Abstract
Glucagon-like peptide-1 (GLP-1) is an incretin hormone shown to be active in the treatment of type-2 diabetes (T2D) and has also been shown as efficacious in Alzheimer’s disease (AD). Dipeptidyl peptidase-4 (DPP-4), an enzyme that is expressed in numerous cells, rapidly inactivates endogenous GLP-1. Therefore, DPP-4 inhibition is employed as a therapeutic avenue to increase GLP-1 levels in the management of T2D. The effectiveness of DPP-4 inhibitors in the treatment of AD has been reported in various animal models of AD. With this background, the present study was designed to examine the effectiveness of linagliptin, a DPP-4 inhibitor in the 3xTg-AD mouse model of Alzheimer’s disease. Nine-month-old 3xTg-AD mice were administered linagliptin orally (5, 10, and 20 mg/kg) for 8 weeks. At the end of the linagliptin treatment, mice were evaluated for cognitive ability on the Morris Water Maze and Y-maze. Following cognitive evaluation, mice were sacrificed to determine the effect of the linagliptin on brain incretin levels, amyloid burden, tau phosphorylation, and neuroinflammation. We confirm that linagliptin treatment for 8 weeks mitigates the cognitive deficits present in 3xTg-AD mice. Moreover, linagliptin also improves brain incretin levels and attenuates amyloid beta, tau phosphorylation as well as neuroinflammation. In conclusion, linagliptin possesses neuroprotective properties that may be attributed to the improvement of incretin levels in the brain.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is a common neurodegenerative disorder, accounting for 80 % of global dementia cases [1] and leads to many cognitive and behavioral deficits. Acetylcholine esterase inhibitors such as rivastigmine, tacrine, galantamine, and donepezil and memantine (N-methyl-D-aspartate receptor antagonist) are the only drugs approved by the US Food and Drug Administration (FDA) for the symptomatic relief of AD [2]. The precise etiology of AD is still unknown and involves numerous mechanisms owing to its diverse and multifactorial nature [3]. Several disease-modifying strategies aimed at rescuing the progression of neurodegeneration including amyloid beta (Aβ) and tau aggregation inhibitors and immunotherapies have failed to alter the disease. Therefore, there is an urgent need to develop safe therapeutics that is effective in reversing the disease. Incretin-based drugs including glucagon-like peptide-1 (GLP-1) analogs are one such strategy that has recently been shown to be therapeutically effective in the treatment of AD. Recent studies have confirmed that GLP-1 analogs reverse the cognitive deficits and ameliorate neurodegeneration in AD [4, 5]. For instance, administration of liraglutide reduced plaques and improved cognitive performance in AD mouse models [6–8]. Other incretins and their analogs including exendin-4, lixisenatide, and Val(8) GLP-1, D-Ala2GIP have also been shown to be therapeutically beneficial in AD models [9–11].
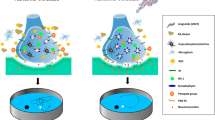
GLP-1 is an incretin hormone released from the L cells of the gastrointestinal tract in response to food intake and regulates insulin secretion from beta cells of the pancreas. This incretin hormone crosses the blood-brain barrier (BBB) and acts as a neurotransmitter in the brain. However, dipeptidyl peptidase-4 (DPP-4), a serine peptidase, inactivates GLP-1 leading to a very short half-life of the intact hormone (<2 min) [12]. Inhibition of DPP-4 is expected to show neuroprotection by increasing circulating GLP-1 levels. DPP-4 inhibition also improves glucose-dependent insulinotropic polypeptide (GIP), neuropeptide Y, brain natriuretic peptide, and stromal derived factor-1 [13]. The neuroprotective effects of GIP [14, 15], neuropeptide Y [16, 17], and stromal-derived factor-1 [18] are well documented. This further supports our hypothesis of DPP-4 inhibition as a novel therapeutic avenue for AD.
Commercially available DPP-4 inhibitors for human treatment include sitagliptin (Januvia), vildagliptin (Galvus), saxagliptin (Onglyza), alogliptin (Vipidia), and linagliptin (Tradjenta). Sitagliptin [19], vildagliptin [20] and saxagliptin [21] were previously reported as neuroprotective agents in animal models. Linagliptin is a moderately selective DPP-4 inhibitor approved by the FDA in 2011. Linagliptin does not pass through the BBB but peripheral DPP-4 inhibition increases incretin levels threefold, which does cross the BBB to afford neuroprotection [13, 22]. A recent study by Kornelius and colleagues [23] verified the neuroprotective activity of linagliptin on amyloid beta (Aβ)-induced cytotoxicity, and Darsalia and colleagues [24] demonstrated similar neuroprotective activity against stroke in normal and diabetic mice. In addition, linagliptin was also proven to be neuroprotective against Aβ-induced neurotoxicity in a Caenorhabditis elegans model of neurodegeneration and improved cognitive ability in a mouse model of ischemia [25, 26]. With respect to these findings, we believe linagliptin could be a possible therapeutic for mitigating the symptoms of AD. Hence, the current project was designed to test the therapeutic activity of linagliptin in the 3xTg-AD mouse model of AD.
Methods
Animals and Treatment
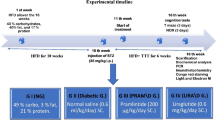
Female 3xTg-AD mice (9–10 months old) (n = 32) were procured from the animal facility of the University of Macau with prior approval from the Institutional Animal Ethical Committee. Reports indicate that female 3xTg-AD mice show greater pathological features than males [27, 28], and therefore, we only used female mice in our experiments. Mice were randomized and divided into four groups (eight mice in each), one control and three experimental groups. Mice from experimental groups received 5, 10, and 20 mg/kg of linagliptin orally while the control mice received 0.5 % sodium carboxymethyl cellulose (CMC-Na) once daily for 8 weeks. All mice were housed in individual ventilated cages in a room maintained with optimum temperature and humidity. An illustrative representation of the experimental scheme is shown in Fig. 1.
