Abstract
Alzheimer’s disease (AD) is the most common progressive neurodegenerative disease. Today, AD affects millions of people worldwide and the number of AD cases will increase with increased life expectancy. The AD brain is marked by severe neurodegeneration like the loss of synapses and neurons, atrophy and depletion of neurotransmitter systems in the hippocampus and cerebral cortex. Recent findings suggest that these pathological changes are causally induced by mitochondrial dysfunction and increased oxidative stress. These changes are not only observed in the brain of AD patients but also in the periphery. In this review, we discuss the potential role of elevated apoptosis, increased oxidative stress and especially mitochondrial dysfunction as peripheral markers for the detection of AD in blood cells especially in lymphocytes. We discuss recent not otherwise published findings on the level of complex activities of the respiratory chain comprising mitochondrial respiration and the mitochondrial membrane potential (MMP). We obtained decreased basal MMP levels in lymphocytes from AD patients as well as enhanced sensitivity to different complex inhibitors of the respiratory chain. These changes are in line with mitochondrial defects obtained in AD cell and animal models, and in post-mortem AD tissue. Importantly, these mitochondrial alterations where not only found in AD patients but also in patients with mild cognitive impairment (MCI). These new findings point to a relevance of mitochondrial function as an early peripheral marker for the detection of AD and MCI.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Mitochondrial Dysfunction and Oxidative Stress—Important Players in Brain Aging and Alzheimer’s Disease
Like other differentiated tissues, the central nervous system is profoundly affected by aging which is characterised by a decline of several physiological abilities including sensory, motor, emotional or cognitive functions [1–5]. Aging brain cells experience increasing amounts of oxidative stress, perturbed energy homeostasis, accumulation of damaged proteins, lesions in their nucleic acids and are characterised by impaired function of signalling mechanisms and altered gene expression. These changes are significantly exacerbated in neurodegenerative disorders and amplified in vulnerable neuronal populations [6]. Beside the described dysfunctions, mitochondrial perturbations are strongly associated with aging. Mitochondria play a central role in producing adenosine-5′-triphosphate (ATP) as a major source of cellular energy and are critical regulators of programmed cell death in brain aging [2, 3, 7]. Mitochondrial function becomes less efficient during the aging process including decreased activities of complex I and to a lesser content of complex III of the respiratory chain, which in turn lead to enhanced reactive oxygen species (ROS) production, reduced Ca2+ buffering capacity, and accumulation of mitochondrial DNA (mtDNA) mutations (review for this topic [8]).
Abnormalities in mitochondrial function and oxidative stress are also relevant for the pathogenesis of Alzheimer’s disease (AD) [9–12]. In brains of AD patients, defective energy metabolism and early defects in glucose utilisation were observed [13]. Moreover, the AD brain is specifically marked by accumulation of the misfolded proteins Aß and hyperphosphorylated tau, both contributing together with aging-related deficits to severe neurodegenerative alterations, such as the loss of synapses and neurons, atrophy and the selective depletion of neurotransmitter systems (e.g. acetylcholine) in the hippocampus and cerebral cortex [14, 15]. At the mitochondrial level, complexes I, IV and V seem to be specifically affected, where tau pathology mainly impairs complexes I and V activity and Aß complex IV activity [10, 16, 17]. Importantly, mitochondrial dysfunction and reduced bioenergetics occur early in the AD pathogenesis and precede the development of plaque formation [10]. Moreover, ours and others findings indicate that mitochondrial dysfunction via ROS production enhances Aß production, closing a vicious circle not only between mitochondrial dysfunction and ROS but also including the toxic effects of Aß [9].
Alzheimer’s Disease Shows Typical Peripheral Affection
Due to the brain-specific typical lesions and histopathological alterations, most of the time AD was considered as a pure brain disease. Observations that measures of oxidative stress and even apoptosis are elevated in several accessible peripheral tissues like fibroblasts and blood cells [18, 19] were rather neglected because they did not dig into the concept of AD being a brain-specific disease. With our advanced knowledge about the pathophysiology of AD, it becomes plausible that many tissues of AD patients where no elevated Aß levels can be detected show mitochondrial dysfunction with enhanced ROS formation and oxidative stress induced damage. Moreover, the observations of substantial mitochondrial dysfunction in peripheral tissues are strong arguments that this aspect represents the primary defect in AD, which by mechanisms not yet fully understood leads also to Aß and Tau pathology in some brain areas. Thus, peripheral measures of mitochondrial dysfunction may also serve as important biomarkers for this major aspect of AD [19–21].
Peripheral tissues used to study aspects of mitochondrial dysfunction in AD patients and AD mouse model mainly include fibroblasts [22–24] but also all types of blood cells but mainly platelets and lymphocytes. A short overview of the use of platelets to study mitochondrial dysfunction in AD gives Table 1 [25–28]. Much less work is available for erythrocytes [25, 29–31]. However, both cell types, erythrocytes as well as platelets have the disadvantage of being dead cells lacking the nucleus. Thus, most groups have used lymphocytes as living cells with even some similarities to neurons [20]. Keeping in mind that ROS induced damage of nuclear as well as mitochondrial DNA seems to be a critical aspect of AD, circulating lymphocytes appear to be the best model to study mitochondrial dysfunction in AD at the peripheral level. Moreover, lymphocytes have also been used as an accessible tissue to study alterations of immunological mechanism in AD [32].
