Abstract
This study aimed to identify clinicopathological factors associated with the outcome of elderly patients with gastric cancer (GC), and to construct a nomogram for individual risk prediction. Tumor characteristics of 143 patients aged ≥ 80 years underwent surgery for GC were collected and analyzed by uni- and multivariate analyses. A prognostic nomogram was constructed using the factors which resulted to be significantly associated with overall survival. Discrimination of nomogram was tested by Kaplan–Meier (KM) curves and boxplots. With a median follow up of 18.37 months, overall 1-year survival rate was 51% and it was 60 and 40% for older and younger than 83 years, respectively (P = 0.003). Univariate analysis indicated that age (P = 0.008), pre-operatory performance status (P < 0.001), depth of invasion (P = 0.007), lymph nodes involvement (P < 0.001), and residual tumor (P < 0.001) were significant prognostic factors. Based on these variables, a nomogram to predict 3, 6, 12, and 24 months survival probability after GC surgery was developed. KM and boxplots according to the range of nomogram total points highlighted the appropriateness of distinguish the patients’ survival in all the subgroups. Moreover, this nomogram exhibited superior prognostic discrimination between intermediate stages (II–III) than AJCC-TNM classification. This study showed that after good surgical selection, the prognosis of elderly GC patients may be influenced by several clinicopathological factors. Therefore, a predictive nomogram to distinguish more accurately fit patients may allow physicians to individualize treatments and to detect those patients who may benefit from an intensive multidisciplinary approach.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The prevalence of elderly patients with gastric cancer (GC) is considerably increased in Europe with the aging of population [1]. Since elderly patients are usually underrepresented or excluded from randomized clinical trials, data about the prognosis of GC patients aged over 80 years old, are still poor. Previous studies on GC treatment have reported good results with surgery [2, 3] and compared outcomes between elderly and younger patients [4]. Meanwhile, stratified analyses suggested that older age, maybe due to the higher risk of postoperative complications, was an independent prognostic factor [5, 6]. In view of the rising proportion of GC diagnosis in the elderly, the authors’ interest to identify more accurately prognostic factors is considerably increasing. Regardless of age, few nomograms have been developed to predict survival of GC patients [7,8,9]. However, nomograms predicting survival properly in elderly GC patients are still lacking.
The present study aimed to compare clinicopathological parameters and post-surgical outcomes of GC patients among our old population (≥ 80 years) who perform surgery followed by or not adjuvant therapy and whose data are collected in our medical record database. Finally, we set out to identify independent prognostic factors and develop a nomogram to predict survival after surgery.
Materials and Methods
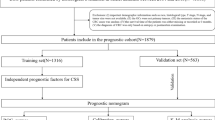
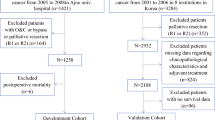
Between January 1, 2007 and December 31, 2016, among patients who underwent gastric cancer surgery at the ASST of Cremona, Hospital of Cremona and Sant’Andrea Hospital of Rome, we collected data for 143 patients aged ≥ 80 years whose clinicopathological parameters were available. This data set included age, sex, performance status (PS) sec. Eastern Cooperative Oncology Group (ECOG), pathologic characteristics location, histology, grading, number of examined lymph nodes, depth of invasion (T), nodes involvement (N), as well as stage according to TNM-AJCC, R (presence of macroscopic or microscopic tumor residual after surgery), D1/2 lymphadenectomy, adjuvant chemo- and/or radio-therapy, and follow up data (follow up duration and survival). The location of the tumor was categorized as upper third (including esophagogastric junction adenocarcinoma), middle third, or lower third by the center of the lesion. Follow-up data were collected from patients medical records. The follow up duration was measured from the time of surgery to the last follow-up date, and the information about the survival status was collected. Clinicopathological parameters and oncologic outcomes were retrospectively reviewed for statistical analysis. The study was performed in accordance to the declaration of Helsinki in its latest version and was approved by our independent ethics committee (Protocol number 16821/17). Prior to surgery, all patients gave written informed consent to use their data exclusively by researchers and for scientific purposes.
