Abstract
Fibroblast growth factor 2 (FGF-2) has a neurotrophic effect on dopaminergic neurons in vitro and in vivo, and exhibits beneficial effects in animal models of neurodegenerative disorders such as Parkinson’s disease (PD). The poor stability and short half-life of FGF-2, however, have hampered its clinical use for neurological diseases. In the present study, we modified native recombinant human FGF-2 (rhFGF-2) by covalently attaching polyethylene glycol (PEG) polymers, named PEGylation, to enhance its neuroprotection efficacy in 6-hydroxydopamine (6-OHDA)-induced model of PD. In vitro, PEG-rhFGF-2 performed better biostability in 6-OHDA-induced PC-12 cells than native rhFGF-2. The in vivo data showed that, compared with native rhFGF-2, PEGylated rhFGF-2 was more efficacious in preventing 6-OHDA-induced lesion upon tyrosine hydroxylase-positive neurons in the substantia nigra (SN), improving the apomorphine-induced rotational behavior and the 6-OHDA-induced decline in tissue concentration of dopamine (DA) and its metabolites. Importantly, our data showed that the superior pharmacological activity of PEGylated rhFGF-2 is probably due to its greater permeability through the blood–brain barrier and better in vivo stability compared to native rhFGF-2. The enhanced stability and bioavailability of PEGylated rhFGF-2 make this molecule a great therapeutic candidate for neurodegenerative diseases such as PD and mood disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson’s disease (PD) is a progressive neurodegenerative disorder characterized by the inability to initiate, execute, and control movement [1]. The main neuropathological hallmark of PD is the significant loss of dopamine-producing neurons in the substantia nigra pars compacta (SNpc) and the nigrostriatal pathway, accompanied by a depletion of dopamine in the striatum [1, 2]. While the etiology of the degeneration of SNpc cells remains unknown, mechanisms that lead to neuronal cell death have been elucidated, including oxidative stress, mitochondrial dysfunction, apoptosis, and inflammation [3]. Despite the evolving advancement of experimental pharmacotherapies for PD in animals, the current available treatments for PD remain symptomatic in nature. There is an abundance of neuroprotective drugs including monoamine inhibitors and dopamine agonists that are able to offer only symptomatic relief for patients. However, they can’t modify the progression of the neurodegenerative process. There is a lack of pharmacotherapies that are specifically halting or reversing the degenerative processes that characterize PD [4].
Basic fibroblast growth factor (FGF-2) exhibits a multitude of activities on nervous tissue, which include promoting neuronal survival and neurite outgrowth, inhibiting apoptosis and inflammation, and protecting against neuronal injury [5, 6]. Previous studies have shown that FGF-2 can enhance neuronal cell survival and promotes neurite outgrowth by preventing apoptosis and by inducing neuroprotective activity [7]. In vitro, FGF-2 displayed neuroprotective effects after transient focal cerebral ischemia [8] and improved development and function of dopaminergic neurons [9]. Given the potent tissue repair activity of FGF-2, and its demonstrated beneficial effects on ischemic stroke [10], brain trauma [11], seizures [12], and neurodegenerative diseases [13] in vivo, the therapeutic potential of FGF-2 as a neurotrophic factor in patients with neurodegenerative diseases such as PD is promising [14]. The clinical development of FGF-2 for the treatment of neurodegenerative diseases, however, has been hampered due to its rapid plasma clearance, molecular instability, and poor permeability through the blood–brain barrier (BBB). One way to mitigate, the aforementioned pharmacokinetic limitations are to modify the FGF-2 with polyethylene glycol (PEG). PEGylation improves molecular stability, suppresses immunogenic activity, and decreases tissue clearance, thus enhancing bioavailability [15]. Using heparin Sepharose as solid-phase matrix, we previously modified recombinant human FGF-2 (rhFGF-2) at the N-terminus with methoxy-PEG-butyraldehyde (mPEG) and showed that this mono-PEGylated rhFGF-2 is more stable in vitro and in vivo [16].
Base on the better stability than native rhFGF-2, we speculated that the pharmacological property of the PEGylated rhFGF-2 would be significantly improved. To test this hypothesis, in this study, we compared the efficacy of rhFGF-2 and PEGylated rhFGF-2 in a 6-OHDA-induced rat model of PD and determined their pharmacokinetic properties, particularly distributions in the striatum and substantia nigra (SN).
Experimental Procedures
Animals and Reagents
Adult male Sprague Dawley rats (280–300 g) were purchased from Chinese Academy of Science-Shanghai Laboratory Animal Center. All animals were maintained on a 12-h light/dark cycle and a temperature of 25 ± 2 °C. Animal care and all animal experiments conformed to the Guide for the Care and Use of Laboratory Animals provided by U.S. National Institutes of Health and approved by the Animal Care and Use Committee of Wenzhou Medical College, China. Rat pheochromocytoma PC-12 cells were obtained from Shanghai Cell Library of Chinese Academy of Sciences. PEGylated rhFGF-2 and native rhFGF-2 were produced by Key Laboratory of Biotechnology and Pharmaceutical Engineering of Zhejiang Province, Wenzhou Medical University. All chemicals and reagents used in these experiments were of analytical grade and purchased from Sigma-Aldrich Co. (St. Louis MO), Santa Cruz Biotechnology (Santa Cruz, CA), Bio-Rad (Hercules, CA), or Millipore (Billerica, MA) unless otherwise noted.
PC-12 Cell Culture and Cell Counting
The rat pheochromocytoma PC-12 was maintained in Dulbecco’s modified Eagle’s medium (DMEM) (Invitrogen, Carlsbad, CA) supplemented with 10 % fetal bovine serum (FBS, Atlanta Biologicals, GA), 100 U/mL penicillin, and 100 mg/mL streptomycin (Invitrogen, Carsbad, CA) at 37 °C in a 5 % CO2 humidified incubator. The culture medium was changed every 2 days, and cells maintained in culture for 7–10 days were used for the experiments. Cell number was determined by staining a small volume of cell suspension with a 0.2 % trypan blue saline solution and examining the cells in a hemocytometer (Countstar, Shanghai, China).