Morris Water Maze (MWM)
Following 8 weeks of linagliptin treatment, learning and memory skills of animals were tested using the Morris Water Maze (MWM) according to Branca et al. [29]. Briefly, the animals were freely allowed to locate a submerged escape platform in opaque water of a circular pool and the latency to reach the platform was measured from days 1 to 4. Throughout the experiment, the temperature of the pool (25 °C) and the location of the platform (14 in. from the south-west (SW) wall) were maintained constant. Mice were trained for 4 days with four trials per day and were assigned four pseudorandom starting points (E, SE, NW, and N) each day. A total of 16 trials were performed with each mouse in the acquisition phase. The animals were positioned facing the wall at one of the four starting positions and allowed to locate the submerged platform, 1.5 cm beneath the surface of the water. A successful trial was recorded when a mouse found the platform within 60 s. The mouse was allowed to stay on the platform for 5 s prior to being returned to its home cage. If a mouse was unable to locate the platform within 60 s, it was gently guided to the platform and allowed to stay on it for 15 s. The time required (latency) to find the escape platform was measured. A 60-s probe trial was performed without the escape platform on day 5. Time spent in the target quadrant where the escape platform was positioned and the number of platform crossings were recorded during this probe trial.
Y-Maze
The Y-maze apparatus consists of three arms of equal-length prepared with white PVC. Arms of the Y-maze are labeled A, B, and C and are positioned at an equal angle of 120° from each other and extend from the central platform. The test was performed as described by Sarnyai and colleagues [30]. Briefly, one arm (C) was closed during the training phase and kept constant for all the groups. The animal was positioned in one of the open arms (A) and allowed 15 min to explore the accessible arms (A and B) of the Y-maze. The maze was cleaned with 75 % alcohol between trials to avoid olfactory clues. All mice were returned to their home cages and given an hour intertrial interval before commencing the next phase. During the test phase, mice were allowed to explore the maze for 5 min with all arms open and the time spent in the novel arm (C) was recorded.
Spontaneous Alternation
A 6-min test was performed to measure spatial memory in the Y-maze by placing the mouse in the center of the maze and allowing the animal to freely explore. The maze was cleaned with 75 % alcohol between each trial to prevent olfactory clues. The arm entry sequence of each mouse was manually recorded. A successful alteration is represented by the animal visiting all three arms consecutively (ABC, ACB, BCA, BAC, CAB, and CBA). Percentage of alternation was calculated according to the formula: spontaneous alternation/total possible alternations × 100.
Biochemical Analysis
For biochemical characterization, 3xTg-AD mice were administered linagliptin or vehicle daily for 8 weeks. Upon completion of treatment, animals were anesthetized and perfused with phosphate buffer saline (PBS). Brains were immediately isolated and divided along the sagittal line into two hemispheres; the right hemisphere was stored at −80 °C for ELISA and Western blot analysis, and the left hemisphere was post-fixed in 4 % paraformaldehyde for histological analysis.
Enzyme-Linked Immunosorbent Assay (ELISA) and Glucose Assay
GLP-1, GIP, Aβ42, and Aβ40 ELISA kits were obtained from Millipore (EGLP-35K and EZRMGIP-55K) and Invitrogen (KMB3441 and KMB3481). Plasma glucose level was measured using an assay kit provided by Shanghai Rongsheng Biotech Co., Ltd. (361500) according to manufacturer instructions. All plates were analyzed on a multimode microplate plate reader (Molecular Devices, Berkshire, UK).
Western Blotting
Brains were homogenized with RIPA buffer containing protease inhibitor cocktail (05892791001, Roche) and phosphatase inhibitor cocktail (04906845001, Roche). The homogenate was centrifuged for 10 min at 21,000×g (4 °C), the resultant supernatant was separated and centrifuged again for 10 min at 21,000×g (4 °C), and the final supernatant was stored at −80 °C until use. All samples were mixed with sample buffer (sodium dodecyl sulfate), boiled for 5 min at 95 °C, loaded on a bisacrylamide gel (10 %), and electrophoresed. Proteins were transferred onto polyvinylidene difluoride (PVDF) membrane and incubated with the following primary antibodies: anti-tau antibody (MAB361, Millipore), phosphor-PHF-tau antibody (MN1020, Thermofisher), anti-GFAP antibody (MAB360, Millipore), anti-APP antibody (2452, Cell Signaling Technology), and anti-GAPDH antibody (MAB374, Millipore). Membranes were blocked with nonfat milk in TBS-T (tris-buffered saline with Tween 20) for 1 h. Primary antibodies were added in nonfat milk and incubated overnight at 4 °C, followed by washing with TBS-T (three washes, 5 min each) and incubated with HRP-conjugated secondary antibodies for 1 h at room temperature. Membranes were washed with TBS-T (three washes, 5 min each) and immunoreactivity was detected by ECL (6883S, Cell Signaling Technology). Immunoreactive species were visualized on a Bio-Rad system using Imagelab version 5.1 software and quantified using ImageJ software.
Immunohistochemistry
Left hemispheres were post-fixed in paraformaldehyde (4 %) for 48 h and transferred into a sucrose solution (30 %) for 72 h before sectioning. Paraffin-embedded sections (20 μm thick) were obtained using a microtome. Sections were washed with TBS (100 mM Tris pH 7.5, 150 mM NaCl) twice for 5 min each. Quenching was performed by incubating the sections with 90 % formic acid for 7 min followed by 30 min incubation with hydrogen peroxide (3 %). Sections were blocked by incubating in TBS-A (100 mM Tris pH 7.5, 150 mM NaCl, 0.1 % Triton X-100) for 15 min and TBS-B (100 mM Tris pH 7.5, 150 mM NaCl, 0.1 % Triton X-100, 2 % bovine serum albumin) for 30 min. Primary antibody Aβ42 (1:200, Biolegend, 805502) was diluted with TBS-B and sections were incubated overnight at 4 °C [29]. Sections were washed twice in TBS and incubated with biotinylated secondary antibody (31800, Thermofisher) for 30 min. Sections were detected using an ABC kit (32020, Thermofisher) and visualized with DAB quanto (TA-060-QHDX, Thermofisher).
