Abstract
Purpose
The development of radioimmunotherapy has provided an impressive alternative approach in improving trastuzumab therapy. However, the mechanisms of trastuzumab and radiation treatment combined to increase therapeutic efficacy are poorly understood. Here, we try to examine the efficacy of cytotoxicity and apoptosis induction for 188Re-HYNIC-trastuzumab in cancer cell lines with various levels of Her2.
Materials and methods
Fluorescence flow cytometry was used to detect the alterations of apoptosis induction after 188Re-HYNIC-trastuzumab treatment in two breast cancer cell lines with different levels of HER2 (BT-474 and MCF-7) and a colorectal carcinoma cell line (HT-29) for control.
Results
Our results indicated that 188Re-HYNIC-trastuzumab led to cell death of breast cancer cells specifically in HER2 level-dependent and radioactivity dose-dependent fashions. In BT-474 cells, 370 kBq/ml of 188Re-HYNIC-trastuzumab enhanced the cytotoxicity to a level nearly 100-fold that of trastuzumab-alone treatment. The results also revealed that the mitochondria-dependent pathway attenuated irradiation-induced apoptosis in HER2-expressing breast cancer cells after 188Re-HYNIC-trastuzumab treatment. In contrast, only after 48 h of 188Re-HYNIC-trastuzumab treatment, BT-474 cells exhibited typical apoptotic changes, including exposure of phospholipid phosphatidylserine on the cell surface, or fragmented DNA formation, in a radioactivity dose-dependent manner.
Conclusion
Briefly, our study demonstrates that 188Re-labeled HYNIC-trastuzumab not only enhances cell death in a radioactivity dose-dependent fashion, but may also prolong the effects of apoptosis involved with the mitochondria-dependent pathway in HER2-overexpressing breast cancer cells. It is possible that the 188Re-HYNIC-trastuzumab treatment induced a second round of apoptosis to prolong the effects of cell kill in these cancer cells. These data revealed that 188Re-HYNIC-trastuzumab has the potential for use as a therapeutic radiopharmaceutical agent in HER2-overexpressing breast cancer cell treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Breast cancer is the second most common type of cancer and the fifth most common cause of cancer death worldwide [1]. Breast tumors are routinely checked for overexpression of human epidermal growth factor receptor-2 (HER2) [2, 3]. HER2, a 185-kDa transmembrane glycoprotein, belongs to the epidermal growth factor family of receptor tyrosine kinases [4]. HER2 overexpression is an adverse prognostic factor in breast cancers, and is estimated to occur in 25–30 % of human breast cancers [5]. HER2 is notable for its role in the pathogenesis of breast cancer that is associated with increased disease recurrence and worse prognosis [5–7]. Since HER2 is related to tumor cell invasion, metastasis and poor prognosis, it is a potentially attractive therapeutic target [7]. Clinically, HER2 is important as the target of the monoclonal antibody trastuzumab (Herceptin®).
Trastuzumab is a humanized IgG1 that recognizes the extracellular domain of the HER2/neu oncoprotein and is indicated for the immunotherapy of HER2-positive breast cancers. Trastuzumab is effective in treatment of breast cancer where the HER2 receptor is overexpressed and shows activity in human trials of women with metastatic breast cancer [8–11]. Although trastuzumab approval for breast cancer treatment represents an important advance, the issue that the majority of cases of advanced disease are resistant to trastuzumab remains unresolved [9, 12].
The development of radioimmunotherapy (RIT) has provided an impressive alternative approach in improving trastuzumab therapy [13]. Trastuzumab serving as a targeting attachment for selective desorption of radionuclide in tumor therapy has been reported in several previous studies [14–19]. However, the mechanisms of trastuzumab and radiation treatment acting in combination to increase therapeutic efficacy are poorly understood.
Previous studies have suggested that apoptosis pathways are involved in the therapeutic action of trastuzumab [9, 10, 12]. Irradiation has also been shown to induce apoptosis and to activate apoptosis pathways [20, 21]. Apoptosis may be initiated through different pathways such as the death receptor (extrinsic) pathway or the mitochondrial (intrinsic) pathway, resulting in a range of events from early to late phases [21, 22]. These events include rapid redistribution and exposure of the anionic phospholipid phosphatidylserine (PS) on the cell surface, spliced or fragmented DNA formation, and serial proteins activated in apoptosis signaling, eventually leading to morphologic changes and cell death [4, 9]. In order to provide a molecular basis for the design of new strategies to overcome tumor resistance to apoptosis, it is necessary to identify the apoptotic mechanism and understand its regulation.
Recently, 6-hydrazinopyridine-3-carboxylic acid (HYNIC) conjugated with trastuzumab has been labeled with Tc-99m and the imaging values have been employed in tumor targeting [23]. 188Re is an attractive radionuclide for use in targeted radiotherapy due to the favorable physical characteristics of high-energy beta particles (E max = 2.11 MeV) and 155 keV gamma photons in 15.88 % abundance [19]. In the present study, we used HYNIC as a bifunctional chelater (BFC) to conjugate with trastuzumab and then labeled it with 188Re isotope. Further, we examined the efficacy of apoptosis induction for 188Re-HYNIC-trastuzumab in two breast cancer cell lines with different levels of HER2 (BT-474 and MCF-7) and one contrasting colorectal carcinoma cell line (HT-29) by using a set of flow cytometry detection assays.