Cell Viability Assay
Cells were detached and reseeded either in 96-well plates (1.0 × 104 per well) or six-well plates (8.0 × 105 per well). The cells were serum-starved overnight prior to stimulation with either PEGylated rhFGF-2 or native rhFGF-2(1 and 2 μM) for 24 h, followed by a 24-h treatment with 6-OHDA (100 μM). Cells cultured in DMEM were used as control group. After the treatment, the cells cultured in 96-well plates were used for 3-(4, 5-Dimethylthiazol-2-yl)-2, 5-Diphenyltetrazolium Bromide (MTT) assay [17] to measure cell viability, and those in six-well plates were used for immunoblot analysis.
Rat Model of Parkinson’s Disease
Rats were divided into two groups, one receiving 6-OHDA treatment (6-OHDA rats; total n = 54) and the other receiving vehicle treatment (sham rats; n = 18). Each rat was anesthetized with an intraperitoneal (i.p.) injection of chloral hydrate (350 mg/kg body weight) and then placed into a stereotactic head frame (Stoelting, Wood Dale, IL). Either 6-OHDA (2 μL at 5 μg/μL, dissolved in 0.1 % ascorbic acid-saline) or vehicle (2 μL of 0.1 % ascorbic acid-saline) was injected into the striatum (AP 1.0 mm, ML 3.0 mm, and DV 4.5 mm) on the right side. The injection rate was 1 μL/min, which was controlled by an auto-injector device attached to the stereotaxic apparatus. After the injection, the injection needle was left in place for an additional 10 min before being slowly retracted to allow ample time for toxicant diffusion from the lesion site into the brain tissue.
After the lesion, for 4 weeks, the rats were tested for rotational behavior induced by an intraperitoneal (i.p.) injection of 0.5 mg/kg apomorphine hydrochloride. Rats exhibiting a significantly high contralaterally rotational rate (more than seven turns per minute) were used as a valid PD model and selected for further studies [18].
Randomization and FGF-2 Treatment
The PD model mice, which treated with 6-OHDA for 4 weeks, were randomly divided into three groups, and rhFGF-2 was administrated 1 day after PD model setup: one treated with 0.5 mL of physiological saline (n = 18), another treated with 0.5 mL of 4 μM PEGylated rhFGF-2 (n = 18), and the third treated with 0.5 mL of 4 μM native rhFGF-2 (n = 18). Sham rats treated with 0.5 mL of physiological saline (n = 18) served as a control. PEGylated rhFGF-2 and native rhFGF-2 were given once a day for 2 weeks via tail vein injection, and appropriate dosages were determined in pilot studies.
Functional Evaluation of PEGylated rhFGF-2 in 6-OHDA Rats
Rotational Behavior Test
After 7 and 14 days of treatment with PEGylated rhFGF-2 or native rhFGF-2, the rotation behavior of 6-OHDA rats was examined using the same method as described above.
Measurement of Monoamine Neurotransmitters and their Metabolites in the Striatum
The concentrations of monoamine neurotransmitters and their metabolites in the striatal tissue were determined by high performance liquid chromatography-electrochemical detection (HPLC-ECD), base on the corresponding standard curves. Six rats were selected from each group, and their striata were quickly dissected on ice immediately after euthanasia. Tissue samples were sonicated and homogenized in chilled 0.1 M HClO4 (1 mL/200 mg tissue). After centrifugation (10,000g for 15 min at 4 °C), the supernatant was collected and diluted with the mobile phase (75 mM of NaH2PO4, 1.7 mM Octane sulphonic acid, 10 % methanol, pH 3.9) and 10 μL of sample was isocratically eluted through a 150 × 3.5 mm C18 column (Angilent, Milford, MA) at a flow rate of 1.0 mL/min. Neurotransmitters and metabolites including dopamine (DA), 3,4-dihydroxyphenylacetic acid (DOPAC), and homovanilic acid (HVA) were detected by a two-channel electrochemical detector (Waters Associates) at a potential of 1.5 mV. Concentrations were normalized to wet tissue weight.
Immunohistochemistry
Six rats selected from each group were deeply anesthetized with sodium pentobarbital, and the brains were perfusion-fixed with 4 % paraformaldehyde in PBS. Their brains were then dissected and post fixed in paraformaldehyde overnight at 4 °C, after which they were transferred into 20 % sucrose in PBS at 4 °C overnight as described previously [19]. Using a cryostat, a series of 40-μm-thick coronal sections were then cut through the ventral mesencephalon. Nigral brain sections were treated with 3 % hydrogen peroxide (H2O2) to block endogenous peroxidase activity and then incubated overnight at room temperature with primary rabbit antibody against TH (Millipore, Billerica, MA, 1:5,000) and GFAP (Abcam, Cambridge, UK, 1:10,000). After multiple rinses with PBS, the sections were incubated for 20 min at 37 °C in biotinylated secondary anti-rabbit antibody (Vector Laboratories, 1:1,000), followed by incubation with streptavidin-HRP conjugate. The results were analyzed by counting the numbers of positive cells using a computerized image analysis system (Leica Qwin 500 image analysis software), as described previously [20]. The total number of TH and GFAP immunoreactive cells on each representative mesencephalic section was counted for the region of SN by persons who were blind to the treatment. Cell counts were determined ten sections through SN corresponding to the Bregma −2.90 to −3.69 mm from each animal. On each section, a 100 × 100 μm2 grid was randomly placed on the image.
