Abstract
Background
Racial differences in anger frequency and expression styles have been found. Further, African Americans receive fewer health benefits from higher education than Whites.
Purpose
This study seeks to investigate racial differences in how anger moderates the association between education and inflammation.
Methods
Midlife in the US participants (n = 1,200; 43.0 % male; 18.5 % African American) provided education and anger data via survey assessments. Interleukin-6 (IL-6) and fibrinogen were determined from a fasting blood sample following an overnight clinic visit.
Results
African Americans reported higher anger-out, IL-6, and fibrinogen and lower anger-control than Whites. Anger-out predicted higher IL-6 and fibrinogen among African Americans with higher education; whereas, trait anger and anger-out predicted lower fibrinogen among Whites with higher education. Anger-out marginally predicted higher IL-6 in less educated Whites.
Conclusions
Findings underscore racial differences in the benefits and consequences of educational attainment, and how social inequities and anger are manifested in inflammatory physiology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
The pernicious health consequences of anger are widely recognized. Prospective studies have shown that high levels of anger and poorly controlled anger predict risk for hypertension, coronary heart disease, and stroke [1–3]. However, less research has addressed the physiological mechanisms underlying this association between anger and disease. Inflammation is a primary candidate pathway through which anger can affect disease processes. Inflammatory and coagulation markers, such as the pro-inflammatory cytokine, interleukin-6 (IL-6), and the clotting factor, fibrinogen, respond to the psychosocial environment and when elevated, contribute to the etiology and pathogenesis of many chronic conditions, including cardiovascular disease and diabetes [4–6]. Anger and hostility are associated with higher circulating levels of inflammatory markers and clotting factors [7–13] and cytokine release from cells when stimulated and cultured in vitro [14].
Missing in the prior literature on anger and inflammation is a consideration of the broader societal context in which these associations occur. Anger is a common emotional reaction to inequality; those of lower socioeconomic status (SES) report more frequent angry experiences, more frequent outward expressions of anger (anger-out), and more frequent suppression of anger (anger-in), while those in higher SES strata report they can better manage their anger (anger-control) when experienced [15–18]. SES is a critically important predictor of health [19], and circulating levels of inflammatory and clotting factors are systematically linked with educational status and income, with the lower strata evincing elevated inflammation relative to those in more favorable positions [20–24]. However, whether or not the associations between anger and inflammation are consistent across the SES gradient is not typically studied, despite some evidence indicating that the frequent experience and expression of anger may be more harmful to the health of individuals already at risk due to disadvantaged SES, especially in childhood [25, 26].
In a prior study of the population-based Midlife in the United States (MIDUS) cohort of middle-aged and older adults, trait anger and anger-out were more strongly associated with higher IL-6 and fibrinogen for those with low educational attainment (i.e., high school education or less) as compared to those with college and professional levels of education. Anger-control also predicted lower IL-6 for those with a high school degree or less, but only among women [27]. Anger-in did not moderate the educational gradients in inflammation. One shortcoming of the prior analyses, however, was the limited representation of racial minorities within the national cohort (only 7.2 % of respondents). The current report addresses this limitation by including a city-specific sample of African Americans from Milwaukee, Wisconsin, permitting us to now examine the influence of race on the associations among IL-6, fibrinogen, education, and anger. Although a city-specific sample does not represent African Americans nationally, Milwaukee is an informative context, given that it is among the most segregated cities in the United States [28]. Publications from this Milwaukee sample have documented higher stress in many life domains (e.g., work, family, and neighborhood) and more early life adversity than for the overall MIDUS national sample [29, 30]. As such, it is an informative urban setting for evaluating the links between anger and health.
The literature regarding race differences in anger is inconsistent, and the role of SES in explaining those effects and the implications for inflammatory biology are largely unexplored. Qualitative research with middle- and upper-class African Americans indicates that anger continues to be a common corollary of higher SES due to persistent experiences of racial discrimination and unfair treatment, even in contexts of educational or occupational success [31]. Recent quantitative research by Williams and colleagues [32] shows that anger and frustration were the most common emotional responses to experiences of racial and non-racial discrimination, regardless of race or SES. In the same paper, Whites and African Americans did not differ on the average number of unfair experiences or treatment, but African American respondents viewed most of their unfair experiences as due to racial causes, whereas White respondents typically viewed them as nonracial. It is also noteworthy that the rates of unfair treatment were higher among low-SES African Americans and Whites than their middle-class counterparts. Additional evidence suggests that African Americans experience less “return” on education—higher educated African Americans have lower levels of occupational and income attainment [33, 34] and poorer health outcomes than similarly educated Whites [35–38].