Increase Oxidative Stress in Lymphocytes of AD Patients
Elevated oxidative stress was also detected in peripheral cells like lymphocytes (Table 2) and fibroblasts [33–35]. The leakage of ROS from mitochondria can be detected by different parameters such as the direct measurement of ROS levels, the antioxidant status or DNA oxidation [20, 36]. Our group showed that lymphocytes from AD patients handle oxidative stress differently than aged-matched controls. Firstly, lymphocytes of AD patients are characterised by increased basal ROS levels and show elevated ROS after treatment with staurosporine [37]. However, ROS levels after treatment with H2O2 were not different between patients and controls [37], probably due to elevated antioxidative defence mechanism. This assumption is supported by results of altered levels and activities of antioxidant enzymes in post-mortem analysis of brain material and other tissues of AD patients. De Leo et al. provided evidence that mRNA levels of Mn-superoxide dismutase are significantly increased in lymphocytes, probably as a response to an increased level of ROS in AD [38]. In line with the presence of oxidative stress in AD, the total plasma antioxidant status was found to be decreased in AD patients. These results are supported by different groups [36, 39–43]. Some also found significantly higher concentrations of 8-hydroxy-2-deoxyguanosine, the major product of DNA oxidations. Supporting the hypothesis of elevated peripheral oxidative stress in AD, significantly lower plasma levels of antioxidants were detected in blood from sporadic AD patients compared with aged healthy controls [42, 44] Another group reported significantly elevated levels of oxidative DNA damage [45] at basal levels in lymphocytes of sporadic AD and after additional oxidative stress induced by H2O2 [39]. Beside, DNA oxidation-mediated altered activity and expression of antioxidant enzymes were found in peripheral blood cells of sporadic AD patients [38].
In lymphoblasts and fibroblasts from familial AD patients with PS and APP mutations, a clear increase in lipid-peroxidation products malondialdehyde and hydroxynonenale was found [40]. Furthermore, the anti-oxidant capacity in lymphoblasts from peripheral blood of familial AD patients was reduced [46]. These results are confirmed by findings in transgenic animals. Elevated ROS levels were found in lymphocytes of PS1 mutant mice [47, 48].
Elevated Apoptosis in Lymphocytes of AD Patients
Studies in lymphocytes from sporadic AD patients have provided evidence for elevated apoptosis (Table 3). Aging itself induces an increase in vulnerability to apoptosis [49]. This enhanced susceptibility seems to be even more pronounced in lymphocytes from sporadic AD patients [50–52]. Elevated DNA fragmentation was seen in freshly prepared AD lymphocytes compared with controls and spontaneous apoptotic cell death after 24 h was significantly elevated [34]. Importantly, elevated basal apoptosis from AD patients correlated significantly with the Mini Mental State Examination (MMSE) of these AD patients. Furthermore, lymphocytes from AD patients showed an increased vulnerability to proapoptotic stimuli like 2-desoxy-ribose or staurosporine. Significantly elevated levels of DNA fragmentation were found in activated AD lymphocytes undergoing spontaneous in vitro apoptosis or enhanced apoptosis after the treatment with D-ribose. These results point to a faster turnover of apoptotic pathways in AD patients [53]. Importantly, a robust difference in cell death sensitivity between AD patients and patients suffering from vascular dementia was detected [52, 54].
Moreover, increased CD 95 expression on the surface of T cells from sporadic AD patients and elevated caspase 3, caspase 8 and caspase 9 levels in comparison with non-demented controls refer to an enhanced proneness of AD lymphocytes to cell death [55–57]. These findings suggest involvement of the extrinsic and intrinsic apoptotic pathway.
The above illustrated findings cannot be explained by changes in the distribution of lymphocyte subsets. No changes in subset distribution of T, B or NK cells were found in AD patients compared with aged controls [34, 50]. In contrast, a significant decrease in T lymphocytes was determined in healthy persons >60 years compared with young persons <30 years [58]. Again, no changes in the distribution of T lymphocyte population in AD patients compared with aged controls were found [34, 50, 55], but a significant loss of CD3+, CD4+ and CD8+ occurred during aging. Interestingly, several recent findings indicate that mainly CD4+ cells contribute to the increased apoptotic levels in peripheral lymphocytes of AD patients, whereas no changes in the susceptibility of CD8+ T cells to apoptosis were determined [34, 50, 55].
Besides aging, apolipoprotein E (ApoE) genotype is the most important risk factor for sporadic AD. The three major human isoforms E2, E3 and E4 differ in two amino acids in the positions 112 and 158. The Isoform ApoE4 is associated with an increased risk to develop AD. Different effects of ApoE 4 contributing to pathophysiology of AD like the modulation of the deposition and clearance of Aß, the impairment of the antioxidative defence system or an increased phosphorylation of Tau are currently discussed [59]. Interestingly, lymphocytes from AD patients bearing one or two Apo ε4 alleles (heterogen ε4/ε3 or homogen ε4/ε4) exhibit a higher rate of apoptotic cell death and caspase 3 activation than Apoε3/ε3 carrier [50, 55]. Furthermore, elevated apoptosis was also found in lymphocytes of familiar AD patients and AD animal models bearing AD relevant APP or PS1 mutations [34, 48, 60], supporting the idea that AD-specific changes lead to the elevated susceptibility of T lymphocytes.