Immunoblot Analysis
Brain tissues and PC-12 cells were homogenized in lysis buffer as described previously [21, 5], and the tissue/cell lysate samples were centrifuged (12,000g, 4 °C) for 15 min. Total protein concentration was determined by BCA kit, and equal amounts of samples (based on total protein concentration) were mixed with Laemmli sample buffer and run on 12 % SDS-polyacrylamide gels at 110 V for 100 min, followed by protein transfer onto polyvinylidine fluoride (PVDF) membranes (Millipore-Billerica, MA, USA). After blocking with 5 % nonfat milk for 2 h at room temperature, PVDF membranes were washed three times with Tris-buffered saline (pH 7.6) containing 0.1 % Tween-20 (TBST) and then incubated at 4 °C overnight with primary antibody to TH (1:5,000), DAT (1:3,000), caspase-3 (1:200), β-actin (1:5,000), or GAPDH (1:5,000). On the following day, the membranes were washed three times with TBST, followed by incubation with HRP-conjugated secondary antibody for 1 h at room temperature. Immunoreactive protein bands were visualized using the ECL system (Rockford, IL, CA) and quantified by optical densitometry.
Pharmacokinetic Evaluation of PEGylated rhFGF-2 and Native rhFGF21 In Vivo
The in vivo pharmacokinetic properties of the two forms of rhFGF-2 were analyzed by intravenous (i.v.) injecting a single dose of 0.5 mL of 4 μM of native or PEGylated rhFGF-2 to 6-OHDA rats and then measuring the dynamic levels of the two forms of rhFGF-2 in the plasma and cerebrospinal fluid (CSF) using ABC-ELISA method. On the basis of the pharmacokinetic curves, the eliminated plasma half-life (t1/2) and other pharmacokinetic parameters were calculated with Drug and Statistics Software (DAS, v 2.0).
Measurement of Exogenous rhFGF-2 Concentration in the Striatum and SN
To determine the dynamic levels of rhFGF-2 and PEGylated rhFGF-2 in the striatum and SN after the relative treatment, rats were deeply anesthetized and perfused with 4 % paraformaldehyde in PBS at the specified time after treatment. All SN and striatal tissues from untreated 6-OHDA rats, 6-OHDA rats treated with PEGylated rhFGF-2 or native rhFGF-2 were homogenized in lysis buffer as described previously [22] and centrifuged at 12,000g at 4 °C for 15 min. Total protein concentration was determined by a bicinchoninic acid (BCA) protein assay kit. RhFGF-2 concentrations were measured by an avidin-biotin-peroxidase complex enzyme-linked immunosorbent assay (ABC-ELISA) as described previously [23].
Statistical Analysis
Data were collected from three independent experiments for the cell-based studies and six rats per group for the in vivo studies, and were expressed as the mean ± standard deviation. One-way ANOVA followed by a post hoc Turkey’s test was used for determining the statistical differences between groups, using Origin 7.5 laboratory data analysis and graphing software. A p value less than 0.05(*) was considered statistically significant.
Results
The Neuroprotective Activity of PEGylated rhFGF-2 in PC-12 Cells
We have recently shown that site-specific PEGylation of rhFGF-2 at its N-terminus significantly increases its thermal stability and retained comparable biological activity with native rhFGF-2. In vivo study also showed that PEGylation endowed rhFGF-2 with improved pharmacokinetic property [16]. PC-12 cell line, the classic cell model for neuroprotective assays relevant to PD, was chosen to further assess the neuroprotective activity and thermal stability of mono-PEGylated rhFGF-2. Freshly prepared samples of PEGylated rhFGF-2 and native rhFGF-2 as well as samples of these proteins that had been incubated at 25 °C for 1 week were used for these studies. The magnitude of the effect elicited by PEGylated rhFGF-2 was similar to that of the native rhFGF-2. Moreover, in contrast to native rhFGF-2, PEGylated rhFGF-2 did not lose its activity when exposed to 25 °C for 1 week (Fig. 1a), which indicated that the PEGylated rhFGF-2 possessed greater thermal stability than the non-PEGylated, native rhFGF-2.
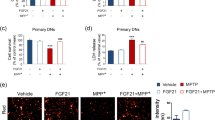
Effects of PEGylated rhFGF-2 on cell viability and apoptosis of 6-OHDA-induced PC12 cells. Effects of PEGylated rhFGF-2 and native rhFGF-2 on the cell viability of 6-OHDA-treated PC12 (a). 6-OHDA-induced PC12 cells were stimulated with PEGylated rhFGF-2 or native rhFGF-2, which had been freshly prepared or incubated at 25 °C for 1 week. Cell stimulation with 6-OHDA or vehicle served as controls. Values are the mean ± SEM (n = 6). *p < 0.05 versus fresh rhFGF-2-treated group. **p < 0.05 versus 1-week incubated rhFGF-2-treated group. Immunoblot analysis for caspase-3 protein expression in PC12 cells (b). Caspase-3 protein expression was normalized to the expression of GAPDH (c). Semiquantitative analysis of the protein bands of the immunoblot shown in panel B. Values are the mean ± SEM (n = 3). *p < 0.05 versus 6-OHDA-treated group
To identify whether anti-apoptotic activity contributed to the neuroprotective action of rhFGF-2, we examined the effect of PEGylated rhFGF-2 and native rhFGF-2 on 6-OHDA-induced apoptosis in PC-12 cells. Protein expression of caspase-3, an important marker for apoptosis, was used as readout for assessing the anti-apoptotic activity of PEGylated rhFGF-2 or native rhFGF-2. As shown in Fig. 1b and c, caspase-3 expression was increased in PC-12 cells treated with 6-OHDA compared to vehicle-treated cells. This effect was reduced by cell co-treatment with PEGylated rhFGF-2 or native rhFGF-2, with no significant difference observed between the PEGylated and the native protein. Together, the data indicated that PEGylated rhFGF-2 retained comparable anti-apoptotic activity with native ligand in PC-12 cells.
