Abstract
Increasing evidence underscores the strong, rapid, and sustained antidepressant properties of ketamine with a good tolerability profile in patients with depression; however, the underlying mechanisms are not fully elucidated. Neuregulin 1 (NRG1) is a bipolar disorder susceptibility gene and a biomarker of major depressive disorder, which regulates pyramidal neuron activity via ErbB4 in parvalbumin interneurons. Moreover, NRG1-ErbB4 signaling is reported to play a key role in the modulation of synaptic plasticity through regulating the neurotransmission. We therefore hypothesized that hypofunction of NRG1-ErbB4 signaling in parvalbumin interneurons is involved in the process of ketamine exerting rapid antidepressant actions in rats subjected to the forced swimming test (FST). The results showed that ketamine reduced the immobility time and latency to feed of rats receiving the FST, downregulated the levels of NRG1, phosphorylated ErbB4 (p-ErbB4), parvalbumin, 67-kDA isoform of glutamic acid decarboxylase (GAD67), gamma-aminobutyric acid (GABA), and upregulated the levels of glutamate in the rat prefrontal cortex and hippocampus. Pretreatment with NRG1 abolished both ketamine’s antidepressant effects and ketamine-induced reduction in p-ErbB4, parvalbumin, GAD67, and GABA levels and increase in glutamate levels. These results suggest that the downregulation of NRG1-ErbB4 signaling in parvalbumin interneurons in the rat brain may be a mechanism underlying ketamine’s antidepressant properties.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Depression represents one of the most disabling illnesses worldwide with a prevalence of approximately 17 % (Kessler et al. 2003). However, current available antidepressant drugs display relatively low efficacy with low-remission rates and time lag for treatment responses (Rosenzweig-Lipson et al. 2007; Skolnick et al. 2009). These limitations highlight a major unmet need for more efficacious and fast-acting antidepressant agents, particularly with the high rates of suicide in depressed subjects.
Recent preclinical and clinical studies have shown that ketamine, an N-methyl-d-aspartate (NMDA) receptor antagonist commonly used as an anesthetic, produces rapid and sustained antidepressant properties in depressed patients and animals (Li et al. 2010; Zarate et al. 2012). However, the molecular mechanisms by which ketamine displays antidepressant-like effects are not fully elucidated.
Neuregulin 1 (NRG1), a member of the family of neurotrophic factors, acts by activating the tyrosine kinase of ErbB receptors and regulates gamma-aminobutyric acid (GABA)ergic transmission (Woo et al. 2007). ErbB4 is the only receptor with a high affinity for NRG1 and an active tyrosine kinase domain (Buonanno 2010). Recent data suggest a key role of the NRG1-ErbB4 signaling in neurotransmission, synaptic plasticity, and synchronization of neuronal network activity in the cortex and hippocampus through raising precisely timed GABA release, which is of great importance for cognition, learning, memory, and emotion (Buonanno 2010; Eto et al. 2010; Fisahn et al. 2009; Woo et al. 2007). Moreover, the interruption of NRG1-ErbB4 signaling leads to the impairment of plasticity and the loss of spines (Fisahn et al. 2009). Importantly, the expression of ErbB4 is largely confined to specific classes of interneurons, particularly parvalbumin interneurons (Fazzari et al. 2010). In the ErbB4-/- mice, glutamic acid decarboxylase (GAD67)-positive and parvalbumin-positive cells are significantly decreased (Gu et al. 2005; Neddens and Buonanno 2010). Parvalbumin interneurons regulate the activity of cortical pyramidal neurons and provide the inhibitory postsynaptic potential to these neurons (Povysheva et al. 2006). Wen and coworkers have demonstrated that the ErbB4 in parvalbumin interneurons is critical for NRG1 in the regulation of pyramidal neuronal activity and long-term potentiation in adult mouse brain (Wen et al. 2010). Meanwhile, NRG1 is reported to be a bipolar disorder susceptibility gene and an interesting state-dependent biological marker of major depressive disorder (Green et al. 2005; Belzeaux et al. 2010). All these studies suggest that parvalbumin interneurons are major cellular target for NRG1-ErbB4 signaling in the brain, and we therefore hypothesized that the hypofunction of NRG1-ErbB4 signaling in parvalbumin interneurons may be involved in the process of ketamine exerting rapid antidepressant actions in rats subjected to the forced swimming test (FST).