Together, these findings suggest that the health ramifications of high anger, or poorly controlled anger, may be stronger in African Americans with more, compared to less, education, in contrast to prior findings in the largely White MIDUS national cohort. Alternatively, in at least one study of African American adolescents, trait anger was found to predict blood pressure more strongly among those from low, as compared to higher SES neighborhoods [26], indicating that anger may be most detrimental among low SES individuals; similar to the association previously reported among White respondents. We tested the predictive value of these perspectives by examining the influence of anger experience and expression as moderators of the association between education and two inflammatory and coagulation markers in African Americans compared to prior findings on primarily White adults [27]. Both groups were included in statistical analyses to test for race differences, which would be evident when there were three-way interactions among race, educational status, and anger, in predicting IL-6 and fibrinogen as outcomes.
Method
Participants were from the second wave of MIDUS (MIDUS II), which began in 2004 with a 75 % retention rate from the first wave (adjusted for mortality). MIDUS I began in 1995 with more than 7,000 non-institutionalized adults, recruited via random digit dialing from the 48 contiguous states, siblings of the random digit dialing sample, and a large sample of twins [39, 40].
Biological data were collected from a subset of respondents who completed both MIDUS I and II survey assessments and agreed to travel to one of three clinics (Madison, WI; Washington, DC; or Los Angeles, CA) for an overnight visit [41]. The biological data sample included individuals from the national cohort (n = 1,054) as well as African Americans from Milwaukee, WI, who were recruited at MIDUS II (n = 201) [30]. A small number of respondents who identified as a race other than White or Black and/or African American were excluded (n = 55). The majority (87.8 %) of African American respondents came from Milwaukee. This study was approved by Institutional Review Boards at University of Wisconsin-Madison, as well as at Georgetown University and the University of California, Los Angeles. All participants provided written informed consent.
Measures
Education
During telephone and home interviews (Milwaukee sample only), respondents reported the highest grade of school or year of college completed. The twelve response categories ranged from no schooling to completion of a professional degree. Education was treated as a continuous variable in analyses.
Anger
Anger was assessed using the trait anger (15 items), anger-out (8 items), and anger-control (4 items) subscales from Spielberger’s State-Trait Anger Expression Inventory [42], which was completed during the clinic visit. Trait anger was measured by respondents indicating how often they generally felt the given statements (e.g., “I have a fiery temper”) on a four-point scale. For the anger-out and anger-control scales, participants respectively indicated how often they expressed their anger outwardly (e.g., “I strike out at whatever infuriates me”) or how often they attempted to manage the expression of their anger (e.g., “I control my temper”) when they felt angry or furious. Internal consistencies were consistent across racial groups, ranging from .69 to .83 in the White sample and from .67 to .89 in the African American sample.
Covariates
Covariates included age, gender, body mass index (BMI), medication usage, current smoking status, regular exercise, alcohol consumption, and chronic health conditions. Age, gender, BMI, medication usage, and chronic health conditions were considered confounding influences known to affect levels of inflammatory markers [43], and we were interested in examining associations among anger, education, and race independent of these factors. Height and weight were measured by nursing staff at each General and Clinical Research Center (GCRC) and used to calculate BMI (weight in kilograms divided by height in meters squared). BMI is a key predictor of inflammatory markers [43, 44]. Antidepressants, anti-hypertensives, cholesterol-lowering medications, and steroid usage (accounted for as four binary-coded variables to indicate current use or non-use) have modulatory effects on IL-6 and fibrinogen [45, 46]. Chronic health conditions (summed score) were self-reported physician diagnosed diseases; inflammation is an important component for many of these chronic illnesses [47]. Smoking status, regular exercise (at least 20 min per day, three or more times per week), and alcohol consumption (drinks per month) were self-reported at the GCRC visit. These factors represent important behavioral pathways that likely contribute to the links among education, anger, and race to chronic inflammation [43]. Fully adjusted models included both confounding influences and health behaviors.
