Abstract
Research on the etiopathogenesis of Parkinson’s disease (PD) has in the very recent years earned many insightful cues about the involvement of xenobiotics and metal pollutants in the onset and exacerbation of this neurodegenerative disorder. Furthermore, particularly for metal pollutants, the hypothesis about the role exerted by impaired mitochondrial function is gaining a leading causative role. In this review, we outline the role of environmental pollution in the pathogenesis of PD, as the prolonged exposure to xenobiotics may account for the majority of PD reported cases, expanding the debate also about some suggested therapeutic approaches.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is a chronic, progressive neurological disorder due to the degeneration of dopamine-producing cells located in a region of the mesencephalon known as substantia nigra (SN), which is an integral element of the basal ganglia [1,2,3]. Dopamine synthesized in these cells takes care of essential functions as a neurotransmitter. Its precursor l-DOPA originates from the l-amino acid tyrosine (Y) via the activity of the tyrosine hydrolase (EC 1.14.16.2), which employs bivalent iron (Fe) and molecular oxygen as enzymatic cofactors. After release, specialized proteins transport dopamine extracellularly, i.e., the dopamine active transporter (DaT), to the synaptic receptors on neurons located, e.g., in the nucleus accumbens, hippocampus, striatum, spinal cord, and to the neocortex [4]. Dopamine deficiency and age-related reduction cause functional changes in the many structures of the brain controlling movement and lead to loss of muscle function [5, 6]. The condition may affect patients’ mobility and independence. The term parkinsonism refers to a group of several diseases that have common symptoms and may be associated with other neurological manifestations. Among these diseases, PD is the best known. The disease is named after the English surgeon James Parkinson (1755–1824), who in 1817 described it [7]. On April 11th, Parkinson’s birthday is celebrated as the yearly World Parkinson’s Day, which is part of the public campaigns to create awareness about PD.
PD symptoms expand slowly over time. Initially, the most apparent are rigidity, tremor, slow movements, and problems in walking, as well as general behavioral problems. Other symptoms include sleep disturbances, altered smell sense, constipation, and depression. In the more advanced stages of PD, cognitive problems are common [8]. The disease progression in subjects with PD, as well as the response to treatment, varies from patient to patient. The exact cause of the dopaminergic cells’ burnout is unknown, although both environmental and genetic factors may contribute [9]. The pathogenesis is accompanied by precipitation of Lewy bodies, i.e., abnormal protein aggregates inside neurons. Specific genetic mutations are involved in some cases of PD, although PD appears to be more commonly caused by environmental factors such as exposure to some pesticides, e.g., rotenone and paraquat [10].
As there are no specific tests to detect PD, the diagnosis is based on the patient’s medical history and clinical symptoms, as well as neurological and physical examinations. Tests such as neuroimaging techniques, spinal fluid analysis, and others may also be addressed to rule out if other conditions are causing the symptoms. Early diagnosis depends on the awareness of the medical doctor, and a supplementary DaT-scan (SPECT imaging using 99mTc-labeled dopamine transporter) may be helpful [11].
The l-dopa-producing enzyme complex tyrosine hydroxylase uses cofactors, such as molecular oxygen and Fe(II), as a vulnerable biochemical site with regard to reactive oxygen species (ROS)-dependent deterioration. Toxic metals/trace elements when present at non-physiological levels, such as manganese (Mn), copper (Cu), and Fe, can trigger the production of ROS, and presumably, even impair the physiological activity of mitochondria and also the activity of detoxifying and scavenger enzymes [12]. This biochemical impairment, alongside an accelerated or exacerbated ROS generation, and subsequently, also neuroinflammation, may be components leading to nigrostriatal cell exhaustion and death. However, the precise mechanisms of cellular death, characteristically starting in pars compacta of SN and subsequently distributed to other regions of the central nervous system (CNS) in PD, are yet not completely understood [9].
In 2015, it was estimated that PD affected about 6.2 million people worldwide. PD commonly appears in people aged 60 years or older, of whom about 1% is affected [13]. More males than females are affected by PD. The disease may also appear in people below the age of 50, and it is then named young-onset PD. In general, PD patients are not expected to live more than 15 years after the diagnosis. The present review summarizes case-control and epidemiologic evidence for environmental factors related to PD.
Basic Causes Involved in Parkinson’s Disease
Pathophysiologically, three findings appear to characterize the development of PD, viz. inhibition of mitochondrial complex I, oxidative stress, and abnormal protein aggregation. Although numerous studies have aimed at identifying genetic risk factors of PD, genetic background accounts only for about 10% of PD patients according to present knowledge, indicating that environmental factors play the most important role in the PD pathogenesis [14].
Abnormal Protein Aggregation in Parkinson’s Disease
One of the pathogenic steps leading to clinical PD is the abnormal accumulation of misfolded alpha-synuclein protein inside neurons, forming Lewy body aggregations [15]. Usually, alpha-synuclein seems to be a factor in maintaining a continuous synaptic vesicle supply, which contains the neurotransmitter dopamine in neuronal presynaptic terminals [16]. Alpha-synuclein in its physiological form is also found in neuronal mitochondria, where it may possess a regulating function on complex I [17]. However, in PD, pathological precipitates of alpha-synuclein, the Lewy bodies, appear in the SN, as well as in areas of the basal forebrain, midbrain, and in the neocortex. Lewy bodies do not necessarily lead to cell death if the abnormal protein is sequestered or removed by autophagy. In advanced cases of PD with dementia, Lewy bodies have frequently been found in the cortical areas [18,19,20].
Normally, aggregations of alpha-synuclein should be cleared by an adequately functioning activity of leucine-rich repeat kinase 2 (LRRK2) [21], which thereby delays the progression of PD. Gene mutations of LRRK2 are known as the most frequent cause of sporadic or familial PD. It accounts for about 5% of the patients with familial PD and about 3% of the sporadic cases. Mutations in the SNCA gene (the alpha-synuclein gene) are also a risk factor for non-familial PD since the gene encodes the protein alpha-synuclein. Moreover, mutations in other genes, including PRKN (the parkin gene), PINK1, GBA, and DJ-1, increase the risk for PD [22].
Mitochondrial Complex I and Parkinson’s Disease
Numerous studies reported that the etiology of PD might be attributed to mitochondrial impairment. From those factors, the NADH-ubiquinone oxidoreductase (complex I) of the respiratory chain appears to be the most responsible [23]. Electrons from reduced cofactors are transferred during oxidative phosphorylation by a series of respiratory chain complexes (complexes I–IV) that are located in the inner membrane of mitochondria [24]. Loss of the mitochondrial complex I catalytic function in the electron transport chain (ETC) is reported in multiple tissues from PD individuals [25, 26]. Reduced nicotinamide adenine dinucleotide (NADH)-driven electron transfer rates through complex I is positively related to a reduction in PD 8 kDa subunit and inversely related to complex I protein oxidation status. Reduced complex I function in PD brain mitochondria correlates with complex I misassembly, and it seems to occur because of subunit oxidation in the internal space, not because of external oxidative stress. The auto-oxidation of complex I may result from irregularities in complex I assembly factors, or complex I toxins, or some combination [25]. Numerous laboratories have found abnormalities of electron transport complexes, in particular in complex I in different tissues of PD patients. On the other hand, questions have been raised about the debilitation of the disease process due to the drug treatments which itself may induce reduced activities of ETC. Therefore, a blinded study of platelet mitochondrial ETC activities in 18 age- and sex-matched controls and 18 early untreated PD patients and in 13 spousal controls has been undertaken, revealing that lower activity of complex I in platelet mitochondria of PD patients was also seen in early untreated disease cases, and therefore cannot be explained from drug therapy or debilitation due to prolonged suffering [26]. The crucial role of complex I in the PD pathogenesis is supported by the action of MPP+ (N-methyl-phenylpyridinium ion), the active metabolite of MPTP, that is a specific inhibitor of the proton-pumping complex I in the mitochondrial respiratory chain [27, 28]. The complex I inhibition can induce declined ATP production and reactive oxygen species (ROS) generation [29]. Complex I is known as a main element of the respiratory chain, and its deficiencies can represent a fundamental instability of the mitochondria and their bioenergetic functions. And it is known that complex I deterioration forms a critical step in the cascade of the process leading to dopaminergic cell death. Decreased activity of complex I has been reported in mitochondria from the frontal cortex as well as platelets and SN of the brain of patients with PD.
Moreover, the activity of complex I was reported to be lower than average in the cybrid system consisting of the mitochondria from PD patients [23]. Biochemical, behavioral, and anatomical characteristics of PD in animal models have resulted from the administration of particular inhibitors of complex I [30, 31]. These and other outcomes propose that the impairments of complex I may be critical in the dopamine neuronal death and PD pathogenesis.