Materials and methods
Materials
Most of the chemicals used in this study were of analytical grade obtained from commercial sources. HYNIC (6-hydrazinopyridine-3-carboxylic acid) was synthesized at the Institute of Nuclear Energy Research, Taiwan (INER), following the reported method [24]. The high radionuclide and radiochemical purity of the 188Re-perrhenate solution was eluted from 188W/188Re generator which was manufactured by INER.
Preparation of 188Re-HYNIC-trastuzumab
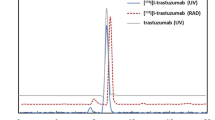
Carrier-free 188Re was eluted with normal saline from a 188W/188Re generator. Glucohepatonate (GH) (50 mg/ml) and SnCl2 (5 mg/ml) were reacted with 188Re-perrhenate solution for 30 min. HYNIC-trastuzumab (1 mg/ml) was added to the solution and reacted for 1 h at room temperature. The radiochemical purity of 188Re-HYNIC-trastuzumab was determined by an instant thin-layer chromatography system (ITLC). The analytical system uses ITLC-SG as the stationary phase and normal saline results in the separation of ReO4 − (R f = 1) from 188Re-HYNIC-trastuzumab and colloidal 188Re. When albumin-presoaked silica gel is used as the stationary phase and the solution of ethanol:ammonia:water (2:1:5) as the mobile phase, ReO4 − and 188Re-HYNIC-trastuzumab migrate with an R f of 1.0, whereas colloidal 188Re remains at the origin. The labeling efficiency was analyzed by a radio-TLC scanner (AR2000, Bioscan, Inc., Washington, DC, USA).
Cell lines and culture conditions
The human breast cancer cell lines MCF-7, BT-474 and the human colorectal cancer cell line HT-29 were obtained from the American Type Tissue Culture Collection (ATCC, Rockville, MA, USA). The MCF-7 cell line was maintained in minimal essential medium (MEM) (GIBCO/Invitrogen, Grand Island, NY, USA) containing 10 % FCS. The BT-474 cell line was cultured with 90 % modified Dulbecco’s medium (American Type Culture Collection, Manassas, VA, USA) and then mixed with 10 % fetal bovine serum and 30 ng/ml epidermal growth factor. The HT-29 cell line was cultured in RPMI-1640 medium (GIBCO/Invitrogen, Grand Island, NY, USA) containing 10 % FCS. All cells were maintained at 37 °C in a humidified, 5 % CO2 atmosphere. Subconfluent cells were harvested after brief incubation with trypsin (0.05 %, w/v)/EDTA (0.02 %, w/v) (Sigma).
For flow cytometric analysis, growing cells were trypsinized and then incubated with 5 μg/ml FITC anti-human erbB2/HER2 monoclonal antibodies (BioLegend, San Diego, CA, USA) at 4 °C for 30 min. After the cells were washed twice with PBS, the fluorescence staining of HER2 was assayed by an FACS flow cytometer (Becton-Dickinson Biosciences, San Jose, CA, USA) and the data were collected and analyzed using CellQuest Software (Becton-Dickinson Biosciences).
Treatment of cells with trastuzumab and 188Re-HYNIC-trastuzumab
All of the cell lines were incubated at 2 × 106 cells/well for subsequent cell culture. Cells were cultured in medium for 1 h before treatment. To assess trastuzumab-mediated cytotoxicity and apoptosis, cells were cultured in the presence of three serial doses (1, 10 and 100 μg/ml) of trastuzumab or were left untreated. Cells were incubated at 37 °C after 24 or 48-h treatments in cell culture media, then washed and further cultured in fresh medium for 24 h. These cells were collected and used for FACS flow cytometric analysis.
Similarly, three different doses of radioactivity (37, 370 and 740 kBq/ml) of 188Re labeled with HYNIC-trastuzumab (1 μg/ml) were added to wells containing 2 × 106 cells/well in 2 ml amounts of cell culture media for each cell line. Controls were treated in the same 24-well plate for each experiment and consisted of medium alone, unlabeled trastuzumab in a concentration of 1 μg/ml and 188Re isotope only (740 kBq/ml), respectively. The samples were then incubated for 24 or 48 h in a 5 % CO2 incubator at 37 °C. The cells were then washed and further cultured in fresh medium for another 24 h. FACS flow cytometric analysis was performed immediately after cell culturing.
Flow cytometric analysis of cytotoxicity and apoptosis
The cell death rates were detected by the BD Cell Viability Kit (BD Biosciences, San Jose, CA, USA). The cultured cells were washed twice with 4 ml cold PBS and resuspended. Then, 4.0 μl of thiazole orange (TO) solution was added for staining of all cells and 2.0 μl of propidium iodide (PI) for staining dead cells to 2 ml of cell suspension. Cells were vortexed and incubated for 5 min at room temperature and then detected by flow cytometry. Data shown are frequencies calculated from cell death rates as follows: −100 × [experimental dead cells (%) − control dead cells (%)]/[1 − control dead cells (%)]. The cells that received no treatment were used for control groups.