Inflammatory Markers
Serum IL-6 levels were measured with the Quantikine® high-sensitivity enzyme linked immunosorbent assay kit (R&D Systems, Minneapolis, MN). Fibrinogen was measured using the BNII nephelometer (Dade Behring Inc., Deerfield, IL). The intra- and inter-assay coefficients of variance were all in an acceptable range (<12 % variance).
Statistical Analyses
All analyses involved comparisons between African American and White respondents in keeping with the central focus on race differences. A small number of IL-6 and fibrinogen values were winsorized to three standard deviations from the mean to reduce the influence of outliers (2 % of total data). IL-6 and BMI were log-transformed to achieve normal distributions. Generalized estimating equations models with random intercepts for each family cluster and an exchangeable within cluster covariance structure were used to address the dependencies in the data from the inclusion of twins and siblings (38 %) in the MIDUS national sample. All continuous variables were mean-centered. Race, education, anger, all possible two-way interactions, and three-way interactions were considered as respective predictors of IL-6 and fibrinogen. Control variables included age, gender, BMI, current smoking status, alcohol consumption, regular exercise, chronic health conditions, and mediation usage. Models were run separately for each dimension of anger and for each inflammatory marker. Significant three-way interactions were probed by examining simple slopes between anger and IL-6 and fibrinogen were examined at high and low levels of education, respectively, for each racial group [48]. For high and low education levels, we centered at the mean level of education among those with a college degree or more and those with a high school education or less, respectively. An alpha level of 0.05 was used for all statistical tests.
Results
Descriptive information is summarized in Table 1. The African American sample had higher IL-6 and fibrinogen [49], and were younger, more likely to be female, less educated, had more chronic conditions, higher BMIs, reported more alcohol use, and were more likely to be current smokers. They were also more likely to be taking anti-hypertensive medication, less likely to get regular exercise, and less likely to be taking cholesterol-lowering or anti-depressant medication than the White respondents. Data from the anger scales portrayed separately by race and educational attainment are provided in Table 2. The African American respondents reported greater anger-out and lower anger-control than did the White respondents. There were no significant main effects of education or education-by-race interactions that predicted any of the anger scales.
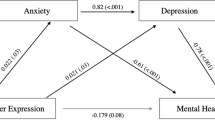
Results from the three-way interaction models are presented in Table 3. Several significant three-way interactions emerged, including between race, education, and trait anger predicting fibrinogen and between race, education, and anger-out predicting both fibrinogen and IL-6. To probe these interactions, simple slopes between trait anger and anger-out and IL-6 and fibrinogen were calculated for African American and White respondents at low and high education levels. They are presented in Table 4 and displayed in Fig. 1. Among African Americans, greater anger-out predicted higher IL-6 and fibrinogen among those with high, but not low, educational status. Among White respondents, anger-out predicted higher IL-6 among those with low, but not high, educational status, though at trend level significance (p = .054). Trait anger and anger-out also predicted lower fibrinogen among White respondents with high, but not low, educational status.
Racial differences in the moderation of educational gradients in IL-6 and fibrinogen by two varieties of anger. Lines represent the simple effects of anger on IL-6 and fibrinogen for White and African American respondents by education. Low education refers to the mean education among individuals with a high school education or less. High education refers to the mean education among individuals with a college degree or more. Effects were adjusted for age, gender, medication usage, chronic health conditions, current smoking status, alcohol consumption, regular exercise, and BMI. Data for White respondents have previously been published [27]
In order to examine whether the effects of anger were independent from general negative affect, we re-ran three-way interaction models adjusting for depressed mood, assessed with the Center for Epidemiologic Studies Depression scale [50], and trait anxiety, which had been assessed with Spielberger’s scale [51]. Results were unchanged by inclusion of depressed mood and trait anxiety as additional covariates in fully adjusted models, suggesting that the previously identified associations were specific to anger and not due to the influence of general negative affect (race × education × trait anger predicting fibrinogen: B(SE) = −0.97(.36), Wald = 7.11, p = .008; race × education × anger-out predicting IL-6: B(SE) = −0.005(.002), Wald = 5.17, p = .023; race × education × anger-out predicting fibrinogen: B(SE) = −1.26(.52), Wald = 5.86, p = .015). Further, when trait anger was added in the models assessing the interactions with anger-out, none of the conclusions were altered (race × education × anger-out predicting IL-6: B(SE) = −.005(.002), Wald = 5.58, p = .018; race × education × anger-out predicting fibrinogen: B(SE) = −1.25(.52), Wald = 5.67, p = .017). Similarly, when anger-out was included in the significant model assessing interactions with trait anger, the findings were also unchanged (race × education × trait anger predicting fibrinogen: B(SE) = −0.98(.36), Wald = 7.40, p = .007).
