continuously for 24 h (Supplementary Fig. 2D) did not affect the growth of BM-MSCs. When BM-MSCs were pretreated with Car or Opr in such a way that their growth was not affected and then co-cultured with NALM-6 cells, the number of NALM-6/Ad was lower than that in co-cultures with untreated BM-MSCs (Fig. 4i–l). These results indicated that not only Bor but also other proteasome inhibitors interfered with the adhesion of NALM-6 cells at concentrations that did not affected the growth of BM-MSCs.
Up-regulation of SPARC protein in BM-MSCs by Bor treatment contributes to the anti-adhesive property of BM-MSCs
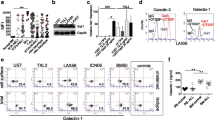
In contrast to adhesion molecules, the involvement of anti-adhesion molecules in the interference of adhesion between cells and other cells or extracellular matrix (ECM) proteins has not been widely investigated [14]. At the cell surface interface, some matricellular proteins, particularly SPARC, which is expressed in bone, have anti-adhesive properties [14,15,16]. As assessed by immunoblot analysis, expression of SPARC protein was increased in BM-MSCs after treatment with Bor for 1 h (Fig. 5a, b). To explore the anti-adhesive function of SPARC, its protein and mRNA expression in BM-MSCs was depleted using SPARC-specific siRNA (Fig. 5c) and then these BM-MSCs were co-cultured with NALM-6 cells. As expected, the number of NALM-6/Ad per BM-MSCs was significantly increased compared with that in co-cultures with BM-MSCs treated with negative control siRNA (Fig. 5d). Conversely, when BM-MSCs were pre-incubated with rhSPARC and then co-cultured with NALM-6 cells, the number of NALM-6/Ad was significantly reduced (Fig. 5e). To further examine the direct contribution of SPARC protein to the interference of adhesion of NALM-6 cells, these cells were cultured on rhSPARC-treated fibronectin-coated plates. The number of NALM-6/Ad was decreased compared with that in cultures on control (PBS-treated) fibronectin-coated plates (Fig. 5f–h). This adhesion to fibronectin was expected to be related to integrin α4β1 (VLA-4) expressed on the surface of NALM-6 cells (Fig. 5i, j). These results suggest that Bor-induced interference of adhesion of NALM-6 cells to BM-MSCs is mediated through up-regulated expression of SPARC protein in BM-MSCs. mRNA expression of SPARC in BM-MSCs was not significantly increased in a time course study upon treatment with Bor for up to 1 h (Fig. 5k). Thus, Bor could prolong the lifetime of SPARC protein, rather than affect translation of SPARC mRNA.
Bor treatment up-regulates SPARC expression in BM-MSCs. a, b Immunoblot analysis showing SPARC protein expression in BM-MSCs treated with (Bor+) or without (Bor−) 100 nM Bor for 1 h. Expression levels of SPARC were measured using densitometry and normalized against the expression level of GAPDH (n = 3). c Immunoblot analysis showing SPARC protein expression in BM-MSCs treated with SPARC-specific siRNA or negative control siRNA (N.C.). d NALM-6 cells were co-cultured with BM-MSCs pretreated with SPARC-specific siRNA (open bar) or negative control siRNA (N.C., closed bar) (n = 7 per group). Y-axis is indicated by the ratio of the number of NALM-6/Ad to the number of BM-MSCs. e The number of NALM-6/Ad in co-cultures with BM-MSCs pre-incubated with (open bar) or without rhSPARC (closed bar) (n = 10 per group). f–h The number of NALM-6 cells that adhered to the bottom of the dish in cultures on rhSPARC-treated (open bar) or PBS-treated (Control, closed bar) fibronectin-coated dishes (n = 12 per group). Cell counting was performed by microscopic observation and is indicated by the number of adherent cells per field at 100× magnification (f). Representative images of cultures on PBS-treated (g, Control) or rhSPARC-treated fibronectin-coated dishes (h, rhSPARC) are shown. Red arrows indicate NALM-6 cells that adhere to the bottom of the dish. Bars 50 μm. i, j Flow cytometric analysis of NALM-6 cells showing their expression of integrin α4 (i) and integrin β1 (j). Filled histograms indicate control staining. k Time course study of SPARC mRNA expression in BM-MSCs treated with (closed bars) or without (open bars) Bor, as assessed by qRT-PCR analysis. The level of SPARC mRNA is shown relative to that of GAPDH mRNA in each sample (n = 6 per group). l, m Immunoblot analysis showing SPARC protein expression in BM-MSCs derived from patients with BCP-ALL (#P1‒#P3) and healthy controls (#C1‒#C3). GAPDH was used as loading control (l). Expression levels of SPARC were measured using densitometry and normalized against the expression level of GAPDH (m). Data are shown as mean values ± SD in (b, d–f, k). *, P < 0.05; **, P < 0.01; n.s., not significant
We examined expression of SPARC protein in BM-MSCs derived from patients with BCP-ALL (Supplementary Table 2). The expression level of SPARC tended to be lower in patients with BCP-ALL than in healthy controls (Fig. 5l, m).