Thioflavin S Staining and Microscopy
Immunofluroscence staining was performed according to Yousefi et al. [31]. Briefly, sections were incubated in Thioflavin S solution for 30 min followed by washing in water, three times (2 min each) and finally by 6 min incubation in 80 % ethanol. Sections were mounted with medium containing DAPI. Fluroscence images were obtained using a fluroscence microscope (Mirax Scan, Carl Zeiss MicroImaging GmbH, Jena, Germany).
Statistical Analyses
Statistical analyses were performed using GraphPad Prism (version 6.01, San Diego, CA, USA) and data expressed as mean ± standard error mean (SEM). One-way analysis of variance (ANOVA) followed by Bonferroni post hoc analysis was used for all the data analysis except MWM, which was analyzed using an unpaired t test. Data equal to or lesser than p < 0.05 was considered significant.
Results
Linagliptin Improves Cognitive Performance in 3xTg-AD Mice
To determine the effect of linagliptin treatment on learning and memory, we treated 3xTg-AD mice for 8 weeks and then tested their performance on the MWM and Y-maze. The MWM test was used to investigate the spatial cognitive behavior of animals treated with linagliptin. Initially, we observed no statistically significant difference (the first 2 days) in performance between the linagliptin-treated and control animals as is expected during the acquisition phase of the task. However, mice administered 10 and 20 mg/kg linagliptin demonstrated a gradual improvement in learning during acquisition trials (days 1–4) and revealed a significant decrease in escape latency. On day 3, latency to reach the platform was significantly reduced (p < 0.01) following 10 and 20 mg/kg linagliptin treatment as compared to control mice. Latency on day 4 was also significantly reduced with p < 0.01 and p < 0.001 at 10 and 20 mg/kg respectively as compared to control mice (Fig. 2). On day 5, during the probe trial, mice treated with 20 mg/kg linagliptin demonstrated a significant improvement in time spent in the platform quadrant (p < 0.01) and number of platform crossings (p < 0.05) compared to control mice (Fig. 2). Path length was also significantly reduced (p < 0.05) on days 3 and 4 by linagliptin treatment at 10 and 20 mg/kg. The outcomes from the behavioral tests indicate that linagliptin treatment facilitates learning and memory in 3xTg-AD mice. Supporting the MWM test, we also evaluated 3xTg-AD mice on a Y-maze to determine the effects of linagliptin treatment. Time spent in the novel arm and the percentage of alterations were measured using the Y-maze test. Mice treated with 20 mg/kg linagliptin displayed a 17.54 % increase in spontaneous alteration and on average spent 66.83 s more time (p < 0.05) in the novel arm compared to the control mice (Fig. 3). The spatial and working memory assessed by MWM and Y-maze indicates that linagliptin improved learning and memory in 3xTg-AD mice. Cognitive deficits displayed at 10 months of age in 3xTg-AD mice compared with wild-type mice (C57BL/6) on MWM and Y-maze performance is shown in the supplementary figures (Fig. S1 and Fig. S2).
Linagliptin reversed cognitive deficits in the Morris Water Maze. a Latency to reach the escape platform and b path length taken to reach the platform during acquisition trials. c Percentage of time spent in the platform quadrant and d number of platform crossings during the probe trial. e Tracking details on day 4 trial 4 of corresponding groups. Significance was analyzed by unpaired t test (n = 8, mean ± SEM) using Graphpad Prism. *p < 0.05 and **p < 0.01, compared with control mice
Linagliptin Increases GLP-1 and GIP in the Brain but Has no Effect on Plasma Glucose Level
DPP-4 inhibition elevates incretin levels, which might be responsible for the neuroprotective activity observed in the current study. To confirm this hypothesis, we measured brain GLP-1 and GIP levels using commercially available ELISA kits. We observed a significant increase in both GLP-1 (p < 0.01) and GIP (p < 0.05) levels in a dose-dependent manner following linagliptin treatment (Fig. 4). However, statistically significant increases in brain GIP and GLP-1 were only observed at medium and high doses of linagliptin (10 and 20 mg/kg). Low-dose linagliptin (5 mg/kg) did not show significant changes in incretin levels. We also evaluated the plasma glucose levels in 3xTg-AD mice following linagliptin treatment using a glucose assay kit. This was performed to evaluate the effect of linagliptin in non-diabetic mice. No significant changes were observed in plasma glucose levels following linagliptin treatment in the 3xTg-AD mice (Fig. 5).
Linagliptin increases glucagon-like peptide-1 (GLP-1) and glucose-dependent insulinotropic polypeptide (GIP) levels in the brain following 8 weeks of treatment. Significance was analyzed by one-way ANOVA (n = 6, mean ± SEM) following Bonferroni post hoc test using Graphpad Prism. *p < 0.05 and **p < 0.01, compared with control mice. Levels of GLP-1 (a) and GIP (b) in the brain
Linagliptin Reduces Aβ42 but not Aβ40
Amyloid burden is one of the cardinal pathological features in AD and it increases with age in 3xTg-AD mice [32]. Increases in plaque load positively correlate with cognitive deficits in the mice. Following behavioral testing, animals were sacrificed to determine the mechanisms underlying the alleviation of cognitive deficits following linagliptin treatment. To define the influence of linagliptin on plaque burden, we performed ELISA of brain homogenates and quantified the levels of Aβ40 and Aβ42. Linagliptin administration for 8 weeks significantly (p < 0.01) reduced the Aβ42 level at a dose of 20 mg/kg as compared to control mice (Fig. 6). There was no significant change in Aβ40 level between the control and treatment groups, demonstrating that linagliptin only affects Aβ42 levels.