To confirm the different phases of apoptosis in the treated cells, flow cytometry was used for the early monitoring of Annexin V and TUNEL staining was used for monitoring of the later stage. For detection of Annexin V, cells were washed twice and resuspended in 100 μl of cold PBS. The cells were incubated with 5 μl of Annexin V-FITC (BD Pharmingen™, San Jose, CA, USA), then gently vortexed and incubated for 15 min at RT in the dark. Then, 200 μl PBS were added and cells were analyzed by flow cytometry within 1 h.
For detection of cell apoptosis by TUNEL assay, the free 3′-OH terminal was labeled with modified fluorescence-labeled nucleotides (dUTP) by catalysis of the enzyme terminal deoxynucleotidyl transferase (TdT). 100 μl of suspended cells was washed in PBS 3 times and fixed with 4 % paraformaldehyde for 1 h at 37 °C. After the cells were washed once with PBS, they were permeabilized (0.1 % Triton X-100 in 0.1 % sodium citrate) for 5 min on ice. The cells were then washed twice with PBS and incubated in 50 μl of TUNEL reaction mixture (BD Pharmingen™, San Jose, CA) for 2 h at 37 °C in the dark. Finally, the cells were washed twice in blocking buffer (0.1 % Triton X-100 in 0.5 % bovine serum albumin), and the labeled DNA fragments were visualized and measured by flow cytometry.
Detection of mitochondrial membrane potential change by flow cytometry
The intrinsic mitochondria-dependent pathway during apoptosis was measured using a JC-1 Mitochondrial Membrane Potential Detection Kit (BD Pharmingen™, San Jose, CA, USA) by flow cytometry as described by the manufacturer. In brief, the cultured cells were washed twice with cold PBS and resuspended. Then 0.5 ml of freshly prepared JC-1 Working Solution was added to each tube and cells were gently resuspended. The cells were then incubated in JC-1 Working Solution for 15 min at 37 °C in a CO2 incubator. Cells were washed twice following incubation and 2 ml of 1× assay buffer was added to each tube. Cells were gently resuspended and then centrifuged at 400×g for 5 min after which the supernatant was discarded. Cells were then resuspended in 0.5 ml of 1× assay buffer and analyzed by flow cytometry.
Immunoreactivity studies
Immunoreactivity studies were performed using the method as described by Lindmo et al. [25]. In short, approximately 2 × 106 BT-474 cells and MCF-7 cells were added separately into 24-well plates and incubated with 2 ml amounts of cell culture media containing 188Re-HYNIC-trastuzumab (370 kBq/1 μg/ml) at 37 °C for 1, 4 and 24 h, respectively. After incubation, the cells were spun down by centrifugation at 1,000×g for 10 min and the supernatants were removed. Then radioactivity in the pellets and supernatants was measured in a gamma counter (Perkin Elmer, Waltham, MA, USA) and the percentage of effective binding radioactivity was calculated as follows: 100 % × [radioactivity in the pellets/radioactivity in the pellets + radioactivity in the supernatants].
Statistical analysis
Statistical differences between groups of tests and controls were determined using the Mann–Whitney U test, and were expressed as p values. A p value of ≤0.05 was considered statistically significant.
Results
HER2 expression of BT-474, MCF-7 and HT-29 cell lines
The cell surface expression level of Her2 was tested by flow cytometric analysis. Figure 1A depicts the fluorescence intensity histograms of the three cell lines labeled with FITC anti-human HER2 mAb. The percentage of BT-474 cells with high fluorescence intensity was 98.45 %, whereas the percentages of MCF-7 (0.23 %) and HT-29 cells (0.39 %) with high fluorescence intensity were miniscule. Our results indicated that HER2 was overexpressed in the BT-474 cell line and low expressed in MCF-7 and HT-29 cell lines in our experimental environment.
