Abstract
Recent studies reported granulocyte colony-stimulating factor (G-CSF) treatment can improve the cognitive function of Alzheimer’s disease (AD) mice, and the mobilized hematopoietic stem cells (HSCs) or bone marrow mesenchymal stem cells (BM-MSCs) are proposed to be involved in this recovery effect. However, the exact role of mobilized HSC/BM-MSC in G-CSF-based therapeutic effects is still unknown. Here, we report that C-X-C chemokine receptor type 4 (CXCR4)/stromal cell-derived factor 1 (SDF-1) chemotaxis was a key mediator in G-CSF-based therapeutic effects, which was involved in the recruitment of repair-competent cells. Furthermore, we found both mobilized HSCs and BM-MSCs were able to infiltrate into the brain, but only BM-MSCs replenished the neural lineage cells and contributed to neurogenesis in the brains of AD mice. Together, our data show that mobilized BM-MSCs are involved in the replenishment of neural lineages following G-CSF treatment via CXCR4/SDF-1 chemotaxis and further support the potential use of BM-MSCs for further autogenically therapeutic applications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is the most common type of dementia, which causes widespread synaptic and neuronal loss leading to the impairment of learning and memory. Deposition of amyloid-β (Aβ) plaque and neurofibrillary tangles are the pathological hallmarks of AD, and several articles have suggested that Aβ is a pivotal instigator [1, 2]. Despite extensive studies focusing on pathological mechanisms and therapeutic strategies, there are currently no treatments that can cure AD.
Stem cell-based therapy is proposed as a potential strategy for treating AD through the reconstitution of impaired neurons or synapses. However, there are obstacles for autogenic applications, even with the discovery of a source of therapeutic, committed stem cells. Previous studies had reported the efficacy of allogenic transplantation of stem cells for the recovery of cognitive function in AD mice [3–5], but the risks of transplant rejection or transplant-induced disruption in tissues are concerning.
Recent studies have suggested that bone marrow (BM) cells may serve as a reservoir of stem cells useful for tissue regeneration [6, 7]. BM-derived stem cells consist of hematopoietic stem cells (HSCs), BM stromal cells (BMSCs, also known as BM mesenchymal stem cells, BM-MSCs), and endothelial progenitor cells (EPCs). They have been generally shown to replenish the blood, muscle, liver, and the vascular endothelium [8]. BM-MSCs were reported to have neural differentiation potency [9], but their commitment for the replenishment of neural lineage cells in the brain is still not well defined [10].
Granulocyte colony-stimulating factor (G-CSF) is a potent hematopoietic factor that can stimulate BM to produce granulocytes and hematopoietic stem cells, mobilizing them into the bloodstream to replenish lymphoid and myeloid lineages [11, 12], thus G-CSF is used to accelerate the recovery of patients with neutropenia [13] or to increase the number of HSCs in the blood of the donor before transplantation [11]. Furthermore, several articles reported that the therapeutic potential of G-CSF in the CNS may ameliorate the neurological disorders including stroke [14], spinal cord injury [15], amyotrophic lateral sclerosis [16], and Alzheimer’s disease [17, 18] through the mobilization of HSCs and direct neurotrophic effects [19, 20]. Nevertheless, the competence of mobilizing HSCs and their contribution to the compensation of neural lineages are still not known. On the other hand, G-CSF may also mobilize BM-MSCs and appear capable of replenishing the myocardium [21], but whether they can infiltrate into brain and replenish neural lineages is still an open question. Given an impaired capacity for neuronal homeostasis may lead to cognitive decline [22], the understanding of the fate of G-CSF-mobilized BM cells and their further implications may be an important issue for AD or other neurological disorders.
Despite the BM-derived stem cells’ potential to be mobilized into peripheral blood, guiding these therapeutic and committed cells to injured target regions for achieving the therapeutic purpose is still problematic. Chemoattraction is important for stem cells involved in organogenesis during development as well as tissue homeostasis throughout adulthood [23]. Several lines of study show that C-X-C chemokine receptor type 4 (CXCR4)/stromal cell-derived factor 1 (SDF-1) chemotaxis tightly modulates the migration and homing of stem cells in the developmental process [24] and diseased conditions [25, 26], and HSCs and BM-MSCs are also involved in this manner [27–29]. Furthermore, in AD, the synergistic effects of G-CSF-induced HSC mobilization combined with SDF-1 intracerebral injection were observed to guide the migration of mobilized HSCs into the brain; this phenomenon underlies the critical role of CXCR4/SDF-1 chemotaxis in the G-CSF-mediated therapeutic effects in AD [18].
We had reported that G-CSF rescues the cognitive impairment of AD mice by increasing their neurogenesis [17], and the role of G-CSF-mobilized HSCs in the modulation of inflammation and the importance of CXCR4/SDF-1 chemotaxis in stem cell homing was also identified [18]. Here, we investigate whether G-CSF-mobilized HSCs or BM-MSCs can target the injured brain and replenish the neural lineages through CXCR4/SDF-1 chemotaxis, aiming not only to characterize the role of CXCR4/SDF-1 chemotaxis in the migration of G-CSF-mobilized BM cells but also to determine the competence of them for the replenishment of neural lineages in the AD brain.
Materials and Methods
AD Mouse Models
Mice were housed in a 12-/12-h light/dark cycle with food and water provided ad libitum in accordance with the guideline of Animal Facility of the Institute of Molecular Biology (IMB), Academia Sinica, Taiwan. Two different mouse models of AD were generated and/or bred for testing the effects of G-CSF therapy. In the transgenic mouse model, Tg2576 mice with the mutated APPswe transgene were purchased from Taconic (Germantown, NY). The acute Aβ-induced model was generated according to a previously described protocol [30, 31]. Eight-week-old C57BL/6 male mice were purchased from the National Laboratorial Animal Center and bred at the Animal Facility of the Institute of Molecular Biology (IMB) as above. The 42 kD of beta-amyloid (Aβ42) solution (500 μM) was prepared from soluble Aβ42 (Sigma-Aldrich) in 0.01 M PBS, pH 7.4. The solution was incubated at 37 °C for 3 days to form the aggregated Aβ42 and stored at −70 °C. Animals were intraperitoneally anesthetized with 40 mg/kg sodium pentobarbital, and the injection of aggregated Aβ was made bilaterally into the dorsal hippocampus using a 33-gauge needle connected to a microsyringe (Hamilton). The animals were subjected to stereotaxic surgery with the incisor bar set at the following coordinates: 2 mm posterior to the bregma, 2.1 mm bilateral to the midline, and 1.8 mm ventral to the skull surface. An injection of aggregated Aβ (1 μL) or PBS (1 μL) was given, and a 7-day period was allowed for AD symptoms to develop in the subjects.
Experimental Procedure, Drug Treatments, and Bromodeoxyuridine (BrdU) Labeling
Experimental design for the drug treatments used in the AD mouse model is shown in Fig. 2a. The Tg2576 mice (12 months old) were divided into six groups, and four of these groups were injected subcutaneously with recombinant human G-CSF (Sigma G0407) 50 μg/kg once daily for five consecutive days. The other groups (control animal of non-Tg and Tg mice) were injected with PBS in parallel. After 3 days of G-CSF injection, three of the G-CSF-injected groups were additionally injected with CXCR4 antibody (Ab) (2.5 mg/kg intraperitoneally; R&D MAB21651) once daily for 2 days, SDF-1 Ab (2.5 mg/kg intraperitoneally; R&D MAB310) once daily for 2 days, and AMD3100 (5 mg/kg, Sigma A5602) twice daily for 2 days [14, 32], respectively. A cumulative labeling method was used to examine the proliferating cell populations, with the mice receiving daily injections of BrdU (50 mg/kg) intraperitoneally for 14 consecutive days, starting on the first day of the G-CSF injection. The BrdU+ cells in both hemispheres of the hippocampus and cortex were counted digitally with the use of a ×20 objective lens (Carl Zeiss LSM510) via a computer imaging analysis system (Imaging Research). For each animal, 40 coronal sections (15 μm thick) throughout the hippocampus and cortex were analyzed.