Materials and Methods
Animals
The present study was approved by the Ethics Committee of Jinling Hospital, Nanjing, China, and was performed in accordance with the Guide for the Care and Use of Laboratory Animals from the National Institutes of Health of the USA. Twenty-four male adult Wistar rats with the body weight of 200–250 g were purchased from the Shanghai Animal Center, Shanghai, China. Four rats were housed per cage with food available ad libitum and a 12-h light/dark cycle (lights on at 7:00 a.m.). After 7 days of accommodation, the rats were randomly divided into three groups (n = 8): control group, ketamine group, and NRG1 + ketamine group.
Intracerebroventricular Cannulation
Rats were anesthetized with 50 mg/kg intraperitoneal pentobarbital, and a 22-G cannula was implanted to the lateral ventricles (coordinates from bregma: −0.9 mm anterior/posterior, −1.5 mm medial/lateral, −3.5 mm dorsal/ventral from dura) (Dwyer et al. 2012). After 7 days of recovery, all rats received a 15-min FST as discussed below, and on the second day, the rats were intraperitoneally infused with ketamine or the same volume of saline and intracerebroventricularly infused with NRG1 or the same volume of dimethyl sulfoxide (DMSO). The injection cannula stayed in the guide cannula for 1 min after infusions.
Drug Administration
To evaluate the ketamine-induced antidepressant effects, animals subjected to the FST received a single intraperitoneal administration of 10 mg/kg ketamine (Gutian Pharmaceutical Company, Fujian, China) (ketamine group and NRG1 + ketamine group) or saline in a volume of 1 ml (control group) and were subjected to behavioral tests at 0.5 h after the administration. The dose of 10 mg/kg to elicit ketamine’s antidepressant effects was selected on the basis of previous studies (Beurel et al. 2011; Li et al. 2010).
To determine whether NRG1 and ErbB4 are involved in the ketamine-mediated antidepressant effects, we added NRG1 (10 μM in 5 μl for intracerebroventricular infusion; R and D Systems, USA) (NRG1 + ketamine group) or an equivalent volume of DMSO (control group and ketamine group) 30 min before ketamine or saline administration. The NRG1 dose was selected based on the study from Tan et al (2011). Behavioral test was performed at 0.5 h after the ketamine or saline administration.
FST
FST was carried out according to a previous study (Li et al. 2010). The FST included two separate exposures to a cylindrical tank. The tank was 65 cm tall, 30 cm in diameter, and filled with water (22–23 °C) to a depth of 40 cm so that rats could not touch the bottom of the tank. All of the procedures were conducted at 9:00–15:00. For the first exposure, rats were placed in the water for 15 min (pretest session). Twenty-four hours later, rats were placed in the water for 6 min (test session). The immobility time during the last 5 min of the test session was recorded in seconds by two expert observers who were blinded to the grouping. Immobility was defined as the rat remained floating in the water without struggling and made only the movements necessary to keep the head above the water. The water in the tank was changed after each test.
Novelty-Suppressed Feeding Test (NSFT)
NSFT was performed as previously described (Warner-Schmidt JL and Duman 2007). Before testing, rats were food-deprived overnight. The rats were placed in an open field (75 cm × 75 cm × 40 cm) with a small amount of food in the center. Animals were allowed to explore the open field for 8 min. The latency to feed, specifically the time it took for the rat to approach and take the first bite of the food, was recorded by a stopwatch. Home cage food intake was measured right after the test as a control value.
Open Field Test (OFT)
Before the test session of the FST, OFT was used to test whether locomotor activity was affected in the experimental rats. Locomotor activity of the rats was evaluated by the OFT at 0.5 h after the administration of saline or ketamine. The apparatus consisted of an arena of 75 × 75-cm square floor surrounded by a 40-cm-high wall. The floor of the arena was divided into 25 equal squares. Rats were placed in the center of the square, and the numbers of crossings and rearing were subsequently recorded by the same two observers in a blinded manner. The open field was cleaned entirely after each test.