Mitochondrial Dysfunction in Lymphocytes as a Potential Biomarker for AD
Mitochondrial dysfunction can also be detected in peripheral tissues like platelets. Several studies showed a decreased cytochrome c activity in human platelets from AD patients [61–63]. In accordance with these findings, platelets of AD patients showed decreased ATP levels and increased levels of ROS [61]. A few newer reports are summarised in Table 1 indicating clear evidence for mitochondrial dysfunction in platelets of AD patients, in most cases already seem in MCI patients. These finding again suggests that even at the platelet level, mitochondrial dysfunction precedes the clinical manifestation of AD.
In lymphocytes of sporadic AD patients only few studies were conducted referring to mitochondrial dysfunction. Two earlier reports found no changes of the respiratory chain complexes in AD lymphocytes [64, 65]. Our group investigated initially a protein factor that acts upstream of mitochondrial dysfunction, Bcl2 [50]. The antiapoptotic Bcl2 protein can form heteromers with the proapoptotic Bax and thereby prevents the apoptogenic activity of Bax [66]. We found a tendency of elevated Bcl2 in T cells of sporadic AD patients compared with aged controls. Again, CD4+ cells were more sensitive compared with AD-related changes. Bcl2 levels were significantly elevated in CD4+ cells compared with CD8+ cells. Very interestingly, when splitting up AD patients into mild (MMSE, >20) and severe (MMSE, <20) AD, a dual regulation was observed. Bcl2 was up-regulated in mild AD while further progression of the disease resulted in Bcl2 content decreases associated with cognitive loss. We suggest that in the early stage of AD, Bcl2 is compensatory upregulated to protect cells against apoptosis.
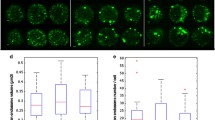
Clear evidence for mitochondrial dysfunction in AD lymphocytes comes from some of our recent not otherwise published experiments (Figs. 1, 2 and 3) using the same measures as previously employed in cell lines or brain cells from transgenic mice overexpressing mutant human APP [10]. In this new cohort of patients, we confirmed our findings of enhanced apoptosis in AD lymphocytes and showed mainly the CD4+ fraction is responsible for this observation (Fig. 1a, b). In the same group of patients, we observed a significant reduction of the mitochondrial membrane potential (MMP) (Fig. 1c, d), again only for the CD4+ fraction. In both cases, MCI lymphocytes were very close to AD lymphocytes (Fig. 1a, c). ROS levels in the present study were reduced and not changed in MCI (Fig. 1e, f). This is different to our previous findings for basal ROS levels in lymphocytes of AD patients but not with ROS levels after stimulation with H2O2 (37). During the course of AD, levels of antioxidant enzymes may get upregulated however with large variances due to several factors such as gender and aging as previously reported in AD brains [67]. This probably explains the divergent findings in AD lymphocytes in the recent cohort compared with the previous findings in AD patients varying in several parameters. Moreover, similar to our observation using PC12 cells transgenic for mutant human APP [68], AD lymphocytes react more susceptible in respect to MMP decrease and elevated apoptosis when they were stressed with inhibitors of complexes I (rotenone), III (antimycin), IV (sodium azide) and V (oligomycin) (Fig. 2). Lymphocytes were incubated for 24 h with the respective complex inhibitor and afterwards apoptosis and MMP were investigated. This effect was again restricted to the CD4+ fraction. Importantly, MCI patients show a similar pattern regarding the susceptibility to complexes I (Fig. 2a) and III (Fig. 2b) stress on MMP as AD patients. In contrast, MMP following sodium azide (VI; Fig. 2c) and oligomycin treatment (complex V; Fig. 2d) was only significantly reduced in AD lymphocytes and not in MCI. These defects on the levels of MMP and apoptosis were confirmed in a subset of AD patients using a high-resolution respiratory protocol established lately by our group [69]. Physiological substrate combinations were used to obtain mitochondrial bioenergetics approaching the most of physiological states in whole cells (Fig. 3). We compared mitochondrial respiration (oxidative phosphorylation (OXPHOS) capacity representing the whole electron transport chain composed of the four mitochondrial enzymes (complexes I to IV) and the F1F0ATP synthase in lymphocytes from six female AD patients with that of six age- and sex-matched controls. Notably, AD lymphocytes exhibited already a reduced endogenous basal rate of respiration (state 1) as well as a significant impairment of total OXPHOS capacity (Fig. 3a). In addition, the respiratory control ratio (RCR: coupled OXPHOS capacity (state3) divided by leak flux (state4)) which is an indicator of the coupling state of mitochondria was significantly decreased in AD lymphocytes (Fig. 3b), whereas mitochondrial mass was unchanged (Fig. 3c) confirming a functional deficit of AD lymphocytes to consume oxygen finally leading to failure in the maintenance in cellular energetics.