Culture, Cell Reconstitution, and Static Injection of BM Stem Cells
The BM cells, BM-derived HSCs, and BM-MSCs were isolated from age-matched green fluorescent protein (GFP)-expressing transgenic mice with APPswe −/GFP + genetic background and cultured as described in previous reports [33–35]. The HSCs were cultured from the BM by utilizing an HSC enrichment set (BD Pharmingen) and cultured on OP9 cells as a feeder layer in Iscoves’s modified Dulbecco’s medium (IMDM) (Invitrogen) supplemented with 10 % fetal bovine serum (FBS), 20 ng/mL stem cell factor (Peprotech), 20 ng/mL thrombopoietin (Peprotech), and 20 ng/mL Flt3-Ligand (Peprotech). The characteristics of cultured HSCs were determined by flow cytometry (BD, FACSCalibur) following immunocytochemistry staining of Sca-1, CD45 (R&D system, FMC003), and CD34 (Biolegend, 119320). For culture of BM-MSCs, in brief, mice were sacrificed and the tibias and femurs were dissected out. The marrow was then washed out with 8 mL of minimum essential medium-α (αMEM; Gibco) and cultured in αMEM supplemented with 20 % FBS, 2 mM l-glutamine, and 100 mg/mL kanamycin, incubated at 37 °C, in 95 % O2 and 5 % CO2. After 48 h, the non-adherent cells were removed by replacing the medium. BM-MSCs were subcultured four times before the following experiments. The BM-MSCs expressing markers were detected by flow cytometry following immunocytochemistry staining of CD29, Sca-1, CD45 (R&D system, FMC003), CD34 (Biolegend, 119320), and CD44 (BD, 550538). For reconstitution of GFP expressing BM cells, HSCs, and BM-MSCs in Tg2576 mice, we followed and modified the protocol from the previous study [36]. Briefly, a total of 6 × 106 of BM cells, BM-HSCs, or BM-MSCs were transplanted intravenously into Tg2576 mice (12 months old) that had been lethally irradiated (10 Gy). To mobilize the reconstituted and settled GFP cells, G-CSF was injected at 5 days after cell reconstitution. For radioprotection [21], each irradiated mouse was simultaneously transplanted with 2 × 105 whole BM cells from B6 mice that did not carry the GFP transgene. The BM-MSC transplantation into cortex was performed with a static apparatus as in a previous study [37].
Behavioral Measurements
Utilizing the Morris water maze (MWM) learning task, animals were subjected to four trials per session and two sessions a day, with one session given in the morning and the other given in the afternoon [38]. For a complete test, a total of six sessions in 3 days were given and performed in a blind manner. In each session, the animals were placed at four different starting positions equally spaced around the perimeter of the pool in a random order. They were allowed to find the platform in 120 s. If an animal could not find the platform in 120 s, it was guided to the platform. After arriving at the platform, the animals were allowed to stay there for 20 s. The time spent by individual mice in reaching the platform was recorded as the escape latency.
In Vitro Migration Assay and SDF-1 ELISA
Migration assays were followed as previous performed with modification [39]. The chemoattractive microenvironment of SDF-1 was generated in the bottom layer of a Transwell plate. Before the migration assay, neural stem cells (2 × 105) were seeded onto the bottom of 24-well plates and were induced to neural differentiation for 7 days with DMEM/F12 medium (Gibco, 12400-024) with 1 % N2 supplement (Gibco, 17502-048), generating neural cells containing neurons and astrocytes. These differentiated cells were then treated with 10 μM Aβ42 for 5 days to mimic the microenvironment of the AD brain. Part of medium was collected for determining the level of SDF-1 by ELISA (R&D Systems, DY460). In the upper layer of the Transwell membrane (Millicell culture inserts; Millipore, cat. no. RIEP12R48). BM-MSCs were detached with trypsin-EDTA, counted, and resuspended in αMEM for a 24-h serum-free starvation period, while the AD-mimicking microenvironment was applied to the lower layer. In migration assay, the serum-starved BM-MSCs (1 × 105 in 100 μl) were then plated onto the upper layer of the Transwell membrane in the 24-well plates. Cells were allowed to migrate through the Transwell membrane for 24 h. The Transwell membranes were then washed with PBS, and the non-migrating cells on the upper side of membrane were removed with a cotton swab. Migrating cells were fixed with 4 % paraformaldehyde, stained with 4′,6-diamidino-2-phenylindole (DAPI), photographed, and counted.
Immunohistochemistry
Mouse brain sections were processed to recover antigen with boiled citrate buffer (pH 6.0) for 20 min and then treated with PBS containing 5 % normal donkey serum and 0.5 % Triton X-100 for 1 h. In the same buffer solution, the sections were incubated overnight in primary antibodies at 4 °C and hybridized on the next day with Alexa 488, 555, or 568 secondary antibodies (Invitrogen) for 1 h at room temperature. To detect neurogenesis, chemoattraction, and the fate of BM-MSCs, the primary antibodies used were as follows: anti-SDF-1 (Santa Cruz, sc-6193), anti-CXCR4 (Abcam, Ab2074-100), anti-BrdU (Abcam, AB6326), anti-CD44 (Millipore, MABF425), anti-NeuN (Millipore, MAB377), anti-GFAP (Chemicon, MAB3402), anti-DCX (Chemicon, AB5910), anti-Olig2 (Millipore, AB9610), and anti-GFP (Millipore, MAB3080 and MAB3580). Quantification of cells expressing CXCR4 and the SDF-1 expressional intensity was carried out using images from the immunofluorescent (IF) staining experiment, acquired from induced AD mice and Tg2576 mice. The value of each mouse was acquired from five random views of the cortex and the hippocampus in one section; total nine sections within dorsal to ventral cortex or hippocampus were evaluated per mouse. The number of CXCR4-positive cells and the intensity of the SDF-1 staining were analyzed by ImageJ software in a blinded manner. Cavalieri’s principle was used in the quantification of BrdU and NeuN-positive cell numbers. The number of BrdU and NeuN double-positive cells was counted in subgranular zone of dentate gyrus, and five random views of the hippocampus in one section were evaluated; total nine sections were evaluated per mouse in a blinded manner. The GFP-positive cell numbers of infiltrated cells were acquired by TissueFAXS and analyzed by TissueQuest (TissueGnostics) as previously described [40]. Stereological evaluations of the hippocampus of each experimental mouse were conducted on every 12th section throughout the hippocampus that contained GFP signals following the Cavalieri principle. The flow cytometry-like data (dot plot) were acquired by TissueQuest, with each dot of the plot representing two specific kinds of immunoreactive intensity from a single cell. The plot accumulated the values of all cells from a region of interest, and then the positive signal number could be identified by gating the immunoreactive intensity.
Statistical Analysis
All data were normally distributed and are presented as means ± SEM. In case of single mean comparisons, data were analyzed by Student’s t tests. For multiple mean comparisons, data were analyzed by ANOVA with Tukey’s post hoc test using the statistical software (Prism 4.0; GraphPad). Correlation analysis was also performed using this statistical software. Statistical significance was set at p < 0.05.