Oxidative Stress and Parkinson’s Disease
Oxidative stress has been presumed to represent a critical effect in dopaminergic neurotoxicity. Environmental factors, such as pesticides, dopamine itself, insecticides, and neurotoxins, in addition to genetic factors, appear to be involved in the mitochondrial dysfunction, which precedes the formation of reactive oxygen species (ROS) in PD. The abnormalities in the normal cellular processes that occur in relation to the aging process are thought to involve elevated susceptibility of dopamine neurons [32]. Selective DA degeneration of neurons in the SN pars compacta (SNpc) proposes that the levels of DA itself may be a source of oxidative stress [33]. Also, it is thought that oxidative stress is the common underlying process that induces the dysfunction of the cell as well as its death. Oxidative stress can occur because of an imbalance between cellular antioxidant activity and ROS production. Superoxide radicals and oxidants are produced as the oxidative phosphorylation products within the cell, particularly in the mitochondria as the main site of ROS production. ROS can affect mitochondrial DNA, which can induce changes in the synthesis of METC components such as the production of adenosine triphosphate (ATP) and the leakage of ROS into the cell’s cytoplasm [34]. The mechanisms regarding the generation of ROS associated with PD include neuroinflammation, DA dysmetabolism, and, mitochondrial dysfunction [32]. Oxidative stress appears to trigger a cascade of reactions that lead to the degeneration of dopamine cells in PD. This cascade is intimately connected to the components of the degenerative process, which include excitotoxicity, nitric oxide toxicity, inflammation, and mitochondrial dysfunction [35]. Jenner and his colleague reported that the degenerate section of neurons in the non-pigmented and pigmented nuclei in the SN of the brain in patients with PD might be particularly sensitive to oxidative stress [36].
Dopamine Function—the Vulnerable Target in the PD Pathogenesis: the Case of Mercury
Dopamine is produced from tyrosine and acts as a monoamine neurotransmitter. It is well known that the major function of dopamine is to regulate motivation and cognition as well as to assist in the modulation of brain activity and to distribute information into different regions of the cortical brain. However, molecular interactions of the dopamine circuitry with xenobiotics and pollutants may account for disturbances leading to the PD onset [37]. For example, Cu dyshomeostasis can induce dopaminergic degeneration, particularly if induced by intrastriatal administration [38]. Metals cause dramatic impairments in the redox signaling, causing neuroinflammation and neurodegeneration.
Moreover, monoamine oxidases (MAO), which catalyze the oxidation of dopamine to dihydrooxphenylacetyldehyde, can exacerbate the redox status [39]. Deficiency of antioxidant defense enzymes such as glutathione peroxidase may then lead to the formation of highly reactive and toxic hydroxyl radicals [40]. It is widely known that dopamine-related neurotoxicity is characterized by increased aggregation of α-synuclein, which is accumulated selectively in the SN in PD [41, 42]. It has been found in studies on the brain of ray-finned fishes that MAO activity is triggered by the mercury (Hg) exposure [43]. In this perspective, it is of interest that MAO inhibitors have been used therapeutically with some effect in PD [44]. In river otters, it has been demonstrated that brain Hg levels are inversely associated with the activity of MAO in the cerebral cortex [45]. In the presence of Hg, an abnormal uptake of dopamine by synaptosomes in rats has been reported. It has been found that dopamine D2 receptors are negatively correlated to Hg exposure in wild mink’s brain [46]. And reduced dopamine D2 receptor binding was demonstrated in the caudate–putamen region in methylmercury (MeHg)-exposed animals [47]. MeHg exposure during development affected both cortical and striatal dopamine D1 and D2-like receptor density [48]. Further reports have shown that MeHg exposure resulted in increased striatal dopamine levels [49].
Moreover, the observed effects on dopamine levels and functions were age-dependent [50]. These outcomes are in agreement with the results reporting a substantial elevation of extracellular dopamine levels in response to intrastriatal Hg salt injections [51, 52]. Chronic low-dose MeHg exposure induces a remarkable decrease in dopaminergic neuron differentiation from murine embryonic stem cells [53]. Using nematodes as a model of chronic Hg exposure, it was found that MeHg induces degeneration of dopamine neurons [54]. These studies reported similar findings as the previously reported data from animal experiments, which indicated MeHg-induced neuronal shrinkage and nucleic chromatin condensation in dopaminergic mesencephalic cells [55].
The role of Hg is only one of the hypothetic causative agents in the dopamine-related dysfunctions leading to PD [56, 57]. And the activity of mixed exposures to toxic metals is particularly complex, as it may not be described merely by a classical dose–response mechanism [58]. Therefore, further research is requested to elucidate the etiopathogenetic role of metal pollutants in PD.
Environmental Factors in Parkinson’s Disease
PD is considered to involve a multifactorial etiology, including a variety of environmental factors [59]. While about 5–10% of the patients have a type of PD that occurs due to gene mutation, these mutations do not necessarily lead to PD. Usually, the mutations represent susceptibility factors elevating the risk to develop PD, whereas other factors influence the severity and the age of onset [60]. Typically, the Fe accumulation reported in SN is related to inclusions of misfolded proteins. The Fe accumulation may be associated with oxidative damage, which is accompanied by neuroinflammation and misfolding [61]. One theory claims that exposure and accumulation of Fe, Cu, Mn [62], or Hg [63] may aggravate the oxidative damage and thus be involved in the pathogenesis of PD.
After reports on parkinsonism caused by the contaminant MPTP in illegal opioid drugs taken intravenously by abusers [64], much attention has been paid to the role of environmental pollutants in the PD pathogenesis. Pesticide exposure, e.g., to paraquat, rotenone, and maneb, have been associated with increased risk of PD development [65,66,67]. Paraquat is also a well-known catalyst for ROS formation. In vivo paraquat undergoes a redox cycling, which leads to ROS generation [68]. In rats, toxicity induced by paraquat has been associated with Parkinson-like neurodegenerative mechanisms [69]. Also, a study found a positive connection between combined exposure to Fe and paraquat in mid-life and infancy Parkinson’s mice in the laboratory [70].
Xenobiotics
General Aspects
A xenobiotic can be defined as exogenous chemicals or any foreign substance presented within an organism that the body does not recognize such as pollutants, drugs, and cosmetics, as well as some food additives. It is not naturally generated or expected to be found within the organism [71, 72]. These substances are rare or unknown in nature and usually found as synthetic chemicals [73]. Examples of such structural elements are rotenone, 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP), maneb, and paraquat. The PD etiology has been elucidating as a complex interaction of environmental and genetic agents.
Rotenone
Rotenone is a natural plant-derived pesticide that is regularly applied for the killing of fish in the pool and as an insecticide. Although it is known as an organic substance that commonly proposes to be human non-toxic, it has been reported to be a toxin for mitochondria that control the electron transport chain in complex I [74], inducing progressive oxidative damage and neurodegeneration of non-dopaminergic and dopaminergic neurons. The auto-oxidation of complex I may result from irregularities in complex I assembly factors, rotenone-like complex I toxins, nuclear or mitochondrial encoded subunits, or some combination [25]. The toxic effect of rotenone and the toxic metabolite of MPTP are attributed to their effect on complex I in the mitochondrial electron transport chain. Both these agents inhibit the electron transfer from NADH in the Fe–sulfur center of complex I to ubiquinone (coenzyme Q10). This transport block in the mitochondrial matrix leads to a back-up of electrons that will generate ROS and disrupt DNA, alpha-synuclein, and other integrates of the mitochondria [75, 76]. Rotenone also can damage mitochondria and give typical symptoms of PD [77]. The administration of rotenone by daily intraperitoneal injection (IP) in rat models created postural instability, rigidity responsive to dopamine, and bradykinesia. Postmortem studies of rats showed that nearly half of striatal neurons and the substantia nigra were lost. Furthermore, polyubiquitin-positive aggregates and alpha-synuclein were found in the enteric nervous system, and dopamine neurons in the substantia nigra, similar to the Lewy bodies reported in PD [78, 79]. Also, the aggregation and phosphorylation of amyloid and tau proteins can be induced by rotenone [80, 81]. In a study, during treatment with rotenone, it has been shown that the overexpressing of Mul1 and Park genes that are known to encode mitochondrial ligases protects neurons. Overexpressed mul1 or park in the Drosophila strains revealed a remarkably decreased degeneration of normal motor activity and dopaminergic neurons during exposure to rotenone. In addition, rotenone can affect synaptic proteins such as Disk Large1, Synaptotagmin, and Synapsin, as well as the structure of synaptic vesicles in the nervous system [77]. Furthermore, human epidemiological studies have shown that PD may develop commonly in people with regular application of rotenone [10, 82]. Moreover, the Farming and Movement Evaluation (FAME) study showed that rotenone was related to PD regardless of the use of protective gloves [83]. Therefore, with the controversially mixed laboratory outputs, many supportive laboratory results and supportive human epidemiologic studies propose that PD is likely correlated with rotenone [84, 85].
1-Methyl-4-phenyl-1,2,3,6-tetrahydropyridine
1-Methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) was the first-described agent that can induce an animal model of Parkinson’s syndrome and/or parkinsonism, although it is not a frequent environmental exposure. It has been reported that different biological properties such as mice strain may lead to insensitivity to the administration of MPTP, reproducibility of lesions in mice, and differing rates of mortality, although there is no documentation on its associated pathological lesions and the possible sensitivity of C57BL/6 mice from various origins to MPTP [86]. MPTP was correlated with the rapid onset of PD in a young victimizer of the drug presented in Northern California [87]. Studies on the mechanism of action of MPTP and its functions may significantly increase our knowledge on the effective role of the nigrostriatal system and dopamine and expand our understanding about the basic mechanisms of cells and about the role of the substantia nigra in health and PD. Among the different models of pharmacological PD, the model of MPTP-stimulated PD has been regularly applied because of no requirements for experimental technology, reproducible and reliable lesions in the nigrostriatal dopaminergic pathway, and similar clinical symptoms with PD patients [88]. MPTP can damage neurons through inhibiting complex I of the electron transport chain [89]. Non-human primates and studies of rodents have reported that MPTP induces depletion of striatal dopamine with selective eradication of dopaminergic neurons in the substantia nigra. Also, other areas of the brain, such as the locus ceruleus, and other non-dopaminergic regions, are significantly spared in MPTP-stimulated parkinsonism. Also, not progressive and stable symptoms, as well as no Lewy Body pathology, may be seen in postmortem analysis after MPTP exposure in developed parkinsonism individuals [64].