Combination treatment with Bor and DXR additively prolongs the survival of BCP-ALL xenograft mice and reduces the population of NALM-6 cells in BM
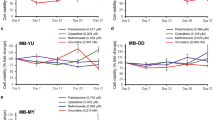
Bor affected the adhesive property of BM-MSCs and reduced the NALM-6/Ad population that was resistant to anti-cancer drugs, thereby contributing to a relative increase in NALM-6 cells that were sensitive to anti-cancer drugs. Therefore, combination treatment with Bor and an anti-cancer drug was expected to be more effective than treatment with an anti-cancer drug alone. We generated BCP-ALL xenograft model mice using NALM-6 cells and treated these mice with DXR and Bor (Fig. 6a). Treatment with DXR alone significantly prolonged the survival of BCP-ALL mice compared with that of non-drug-treated mice (Fig. 6b, orange line versus blue line). As expected, co-treatment with DXR and Bor significantly further prolonged the survival of BCP-ALL mice compared with DXR or Bor treatment alone (Fig. 6b, yellow line versus orange line or gray line). In the BM of mice treated with DXR or Bor alone, the proportion of NALM-6 cells was not reduced compared with that in non-drug-treated mice (Fig. 6c). Treatment with both Bor and DXR significantly reduced the proportion of NALM-6 cells in BM compared with that in BM of mice treated with DXR or Bor alone (Fig. 6c). To exclude a direct effect of Bor on NALM-6 cells, these cells were directly treated with Bor and/or DXR for 1 h. Compared with the non-treated control, the number of NALM-6 cells was significantly reduced at 24 h after treatment with DXR alone, but not at 24 h after treatment with Bor alone (Fig. 6d). Co-treatment with Bor and DXR did not significantly reduce the number of NALM-6 cells compared with DXR treatment alone (Fig. 6d). These effects were also observed at 48 h after treatment with Bor and/or DXR (Fig. 6e). Therefore, the prolonged survival of mice along with the reduced NALM-6 cell population in BM upon Bor treatment in combination with DXR was not necessarily mediated by a cytotoxic effect of Bor on NALM-6 cells, but rather possibly by the effect of Bor on BM-MSCs.
Combination treatment with DXR and Bor in BCP-ALL xenograft mice using NALM-6 cells. a Schema of the preclinical experiment using BCP-ALL xenograft mice. On day 0, 6–7-week-old male SCID mice were irradiated with 2 Gy and then injected with NALM-6 cells (1 × 107 cells). These mice received DXR treatment and/or Bor treatment on day 28 after NALM-6 cell injection. The survival of mice was observed each day until day 91 after NALM-6 cell injection. In some experiments, the mice were sacrificed on day 35 to harvest BM cells for further analysis. b Survival curves of mice. The median survival period of mice that were treated with PBS (blue line, n = 5), Bor alone (gray line, n = 6), DXR alone (orange line, n = 6), and DXR in combination with Bor (yellow line, n = 6) was 35, 39, 47.5, and 57.5 days, respectively. c The proportion of NALM-6 cells in BM of mice treated with DXR or Bor alone and DXR in combination with Bor at day 35 after NALM-6 cell injection. d, e The number of NALM-6 cells at 24 h (n = 5 per group) (d) and 48 h (n = 5 per group) (e) after treatment with DXR with or without Bor in vitro. Data are mean values ± SD in (c–e). *, P < 0.05; **, P < 0.01; n.s., not significant
Discussion
Adult BCP-ALL is one of the most aggressive hematological malignancies [17]. Recent progress in the understanding of mechanisms and the development of therapies has improved the outcomes of this disease [4, 18]. Nevertheless, a substantial number of adult patients eventually experience relapse of leukemia and the prognosis is still poor [1, 18, 19]. Various environmental components in the BM, particularly BM-MSCs, regulate the proliferation, apoptosis, survival, and drug resistance of BCP-ALL cells through indirect and direct interactions [9, 20, 21]. Accordingly, not only direct killing of BCP-ALL cells but also targeting BM-MSCs that protect leukemia cells in the BM microenvironment should be considered as a therapeutic strategy to eradicate BCP-ALL cells and to achieve an eventual cure. In the present study, we showed that a proteasome inhibitor, Bor, acted on BM-MSCs to interfere with adhesion of BCP-ALL cells and contributed to a reduction of leukemia cells in combination with anti-cancer drugs in vitro and in vivo. Importantly, combination treatment with Bor and an anti-cancer drug prolonged the survival of BCP-ALL xenograft mice in a preclinical model. Our study could provide a rationale for a pharmacological BM-MSC-targeted strategy to treat patients with BCP-ALL. Of note, Bor is already clinically available for MM; therefore, early clinical application of Bor for BCP-ALL would be warranted with minimized safety and toxicity clinical study.