Linagliptin decreases brain amyloid burden following 8 weeks of treatment by decreasing amyloid beta 1–42 levels. Significance was analyzed by one-way ANOVA (n = 6, mean ± SEM) following Bonferroni post hoc test using Graphpad Prism. **p < 0.01, compared with control mice. a Levels of Aβ42 and b Aβ40 in the brain
Linagliptin Reduces Phosphorylated Tau and Neuroinflammation
Tau phosphorylation is also a major feature in the progression of AD and also worsens with age in 3xTg-AD mice [32]. To access the outcome of linagliptin treatment on tau phosphorylation, we performed Western blotting using AT8 primary antibody that detects phosphorylated tau at Ser202/Thr205. A significant (p < 0.01) reduction in p-tau at 20 mg/kg of linagliptin as compared to control mice was observed. Chronic neuroinflammation is an additional pathological feature in the AD brain. Interestingly, linagliptin at 20 mg/kg also reduced (p < 0.05) GFAP immunoreactivity, a marker for inflammation. We also examined levels of the amyloid precursor protein (APP) (Fig. 7) and total tau (data not shown) following linagliptin treatment but failed to observe any changes in these proteins.
Linagliptin reduces tau phosphorylation and neuroinflammation following 8 weeks of treatment. Significance was analyzed by one-way ANOVA (n = 5, mean ± SEM) following Bonferroni post hoc test using Graphpad Prism. *p < 0.05 and **p < 0.01, compared with control mice. a Representative immunoreactive species of GFAP, P-tau, APP, and GAPDH in control and treated mice and b their corresponding densities. Lane 1: control, Lane 2: linagliptin 5 mg/kg, Lane 3: linagliptin 10 mg/kg, and Lane 4: linagliptin 20 mg/kg
Histology of Brain Sections Following Linagliptin Treatment
The efficacy of treatment on plaque deposition was examined by immunohistochemistry using the mouse monoclonal anti-Aβ42 antibody 12F4 and by immunofluorescence using thioflavin S staining. Figures 8 and 9 represent images from brain sections of control and treated mice after immunohistochemistry and thioflavin S staining. Plaque load in the control mice was taken as reference (100 %) to determine the treatment effects of linagliptin. Immunohistochemistry of different groups proved that Aβ deposits in the linagliptin-treated (20 mg/kg) animals were reduced significantly (p < 0.01) as compared with control mice (Fig. 8). Plaque load was also confirmed by thioflavin S staining and quantification of plaques. Thioflavin S positive plaques were also significantly reduced (p < 0.05 and p < 0.01) by linagliptin treatment at 10 and 20 mg/kg, respectively (Fig. 9). Taken together, linagliptin treatment for 8 weeks effectively ameliorated plaque deposition in the 3xTg-AD mouse model of AD.
Immunohistochemical analysis of amyloid plaques shows that linagliptin reduces amyloid burden following 8 weeks of treatment. Significance was analyzed by one-way ANOVA (n = 5, mean ± SEM) following Bonferroni post hoc test using Graphpad Prism. **p < 0.01 compared with control mice. a Representative images of immunohistochemistry at 2×, and b the plaque count per section
Thioflavin S staining of amyloid plaques shows that linagliptin reduces amyloid plaques following 8 weeks of treatment. Significance was analyzed by one-way ANOVA (n = 5, mean ± SEM) following Bonferroni post hoc test using Graphpad Prism. *p < 0.05 and **p < 0.01, compared with control mice. a Representative images of thioflavin S staining at 5×, and b the plaque count per section
Discussion
Aging is a major risk factor contributing to AD. A wide range of diseases are linked with aging including diabetes and cardiovascular disorders [29]. Type-2-diabetes (T2D) is a recently identified risk factor and shares many features with AD [33, 34] that has led to the suggestion that treatments used for T2D might be beneficial in treating the pathologies associated with AD. Metformin and pioglitazone, two drugs used for T2D, have demonstrated promising results in preclinical models of AD [35, 36]. DPP-4 inhibitors are a novel class of T2D medications that have also shown beneficial effects in AD animal models [19–21]. We previously demonstrated that administration of vildagliptin [20] and saxagliptin [21] to streptozotocin-induced AD rats afforded neuroprotective effects. In the present study, 9–10-month-old female 3xTg-AD mice were treated daily with a DPP-4 inhibitor, linagliptin for a period of 8 weeks. This treatment period was chosen based on a previous study by Ma and colleagues [25] who demonstrated that treatment with linagliptin for 8 weeks resulted in the amelioration of cognitive impairment and brain atrophy induced by transient cerebral ischemia in type 2 diabetic mice. Our data reveal that, under controlled environmental conditions, linagliptin improves learning and memory and alleviates clinical manifestations observed in 3xTg-AD mice. Taken together, the present data enhance the existing knowledge and contribute to the basic understanding of the role of DPP-4 inhibitors in AD.
The triple transgenic mouse model of AD (3xTg-AD) is a phenotypically well-characterized model and is ideally suited to screen therapeutic molecules against AD. 3xTg-AD mice have been reported to show cognitive deficits by 6 months, which worsens with age [37]. In the current study, the MWM and Y-maze tasks were used to test memory deficits in 3xTg-AD female mice at the age of 11–12 months. The MWM was carried out to observe spatial learning and memory whereas the Y-maze was used to monitor working memory; both tasks are highly sensitive tests and ideally suited to determine the effects of therapeutics in 3xTg-AD mice [38, 39]. Learning and memory enhancement was observed following linagliptin treatment and this is consistent with previous reports employing other DPP-4 inhibitors [19–21, 40, 41]. Sitagliptin and vildagliptin were also shown to improve cognitive function in insulin-resistant animal models [42, 43]. In the current study, linagliptin-treated mice demonstrated improved memory in the MWM compared to control mice. The treated mice also demonstrated enhanced spatial awareness by spending increased periods of time in the platform quadrant during the probe trial. The role of GLP-1 and GIP in cognitive function has been proved in receptor-knockout mice [44, 45]. We now extend this work by demonstrating that blocking the peripheral action of DPP-4 and thereby increasing levels of GLP-1 and GIP crossing the blood-brain barrier leads to cognitive enhancement in a disease-relevant animal model. Additional work will be necessary to decipher the mechanisms underlying the cognitive improvement observed in the present study.