Furthermore, postmortem tissue evaluation has also reported ongoing, active inflammation with the presence of extracellular melanin, microglia, and neurodegeneration, after some years of MPTP exposure, suggesting to the concept of “long-latency neurotoxicity” after first exposure [64]. It has been hypothesized that ongoing inflammation and oxidative stress can lead to nigral cell loss and are proposed as the mechanism for the continued and progressive degeneration [90].
Maneb and Paraquat
The fungicide maneb and the herbicide paraquat are known as the oxidative stressor that was correlated with PD [10, 65, 91, 92]. The chemical structure of paraquat is closely similar to the active metabolite of MPTP. Maneb and paraquat also likely have synergistic effects [93]. Paraquat induces tissue damage through the subsets of the redox cycle that produces toxic superoxide free radicals. In Drosophila flies, a mimetic enzyme of superoxide dismutase has been reported to decrease the mitochondrial damage induced by paraquat [94].
Moreover, in vivo animal investigations reported that paraquat induced the glutamate efflux initiating excitotoxicity regulated by reactive nitrogen species [95]. Other studies also have reported that paraquat stimulates the upregulation of alpha-synuclein [96], microglial activation, and aggregate formation [97, 98]. Dopaminergic neuronal cell death in the basal ganglia also can be induced by systemic subchronic exposure to paraquat in mice, although the levels of dopamine remained unchanged [99]. Furthermore, elevated doses of chronic paraquat exposure did induce delayed decrease of dopaminergic neurotransmission and slow progressive degeneration of nigrostriatal neurons, indicating that paraquat may induce “subclinical” results and additional genetic or environmental agents may be demanded if PD develops. Also, an epidemiologic study revealed a significant decrease in the glutathione transferase gene that induces cellular protection against oxidative stress was associated with an elevated risk of PD when male subjects were exposed to paraquat [100]. Also, dopamine transporter susceptibility alleles may be seen in exposure to paraquat and maneb and led to a higher PD risk [101]. The results of a study also showed that NADPH oxidase is involved in maneb- and paraquat-stimulated dopaminergic neurodegeneration by ferroptosis, suggesting a new potential mechanism for pesticide-stimulated dopaminergic neurotoxicity [102].
Furthermore, the rapid influx of extracellular zinc (Zn2+) into dopaminergic neurons by transient receptor potential melastatin 2 (TRPM2) cation channel activation induced by paraquat can accelerate the degeneration of nigrostriatal dopaminergic in aged rats. It is possible that vulnerability to paraquat-induced pathogenesis in the aged substantia nigra pars compacta is due to accelerated dysregulation of intracellular Zn2+ [103]. This area needs more human studies since our knowledge was restricted by exposure to multiple pesticides in addition to paraquat and small sample size.
β-Methylamino-l-alanine
β-Methylamino-l-alanine (BMAA) is an excitotoxin that allegedly globally contributed to neurodegenerative diseases such as the Parkinson–dementia complex (PDC), a neurological disorder with motor neuron disease symptoms [104]. Numerous in vitro studies performed on leeches, rats, mice, and human cells have reported the detrimental effects of BMAA on neurons [88]. It has been reported that the most commonly involved mechanism for the action of BMAA is the process of cell death-inducing because of excitatory amino acid (EAA) receptor activation (particularly glutamate receptors). BMAA is correlated with the three potential approaches of degeneration in PD, including excitotoxicity, mitochondrial dysfunction, and non-cell autonomous death [105]. Also, BMAA exposure induces CNS cell death in the mice through the examining glial response and neuronal numbers in the brain and the spinal cord. No motor, neuropathological, or cognitive outcome resulted from this feeding pattern, indicating a lack of neuropathological and behavioral effects of dietary BMAA in mice [104].
Furthermore, another investigation reported that BMAA might be involved in human neurodegenerative diseases [106]. Following numerous exposure, BMAA can accumulate in the brain. However, in the male rats, BMAA was slowly eradicated from other tissues and blood (half-lives ≥ 48 h). On the other hand, there is no higher affinity for accumulation in the brain compared with the other tissues and organs [106]. Numerous studies on BMAA effects showed conflicting effects, although some in vitro data are revealing a neurotoxic effect, and experimental animal evidence failing to replicate the neurodegeneration pattern of these human Parkinson–dementia complex (PDC), even at very high exposures.
Metals and Parkinson’s Disease
General Aspects
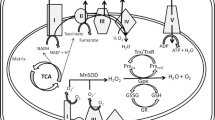
The role of dopamine in PD is well established. However, its wide activity in many regions of the midbrain makes the toxic role of xenobiotics as promoting ROS exacerbation of the utmost role not only in PD but in many degenerative neurological diseases (Fig. 1). The effective function of metals in the pathogenesis of PD is known as a great concern in medical chemistry and neurotoxicology [56, 107]. This role is known either by a decrease in essential metals or by metallic toxicants for human health. For example, numerous epidemiological researches also have reported a positive relevance between long-term exposure and PD to metals such as Mn, Hg, Cu, lead (Pb), Zn, Fe, bismuth (Bi), aluminum (Al), and titanium (Ti) after chronic exposure to multiple metals [108,109,110]. The important sources of exposure comprised occupational exposure, contaminated seafood, environmental pollution, dental metal restorations such as amalgam fillings, and medications [56]. Occupational exposures to Al, Mn, and Fe have been reported to double the risk of occurrence of PD [109, 111]. Synergistic effects also were reported between PD and metals with combined exposures of Pb–Cu, Pb–Fe, and Fe–Cu in comparison with the effects of single metals [112, 113]. Also, metals stimulate the α-synuclein aggregation that is a highly abundant, small, and conserved presynaptic protein with neurodegenerative function in the PD etiology [114, 115]. Finally, it has been demonstrated that Hg and other metals may be involved in PD development.
The possible major pathways involved in the dopamine-related actions causing neurodegeneration. Considering that the impaired signaling of reactive oxygen species (ROS) provoked by metal pollutants and xenobiotics induces a dopamine activity disorder, this may involve thalamic response to dopamine, with the onset of psychotic and cognitive impairments, and the hypothalamus, with circadian regulation. Toxic metals can also modulate or exacerbate the relationship dopamine/prolactin, while melatonin can modulate the impairment of dopamine in circadian and seasonal rhythms acting on the dopamine circuitry in the hippocampus. Many of these activities are included in several signs of neurodegenerative and aging-related neurological disorders. This should give suggestions about the widest role of the dopamine signaling in neurodegenerative diseases
Manganese
Several studies of rapid-onset parkinsonism have reported that exposure to Mn of young intravenous drug users through ephedrone (methcathinone) abuse can be the critical factor of PD [116,117,118]. Manganese also is known as a basal ganglia toxin related to PD, although there are controversial results about its relevance with idiopathic PD [119, 120]. The neurotoxicity mechanism of Mn is the globus pallidum degeneration regulated through the disruption of the apoptosis and cell death mitochondria by the formation of elevated ROS [121]. Manganese can inhibit glutamate transport, inducing the elevation contents of glutamate and therefore induce cytotoxicity [122]. Also, Mn is rapidly absorbed by the mitochondria and stimulates the accumulation of calcium and controls oxidative phosphorylation, leading to ATP depletion [123]. The exposure to a low concentration of Mn was related to elevation of contents of astrocytosis in the motor and striatum as well as specific motor symptoms similar to PD, indicating Mn is a great neurotoxicant. The toxicity of Mn is reported in the central nervous system, particularly in the nigrostriatal neuronal circuitry, and consequences include motor and behavioral impairments [124]. Also, there is a rare understanding about neurobehavioral mechanisms among patients with idiopathic PD and patients with manganism, although there is a study with 13 patients with PD, 34 patients with manganism, and 43 healthy workers as the reference group. In this study, it was revealed that PD patients had greater postural tremor intensity with narrower frequency dispersion compared with the patients with manganism. However, the asymmetrical neurobehavioral performance was reported commonly in PD patients compared to manganism patients, particularly science testing for static steadiness, tremor intensity, and grooved pegboard suggesting lateralized impairment in the PD patients [125]. Therefore, it has been reported that Mn can be described as a neurotoxic substance because of neuroinflammation mitochondrial dysfunction and oxidative stress, and protein trafficking and misfolding [125]. Furthermore, despite the distinction between idiopathic PD and Mn neurotoxicity, there are some supportive studies that highlight the exposure with Mn can be a risk factor for PD [113].