Results
Elevated Expression of SDF-1 in the Brain of AD Mice
Chemokines are involved in inflammatory cell recruitment in the maintenance of CNS homeostasis [41]. Of these chemokine effects, CXCR4/SDF-1 chemotaxis is identified that plays an important role in the regulation of stem/progenitor cell migration in stroke [26, 42] and multiple sclerosis [24]. However in AD, the role of this chemotaxis is still controversial [43, 44]. To evaluate whether the levels of SDF-1 were upregulated by Aβ deposition in the AD brain, we first adopted an induced AD mouse model by static microinjection of Aβ. Seven days after Aβ injection, a significant elevation in SDF-1 expression had occurred in the Aβ-injected regions in contrast to PBS-injected mice that observed by IF staining (Fig. 1a). We further characterized the SDF-1 level in a disease onset transgenic AD mouse model (Fig. 1b) at the age of 12 months (Tg2576, AD-Tg), which expresses the mutated APPswe gene [45]. The quantified result indicated that SDF-1 was consistently upregulated in the brain of AD-Tg mice compared with the wild-type control (Fig. 1c). Furthermore, given previous studies reported that SDF-1 was involved in the anxiety of behavioral abnormalities [46], we thus further evaluated the novel object recognition ability in AD-Tg mice (n = 5 per group; Fig. S1). The data showed AD-Tg mice displayed abnormal exploring behavior, and they were not able to recognize the correct novel object during the test, suggesting the impairment of cognitive function and implying that SDF-1 is involved in behavioral abnormalities.
Aβ deposition-induced SDF-1 elevation recruits CXCR4-positive cells in the AD brain. a IF staining of SDF-1 in Aβ-induced AD mice. Arrow points to the Aβ injection site in Aβ-induced AD mice. Bar, 50 μm. b IF staining of SDF-1 in Tg2576 (AD-Tg) mice. Bar, 50 μm. c Quantified data indicates the intensity of SDF-1 in AD-Tg mice (n = 5 per group; data are presented in fold; *p < 0.05 by unpaired t test). d Astrocytes and microglia migration associated with the expression of SDF-1 observed by IF staining of SDF-1 and GFAP or Iba1 in AD-Tg mice. CA1, hippocampal CA1 layer. Bar, 50 μm. e Upper panel: IF staining of SDF-1 and CXCR4 in induced AD and AD-Tg mice. The accumulation of CXCR4-positive cells was highly associated with the expression of SDF-1 in both AD mouse models. Bar, 100 μm. Lower panel: Higher power photographs of the staining shown in the white square in the upper panel present respective immunoreactivity. Bar, 50 μm. f, g IF staining of SDF-1 and CXCR4 in confocal-based data in G-CSF-treated AD-Tg mice. g Immunoreactivity of SDF-1 located around CXCR4-expressing cells in the characterization of orthogonal view using confocal microscopy. Bar, 25 μm. h The SDF-1 immunoreactivity in the subregion of cell was further characterized by confocal 1D graph. i Pearson correlation analysis of SDF-1 expression and the number of CXCR4-positive cells. The expression of SDF-1 correlated with the number of CXCR4-positive cells in each view (induced AD mice, n = 3; AD-Tg mice, n = 3; ***p < 0.0001 by unpaired t test)
In addition, using IF staining of SDF-1 and GFAP or Iba1, we found higher immunoreactivities of SDF-1, GFAP, and Iba1 in the brains of AD-Tg mice. The immunoreactivity of SDF-1 was mainly expressed in extracellular, and its distribution was associated with the immunoreactivity of GFAP and Iba1 in the hippocampi of AD-Tg mice (Fig. 1d), suggesting that an elevated inflammatory response exists in the AD-Tg brain, and astrocytes as well as microglia cells are involved in the deposition of the SDF-1.
Migration of CXCR4-Expressing Cells Correlates with SDF-1 Level in the AD-Tg Brain
In disease conditions, previous studies reported that CXCR4/SDF-1-mediated cell migration is highly associated with tissue repair [47, 48]. We thus examined whether CXCR4-expressing cells are involved in tissue regeneration in the AD-Tg brain. By IF staining of SDF-1 and CXCR4, the data indicated that the distributions of CXCR4-expressing cells were highly associated with the expression of SDF-1 in the both AD models, and a part of the immunoreactivities of both SDF-1 and CXCR4 was co-localized (Fig. 1e). We further confirmed the immunoreactivity of SDF-1 located around the cell surface and co-localized with its receptor CXCR4 by confocal microscopy (Fig. 1f, g). In addition, the specific interaction between CXCR4 and SDF-1 was characterized rounding the cell surface in confocal 1D projection (Fig. 1h). Further evaluation for the correlation between the number of CXCR4-expressing cells and the immunoreactive intensity of SDF-1 showed that the level of SDF-1 was correlated with the number of CXCR4-positive migrated cells (Fig. 1i), suggesting that CXCR4/SDF-1 chemotaxis is a key mediator for repair-competent cells homing to the brain in AD mice.
CXCR4/SDF-1 Chemotaxis Involvement in the G-CSF-Based Amelioration of Cognitive Function
Despite the therapeutic potential of G-CSF reported for amelioration of cognitive dysfunction in AD mice, its exact therapeutic mechanism is still controversial, with both trophic effects and cell replacement being suggested. Given elevated CXCR4/SDF-1 interactions that exist in our AD mouse models, we evaluated whether the G-CSF-mobilized HSCs/BM-MSCs replenish the damaged neural cells in the AD-Tg brain through CXCR4/SDF-1 chemotaxis. A 5-day course of G-CSF treatment was carried out in disease onset of AD-Tg mice at age 12 months to mobilize BM-derived stem cells and accompanied intraperitoneal (i.p.) injection of CXCR4 antibody (Ab), AMD3100, and SDF-1 Ab on the last 2 days of G-CSF treatment, each respectively, to block the CXCR4/SDF-1 chemotaxis in vivo (Fig. 2a). By using the MWM task, we found that non-Tg mice with vehicle injection were able to learn and remember the platform position in the water maze; thus, their escape latency was rapidly decreased within the training sessions. However, the AD-Tg mice were impaired to acquire the platform revealing the deficits of learning/memory. Importantly, G-CSF treatment rescued the spatial memory of AD-Tg mice with respect to the escape latency. However, this amelioration was inhibited following blockade of CXCR4 and SDF-1 in vivo (Fig. 2b), suggesting that BM-derived stem cells are potentially involved in this therapeutic effect of CXCR4/SDF-1 chemotaxis.