Effect of PEGylated rhFGF-2 on Apomorphine-induced Rotational Behavior and Levels of DA, HVA, and DOPAC in the Striatum of 6-OHDA Rats
Encouraged by these cell-based results, we undertook in vivo studies aimed at investigating whether PEGylation improves the efficacy of rhFGF-2 in treating PD. The results of apomorphine-induced rotational behavior were shown in Fig. 2a. After 2 weeks of treatment, PEGylated rhFGF-2 causes a 70 % reduction in apomorphine-induced contralateral rotation in 6-OHDA rats, whereas treatment with a native rhFGF-2 only led to a 30 % reduction. These data demonstrate that PEGylation enhances the efficacy of rhFGF-2 in ameliorating 6-OHDA-induced this neurobehavioral deficit.
Effects of PEGylated rhFGF-2 on apomorphine-induced rotational behavior and concentrations of monoamine neurotransmitters and their metabolites. Effects of PEGylated rhFGF-2 and native rhFGF-2 on apomorphine-induced rotational behavior after 7 and 14 days of treatment (a). DA (b), HVA and DOPAC (c) concentrations in striatum tissue from sham rats and 6-OHDA rats treated with PEGylated rhFGF-2, native rhFGF-2, or vehicle. Note that the striatal tissue concentrations of all these monoamine neurotransmitters and neurotransmitter metabolites tested here are significantly higher in 6-OHDA rats treated with PEGylated rhFGF-2 than in those treated with native rhFGF-2 or vehicle. n = 6 per group. All data are presented as mean ± SEM. *p < 0.05 vs. native rhFGF-2-treated group
Behavior change probably was associated with varying concentrations of monoamine neurotransmitters and their metabolites such as DA, HVA, and DOPAC. Hence, we examined whether PEGylated rhFGF-2 and native rhFGF-2 changed concentrations of DA, HVA, and DOPAC in the lesioned striatal. As shown in the Fig. 2b, the concentrations of DA, HVA, and DOPAC in the lesioned striatum were reduced to 27, 42, and 40 %, respectively, as compared to the sham group. Treatment with either PEGylated rhFGF-2 or native rhFGF-2 for 2 weeks can increase the striatal concentrations of DA, HVA, and DOPAC in 6-OHDA rats (Fig. 2b). Consistent with behavior effects, the striatal concentrations of DA, HVA, and DOPAC (75, 74, and 80 %, respectively) of PEGylated rhFGF-2 treatment group were significantly higher than that of native rhFGF-2 (43, 52, and 57 %) (Fig. 2b). These results demonstrate that PEGylated rhFGF-2 exhibits greater efficacy in protecting against 6-OHDA-induced neurotransmitter deficiency than native rhFGF-2 does.
Effects of PEGylated rhFGF-2 on the Dopaminergic Neurons in the Substantia Nigra (SN) of 6-OHDA Rats
The effects of PEGylated rhFGF-2 and native rhFGF-2 on dopaminergic neurons were compared using immunostaining for TH-positive neurons within the SN and immunoblot analysis for TH protein. Injection of 6-OHDA toxin resulted in a marked loss of TH-positive dopaminergic neurons in the lesioned side of SN (Fig. 3a) and a concurrent reduction in TH protein expression (Fig. 3c, d). A 2-week treatment with either native rhFGF-2 or PEGylated rhFGF-2 prevented the loss of TH-positive neurons in the SN of 6-OHDA rats. Notably, the number of TH-positive neurons in the PEGylated rhFGF-2 treatment group approached sham group’s level, whereas the number of TH-positive neurons in the native rhFGF-2 treatment group was significantly lower than that of the sham group. As shown in Fig. 3b, the IHS values were higher in both rhFGF-2 treatment groups (native rhFGF-2 group, 72 ± 9.04; PEGylated rhFGF-2 group, 144 ± 12.12) compared to untreated 6-OHDA rats (42 ± 5.19). Consistent with the IHS data, treatment with PEGylated rhFGF-2 led to a greater increase in TH protein expression than treatment with native rhFGF-2 (Fig. 3c, d). In addition, DAT protein expression was markedly increased in the striatum of 6-OHDA rats treated with PEGylated rhFGF-2 compared to 6-OHDA rats receiving native rhFGF-2 treatment or no treatment (Fig. 3e, f).
Effects of PEGylated rhFGF-2 on the number of TH-positive neurons and TH/DAT expression in 6-OHDA-lesioned SN tissue. SN tissue sections immunostained for TH (a) and quantitative analysis of the immunostaining (b). Note the significant increase in the number of TH-positive neurons in lesioned SN tissue from 6-OHDA rats treated with PEGylated rhFGF-2 compared to 6-OHDA rats treated with native rhFGF-2 or vehicle. Immunoblot analysis for TH expression in SN tissue (c). TH protein expression was normalized to the expression of Actin (d). Immunoblot analysis for DAT expression in SN tissue (e and f). n = 6 per group. All data are presented as mean ± SEM.*p < 0.05 versus native rhFGF-2-treated group. Scale bar is 100 μm
Effect of PEGylated rhFGF-2 on the Number of GFAP-immunopositive Astrocytes
GFAP immunoreactivity is another widely accepted method for evaluating the activation of SN in 6-OHDA-induced Parkinsonism in rodents. Thus, we immunostained SN tissues from treated and untreated 6-OHDA rats for GFAP. As shown in Fig. 4, the number of GFAP-immunopositive astrocytes was greatly increased in 6-OHDA rats compared to sham rats. Two-week treatment of 6-OHDA rats with either PEGylated rhFGF-2 or native rhFGF-2 reduced the number of GFAP-immunopositive astrocytes, with PEGylated rhFGF-2 treatment showing a greater effect than native rhFGF-2 treatment (Fig. 4).