Mercury
Remarkably elevated blood levels of Hg were reported in patients with PD regarding controls, and it has been demonstrated that Hg exposure was correlated with an eightfold increase in the PD risk [126]. However, particular neurodegenerative effects and neuronal modifications that have been seen in PD are only detectable with the Hg exposure at the lowest contents. Particularly, nigral dopaminergic neurons are very sensitive to Hg because of elevated glutamate toxicity and their high content of tubulin [56]. PD onset has been associated with exposure to elevated levels of Hg [58]. Numerous similarities between the effects of Hg ingestion/exposure and the consequences/symptoms of patients with PD have been reported, although Hg has not only been related to the PD incidence [56]. It has been reported that in patients with PD, the detectable blood Hg contents were six times more frequent compared with healthy individuals [127]. The sources of Hg exposure comprised long-lived fish consumption (such as tuna), dental amalgam, occupational exposures, and medications. A significant dose–response relevance was found between PD patients and blood Hg levels [128]. It has been found that intoxication with Hg can induce parkinsonism in a 47-year-old dentist, and consequences chelation treatment, induced health [129]. Methylmercury can cross through placental barriers and the blood–brain barrier, inducing neuronal damage in the central nervous system. Also, Hg vapor, being highly lipid-soluble and volatile, can pass through the lipid cell membranes and the blood–brain barrier and can be stored into the cells in its inorganic forms [130]. In vitro studies reported that exposure with Hg was importantly contributed in apoptotic processes and oxidative stress. Furthermore, neural loss and cognitive and motor impairment have been showed in different studies carried out in animal models [41, 130, 131]. Finally, observational investigations on PD patients with neurodegenerative diseases reported conflicting data on the possible involvement of Hg [132, 133].
Iron
Iron has been reported to be possibly connected with the PD pathophysiology in numerous laboratory investigations, although the documented data of human exposure is rare [134, 135]. Some studies have reported that increased dietary Fe is associated with PD [97, 98], while there are conflicting data on serum Fe levels and their relevance with PD [136, 137]. A deficiency of Fe can impair the function of the central or peripheral nervous system, which may induce restless legs syndrome with PD [138]. Also, in a case–control study with idiopathic PD and controls, the effective role of occupational exposure to Fe, Mn, Cu, Zn, Pb, and Hg as potential risk factors for PD has been investigated. The result of this study reported that chronic exposure to each or a combination of these metals is related to PD [113]. Substantia nigra neurons have some neuromelanin that can link with the Fe and generate free radicals that affect cell death and lipid peroxidation [139]. Iron also can induce dopamine oxidation in substantia nigra neurons, which led to the release of further free radicals [140]. Higher concentrations of Fe in the substantia nigra of patients with PD also have been reported in pathological studies [141]. Also, animal experiments have reported that in MPTP-stimulated parkinsonism, Fe chelation has shown therapeutic effects [142]. A total of 135 patients with PD were divided according to the ratio of mean tremor score to the mean bradykinesia/rigid score of the Unified Parkinson’s Disease Rating Scale (UPDRS) III and showed the interaction between relevant inflammation and disturbed metabolism of Fe might regulate clinical phenotypes of PD [143]. Abnormal accumulation of Fe is correlated to a host of neurodegenerative diseases, such as PD through a malfunction of Fe homeostasis or the abnormal deposition in specific brain regions [144]. Most of the investigations with PD patients focus on the Fe overload of the brain in regions, including the putamen, globus pallidus, and substantia nigra neurons [145, 146]. A study also has confirmed that the Fe depositions in the red nucleus dentate and the nucleus of the cerebellum are associated with tremor in patients with PD [147]. However, more studies need to be done on the relevance of Fe and its metabolism-related proteins in both the peripheral and central systems, and different motor PD phenotypes. Finally, whether the accumulation of Fe can stimulate the substantia nigra neuron injury or occurs as a subsequence of neuronal degeneration needs clarification.
Metal Chelators and Neurotoxicity
Chelators bind to some substances such as metals in different degrees. The mechanism of chelators is composed of the construction of chelator–metal complexes (chelates) that are secreted in urine [148]. A chelating antidote may be used orally or intravenously in cases of metal toxicity. Depending on the chemical affinity for the toxic metal, some compounds such as 2,3-dimercaptopropane-1-sulfonic acid (DMPS, Dimaval, Unithiol), ethylenediaminetetraacetic acid (EDTA), or meso-2,3-dimercaptosuccinic acid (DMSA, Succimer) are given as intermittent courses or continuously for several days. Some studies proposed that oral DMSA is the safest and efficient chelation treatment regimen directly available in moderately Pb-poisoned cases. Human and animal data suggest that DMSA should be evaluated as the approved antidote to move Pb from soft tissues [149]. Also, DMPS treatment can increase the urinary excretion of Zn and Cu [150, 151], in which case deficiency symptoms may be reported in some patients. Also, it has been identified that the combination of DMSA and Monensin, a polyether antibiotic, is even more effective in Pb mobilization from the kidneys and brain in comparison with their being used alone. The proposed pathways for this is that Monensin can act as a Pb shuttle in exchange for external sodium [152]. Numerous studies have reported the concerns of the Pb–EDTA complex that might be redistributed in the brain. Therefore, they suggest that DMSA is safer than CaEDTA because of extracellular scavenging of Pb [153]. It has been reported that EDTA can induce greater losses of essential minerals such as Fe, Zn, Mg, and Ca in comparison with DMPS and DMSA [154]. Other reported side effects of EDTA chelation include lacrimation, mucocutaneous lesions, glucosuria, nasal congestion, and hypotension [148]. Therefore, a promising chelating agent can generate less toxic metal complexes and reach the body’s metal storage sites. Also, a good chelator should have a high affinity for the toxic metals at the pH of the body fluids, be easily soluble in water, and be resistant to biotransformation [155, 156].
Deferiprone, other iron chelators, and PD
In the PD brain, a feature is the crucial accumulation of Fe in degenerative regions [157]. Although Fe levels in the PD brain may be moderately increased in several regions, in early PD is neuronal loss limited to SN [158] where a pronounced Fe deposition is reported in PD brains [159]. An interaction between an extra-vesicular fraction of dopamine and electrophilic Fe ions is thought to have an important role in SN progressive degeneration, which initially creates an unstable complex that increases the neurotoxic products particularly in sensitive regions of the brain [160]. One theory involves the production of dopamine-quinones (DA-quinones), o-quinones, and 6-hydroxydopamine (6-OHDA) [161]. The latter is in animal PD models, a frequently used neurotoxin [160]. In the cell, DA-quinones interact with the protein thiols and sulfhydryl groups of glutathione (GSH) to produce changed proteins [162] that induce cellular toxicity [163]. It has been suggested that 6-OHDA formation initiates a cascade of mechanisms that increase the labile e pool in the cell, therefore great protective antioxidant pathways [160].
Devos et al. (2014) studied the effect of Fe chelation with deferiprone in both mice and minor clinical trials of patients with early-stage PD [164]. In mice, dopaminergic dysfunction after chelation treatment was shown to be reduced due to subsequent administration of MPTP. MRI was used to quantify the deposition of nigral Fe, and the improvements of the patients after deferiprone treatment were assessed using the Unified Parkinson’s Disease Rating Scale. It has not yet evidently been reported in PD that chelation therapy of Fe restores the dopaminergic system integrity. However, these data support the hypothesis that deferiprone may modify the PD progression. It is possible that chelation of Fe can be even more useful if initiated in a subclinical or early stage of PD. Experimental studies by the same or other research group support the observations of a therapeutic effect of Fe chelation with deferiprone or deferasirox in PD [165]. It has been reported that after 6 months of chelator deferiprone therapy, it can be effective through the improvement of gait and reduction in dyskinesias in neurodegeneration associated with brain Fe overload [166]. It can cross the blood–brain barrier in effective concentrations and lead to progress in the phase II trial for deferiprone to evaluate its efficacy and safety as an Fe chelator for excess contents of Fe in the PD treatment [167]. In a pilot, double-blind, placebo-controlled randomized clinical trial study, deferiprone remarkably decreased biological damage and labile Fe in oxidation-stressed animals and cells at 30 mg/kg/day through the improvement of motor functions in increased striatal dopamine [164].
Concluding Remarks
The present paper has highlighted the role of environmental factors in the pathogenesis of PD since lifestyle factors, exposures to metals, pesticides, and drugs, seem at least to account for 90% of the cases. Preventive measures in PD have to take into consideration that primary causes in the development of the disease are abnormal protein aggregation and inhibition of mitochondrial complex I, and in particular pathological oxidative stress in the nigrostriatal neurons. Since excesses of Fe that have been identified in SN regions can speed up the oxidative stress, mobilization of this element from the vulnerable areas is anticipated to slow down the progression. Such mobilization can be obtained by chelating agents (deferiprone or deferasirox).
Early clinical signs of PD are reduced ability to move with slow movements, and the steps of these patients may become shorter when walking. Muscle stiffness may occur in any part of the body, often distally in extremities. Some tremor may occur already in the early stages. Similar symptoms are also described in another neurological disease, the so-called Skogholt disease, characterized by neuroinflammation and concomitant notable increases in levels of Fe and Cu in CSF. And it has been suggested that the latter disease is also caused by combined toxicity of Fe and Cu accompanied by oxidative stress, i.e., in regions in basal ganglia.