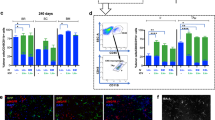
CXCR4/SDF-1 chemotaxis is involved in G-CSF-mediated amelioration of cognitive impairment. a Timeline of experimental procedures for G-CSF treatments and the administration of inhibitors of CXCR4/SDF-1 chemotaxis. AD-Tg mice were injected subcutaneously with PBS or 50 μg/kg of G-CSF once daily for 5 days. At the fourth and fifth days of the PBS or G-CSF injection course, CXCR4 Ab or AMD3100 was given to block CXCR4/SDF-1 chemotaxis. Finally, mice were subjected to the MWM test on day 28. b G-CSF treatment improved the cognitive impairment of AD-Tg mice, but the mice with CXCR4 blockade after treatment with CXCR4 Ab or AMD3100 displayed an inability to recover their cognitive function in MWM task (n = 6 for each group, ***p < 0.001 by one-way ANOVA)
Mobilized BM Cells Infiltrate into the Brain and Express CXCR4
To investigate whether the commitment of BM cells is involved in the replenishment of neural lineages in the AD brain following G-CSF treatment, we reconstituted GFP expressing BM cells in irradiated AD-Tg mice and accompanied with a 5-day course of G-CSF treatment (Fig. 3a). Two weeks following BM cell reconstitution and G-CSF treatment, we evaluated the efficiency of G-CSF-induced BM cell infiltration into the hippocampal region by counting the GFP cell number in the IF-stained sections. The data showed G-CSF treatment significantly improved the infiltration efficiency of BM cells in the hippocampus (Fig. 3b; n = 3 per group) and the reconstituted BM cells were capable of infiltrating into the cortex and hippocampus of the AD-Tg brain. The distribution of the BM cells revealed a major population located in the dentate gyrus as well as neared the central and lateral ventricles (Fig. 3c), implying that a part of BM cells can infiltrate into the brain from the ventricles. The reconstituted BM cells were also immunoreactive to CXCR4 in the hippocampus and cortex (Fig. 3d), showing their potential of homing in BM and migration by SDF-1 chemoattraction. Furthermore, the infiltrated BM cells expressed CD34 and CD44 at 2 weeks following transplantation (Fig. 3e, f), suggesting mobilized BM cells with the characteristic of HSCs and BM-MSCs after reconstitution in AD-Tg mice.
Reconstituted BM cells infiltrate into the brain and express CXCR4 in AD-Tg mice. a Timeline of procedures for the reconstitution of GFP expressing BM cells and G-CSF treatment. Five days after AD-Tg, mice were subjected to lethal irradiation (10 Gy), and GFP expressing BM cells were transplanted into the irradiated mice by intravenous injection. A 5-day course of G-CSF treatment was started at the fifth day after BM cell transplantation. The mice were sacrificed for analysis of IF staining at 2 weeks after G-CSF treatment. b Quantification for the infiltrated BM cell number in the hippocampus of AD-Tg mice with or without G-CSF treatment (n = 3 per group; data are presented as mean ± SEM; **p < 0.01 by unpaired t test). c The reconstituted BM cells (arrows) were mobilized by G-CSF treatment, infiltrated into the brain, and were identified in the cortex and hippocampus. Bar, 50 μm. d Upper panels: IF staining of GFP and CXCR4. Reconstituted BM cells were competent for migration to the hippocampus (left) and the cortex (right) with immunoreactivity of CXCR4. Bar, 100 μm. Lower panels: Higher power photographs of the staining shown in the white square in the upper panel present respective immunoreactivity. Bar, 50 μm. e, f Mobilized BM cells were immunopositive for CD34 and CD44 following reconstitution. Bar, 50 μm
Mobilized HSCs Infiltrate into the Brain with No Evidence of Involvement in Neurogenesis
Subsequently, we attempted to characterize which type of BM-derived cells may replenish the neural lineages following G-CSF treatment. As previously study reported that microglia derived from mobilized HSCs are involved in the G-CSF-based therapeutic effects [18], we thus investigated whether G-CSF-mobilized HSCs are involved in neurogenic replenishment in the AD brain. In order to trace the fate of mobilized HSCs in the AD brain, we reconstituted HSCs in irradiated AD-Tg mice using GFP expressing HSCs with CD34+Sca-1+CD45− characters (Fig. S2) via tail vein injection and accompanied with a 5-day course of G-CSF treatment to mobilize the reconstituted HSCs (Fig. 4a). Four weeks after G-CSF treatment, we found much GFP expressing cells distribute in the hippocampus of G-CSF treated AD-Tg mice but not vehicle-treated mice (Fig. 4b; n = 3 per group), suggesting G-CSF is essential for HSC mobilization. Furthermore, IF staining of GFP and Iba-1 indicated that part of the immunoreactivity was co-localized (Fig. 4c), suggesting that the reconstituted HSCs are competent to replenish microglia. However, no direct co-localized immunoreactivity containing both GFP and MAP2 was detected in all experimental mice (n = 5; Fig. 4d). Therefore, we found no evidence showing that HSCs were involved in the replenishment of neurogenic cells in G-CSF-treated AD-Tg mice. Considering BM-MSCs have been reported with the potential for the neural fate [9], we therefore shifted our scope of study to BM-MSCs.
Mobilized HSCs are involved in the replenishment of microglia but not neurons. a Timeline of procedures for the reconstitution of GFP expressing HSCs and G-CSF treatment. The mice were sacrificed for analysis of IF staining at 4 weeks after G-CSF treatment. b Quantification for the infiltrated HSC cell number in the hippocampus of AD-Tg mice with or without G-CSF treatment (n = 3 per group; data are presented as mean ± SEM; *p < 0.05 by unpaired t test). c Upper panel: Four weeks after reconstitution of GFP expressing HSCs and a 5-day course of G-CSF treatment, both immunoreactivities of GFP and Iba-1 were co-localized, suggesting the potential of HSCs to replenish microglia in the AD brain. Bar, 100 μm. Lower panel: Higher power photographs of the staining shown in the white square in upper panel present respective immunoreactivity. Bar, 50 μm. d Upper panel: The immunoreactivity of GFP and MAP2 appeared separate, casting doubt on the competence of mobilized HSCs for neuronal differentiation. Bar, 100 μm. Lower panel: Higher power photographs of the staining shown in the white square in the upper panel present respective immunoreactivity. Bar, 50 μm
Mobilized BM-MSCs Are Involved in Replenishment of Neural Lineages
To characterize whether G-CSF-mobilized BM-MSCs replenish the neural lineages of AD brain, we reconstituted GFP expressing BM-MSCs in AD-Tg mice, mobilized the reconstituted BM-MSCs by G-CSF treatment, and traced the fate of BM-MSCs at 4 weeks after G-CSF treatment (Fig. 5a). Before the reconstitution, GFP expressing BM-MSCs were expanded through their adherence to plastic dishes, and their surface marker characteristics were confirmed by flow cytometry with CD29+Sca-1+CD44+CD45−CD34− phenotypes (Fig. S3). Here, we confirmed again that G-CSF was necessary for mobilizing the BM-MSCs, and AD-Tg mice with G-CSF treatment exhibited significantly more GFP BM-MSC number comparing to vehicle treated mice in the hippocampus (Fig. 5b; n = 3 per group). In addition, by IF staining of GFP and GFAP (Fig. 5c) or Olig2 (Fig. 5d), we found that immunoreactivities of GFP and GFAP as well as GFP and olig2 were partly co-localized, suggesting that mobilized BM-MSCs are involved in the replenishment of astrocytes and oligodendrocytes in the brains of AD-Tg mice.
Mobilized BM-MSCs are involved in the replenishment of neural lineages. a Timeline of procedures for reconstitution with GFP expressing BM-MSCs and G-CSF treatment. b Quantification for the infiltrated BM-MSC cell number in the hippocampus of AD-Tg mice with or without G-CSF treatment (n = 3 per group; data are presented as mean ± SEM. *p < 0.05 by unpaired t test). c, d Upper panels: IF staining of GFP and GFAP as well as GFP and Olig2 showed that astrocytes and oligodendrocytes were derived from mobilized BM-MSCs in G-CSF-treated AD-Tg mice. Bar, 100 μm. Lower panels: Higher power photographs of the staining shown in the white square in upper panel present respective immunoreactivity. Bar, 50 μm. e In IF staining of GFP and NeuN, a part of the immunoreactivity of NeuN was co-localized with the immunoreactivities of GFP. Bar, 100 μm
As neuronal loss is the one of major pathological features of AD, appearing highly correlated with the pathogenesis of cognitive impairment, we therefore evaluated if BM-MSCs can contribute to neurogenesis in the AD-Tg brain at 4 weeks after reconstitution. By tracing the reconstituted BM-MSCs, we surprisingly found that part of mobilized BM-MSCs is immunoreactive to NeuN (Fig. 5e), suggesting they have the potential to replenish neurons in the AD-Tg brain following G-CSF treatment.