Basal level of apoptosis, MMP and ROS in Cd4+ lymphocytes and Cd4− lymphocytes in aged controls, MCI and AD patients. Basal levels of apoptosis are increased in MCI and AD patients compared with age-matched controls in CD4+ lymphocytes. No differences were seen in CD4− lymphocytes (unpaired t test ctl against MCI (*p < 0.05) and ctl against AD patients (**p < 0.01)). MMP was decreased in MCI and AD patients in CD4+ lymphocytes. Again no difference was obtained in CD4− lymphocytes (unpaired t test ctl against AD or MCI (*p < 0.05)). Superoxide anion levels were significantly reduced in AD patients compared with MCI and healthy age-matched controls (e). No changes were detected in CD4− lymphocytes (unpaired t test ctl against AD (***p < 0.001) and MCI against AD (+++p < 0.01))
Enhanced susceptibility of complexes I, III, IV and V in AD patients and MCI. MMP and apoptosis in CD4+ lymphocytes were measured in the presence of the complex I inhibitor rotenone (10 μM), the complex III inhibitor antimycin (10 μM), the complex IV inhibitor NaN3 (10 mM) and the complex V inhibitor oligomycin (10 μM). Complexes I (a) and III (b) showed a significantly enhanced vulnerability in apoptosis as well as in MMP in MCI and AD patients (unpaired t test, *p < 0.05; p < 0.01 ctl against MCI or AD). After the incubation with the inhibitors of complexes IV (c) and V (d), only MMP in AD patients was significantly reduced
Mitochondrial respiration in lymphocytes from AD patients and controls. O2 flux and O2 consumption were measured after addition of different agents: pyruvate/glutamate (glu/mal), ADP, FCCP and rotenone (rot). a Two-way ANOVA revealed a significant decrease of the total cellular respiration in AD cells compared with that of control (ctl) cells (group effect: AD versus control (p < 0.05)). Post-hoc analysis for single experimental conditions: **p < 0.01 AD vs. control cells. b Respiratory control ratio (RCR) represents the mitochondrial coupling state. RCR was significantly decreased in AD cells (unpaired t test, *p < 0.05). c Using MitoTracker Green FM (fluorescence units/1 × 106 cells), no change in mitochondrial mass was observed between cells from AD patients and controls. a–c Values represent the means ± SE from n = 6 subjects/group
Conclusions
In several studies, lymphocytes were shown to be a suitable cell model studying mitochondrial dysfunction. Increased basal apoptosis, elevated ROS levels, altered levels of antioxidant enzymes, elevated hydroxyl radical-induced DNA oxidation and increased mitochondrial susceptibility were found in AD patients compared with controls. Moreover, our new findings of substantial mitochondrial dysfunction in lymphocytes of AD and MCI patients without any Aß or Tau pathology underlines the relevance of this parameter for the complex scenario finally leading to the specific brain lesions in AD.
Materials and Methods
Human Subjects
Twenty-three patients (12 females and 11 males; mean age, 73.4 ± 10.6 years) with sporadic AD, 17 MCI patients (eight females and nine males; mean age, 66.9 ± 9.7 years) and 15 elderly non-demented controls (ten females and five males; mean age, 72.3 ± 9.3) were included in this study to measure apoptosis, MMP and ROS. To investigate mitochondrial respiration, six patients (six females; mean age, 80.3 ± 7.1) and six age-matched controls (six females; mean age, 79.0 ± 7.1) were enrolled in this study. Diagnosis of AD was achieved following the guidelines of the National Institute of Neurological and Communicative Disorders and Stroke-Alzheimer’s Disease and Related Disorders (NINCDS-ADRDA) and DSM IV criteria. Diagnosis of MCI was conducted according to the criteria of Petersen [70]. In the cohort to measure MMP, apoptosis and ROS levels, the MMSE for AD patients was 19.6 ± 6.6, for MCI patients 28.7 ± 1.6 and for aged controls 29.8 ± 0.4. For respiratory analysis, the MMSE was 18.8 ± 1.7 in the AD group and 29.8 ± 0.4 in the aged control group. All individuals were free of acute infections and in good physical condition. Subjects with pathological distribution of lymphocyte subpopulations in flow cytometric analysis were excluded from the study. In all three groups, chronic cardiovascular disease, dysfunction of the thyroid, diabetes and hypercholesterolemia were common diseases. None of the aged controls or MCI and AD patients received antioxidant treatment or psychotropic medication. The study was approved by the responsible Ethical Committee, and written informed consent from all subjects was received or, where appropriate, from their caregivers.
Isolation of Lymphocytes
Peripheral blood lymphocytes were separated from heparinised blood by centrifugation on Ficoll–Hypaque (Biocrom KG, Berlin, Germany) density gradient at 400×g for 30 min as described previously [32, 58]. The study was approved by the responsible Ethical Committee and written informed consent from all subjects was received, where appropriate, from their caregivers.
Fluorescence Activated Cytometry
Whole Blood Analysis
The surface-expressed receptors CD3, CD4, CD19, CD8, CD56þCD16, CD95 and HLA-DR were determined with the Simulset Kit™ (Becton Dickinson). Whole blood anticoagulated with EDTA was stained with the appropriate antibodies following the manufacturer’s manual. Briefly, whole blood was double stained with antibodies against leukocyte surface antigens. After incubation for 15–30 min, erythrocytes were lysed. The samples were washed twice with Cellwash™ (Becton Dickinson, Germany) and analysed by flow cytometry using Simulset™ software (BD). Forward and side angle-scattered light-gating excluded debris, granulocytes and monocytes. For each sample, 10,000 events were acquired.
Detection of Reactive Oxygen Species
ROS were measured with the fluorescence dye dihydroethidium (DHE). Upon oxidation, DHE forms ethidium that intercalates with DNA double strands in the cell. When stacked between the bases, the π-electrons of the dye interact with the π-electrons of the DNA bases, resulting in altered fluorescence properties. For basal levels of ROS, lymphocytes (1 Mio/ml) were incubated with DHE (5 μM) at 37 °C for 60 min, washed twice, and resuspended for flow-cytometric analysis with Becton–Dickinson (Heidelberg, Germany) FACS Calibur utilising CellQuest Pro software. A minimum of 8,000 events were recorded per single measurement. Cells were analysed immediately after staining and always kept on ice in the dark until measurement.