References
Poewe W, Seppi K, Tanner CM, Halliday GM, Brundin P, Volkmann J, Schrag A-E, Lang AE (2017) Parkinson disease. Nature reviews Disease primers 3:17013
Mou L, Ding W, Fernandez-Funez P (2019) Open questions on the nature of Parkinson’s disease: from triggers to spreading pathology. J Med Genet
Wong YC, Luk K, Purtell K, Burke Nanni S, Stoessl AJ, Trudeau LE, Yue Z, Krainc D, Oertel W, Obeso JA (2019) Neuronal vulnerability in Parkinson disease: should the focus be on axons and synaptic terminals? Mov Disord
Masato A, Plotegher N, Boassa D, Bubacco L (2019) Impaired dopamine metabolism in Parkinson’s disease pathogenesis. Mol Neurodegener 14(1):1–21
Guenther M, Bartsch RP, Shahar YM, Hassin-Baer S, Inzelberg R, Kurths J, Plotnik MP, Kantelhardt JW (2019) Coupling between leg muscle activation and EEG during normal walking, intentional stops, and freezing of gait. Front Physiol 10:870
Lee H, Chang M (2017) Degeneration of the corticofugal tract from the secondary motor area in a Parkinson’s disease patient with limb-kinetic apraxia: a case report. Medicine 96(50)
Parkinson J (1817) An essay on the shaking palsy. (Printed by Whittingham and Rowland for Sherwood, Neely, and Jones). London,
Sveinbjornsdottir S (2016) The clinical symptoms of Parkinson’s disease. J Neurochem 139:318–324
Kalia LV, Lang AE (2016) Parkinson disease in 2015: evolving basic, pathological and clinical concepts in PD. Nat Rev Neurol 12(2):65–66
Tanner CM, Kamel F, Ross GW, Hoppin JA, Goldman SM, Korell M, Marras C, Bhudhikanok GS et al (2011) Rotenone, paraquat, and Parkinson’s disease. Environ Health Perspect 119(6):866
Sasannezhad P, Juibary AG, Sadri K, Sadeghi R, Sabour M, Kakhki VRD, Alizadeh H (2017) 99mTc-TRODAT-1 SPECT imaging in early and late onset Parkinson’s disease. Asia Oceania J Nucl Med Biol 5(2):114
Lan A, Chen J, Chai Z, Hu Y (2016) The neurotoxicity of iron, copper and cobalt in Parkinson’s disease through ROS-mediated mechanisms. Biometals 29(4):665–678
Lee A, Gilbert RM (2016) Epidemiology of Parkinson disease. Neurol Clin 34(4):955–965
Dauer W, Przedborski S (2003) Parkinson’s disease: mechanisms and models. Neuron 39(6):889–909
Spillantini MG, Schmidt ML, Lee VM-Y, Trojanowski JQ, Jakes R, Goedert M (1997) α-Synuclein in Lewy bodies. Nature 388(6645):839
George JM, Jin H, Woods WS, Clayton DF (1995) Characterization of a novel protein regulated during the critical period for song learning in the zebra finch. Neuron 15(2):361–372
Liu G, Zhang C, Yin J, Li X, Cheng F, Li Y, Yang H, Uéda K et al (2009) α-Synuclein is differentially expressed in mitochondria from different rat brain regions and dose-dependently down-regulates complex I activity. Neurosci Lett 454(3):187–192
Beyer K (2007) Mechanistic aspects of Parkinson’s disease: α-synuclein and the biomembrane. Cell Biochem Biophys 47(2):285–299
Galvagnion C (2017) The role of lipids interacting with α-synuclein in the pathogenesis of Parkinson’s disease. J Park Dis 7(3):433–450
Schulz-Schaeffer WJ (2010) The synaptic pathology of α-synuclein aggregation in dementia with Lewy bodies, Parkinson’s disease and Parkinson’s disease dementia. Acta Neuropathol 120(2):131–143
Volpicelli-Daley LA, Abdelmotilib H, Liu Z, Stoyka L, Daher JPL, Milnerwood AJ, Unni VK, Hirst WD et al (2016) G2019S-LRRK2 expression augments α-synuclein sequestration into inclusions in neurons. J Neurosci 36(28):7415–7427
Kalinderi K, Bostantjopoulou S, Fidani L (2016) The genetic background of Parkinson’s disease: current progress and future prospects. Acta Neurol Scand 134(5):314–326
Marella M, Seo BB, Yagi T, Matsuno-Yagi A (2009) Parkinson’s disease and mitochondrial complex I: a perspective on the Ndi1 therapy. J Bioenerg Biomembr 41(6):493–497
Jin H, Kanthasamy A, Ghosh A, Anantharam V, Kalyanaraman B, Kanthasamy AG (2014) Mitochondria-targeted antioxidants for treatment of Parkinson’s disease: preclinical and clinical outcomes. Biochim Biophys Acta 1842(8):1282–1294
Keeney PM, Xie J, Capaldi RA, Bennett JP (2006) Parkinson’s disease brain mitochondrial complex I has oxidatively damaged subunits and is functionally impaired and misassembled. J Neurosci 26(19):5256–5264
Haas RH, Nasirian F, Nakano K, Ward D, Pay M, Hill R, Shults CW (1995) Low platelet mitochondrial complex I and complex II/III activity in early untreated Parkinson’s disease. Ann Neurol 37(6):714–722
Khan SZ (2006) Mitochondrial complex-1 in Parkinson’s disease. Neurol India 54:351
Schapira A, Cooper J, Dexter D, Clark J, Jenner P, Marsden C (1990) Mitochondrial complex I deficiency in Parkinson’s disease. J Neurochem 54(3):823–827
Ramsay RR, Salach JI, Dadgar J, Singer TP (1986) Inhibition of mitochondrial NADH dehydrogenase by pyridine derivatives and its possible relation to experimental and idiopathic parkinsonism. Biochem Biophys Res Commun 135(1):269–275
Betarbet R, Sherer TB, MacKenzie G, Garcia-Osuna M, Panov AV, Greenamyre JT (2000) Chronic systemic pesticide exposure reproduces features of Parkinson’s disease. Nat Neurosci 3(12):1301
Thiruchelvam M, Richfield EK, Baggs RB, Tank AW, Cory-Slechta DA (2000) The nigrostriatal dopaminergic system as a preferential target of repeated exposures to combined paraquat and maneb: implications for Parkinson’s disease. J Neurosci 20(24):9207–9214
Blesa J, Trigo-Damas I, Quiroga-Varela A, Jackson-Lewis VR (2015) Oxidative stress and Parkinson’s disease. Front Neuroanat 9:91
Segura-Aguilar J, Paris I, Muñoz P, Ferrari E, Zecca L, Zucca FA (2014) Protective and toxic roles of dopamine in Parkinson’s disease. J Neurochem 129(6):898–915
Brieger K, Schiavone S, Miller FJ Jr, Krause K-H (2012) Reactive oxygen species: from health to disease. Swiss Med Wkly 142:w13659
Nikam S, Nikam P, Ahaley S, Sontakke AV (2009) Oxidative stress in Parkinson’s disease. Indian J Clin Biochem 24(1):98–101
Jenner P (2007) Oxidative stress and Parkinson’s disease. Handb Clin Neurol 83:507–520
Tamano H, Nishio R, Morioka H, Takeda A (2019) Extracellular Zn 2+ influx into nigral dopaminergic neurons plays a key role for pathogenesis of 6-hydroxydopamine-induced Parkinson’s disease in rats. Mol Neurobiol 56(1):435–443
Cruces-Sande A, Rodríguez-Pérez AI, Herbello-Hermelo P, Bermejo-Barrera P, Méndez-Álvarez E, Labandeira-García JL, Soto-Otero R (2019) Copper increases brain oxidative stress and enhances the ability of 6-hydroxydopamine to cause dopaminergic degeneration in a rat model of Parkinson’s disease. Mol Neurobiol 56(4):2845–2854
Dézsi L, Vécsei L (2017) Monoamine oxidase B inhibitors in Parkinson’s disease. CNS Neurol Disord Drug Targets 16(4):425–439
Schaffroth C, Bogacz M, Dirdjaja N, Nißen A, Krauth-Siegel RL (2016) The cytosolic or the mitochondrial glutathione peroxidase-type tryparedoxin peroxidase is sufficient to protect procyclic T rypanosoma brucei from iron-mediated mitochondrial damage and lysis. Mol Microbiol 99(1):172–187
Xu J, Kao S-Y, Lee FJ, Song W, Jin L-W, Yankner BA (2002) Dopamine-dependent neurotoxicity of α-synuclein: a mechanism for selective neurodegeneration in Parkinson disease. Nat Med 8(6):600
Michel PP, Hirsch EC, Hunot S (2016) Understanding dopaminergic cell death pathways in Parkinson disease. Neuron 90(4):675–691
Shaban NZ, Masoud MS, Awad D, Mawlawi MA, Sadek OM (2014) Effect of Cd, Zn and Hg complexes of barbituric acid and thiouracil on rat brain monoamine oxidase-B (in vitro). Chem Biol Interact 208:37–46
Youdim MB, Bakhle Y (2006) Monoamine oxidase: isoforms and inhibitors in Parkinson’s disease and depressive illness. Br J Pharmacol 147(S1)
Basu N, Scheuhammer A, Evans R, O'Brien M, Chan H (2007) Cholinesterase and monoamine oxidase activity in relation to mercury levels in the cerebral cortex of wild river otters. Hum Exp Toxicol 26(3):213–220