Discussion
The primary objective was to examine racial differences in how different types of anger (trait anger, anger-out, and anger-control) moderated the association between educational attainment and two markers of inflammation, IL-6 and fibrinogen. For half of the tested interactions, the results revealed that among African American respondents, those with higher education and greater anger had elevated inflammatory profiles. In contrast, those with low education and high anger in the White sample had the highest levels of IL-6, although this trend just approached significance (p = .054). In addition for the White respondents, anger was negatively related to fibrinogen among those with higher education. These effects were significant after taking many key demographic and health variables into consideration. The specific findings just for the White respondents have already been discussed in greater detail in a prior publication [27]. However, overall, the combined analyses support the additional hypothesis that there are important racial differences in how anger experience and expression affect inflammatory physiology and its association with educational attainment.
With regard to trait anger and anger-out, opposite patterns emerged between college-educated Whites and African Americans. That is, anger was negatively related to fibrinogen among college educated White respondents, and positively related to fibrinogen among college educated African Americans. Highly educated White adults who express anger may do so as a symbol of their status and dominance [52], which may not be biologically costly. However, these psychosocial benefits and salubrious inflammatory correlates seen in educated Whites did not extend to African Americans, consistent with prior evidence that African Americans get less health “returns” from advanced educational attainment [35–38]. There may be possible social sanctions against African American men and women who express anger—such as being labeled with the “angry black woman/man” stereotype [53, 54]. The threat of this label may function to limit anger expression [53] and prompt careful tailoring of self-presentation, especially among middle class African Americans in primarily White contexts [55, 56]. The current data support the inflammatory costs of expressing anger for higher educated African Americans, perhaps related to these social sanctions.
Inflammatory dysregulation is a major contributor to the development and pathogenesis of age-related chronic diseases [4]. As an index of relative effect size, we compared differences in predicted IL-6 and fibrinogen at high trait anger and anger-out (one standard deviation above the mean) between high and low education groups among African American and White respondents separately as a function of age. We found that African Americans with higher education and high anger had inflammatory profiles indicative of being approximately 10 years older than less educated African Americans with high anger. This pattern was reversed among White respondents. That is, White respondents with more education and high anger had inflammatory profiles that were approximately 10 years younger than less educated White respondents with high anger.
Anger-in (i.e., anger suppression) was not examined given that there was no evidence of an association between anger-in and inflammation in the national sample [27], and there was no evidence of anger-control moderating racial or educational gradients in inflammation. But African Americans did report lower anger control than White respondents. Among White respondents, we previously found that anger control predicted lower IL-6 among women with a high school education or less only [27]. Small cell sizes preclude consideration of gender as an additional substantive variable within the African American sample. However, prior papers indicate that women use more anger diffusion strategies than men when angry [57], and evidence from the General Social Survey suggests that sense of control is more strongly related to lower anger intensity in African Americans than in Whites [58]. Thus, considering gender and racial differences concurrently is an important avenue for future work.
Why would higher, as compared to lower, educated African Americans show that high anger moderates their inflammatory profiles? One possibility is that higher educated African Americans may interact more frequently in racially integrated occupational situations that highlight and perhaps reinforce societal inequalities, while also underscoring the pressures and toll associated with social advancement. These experiences can contribute to feelings and expressions of anger, which may exact a physiological toll. African Americans with less education, on the other hand, may reside and work in less diverse settings and thus be protected from the same types of social threats. Although we did not find evidence of educational differences in the frequency of experiencing or expressing anger among African Americans, the results nonetheless point to possible physiological ramifications of anger, especially among the highly educated. Cose (1993) reported on interviews with African Americans who had achieved educational or occupational success but still felt that anger was evoked as a frequent reaction to perceived discrimination and inequitable treatment due to race [31]. Future work that considers other indicators of SES, such as employment status and occupational prestige, is warranted and may shed light on these ideas.