Effects of PEGylated rhFGF-2 on GFAP-immunopositive astrocytes in the SN tissues from 6-OHDA rats. SN tissue sections immunostained for GFAP (a) and quantitative analysis of the immunostaining (b). n = 6 per group. All data are presented as mean ± SEM. *p < 0.05 versus native rhFGF-2-treated group. Scale bar is 100 μm
Prolonged Effect of PEGylated rhFGF-2 on the TH-positive Neurons and GFAP-Immunopositive Astrocytes Located in the SN
We have previously shown that PEGylated rhFGF-2 is more stable than unconjugated, native rhFGF-2 [16]. Hence, the superior efficacy of PEGylated rhFGF-2 over native rhFGF2 could be attributable to its increased biostability. To test this, we quantitated TH and GFAP immunoreactivity in SN sections 5 days after cessation of a 2-week treatment of 6-OHDA rats with native rhFGF-2 or PEGylated rhFGF-2. As shown in Fig. 5, following treatment with PEGylated rhFGF-2, the number of TH-positive neurons and GFAP-immunopositive astrocytes located in the SN was comparable to that observed in sham rats and remained stable at that level without significant deviation even 5 days after cessation of the treatment. These results strongly support our hypothesis that increased in vivo biostability conferred on rhFGF-2 by PEGylation accounts for the robust and long-lasting protective effects against the neurotoxic changes induced by 6-OHDA.
Persistent effect of PEGylated rhFGF-2 on TH-positive neurons and GFAP-immunopositive astrocytes located in the SN of 6-OHDA rats. SN tissue sections immunostained for TH (a) and quantitative analysis of the immunostaining (b). SN tissue sections immunostained for GFAP (c) and quantitative analysis of the immunostaining (d). SN tissues were isolated from 6-OHDA rats 5 days after cessation of 2-week treatment with PEGylated rhFGF-2 or native rhFGF-2. Note that the number of TH-positive neurons remains at high levels; however, GFAP-immunopositive astrocytes remain at low levels in the SN of 6-OHDA rats that had been treated with PEGylated rhFGF-2. n = 6 per group. All data are presented as mean ± SEM. Scale bar is 100 μm
Bioavailability of Exogenous rhFGF-2 in the Striatum
As showed in Fig. 6a and Table 1, compared with the half-life of native rhFGF-2(22.8 min), the PEGylated rhFGF-2 prolonged the plasma half-life of rhFGF-2 to 201.3 min. Additionally, the PEGylated rhFGF-2 variant also increased the bioavailability and half-life of rhFGF-2 in CSF (Fig. 6b).
The pharmacokinetics and bioavailability of PEG-rhFGF-2 in vivo. Pharmacokinetic profiles of native and PEGylated rhFGF-2. 6-OHDA rats were injected intravenously with 4 μM native and PEGylated rhFGF-2. Plasma and CSF samples were collected at the indicated time points (a and b). Determination of rhFGF-2 concentration in the SN and striatum of 6-OHDA rats treated with PEGylated rhFGF-2 and native rhFGF-2 (c and d). Note the tissue levels of rhFGF-2 reached with PEGylated rhFGF-2 treatment that by far exceed those reached with native rhFGF-2. n = 6 per group. All data are presented as mean ± SEM. *p < 0.05 versus native rhFGF-2-treated group
In addition to enhanced biostability, improved permeability of PEGylated rhFGF-2 through the BBB may also contribute to its greater efficacy compared to native rhFGF-2. To test this, rhFGF-2 concentration in SN and striatum from 6-OHDA rats was measured 0.5, 1, 4, 8, and 12 h after treatment with native rhFGF-2 or PEGylated rhFGF-2 (Fig. 6). Interestingly, the rhFGF-2 concentrations measured in the PEGylated rhFGF-2 treatment group were significantly greater than those measured in the native rhFGF-2 treatment group at the beginning of 4 h. These data indicate an enhanced bioavailability of the PEGylated rhFGF-2 in the brain of 6-OHDA rats compared to native rhFGF-2.
Discussion
In this study, we evaluated in a widely accepted rat model of PD the therapeutic efficacy of an N-terminal PEG conjugate of rhFGF-2 in comparison to the native ligand with the aim of developing FGF-2 into a biotherapeutic for the treatment of neurodegenerative disorders such as PD. In light of therapeutic potential, we have found that PEGylated rhFGF-2 is more effective than native rhFGF-2 in neuroprotection against 6-OHDA-induced lesion in rats.
As described previously, FGF-2 is expressed in both striatal and nigral neurons [24], thus damage to either area produces a state of local FGF-2 deficiency that precludes a generalized neurogenesis response to injury. This would be consistent with the finding that stroke-induced neurogenesis is reduced in FGF-2 knockout mice and restored by i.c.v. administration of an FGF-2-expressing herpes simplex virus amplicon vector [25]. In addition, when FGF-2 is depleted from the SN in 4-phenyl-1,2,3,6-tetrahydropyridine(MPTP)-induced Parkinsonism in mice, treatment with FGF-2 enhanced histological and biochemical recovery from MPTP toxicity [26]. Hence, we used 6-OHDA-induced PD rats to investigate and compare the neuroprotective effects of native rhFGF-2 and PEGylated rhFGF-2. Besides MPTP, 6-OHDA is another classic neurotoxin that is commonly used for induction of Parkinsonism and testing of therapeutic candidates. 6-OHDA simulates neurological changes characteristic for PD and also induces quantifiable rotational behavior in mice, making it an ideal tool for the study of potential therapeutics for PD [27].