The affinity of cell binding on Her2 receptor of different cell line. a Expression of Her2 protein in BT-474, MCF-7 and HT-29 cells by flow cytometric analysis. FITC-conjugated mouse anti-human erbB2/HER2 immunoglobulin was used to stain HER2 proteins on all of the cell surfaces. Histograms depict the frequencies of Her2-expressed cells from different cell lines. The numbers on each histogram represent the mean frequencies. The data shown is representative of a typical result. b Comparison of 188Re-HYNIC-trastuzumab binding affinity between BT-474 and MCF-7 breast cancer cell lines. The cell-binding percentages of 188Re-HYNIC-trastuzumab on BT-474 (black bars) and MCF-7 (white bars) were measured with respect to the total amount of radioactivity added to incubation media. Data from three separate experiments are expressed as the mean ± SEM. *p < 0.05, **p < 0.01 when compared between two breast cancer cell lines
Labeling and immunoreactivity study of 188Re-HYNIC-trastuzumab
After the reaction of 188Re-perrhenate with GH and stannous chloride, HYNIC-trastuzumab (1 mg/ml) was added to the 188Re-GH solution in order to obtain the final product of 188Re-HYNIC-trastuzumab. The radio thin-layer chromatographs of 188Re-HYNIC-trastuzumab obtained 1 h after mixing 188Re and HYNIC-trastuzumab at room temperature showed that the 94.5 % radioactivity stayed at the origin site in the normal saline system, while in the albumin-presoaked ITLC-SG developing system, most of the radioactivity moved to the solvent front position with few colloids. The radiochemical purity (RCP) of 188Re-HYNIC-trastuzumab was more than 90 % in the radio-TLC system. In receptor-binding assays, the binding percentage of 188Re-HYNIC-trastuzumab in BT-474 cells had reached 60.77 and 77.42 % of the incubation radioactivity in the medium at 1 and 4 h, respectively, significantly higher than 18.97 and 25.23 % of MCF-7 cells (Fig. 1b) (p < 0.05). After 24 h, there was still an around 1.5-fold significant superiority in the receptor-binding affinity for 188Re-HYNIC-trastuzumab to BT-474 cells compared with that in MCF-7 cells, with which the immunoreactivity of 62.18 % was achieved (Fig. 1b) (p < 0.05).
Detection of apoptosis induction by trastuzumab in different HER2-expressing breast cancer cells
Fluorescence flow cytometry was used to detect the alterations of apoptosis induction after trastuzumab treatment in the two breast cancer cell lines with different levels of HER2 (BT-474 and MCF-7) and a colorectal carcinoma cell line (HT-29) for control. As shown in Fig. 2, the cell death rate of BT-474 cells increased significantly in a dose-dependent manner after 24 h of trastuzumab treatment. The results were similar to those obtained 48 h after trastuzumab treatment initiation (p < 0.05). In contrast, the cell death rate of MCF-7 cells only increased in the groups that were treated with 100 μg of trastuzumab for 48 h. In addition, there was no difference in the percentages of HT-29 cells after trastuzumab treatment.
Comparison of trastuzumab-induced mortality in BT-474, MCF-7 and HT-29 cells by FACS analysis. BT-474, MCF-7 and HT-29 cells were treated with different doses of trastuzumab as indicated. The cells treated with different doses of trastuzumab were removed and replaced with new media after 24 or 48-h treatments. Twenty-four hours after treatment, the percentage of dead cells was measured by FACS analysis. Data from 3 to 5 separate experiments are expressed as the mean ± SEM. *p < 0.05 when compared with the normal control, respectively
In order to observe further effects of apoptotic activation, we performed flow cytometry to detect the cells stained positively for Annexin V and TUNEL assay. Trastuzumab was found to induce a dose-dependent effect of apoptosis in breast cancer cells, as seen in Fig. 3. A significant increase of BT-474 cells in TUNEL assay occurred at 24 h after 100 μg of treatment (Fig. 3b). Forty-eight hours after treatment initiation, the percentages of positive cells in the apoptotic induction were similar in the control and treatment samples of BT-474 cells, except the 100 μg group. In contrast, the apoptotic activations, including Annexin V and DNA fragmentation in MCF-7 cells, were significantly enhanced after 48 h of treatment. In addition, all apoptotic detections of HT-29 cells among treated cells were similar to those of control cells (Fig. 3). Further, we investigated whether mitochondria could play a role in trastuzumab-induced apoptosis by observing changes in mitochondrial membrane potential. The changes in the membrane potential of BT-474 cells increased significantly in a dose-dependent manner after 24 and 48 h of trastuzumab treatment. However, the changes in the membrane potential of MCF-7 cells only increased dose-dependently after 48 h of trastuzumab treatment (Fig. 3c). After examining all the data, we chose 1 μg of trastuzumab for radiolabeling of antibodies in further experiments. Since the effects of trastuzumab-induced apoptosis in the groups treated with 1 μg were weaker and there was no significant difference here, it may be more appropriate to use this dosage in evaluating the highlighted efficacy of targeted radiotherapy with trastuzumab.
Comparison of different trastuzumab-induced apoptosis phenotypes in BT-474, MCF-7 and HT-29 cells by FACS analysis. BT-474, MCF-7 and HT-29 cells were treated with different doses of trastuzumab as indicated. The cells treated with different doses of trastuzumab were removed and replaced with new media after 24 or 48-h treatments. Twenty-four hours after irradiation, the percentages of a Annexin V positive cells, b apoptotic cells with fragmented nuclei and c mitochondrial membrane potential depolarization were measured by FACS analysis, respectively. Data from 3 to 5 separate experiments are expressed as the mean ± SEM. *p < 0.05, **p < 0.01 when compared with the normal control, respectively
Increased effects of 188Re-HYNIC-trastuzumab on cell death of HER2-overexpressing breast cancer cells
The two human breast cancer cell lines and one colorectal cancer cell line were incubated with increasing activity doses of 188Re-HYNIC-trastuzumab from 37, 370 to 740 kBq for 24 and 48 h following 188Re-HYNIC-trastuzumab treatment; another group was incubated with 740 kBq 188Re for isotope control. BT-474 cells showed markedly elevated cell death rates in a radioactivity dose-dependent fashion. Increasing the radioactivity dose from 37 to 740 kBq caused a proportional augmentation of cell death at 24 h from 65 % at 37 kBq to 86 % at 740 kBq and at 48 h from 77 % at 37 kBq to 86 % at 740 kBq (p < 0.05) (Fig. 4). In comparison, 740 kBq 188Re, which was diluted in medium and not bound to trastuzumab, only caused 57 and 64 % cell death at 24 and 48 h, respectively. But, treatment with 740 kBq 188Re caused up to 50 % cell death of MCF-7 cells at 24 h, which was significantly higher than the other groups at this time period (p < 0.05).
