Abstract
Astrocyte inflammation plays important roles both in physiological and pathological processes in the central nervous system (CNS). Ischemic injury in the CNS causes damage to astrocytes and the release of proinflammatory cytokines, such as tumor necrosis factor-α, interleukin-1β, and interleukin-6. This current study investigates whether mesencephalic astrocyte-derived neurotrophic factor (MANF) inhibits oxygen–glucose deprivation (OGD)-induced cell damage and inflammatory cytokine secretion by suppressing endoplasmic reticulum stress in rat primary astrocytes. We found that MANF alleviated OGD-induced astrocyte damage and rescued the cell viability, and the upregulation of GRP78 (endoplasmic reticulum (ER) stress marker) and NF-κB p65 (one of the central mediators of proinflammatory pathways) induced by OGD were significantly reduced by preincubation of MANF. In addition, the increases of secretion and mRNA expression levels of the proinflammatory cytokines IL-1β, IL-6, and TNF-α in astrocytes induced by OGD were significantly suppressed by MANF. These findings demonstrate that MANF shows the potential to alleviate cell damage and inflammation in rat primary astrocytes by suppressing ER stress, indicating that MANF plays an important role in astrocyte inflammation and functioning and may suggest a promising strategy for neuroprotection in the CNS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inflammation is an important contributing factor in central nervous system (CNS) injury. Astrocyte plays an important role in the processes of inflammatory response in the CNS. They respond swiftly to subtle changes in the microenvironment and secrete an array of proinflammatory and anti-inflammatory cytokines, chemokines, and trophic factors to modify the ambient microenvironment (Lau and Yu 2001). Astrocyte-derived factors are important in neuronal survival, neurogenesis, and neuron repair (Song et al. 2002; Emsley et al. 2004). The ischemic injury of the brain and spinal cord stimulates damage to astrocytes and the release of proinflammatory cytokines, such as tumor necrosis factor-α, interleukin-1β, and interleukin-6 (Dong and Benveniste 2001). Astrocyte damage and the inflammation caused by ischemic injury are crucial pathological processes in the CNS.
In the present study, we use oxygen–glucose deprivation (OGD) to trigger the hypoxia–ischemia situation of astrocytes in vitro. In the CNS ischemic injury, endoplasmic reticulum stress (ERS) is caused by hypoxia–ischemia, glucose starvation, ATP depletion, oxidative stress, and Ca2+ homeostasis disorders. There are three ER-localized protein sensors for ER stress: inositol-requiring enzyme 1α, double-stranded RNA-dependent protein kinase-like ER kinase, and activating transcription factor 6. In ERS, these sensors activate the unfolded-protein response (UPR) processes such as the increases of expression of glucose-regulated protein 78 (GRP78). GRP78 is a prominent ER-resident chaperone binding to these three ER stress sensors, but more stably interacts with misfolded or unfolded proteins (Ron and Walter 2007). Therefore, upregulation of GRP78 is used as an ER stress marker most commonly (Li et al. 2009). Astrocyte damage and inflammatory responses are then induced by ERS through the accumulation of unfolded or misfolded proteins in a subcellular organelle mainly referred to as a protein-folding factory known as the ER (Ron and Walter 2007; Zhang and Kaufman 2008; Hosoi and Ozawa 2010; Hotamisligil 2010).
Prior research failed to find an effective therapy to treat the CNS ischemic injury; however, a novel neurotrophic factor, mesencephalic astrocyte-derived neurotrophic factor (MANF) (Lindholm and Saarma 2010), may provide a potential method. Previous evidence suggests that MANF is an ER stress response protein and is able to protect cells against ER stress-induced cell death in vitro (Apostolou et al. 2008). However, the role of MANF in the damage and inflammatory response of astrocytes is not clear; therefore, we investigated the effect of MANF on OGD-induced cell damage and inflammatory cytokine secretion in astrocytes in vitro.