Endogenous GLP-1 and GIP have a very short half-life and in order to prevent degradation from DPP-4, incretins that are DPP-4 resistant and possess longer half-life have been developed. Endogenous incretins and their analogs can cross the BBB, and a few studies suggest that DPP-4 inhibition may also increase GLP-1 levels in the brain [13, 22]. GLP-1 and GIP as well as their agonists promote cell differentiation, proliferation, and growth in the brain [46, 47]. In the current study, linagliptin administration for 8 weeks enhanced incretin levels in the brain. This suggests that there is a direct effect of incretins in mitigating the pathological markers of AD, including amyloid and tau in 3xTg-AD mice. Our study demonstrates that linagliptin reduced amyloid burden and tau phosphorylation following 8 weeks of treatment in 3xTg-AD mice. Reduced plaque load might be due to reduced production of Aβ since GLP-1 reduces APP processing by binding to its C-terminus. Similarly, GLP-1 protects SH-SY5Y neuroblastoma cells against Aβ-induced apoptosis [48, 49]. Prior reports have also shown that exendin-4, a GLP-1 receptor analog, downregulates glycogen synthase kinase 3β (GSK3β) and decreases the phosphorylation of tau [50]. It is plausible that the reduced tau hyperphosphorylation observed in our study might be due to downregulation of GSK3β. However, the relationship between tau phosphorylation and amyloid burden is highly complex. GLP-1 and its analogs have been proposed to prevent neurodegeneration by improving long-term potentiation and modifying synaptic plasticity [51, 52]. The neuroprotection afforded by incretins is well reported in animal models [4, 6–11, 15, 53, 54]. Clinical trials on exendin-4 and liraglutide in patients with AD are ongoing. Furthermore, previous studies on DPP-4 inhibitors against AD have shown consistent results on reducing both amyloid burden and tau phosphorylation in animal models [19–21]. In addition, our immunohistochemistry and thioflavin S staining results also reveal the reduction of overall plaque load in 11–12-month-old 3xTg-AD mice following linagliptin treatment.
Neuroinflammation is another well-known feature observed in the brain of Alzheimer’s patients. The decreased cognitive capacity in AD might be attributed to increased production of cytokines including interleukins and tumor necrosis factor. Aβ production and tau phosphorylation are upregulated by activated glia which appears to be an initial cause in AD pathophysiology [55]. In the present study, linagliptin mitigates neuroinflammation by significantly reducing GFAP, which is consistent with the previous reports on DPP-4 inhibitors [19–21]. Recent studies on DPP-4 inhibitors have demonstrated the reduction of inflammatory cytokine levels in chronic inflammatory conditions including atherosclerosis and myocarditis [56, 57]. In addition, GLP-1 and GIP act as anti-inflammatory mediators and counteract neuroinflammation in AD [34, 58]. GLP-1, GIP, and their analogs are also well known for their neuroprotective activity by reducing neuroinflammation [9, 59, 60]. This demonstrates that DPP-4 inhibition and incretins have independent roles in mitigating neuroinflammation.
Collectively, our investigation shows that the DPP-4-targeting molecule linagliptin mitigates plaque load and reduces tau phosphorylation, two cardinal pathologies observed in Alzheimer’s disease. 3xTg-AD mice administered 20 mg/kg linagliptin demonstrate reduced cognitive deficits and improved performance on MWM and Y-maze. Linagliptin dose-dependently improves brain levels of both GLP-1 and GIP incretins and reduces neuroinflammation, which may be attributed to the reduced amyloid burden and increased incretin levels. In conclusion, we have shown that DPP-4 inhibitors represent a promising therapeutic avenue in the management of AD.
References
Kumar A, Singh A, Ekavali (2015) A review on Alzheimer’s disease pathophysiology and its management: an update. Pharmacol Reports 67:195–203. doi:10.1016/j.pharep.2014.09.004
Auld DS, Kornecook TJ, Bastianetto S, Quirion R (2002) Alzheimer’s disease and the basal forebrain cholinergic system: relations to beta-amyloid peptides, cognition, and treatment strategies. Prog Neurobiol 68:209–245. doi:10.1016/s0301-0082(02)00079-5
Kazim SF, Blanchard J, Dai C-L, Tung Y-C, LaFerla FM, Iqbal I-G, Iqbal K et al (2014) Disease modifying effect of chronic oral treatment with a neurotrophic peptidergic compound in a triple transgenic mouse model of Alzheimer’s disease. Neurobiol Dis 71:110–130. doi:10.1016/j.nbd.2014.07.001
Calsolaro V, Edison P (2015) Novel GLP-1 (Glucagon-Like Peptide-1) Analogues and Insulin in the Treatment for Alzheimer’s Disease and Other Neurodegenerative Diseases. CNS Drugs 29:1023–1039. doi:10.1007/s40263-015-0301-8
Holscher C (2010) Incretin analogues that have been developed to treat type 2 diabetes hold promise as a novel treatment strategy for Alzheimer’s disease. Recent Pat CNS Drug Discov 5:109–117