Detection of Apoptosis in Lymphocyte Subsets by Flow Cytometry
Apoptosis was measured using the actinomycin D analogue, 7-aminoactinomycin (7AAD; Molecular Probes, Leiden, The Netherlands) which is able to bind to the GC regions of the DNA. During the cell death process, the plasma membrane becomes permeable to the dye. Freshly isolated lymphocytes or 24-h cultured cells were triple stained with PE-conjugated anti-CD4 (clone SK3, PE labelled, FL-2 channel, Becton Dickinson, Heidelberg, Germany) antibody and the nuclear dye 7-AAD (FL-3 channel) as previously described [34]. Briefly, 1 ml of each antibody and 7-AAD (6 mM) were added to the 96-well plate for 15 min at room temperature in the dark. Cells were harvested, washed twice with PBS and kept in the dark before flow cytometry analysis (FACS Calibur) using Cellquest™ software (both Becton Dickinson, Heidelberg, Germany). A total of 10,000 individual nuclei per measurement were analysed in each experiment providing valid quantitative data. To investigate long term effects (24 h) of the different complex inhibitors (complex I rotenone, 10 μM; complex II TTFA, 500 μM; complex III antimycine, 10 μM; complex IV sodium azide, 10 mM; and complex V oligomycine, 10 μM) on apoptosis, lymphocytes were seeded at a density of 2.5 × 104 in 48-well plates and kept for 24 h at 37 °C/5 % CO2. Afterwards, lymphocytes were handled as described before.
Detection of Mitochondrial Membrane Potential
The MMP of lymphocytes was measured using the fluorescence dye rhodamine 123 (0.4 μM). For basal MMP, R123 was incubated for 15 min, washed twice, and resuspended for flow-cytometric analysis with Becton–Dickinson (Heidelberg, Germany) FACS Calibur utilising CellQuest Pro software. For long-term incubation, lymphocytes were plated at a density of 2.5 × 104 cells/well in a 48-well plate and kept at 37 °C/5 % CO2. Afterwards, lymphocytes were handled as described before.
Mitochondrial Respiration in Lymphocytes
Mitochondrial oxygen consumption was measured at 37 °C using an Oroboros Oxygraph-2 k system. Four millions of lymphocytes were added to 2 ml of a mitochondrial respiration medium containing 0.5 mM EGTA, 3 mM MgCl2, 60 mM K-lactobionate, 20 mM taurine, 10 mM KH2P04, 20 mM HEPES, 110 mM sucrose and 1 g/l BSA (pH 7.1). First, endogenous basal respiration of cells was measured (state). To measure the state 4 (=state 2) of the complex I, 10 mM glutamate and 2 mM malate were added and cells were permeabilised with 15 μg/ml digitonin. Afterwards, 2 mM ADP was added to measure state 3 respiration. The integrity of the mitochondrial membrane was checked through the addition of 10 μM cytochrome c. After determining coupled respiration, 0.8 μM FCCP (carbonyl cyanide p-(trifluoro-methoxy) phenyl-hydrazone) was added and respiration was measured in the absence of a proton gradient. In order to inhibit respiration 0.5 μM rotenone was added.
Mitochondrial Number/Mass
Mitochondrial number/mass was measured using the cell-permeable mitochondria-selective dye MitoTracker Green FM (Molecular Probes, Invitrogen, Lucerne, Switzerland) (400 nM, 15 min). Fluorescence was determined using a Fluoroskan Ascent FL multiplate reader (Labsystems) at 490 nm (excitation)/516 nm (emission).
Statistics
All data are means ± SEM. Statistical analysis was performed by unpaired Student’s t test or two-way ANOVA (PRISM 4, GraphPad software, San Diego, CA, USA). P values less than 0.05 were considered to be statistically significant.
References
Mattson MP, Magnus T (2006) Ageing and neuronal vulnerability. Nat Rev Neurosci 4:278–294
Balaban RS, Nemoto S, Finkel T (2005) Mitochondria, oxidants, and aging. Cell 4:483–495
Sastre J, Pallardo FV, de la Asuncion JG, Vina J (2000) Mitochondria, oxidative stress and aging. Free Radic Res 3:189–198
Floyd RA, Hensley K (2002) Oxidative stress in brain aging. Implications for therapeutics of neurodegenerative diseases. Neurobiol Aging 5:795–807
Onyango IG, Lu JH, Rodova M, Lezi E, Crafter AB, Swerdlow RH (2010) Regulation of neuron mitochondrial biogenesis and relevance to brain health. Biochim Biophys Acta 1:228–234
Marchi S, Giorgi C, Suski JM, Agnoletto C, Bononi A, Bonora M, De Marchi E, Missiroli S, Patergnani S, Poletti F et al (2012) Mitochondria-ros crosstalk in the control of cell death and aging. J Signal Transduct (in press)
Atamna H (2004) Heme, iron, and the mitochondrial decay of ageing. Ageing Res Rev 3:303–318
Mattson MP (2006) Neuronal life-and-death signaling, apoptosis, and neurodegenerative disorders. Antioxid Redox Signal 11–12:1997–2006