Basu N, Stamler CJ, Loua KM, Chan HM (2005) An interspecies comparison of mercury inhibition on muscarinic acetylcholine receptor binding in the cerebral cortex and cerebellum. Toxicol Appl Pharmacol 205(1):71–76
Daré E, Fetissov S, Hökfelt T, Hall H, Ögren SO, Ceccatelli S (2003) Effects of prenatal exposure to methylmercury on dopamine-mediated locomotor activity and dopamine D 2 receptor binding. Naunyn Schmiedebergs Arch Pharmacol 367(5):500–508
Coccini T, Roda E, Castoldi AF, Poli D, Goldoni M, Vettori MV, Mutti A, Manzo L (2011) Developmental exposure to methylmercury and 2, 2′, 4, 4′, 5, 5′-hexachlorobiphenyl (PCB153) affects cerebral dopamine D1-like and D2-like receptors of weanling and pubertal rats. Arch Toxicol 85(10):1281–1294
Faro L, Do Nascimento J, Alfonso M, Duran R (2002) Mechanism of action of methylmercury on in vivo striatal dopamine release: possible involvement of dopamine transporter. Neurochem Int 40(5):455–465
Dreiem A, Shan M, Okoniewski RJ, Sanchez-Morrissey S, Seegal RF (2009) Methylmercury inhibits dopaminergic function in rat pup synaptosomes in an age-dependent manner. Neurotoxicol Teratol 31(5):312–317
Faro L, Duran R, Do Nascimento J, Perez-Vences D, Alfonso M (2003) Effects of successive intrastriatal methylmercury administrations on dopaminergic system. Ecotoxicol Environ Saf 55(2):173–177
Vidal L, Alfonso M, Faro LF, Campos F, Cervantes R, Durán R (2007) Evaluation of the effects and mechanisms of action of mercuric chloride on striatal dopamine release by using in vivo microdialysis in freely moving rats. Toxicology 236(1-2):42–49
Zimmer B, Schildknecht S, Kuegler PB, Tanavde V, Kadereit S, Leist M (2011) Sensitivity of dopaminergic neuron differentiation from stem cells to chronic low-dose methylmercury exposure. Toxicol Sci 121(2):357–367
VanDuyn N, Settivari R, Wong G, Nass R (2010) SKN-1/Nrf2 inhibits dopamine neuron degeneration in a Caenorhabditis elegans model of methylmercury toxicity. Toxicol Sci 118(2):613–624
Götz M, Koutsilieri E, Riederer P, Ceccatelli S, Dare E (2002) Methylmercury induces neurite degeneration in primary culture of mouse dopaminergic mesencephalic cells. J Neural Transm 109(5-6):597–605
Bjørklund G, Stejskal V, Urbina MA, Dadar M, Chirumbolo S, Mutter J (2018) Metals and Parkinson’s disease: mechanisms and biochemical processes. Curr Med Chem 25(19):2198–2214
Hsu Y-C, Chang C-W, Lee H-L, Chuang C-C, Chiu H-C, Li W-Y, Horng J-T, Fu E (2016) Association between history of dental amalgam fillings and risk of Parkinson’s disease: a population-based retrospective cohort study in Taiwan. PLoS One 11(12):e0166552
Lafuente A, González-Carracedo A, Romero A, Cabaleiro T, Esquifino A (2005) Toxic effects of cadmium on the regulatory mechanism of dopamine and serotonin on prolactin secretion in adult male rats. Toxicol Lett 155(1):87–96
Savica R (2019) Livin’on the edge: risky behaviors and Parkinson disease: genes, environment, or both? AAN Enterprises
Marras C, Canning CG, Goldman SM (2019) Environment, lifestyle, and Parkinson’s disease: implications for prevention in the next decade. Mov Disord
Jiang H, Song N, Jiao Q, Shi L, Du X (2019) Iron pathophysiology in Parkinson diseases. In: Brain iron metabolism and CNS diseases. Springer, pp. 45–66
Dusek P, Roos PM, Litwin T, Schneider SA, Flaten TP, Aaseth J (2015) The neurotoxicity of iron, copper and manganese in Parkinson’s and Wilson’s diseases. J Trace Elem Med Biol 31:193–203
Bjørklund G, Dadar M, Mutter J, Aaseth J (2017) The toxicology of mercury: current research and emerging trends. Environ Res 159:545–554
Langston JW, Ballard P (1984) Parkinsonism induced by 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine (MPTP): implications for treatment and the pathogenesis of Parkinson’s disease. Can J Neurol Sci 11(S1):160–165
Liou H, Tsai M, Chen C, Jeng J, Chang Y, Chen S, Chen R (1997) Environmental risk factors and Parkinson’s disease a case-control study in Taiwan. Neurology 48(6):1583–1588
Pezzoli G, Cereda E (2013) Exposure to pesticides or solvents and risk of Parkinson disease. Neurology 80(22):2035–2041
Qi Z, Miller GW, Voit EO (2014) Rotenone and paraquat perturb dopamine metabolism: a computational analysis of pesticide toxicity. Toxicology 315:92–101
Bus JS, Gibson JE (1984) Paraquat: model for oxidant-initiated toxicity. Environ Health Perspect 55:37–46
Ossowska K, Śmiałowska M, Kuter K, Wierońska J, Zięba B, Wardas J, Nowak P, Dąbrowska J et al (2006) Degeneration of dopaminergic mesocortical neurons and activation of compensatory processes induced by a long-term paraquat administration in rats: implications for Parkinson’s disease. Neuroscience 141(4):2155–2165
Peng J, Peng L, Stevenson FF, Doctrow SR, Andersen JK (2007) Iron and paraquat as synergistic environmental risk factors in sporadic Parkinson’s disease accelerate age-related neurodegeneration. J Neurosci 27(26):6914–6922
Koppel N, Rekdal VM, Balskus EP (2017) Chemical transformation of xenobiotics by the human gut microbiota. Science 356(6344):eaag2770
Steventon GB, Sturman S, Waring RH, Williams AC (2001) A review of xenobiotic metabolism enzymes in Parkinson’s disease and motor neuron disease. Drug Metabol Drug Interact 18(2):79–98
Dmitriev A, Rudik A, Filimonov D, Lagunin A, Pogodin P, Dubovskaja V, Bezhentsev V, Ivanov S et al (2017) Integral estimation of xenobiotics’ toxicity with regard to their metabolism in human organism. Pure Appl Chem 89(10):1449–1458
Saravanan KS, Sindhu KM, Mohanakumar KP (2005) Acute intranigral infusion of rotenone in rats causes progressive biochemical lesions in the striatum similar to Parkinson’s disease. Brain Res 1049(2):147–155
Gao H-M, Liu B, Hong J-S (2003) Critical role for microglial NADPH oxidase in rotenone-induced degeneration of dopaminergic neurons. J Neurosci 23(15):6181–6187
Smeyne RJ, Jackson-Lewis V (2005) The MPTP model of Parkinson’s disease. Mol Brain Res 134(1):57–66
Doktór B, Damulewicz M, Pyza E (2019) Overexpression of mitochondrial ligases reverses rotenone-induced effects in a Drosophila model of Parkinson’s disease Front Neurosci:13
Cannon JR, Tapias V, Na HM, Honick AS, Drolet RE, Greenamyre JT (2009) A highly reproducible rotenone model of Parkinson’s disease. Neurobiol Dis 34(2):279–290
Venkatesh VG, Rajasankar S, Swaminathan WJ, Prabu K, Ramkumar M (2019) Antiapoptotic role of Agaricus blazei extract in rodent model of Parkinson’s disease. Frontiers in bioscience (Elite edition) 11:12–19
Hongo H, Kihara T, Kume T, Izumi Y, Niidome T, Sugimoto H, Akaike A (2012) Glycogen synthase kinase-3β activation mediates rotenone-induced cytotoxicity with the involvement of microtubule destabilization. Biochem Biophys Res Commun 426(1):94–99
Höglinger GU, Lannuzel A, Khondiker ME, Michel PP, Duyckaerts C, Féger J, Champy P, Prigent A et al (2005) The mitochondrial complex I inhibitor rotenone triggers a cerebral tauopathy. J Neurochem 95(4):930–939
Dhillon AS, Tarbutton GL, Levin JL, Plotkin GM, Lowry LK, Nalbone JT, Shepherd S (2008) Pesticide/environmental exposures and Parkinson’s disease in East Texas. J Agromedicine 13(1):37–48
Furlong M, Tanner CM, Goldman SM, Bhudhikanok GS, Blair A, Chade A, Comyns K, Hoppin JA et al (2015) Protective glove use and hygiene habits modify the associations of specific pesticides with Parkinson’s disease. Environ Int 75:144–150
Javed H, Azimullah S, Meeran M, Ansari SA, Ojha S (2019) Neuroprotective effects of thymol, a dietary monoterpene against dopaminergic neurodegeneration in rotenone-induced rat model of parkinson’s disease. Int J Mol Sci 20(7):1538
Kavuri S, Sivanesan S (2019) Evaluation of haematological alterations in intraperitoneal and oral rotenone induced parkinson’s disease wistar rats. Int J Pharm Res Allied Sci 8(2)