Statistical analysis
Categorical variables are presented as number with percentage in descriptive tables, and they were compared with Fisher’s exact test or Pearson’s χ2 test. Patients’ overall survival (OS) was analyzed using Kaplan–Meier (KM) method and log-rank tests. Prognostic clinicopathological factors were analyzed by univariate and multivariate Cox proportional hazards regression analysis. Variables that were deemed of potential importance to the univariate analysis (P > 0.1) were included in the multivariate analysis. Results for significant prognostic factors were expressed as the hazard ratio for each category and its 95% confidence interval. A P < 0.05 was considered statistically significant. Statistical analyses were performed using R-package software.
Construction and validation of the nomogram
Significant prognostic factors identified by the Cox PH regression model were used to construct a nomogram for predicting 3, 6, 12, and 24 months of OS after gastric surgery. Discrimination was evaluated using a concordance index and tested by KM curves. The Pearson’s product-moment correlation has been calculated from total points and stage. According to KM method, survival curves of both AJCC-TNM stages and nomogram ranges (4 groups based on cutoff calculated using the 25th, 50th, and 75th percentile) have been calculated. Boxplots of survival months against stages and the range of total points have been also calculated.
Results
One-hundred forty-three GC patients over 80 years old were enrolled in this study. Overall, the median age was 83 years (range 80–92). Most of the patients were male, showed a good pre-operatory performance status (PS sec. ECOG = 1 in 50.4% of cases), and were affected with differentiated (46.9%), intestinal (67.1%) locally advanced (II and III stage in 32 and 44% of patients, respectively) GC. Other descriptive clinicopathological parameters are reported in Table 1. The median follow-up period after gastric resection was 18.37 months (range 0, 66–107, 43 months).
Overall survival
All 143 treated patients were assessable for OS. At the time of the analysis, 140 (97,9%) patients had died. The median OS was 12.27 months (95% CI 8,50–16,03 months). As showed in KM curves, patients aged > 83 years old, with an ECOG PS before surgery = 3, T3–4, N2–3, and R1 pathological factors, demonstrated a significantly worse OS (Fig. 1).
Based on univariate and multivariate analysis, the hazard ratios of the examined variables were reported in Table 2. At the univariate analysis age, T, N, R, and ECOG PS before surgery, were significantly associated with OS; while sex, location, histology, grading, lymphadenectomy, and adjuvant treatment (chemotherapy ± radiotherapy) were not found to be significant. Multivariate Cox analysis revealed that age, T, N, R, and pre-operatory ECOG-PS were significantly associated with OS (Table 2).
Nomogram analysis
Based on the estimated regression coefficients in the Cox analysis, a prognostic nomogram for elderly GC patient was developed to assign their probability of survival at 3, 6, 12, and 24 months after surgery (Fig. 2). As showed in the nomogram, patients having > 83 years, T-stage ≥ 3, R = 1, N ≥ 1, and a pre-operatory ECOG PS = 3 have a lower survival probability (Fig. 2).
KM curves according the range of calculated total points using the nomogram (range I and IV are associated to a poor and good prognosis, respectively) show a strong correlation (P = 0.000115) (Fig. 3a) as well as KM curves according the AJCC-TNM stage (P = 0.000212) (Fig. 3b).
AJCC-TNM staging and nomogram ranges show a good correlation (cor =− 0.7783598, Pearson’s product-moment correlation, P value < 2.2e-16). However, the OS curves at 24 months seems to be more clearly separated in the box plot for nomogram (Fig. 4a) according to the investigated quartiles (i.e., ranges) than AJCC-TNM staging in which the outcome of intermediate stages (II and III) appeared to be similar at 24 months (Fig. 4b).
Discussion
Most of data about elderly GC patients comes from Asiatic retrospective studies. However, in Europe, with the increasing of life expectancy, the diagnosis of GC in elderly patients occur more frequently. However, few data are published concerning GC in elderly, due to the rigorous selection and under representation of the elderly in clinical trials. Therefore, the identification of definite prognostic factors that may help physician in the treatment’s choice, could be very useful.
In this study, we defined our elderly group as patients aged over 80 years old and, analyzing their clinicopathological factors, a nomogram predicting survival has been developed.