Stereotype Rating
To study psychosis-like behavior, stereotype rating was performed at 0.5 h after the last administration of saline or ketamine as in the studies of Huang et al. (1997) and Zuo et al. (2007). This activity was observed for 5 min. For the test, the same two observers rated the stereotyped behavior every 1 min in this procedure in a blinded manner: score 1, lying down, eyes closed (asleep); score 2, lying down, eyes open (inactive); score 3, normal grooming or chewing cage litter (in place activities); score 4, moving about in the cage, sniffing, rearing (normal, alert, and active); score 5, running movement (hyperactive); score 6, repetitive exploration of the cage at normal level of activity (slow patterned); score 7, repetitive exploration of the cage with hyperactivity (fast patterned); score 8, remaining in the same place in the cage with fast repetitive head and/or foreleg movement (restricted); and score 9, backing up, jumping, seizures, abnormally maintained postures, dyskinetic movements (dyskinetic-reactive).
Tissue Preparation
Immediately after the FST, the rats were sacrificed by decapitation, and the hippocampus and prefrontal cortex (PFC) were rapidly dissected out on an ice-cold plate, frozen, and stored at −80 °C until used.
Western Blot
The ErbB4, p-ErbB4, parvalbumin, and GAD67 levels in the hippocampus and PFC (n = 4 for each group) were assessed by the western blot after the behavior test. The normalized protein samples were subjected to sodium dodecyl sulfate polyacrylamide gel electrophoresis and then were transferred onto polyvinylidene difluoride membranes (Immobilon-P; Millipore, IPVH00010). Membranes were blocked with 5 % skim milk in Tris-buffered saline with Tween 20 (TBST) for 1 h and then incubated with rabbit anti-ErbB4 (Santa Cruz, CA, USA), rabbit anti-p-ErbB (Santa Cruz, CA, USA), rabbit anti-β-Actin (Cell Signaling, USA), rabbit anti-parvalbumin (Abcam, UK), and anti-GAD67 (Santa Cruz, CA, USA) overnight at 4 °C room temperature. After thorough washing, membranes were incubated in TBST with the secondary antibody (goat anti-rabbit and goat anti-mouse; Santa Cruz, CA, USA) diluted 1:1,000 for 1 h at room temperature. Bands were visualized by ECL and quantitated with the ImageQuant software.
Enzyme-Linked Immunosorbent Assay (ELISA)
Levels of NRG1, GABA, and glutamate were determined using a commercial ELISA kit (Jiancheng Biologic Project Company, Nanjing, China) following the manufacturer’s instructions. The readings were normalized to the amount of standard protein.
Statistical Analysis
Data are expressed as mean ± SEM and analyzed by the Statistical Product for Social Sciences (SPSS version 16.0, IL, USA). Comparisons were made by using one-way analysis of variance with Bonferroni tests for post hoc comparisons. Difference was defined as significant at P < 0.05.
Results
FST and Drug Administration Had No Significant Effects on the Locomotor Activity and the Stereotypic Movements of Rats
Compared with the controls subjected to the FST, the rats that received drugs did not present any significant changes in the crossings and rearings (P > 0.05, Fig. 1a) and the stereotypic movements (P > 0.05, Fig. 1b) 0.5 h after administration.
NRG1 and Apocynin Attenuated the Rapid-Acting Antidepressant Actions of Ketamine in Rats During the FST and NSFT
Compared with the controls, the rats that received 10 mg/kg ketamine administration presented a significant decrease in the immobility time (P < 0.001, Fig. 2a) and latency to feed (P < 0.01, Fig. 2b) 0.5 h after administration. To investigate the effects of NRG1 on the behavior of the rats, we analyzed the immobility time and latency to feed of rats subjected to the FST and NSFT after the treatment of NRG1 and ketamine. Preadministration with NRG1 before ketamine administration prevented the ketamine-induced decrease in immobility time (Fig. 2a) and latency to feed (Fig. 2b).