Materials and Methods
Animals and Primary Astrocyte Culture
Neonatal Wistar rats were obtained from the Laboratory Animal Center of Shandong University. The International Guiding Principles for Animal Research were followed in the handling and care of all animals, as adopted by the Laboratory Animal Center of Shandong University. All efforts were made to minimize pain and the number of animals used. Primary astrocytes were prepared from neonatal Wistar rats postnatal day 1, as previously described (Aronica et al. 2012). Briefly, the cortical tissues freed of meninges and blood vessels were mechanically dissociated, and the cell suspension was seeded at a density of 1 × 106 cells/mL in Dulbecco’s modified Eagle medium (5.5 mmol/L glucose) (DMEM, Gibco, Grand Island, NJ) supplemented with 10 % fetal bovine serum (FBS, Gibco, Grand Island, NJ), 2 mM l-glutamine, 100 U/mL penicillin, and 100 mg/mL streptomycin (Sigma-Aldrich, St. Louis, MO). When the culture reached confluency, the microglia and oligodendrocytes were removed by an orbital shaker; the remaining cells, a majority of them being astrocytes, were replated. Before each experiment, the plated cells were incubated with serum-free DMEM medium for 1 h.
Immunocytochemistry
Primary astrocytes were subcultured on sterile glass cover slips for 12–16 h, washed in PBS, fixed in 4 % formaldehyde for 10 min at 37 °C, permeabilised in 0.2 % Triton-X 100 for 10 min at room temperature, washed in PBS, and then blocked in 1 % BSA in PBS for 20 min at room temperature. The cells were then incubated with primary antibodies (mouse monoclonal anti-GFAP 1:100, Abcam, Cambridge, MA) overnight at 4 °C. Cells were then washed in PBS and incubated with secondary antibodies (Texas Red-conjugated anti-mouse IgG 1:1,000; Invitrogen, Life Tech, CA) in PBS for 40 min at 37 °C. Images were captured using a Nikon Eclipse 80i fluorescence microscope (Nikon, Tokyo, Japan).
Interventions of Primary Astrocytes
Cultured astrocytes were seeded in six-well plates (Corning, Corning, NY) at a density of 5 × 104/well, and 1 mL Dulbecco’s modified Eagle medium (5.5 mmol/L glucose) with 10 % FBS was added to each well. After 24 h, the medium was removed and replaced with 1 mL of fresh culture medium without FBS and was allowed to sit in culture for the next 24 h. The cells were then pretreated with vehicle (control) and recombinant human MANF (R&D Systems, Inc., Minneapolis, MN) at the concentration of 50 and 100 ng/mL for 1 h. The concentrations and preincubation period of MANF were chosen according to the results of our preexperiments (Supplemental Material). MANF was dissolved in phosphate-buffered saline (PBS, pH 7.4), and the same volume of PBS was used as the vehicle. Then, the astrocytes were stimulated with or without the treatment of OGD. The isotonic OGD solution (pH 7.4) contained (in millimolar, at 37 °C) the following: 0 glucose, 21 NaHCO3, 120 NaCl, 5.36 KCl, 0.33 Na2HPO4,0.44 KH2PO4, 1.27 CaCl2, and 0.81 MgSO4 (Kintner et al. 2007). Cells were incubated in 1.0 mL of the OGD solution in a hypoxic incubator (Forma Scientific Inc., Marietta, OH) containing 94 % N2, 1 % O2, and 5 % CO2 for 2 h (Begum et al. 2012). Normoxic control cells were incubated in 5 % CO2 and atmospheric air in an isotonic control solution for 2 h.
MTT Assay
Astrocyte viability was detected by the 3-[4, 5-dimethylthiazol-2-yl]-2,5-diphenyltetrazolium bromide (MTT) assay. Astrocytes were plated into 96-well culture plates at a density of 1 × 106 cells/mL with 200 μL of culture medium per well in triplicate. When reaching 80 % confluency, the cells were pretreated with or without MANF for 1 h and then stimulated with or without OGD for an additional 2 h. Then, 20 μL MTT solution (5 mg/mL, Sigma-Aldrich) was added to each well and incubated at 37 °C for 4 h. The culture medium was aspirated and followed by an addition of 200 μL dimethyl sulfoxide. The absorbance value was measured in a Varioskan Flash Multimode Reader (Thermo Scientific) at 490 nm.