Environment-mediated drug resistance includes cell adhesion-mediated drug resistance (CAM-DR) that is attributed to the interaction between adhesion molecules in tumor cells and their ligands in stromal cells or ECM proteins [22, 23]. With regard to hematological malignancies, the role of the β1 integrin-fibronectin interaction in mediating CAM-DR has been extensively studied in MM and myeloid leukemia [22]. Actually, multiple adhesion molecules are involved in adhesion of leukemia cells to BM-MSCs, which evokes multiple intracellular events that synergistically cooperate to induce chemotherapy resistance in leukemia cells. Notably, the PI3K/Akt pathway protects leukemia cells by up-regulating Bcl-2 [24, 25], and α4β1 integrin (VLA-4)-specific antibodies abrogate PI3K/Akt/Bcl-2 pathway-mediated resistance to drug-induced apoptosis in acute myelogenous leukemia cells [25]. Consistent with these findings, we found that NALM-6 cells that adhered to BM-MSCs (NALM-6/Ad) had pro-survival characteristics, with increased Bcl-2 expression and Akt phosphorylation. Furthermore, the populations in the G0 and S/G2/M stages were increased among NALM-6/Ad, which supports the clinical findings of chemoresistance and rapid recurrence of BCP-ALL [26].
SPARC belongs to a group of matricellular proteins that are present in the ECM and have various functions including regulation of matrix remodeling and growth factor signaling [27,28,29]. Our study demonstrated that SPARC serves as an anti-adhesion molecule to interfere with adhesion of NALM-6 cells to BM-MSCs and fibronectin. The receptor of SPARC is not known. SPARC has been suggested to interact with β1 integrin [30, 31]. NALM-6 cells express β1 integrin. BM-MSCs express fibronectin, which is a ligand of β1 integrins [32]. Thus, up-regulation of SPARC in BM-MSCs by Bor, as observed in our study, might affect this β1 integrin-ligand interaction. Clinically, high levels of SPARC expression correlate with metastasis of cancer cells and poor prognosis in patients with solid tumors such as melanoma [28, 33, 34], which indicates that the anti-adhesive function of SPARC mediates the invasion or migration of tumor cells [28]. Although the number of samples examined was limited in our study, BM-MSCs from patients with BCP-ALL showed lower protein expression of SPARC than healthy controls. This result might imply that BCP-ALL cells influence BM-MSCs to suppress SPARC expression and thereby promote their survival through adhesion. The involvement of SPARC in BM-MSCs in the pathogenesis of BCP-ALL needs to be revealed by the analysis of more human patient samples and by the investigation of SPARC expression in BM-MSCs of mice that were treated with PBS, Bor, DXR, and DXR and Bor.
While the effects of Bor on anti-adhesion molecules including SPARC have not been investigated, those on adhesion molecules were demonstrated in the previous reports [35, 36]. In the study of MM, Hideshima et al. reported that Bor did not show obvious influence on the expressions of VCAM-1 or ICAM-1 in BM-MSCs and did not inhibit adhesion of MM cells to BM-MSCs [35]. Circulating levels of VCAM-1 and ICAM-1 were decreased in the serum of MM patients after the treatment with Bor and dexamethasone [36]. Comprehensive understanding of CAM-DR mechanisms mediated by various adhesion/anti-adhesion molecules needs to be warranted to improve outcomes of intractable hematological diseases including BCP-ALL.
In summary, we demonstrated that BCP-ALL cells were resistant to anti-cancer drugs when they were adhered to BM-MSCs and that Bor interfered with the adhesion of leukemic cells to BM-MSCs through SPARC up-regulation. Combination treatment with an anti-cancer drug and Bor effectively prolonged the survival of BCP-ALL model mice with a reduced population of leukemia cells. Our findings offer a novel strategy for the treatment of patients with BCP-ALL by targeting BM-MSCs.