Clinical use of classical neurotrophins or neuroprotective cytokines (e.g., erythropoietin or brain-derived neurotrophic factor) for the treatment of neurodegenerative diseases is hampered by the rapid serum clearance of these cytokines and the inconvenience of frequent parenteral or intrathecal administration [28]. Molecular modification of therapeutic proteins with synthetic macromolecules such as poly (ethylene glycol) (PEG) represents an important, novel strategy to improve the pharmacokinetic properties and biostability of protein-based drugs [16]. It has been previously reported that PEG-conjugated therapeutic peptides or proteins exhibit clinical properties superior to those of their corresponding unmodified parental counterparts by prolonging the half-life of drugs and reducing the frequency of drug injections [29]. This study is the first to utilize PEGylated rhFGF-2 to enhance its in vivo efficacy in a commonly used animal model of PD. The PEGylated rhFGF-2 used in this study was modified by a novel solid-phase PEGylation, which retained comparable biological activity and secondary structure of rhFGF-2. In vivo study showed that this PEGylated rhFGF-2 showed improved pharmacokinetic properties [16]. For these reasons, PEGylated rhFGF-2 was hypothesized to have enhanced neuroprotective capabilities in vivo compared to native rhFGF-2. Indeed, as confirmed in this study, PEGylation significantly enhances rhFGF-2’s neuroprotective potential by enhanced stability and bioavailability of PEGylated rhFGF-2.
6-OHDA induced a significant decline in the concentrations of striatal monoamine neurotransmitters and their metabolites (DA, HVA, and DOPAC), as well as enzymes (TH) and transporters (DAT) that participate in dopamine metabolism. PEGylated rhFGF-2 treatment significantly reversed this decline (Figs. 2 and 3), and the amounts of certain posttreatment neurochemicals reached levels similar to those measured in the sham group. In contrast, the differences in these striatal neurochemical concentrations between 6-OHDA rats treated with native rhFGF-2 and untreated 6-OHDA rats were not as significant. This finding is consistent with the immunohistochemistry results. As shown in Fig. 3, the populations of TH-positive neurons in the SN were significantly increased in 6-OHDA rats that had been treated with PEGylated rhFGF-2 compared untreated 6-OHDA rats. TH intensity and expression levels were noticeably lower in the SN from the native rhFGF-2 group than in those from the PEGylated treatment group and the sham group.
Several studies in the 6-OHDA-lesioned animal model of PD have found that GFAP levels were elevated for up to 1 month post-lesion, indicating the inevitable reactive astrogliosis process that occurs after dopaminergic neuronal death [30]. In our study, GFAP-positive neurons in the striatum displayed lower intensities in the PEGylated rhFGF-2 treatment group than the untreated 6-OHDA rat group (Figs. 4 and 5). Whether PEGyated rhFGF-2 treatment reduced GFAP expression via prevention of primary neuronal cell death or inhibiting reactive astrogliosis remains to be elucidated.
Apoptosis is the cellular reaction that signifies irreversible neuronal damage. In PD, it is the apoptosis of dopaminergic neurons that defines its disease pathology [31]. To assess the anti-apoptotic activity of PEGylated rhFGF-2 in comparison to native rhFGF-2, we examined apoptosis-induced caspase-3 protein expression in PC-12 cells in response to cell stimulation with PEGylated rhFGF-2 or native rhFGF-2. Miho Y et al. have shown previously that rhFGF-2 can suppress caspase-3 protein expression and inhibits processing of caspase-3 into its active form [32]. Consistent with those findings, the expression levels of caspase-3 in 6-OHDA treated PC-12 cells were significantly lower in cells co-treated with either PEGylated rhFGF-2 or native rhFGF-2 than in cells treated with 6-OHDA only (Fig. 1), indicating that rhFGF-2 downregulated the expression of caspase-3 and halted the apoptosis signaling pathway. In addition, we found that the expression level of caspase-3 in PC-12 cells co-treated with 6-OHDA and PEGylated rhFGF-2 was comparable to that in cells co-treated with 6-OHDA and native rhFGF-2, indicating that the PEGylated rhFGF-2 fully retained the anti-apoptotic activity of rhFGF-2. These findings suggest that PEGylated rhFGF-2 is equally effective as native rhFGF-2 in protecting neuronal cells from 6-OHDA-induced lesion and neurodegeneration.
Finally, the BBB poses another challenge for the use of large molecules such as growth factors for the treatment of neurodegenerative disorders. This tight barrier serves as a gatekeeper in higher organisms that controls which molecules have access to the nervous system [33]. This structure provides a physical barrier in the form of tight junctions with membrane proteins and lipids that seal the gaps between endothelial cells. It also provides a chemical barrier that regulates the transport of material through these cells and pumps foreign substances away from the brain. The BBB is a double-edged sword in that it effectively protects the brain against foreign substances, but at the same time limits access to many therapeutic agents designed to treat neurological disorders. It has been proven that PEGylation not only increases the biologic half-life of proteins, but also enhances their distribution in tissues by enhancing penetration of target proteins into tissue [34]. As shown in Fig. 6, rhFGF-2 protein levels in SN and striatal from the PEGylated rhFGF-2 treatment group were significantly higher than that of the native rhFGF-2 treatment group. This implies that PEGylation can enhance rhFGF-2 penetration of the BBB and hence improve its delivery into the brain. This finding, combined with the ability of PEGylation to improve the stability and half-life of rhFGF-2, demonstrates that PEGylated rhFGF-2 has a pharmacokinetic profile that is more favorable than that of native rhFGF-2 with regard to the use of FGF-2 as a neuroprotective therapeutic agent.