McClean PL, Jalewa J, Hölscher C (2015) Prophylactic liraglutide treatment prevents amyloid plaque deposition, chronic inflammation and memory impairment in APP/PS1 mice. Behav Brain Res 293:96–106. doi:10.1016/j.bbr.2015.07.024
Qi L, Ke L, Liu X, Liao L, Ke S, Liu X, Wang Y, Lin X et al (2016) Subcutaneous administration of liraglutide ameliorates learning and memory impairment by modulating tau hyperphosphorylation via the glycogen synthase kinase-3β pathway in an amyloid β protein induced alzheimer disease mouse model. Eur J Pharmacol 783:23–32. doi:10.1016/j.ejphar.2016.04.052
Hansen HH, Fabricius K, Barkholt P, Niehoff ML, Morley JE, Jelsing J, Pyke C, Knudsen LB et al (2015) The GLP-1 Receptor Agonist Liraglutide Improves Memory Function and Increases Hippocampal CA1 Neuronal Numbers in a Senescence-Accelerated Mouse Model of Alzheimer’s Disease. J Alzheimer’s Dis 46:877–888. doi:10.3233/JAD-143090
Duffy AM, Holscher C (2013) The incretin analogue D-Ala2GIP reduces plaque load, astrogliosis and oxidative stress in an APP/PS1 mouse model of Alzheimer’s disease. Neuroscience 228:294–300. doi:10.1016/j.neuroscience.2012.10.045
McClean PL, Hölscher C (2014) Lixisenatide, a drug developed to treat type 2 diabetes, 15 shows neuroprotective effects in a mouse model of Alzheimer’s disease. Neuropharmacology 86:241–258. doi:10.1016/j.neuropharm.2014.07.015
Jia X, Ye-Tian Y-L, Zhang GJ, Liu ZD, Di ZL, Ying XP, Fang Y et al (2016) Exendin-4, a glucagon-like peptide 1 receptor agonist, protects against amyloid-β peptide-induced impairment of spatial learning and memory in rats. Physiol Behav 159:72–79. doi:10.1016/j.physbeh.2016.03.016
Katsurada K, Yada T (2016) Neural effects of gut- and brain-derived glucagon-like peptide-1 and its receptor agonist. J Diabetes Investig 7:64–69. doi:10.1111/jdi.12464
Shannon RP (2013) DPP-4 inhibition and neuroprotection: do mechanisms matter? Diabetes 62:1029–1031. doi:10.2337/db12-1794
Metcalfe MJ, Figueiredo-Pereira ME (2010) Relationship between tau pathology and neuroinflammation in Alzheimer’s disease. Mt Sinai J Med 77:50–58. doi:10.1002/msj.20163
Ji C, Xue G-F, Lijun C, Feng P, Li D, Li L, Li G, Holscher C et al (2016) A novel dual GLP-1 and GIP receptor agonist is neuroprotective in the MPTP mouse model of Parkinson’s disease by increasing expression of BNDF. Brain Res 11:326–331. doi:10.1016/j.brainres.2015.09.035
Angelucci F, Gelfo F, Fiore M, Croce N, Mathe AA, Bernardini S, Caltagirone C et al (2014) The effect of neuropeptide Y on cell survival and neurotrophin expression in in-vitro models of Alzheimer’s disease. Can J Physiol Pharmacol 92:621–630. doi:10.1139/cjpp-2014-0099
Spencer B, Potkar R, Metcalf J, Thrin I, Adame A, Rockenstein E, Masliah E et al (2016) Systemic central nervous system (CNS)-targeted delivery of neuropeptide y (NPY) reduces neurodegeneration and increases neural precursor cell proliferation in a mouse model of Alzheimer disease. J Biol Chem 291:1905–1920. doi:10.1074/jbc.M115.678185
Wang Q, Xu Y, Chen J-C, Qin YY, Liu M, Liu Y, Xie MJ, Yu ZY et al (2012) Stromal cell-derived factor 1α decreases β-amyloid deposition in Alzheimer’s disease mouse model. Brain Res 1459:15–26. doi:10.1016/j.brainres.2012.04.011
D’Amico M, Di Filippo C, Marfella R, Abbatecola AM, Ferraraccio F, Rossi F, Paolisso G et al (2010) Long-term inhibition of dipeptidyl peptidase-4 in Alzheimer’s prone mice. Exp Gerontol 45:202–207. doi:10.1016/j.exger.2009.12.004
Kosaraju J, Murthy V, Khatwal RB, Dubala A, Chinni S, Muthureddy Nataraj SK, Basavan D et al (2013) Vildagliptin: an anti-diabetes agent ameliorates cognitive deficits and pathology observed in streptozotocin-induced Alzheimer’s disease. J Pharm Pharmacol 65:1773–1784. doi:10.1111/jphp.1214816
Kosaraju J, Gali CC, Khatwal RB, Dubala A, Chinni S, Holsinger RM, Madhunapantula VS, Muthureddy Nataraj SK et al (2013) Saxagliptin: a dipeptidyl peptidase-4 inhibitor ameliorates streptozotocin induced Alzheimer’s disease. Neuropharmacology 72:291–300. doi:10.1016/j.neuropharm.2013.04.008
Deacon CF (2011) Dipeptidyl peptidase-4 inhibitors in the treatment of type 2 diabetes: a comparative review. Diabetes, Obes Metab 13:7–18. doi:10.1111/j.1463-1326.2010.01306.x
Kornelius E, Lin C-L, Chang H-H, Li HH, Huang WN, Yang WS, Lu YL, Peng CH et al (2015) DPP-4 inhibitor Linagliptin attenuates Aβ-induced cytotoxicity through activation of AMPK in neuronal cells. CNS Neurosci Ther 21:549–557. doi:10.1111/cns.12404
Darsalia V, Ortsäter H, Olverling A, Darlof E, Wolbert P, Nystrom T, Klein T, Sjoholm A et al (2013) The DPP-4 inhibitor linagliptin counteracts stroke in the normal and diabetic mouse brain: A comparison with glimepiride. Diabetes 62:1289–1296. doi:10.2337/db12-0988
Ma M, Hasegawa Y, Koibuchi N, Toyama K, Uekawa K, Nakagawa T, Lin B, Kim- Mitsuyama S et al (2015) DPP-4 inhibition with linagliptin ameliorates cognitive impairment and brain atrophy induced by transient cerebral ischemia in type 2 diabetic mice. Cardiovasc Diabetol 14:54. doi:10.1186/s12933-015-0218-z
Wongchai K, Schlotterer A, Lin J, Humpert PM, Klein T, Hammes H-P, Morcos M et al (2015) Protective Effects of Liraglutide and Linagliptin in C. elegans as a New Model for Glucose-Induced Neurodegeneration. Horm Metab Res 48:70–75. doi:10.1055/s-0035-1549876