The role of discrimination, as a possible precursor to anger and inflammatory dysregulation, warrants further investigation, thus extending evidence of effects on stress-related hormones such as cortisol. In the same MIDUS sample, perceived discrimination predicted less healthy, flattened cortisol slopes across the day among Whites [59], and more healthy slopes among African Americans, supporting the view that awareness of racism may be protective among minority group members. However, in line with current findings, perceiving discrimination was less protective for higher (compared to lower) SES African Americans. Relatedly, it is known that African Americans are not as likely to experience other benefits of education advancement, including weight control and the opportunity for regular exercise. These differences may explain lingering effects on inflammatory physiology mediated through adiposity [36]. Thus, African Americans and other minority group members may experience fewer health benefits of being higher SES than Whites, due in part to racial discrimination and the ensuing anger [31, 60, 61].
Several limitations should be acknowledged. First, the African American sample was recruited primarily from one city, thus limiting our ability to generalize to all regions. Nonetheless, Milwaukee is an informative urban environment for studying anger and health, given that it is among the most segregated cities in the United States [28]. Second, we are unable to rule out acute infection status of MIDUS respondents, which may affect levels of inflammatory markers. However, there were no significant associations between body temperature at the time of the biological assessments and any of the predictor variables (p’s > .10), and fever is a standard sign of an acute inflammatory response. We note that very few MIDUS respondents presented with fever ≥37.5 °C (n = 11, < 1 %). Third, causality cannot be definitively delineated, given the cross-sectional design, although education is generally completed early in adulthood, and thus, is temporally antecedent to the midlife assessment of inflammatory markers. Using education as the sole index of SES is another limitation, given that there may be racial differences in returns of higher education. An important extension of this work will consider other indicators of SES, especially related to employment status and occupational prestige. Finally, several interactions were tested, given the analytic focus on several anger varieties and two inflammatory markers. Our findings underscore that not all features of anger have an equivalent, detrimental effect on inflammatory profiles, a conclusion that needs to be replicated and extended.
In summary, these analyses show that anger expression was associated with elevated IL-6 and fibrinogen among African American respondents with a college degree, comparable to the associations among White respondents with a high school education or less. An additional unique strength of the study was the inclusion of several dimensions of anger. It is clear that race, educational attainment, and perceptions about one’s status in society are critically important in understanding the biological concomitants of anger, a central aspect of emotional life.
References
Chida Y, Steptoe A. The association of anger and hostility with future coronary heart disease: A meta-analytic review of prospective evidence. J Am Coll Cardiol. 2009; 53(11): 936-946. doi:10.1016/j.jacc.2008.11.044.
Everson SA, Kaplan GA, Goldberg DE, Lakka TA, Sivenius J, Salonen JT. Anger expression and incident stroke: Prospective evidence from the Kuopio ischemic heart disease study. Stroke. 1999; 30(3): 523-528.
Schum JL, Jorgensen RS, Verhaeghen P, Sauro M, Thibodeau R. Trait anger, anger expression, and ambulatory blood pressure: A meta-analytic review. J Behav Med. 2003; 26(5): 395-415. http://www.ncbi.nlm.nih.gov/pubmed/14593850.
Ershler WB, Keller ET. Age-associated increased interleukin-6 gene expression, late-life diseases, and frailty. Annu Rev Med. 2000; 51: 245-270.
Everson-Rose SA, Lewis TT. Psychosocial factors and cardiovascular diseases. Annu Rev Public Health. 2005; 26: 469-500. doi:10.1146/annurev.publhealth.26.021304.144542.
Miller G, Chen E, Cole SW. Health psychology: Developing biologically plausible models linking the social world and physical health. Annu Rev Psychol. 2009; 60: 501-524. doi:10.1146/annurev.psych.60.110707.163551.
Ranjit N, Diez-Roux AV, Shea S, et al. Psychosocial factors and inflammation in the multi-ethnic study of atherosclerosis. Arch Intern Med. 2007; 167(2): 174-181. doi:10.1001/archinte.167.2.174.
Suarez EC. C-reactive protein is associated with psychological risk factors of cardiovascular disease in apparently healthy adults. Psychosom Med. 2004; 66(5): 684-691. doi:10.1097/01.psy.0000138281.73634.67.
Marsland AL, Prather AA, Petersen KL, Cohen S, Manuck SB. Antagonistic characteristics are positively associated with inflammatory markers independently of trait negative emotionality. Brain Behav Immun. 2008; 22(5): 753-761. doi:10.1016/j.bbi.2007.11.008.