LDH Release Assay
Astrocytes cultured in six-well plates were pretreated with or without MANF for 1 h and then stimulated with or without OGD for an additional 2 h. To measure the extent of damage to the cells, the stable cytosolic enzyme resulting from cell lysis, lactate dehydrogenase (LDH) was measured in the cell culture medium using an LDH Cytotoxicity Assay Kit II (Roche Applied Science, Mannheim, Germany). Simply stated, the clear medium (10 μL/well) was transferred into an optically clear 96-well plate, then 100 μL of LDH Reaction Mix was added to each well, mixed, and incubated at room temperature for 30 min. The absorbance at 450 nm was measured by a Varioskan Flash Multimode Reader (Thermo Scientific).
Western Blot Analysis
After the stimulation with or without OGD for 2 h, the immunoreactivity of GRP78 and NF-κB p65 in astrocytes was determined by Western blot. Astrocytes were washed twice with ice-cold phosphate-buffered saline (PBS) and harvested in a lysis buffer containing 1 mM PMSF. The extract was centrifuged at 12,000×g for 5 min at 4 °C to remove cell debris. Nuclear extraction was performed as described previously (Lee et al. 2006). Protein concentration was determined by a BCA Protein Assay Kit according to the manufacturer’s instructions. Equivalent amounts of protein (10 μg) for each sample were separated by 10 % acrylamide–SDS-PAGE using 5 % stacking and 12 % separating gels and were subsequently transferred to polyvinylidene difluoride membranes (Millipore, Billerica, MA). Primary antibodies (anti-GRP78 antibody and anti-NF-κB p65, 1:1,000 dilution; Cell Signaling Technologies, Danvers, MA) and horseradish peroxidase (HRP)-conjugated secondary antibodies (1:30,000 dilution; Cell Signaling Technology, Danvers, MA) were utilized. Equal amounts of protein loading were confirmed by reprobing the membranes with the mouse anti-GAPDH-HRP (1:10,000 dilution; Abcam, Cambridge, MA). Immunoblots were visualized by FluorChem E Chemiluminescent Western Blot Imaging System (Cell Biosciences, Santa Clara, CA). The results were quantified using the Image J software (National Institutes of Health, USA). For the quantification of specific bands, the same size square was drawn around each band to measure the intensity, and then the value was adjusted by the intensity of the background near that band. The results were expressed as a relative ratio of the target protein to reference protein GAPDH. The relative ratio of the target protein of control group is standardized as 1.
ELISA
After the treatment of OGD for 2 h, the immunoreactivity of the proinflammatory cytokines (IL-1β, IL-6, and TNF-α) was determined, and the levels of these secreted cytokines in the astrocyte culture medium were detected by ELISA (Rat IL-1 beta/IL-1F2 Quantikine ELISA Kit, Rat IL-6 Quantikine ELISA Kit, and Rat TNF-α Quantikine ELISA Kit; R&D Systems Inc., Minneapolis, MN), as described by the manufacturer. ODs were determined using a Varioskan Flash Multimode Reader (Thermo Scientific) at 450 nm. Cytokine concentrations in the medium were determined from standards containing known concentrations of the proteins.
RNA Extraction and Real-Time Reverse Transcription-PCR Assay
Astrocytes were pretreated with or without MANF (100 ng/mL) for 1 h and then stimulated with or without OGD for an additional 2 h. Then the total cellular RNA was extracted using TRIzol Reagent (Takara, Otsu, Shiga, Japan). Identical amounts of RNA (0.5 ng) were reverse transcribed into complement DNA by using a commercial reverse transcription (RT)-PCR kit (Fermentas, Vilnius, Lithuania) according to the manufacturer’s instructions. The primers and PCR conditions for amplification were used as described previously (Wang et al. 2012). The quantification data were analyzed with LightCycler analysis software version 4.0 (Roche Applied Science, Mannheim, Germany). The relative expression was normalized on the basis of β-actin. At least three independent experiments were conducted for each condition.
Statistical Analysis
Quantitative data were presented as the mean ± SD of at least three independent experiments. Statistical analysis of data was performed using a Student’s t test or by one-way ANOVA using a Dunnett’s test in multiple comparisons of means. Differences were considered to be statistically significant if the P value was <0.05 (*) or <0.01 (**).