Hirata-Fukae C, Li HF, Hoe HS, Gray AJ, Minami SS, Hamada K, Niikura T, Hua F et al (2008) Females exhibit more extensive amyloid, but not tau, pathology in an Alzheimer transgenic model. Brain Res 1216:92–103. doi:10.1016/j.brainres.2008.03.079
Clinton LK, Billings LM, Green KN, Caccamo A, Nqot J, Oddo S, McGauqh JL, LaFerla FM et al (2007) Age-dependent sexual dimorphism in cognition and stress response in the 3xTg-AD mice. Neurobiol Dis 28:76–82. doi:10.1016/j.nbd.2007.06.013
Branca C, Wisely EV, Hartman LK, Caccamo A, Oddo S et al (2014) Administration of a selective β2 adrenergic receptor antagonist exacerbates neuropathology and cognitive deficits in a mouse model of Alzheimer’s disease. Neurobiol Aging 35:2726–2735. doi:10.1016/j.neurobiolaging.2014.06.011
Sarnyai Z, Sibille EL, Pavlides C, Fenster RJ, McEwen BS, Toth M et al (2000) Impaired hippocampal-dependent learning and functional abnormalities in the hippocampus in mice lacking serotonin(1A) receptors. Proc Natl Acad Sci U S A 97:14731–14736. doi:10.1073/pnas.97.26.1473117
Yousefi BH, von Reutern B, Scherübl D, Manook A, Schwaiger M, Grimmer T, Henriksen G, Förster S et al (2015) FIBT versus florbetaben and PiB: a preclinical comparison study with amyloid-PET in transgenic mice. EJNMMI Res 5:20. doi:10.1186/s13550-015-0090-6
Puzzo D, Lee L, Palmeri A, Calabrese G, Arancio O et al (2014) Behavioral assays with mouse models of Alzheimer’s disease: Practical considerations and guidelines. Biochem Pharmacol 88:450–467. doi:10.1016/j.bcp.2014.01.011
Mittal K, Mani RJ, Katare DP (2016) Type 3 Diabetes: Cross Talk between Differentially Regulated Proteins of Type 2 Diabetes Mellitus and Alzheimer’s Disease. Sci Rep 6:25589. doi:10.1038/srep25589
Yu Y-W, Hsieh T-H, Chen K-Y, Wu JC, Hoffer BJ, Greig NH, Li Y, Lai JH et al (2016) Glucose-Dependent Insulinotropic Polypeptide Ameliorates Mild Traumatic Brain Injury-Induced Cognitive and Sensorimotor Deficits and Neuroinflammation in Rats. J Neurotrauma. doi:10.1089/neu.2015.4229
Asadbegi M, Yaghmaei P, Salehi I, Ebrahim-Habibi A, Komaki A et al (2016) Neuroprotective effects of metformin against Aβ-mediated inhibition of long-term potentiation in rats fed a high-fat diet. Brain Res Bull 121:178–185. doi:10.1016/j.brainresbull.2016.02.005
Toba J, Nikkuni M, Ishizeki M, Yoshii A, Watamura N, Inoue T, Ohshima T et al (2016) PPARγ agonist pioglitazone improves cerebellar dysfunction at pre-Aβ deposition stage in APPswe/PS1dE9 Alzheimer’s disease model mice. Biochem Biophys Res Commun 473:1039–1044. doi:10.1016/j.bbrc.2016.04.012
Stevens LM, Brown RE (2015) Reference and working memory deficits in the 3xTg-AD mouse between 2 and 15-months of age: A cross-sectional study. Behav Brain Res 278:496–505. doi:10.1016/j.bbr.2014.10.033
Baeta-Corral R, Giménez-Llort L (2015) Persistent hyperactivity and distinctive strategy features in the Morris water maze in 3xTg-AD mice at advanced stages of disease. Behav Neurosci 129:129–137. doi:10.1037/bne0000027
Stover KR, Campbell MA, Van Winssen CM, Brown RE (2015) Early detection of cognitive deficits in the 3xTg-AD mouse model of Alzheimer’s disease. Behav Brain Res 289:29–38. doi:10.1016/j.bbr.2015.04.012
Matteucci E, Giampietro O (2015) Mechanisms of neurodegeration in type 2 diabetes and the neuroprotective potential of dipeptidyl peptidase 4 inhibitor. Curr Med Chem 22:1573–1581
Jain S, Sharma B (2015) Neuroprotective effect of selective DPP-4 inhibitor in experimental vascular dementia. Physiol Behav 152:182–193. doi:10.1016/j.physbeh.2015.09.007
Pintana H, Apaijai N, Chattipakorn N, Chattipakorn SC (2013) DPP-4 inhibitors improve cognition and brain mitochondrial function of insulin-resistant rats. J Endocrinol 218:1–11. doi:10.1530/JOE-12-0521
Sakr HF (2013) Effect of sitagliptin on the working memory and reference memory in type 2 diabetic Sprague-Dawley rats: possible role of adiponectin receptors 1. J Physiol Pharmacol 64:613–623
Abbas T, Faivre E, Hölscher C (2009) Impairment of synaptic plasticity and memory formation in GLP-1 receptor KO mice: Interaction between type 2 diabetes and Alzheimer’s disease. Behav Brain Res 205:265–271. doi:10.1016/j.bbr.2009.06.035
Faivre E, Gault VA, Thorens B, Hölscher C (2011) Glucose-dependent insulinotropic polypeptide receptor knockout mice are impaired in learning, synaptic plasticity, and neurogenesis. J Neurophysiol 105:1574–1580. doi:10.1152/jn.00866.2010
Faivre E, Hamilton A, Hölscher C (2012) Effects of acute and chronic administration of GIP analogues on cognition, synaptic plasticity and neurogenesis in mice. Eur J Pharmacol 674:294–306. doi:10.1016/j.ejphar.2011.11.007
Nyberg J (2005) Glucose-Dependent Insulinotropic Polypeptide Is Expressed in Adult Hippocampus and Induces Progenitor Cell Proliferation. J Neurosci 25:1816–1825. doi:10.1523/JNEUROSCI.4920-04.2005