Leuner K, Schutt T, Kurz C, Eckert SH, Schiller C, Occhipinti A, Mai S, Jendrach M, Eckert GP, Kruse SE et al (2012) Mitochondrion-derived reactive oxygen species lead to enhanced amyloid beta formation. Antioxid Redox Signal 16(12):1421–1433
Hauptmann S, Scherping I, Drose S, Brandt U, Schulz KL, Jendrach M, Leuner K, Eckert A, Muller WE (2009) Mitochondrial dysfunction: an early event in Alzheimer pathology accumulates with age in AD transgenic mice. Neurobiol Aging 10:1574–1586
Bonda DJ, Wang X, Perry G, Nunomura A, Tabaton M, Zhu X, Smith MA (2010) Oxidative stress in Alzheimer disease: a possibility for prevention. Neuropharmacology 4–5:290–294
Reddy PH (2009) Role of mitochondria in neurodegenerative diseases: mitochondria as a therapeutic target in Alzheimer's disease. CNS Spectr 8(Suppl 7):8–13
Munch G, Schinzel R, Loske C, Wong A, Durany N, Li JJ, Vlassara H, Smith MA, Perry G, Riederer P (1998) Alzheimer’s disease–synergistic effects of glucose deficit, oxidative stress and advanced glycation endproducts. J Neural Transm 4–5:439–461
Haass C, Selkoe DJ (2007) Soluble protein oligomers in neurodegeneration: lessons from the Alzheimer's amyloid beta-peptide. Nat Rev Mol Cell Biol 2:101–112
Querfurth HW, LaFerla FM (2010) Alzheimer’s disease. N Engl J Med 4:329–344
Rhein V, Song X, Wiesner A, Ittner LM, Baysang G, Meier F, Ozmen L, Bluethmann H, Drose S, Brandt U et al (2009) Amyloid-beta and tau synergistically impair the oxidative phosphorylation system in triple transgenic Alzheimer's disease mice. Proc Natl Acad Sci U S A 47:20057–20062
David DC, Hauptmann S, Scherping I, Schuessel K, Keil U, Rizzu P, Ravid R, Drose S, Brandt U, Muller WE et al (2005) Proteomic and functional analyses reveal a mitochondrial dysfunction in P301L Tau transgenic mice. J Biol Chem 25:23802–23814
Gibson GE, Huang HM (2005) Oxidative stress in Alzheimer’s disease. Neurobiol Aging 5:575–578
Ankarcrona M, Winblad B (2005) Biomarkers for apoptosis in Alzheimer’s disease. Int J Geriatr Psychiatry 2:101–105
Leuner K, Pantel J, Frey C, Schindowski K, Schulz K, Wegat T, Maurer K, Eckert A, Muller WE (2007) Enhanced apoptosis, oxidative stress and mitochondrial dysfunction in lymphocytes as potential biomarkers for Alzheimer’s disease. J Neural Transm Suppl 72:207–215
Sultana R, Mecocci P, Mangialasche F, Cecchetti R, Baglioni M, Butterfield DA (2011) Increased protein and lipid oxidative damage in mitochondria isolated from lymphocytes from patients with Alzheimer’s disease: insights into the role of oxidative stress in Alzheimer's disease and initial investigations into a potential biomarker for this dementing disorder. J Alzheimers Dis 1:77–84
Cecchi C, Fiorillo C, Nassi P, Liguri G, Sorbi S, Latorraca S, Bagnoli S (2002) Oxidative injury and antioxidant defences in peripheral cells from Alzheimer patients. Neurobiol Aging (Suppl 1):S513–S513
Moreira PI, Harris PL, Zhu X, Santos MS, Oliveira CR, Smith MA, Perry G (2007) Lipoic acid and N-acetyl cysteine decrease mitochondrial-related oxidative stress in Alzheimer disease patient fibroblasts. J Alzheimers Dis 2:195–206
Naderi J, Lopez C, Pandey S (2006) Chronically increased oxidative stress in fibroblasts from Alzheimer’s disease patients causes early senescence and renders resistance to apoptosis by oxidative stress. Mech Ageing Dev 1:25–35
Kawamoto EM, Munhoz CD, Glezer I, Bahia VS, Caramelli P, Nitrini R, Gorjao R, Curi R, Scavone C, Marcourakis T (2005) Oxidative state in platelets and erythrocytes in aging and Alzheimer’s disease. Neurobiol Aging 6:857–864
Valla J, Schneider L, Niedzielko T, Coon KD, Caselli R, Sabbagh MN, Ahern GL, Baxter L, Alexander G, Walker DG et al (2006) Impaired platelet mitochondrial activity in Alzheimer’s disease and mild cognitive impairment. Mitochondrion 6:323–330
Shi C, Guo K, Yew DT, Yao Z, Forster EL, Wang H, Xu J (2008) Effects of ageing and Alzheimer’s disease on mitochondrial function of human platelets. Exp Gerontol 6:589–594
Casoli T, Di Stefano G, Giorgetti B, Balietti M, Recchioni R, Moroni F, Marcheselli F, Bernardini G, Fattoretti P, Bertoni-Freddari C (2008) Platelet as a physiological model to investigate apoptotic mechanisms in Alzheimer beta-amyloid peptide production. Mech Ageing Dev 3:154–162
Cristalli DO, Arnal N, Marra FA, de Alaniz MJ, Marra CA (2012) Peripheral markers in neurodegenerative patients and their first-degree relatives. J Neurol Sci 1–2:48–56
Torres LL, Quaglio NB, de Souza GT, Garcia RT, Dati LM, Moreira WL, Loureiro AP, Souza-Talarico JN, Smid J, Porto CS et al (2011) Peripheral oxidative stress biomarkers in mild cognitive impairment and Alzheimer’s disease. J Alzheimers Dis 1:59–68