Hwang D-J, Kwon K-C, Song H-K, Kim K-S, Jung Y-S, Hwang D-Y, Cho J-Y (2019) Comparative analysis of dose-dependent neurotoxic response to 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine in C57BL/6 N mice derived from three different sources. Lab Anim Res 35(1):10
Langston JW (1985) MPTP and Parkinson’s disease. Trends Neurosci 8:79–83
Przedborski S, Jackson-Lewis V, Naini AB, Jakowec M, Petzinger G, Miller R, Akram M (2001) The parkinsonian toxin 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine (MPTP): a technical review of its utility and safety. J Neurochem 76(5):1265–1274
Nicklas W, Vyas I, Heikkila RE (1985) Inhibition of NADH-linked oxidation in brain mitochondria by 1-methyl-4-phenyl-pyridine, a metabolite of the neurotoxin, 1-methyl-4-phenyl-1, 2, 5, 6-tetrahydropyridine. Life Sci 36(26):2503–2508
Ghosh A, Langley MR, Harischandra DS, Neal ML, Jin H, Anantharam V, Joseph J, Brenza T et al (2016) Mitoapocynin treatment protects against neuroinflammation and dopaminergic neurodegeneration in a preclinical animal model of Parkinson’s disease. J NeuroImmune Pharmacol 11(2):259–278
Kamel F, Tanner C, Umbach D, Hoppin J, Alavanja M, Blair A, Comyns K, Goldman S et al (2006) Pesticide exposure and self-reported Parkinson’s disease in the agricultural health study. Am J Epidemiol 165(4):364–374
Costello S, Cockburn M, Bronstein J, Zhang X, Ritz B (2009) Parkinson’s disease and residential exposure to maneb and paraquat from agricultural applications in the central valley of California. Am J Epidemiol 169(8):919–926
Wang A, Costello S, Cockburn M, Zhang X, Bronstein J, Ritz B (2011) Parkinson’s disease risk from ambient exposure to pesticides. Eur J Epidemiol 26(7):547–555
Filograna R, Godena VK, Sanchez-Martinez A, Ferrari E, Casella L, Beltramini M, Bubacco L, Whitworth AJ et al (2016) Superoxide dismutase (SOD)-mimetic M40403 is protective in cell and fly models of paraquat toxicity implications for parkinson disease. J Biol Chem 291(17):9257–9267
Shimizu K, Matsubara K, Ohtaki K, Fujimaru S, Saito O, Shiono H (2003) Paraquat induces long-lasting dopamine overflow through the excitotoxic pathway in the striatum of freely moving rats. Brain Res 976(2):243–252
Manning-Bog AB, McCormack AL, Li J, Uversky VN, Fink AL, Di Monte DA (2002) The herbicide paraquat causes up-regulation and aggregation of α-synuclein in mice paraquat and α-synuclein. J Biol Chem 277(3):1641–1644
Cicchetti F, Lapointe N, Roberge-Tremblay A, Saint-Pierre M, Jimenez L, Ficke BW, Gross RE (2005) Systemic exposure to paraquat and maneb models early Parkinson’s disease in young adult rats. Neurobiol Dis 20(2):360–371
Saint-Pierre M, Tremblay MÈ, Sik A, Gross RE, Cicchetti F (2006) Temporal effects of paraquat/maneb on microglial activation and dopamine neuronal loss in older rats. J Neurochem 98(3):760–772
McCormack AL, Thiruchelvam M, Manning-Bog AB, Thiffault C, Langston JW, Cory-Slechta DA, Di Monte DA (2002) Environmental risk factors and Parkinson’s disease: selective degeneration of nigral dopaminergic neurons caused by the herbicide paraquat. Neurobiol Dis 10(2):119–127
Goldman SM, Kamel F, Ross GW, Bhudhikanok GS, Hoppin JA, Korell M, Marras C, Meng C et al (2012) Genetic modification of the association of paraquat and Parkinson’s disease. Mov Disord 27(13):1652–1658
Ritz BR, Manthripragada AD, Costello S, Lincoln SJ, Farrer MJ, Cockburn M, Bronstein J (2009) Dopamine transporter genetic variants and pesticides in Parkinson’s disease. Environ Health Perspect 117(6):964–969
Hou L, Huang R, Sun F, Zhang L, Wang Q (2019) NADPH oxidase regulates paraquat and maneb-induced dopaminergic neurodegeneration through ferroptosis. Toxicology 417:64–73
Tamano H, Nishio R, Morioka H, Furuhata R, Komata Y, Takeda A (2019) Paraquat as an environmental risk factor in Parkinson’s disease accelerates age-related degeneration via rapid influx of extracellular Zn 2+ into Nigral dopaminergic neurons. Mol Neurobiol:1–11
Cruz-Aguado R, Winkler D, Shaw CA (2006) Lack of behavioral and neuropathological effects of dietary β-methylamino-L-alanine (BMAA) in mice. Pharmacol Biochem Behav 84(2):294–299
Chiu AS, Gehringer MM, Braidy N, Guillemin GJ, Welch JH, Neilan BA (2013) Gliotoxicity of the cyanotoxin, β-methyl-amino-L-alanine (BMAA). Sci Rep 3:1482
Waidyanatha S, Ryan K, Sanders JM, McDonald JD, Wegerski CJ, Doyle-Eisle M, Garner CE (2018) Disposition of β-N-methylamino-l-alanine (L-BMAA), a neurotoxin, in rodents following a single or repeated oral exposure. Toxicol Appl Pharmacol 339:151–160
Montgomery EB Jr (1995) Heavy metals and the etiology of Parkinson’s disease and other movement disorders. Toxicology 97(1-3):3–9
Falup-Pecurariu C, Ferreira J, Martinez-Martin P, Chaudhuri KR (2017) Movement disorders curricula. Springer
Zayed J, Ducic S, Campanella G, Panisset J, Andre P, Masson H, Roy M (1990) Environmental factors in the etiology of Parkinson’s disease. Can J Neurol Sci 17(3):286–291
Miller K, Ochudło S, Opala G, Smolicha W, Siuda J (2003) Parkinsonism in chronic occupational metallic mercury intoxication. Neurol Neurochir Pol 37:31–38
Hegde ML, Shanmugavelu P, Vengamma B, Rao TS, Menon RB, Rao RV, Rao KJ (2004) Serum trace element levels and the complexity of inter-element relations in patients with Parkinson’s disease. J Trace Elem Med Biol 18(2):163–171
Winkel R, Kuhn W, Przuntek H (1995) Chronic intoxication with lead-and sulfur compounds may produce Parkinson’s disease. J Neural Transm Suppl 46:183–187
Gorell J, Johnson C, Rybicki B, Peterson E, Kortsha G, Brown G, Richardson R (1997) Occupational exposures to metals as risk factors for Parkinson’s disease. Neurology 48(3):650–658
Uversky VN, Li J, Fink AL (2001) Metal-triggered structural transformations, aggregation, and fibrillation of human α-synuclein a possible molecular link between parkinson’s disease and heavy metal exposure. J Biol Chem 276(47):44284–44296
Uversky VN (2017) Looking at the recent advances in understanding α-synuclein and its aggregation through the proteoform prism. F1000Research 6
de Bie RM, Gladstone RM, Strafella AP, Ko J-H, Lang AE (2007) Manganese-induced Parkinsonism associated with methcathinone (Ephedrone) abuse. Arch Neurol 64(6):886–889
Sanotsky Y, Lesyk R, Fedoryshyn L, Komnatska I, Matviyenko Y, Fahn S (2007) Manganic encephalopathy due to “ephedrone” abuse. Mov Disord 22(9):1337–1343
Sikk K, Taba P, Haldre S, Bergquist J, Nyholm D, Zjablov G, Asser T, Aquilonius SM (2007) Irreversible motor impairment in young addicts–ephedrone, manganism or both? Acta Neurol Scand 115(6):385–389
Olanow CW (2004) Manganese-induced parkinsonism and Parkinson’s disease. Ann N Y Acad Sci 1012(1):209–223
Guilarte TR (2010) Manganese and Parkinson’s disease: a critical review and new findings. Environ Health Perspect 118(8):1071–1080
Roth JA, Garrick MD (2003) Iron interactions and other biological reactions mediating the physiological and toxic actions of manganese. Biochem Pharmacol 66(1):1–13
Roth JA (2009) Are there common biochemical and molecular mechanisms controlling manganism and parkisonism. NeuroMolecular Med 11(4):281–296
Roth JA, Feng L, Walowitz J, Browne RW (2000) Manganese-induced rat pheochromocytoma (PC12) cell death is independent of caspase activation. J Neurosci Res 61(2):162–171
Harischandra DS, Ghaisas S, Zenitsky G, Jin H, Kanthasamy A, Anantharam V, Kanthasamy A (2019) Manganese-induced neurotoxicity: new insights into protein misfolding, mitochondrial impairment and neuroinflammation. Front Neurosci 13:654
Ellingsen DG, Shvartsman G, Bast-Pettersen R, Chashchin M, Thomassen Y, Chashchin V (2019) Neurobehavioral performance of patients diagnosed with manganism and idiopathic Parkinson disease. Int Arch Occup Environ Health 92(3):383–394