References
Jinnai I, Sakura T, Tsuzuki M, Maeda Y, Usui N, Kato M, et al. Intensified consolidation therapy with dose-escalated doxorubicin did not improve the prognosis of adults with acute lymphoblastic leukemia: the JALSG-ALL97 study. Int J Hematol. 2010;92:490–502.
Huguet F, Leguay T, Raffoux E, Thomas X, Beldjord K, Delabesse E, et al. Pediatric-inspired therapy in adults with Philadelphia chromosome-negative acute lymphoblastic leukemia: the GRAALL-2003 study. J Clin Oncol. 2009;27:911–8.
Storring JM, Minden MD, Kao S, Gupta V, Schuh AC, Schimmer AD, et al. Treatment of adults with BCR-ABL negative acute lymphoblastic leukaemia with a modified paediatric regimen. Br J Haematol. 2009;146:76–85.
Dhédin N, Huynh A, Maury S, Tabrizi R, Beldjord K, Asnafi V, et al. Role of allogeneic stem cell transplantation in adult patients with Ph-negative acute lymphoblastic leukemia. Blood. 2015;125:2486–96.
Bassan R, Spinelli O, Oldani E, Intermesoli T, Tosi M, Peruta B, et al. Improved risk classification for risk-specific therapy based on the molecular study of minimal residual disease (MRD) in adult acute lymphoblastic leukemia (ALL). Blood. 2009;113:4153–62.
Colmone A, Amorim M, Pontier AL, Wang S, Jablonski E, Sipkins DA. Leukemic cells create bone marrow niches that disrupt the behavior of normal hematopoietic progenitor cells. Science. 2008;322:1861–5.
Jacamo R, Chen Y, Wang Z, Ma W, Zhang M, Spaeth EL, et al. Reciprocal leukemia-stroma VCAM-1/VLA-4-dependent activation of NF-κB mediates chemoresistance. Blood. 2014;123:2691–702.
Miura Y. Human bone marrow mesenchymal stromal/stem cells: current clinical applications and potential for hematology. Int J Hematol. 2016;103:122–8.
Juarez J, Dela Pena A, Baraz R, Hewson J, Khoo M, Cisterne A, et al. CXCR4 antagonists mobilize childhood acute lymphoblastic leukemia cells into the peripheral blood and inhibit engraftment. Leukemia. 2007;21:1249–57.
Yoshioka S, Miura Y, Yao H, Satake S, Hayashi Y, Tamura A, et al. CCAAT/enhancer-binding protein β expressed by bone marrow mesenchymal stromal cells regulates early B-cell lymphopoiesis. Stem Cells. 2014;32:730–40.
Yang Y, Mallampati S, Sun B, Zhang J, Kim SB, Lee JS, et al. Wnt pathway contributes to the protection by bone marrow stromal cells of acute lymphoblastic leukemia cells and is a potential therapeutic target. Cancer Lett. 2013;333:9–17.
Richardson PG, Barlogie B, Berenson J, Singhal S, Jagannath S, Irwin D, et al. A phase 2 study of bortezomib in relapsed, refractory myeloma. N Engl J Med. 2003;348:2609–17.
Hideshima T, Anderson KC. Preclinical studies of novel targeted therapies. Hematol Oncol Clin North Am. 2007;21:1071–91.
Murphy-Ullrich JE, Sage EH. Revisiting the matricellular concept. Matrix Biol. 2014;37:1–14.
Brekken RA, Sage EH. SPARC, a matricellular protein: at the crossroads of cell-matrix communication. Matrix Biol. 2001;19:816–27.
Termine JD, Kleinman HK, Whitson SW, Conn KM, McGarvey ML, Martin GR. Osteonectin, a bone-specific protein linking mineral to collagen. Cell. 1981;26:99–105.
Pui CH, Evans WE. Acute lymphoblastic leukemia. N Engl J Med. 1998;339:605–15.
DeAngelo DJ, Stevenson KE, Dahlberg SE, Silverman LB, Couban S, Supko JG, et al. Long-term outcome of a pediatric-inspired regimen used for adults aged 18–50 years with newly diagnosed acute lymphoblastic leukemia. Leukemia. 2015;29:526–34.
Rowe JM. Prognostic factors in adult acute lymphoblastic leukaemia. Br J Haematol. 2010;150:389–405.
Nishii K, Katayama N, Miwa H, Shikami M, Masuya M, Shiku H, et al. Survival of human leukaemic B-cell precursors is supported by stromal cells and cytokines: association with the expression of bcl-2 protein. Br J Haematol. 1999;105:701–10.
Boyerinas B, Zafrir M, Yesilkanal AE, Price TT, Hyjek EM, Sipkins DA. Adhesion to osteopontin in the bone marrow niche regulates lymphoblastic leukemia cell dormancy. Blood. 2013;121:4821–31.