Comparison of 188Re-HYNIC-trastuzumab-induced mortality in BT-474, MCF-7 and HT-29 cells by FACS analysis. BT-474, MCF-7 and HT-29 cells were treated with different activity doses of 188Re-HYNIC-trastuzumab or trastuzumab alone (1 μg) or 188Re alone as indicated. The cells treated with different doses of 188Re-HYNIC-trastuzumab were removed and replaced with new media after 24 or 48-h treatments. Twenty-four hours after irradiation, the percentage of dead cells was measured by FACS analysis. The percentage of cell death was calculated as described in the text. Data from 3 to 5 separate experiments are expressed as the mean ± SEM. *p < 0.05, **p < 0.01 when compared with the normal control, respectively. # p < 0.05 when compared with the trastuzumab-only group as negative control, respectively
The inhibitory rates of 188Re-radiolabeled trastuzumab were also increased, respectively, at 24 h from nearly 40 % at 37 kBq to 86 % at 740 kBq or at 48 h from nearly 23 % at 37 kBq to 38 % at 740 kBq, which were both higher than the 19 % at 24 h and 10 % at 48 h with trastuzumab treatment only (Table 1). On the other hand, 188Re-HYNIC-trastuzumab treatment in MCF-7 cells revealed only slightly elevated cell death rates at 24 h with no dose-dependence on radioactivity and no increase at 48 h. Additionally, treating cells with 740 kBq 188Re alone increased the cell death rates of the two breast cancer cell lines to 20 % at 24 h, and then decreased these rates at 48 h. Moreover, the number of HT-29 cells increased and there were negative inhibitory rates at either 24 or 48 h after 188Re-HYNIC-trastuzumab treatment (Table 1).
188Re-HYNIC-trastuzumab treatment results in increased apoptosis induction
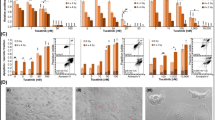
The above-mentioned data revealed that 188Re-HYNIC-trastuzumab treatment caused an increase in cell death. To address the issue of cell death through apoptosis, a set of apoptosis detection assays was assessed. After 188Re-HYNIC-trastuzumab treatment, BT-474 cells showed typical apoptotic changes at 48 h in a radioactivity dose-dependent manner, i.e., exposure of the anionic PS on the cell surface or DNA fragmentation. Annexin V staining showed that after 48 h of 188Re-HYNIC-trastuzumab treatment the number of apoptotic cells was increased from 38.37 ± 1.35 at 37 kBq to 74.46 ± 14.77 at 740 kBq (p < 0.05), and the apoptotic cells detected in the TUNEL assay were increased from nearly 78.52 ± 7.02 at 37 kBq to 91.45 ± 4.03 at 740 kBq (p < 0.05). All of the results were significantly higher than those of the trastuzumab-only group (p < 0.05) or the 188Re-only group (Fig. 5a, b). In contrast, no apparent apoptotic induction was observed in MCF-7 cells when 188Re-HYNIC-trastuzumab treatment was compared to trastuzumab-only treatment. The apoptotic effects in MCF-7 cells were only observed after 740 kBq 188Re-only treatment for 48 h (p < 0.05). In HT-29 cells treated with 188Re-HYNIC-trastuzumab, the tendency was different with breast cancer cells and a decrease in cells stained positively for TUNEL was even observed (Fig. 5). Furthermore, in mitochondrial membrane potential detecting experiments, the percentages of BT-474 cells were greatly enhanced in a radioactivity dose-dependent manner after 24-h post-treatment with 188Re-HYNIC-trastuzumab, when compared to either the trastuzumab-alone group or the control group (p < 0.05). And after 48 h with 188Re-HYNIC-trastuzumab treatment, the MCF-7 cell levels were significantly higher only at 740 kBq treated group. A similar tendency was found in HT-29 cells after 24 h of 188Re-HYNIC-trastuzumab treatment, especially at 370 and 740 kBq. Also, the mitochondrial effects of MCF-7 cells were significantly induced in the 740 kBq 188Re-only group, to an even higher degree than that with 188Re-HYNIC-trastuzumab treatment (p < 0.05) (Fig. 5c).