To further confirm the potentially neural fate of BM-MSCs following mobilization, we directly transplanted these BM-MSCs into the cortex of AD-Tg mice by stereotactic injection. Four weeks after transplantation, IF staining of GFP and MAP2 indicated that engrafted BM-MSCs were potentially capable to express neuronal dendritic marker (Fig. S4a). Moreover, IF staining of GFP and GFAP also showed the BM-MSCs might also commit to express astrocytic marker (Fig. S4b). These data provide insights into the potential of mobilized BM-MSCs for replenishment of neural lineages in G-CSF-treated AD-Tg mice.
In Vitro SDF-1 Recruits BM-MSC Migration by CXCR4/SDF-1 Chemotaxis
To characterize the repair competence of BM-MSCs following G-CSF treatment, we further adopted a Transwell assay to evaluate whether the mobilized BM-MSCs are recruited by SDF-1 chemoattraction (Fig. 6a). We first determined whether the SDF-1 level of co-cultured astrocytes and neurons is upregulated responding to Aβ treatment (Fig. 6b). The ELISA-based data showed that Aβ significantly induced the upregulation of SDF-1 in the culture medium (n = 5 independent experiments; Fig. 6c), a consistent result with our AD-Tg mice (Fig. 1a). We thus further investigated whether SDF-1/CXCR4 is involved in the homing and migration of BM-MSCs by in vitro Transwell assay. To mimic the microenvironment of the AD brain, we treated Aβ into the medium of co-cultured cells in the bottom layer of well for 5 days, and the Transwell insert was added into the well for 1 day to evaluate the BM-MSC migration. Following migration for 24 h, the nuclei of the migrated CD44+ BM-MSCs from the series of groups were labeled by DAPI staining, then photographed and analyzed by microscopy (Fig. 6d). The quantified data showed that BM-MSCs were not responding to vehicle or pure medium with Aβ, but they were significantly recruited by Aβ-treated co-cultured cell medium, and this outcome was inhibited while CXCR4 was blocked by CXCR4 antibody (Fig. 6e). Together, this data reveals that the migration of BM-MSCs is dependent on CXCR4/SDF-1 chemotaxis.
In vitro Aβ-induced SDF-1 upregulation recruits BM-MSCs via CXCR4/SDF-1 chemotaxis. a Experimental design of the Transwell assay. In the bottom layer of each well, neural cells including astrocytes and neurons were derived from primary cultured neural stem cells (NSCs) and were treated with Aβ to generate SDF-1-conditioned media, which was then collected for ELISA. In the upper compartment of the Transwell, the cultured BM-MSCs were seeded for testing chemoattraction. b Immunocytochemistry of GFAP and MAP2 in cultured neural cells on the bottom layer. c SDF-1 ELISA indicates that Aβ treatment can induce SDF-1 upregulation in the medium of the astrocyte-neuron co-culture (n = 5 independent experiments. Data are represented as mean ± SEM. *p < 0.05 by unpaired t test). d BM-MSCs on the Transwell membrane were immunopositive for CD44 (left top image). Migration of BM-MSCs was recognized with DAPI staining and cells were counted. Bar, 50 μm. e Quantified data indicates that the medium of Aβ-treated neural cells can recruit BM-MSCs; CXCR4 Ab pre-treatment of BM-MSCs inhibits the migration. Mouse IgG treatment was used as an internal control. (BM-MSCs → vehicle: MSC migration toward PBS-treated neural cells; BM-MSCs → Aβ: MSC migration toward Aβ only medium; BM-MSCs → Aβ-NCs: MSC migration toward Aβ-treated neural cells; CXCR4-BM-MSCs → Aβ-NCs: MSCs pretreated with CXCR4 Ab and their migration toward Aβ-treated neural cells; IgG-BM-MSCs → Aβ-NCs: MSC pretreated with mouse IgG and their migration toward Aβ-treated cells (n = 6 independent experiments; data are presented as mean ± SEM. **p < 0.01, ***p < 0.001 by one-way ANOVA)
Mobilized BM-MSC-mediated Neurogenesis Is Reduced while Blocking CXCR4/SDF-1 Chemotaxis
We subsequently investigated whether CXCR4/SDF-1 chemotaxis is involved in neurogenesis in the AD-Tg brain following G-CSF treatment. BrdU labeling was employed to identify the newly proliferating cells, and additional CXCR4 Ab and AMD3100 were i.p. injected to block CXCR4/SDF-1 chemotaxis in vivo (Fig. 7a). By IF staining of NeuN and BrdU, we found that G-CSF treatment significant improved the neurogenesis of AD-Tg mice relative to PBS-injected mice (Fig. 7b), but this beneficial effect was inhibited in CXCR4 Ab and AMD3100-treated mice (Fig. 7c), suggesting that CXCR4/SDF-1 chemotaxis is an indispensable mediator for neurogenesis in the brain of AD-Tg mouse.
Blockade of CXCR4/SDF-1 chemotaxis inhibits neurogenesis in G-CSF-treated AD-Tg mice. a Experimental schedule for the treatment of AD-Tg mice with G-CSF and CXCR4 Ab or AMD3100. BrdU was used to label newly proliferating cells for 14 days starting from the first day of G-CSF treatment. b IF staining of NeuN and BrdU was performed 4 weeks after G-CSF treatment. Bar, 100 μm. c The G-CSF treatment significantly improved neurogenesis in the brain of AD-Tg mice. Furthermore, the G-CSF-mediated neurogenesis was inhibited by blocking the CXCR4/SDF-1 chemotaxis (n = 6 in each group; data are presented as mean ± SEM; *p < 0.05 by one-way ANOVA)
Discussion
In present study, we report elevated SDF-1 levels in the brains of AD mice and that this elevation was correlated with the migration of repair-competent cells (Fig. 1). Furthermore, G-CSF-mobilized repair-competent cells may contribute to the recovery of cognitive function via CXCR4/SDF-1 chemotaxis (Fig. 2). Whereas both mobilized HSCs and BM-MSCs were capable of infiltrating the brain after G-CSF treatment (Fig. 3), only BM-MSCs appeared to be involved in the replenishment of neural lineage cells in AD-Tg mice (Figs. 4 and 5). Our data further indicate that CXCR4/SDF-1 chemotaxis was essential for the migration of G-CSF-mobilized BM-MSCs and was also involved in G-CSF-mediated neurogenesis (Figs. 6 and 7). These findings explain how G-CSF treatment improves the cognition in AD mice, underlining that mobilized BM-MSCs can serve as an autogenic stem cell source for the applications in CNS diseases therapy, while further providing insights into endogenous stem cell-based therapies.