Baldeiras I, Santana I, Proenca MT, Garrucho MH, Pascoal R, Rodrigues A, Duro D, Oliveira CR (2008) Peripheral oxidative damage in mild cognitive impairment and mild Alzheimer’s disease. J Alzheimers Dis 1:117–128
Schindowski K, Eckert A, Peters J, Gorriz C, Schramm U, Weinandi T, Maurer K, Frolich L, Muller WE (2007) Increased T-cell reactivity and elevated levels of CD8+ memory T-cells in Alzheimer's disease-patients and T-cell hyporeactivity in an Alzheimer’s disease-mouse model: implications for immunotherapy. Neuromol Med 4:340–354
Huang HM, Fowler C, Xu H, Zhang H, Gibson GE (2005) Mitochondrial function in fibroblasts with aging in culture and/or Alzheimer’s disease. Neurobiol Aging 6:839–848
Schindowski K, Kratzsch T, Peters J, Steiner B, Leutner S, Touchet N, Maurer K, Czech C, Pradier L, Frolich L et al (2003) Impact of aging: sporadic, and genetic risk factors on vulnerability to apoptosis in Alzheimer’s disease. Neuromol Med 3:161–178
Drouet M, Lauthier F, Charmes JP, Sauvage P, Ratinaud MH (1999) Age-associated changes in mitochondrial parameters on peripheral human lymphocytes. Exp Gerontol 7:843–852
Kadioglu E, Sardas S, Aslan S, Isik E, Esat KA (2004) Detection of oxidative DNA damage in lymphocytes of patients with Alzheimer’s disease. Biomarkers 2:203–209
Leutner S, Schindowski K, Frolich L, Maurer K, Kratzsch T, Eckert A, Muller WE (2005) Enhanced ROS-generation in lymphocytes from Alzheimer’s patients. Pharmacopsychiatry 6:312–315
De Leo ME, Borrello S, Passantino M, Palazzotti B, Mordente A, Daniele A, Filippini V, Galeotti T, Masullo C (1998) Oxidative stress and overexpression of manganese superoxide dismutase in patients with Alzheimer’s disease. Neurosci Lett 3:173–176
Morocz M, Kalman J, Juhasz A, Sinko I, McGlynn AP, Downes CS, Janka Z, Rasko I (2002) Elevated levels of oxidative DNA damage in lymphocytes from patients with Alzheimer’s disease. Neurobiol Aging 1:47–53
Cecchi C, Fiorillo C, Sorbi S, Latorraca S, Nacmias B, Bagnoli S, Nassi P, Liguri G (2002) Oxidative stress and reduced antioxidant defenses in peripheral cells from familial Alzheimer’s patients. Free Radic Biol Med 10:1372–1379
Mecocci P, Cherubini A, Senin U (1997) Increased oxidative damage in lymphocytes of Alzheimer’s disease patients. J Am Geriatr Soc 12:1536–1537
Mecocci P, Polidori MC, Cherubini A, Ingegni T, Mattioli P, Catani M, Rinaldi P, Cecchetti R, Stahl W, Senin U et al (2002) Lymphocyte oxidative DNA damage and plasma antioxidants in Alzheimer disease. Arch Neurol 5:794–798
Migliore L, Fontana I, Trippi F, Colognato R, Coppede F, Tognoni G, Nucciarone B, Siciliano G (2005) Oxidative DNA damage in peripheral leukocytes of mild cognitive impairment and AD patients. Neurobiol Aging 5:567–573
Straface E, Matarrese P, Gambardella L, Vona R, Sgadari A, Silveri MC, Malorni W (2005) Oxidative imbalance and cathepsin D changes as peripheral blood biomarkers of Alzheimer disease: a pilot study. FEBS Lett 13:2759–2766
Dezor M, Dorszewska J, Florczak J, Kempisty B, Jaroszewska-Kolecka J, Rozycka A, Polrolniczak A, Bugaj R, Jagodzinski PP, Kozubski W (2011) Expression of 8-oxoguanine DNA glycosylase 1 (OGG1) and the level of p53 and TNF-alpha proteins in peripheral lymphocytes of patients with Alzheimer’s disease. Folia Neuropathol 2:123–131
Cecchi C, Latorraca S, Sorbi S, Iantomasi T, Favilli F, Vincenzini MT, Liguri G (1999) Gluthatione level is altered in lymphoblasts from patients with familial Alzheimer’s disease. Neurosci Lett 2:152–154
Schuessel K, Frey C, Jourdan C, Keil U, Weber CC, Muller-Spahn F, Muller WE, Eckert A (2006) Aging sensitizes toward ROS formation and lipid peroxidation in PS1M146L transgenic mice. Free Radic Biol Med 5:850–862
Eckert A, Schindowski K, Leutner S, Luckhaus C, Touchet N, Czech C, Muller WE (2001) Alzheimer’s disease-like alterations in peripheral cells from presenilin-1 transgenic mice. Neurobiol Dis 2:331–342
Schindowski K, Leutner S, Muller WE, Eckert A (2000) Age-related changes of apoptotic cell death in human lymphocytes. Neurobiol Aging 5:661–670
Schindowski K, Peters J, Gorriz C, Schramm U, Weinandi T, Leutner S, Maurer K, Frolich L, Muller WE, Eckert A (2006) Apoptosis of CD4+ T and natural killer cells in Alzheimer’s disease. Pharmacopsychiatry 6:220–228
Eckert A, Keil U, Marques CA, Bonert A, Frey C, Schussel K, Muller WE (2003) Mitochondrial dysfunction, apoptotic cell death, and Alzheimer’s disease. Biochem Pharmacol 8:1627–1634