Comparison of different 188Re-HYNIC-trastuzumab-induced apoptosis phenotypes in BT-474, MCF-7 and HT-29 cells by FACS analysis. BT-474, MCF-7 and HT-29 cells were treated with different activity doses of 188Re-HYNIC-trastuzumab or trastuzumab alone (1 μg) or 188Re alone as indicated. The cells treated with different doses of 188Re-HYNIC-trastuzumab were removed and replaced with new media after 24 or 48-h treatments. Twenty-four hours after irradiation, the percentages of a Annexin V positive cells, b apoptotic cells with fragmented nuclei and c mitochondrial membrane potential depolarization were measured by FACS analysis, respectively. Data from 3 to 5 separate experiments are expressed as the mean ± SEM. *p < 0.05, **p < 0.01 when compared with the normal control, respectively. # p < 0.05 when compared with the trastuzumab-only group as negative control, respectively
Discussion
Radiotherapy treatment of trastuzumab-resistant HER2 overexpressing breast cancer cells has been reported previously. Using the existing high HER2 expression for targeting of HER2-binding radioactive agents is an attractive therapeutic approach [18, 26]. This study analyzed the sequential cellular and molecular events that initiate apoptosis in different HER2-expressing breast cancer cells incubated with 188Re-HYNIC-trastuzumab. The present results demonstrate that the cytotoxicity of 188Re-HYNIC-trastuzumab against breast cancer cells in vitro was specific in a radioactivity dose-dependent manner, and directly correlated with the expression level of HER2.
Trastuzumab represents an important development in the treatment of HER2-positive breast cancer cells [4, 12]. Blocking HER2 with trastuzumab led to an increase in chemotherapy-induced apoptosis in HER2 overexpressing cells [27]. Our results indicated trastuzumab induced cell death of overexpressing HER2 breast cancer cell lines through triggering apoptotic inductions in a short time, whereas the increase of cell death rate and apoptosis in MCF-7 cells (low HER2-expression) was slower. The mitochondrial membrane potential experiment further showed the mitochondria-dependent pathway is the crucial influence on trastuzumab-induced cytotoxicity. However, the HT-29 cells treated with trastuzumab for control showed no change either in cell death rate or apoptosis induction. Based on these data, we constructed the model for evaluating the efficacy of radiolabeled trastuzumab in the sequential experiments.
There have been several studies on the efficacy of radioimmunotherapy and trastuzumab in combination for cancer therapy [7, 28]. Zhang et al. [15] demonstrated that 213Bi-trastuzumab was cytotoxic to human breast cancer cell lines through apoptosis. In this study, we revealed that 188Re-HYNIC-trastuzumab led to cell death of breast cancer cells specifically in a HER2 level-dependent and radioactivity dose-dependent fashion. In BT-474 cells, 1 μg of trastuzumab labeled with 370 kBq 188Re radionuclide enhanced the cytotoxicity to nearly the level of 100 μg trastuzumab-alone treatment. In contrast, these effects did not appear in MCF-7 cells or HT-29 cells. The specificity and lasting cytotoxic effects of 188Re-HYNIC-trastuzumab were also revealed when compared with both types of breast cancer cells (BT-474 and MCF-7) treated with 188Re only. The data suggest that 188Re-HYNIC-trastuzumab has the potential for use as a therapeutic radiopharmaceutical in treatment of HER2-overexpressing breast cancer cells. A previous study showed that 188Re-labeled trastuzumab accumulated rapidly and specifically targeted BT-474 tumors [19]. Our results also demonstrated that 188Re-HYNIC-trastuzumab retained immunoreactivity toward HER2/neu over-expressing BT-474 human breast cancer cells (Fig. 1b). Trastuzumab is not only a very attractive targeting ligand on HER2-positive tumor itself, but also an effective anti-tumor drug in the treatment of breast cancer [29]. It is suggested 188Re-HYNIC-trastuzumab which was a β-emitting radiolabeled antibody and directs the radiation to tumors, thereby minimizing exposure of normal tissue, has the potential to be used as a therapeutic radiopharmaceutical for breast cancer treatment.
Irradiation has been shown to activate apoptosis pathways in leukemia and solid tumors [8, 21, 30]. Antibodies, when bound to key substances found on the cell surface, also can induce cells to undergo apoptosis [28]. The activation of a delayed type of apoptosis might be an important mechanism involved in cell death following the RIT of solid tumors with 131I radionuclides [31]. In this study, fluorescence staining for mitochondrial membrane potential changes revealed that the mitochondria-dependent pathway plays an important role in irradiation-induced apoptosis since the mitochondrial potential of all cells had been depolarized at 24 h. But the depolarization was only sustained specifically in HER2-expressing breast cancer cells after 48 h of 188Re-HYNIC-trastuzumab treatment. The effects of apoptosis by mitochondria-dependent pathway in BT-474 cells appeared rapidly at 24-h treatment, and accelerated most cells into DNA fragmentation. Our results were in line with those of previous studies indicating the critical role of the mitochondrial pathway in β-irradiation-induced apoptosis [21, 32]. The basic apoptosis levels were determined, respectively, by the early-monitor Annexin V technique and TUNEL staining monitors in the later stage of apoptosis for reflecting the different phases in the apoptotic process. Our data showed that after 188Re-HYNIC-trastuzumab treatment, typical apoptotic changes were induced in BT-474 cells after 48 h in a radioactivity dose-dependent manner. The study by Mirzaie-Joniani et al. [33] revealed that cells in the very late stage of apoptosis disintegrate and are no longer technically counted in the flow cytometry data. This may be the reason why the higher frequency of apoptotic cells only appeared after 48 h of treatment which may cause a larger initial induction of apoptosis. In a similar vein, Eriksson and his colleagues [31, 34] indicated that RIT with β-emitting radionuclides seems to generate a slower but longer lasting effect for a delayed type of apoptosis.