The role of SDF-1 in the brain of AD individuals remains debatable [43, 44], but here we show that SDF-1 levels were increased and correlated with the migration of CXCR4-expressing cells (Fig. 1), suggesting an association between Aβ deposition and astrocyte distribution in the brain of induced AD mice and AD-Tg mice. Therefore, we speculate that the elevation of SDF-1 represents an endogenous self-repair mechanism in the AD-Tg brain that facilitates the homing of repair-competent cells to the injured region of brain for tissue regeneration. Accordingly, further mobilization of BM-MSCs into bloodstream by G-CSF treatment may promote more repair-competent cells to take part in this ameliorating mechanism. Interestingly, the data with a blockade of the CXCR4/SDF-1 chemotaxis show the G-CSF-based therapeutic potential was reduced, suggesting that the chemoattraction axis is an indispensable mediator for mobilized cells targeting damaged regions. These findings support that elevated SDF-1 is involved in tissue regeneration of AD brain and CXCR4/SDF-1 chemotaxis plays an essential role in cognitive improvement.
In the present study, we extend the knowledge of G-CSF-mediated therapeutic effects in AD that involves the mobilization of repair-competent cell in addition to trophic effects. Of these cells, mobilized BM-MSCs are indispensible for the replenishment of neural lineage cells. Regarding BM-MSC transdifferentiation into neural lineages, numerous studies reported that BM-MSCs have the potential of neural fate determination. For instance, BM-MSCs are identified to express a basal level of neural genes [9, 10], and they may be heterogeneous, with a subpopulation originating from neurocrest [49, 50] or consisting of early embryonic-like stem cells [51]. Therefore, they can potentially migrate and express neural markers after transplantation [37, 52] and further be induced to differentiate into specific types of neurons by additional gene engineering [53, 54].
Here, our data demonstrated that the G-CSF-mobilized BM-MSCs could contribute in neurogenesis in the AD-Tg brain; this finding opens another window for the application of endogenous stem cells and also provides evidence that G-CSF treatment is efficient for mobilizing BM-MSCs as repair-competent cells for neural lineage replenishment. Although G-CSF has already been used for decades, as in the case of ALS and multiple sclerosis, it has further been tested in clinical trials [55, 56]. Therefore, the safety and reliability of G-CSF should allow the easy transfer to a clinical study for AD.
Although this study focused on the commitment of mobilized BM-MSCs for the replenishment of neural cells following G-CSF treatment, the ameliorating effects on cognitive impairment may not be solely attributed to these cells. The additional effects of G-CSF treatment for the AD brain may also include the mobilization of HSCs for the modulation of inflammatory responses [18] and the presence of endothelial progenitors for neovascularization [57]. Furthermore, several studies reported BM cell fusion with host cells after transplantation into various kinds of organs or co-culturing with donor cells [58–60]. For this reason, cell fusion has recently been proposed as an explanation for stem cell plasticity. Interestedly, cell fusion was reported with benefits for the recipient’s cells, including amelioration of cell apoptosis [61] as well as tissue protection through mitochondria transfer [62]. Here, we may not exclude that part of the newly generated neural cells is derived from cell fusion, and we further postulate that cell fusion mediated tissue protection may be also involved in the therapeutic effects of G-CSF-mobilized BM-MSCs.
Autologous cell therapy has high potential for neurological disorders, and G-CSF-mobilized BM-MSCs can be a practicable cell source in this strategy. In vivo, the mobilized BM-MSC may directly contribute to tissue regeneration. Ex vivo, these mobilized BM-MSCs may be isolated from peripheral blood and processed through expansion of cell numbers and gene modification, and they have the potential to be developed for the therapeutic purposes of ex vivo gene therapy [63, 64]. In light of autologous application for treatment of neurological disorders, BM-MSC-based cell reprogramming is a promising approach. For instance, by knocking out the RE1 silencing factor or overexpressing LMX1a, MSCs can be induced to differentiate into dopaminergic neurons with electrophysiological characteristics [53, 54], and by overexpressing neurogenin 1, MSCs can be programmed to a neural cell fate, ultimately expressing voltage-gated channels [65].
Conclusion
Collectively, in present study, we identified that elevated SDF-1 was essential for the recruitment of repair-competent cells via CXCR4/SDF-1 chemotaxis in the AD brain, and G-CSF-mobilized BM-MSCs, but not HSCs, played the essential role in replenishment of neural lineages. These findings provide insights into the therapeutic mechanisms of G-CSF treatment in AD and underline that BM-MSCs may act as an autologous cell resource for developing treatments of neurological disorders.
Reference
Hardy J, Selkoe DJ (2002) The amyloid hypothesis of Alzheimer’s disease: progress and problems on the road to therapeutics. Science 297:353–356
Benilova I, Karran E, De Strooper B (2012) The toxic Abeta oligomer and Alzheimer’s disease: an emperor in need of clothes. Nat Neurosci 15:349–357
Blurton-Jones M, Kitazawa M, Martinez-Coria H, Castello NA, Muller FJ, Loring JF, Yamasaki TR, Poon WW et al (2009) Neural stem cells improve cognition via BDNF in a transgenic model of Alzheimer disease. Proc Natl Acad Sci U S A 106:13594–13599
Nivet E, Vignes M, Girard SD, Pierrisnard C, Baril N, Deveze A, Magnan J, Lante F et al (2011) Engraftment of human nasal olfactory stem cells restores neuroplasticity in mice with hippocampal lesions. J Clin Invest 121:2808–2820
Lee JK, Jin HK, Endo S, Schuchman EH, Carter JE, Bae JS (2010) Intracerebral transplantation of bone marrow-derived mesenchymal stem cells reduces amyloid-beta deposition and rescues memory deficits in Alzheimer’s disease mice by modulation of immune responses. Stem Cells 28:329–343
Weissman IL, Anderson DJ, Gage F (2001) Stem and progenitor cells: origins, phenotypes, lineage commitments, and transdifferentiations. Annu Rev Cell Dev Biol 17:387–403
Poulsom R, Alison MR, Forbes SJ, Wright NA (2002) Adult stem cell plasticity. J Pathol 197:441–456
Blau HM, Brazelton TR, Weimann JM (2001) The evolving concept of a stem cell: entity or function? Cell 105:829–841
Blondheim NR, Levy YS, Ben-Zur T, Burshtein A, Cherlow T, Kan I, Barzilai R, Bahat-Stromza M et al (2006) Human mesenchymal stem cells express neural genes, suggesting a neural predisposition. Stem Cells Dev 15:141–164
Montzka K, Lassonczyk N, Tschoke B, Neuss S, Fuhrmann T, Franzen R, Smeets R, Brook GA et al (2009) Neural differentiation potential of human bone marrow-derived mesenchymal stromal cells: misleading marker gene expression. BMC Neurosci 10