By the Munich Cancer Registry analysis, the 5-year relative survival was 23% for GC patients aged ≥80 years [10]. In our study, the survival rate was 50 and 30% at 1 and 3-year, respectively. The increase of age, depth of invasion, lymph-nodes and/or surgical margin involvement, and the pre-operatory ECOCG PS was found to be independent prognostic factors of survival. According to the score given to each prognostic variable, a nomogram allowing to predict the probability of survival at 3, 6, 12, and 24 months after surgery, for elderly GC patients, was constructed.
In a retrospective analysis on 113 GC patients of age 85 and older, limited lymphadenectomy, cT3-4, pT3-4, pN+, stage, and positive venous invasion were identified as significantly prognostic factors of worse survival [11]. However, only advanced pT and limited lymphadenectomy resulted to be independent prognostic factors in the multivariate analysis (HR 4.68, 95% CI 1.29–20.7, P = 0.02 and HR 2.19, 95% CI 1.00–4.97, P = 0.05, respectively).
As reported in literature [5, 12], clinicopathological features of GC in elderly patients are distinct characteristics. Indeed, GC of the upper third of the stomach, the differentiated histology and less-invasive surgery were reported in the most of cases with advancing age. Accordingly, in the present study, 62.6 and 65.7% of D1 lymphadenectomy and differentiated histology were reported, respectively.
As described in other studies [5, 11, 13] for elderly patients, a limited lymphadenectomy was performed more frequently than D2 lymphadenectomy, regardless of clinical stage. Contrary to stage II/III, the leading cause of death in stage I GC was non-cancer specific death, and so a limited lymphadenectomy or less-invasive surgery may be eligible for earlier stage [3]. Moreover, the survival rate of the elderly in stage II/III resulted to be slightly low [14, 15] or similar [3] compared to that of younger GC patients. Therefore, a radical lymphadenectomy was expected to improve survival of locally advanced GC in elderly patients [2]. However, the definitive indication of radical versus limited lymphadenectomy is not determined [16, 17] and the increasing of post-operative complications after surgery influence survival [18,19,20].
Data about type of surgical gastric resection are also controversy [21, 22]. A previous study [21] on a small sample of older than 70 GC patients suggests that gastrectomy can be carried out safely in elderly patients. However, in the elderly, according to the study of Pisanu et al., surgical strategies must be modulated mostly on the bases of comorbidity and future quality of life [22]. So, a subtotal gastrectomy rather than total gastrectomy should be the procedure of choice.
Liang et al. study [5] compared the common clinicopathological characteristics and surgical outcome among three aged-groups: elderly patients (≥ 70 years, 273 patients), middle-aged (50–69 years), and younger patients (< 50 years). Among elderly patients, adjuvant chemotherapy, consisted of 5-fluorouracil, leucovorin, and oxaliplatin (FOLFOX-6), was done only in 36 (13.2%) patients according to tumor stage, clinical condition, and willingness of the patient. With a median follow-up of 26 months, elderly patients demonstrated a significantly lower 5-year OS rate than the other two groups (22%, vs. 36.6% vs. 38% in elderly, middle-aged, and younger, respectively). In this study, R, pT4, lymph node metastasis, M1, and sex were independent prognostic factors in the multivariate analysis for OS.
In a more recent study [20], the above-mentioned pathological factors plus clinical PS per anesthesiologists-physical status (ASA-PS) score and postoperative complications were identified as independent prognostic factors for both OS and disease specific survival.
Another Japanese retrospective analysis [23] on GC patients who underwent surgery, including patients aged ≥80 years, showed no significant differences in sex, body mass index, length of hospital stay, depth of invasion, nodal metastasis, histologic type, or tumor size between young patients (< 80 years old) versus older ones. Both postoperative morbidity and mortality did not differ between the two groups, too. However, this study was conducted in a limited number of 32 (7% of the entire study population) elderly patients, and so the results has not showed much relevance.
Finally, Pak et al. study [24], including patients with advanced GC stage and treated with different modality, demonstrated that conservative treatment in the elderly correlated with poorer survival (HR 3.57, 95% 2.37–5.38) compared to surgical resection or chemotherapy.
However, no data are so strong to reach final conclusions. Moreover, the role of adjuvant chemotherapy in elderly GC patients is still debuted. Surely, higher number of comorbidities and the age-related clinical status of older patients may increase the incidence of chemotherapy-related toxicity and the worsening of quality of life compared with younger patients.