Shivpuri S, Gallo LC, Mills PJ, Matthews KA, Elder JP, Talavera GA. Trait anger, cynical hostility and inflammation in Latinas: Variations by anger type? Brain Behav Immun. 2011; 25(6): 1256-1263. doi:10.1016/j.bbi.2011.04.016.
Carroll JE, Low CA, Prather AA, et al. Negative affective responses to a speech task predict changes in interleukin (IL)-6. Brain Behav Immun. 2011; 25(2): 232-238. doi:10.1016/j.bbi.2010.09.024.
Elovainio M, Merjonen P, Pulkki-Råback L, et al. Hostility, metabolic syndrome, inflammation and cardiac control in young adults: The young Finns study. Biol Psychol. 2011; 87(2): 234-240. doi:10.1016/j.biopsycho.2011.03.002.
Graham JE, Robles TF, Kiecolt-Glaser JK, Malarkey WB, Bissell MG, Glaser R. Hostility and pain are related to inflammation in older adults. Brain Behav Immun. 2006; 20(4): 389-400. doi:10.1016/j.bbi.2005.11.002.
Janicki-Deverts D, Cohen S, Doyle WJ. Cynical hostility and stimulated Th1 and Th2 cytokine production. Brain Behav Immun. 2010; 24(1): 58-63. doi:10.1016/j.bbi.2009.07.009.
Eaker ED, Sullivan LM, Kelly-Hayes M, D’Agostino RB, Benjamin EJ. Anger and hostility predict the development of atrial fibrillation in men in the Framingham offspring study. Circulation. 2004; 109(10): 1267-1271. doi:10.1161/01.CIR.0000118535.15205.8F.
Haukkala A. Socioeconomic differences in hostility measures- a population based study. Psychol Health. 2002; 17(2): 191-202.
Schieman S. Education and the activation, course, and management of anger. J Health Soc Behav. 2000; 41(1): 20-39.
Schieman S. The sociological study of anger: Basic social patterns and contexts. In: Potegal M, Stemmler G, Spielberger C, eds. International Handbook of Anger. New York: Springer Science + Business Media, LLC; 2010: 329-348.
Adler NE, Rehkopf DH. U.S. disparities in health: Descriptions, causes, and mechanisms. Annu Rev Public Health. 2008; 29: 235-252. doi:10.1146/annurev.publhealth.29.020907.090852.
Koster A, Bosma H, Penninx BWJH, et al. Association of inflammatory markers with socioeconomic status. J Gerontol Ser A Biol Sci Med Sci. 2006; 61A(3): 284-290.
Friedman EM, Herd P. Income, education, and inflammation: Differential associations in a national probability sample (The MIDUS study). Psychosom Med. 2010; 72(3): 290-300. doi:10.1097/PSY.0b013e3181cfe4c2.
Morozink JA, Friedman EM, Coe CL, Ryff CD. Socioeconomic and psychosocial predictors of interleukin-6 in the MIDUS national sample. Health Psychol. 2010; 29(6): 626-635. doi:10.1037/a0021360.
Ranjit N, Diez-Roux AV, Shea S, Cushman M, Ni H, Seeman T. Socioeconomic position, race/ethnicity, and inflammation in the multi-ethnic study of atherosclerosis. Circulation. 2007; 116(21): 2383-2390. doi:10.1161/CIRCULATIONAHA.107.706226.
Gruenewald TL, Cohen S, Matthews KA, Tracy R, Seeman TE. Association of socioeconomic status with inflammation markers in black and white men and women in the Coronary Artery Risk Development in Young Adults (CARDIA) study. Soc Sci Med. 2009; 69(3): 451-459. doi:10.1016/j.socscimed.2009.05.018.
Merjonen P, Pulkki-Råback L, Puttonen S, et al. Anger is associated with subclinical atherosclerosis in low SES but not in higher SES men and women. The cardiovascular risk in young Finns study. J Behav Med. 2008; 31(1): 35-44. doi:10.1007/s10865-007-9131-6.
Beatty DL, Matthews KA. Unfair treatment and trait anger in relation to nighttime ambulatory blood pressure in African American and white adolescents. Psychosom Med. 2009; 71(8): 813-820. doi:10.1097/PSY.0b013e3181b3b6f8.