Kondo M, Wagers AJ, Manz MG, Prohaska SS, Scherer DC, Beilhack GF, Shizuru JA, Weissman IL (2003) Biology of hematopoietic stem cells and progenitors: implications for clinical application. Annu Rev Immunol 21:759–806
Souza LM, Boone TC, Gabrilove J, Lai PH, Zsebo KM, Murdock DC, Chazin VR, Bruszewski J et al (1986) Recombinant human granulocyte colony-stimulating factor: effects on normal and leukemic myeloid cells. Science 232:61–65
Sheridan WP, Begley CG, Juttner CA, Szer J, To LB, Maher D, McGrath KM, Morstyn G et al (1992) Effect of peripheral-blood progenitor cells mobilised by filgrastim (G-CSF) on platelet recovery after high-dose chemotherapy. Lancet 339:640–644
Shyu WC, Lin SZ, Yang HI, Tzeng YS, Pang CY, Yen PS, Li H (2004) Functional recovery of stroke rats induced by granulocyte colony-stimulating factor-stimulated stem cells. Circulation 110:1847–1854
Koda M, Nishio Y, Kamada T, Someya Y, Okawa A, Mori C, Yoshinaga K, Okada S et al (2007) Granulocyte colony-stimulating factor (G-CSF) mobilizes bone marrow-derived cells into injured spinal cord and promotes functional recovery after compression-induced spinal cord injury in mice. Brain Res 1149:223–231
Pitzer C, Kruger C, Plaas C, Kirsch F, Dittgen T, Muller R, Laage R, Kastner S et al (2008) Granulocyte-colony stimulating factor improves outcome in a mouse model of amyotrophic lateral sclerosis. Brain 131:3335–3347
Tsai KJ, Tsai YC, Shen CK (2007) G-CSF rescues the memory impairment of animal models of Alzheimer’s disease. J Exp Med 204(6):1273–1280
Shin JW, Lee JK, Lee JE, Min WK, Schuchman EH, Jin HK, Bae JS (2011) Combined effects of hematopoietic progenitor cell mobilization from bone marrow by granulocyte colony stimulating factor and AMD3100 and chemotaxis into the brain using stromal cell-derived factor-1alpha in an Alzheimer’s disease mouse model. Stem Cells 29:1075–1089
Diederich K, Sevimli S, Dorr H, Kosters E, Hoppen M, Lewejohann L, Klocke R, Minnerup J et al (2009) The role of granulocyte-colony stimulating factor (G-CSF) in the healthy brain: a characterization of G-CSF-deficient mice. J Neurosci 29:11572–11581
Schneider A, Kruger C, Steigleder T, Weber D, Pitzer C, Laage R, Aronowski J, Maurer MH et al (2005) The hematopoietic factor G-CSF is a neuronal ligand that counteracts programmed cell death and drives neurogenesis. J Clin Invest 115:2083–2098
Kawada H, Fujita J, Kinjo K, Matsuzaki Y, Tsuma M, Miyatake H, Muguruma Y, Tsuboi K et al (2004) Nonhematopoietic mesenchymal stem cells can be mobilized and differentiate into cardiomyocytes after myocardial infarction. Blood 104:3581–3587
Verret L, Jankowsky JL, GM X, Borchelt DR, Rampon C (2007) Alzheimer’s-type amyloidosis in transgenic mice impairs survival of newborn neurons derived from adult hippocampal neurogenesis. J Neurosci 27:6771–6780
Laird DJ, von Andrian UH, Wagers AJ (2008) Stem cell trafficking in tissue development, growth, and disease. Cell 132:612–630
Zou YR, Kottmann AH, Kuroda M, Taniuchi I, Littman DR (1998) Function of the chemokine receptor CXCR4 in haematopoiesis and in cerebellar development. Nature 393:595–599
Carbajal KS, Schaumburg C, Strieter R, Kane J, Lane TE (2010) Migration of engrafted neural stem cells is mediated by CXCL12 signaling through CXCR4 in a viral model of multiple sclerosis. Proc Natl Acad Sci U S A 107:11068–11073
Imitola J, Raddassi K, Park KI, Mueller FJ, Nieto M, Teng YD, Frenkel D, Li J et al (2004) Directed migration of neural stem cells to sites of CNS injury by the stromal cell-derived factor 1alpha/CXC chemokine receptor 4 pathway. Proc Natl Acad Sci U S A 101:18117–18122
Aiuti A, Webb IJ, Bleul C, Springer T, Gutierrez-Ramos JC (1997) The chemokine SDF-1 is a chemoattractant for human CD34+ hematopoietic progenitor cells and provides a new mechanism to explain the mobilization of CD34+ progenitors to peripheral blood. J Exp Med 185:111–120
Shichinohe H, Kuroda S, Yano S, Hida K, Iwasaki Y (2007) Role of SDF-1/CXCR4 system in survival and migration of bone marrow stromal cells after transplantation into mice cerebral infarct. Brain Res 1183:138–147
Petit I, Szyper-Kravitz M, Nagler A, Lahav M, Peled A, Habler L, Ponomaryov T, Taichman RS et al (2002) G-CSF induces stem cell mobilization by decreasing bone marrow SDF-1 and up-regulating CXCR4. Nat Immunol 3:687–694
Stephan A, Laroche S, Davis S (2001) Generation of aggregated beta-amyloid in the rat hippocampus impairs synaptic transmission and plasticity and causes memory deficits. J Neurosci 21:5703–5714
Giulian D, Ingeman JE (1988) Colony-stimulating factors as promoters of ameboid microglia. J Neurosci 8:4707–4717
Stumm RK, Rummel J, Junker V, Culmsee C, Pfeiffer M, Krieglstein J, Hollt V, Schulz S (2002) A dual role for the SDF-1/CXCR4 chemokine receptor system in adult brain: isoform-selective regulation of SDF-1 expression modulates CXCR4-dependent neuronal plasticity and cerebral leukocyte recruitment after focal ischemia. J Neurosci 22:5865–5878
Li P, Huang J, Tian HJ, Huang QY, Jiang CH, Gao YQ (2011) Regulation of bone marrow hematopoietic stem cell is involved in high-altitude erythrocytosis. Exp Hematol 39:37–46
Dezawa M, Kanno H, Hoshino M, Cho H, Matsumoto N, Itokazu Y, Tajima N, Yamada H et al (2004) Specific induction of neuronal cells from bone marrow stromal cells and application for autologous transplantation. J Clin Invest 113:1701–1710
Ishigaki T, Sudo K, Hiroyama T, Miharada K, Ninomiya H, Chiba S, Nagasawa T, Nakamura Y (2009) Human hematopoietic stem cells can survive in vitro for several months. Adv Hematol 2009:936761
Kawada H, Takizawa S, Takanashi T, Morita Y, Fujita J, Fukuda K, Takagi S, Okano H et al (2006) Administration of hematopoietic cytokines in the subacute phase after cerebral infarction is effective for functional recovery facilitating proliferation of intrinsic neural stem/progenitor cells and transition of bone marrow-derived neuronal cells. Circulation 113:701–710
Deng J, Petersen BE, Steindler DA, Jorgensen ML, Laywell ED (2006) Mesenchymal stem cells spontaneously express neural proteins in culture and are neurogenic after transplantation. Stem Cells 24:1054–1064
Tsai KJ, Yang CH, Fang YH, Cho KH, Chien WL, Wang WT, TW W, Lin CP et al (2010) Elevated expression of TDP-43 in the forebrain of mice is sufficient to cause neurological and pathological phenotypes mimicking FTLD-U. J Exp Med 207:1661–1673
Schenk S, Mal N, Finan A, Zhang M, Kiedrowski M, Popovic Z, McCarthy PM, Penn MS (2007) Monocyte chemotactic protein-3 is a myocardial mesenchymal stem cell homing factor. Stem Cells 25:245–251
CC W, Lien CC, Hou WH, Chiang PM, Tsai KJ (2016) Gain of BDNF function in engrafted neural stem cells promotes the therapeutic potential for Alzheimer’s disease. Sci Rep 6:27358
Mennicken F, Maki R, de Souza EB, Quirion R (1999) Chemokines and chemokine receptors in the CNS: a possible role in neuroinflammation and patterning. Trends Pharmacol Sci 20:73–78