In conclusion, this study demonstrates the efficacy of 188Re-HYNIC-trastuzumab in inducing significant cell death in a radioactivity dose-dependent fashion. 188Re-labeled HYNIC-trastuzumab not only enhances, but may also prolong the effects of apoptosis induced by trastuzumab in HER2-overexpressing breast cancer cells. The mitochondria-dependent pathway is apparently involved in the processes of apoptosis. However, more in-depth investigations into the efficacy of 188Re-HYNIC-trastuzumab in radioimmunotherapeutic treatment of metastatic breast cancer are needed, especially in cases resistant to trastuzumab.
References
International Agency for research on cancer WHO. “World Cancer Report” (2003).
Anderson BO, Distelhorst SR. Guidelines for international breast health and cancer control-implementation. Introduction. Cancer. 2008;113(8 Suppl):2215–6.
Anderson BO, Jakesz R. Breast cancer issues in developing countries: an overview of the Breast Health Global Initiative. World J Surg. 2008;32(12):2578–85.
Menard S, Tagliabue E, Campiglio M, Pupa SM. Role of HER2 gene overexpression in breast carcinoma. J Cell Physiol. 2000;182(2):150–62.
Slamon DJ, Clark GM, Wong SG, Levin WJ, Ullrich A, McGuire WL. Human breast cancer: correlation of relapse and survival with amplification of the HER-2/neu oncogene. Science. 1987;235(4785):177–82.
Pauletti G, Dandekar S, Rong H, Ramos L, Peng H, Seshadri R, Slamon DJ. Assessment of methods for tissue-based detection of the HER-2/neu alteration in human breast cancer: a direct comparison of fluorescence in situ hybridization and immunohistochemistry. J Clin Oncol. 2000;18(21):3651–64.
Song YJ, Qu CF, Rizvi SM, Li Y, Robertson G, Raja C, Morgenstern A, Apostolidis C, Perkins AC, Allen BJ. Cytotoxicity of PAI2, C595 and Herceptin vectors labeled with the alpha-emitting radioisotope Bismuth-213 for ovarian cancer cell monolayers and clusters. Cancer Lett. 2006;234(2):176–83.
Liang K, Lu Y, Jin W, Ang KK, Milas L, Fan Z. Sensitization of breast cancer cells to radiation by trastuzumab. Mol Cancer Ther. 2003;2(11):1113–20.
Hudis CA. Trastuzumab—mechanism of action and use in clinical practice. N Engl J Med. 2007;357(1):39–51.
Santin AD, Bellone S, Roman JJ, McKenney JK, Pecorelli S. Trastuzumab treatment in patients with advanced or recurrent endometrial carcinoma overexpressing HER2/neu. Int J Gynaecol Obstet. 2008;102(2):128–31.
Fulda S. Tumor resistance to apoptosis. Int J Cancer. 2009;124(3):511–5.
Milella M, Trisciuoglio D, Bruno T, Ciuffreda L, Mottolese M, Cianciulli A, et al. Trastuzumab down-regulates Bcl-2 expression and potentiates apoptosis induction by Bcl-2/Bcl-XL bispecific antisense oligonucleotides in HER-2 gene-amplified breast cancer cells. Clin Cancer Res. 2004;10(22):7747–56.
Boerman OC, Koppe MJ, Postema EJ, Corstens FH, Oyen WJ. Radionuclide therapy of cancer with radiolabeled antibodies. Anticancer Agents Med Chem. 2007;7(3):335–43.
Li G, Wang Y, Huang K, Zhang H, Peng W, Zhang C. The experimental study on the radioimmunotherapy of the nasopharyngeal carcinoma overexpressing HER2/neu in nude mice model with intratumoral injection of 188Re-herceptin. Nucl Med Biol. 2005;32(1):59–65.
Zhang DY, Li Y, Rizvi SM, Qu C, Kearsley J, Allen BJ. Cytotoxicity of breast cancer cells overexpressing HER2/neu by 213Bi-Herceptin radioimmunoconjugate. Cancer Lett. 2005;218(2):181–90.
Li GP, Zhang YF, Wang YX. 188Re-labeled herceptin inhibits proliferation of breast cancer cell line SKBR-3 in vitro. Nan Fang Yi Ke Da Xue Xue Bao. 2006;26(10):1455–7.