Eckert A, Oster M, Zerfass R, Hennerici M, Muller WE (2001) Elevated levels of fragmented DNA nucleosomes in native and activated lymphocytes indicate an enhanced sensitivity to apoptosis in sporadic Alzheimer’s disease—specific differences to vascular dementia. Demen Geriatr Cogn Disord 2:98–105
Eckert A, Steiner B, Marques C, Leutz S, Romig H, Haass C, Muller WE (2001) Elevated vulnerability to oxidative stress-induced cell death and activation of caspase-3 by the Swedish amyloid precursor protein mutation. J Neurosci Res 2:183–192
Gatta L, Cardinale A, Wannenes F, Consoli C, Armani A, Molinari F, Mammi C, Stocchi F, Torti M, Rosano GM et al (2009) Peripheral blood mononuclear cells from mild cognitive impairment patients show deregulation of Bax and Sod1 mRNAs. Neurosci Lett 1:36–40
Frey C, Bonert A, Kratzsch T, Rexroth G, Rosch W, Muller-Spahn F, Maurer K, Muller WE, Eckert A (2006) Apolipoprotein E epsilon 4 is associated with an increased vulnerability to cell death in Alzheimer’s disease. J Neural Transm 11:1753–1761
Tacconi S, Perri R, Balestrieri E, Grelli S, Bernardini S, Annichiarico R, Mastino A, Caltagirone C, Macchi B (2004) Increased caspase activation in peripheral blood mononuclear cells of patients with Alzheimer’s disease. Exp Neurol 1:254–262
Lombardi VR, Fernandez-Novoa L, Etcheverria I, Seoane S, Cacabelos R (2004) Association between APOE epsilon4 allele and increased expression of CD95 on T cells from patients with Alzheimer’s disease. Methods Find Exp Clin Pharmacol 7:523–529
Schindowski K, Frohlich L, Maurer K, Muller WE, Eckert A (2002) Age-related impairment of human T lymphocytes’ activation: specific differences between CD4(+) and CD8(+) subsets. Mech Ageing Develop 4:375–390
Huang YD (2006) Apolipoprotein E and Alzheimer disease. Neurology 66:S79–S85
Parshad R, Sanford KK, Price FM, Melnick LK, Nee LE, Schapiro MB, Tarone RE, Robbins JH (1996) Fluorescent light-induced chromatid breaks distinguish Alzheimer disease cells from normal cells in tissue culture. Proc Natl Acad Sci U S A 10:5146–5150
Cardoso SM, Proenca MT, Santos S, Santana I, Oliveira CR (2004) Cytochrome c oxidase is decreased in Alzheimer’s disease platelets. Neurobiol Aging 1:105–110
Bosetti F, Brizzi F, Barogi S, Mancuso M, Siciliano G, Tendi EA, Murri L, Rapoport SI, Solaini G (2002) Cytochrome c oxidase and mitochondrial F1F0-ATPase (ATP synthase) activities in platelets and brain from patients with Alzheimer’s disease. Neurobiol Aging 3:371–376
Mancuso M, Filosto M, Bosetti F, Ceravolo R, Rocchi A, Tognoni G, Manca ML, Solaini G, Siciliano G, Murri L (2003) Decreased platelet cytochrome c oxidase activity is accompanied by increased blood lactate concentration during exercise in patients with Alzheimer disease. Exp Neurol 2:421–426
Molina JA, deBustos F, JimenezJimenez FJ, BenitoLeon J, Gasalla T, OrtiPareja M, Vela L, Bermejo F, Martin MA, Campos Y et al (1997) Respiratory chain enzyme activities in isolated mitochondria of lymphocytes from patients with Alzheimer’s disease. Neurology 3:636–638
Casademont J, Miro O, Rodriguez-Santiago B, Viedma P, Blesa R, Cardellach F (2003) Cholinesterase inhibitor rivastigmine enhance the mitochondrial electron transport chain in lymphocytes of patients with Alzheimer’s disease. J Neurol Sci 1:23–26
Culmsee C, Landshamer S (2006) Molecular insights into mechanisms of the cell death program: role in the progression of neurodegenerative disorders. Curr Alzheimer Res 4:269–283
Schuessel K, Leutner S, Cairns NJ, Muller WE, Eckert A (2004) Impact of gender on upregulation of antioxidant defence mechanisms in Alzheimer’s disease brain. J Neural Transm 9:1167–1182
Keil U, Bonert A, Marques CA, Scherping I, Weyermann J, Strosznajder JB, Muller-Spahn F, Haass C, Czech C, Pradier L et al (2004) Amyloid beta-induced changes in nitric oxide production and mitochondrial activity lead to apoptosis. J Biol Chem 48:50310–50320
Rhein V, Baysang G, Rao S, Meier F, Bonert A, Muller-Spahn F, Eckert A (2009) Amyloid-beta leads to impaired cellular respiration, energy production and mitochondrial electron chain complex activities in human neuroblastoma cells. Cell Mol Neurobiol 6–7:1063–1071
Petersen RC (2004) Mild cognitive impairment as a diagnostic entity. J Intern Med 3:183–194
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Leuner, K., Schulz, K., Schütt, T. et al. Peripheral Mitochondrial Dysfunction in Alzheimer’s Disease: Focus on Lymphocytes. Mol Neurobiol 46, 194–204 (2012). https://doi.org/10.1007/s12035-012-8300-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-012-8300-y