Our findings are consistent with these reports and by selecting pT, pN, R, and ECOG PS as significant prognostic factors, a useful nomogram to predict survival at 3, 6, 12 e 24 months was developed.
Patients comorbidities were not examined for this study as obviously various comorbidities affected those elderly population. Moreover, the diversity of comorbidity makes difficult to categorize variables for nomogram construction. However, since patients affected with other severe malignancies were excluded from the analysis, the impact of comorbidity on survival should result to be minimal.
Taking in to account the explained literature data, it is reinforced the need to identify among those elderly GC patients, who show an outcome like to the younger, potentially candidate for more radical treatment and adjuvant chemotherapy.
Therefore, a nomogram that accurately predicts survival of elderly GC patients may be a useful chance to optimize therapeutic choice for such fragile patient population in each stage of disease and to prevent post-operative death. Our nomogram may be a useful tool to avoid unnecessary treatment for patients with more than one adverse prognostic factor and with a total point < 137 (range I and II) (survival probability at 1 year around 20%). But it may also be used to recognize patients with better prognosis (range III and IV) who are possible candidates to adjuvant chemotherapy.
Conclusions
The distinguishing characteristics and prognosis of elderly patients underlines the required identification of independent predictors of survival to optimize the treatment’s physician choice for GC elderly patients. Moreover, none clinicopathological factor alone may be considered sufficient to withhold curative treatment for elderly GC patients. Therefore, we developed a nomogram providing an individualized prediction of survival for older patients with 1–4 examined prognostic factors (pT, pN, R, and pre-operatory ECOG PS).
As we have described, this nomogram could be useful to detect those older patients with a better survival and who may benefit from an intensive multidisciplinary treatment. However, for a generalized use of this nomogram in elderly patients affected with GC and underwent surgery, a validation by a wider cohort is required.
References
Population structure and ageing - Statistics Explained, http://ec.europa.eu/eurostat/statistics-explained/index.php/Population_structure_and_ageing.
Endo S, Dousei T, Yoshikawa Y, Hatanaka N, Kamiike W, Nishijima J. Prognosis of gastric carcinoma patients aged 85 years or older who underwent surgery or who received best supportive care only. Int J Clin Oncol. 2013;18(6):1014–9.
Endo S, Yoshikawa Y, Hatanaka N, Tominaga H, Shimizu Y, Hiraoka K, Nishitani A, Irei T, Nakashima S, Park M-H, Takahashi H, Wakahara M, Kamiike W. Treatment for gastric carcinoma in the oldest old patients. Gastric Cancer. 2011;14(2):139–43.
Fujimoto S, Takahashi M, Ohkubo H, Mutou T, Kure M, Masaoka H, Kobayashi K. Comparative clinicopathologic features of early gastric cancer in young and older patients. Surgery. 1994;115(4):516–20.
Liang Y-X, Deng J-Y, Guo H-H, Ding X-W, Wang X-N, Wang B-G, Zhang L, Liang H. Characteristics and prognosis of gastric cancer in patients aged ≥ 70 years. World J Gastroenterol. 2013;19(39):6568.
Song P, Wu L, Jiang B, Liu Z, Cao K, Guan W. Age-specific effects on the prognosis after surgery for gastric cancer: a SEER population-based analysis. Oncotarget. 2016;7(30):48614–24.
Kim Y, Spolverato G, Ejaz A, Squires MH, Poultsides G, Fields RC, Bloomston M, Weber SM, Votanopoulos K, Acher AW, Jin LX, Hawkins WG, Schmidt C, Kooby D, Worhunsky D, Saunders N, Levine EA, Cho CS, Maithel SK, Pawlik TM. A nomogram to predict overall survival and disease-free survival after curative resection of gastric adenocarcinoma. Ann Surg Oncol. 2015;22(6):1828–35.
Han D-S, Suh Y-S, Kong S-H, Lee H-J, Choi Y, Aikou S, Sano T, Park B-J, Kim W-H, Yang H-K. Nomogram predicting long-term survival after d2 gastrectomy for gastric cancer. J Clin Oncol. 2012;30(31):3834–40.