In summary, in this study, we investigated the in vivo and in vitro effects of PEGylated rhFGF-2 and native rhFGF-2 in the widely accepted rat model of 6-OHDA-induced PD, and our data provide a solid evidence that solid-phase mono-PEGylation of rhFGF-2 improves rhFGF-2’s efficacy in modulating neuromuscular behavior, tissue pathology, and neurochemical change, while retaining neuroprotective activity of rhFGF-2. Hence, PEGylated rhFGF-2 is an ideal disease-modifying candidate to consider for the treatment of PD and potentially other neurodegenerative disorders.
References
Aarsland D, Pahlhagen S, Ballard CG, Ehrt U, Svenningsson P (2012) Depression in Parkinson disease—epidemiology, mechanisms and management. Nat Rev Neurol 8(1):35–47. doi:10.1038/nrneurol.2011.189
Schapira AH, Olanow CW (2004) Neuroprotection in Parkinson disease: Mysteries, myths, and misconceptions. JAMA 291(3):358–364. doi:10.1001/jama.291.3.358
Shrivastava P, Vaibhav K, Tabassum R, Khan A, Ishrat T, Khan MM, Ahmad A, Islam F, Safhi MM (2013) Anti-apoptotic and anti-inflammatory effect of Piperine on 6-OHDA induced Parkinson’s rat model. J Nutr Biochem 24(4):680–687. doi:10.1016/j.jnutbio.2012.03.018
Hardwick A, Ward H, Hassan A, Romrell J, Okun MS (2013) Clozapine as a potential treatment for refractory impulsive, compulsive, and punding behaviors in Parkinson’s disease. Neurocase 19(6):587–591. doi:10.1080/13554794.2012.713490
Litteljohn D, Hayley S (2012) Cytokines as potential biomarkers for Parkinson’s disease: a multiplex approach. Methods Mol Biol 934:121–144. doi:10.1007/978-1-62703-071-7_7
de Oliveira GP, Duobles T, Castelucci P, Chadi G (2010) Differential regulation of FGF-2 in neurons and reactive astrocytes of axotomized rat hypoglossal nucleus. A possible therapeutic target for neuroprotection in peripheral nerve pathology. Acta Histochem 112(6):604–617. doi:10.1016/j.acthis.2009.06.008
Rose K, Litterscheid S, Klumpp S, Krieglstein J (2009) Fibroblast growth factor 2 requires complex formation with ATP for neuroprotective activity. Neuroscience 164(4):1695–1700. doi:10.1016/j.neuroscience.2009.09.055
Ma YP, Ma MM, Cheng SM, Ma HH, Yi XM, Xu GL, Liu XF (2008) Intranasal bFGF-induced progenitor cell proliferation and neuroprotection after transient focal cerebral ischemia. Neurosci Lett 437(2):93–97. doi:10.1016/j.neulet.2008.04.003
Klejbor I, Myers JM, Hausknecht K, Corso TD, Gambino AS, Morys J, Maher PA, Hard R, Richards J, Stachowiak EK, Stachowiak MK (2006) Fibroblast growth factor receptor signaling affects development and function of dopamine neurons—Inhibition results in a schizophrenia-like syndrome in transgenic mice. J Neurochem 97(5):1243–1258. doi:10.1111/j.1471-4159.2006.03754.x
Kawamata T, Dietrich WD, Schallert T, Gotts JE, Cocke RR, Benowitz LI, Finklestein SP (1997) Intracisternal basic fibroblast growth factor enhances functional recovery and up-regulates the expression of a molecular marker of neuronal sprouting following focal cerebral infarction. Proc Natl Acad Sci U S A 94(15):8179–8184
Yoshimura S, Teramoto T, Whalen MJ, Irizarry MC, Takagi Y, Qiu J, Harada J, Waeber C, Breakefield XO, Moskowitz MA (2003) FGF-2 regulates neurogenesis and degeneration in the dentate gyrus after traumatic brain injury in mice. J Clin Invest 112(8):1202–1210. doi:10.1172/JCI16618
Liu Z, Holmes GL (1997) Basic fibroblast growth factor is highly neuroprotective against seizure-induced long-term behavioural deficits. Neuroscience 76(4):1129–1138
Jin K, LaFevre-Bernt M, Sun Y, Chen S, Gafni J, Crippen D, Logvinova A, Ross CA, Greenberg DA, Ellerby LM (2005) FGF-2 promotes neurogenesis and neuroprotection and prolongs survival in a transgenic mouse model of Huntington’s disease. Proc Natl Acad Sci U S A 102(50):18189–18194. doi:10.1073/pnas.0506375102
Drinkut A, Tereshchenko Y, Schulz JB, Bahr M, Kugler S (2012) Efficient gene therapy for Parkinson’s disease using astrocytes as hosts for localized neurotrophic factor delivery. Mol Ther J Am Soc Gene Ther 20(3):534–543. doi:10.1038/mt.2011.249
Jevsevar S, Kunstelj M, Porekar VG (2010) PEGylation of therapeutic proteins. Biotechnol J 5(1):113–128. doi:10.1002/biot.200900218
Huang Z, Ye C, Liu Z, Wang X, Chen H, Liu Y, Tang L, Zhao H, Wang J, Feng W, Li X (2012) Solid-phase N-terminus PEGylation of recombinant human fibroblast growth factor 2 on heparin-sepharose column. Bioconjug Chem 23(4):740–750. doi:10.1021/bc200550f
Wang Z, Zhang H, Xu X, Shi H, Yu X, Wang X, Yan Y, Fu X, Hu H, Li X, Xiao J (2012) bFGF inhibits ER stress induced by ischemic oxidative injury via activation of the PI3K/Akt and ERK1/2 pathways. Toxicol Lett 212(2):137–146. doi:10.1016/j.toxlet.2012.05.006