Levels of NRG1 in the Rat Hippocampus and PFC
As shown in Fig. 3, 10 mg/kg ketamine downregulated NRG1 in the hippocampus (P < 0.01, Fig. 3a) and PFC (P < 0.001, Fig. 3b). To confirm whether NRG1-ErbB4 signaling plays a role in the downregulation of NRG1 by ketamine, we applied NRG1 to the rats subjected to the FST. Preadministration with NRG1 significantly reversed the downregulation of NRG1 induced by ketamine in the hippocampus (P < 0.05, Fig. 3a) and PFC (P < 0.01, Fig. 3b).
Levels of p-ErbB4 and ErbB4 in the Rat Hippocampus and PFC
As shown in Fig. 4, 10 mg/kg ketamine downregulated p-ErbB4 in the hippocampus (P < 0.05, Fig. 4a) and PFC (P < 0.01, Fig. 4b). To confirm whether NRG1-ErbB4 signaling plays a role in the downregulation of p-ErbB4 by ketamine, we applied NRG1 to the rats subjected to the FST. Preadministration with NRG1 significantly reversed the downregulation of p-ErbB4 induced by ketamine in the hippocampus (P < 0.05, Fig. 4a) and PFC (P < 0.05, Fig. 4b). There was no significant difference with respect to the levels of ErbB4 in the hippocampus and PFC among the groups (P > 0.05, Fig. 4).
Levels of Parvalbumin and GAD67 in the Rat Hippocampus and PFC
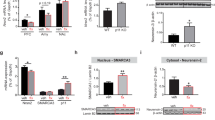
As shown in Fig. 5, 10 mg/kg ketamine downregulated parvalbumin in the hippocampus (P < 0.05, Fig. 5a) and PFC (P < 0.05, Fig. 5b), and GAD67 in the hippocampus (P < 0.05, Fig. 5c) and PFC (P < 0.01, Fig. 5d). To confirm whether NRG1-ErbB4 signaling plays a role in the downregulation of parvalbumin and GAD67 by ketamine, we applied NRG1 to the rats subjected to the FST. Preadministration with NRG1 reversed the downregulation of parvalbumin in the hippocampus (P < 0.05, Fig. 5a) and PFC (P < 0.05, Fig. 5b), and GAD67 in the hippocampus (P < 0.05, Fig. 5c) and PFC (P < 0.01, Fig. 5d) induced by ketamine.
Effects of ketamine administration and NRG1 preadministration on the parvalbumin and GAD67 levels in the rat hippocampus (a, c) and PFC (b, d) after the FST. Data are expressed as mean ± SEM of four rats per group. *P < 0.05 and **P < 0.01 versus control; # P < 0.05 and ## P < 0.01 versus ket. ket ketamine
Levels of GABA and Glutamate in the Rat Hippocampus and PFC
As shown in Fig. 6, 10 mg/kg ketamine downregulated GABA in the hippocampus (P < 0.05, Fig. 6a) and PFC (P < 0.05, Fig. 6b) and upregulated glutamate in the hippocampus (P < 0.001, Fig. 6c) and PFC (P < 0.001, Fig. 6d). To confirm whether NRG1-ErbB4 signaling plays a role in the change of GABA and glutamate by ketamine, we applied NRG1 to the rats subjected to the FST. Preadministration with NRG1 reversed the downregulation of GABA in the hippocampus (P < 0.05, Fig. 6a) and PFC (P < 0.05, Fig. 6b) and the upregulation of glutamate in the hippocampus (P < 0.001, Fig. 6c) and PFC (P < 0.001, Fig. 6d) induced by ketamine.
Effects of ketamine administration and NRG1 preadministration on the GABA and glutamate levels in the rat hippocampus (a, c) and PFC (b, d) after the FST. Data are expressed as mean ± SEM of eight rats per group. *P < 0.05 and ***P < 0.001 versus control; # P < 0.05 and ### P < 0.001 versus ket. ket ketamine
Discussion
The results of the present study showed that a subanesthetic dose of ketamine elicited antidepressant effects associated with the decreased levels of NRG1, p-ErbB4, parvalbumin, GAD67, and GABA and the increased levels of glutamate in the rat hippocampus and PFC. More importantly, we found for the first time that NRG1 reversed ketamine-induced antidepressant effects, downregulation of p-ErbB4, parvalbumin, GAD67, GABA, and upregulation of glutamate. These results indicated that dysfunction of NRG1-ErbB4 signaling plays a key role in ketamine-induced antidepressant effects in the rats subjected to the FST.