Boylan JM, Ryff CD. Varieties of anger and the inverse link between education and inflammation: Toward an integrative framework. Psychosom Med. 2013; 75(6): 566-574. doi:10.1097/PSY.0b013e31829683bd.
Frey WH. 100 Largest Metros: Black White Segregation Indices Sorted by 2005–9 Segregation.; 2010. http://www.psc.isr.umich.edu/dis/census/segregation.html.
Slopen N, Lewis TT, Gruenewald TL, et al. Early life adversity and inflammation in African Americans and whites in the midlife in the United States survey. Psychosom Med. 2010; 72(7): 694-701. doi:10.1097/PSY.0b013e3181e9c16f.
Slopen N, Dutra L, Williams DR, et al. Psychosocial stressors and cigarette smoking among African American adults in midlife. Nicotine Tob Res. 2012; 14(10): 1161-1169.
Cose E. The rage of a privileged class: Why are middle-class Blacks angry? Why should America care? New York: Harper Perennial; 1993.
Williams DR, John DA, Oyserman D, Sonnega J, Mohammed SA, Jackson JS. Research on discrimination and health: An exploratory study of unresolved conceptual and measurement issues. Am J Public Health. 2012; 102(5): 975-978. doi:10.2105/AJPH.2012.300702.
U.S. Census Bureau. The big payoff: Educational attainment and synthetic estimates of work-life earnings. 2002. http://www.census.gov/prod/2002pubs/p23-210.pdf.
Williams DR, Collins C. US socioeconomic and racial differences in health: Patterns and explanations. Annu Rev Sociol. 1995; 21: 349-386.
Braveman PA, Cubbin C, Egerter S, Williams DR, Pamuk E. Socioeconomic disparities in health in the United States: What the patterns tell us. Am J Public Health. 2010; 100(Suppl): S186-S196. doi:10.2105/AJPH.2009.166082.
Lewis TT, Everson-Rose SA, Sternfeld B, Karavolos K, Wesley D, Powell LH. Race, education, and weight change in a biracial sample of women at midlife. Arch Intern Med. 2005; 165(5): 545-551. doi:10.1001/archinte.165.5.545.
Schoendorf K, Hogue C, Kleinman J, Rowley D. Mortality among infants of black as compared with white college-educated parents. N Engl J Med. 1992; 326: 1522-1526.
Albano JD, Ward E, Jemal A, et al. Cancer mortality in the United States by education level and race. J Natl Cancer Inst. 2007; 99(18): 1384-1394. doi:10.1093/jnci/djm127.
Brim OG, Ryff CD, Kessler RC. How healthy are we: A national study of well-being at midlife. Chicago: The University of Chicago Press; 2004.
Radler BT, Ryff CD. Who participates? Accounting for longitudinal retention in the MIDUS national study of health and well-being. J Aging Health. 2010; 22(3): 307-331. doi:10.1177/0898264309358617.
Love GD, Seeman TE, Weinstein M, Ryff CD. Bioindicators in the MIDUS national study: Protocol, measures, sample, and comparative context. J Aging Health. 2010; 22(8): 1059-1080. doi:10.1177/0898264310374355.
Spielberger CD. State-trait anger expression inventory: Professional manual. Odessa, FL; 1996.
O’Connor M-F, Bower JE, Cho HJ, et al. To assess, to control, to exclude: Effects of biobehavioral factors on circulating inflammatory markers. Brain Behav Immun. 2009; 23(7): 887-897. doi:10.1016/j.bbi.2009.04.005.
Mohamed-Ali V, Goodrick S, Rawesh A, et al. Subcutaneous adipose tissue releases interleukin-6, but not tumor necrosis factor-alpha, in vivo. J Clin Endocrinol Metab. 1997; 82(12): 4196-4200.
Jain MK, Ridker PM. Anti-inflammatory effects of statins: Clinical evidence and basic mechanisms. Nat Rev Drug Discov. 2005; 4(12): 977-987. doi:10.1038/nrd1901.
Kenis G, Maes M. Effects of antidepressants on the production of cytokines. Int J Neuropsychopharmacol. 2002; 5: 401-412.
Libby P. Inflammation in atherosclerosis. Nature. 2002; 420: 868-874.
Jaccard J, Turrisi R. Interaction Effects in Multiple Regression. 2nd ed. Thousand Oaks, CA: Sage; 2003.