Ngim C-H, Devathasan G (1989) Epidemiologic study on the association between body burden mercury level and idiopathic Parkinson’s disease. Neuroepidemiology 8(3):128–141
Dantzig PI (2006) Parkinson’s disease, macular degeneration and cutaneous signs of mercury toxicity. J Occup Environ Med 48(7):656
Sun H (2018) Association of soil selenium, strontium, and magnesium concentrations with Parkinson’s disease mortality rates in the USA. Environ Geochem Health 40(1):349–357
Goldman S, Tanner C, Olanow C, Watts R, Field R, Langston J (2005) Occupation and parkinsonism in three movement disorders clinics. Neurology 65(9):1430–1435
Cariccio VL, Samà A, Bramanti P, Mazzon E (2019) Mercury involvement in neuronal damage and in neurodegenerative diseases. Biol Trace Elem Res 187(2):341–356
Xu F, Farkas S, Kortbeek S, Zhang F-X, Chen L, Zamponi GW, Syed NI (2012) Mercury-induced toxicity of rat cortical neurons is mediated through N-methyl-D-Aspartate receptors. Molecular brain 5(1):30
Björkblom B, Adilbayeva A, Maple-Grødem J, Piston D, Ökvist M, Xu XM, Brede C, Larsen JP et al (2013) Parkinson disease protein DJ-1 binds metals and protects against metal-induced cytotoxicity. J Biol Chem 288(31):22809–22820
Tysnes O-B, Storstein A (2017) Epidemiology of Parkinson’s disease. J Neural Transm 124(8):901–905
Goldman SM (2014) Environmental toxins and Parkinson’s disease. Annu Rev Pharmacol Toxicol 54:141–164
Bjørklund G, Hofer T, Nurchi VM, Aaseth J (2019) Iron and other metals in the pathogenesis of Parkinson’s disease: toxic effects and possible detoxification. J Inorg Biochem:110717
Logroscino G, Gao X, Chen H, Wing A, Ascherio A (2008) Dietary iron intake and risk of Parkinson’s disease. Am J Epidemiol 168(12):1381–1388
Miyake Y, Tanaka K, Fukushima W, Sasaki S, Kiyohara C, Tsuboi Y, Yamada T, Oeda T et al (2011) Dietary intake of metals and risk of Parkinson’s disease: a case-control study in Japan. J Neurol Sci 306(1-2):98–102
Piao Y-S, Lian T-H, Hu Y, Zuo L-J, Guo P, Yu S-Y, Liu L, Jin Z et al (2017) Restless legs syndrome in Parkinson disease: clinical characteristics, abnormal iron metabolism and altered neurotransmitters. Sci Rep 7(1):10547
Bharath S, Hsu M, Kaur D, Rajagopalan S, Andersen JK (2002) Glutathione, iron and Parkinson’s disease. Biochem Pharmacol 64(5-6):1037–1048
Ben-Shachar D, Zuk R, Glinka Y (1995) Dopamine neurotoxicity: inhibition of mitochondrial respiration. J Neurochem 64(2):718–723
Dexter D, Carayon A, Javoy-Agid F, Agid Y, Wells F, Daniel S, Lees A, Jenner P et al (1991) Alterations in the levels of iron, ferritin and other trace metals in Parkinson’s disease and other neurodegenerative diseases affecting the basal ganglia. Brain 114(4):1953–1975
Kaur D, Yantiri F, Rajagopalan S, Kumar J, Mo JQ, Boonplueang R, Viswanath V, Jacobs R et al (2003) Genetic or pharmacological iron chelation prevents MPTP-induced neurotoxicity in vivo: a novel therapy for Parkinson’s disease. Neuron 37(6):899–909
Lian T-H, Guo P, Zuo L-J, Hu Y, Yu S-Y, Yu Q-J, Jin Z, Wang R-D et al (2019) Tremor-dominant in Parkinson disease: the relevance to iron metabolism and inflammation. Front Neurosci 13:255
Sian-Hülsmann J, Mandel S, Youdim MB, Riederer P (2011) The relevance of iron in the pathogenesis of Parkinson’s disease. J Neurochem 118(6):939–957
Yu S-y, C-j C, L-j Z, Z-j C, T-h L, Wang F, Hu Y, Y-s P et al (2018) Clinical features and dysfunctions of iron metabolism in Parkinson disease patients with hyper echogenicity in substantia nigra: a cross-sectional study. BMC Neurol 18(1):9
Xuan M, Guan X, Gu Q, Shen Z, Yu X, Qiu T, Luo X, Song R et al (2017) Different iron deposition patterns in early-and middle-late-onset Parkinson’s disease. Parkinsonism Relat Disord 44:23–27
Guan X, Xuan M, Gu Q, Xu X, Huang P, Wang N, Shen Z, Xu J et al (2017) Influence of regional iron on the motor impairments of Parkinson’s disease: a quantitative susceptibility mapping study. J Magn Reson Imaging 45(5):1335–1342
Bjørklund G (2015) Clinical use of the metal chelators calcium disodium edetate, DMPS, and DMSA. Saudi J Kidney Dis Transpl 26(3):611
Cao Y, Chen A, Jones RL, Radcliffe J, Dietrich KN, Caldwell KL, Peddada S, Rogan WJ (2011) Efficacy of succimer chelation of mercury at background exposures in toddlers: a randomized trial. J Pediatr 158(3):480–485. e481
Rooney JP (2007) The role of thiols, dithiols, nutritional factors and interacting ligands in the toxicology of mercury. Toxicology 234(3):145–156
Joshi D, Patel J, Flora S, Kalia K (2008) Arsenic accumulation by Pseudomonas stutzeri and its response to some thiol chelators. Environ Health Prev Med 13(5):257–263
Hamidinia SA, Erdahl WL, Chapman CJ, Steinbaugh GE, Taylor RW, Pfeiffer DR (2005) Monensin improves the effectiveness of meso-dimercaptosuccinate when used to treat lead intoxication in rats. Environ Health Perspect 114(4):484–493
Crisponi G, Nurchi VM (2016) Chelating agents as therapeutic compounds—basic principles. Chelation therapy in the treatment of metal intoxication, academic press, Elsevier, London:35–61
Sears ME (2013) Chelation: harnessing and enhancing heavy metal detoxification—a review. Sci World J 2013
Flora G, Seth P, Prakash A, Mathur R (1995) Therapeutic efficacy of combined meso 2, 3-dimercaptosuccinic acid and calcium disodium edetate treatment during acute lead intoxication in rats. Hum Exp Toxicol 14(5):410–413
Flora SJ, Pachauri V (2010) Chelation in metal intoxication. Int J Environ Res Public Health 7(7):2745–2788
Ward RJ, Zucca FA, Duyn JH, Crichton RR, Zecca L (2014) The role of iron in brain ageing and neurodegenerative disorders. The Lancet Neurology 13(10):1045–1060
Double K, Reyes S, Werry E, Halliday G (2010) Selective cell death in neurodegeneration: why are some neurons spared in vulnerable regions? Prog Neurobiol 92(3):316–329
Barbosa JHO, Santos AC, Tumas V, Liu M, Zheng W, Haacke EM, Salmon CEG (2015) Quantifying brain iron deposition in patients with Parkinson’s disease using quantitative susceptibility mapping, R2 and R2. Magn Reson Imaging 33(5):559–565
Hare DJ, Double KL (2016) Iron and dopamine: a toxic couple. Brain 139(4):1026–1035
Zhang L, Yagnik G, Jiang D, Shi S, Chang P, Zhou F (2012) Separation of intermediates of iron-catalyzed dopamine oxidation reactions using reversed-phase ion-pairing chromatography coupled in tandem with UV–visible and ESI-MS detections. J Chromatogr B 911:55–58
Stokes AH, Hastings TG, Vrana KE (1999) Cytotoxic and genotoxic potential of dopamine. J Neurosci Res 55(6):659–665
Asanuma M, Miyazaki I, Ogawa N (2003) Dopamine-or L-DOPA-induced neurotoxicity: the role of dopamine quinone formation and tyrosinase in a model of Parkinson’s disease. Neurotox Res 5(3):165–176
Devos D, Moreau C, Devedjian JC, Kluza J, Petrault M, Laloux C, Jonneaux A, Ryckewaert G et al (2014) Targeting chelatable iron as a therapeutic modality in Parkinson’s disease. Antioxid Redox Signal 21(2):195–210
Dexter DT, Statton SA, Whitmore C, Freinbichler W, Weinberger P, Tipton KF, Della Corte L, Ward RJ et al (2011) Clinically available iron chelators induce neuroprotection in the 6-OHDA model of Parkinson’s disease after peripheral administration. J Neural Transm 118(2):223–231
Forni GL, Balocco M, Cremonesi L, Abbruzzese G, Parodi RC, Marchese R (2008) Regression of symptoms after selective iron chelation therapy in a case of neurodegeneration with brain iron accumulation. Mov Disord 23(6):904–907
Mounsey RB, Teismann P (2012) Chelators in the treatment of iron accumulation in Parkinson’s disease. Int J Cell Biol 2012
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Bjørklund, G., Dadar, M., Chirumbolo, S. et al. The Role of Xenobiotics and Trace Metals in Parkinson’s Disease. Mol Neurobiol 57, 1405–1417 (2020). https://doi.org/10.1007/s12035-019-01832-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-019-01832-1