Meads MB, Hazlehurst LA, Dalton WS. The bone marrow microenvironment as a tumor sanctuary and contributor to drug resistance. Clin Cancer Res. 2008;14:2519–26.
Meads MB, Gatenby RA, Dalton WS. Environment-mediated drug resistance: a major contributor to minimal residual disease. Nat Rev Cancer. 2009;9:665–74.
Lee BH, Ruoslahti E. alpha5beta1 integrin stimulates Bcl-2 expression and cell survival through Akt, focal adhesion kinase, and Ca2+/calmodulin-dependent protein kinase IV. J Cell Biochem. 2005;95:1214–23.
Matsunaga T, Takemoto N, Sato T, Takimoto R, Tanaka I, Fujimi A, et al. Interaction between leukemic-cell VLA-4 and stromal fibronectin is a decisive factor for minimal residual disease of acute myelogenous leukemia. Nat Med. 2003;9:1158–65.
Oriol A, Vives S, Hernández-Rivas JM, Tormo M, Heras I, Rivas C, et al. Outcome after relapse of acute lymphoblastic leukemia in adult patients included in four consecutive risk-adapted trials by the PETHEMA Study Group. Haematologica. 2010;95:589–96.
Bornstein P. Cell-matrix interactions: the view from the outside. Methods Cell Biol. 2002;69:7–11.
Nagaraju GP, Dontula R, El-Rayes BF, Lakka SS. Molecular mechanisms underlying the divergent roles of SPARC in human carcinogenesis. Carcinogenesis. 2014;35:967–73.
Chlenski A, Cohn SL. Modulation of matrix remodeling by SPARC in neoplastic progression. Semin Cell Dev Biol. 2010;21:55–65.
Murphy-Ullrich JE, Lane TF, Pallero MA, Sage EH. SPARC mediates focal adhesion disassembly in endothelial cells through a follistatin-like region and the Ca(2+)-binding EF-hand. J Cell Biochem. 1995;57:341–50.
Nie J, Chang B, Traktuev DO, Sun J, March K, Chan L, et al. IFATS collection: combinatorial peptides identify alpha5beta1 integrin as a receptor for the matricellular protein SPARC on adipose stromal cells. Stem Cells. 2008;26:2735–45.
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, et al. Multilineage potential of adult human mesenchymal stem cells. Science. 1999;284:143–7.
Thomas SL, Alam R, Lemke N, Schultz LR, Gutiérrez JA, Rempel SA. PTEN augments SPARC suppression of proliferation and inhibits SPARC-induced migration by suppressing SHC-RAF-ERK and AKT signaling. Neuro Oncol. 2010;12:941–55.
Massi D, Franchi A, Borgognoni L, Reali UM, Santucci M. Osteonectin expression correlates with clinical outcome in thin cutaneous malignant melanomas. Hum Pathol. 1999;30:339–44.
Hideshima T, Chauhan D, Schlossman R, Richardson P, Anderson KC. The role of tumor necrosis factor alpha in the pathophysiology of human multiple myeloma: therapeutic applications. Oncogene. 2001;20:4519–27.
Terpos E, Migkou M, Christoulas D, Gavriatopoulou M, Eleutherakis-Papaiakovou E, Kanellias N, et al. Increased circulating VCAM-1 correlates with advanced disease and poor survival in patients with multiple myeloma: reduction by post-bortezomib and lenalidomide treatment. Blood Cancer J. 2016;6:e428.
Acknowledgements
We thank Ms. Yoko Nakagawa for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Grants
This work was supported in part by a Grant-in-Aid from the Ministry of Education, Culture, Sports, Science, and Technology in Japan (#26293277 and #15K09453, Y.M. and T.I.; #16H00656, N.S.). This work was also supported in part by the Program of the network-type joint Usage/Research Disaster Medical Science of Hiroshima University, Nagasaki University, and Fukushima Medical University (Y.M., S.F., and T.I.), the Kyoto Prevention Medical Center (Y.M.), and the Takeda Science Foundation (Y.M.).
Conflict of interest
The authors declare no conflict of interest.
Additional information
An erratum to this article is available at http://dx.doi.org/10.1007/s12185-017-2182-8.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Iwasa, M., Miura, Y., Fujishiro, A. et al. Bortezomib interferes with adhesion of B cell precursor acute lymphoblastic leukemia cells through SPARC up-regulation in human bone marrow mesenchymal stromal/stem cells. Int J Hematol 105, 587–597 (2017). https://doi.org/10.1007/s12185-016-2169-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12185-016-2169-x