NRG1-ErbB4 signaling is critical in various neurophysiology processes including neuron development and migration, synapse plasticity, and synthesis and secretion of neurotransmitter (Buonanno 2010). Neuronal excitability relies on the summation of excitatory and inhibitory signals, which is in turn regulated by the number of excitatory and inhibitory synaptic contacts (Keith and El-Husseini 2008). Therefore, the promoting effect of NRG1 on excitatory synapses is critical to the function of GABAergic interneurons. Fazzari et al (2010) have reported that NRG1-ErbB4 signaling controls the development of GABAergic circuits in the cerebral cortex, and postsynaptic ErbB4 expression is necessary for parvalbumin interneurons to receive a normal complement of excitatory synapses. The present study reported for the first time that ketamine reversed the changes in NRG1 and p-ErbB4 expressions in rats subjected to FST. Moreover, we used a pharmacological approach by an intervention treatment with the NRG1 to activate ErbB4, which subsequently attenuated the antidepressant effects of ketamine and blocked ketamine-induced downregulation of p-ErbB4, indicating a critical role of ErbB4 in antidepressant procedure of ketamine by NRG1. Despite that the specific mechanisms of NRG1-ErbB4 signaling regulating parvalbumin interneurons remain not fully understood, Li et al. (2011) have reported that NRG1 regulates the excitability of parvalbumin interneurons through Kv1.1 in mice. Therefore, identification of the specific cellular pathway activated by NRG1-ErbB4 signaling in parvalbumin interneurons will contribute to understanding the pathogenesis and treatment of depression.
Parvalbumin-positive interneurons, the major subpopulation of GABAergic interneurons, which are characterized by the fast-spiking discharge pattern, are very important in controlling brain excitability (Morris et al. 1999). Parvalbumin interneurons can release GABA and provide inhibitory postsynaptic potentials to regulate the activity of cortical pyramidal neurons and glutamate neurotransmission (Povysheva et al. 2006). In addition, the function of parvalbumin interneurons is intimately linked to the generation of gamma oscillation (Cardin et al. 2009; Sohal et al. 2009; Volman et al. 2011), an emergent property of cortical circuits linked to information processing and working memory (Jensen et al. 2007), and the disruption of parvalbumin interneurons contributes to the pathogenesis of depression (Liu et al. 2012). In the present study, we presented that ketamine downregulated the activity of parvalbumin interneurons by reducing the levels of parvalbumin and GAD67 and thus downregulating GABA and upregulating glutamate in the rat hippocampus and PFC, suggesting that parvalbumin interneurons may be involved in ketamine’s antidepressant effects.
Nevertheless, a postmortem study comparing the densities of GABAergic interneurons has shown no significant change in parvalbumin interneurons in depressed patients (Zhang and Reynolds 2002). In addition, there is a report that parvalbumin interneurons and parvalbumin-immunoreactive neuropil do not significantly change in the medial prefrontal cortex of rats exposed to chronic stress models (Zadrozna et al. 2011). For technical reasons, we still cannot verify whether ketamine exposure specifically affects the NRG1-ErbB4 signaling in the parvalbumin-positive interneurons although most of the ErbB4 are expressed in the parvalbumin-positive interneurons.
In conclusion, the results show the first evidence that the downregulation of NRG1-ErbB4 signaling in parvalbumin interneurons in the rat brain may contribute to the antidepressant actions of ketamine, suggesting some novel targets for depression treatment.