Hashitani T, Mizukawa K, Kumazaki M, Nishino H (1998) Dopamine metabolism in the striatum of hemiparkinsonian model rats with dopaminergic grafts. Neurosci Res 30(1):43–52
Han B, Hu J, Shen J, Gao Y, Lu Y, Wang T (2013) Neuroprotective effect of hydroxysafflor yellow A on 6-hydroxydopamine-induced Parkinson’s disease in rats. Eur J Pharmacol 714(1–3):83–88. doi:10.1016/j.ejphar.2013.06.011
Soslow RA, Dannenberg AJ, Rush D, Woerner BM, Khan KN, Masferrer J, Koki AT (2000) COX-2 is expressed in human pulmonary, colonic, and mammary tumors. Cancer 89(12):2637–2645
Zhang HY, Zhang X, Wang ZG, Shi HX, Wu FZ, Lin BB, Xu XL, Wang XJ, Fu XB, Li ZY, Shen CJ, Li XK, Xiao J (2013) Exogenous basic fibroblast growth factor inhibits ER stress-induced apoptosis and improves recovery from spinal cord injury. CNS Neuroscience & Therapeutics 19(1):20–29. doi:10.1111/cns.12013
Yang F, Yang YP, Mao CJ, Cao BY, Cai ZL, Shi JJ, Huang JZ, Zhang P, Liu CF (2009) Role of autophagy and proteasome degradation pathways in apoptosis of PC12 cells overexpressing human alpha-synuclein. Neurosci Lett 454(3):203–208. doi:10.1016/j.neulet.2009.03.027
Huang Z, Zheng Q, Wu X, Su Z, Xu H, Tan Y, Feng W, Li X, Cai L (2007) Enhanced protection of modified human acidic fibroblast growth factor with polyethylene glycol against ischemia/reperfusion-induced retinal damage in rats. Toxicol Lett 170(2):146–156. doi:10.1016/j.toxlet.2007.03.001
Gonzalez AM, Berry M, Maher PA, Logan A, Baird A (1995) A comprehensive analysis of the distribution of FGF-2 and FGFR1 in the rat brain. Brain Res 701(1–2):201–226
Yoshimura S, Takagi Y, Harada J, Teramoto T, Thomas SS, Waeber C, Bakowska JC, Breakefield XO, Moskowitz MA (2001) FGF-2 regulation of neurogenesis in adult hippocampus after brain injury. Proc Natl Acad Sci U S A 98(10):5874–5879. doi:10.1073/pnas.101034998
Date I, Yoshimoto Y, Imaoka T, Miyoshi Y, Gohda Y, Furuta T, Asari S, Ohmoto T (1993) Enhanced recovery of the nigrostriatal dopaminergic system in MPTP-treated mice following intrastriatal injection of basic fibroblast growth factor in relation to aging. Brain Res 621(1):150–154
Young CK, Koke SJ, Kiss ZH, Bland BH (2009) Deep brain stimulation of the posterior hypothalamic nucleus reverses akinesia in bilaterally 6-hydroxydopamine-lesioned rats. Neuroscience 162(1):1–4. doi:10.1016/j.neuroscience.2009.04.053
Epstein SE, Fuchs S, Zhou YF, Baffour R, Kornowski R (2001) Therapeutic interventions for enhancing collateral development by administration of growth factors: basic principles, early results and potential hazards. Cardiovasc Res 49(3):532–542
Hu J, Duppatla V, Harth S, Schmitz W, Sebald W (2010) Site-specific PEGylation of bone morphogenetic protein-2 cysteine analogues. Bioconjug Chem 21(10):1762–1772. doi:10.1021/bc9005706
Teismann P, Schulz JB (2004) Cellular pathology of Parkinson’s disease: astrocytes, microglia and inflammation. Cell Tissue Res 318(1):149–161. doi:10.1007/s00441-004-0944-0
Tatton WG, Chalmers-Redman R, Brown D, Tatton N (2003) Apoptosis in Parkinson’s disease: Signals for neuronal degradation. Ann Neurol 53(Suppl 3):S61–S70. doi:10.1002/ana.10489, discussion S70-62
Miho Y, Kouroku Y, Fujita E, Mukasa T, Urase K, Kasahara T, Isoai A, Momoi MY, Momoi T (1999) bFGF inhibits the activation of caspase-3 and apoptosis of P19 embryonal carcinoma cells during neuronal differentiation. Cell Death Differ 6(5):463–470. doi:10.1038/sj.cdd.4400506
Abbott NJ, Patabendige AA, Dolman DE, Yusof SR, Begley DJ (2010) Structure and function of the blood–brain barrier. Neurobiol Dis 37(1):13–25. doi:10.1016/j.nbd.2009.07.030
Liu Y, Li J, Shao K, Huang R, Ye L, Lou J, Jiang C (2010) A leptin derived 30-amino-acid peptide modified pegylated poly-L-lysine dendrigraft for brain targeted gene delivery. Biomaterials 31(19):5246–5257. doi:10.1016/j.biomaterials.2010.03.011
Acknowledgments
The authors are thankful to Dr. Regina Goetz and Moosa Mohammadi for critically reading the manuscript and making thoughtful suggestions. This work was supported, in part, by grants from Natural Science Foundation of China, 81102486, 81010012 (to Z.H. and X.L.); Zhejiang Key Group Project in Scientific Innovation 2010R10042-01 (to Z.H.); Ningbo Natural Science Foundation (2013A610272 to C.Y.).
Author information
Authors and Affiliations
Corresponding authors
Additional information
Guanghui Zhu, Ganping Chen, Lu Shi, and Jenny Feng contributed equally to this work.
Rights and permissions
About this article
Cite this article
Zhu, G., Chen, G., Shi, L. et al. PEGylated rhFGF-2 Conveys Long-term Neuroprotection and Improves Neuronal Function in a Rat Model of Parkinson’s Disease. Mol Neurobiol 51, 32–42 (2015). https://doi.org/10.1007/s12035-014-8750-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-014-8750-5