Paczkowska E, Kucia M, Koziarska D, Halasa M, Safranow K, Masiuk M, Karbicka A, Nowik M et al (2009) Clinical evidence that very small embryonic-like stem cells are mobilized into peripheral blood in patients after stroke. Stroke 40:1237–1244
Laske C, Stellos K, Eschweiler GW, Leyhe T, Gawaz M (2008) Decreased CXCL12 (SDF-1) plasma levels in early Alzheimer’s disease: a contribution to a deficient hematopoietic brain support? J Alzheimers Dis 15:83–95
Leyhe T, Hoffmann N, Stransky E, Laske C (2009) Increase of SCF plasma concentration during donepezil treatment of patients with early Alzheimer’s disease. Int J Neuropsychopharmacol 12:1319–1326
Hsiao K, Chapman P, Nilsen S, Eckman C, Harigaya Y, Younkin S, Yang F, Cole G (1996) Correlative memory deficits, Abeta elevation, and amyloid plaques in transgenic mice. Science 274:99–102
Oglodek EA, Szota AM, Just MJ, Mos DM, Araszkiewicz A (2015) The MCP-1, CCL-5 and SDF-1 chemokines as pro-inflammatory markers in generalized anxiety disorder and personality disorders. Pharmacol Rep 67:85–89
Wang Y, Deng Y, Zhou GQ (2008) SDF-1alpha/CXCR4-mediated migration of systemically transplanted bone marrow stromal cells towards ischemic brain lesion in a rat model. Brain Res 1195:104–112
Kitaori T, Ito H, Schwarz EM, Tsutsumi R, Yoshitomi H, Oishi S, Nakano M, Fujii N et al (2009) Stromal cell-derived factor 1/CXCR4 signaling is critical for the recruitment of mesenchymal stem cells to the fracture site during skeletal repair in a mouse model. Arthritis Rheum 60:813–823
Morikawa S, Mabuchi Y, Niibe K, Suzuki S, Nagoshi N, Sunabori T, Shimmura S, Nagai Y et al (2009) Development of mesenchymal stem cells partially originate from the neural crest. Biochem Biophys Res Commun 379:1114–1119
Takashima Y, Era T, Nakao K, Kondo S, Kasuga M, Smith AG, Nishikawa S (2007) Neuroepithelial cells supply an initial transient wave of MSC differentiation. Cell 129(7):1377–1388
Ratajczak MZ, Zuba-Surma EK, Machalinski B, Ratajczak J, Kucia M (2008) Very small embryonic-like (VSEL) stem cells: purification from adult organs, characterization, and biological significance. Stem Cell Rev 4:89–99
Kopen GC, Prockop DJ, Phinney DG (1999) Marrow stromal cells migrate throughout forebrain and cerebellum, and they differentiate into astrocytes after injection into neonatal mouse brains. Proc Natl Acad Sci U S A 96:10711–10716
Barzilay R, Ben-Zur T, Bulvik S, Melamed E, Offen D (2009) Lentiviral delivery of LMX1a enhances dopaminergic phenotype in differentiated human bone marrow mesenchymal stem cells. Stem Cells Dev 18:591–601
Trzaska KA, Reddy BY, Munoz JL, Li KY, Ye JH, Rameshwar P (2008) Loss of RE-1 silencing factor in mesenchymal stem cell-derived dopamine progenitors induces functional maturity. Mol Cell Neurosci 39:285–290
Cashman N, Tan LY, Krieger C, Madler B, Mackay A, Mackenzie I, Benny B, Nantel S et al (2008) Pilot study of granulocyte colony stimulating factor (G-CSF)-mobilized peripheral blood stem cells in amyotrophic lateral sclerosis (ALS. Muscle Nerve 37:620–625
Mancardi G, Saccardi R (2008) Autologous haematopoietic stem-cell transplantation in multiple sclerosis. Lancet Neurol 7(7):626–636
Lapidot T, Petit I (2002) Current understanding of stem cell mobilization: the roles of chemokines, proteolytic enzymes, adhesion molecules, cytokines, and stromal cells. Exp Hematol 30:973–981
Alvarez-Dolado M, Pardal R, Garcia-Verdugo JM, Fike JR, Lee HO, Pfeffer K, Lois C, Morrison SJ et al (2003) Fusion of bone-marrow-derived cells with Purkinje neurons, cardiomyocytes and hepatocytes. Nature 425:968–973
Spees JL, Olson SD, Ylostalo J, Lynch PJ, Smith J, Perry A, Peister A, Wang MY et al (2003) Differentiation, cell fusion, and nuclear fusion during ex vivo repair of epithelium by human adult stem cells from bone marrow stroma. Proc Natl Acad Sci U S A 100:2397–2402
Terada N, Hamazaki T, Oka M, Hoki M, Mastalerz DM, Nakano Y, Meyer EM, Morel L et al (2002) Bone marrow cells adopt the phenotype of other cells by spontaneous cell fusion. Nature 416:542–545
Yang WJ, Li SH, Weisel RD, Liu SM, Li RK (2012) Cell fusion contributes to the rescue of apoptotic cardiomyocytes by bone marrow cells. J Cell Mol Med 16:3085–3095
Islam MN, Das SR, Emin MT, Wei M, Sun L, Westphalen K, Rowlands DJ, Quadri SK et al (2012) Mitochondrial transfer from bone-marrow-derived stromal cells to pulmonary alveoli protects against acute lung injury. Nat Med 18:759–765
Kurozumi K, Nakamura K, Tamiya T, Kawano Y, Ishii K, Kobune M, Hirai S, Uchida H et al (2005) Mesenchymal stem cells that produce neurotrophic factors reduce ischemic damage in the rat middle cerebral artery occlusion model. Mol Ther 11:96–104
Kurozumi K, Nakamura K, Tamiya T, Kawano Y, Kobune M, Hirai S, Uchida H, Sasaki K et al (2004) BDNF gene-modified mesenchymal stem cells promote functional recovery and reduce infarct size in the rat middle cerebral artery occlusion model. Mol Ther 9:189–197
Kim SS, Yoo SW, Park TS, Ahn SC, Jeong HS, Kim JW, Chang DY, Cho KG et al (2008) Neural induction with neurogenin1 increases the therapeutic effects of mesenchymal stem cells in the ischemic brain. Stem Cells 26:2217–2228
Acknowledgments
The authors are grateful to Ya-Chun Hsiao for the services regarding image acquisition and analysis from the FACS-like tissue cytometry in the Center of Clinical Medicine, NCKU Hospital, and Ming-Tai Yu and Yi-Ru Gu for the technical support. This study is partly supported by NCKU Academic Summit Program and the Ministry of Science and Technology grant (MOST-105-2321-B-006-002, MOST-104-2321-B-006-010, MOST-103-2321-B-006 -028, MOST-105-2628-B-006-016-MY3, and NSC-102-2320-B-006-040-MY3).
Author Contribution
Cheng-Chun conceived and designed the study, collected and assembled the data, analyzed and interpreted the data, and wrote the manuscript. I-Fang provisioned the study material and analyzed and interpreted the data. Po-Min conceived and designed the study and collected and assembled the data. Liang-Chao conceived and designed the study and collected and assembled the data. Che-Kun James provisioned the study material and analyzed and interpreted the data. Kuen-Jer conceived and designed the study, collected and assembled the data, analyzed and interpreted the data, wrote the manuscript, and approved the final version of manuscript.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflicts of Interest
The authors have no conflict of interest in this study.
Additional information
Cheng-Chun Wu and I-Fang Wang contributed equally to this study.
Electronic Supplementary Material
ESM 1
(DOC 1524 kb)
Rights and permissions
About this article
Cite this article
Wu, CC., Wang, IF., Chiang, PM. et al. G-CSF-mobilized Bone Marrow Mesenchymal Stem Cells Replenish Neural Lineages in Alzheimer’s Disease Mice via CXCR4/SDF-1 Chemotaxis. Mol Neurobiol 54, 6198–6212 (2017). https://doi.org/10.1007/s12035-016-0122-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-016-0122-x