References
Belzeaux R, Formisano-Tréziny C, Loundou A, Boyer L, Gabert J, Samuelian JC, Féron F, Naudin J, Ibrahim EC (2010) Clinical variations modulate patterns of gene expression and define blood biomarkers in major depression. J Psychiatr Res 44:1205–1213
Beurel E, Song L, Jope RS (2011) Inhibition of glycogen synthase kinase-3 is necessary for the rapid antidepressant effect of ketamine in mice. Mol Psychiatry 16:1068–1070
Buonanno A (2010) The neuregulin signaling pathway and schizophrenia: from genes to synapses and neural circuits. Brain Res Bull 83:122–131
Cardin JA, Carlén M, Meletis K, Knoblich U, Zhang F, Deisseroth K, Tsai LH, Moore CI (2009) Driving fast-spiking cells induces gamma rhythm and controls sensory responses. Nature 459:663–667
Dwyer JM, Lepack AE, Duman RS (2012) mTOR activation is required for the antidepressant effects of mGluR2/3 blockade. Int J Neuropsychopharmacol 15:429–434
Eto K, Hommyo A, Yonemitsu R, Abe S (2010) ErbB4 signals Neuregulin1-stimulated cell proliferation and c-fos gene expression through phosphorylation of serum response factor by mitogen-activated protein kinase cascade. Mol Cell Biochem 339:119–125
Fazzari P, Paternain AV, Valiente M, Pla R, Luján R, Lloyd K, Lerma J, Marín O, Rico B (2010) Control of cortical GABA circuitry development by NRG1 and ErbB4 signalling. Nature 464(7293):1376–1380
Fisahn A, Neddens J, Yan L, Buonanno A (2009) Neuregulin-1 modulates hippocampal gamma oscillations: implications for schizophrenia. Cereb Cortex 19:612–618
Green EK, Raybould R, Macgregor S, Gordon-Smith K, Heron J, Hyde S, Grozeva D, Hamshere M, Williams N, Owen MJ, O'Donovan MC, Jones L, Jones I, Kirov G, Craddock N (2005) Operation of the schizophrenia susceptibility gene, neuregulin 1, across traditional diagnostic boundaries to increase risk for bipolar disorder. Arch Gen Psychiatry 62:642–648
Gu Z, Jiang Q, Fu AK, Ip NY, Yan Z (2005) Regulation of NMDA receptors by neuregulin signaling in prefrontal cortex. J Neurosci 25:4974–4984
Huang NK, Wan FJ, Tseng CJ, Tung CS (1997) Amphetamine induces hydroxyl radical formation in the striatum of rats. Life Sci 61:2219–2229
Jensen O, Kaiser J, Lachaux JP (2007) Human gamma-frequency oscillations associated with attention and memory. Trends Neurosci 30:317–324
Keith D, El-Husseini A (2008) Excitation control: balancing PSD-95 function at the synapse. Front Mol Neurosci 1:4
Kessler RC, Berglund P, Demler O, Jin R, Koretz D, Merikangas KR, Rush AJ, Walters EE, Wang PS, National Comorbidity Survey Replication (2003) The epidemiology of major depressive disorder: results from the National Comorbidity Survey Replication (NCS-R). JAMA 289:3095–3105
Li KX, Lu YM, Xu ZH, Zhang J, Zhu JM, Zhang JM, Cao SX, Chen XJ, Chen Z, Luo JH, Duan S, Li XM (2011) Neuregulin 1 regulates excitability of fast-spiking neurons through Kv1.1 and acts in epilepsy. Nat Neurosci 15:267–273
Li N, Lee B, Liu RJ, Banasr M, Dwyer JM, Iwata M, Li XY, Aghajanian G, Duman RS (2010) mTOR-dependent synapse formation underlies the rapid antidepressant effects of NMDA antagonists. Science 329:959–964
Liu TY, Hsieh JC, Chen YS, Tu PC, Su TP, Chen LF (2012) Different patterns of abnormal gamma oscillatory activity in unipolar and bipolar disorder patients during an implicit emotion task. Neuropsychologia 50:1514–1520
Morris NP, Harris SJ, Henderson Z (1999) Parvalbumin-immunoreactive, fast-spiking neurons in the medial septum/diagonal band complex of the rat: intracellular recordings in vitro. Neuroscience 92:589–600