Coe CL, Love GD, Karasawa M, et al. Population differences in proinflammatory biology: Japanese have healthier profiles than Americans. Brain Behav Immun. 2011; 25(3): 494-502. doi:10.1016/j.bbi.2010.11.013.
Radloff LS. The CES-D scale: A self-report depression scale for research in the general population. Appl Psychol Meas. 1977; 1(3): 385-401.
Spielberger CD, Sydeman SJ. State-trait anxiety inventory and state-trait anger expression inventory. In: Maruish ME, ed. The Use of Psychological Testing for Treatment Planning and Outcome Assessment. 1st ed. Mahwah, NJ: Lawrence Erlbaum Associates; 1994: 292-321.
Tiedens LZ. Anger and advancement versus sadness and subjugation: The effect of negative emotion expressions on social status conferral. J Pers Soc Psychol. 2001; 80(1): 86-94.
Harvey WA. The modern mammy and the angry black man: African American professionals’ experiences with gendered racism in the workplace. Race Gender Cl. 2007; 14: 196-212.
Jackson BA, Harvey WA. Getting angry to get ahead: Black college men, emotional performance, and encouraging respectable masculinity. Symb Interact. 2013; 36(3): 275-292. doi:10.1002/symb.63.
Feagin JR, Sikes MP. Living with racism: The Black middle-class experience. Beacon Press; 1994:398.
Lacy KR. Blue-chip Black: Race, class, and status in the new Black middle class. University of California Press; 2007:302.
Linden W, Hogan BE, Rutledge T, Chawla A, Lenz JW, Leung D. There is more to anger coping than “in” or “out”. Emotion. 2003; 3(1): 12-29. doi:10.1037/1528-3542.3.1.12.
Mabry JB, Kiecolt KJ. Anger in black and white: Race, alienation, and anger. J Health Soc Behav. 2005; 46(1): 85-101. doi:10.1177/002214650504600107.
Fuller-Rowell TE, Doan SN, Eccles JS. Differential effects of perceived discrimination on the diurnal cortisol rhythm of African Americans and Whites. Psychoneuroendocrinology. 2012; 37(1): 107-118. doi:10.1016/j.psyneuen.2011.05.011.
Gee GC. A multilevel analysis of the relationship between institutional and individual racial discrimination and health status. Am J Public Health. 2002; 92: 615-623.
Yen IH, Ragland DR, Greiner BA, Fisher JM. Workplace discrimination and alcohol consumption: Findings from the San Francisco Muni health and safety study. Ethn Dis. 1999; 9(1): 70-80.
Authors’ Statement of Conflict of Interest and Adherence to Ethical Standards
Authors Jennifer Morozink Boylan, Tené T. Lewis, Christopher L. Coe, and Carol D. Ryff declare that they have no conflict of interest. All participants provided written informed consent. All procedures followed were in accordance with the American Psychological Association ethical standards and with the Helsinki Declaration. This study was approved by the Institutional Review Boards at University of Wisconsin-Madison, as well as at Georgetown University and the University of California, Los Angeles.
Author information
Authors and Affiliations
Corresponding author
Additional information
Author Note
This research was supported by a grant from the National Institute on Aging (P01-AG020166) to conduct a longitudinal follow-up of the MIDUS investigation. The original study was supported by the John D. and Catherine T. MacArthur Foundation Research Network on Successful Midlife Development. J.M.B. was supported by a training grant from the National Institute of Child Health and Human Development (2T32HD049302-06). We thank the staff of the Clinical Research Centers at the University of Wisconsin- Madison, UCLA, and Georgetown University for their support in conducting this study. Supported by the following grants M01-RR023942 (Georgetown), M01-RR00865 (UCLA) from the General Clinical Research Centers Program and 1UL1RR025011 (UW) from the Clinical and Translational Science Award (CTSA) program of the National Center for Research Resources, National Institutes of Health. The authors wish to thank Gayle Love, Barry Radler, and Dorothy Brar for their commitment and continual support to the MIDUS project.
About this article
Cite this article
Boylan, J.M., Lewis, T.T., Coe, C.L. et al. Educational Status, Anger, and Inflammation in the MIDUS National Sample: Does Race Matter?. ann. behav. med. 49, 570–578 (2015). https://doi.org/10.1007/s12160-015-9687-2
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12160-015-9687-2