Qin Z, Sun Z, Huang J, Hu Y, Wu Z, Mei B et al (2008) Mutated recombinant human glucagon-like peptide-1 protects SH-SY5Y cells from apoptosis induced by amyloid-beta peptide (1-42). Neurosci Lett 444:217–221. doi:10.1016/j.neulet.2008.08.047
Perry T, Greig NH (2002) The glucagon-like peptides: a new genre in therapeutic targets for intervention in Alzheimer’s disease. J Alzheimers Dis 4:487–496
Chen S, Liu AR, An FM, Yao WB, Gao XD et al (2012) Amelioration of neurodegenerative changes in cellular and rat models of diabetes-related Alzheimer’s disease by exendin-4. Age (Omaha) 34:1211–1224. doi:10.1007/s11357-011-9303-8
Gault VA, Hölscher C (2008) GLP-1 agonists facilitate hippocampal LTP and reverse the impairment of LTP induced by beta-amyloid. Eur J Pharmacol 587:112–117. doi:10.1016/j.ejphar.2008.03.02519
McClean PL, Gault VA, Harriott P, Hölscher C (2010) Glucagon-like peptide-1 analogues enhance synaptic plasticity in the brain: A link between diabetes and Alzheimer’s disease. Eur J Pharmacol 630:158–162. doi:10.1016/j.ejphar.2009.12.023
Hansen HH, Barkholt P, Fabricius K, Jelsing J, Terwel D, Pyke C, Knudsen LB, Vrang N et al (2016) The GLP-1 receptor agonist liraglutide reduces pathology-specific tau phosphorylation and improves motor function in a transgenic hTauP301L mouse model of tauopathy. Brain Res 1634:158–170. doi:10.1016/j.brainres.2015.12.052
McClean PL, Hölscher C (2014) Liraglutide can reverse memory impairment, synaptic loss and reduce plaque load in aged APP/PS1 mice, a model of Alzheimer’s disease. Neuropharmacology 76:57–67. doi:10.1016/j.neuropharm.2013.08.005
Calsolaro V, Edison P (2016) Neuroinflammation in Alzheimer’s disease: Current evidence and future directions. Alzheimers Dement 12:719–732. doi:10.1016/j.jalz.2016.02.010
Hirakawa H, Zempo H, Ogawa M, Watanabe R, Suzuki J, Akazawa H, Komuro I, Isobe M et al (2015) A DPP-4 inhibitor suppresses fibrosis and inflammation on experimental autoimmune myocarditis in mice. PLoS One 10, e0119360. doi:10.1371/journal.pone.0119360
Shah Z, Kampfrath T, Deiuliis JA, Zhong J, Pineda C, Ying Z, Xu X, Lu B et al (2011) Long-term dipeptidyl-peptidase 4 inhibition reduces atherosclerosis and inflammation via effects on monocyte recruitment and chemotaxis. Circulation 124:2338–2349. doi:10.1161/CIRCULATIONAHA.111.041418
Song X, Jia H, Jiang Y, Wang L, Zhang Y, Mu Y, Liu Y et al (2015) Anti-atherosclerotic effects of the glucagon-like peptide-1 (GLP-1) based therapies in patients with type 2 Diabetes Mellitus: A meta-analysis. Sci Rep 5:10202. doi:10.1038/srep10202
Long-Smith CM, Manning S, McClean PL, Coakley MF, O’Halloran DJ, Holscher C, O’Neill C et al (2013) The diabetes drug liraglutide ameliorates aberrant insulin receptor localisation and signalling in parallel with decreasing both amyloid-β plaque and glial pathology in a mouse model of Alzheimer’s disease. Neuro Mol Med 15:102–114. doi:10.1007/s12017-012-8199-5
McClean PL, Parthsarathy V, Faivre E, Holscher C (2011) The Diabetes Drug Liraglutide Prevents Degenerative Processes in a Mouse Model of Alzheimer’s Disease. J Neurosci 31:6587–6594. doi:10.1523/JNEUROSCI.0529
Acknowledgments
We thank Shun Ming Yuen from Histopathology Core (Faculty of Health Sciences, University of Macau) for assistance in histological analysis and Shaolin Zhang for verifying the purity of linagliptin. We thank the Science and Technology Development Fund, Macao S.A. R (FDCT) (project reference no.: 118/2013/A3) for the financial support.
Authors’ Contribution
JK executed most of the study including dosing, behavioral studies, immunoblotting, histology, data interpretation, and manuscript writing. RMDH supported in analyzing the results and manuscript editing. LG involved in data interpretation. KYT supervised and guided all phases of the project, including the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Electronic Supplementary Material
Fig S1
Cognitive assessment in 10 month old control (C57BL/6) and 3xTg-AD female mice in the Morris Water Maze test. (A) Latency to reach the escape platform and (B) path length taken to reach the platform during acquisition trials. (C) Percentage of time spent in the platform quadrant and (D) number of platform crossings during the probe trial. (E) Tracking details on day 4 trial 2 of corresponding groups. Significance was analyzed by unpaired t test (n = 6, mean ± SEM) using Graphpad Prism. **p < 0.01 and ***p < 0.001, compared to control mice (C57BL/6). (TIFF 71729 kb)
Fig S2
Cognitive assessment in 10 month old control (C57BL/6) and 3xTg-AD female mice in the Y-maze test. (A) Time spent in the novel arm and (B) percentage of alterations. Significance was analyzed by unpaired t test (n = 6, mean ± SEM) using Graphpad Prism. ***p < 0.001, compared with control mice (C57BL/6). (TIFF 39998 kb)
Rights and permissions
About this article
Cite this article
Kosaraju, J., Holsinger, R.M.D., Guo, L. et al. Linagliptin, a Dipeptidyl Peptidase-4 Inhibitor, Mitigates Cognitive Deficits and Pathology in the 3xTg-AD Mouse Model of Alzheimer’s Disease. Mol Neurobiol 54, 6074–6084 (2017). https://doi.org/10.1007/s12035-016-0125-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-016-0125-7