Neddens J, Buonanno A (2010) Selective populations of hippocampal interneurons express ErbB4 and their number and distribution is altered in ErbB4 knockout mice. Hippocampus 20:724–744
Povysheva NV, Gonzalez-Burgos G, Zaitsev AV, Kroner S, Barrionuevo G, Lewis DA, Krimer LS (2006) Properties of excitatory synaptic responses in fast-spiking interneurons and pyramidal cells from monkey and rat prefrontal cortex. Cereb Cortex 16:541–552
Rosenzweig-Lipson S, Beyer CE, Hughes ZA, Khawaja X, Rajarao SJ, Malberg JE, Rahman Z, Ring RH, Schechter LE (2007) Differentiating antidepressants of the future: efficacy and safety. Pharmacol Ther 113:134–153
Skolnick P, Popik P, Trullas R (2009) Glutamate-based antidepressants: 20 years on. Trends Pharmacol Sci 30:563–569
Sohal VS, Zhang F, Yizhar O, Deisseroth K (2009) Parvalbumin neurons and gamma rhythms enhance cortical circuit performance. Nature 459:698–702
Tan GH, Liu YY, Hu XL, Yin DM, Mei L, Xiong ZQ (2011) Neuregulin 1 represses limbic epileptogenesis through ErbB4 in parvalbumin-expressing interneurons. Nat Neurosci 15(2):258–266
Volman V, Behrens MM, Sejnowski TJ (2011) Downregulation of parvalbumin at cortical GABA synapses reduces network gamma oscillatory activity. J Neurosci 31:18137–18148
Warner-Schmidt JL, Duman RS (2007) VEGF is an essential mediator of the neurogenic and behavioral actions of antidepressants. Proc Natl Acad Sci U S A 104:4647–4652
Wen L, Lu YS, Zhu XH, Li XM, Woo RS, Chen YJ, Yin DM, Lai C, Terry AV Jr, Vazdarjanova A, Xiong WC, Mei L (2010) Neuregulin 1 regulates pyramidal neuron activity via ErbB4 in parvalbumin-positive interneurons. Proc Natl Acad Sci U S A 107:1211–1216
Woo RS, Li XM, Tao Y, Carpenter-Hyland E, Huang YZ, Weber J, Neiswender H, Dong XP, Wu J, Gassmann M, Lai C, Xiong WC, Gao TM, Mei L (2007) Neuregulin-1 enhances depolarization-induced GABA release. Neuron 54:599–610
Zadrozna M, Nowak B, Lason-Tyburkiewicz M, Wolak M, Sowa-Kucma M, Papp M, Ossowska G, Pilc A, Nowak G (2011) Different pattern of changes in calcium binding proteins immunoreactivity in the medial prefrontal cortex of rats exposed to stress models of depression. Pharmacol Rep 63:1539–1546
Zarate CA Jr, Brutsche NE, Ibrahim L, Franco-Chaves J, Diazgranados N, Cravchik A et al (2012) Replication of ketamine’s antidepressant efficacy in bipolar depression: a randomized controlled add-on trial. Biol Psychiatry 71:939–946
Zhang ZJ, Reynolds GP (2002) A selective decrease in the relative density of parvalbumin-immunoreactive neurons in the hippocampus in schizophrenia. Schizophr Res 55:1–10
Zuo DY, Wu YL, Yao WX, Cao Y, Wu CF, Tanaka M (2007) Effect of MK-801 and ketamine on hydroxyl radical generation in the posterior cingulate and retrosplenial cortex of free-moving mice, as determined by in vivo microdialysis. Pharmacol Biochem Behav 86:1–7
Acknowledgment
The present study was supported by the National Natural Science Foundation of China (No. 81271216).
Author information
Authors and Affiliations
Corresponding author
Additional information
Nan Wang and Guang-Fen Zhang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Wang, N., Zhang, GF., Liu, XY. et al. Downregulation of Neuregulin 1-ErbB4 Signaling in Parvalbumin Interneurons in the Rat Brain May Contribute to the Antidepressant Properties of Ketamine. J Mol Neurosci 54, 211–218 (2014). https://doi.org/10.1007/s12031-014-0277-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-014-0277-8