Costantini DL, Bateman K, McLarty K, Vallis KA, Reilly RM. Trastuzumab-resistant breast cancer cells remain sensitive to the auger electron-emitting radiotherapeutic agent 111In-NLS-trastuzumab and are radiosensitized by methotrexate. J Nucl Med. 2008;49(9):1498–505.
Chen KT, Lee TW, Lo JM. In vivo examination of (188)Re(I)-tricarbonyl-labeled trastuzumab to target HER2-overexpressing breast cancer. Nucl Med Biol. 2009;36(4):355–61.
Luo TY, Tang IC, Wu YL, Hsu KL, Liu SW, Kung HC, et al. Evaluating the potential of 188Re-SOCTA-trastuzumab as a new radioimmunoagent for breast cancer treatment. Nucl Med Biol. 2009;36(1):81–8.
Li L, Story M, Legerski RJ. Cellular responses to ionizing radiation damage. Int J Radiat Oncol Biol Phys. 2001;49(4):1157–62.
Friesen C, Lubatschofski A, Kotzerke J, Buchmann I, Reske SN, Debatin KM. Beta-irradiation used for systemic radioimmunotherapy induces apoptosis and activates apoptosis pathways in leukaemia cells. Eur J Nucl Med Mol Imaging. 2003;30(9):1251–61.
Blankenberg FG. Imaging the molecular signatures of apoptosis and injury with radiolabeled annexin V. Proc Am Thorac Soc. 2009;6(5):469–76.
Tang Y, Scollard D, Chen P, Wang J, Holloway C, Reilly RM. Imaging of HER2/neu expression in BT-474 human breast cancer xenografts in athymic mice using [(99m)Tc]-HYNIC-trastuzumab (Herceptin) Fab fragments. Nucl Med Commun. 2005;26(5):427–32.
Abrams MJ, Juweid M, tenKate CI, Schwartz DA, Hauser MM, Gaul FE, et al. Technetium-99m-human polyclonal IgG radiolabeled via the hydrazino nicotinamide derivative for imaging focal sites of infection in rats. J Nucl Med. 1990;31(12):2022–8.
Lindmo T, Boven E, Cuttitta F, Fedorko J, Bunn PA Jr. Determination of the immunoreactive fraction of radiolabeled monoclonal antibodies by linear extrapolation to binding at infinite antigen excess. J Immunol Methods. 1984;72(1):77–89.
Carlsson J, Nordgren H, Sjostrom J, Wester K, Villman K, Bengtsson NO, et al. HER2 expression in breast cancer primary tumours and corresponding metastases. Original data and literature review. Br J Cancer. 2004;90(12):2344–8.
Simeone AM, Broemeling LD, Rosenblum J, Tari AM. HER2/neu reduces the apoptotic effects of N-(4-hydroxyphenyl)retinamide (4-HPR) in breast cancer cells by decreasing nitric oxide production. Oncogene. 2003;22(43):6739–47.
Sharkey RM, Goldenberg DM. Targeted therapy of cancer: new prospects for antibodies and immunoconjugates. CA Cancer J Clin. 2006;56(4):226–43.
Tan AR, Swain SM. Ongoing adjuvant trials with trastuzumab in breast cancer. Semin Oncol. 2003;30(5 Suppl 16):54–64.
Friesen C, Glatting G, Koop B, Schwarz K, Morgenstern A, Apostolidis C, et al. Breaking chemoresistance and radioresistance with [213Bi]anti-CD45 antibodies in leukemia cells. Cancer Res. 2007;67(5):1950–8.
Eriksson D, Blomberg J, Lindgren T, Lofroth PO, Johansson L, Riklund K, et al. Iodine-131 induces mitotic catastrophes and activates apoptotic pathways in HeLa Hep2 cells. Cancer Biother Radiopharm. 2008;23(5):541–9.
Friesen C, Lubatschofski A, Glatting G, Debatin KM, Reske SN. Activation of intrinsic apoptotic pathway by Re-188 irradiation and paclitaxel in coronary artery smooth muscle cells. Q J Nucl Med Mol Imaging. 2008;52(3):289–95.
Mirzaie-Joniani H, Eriksson D, Sheikholvaezin A, Johansson A, Lofroth PO, Johansson L, Stigbrand T. Apoptosis induced by low-dose and low-dose-rate radiation. Cancer. 2002;94(4 Suppl):1210–4.
Eriksson D, Joniani HM, Sheikholvaezin A, Lofroth PO, Johansson L, Riklund Ahlstrom K, et al. Combined low dose radio- and radioimmunotherapy of experimental HeLa Hep 2 tumours. Eur J Nucl Med Mol Imaging. 2003;30(6):895–906.
Author information
Authors and Affiliations
Corresponding authors
Rights and permissions
About this article
Cite this article
Luo, TY., Cheng, PC., Chiang, PF. et al. 188Re-HYNIC-trastuzumab enhances the effect of apoptosis induced by trastuzumab in HER2-overexpressing breast cancer cells. Ann Nucl Med 29, 52–62 (2015). https://doi.org/10.1007/s12149-014-0908-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12149-014-0908-8