Muneoka Y, Akazawa K, Ishikawa T, Ichikawa H, Nashimoto A, Yabusaki H, Tanaka N, Kosugi S-I, Wakai T. Nomogram for 5-year relapse-free survival of a patient with advanced gastric cancer after surgery. Int J Surg. 2016;35:153–9.
Schlesinger-Raab A, Mihaljevic AL, Egert S, Emeny R, Jauch K-W, Kleeff J, Novotny A, Nüssler NC, Rottmann M, Schepp W, Schmitt W, Schubert-Fritschle G, Weber B, Schuhmacher C, Engel J. Outcome of gastric cancer in the elderly: a population-based evaluation of the Munich Cancer Registry. Gastric Cancer. 2016;19(3):713–22.
Konishi H, Ichikawa D, Itoh H, Fukuda K, Kakihara N, Takemura M, Okugawa K, Uchiyama K, Nakata M, Nishi H, Kosuga T, Komatsu S, Okamoto K, Otsuji E. Surgery for gastric cancer patients of age 85 and older: multicenter survey. World J Gastroenterol. 2017;23(7):1215.
Saif MW, Makrilia N, Zalonis A, Merikas M, Syrigos K. Gastric cancer in the elderly: an overview. Eur J Surg Oncol. 2010;36(8):709–17.
Schwarz RE, Smith DD. Clinical impact of lymphadenectomy extent in resectable gastric cancer of advanced stage. Ann Surg Oncol. 2007;14(2):317–28.
Sun DS, Jeon EK, Won HS, Park JC, Shim BY, Park SY, Hong YS, Kim HK, Ko YH. Outcomes in elderly patients treated with a single-agent or combination regimen as first-line chemotherapy for recurrent or metastatic gastric cancer. Gastric Cancer. 2015;18(3):644–52.
Desai AM, Lichtman SM. Systemic therapy of non-colorectal gastrointestinal malignancies in the elderly. Cancer Biol Med. 2015;12(4):284–91.
Kwon IG, Cho I, Guner A, Kim H, Noh SH, Hyung WJ. Minimally invasive surgery as a treatment option for gastric cancer in the elderly: comparison with open surgery for patients 80 years and older. Surg Endosc. 2015;29(8):2321–30.
Ruspi L, Galli F, Pappalardo V, Inversini D, Martignoni F, Boni L, Dionigi G, Rausei S. “Lymphadenectomy in elderly/high risk patients: should it be different?”. Transl Gastroenterol Hepatol. 2017;2:5.
Orsenigo E, Tomajer V, Di Palo S, Carlucci M, Vignali A, Tamburini A, Staudacher C. Impact of age on postoperative outcomes in 1118 gastric cancer patients undergoing surgical treatment. Gastric Cancer. 2007;10(1):39–44.
Eguchi T, Fujii M, Takayama T. Mortality for gastric cancer in elderly patients. J Surg Oncol. 2003;84(3):132–6.
Ueno D, Matsumoto H, Kubota H, Higashida M, Akiyama T, Shiotani A, Hirai T. Prognostic factors for gastrectomy in elderly patients with gastric cancer. World J Surg Oncol. 2017;15(1):59.
Saidi RF, Bell JL, Dudrick PS. Surgical resection for gastric cancer in elderly patients: is there a difference in outcome? J Surg Res. 2004;118(1):15–20.
Pisanu A, Montisci A, Piu S, Uccheddu A. Curative surgery for gastric cancer in the elderly: treatment decisions, surgical morbidity, mortality, prognosis and quality of life. Tumori. 2007;93(5):478–84.
Kim MS, Kim S. Outcome of gastric cancer surgery in elderly patients. J Gastric Cancer. 2016;16(4):254–9.
Pak LM, Wang J. The appropriate treatment for elderly gastric cancer patients. Art Surg. 2017;1:4.
Funding
This research did not receive any specific Grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors report no conflicts of interest.
Rights and permissions
About this article
Cite this article
Roberto, M., Botticelli, A., Strigari, L. et al. Prognosis of elderly gastric cancer patients after surgery: a nomogram to predict survival. Med Oncol 35, 111 (2018). https://doi.org/10.1007/s12032-018-1166-8
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12032-018-1166-8