Results
MANF Inhibits OGD-Induced Astrocyte Damage
After three passages, astrocytes that appeared flat and polygonal were grown in a monolayer and detected by a fluorescence microscope. More than 95 % of the cells were GFAP-positive, which means that they were identified as astrocytes (Fig. 1a).
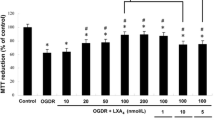
Identified astrocytes and the cell damage detected by MTT and LDH release assay. a More than 95 % of the cells were GFAP-positive, which means that they were identified as astrocytes. b Preincubation of MANF (50 and 100 ng/ml) alleviated the decrease of the cell viability caused by OGD for 2 h (*P < 0.05 vs. OGD group). c MANF significantly reduced the percentage of LDH released in MANF 50 ng/mL + OGD 2 h group (*P < 0.05 vs. OGD group) and MANF 100 ng/mL + OGD 2 h group (**P < 0.01 vs. OGD group), which indicates that MANF inhibits OGD-induced astrocyte damage
To determine the effect of MANF on astrocytes induced by OGD, MTT and LDH release assays were performed. MTT result showed that OGD decreased the cell viability of astrocyte (0.27 ± 0.032) compared with the blank control (0.27 ± 0.032); MANF 50 ng/mL (0.39 ± 0.043) and MANF 100 ng/mL (0.42 ± 0.045) alleviated the decrease of the cell viability (P < 0.05 vs. OGD group) (Fig. 1b).
This is consistent with the results of LDH release assay. The percentage of LDH released in the blank control was 1.78 % ± 0.012 and in the OGD treatment group was 22.77 % ± 0.015, indicating that OGD increased the cell damage of astrocytes; while MANF pretreatment significantly reduced the percentage of LDH released in OGD + MANF 50 ng/mL group (17.32 % ± 0.029, P < 0.05 vs. OGD group) and OGD + MANF 100 ng/mL group (12.88 % ± 0.040, P < 0.01 vs. OGD group), which indicate that MANF inhibits OGD-induced astrocyte damage (Fig. 1c).
MANF Reduces the Expression of GRP78 and NF-κB p65 in Astrocytes Induced by OGD
GRP78 is most commonly used as an ER stress marker (Li et al. 2009). And ER stress has been shown to mediate cell-autonomous proinflammatory transcriptional programs, which are mainly governed by transcription factors such as NF-κB, one of the central mediators of proinflammatory pathways (Hotamisligil and Erbay 2008; Zhang and Kaufman 2008; Verfaillie et al. 2013). The level of the p65 subunit of NF-κB in the nucleus represents the translocation (activation) level of NF-κB. To investigate the effects of MANF on ER stress and NF-κB pathway, we measured levels of GRP78, p65 in astrocytes induced by OGD with or without pretreatment of MANF. Western blot showed that the levels of GRP78 and p65 in astrocytes were significantly increased after OGD treatment compared with the blank control. And the increases of GRP78 and NF-κB p65 in OGD-induced astrocytes were substantially reduced by pretreatment of MANF at the concentration of 50 ng/mL and, more markedly, 100 ng/mL. These results indicate that MANF alleviates the activation of NF-κB, one of the central mediators of proinflammatory pathways, by suppressing the ER stress in primary astrocytes (Fig. 2).
The protein levels of GRP78 and NF-κB p65 in astrocytes induced by OGD for 2 h with or without MANF pretreatment. a Western blot of GRP78 protein, an ER stress marker. b Western blot of the p65 in the nucleus, representing the translocation (activation) level of NF-κB. c and d The levels of GRP78 and NF-κB p65 were expressed as a relative ratio of the target protein to GAPDH and standardized. The increases of GRP78 and NF-κB p65 in OGD-induced astrocytes were substantially reduced by pretreatment of MANF at the concentration of 50 ng/mL (*P < 0.05 vs. OGD group) and, more markedly, 100 ng/mL (**P < 0.01 vs. OGD group)
MANF Alleviates Secretion of Inflammatory Cytokines in Astrocytes Induced by OGD
Two hours after the treatment of OGD, inflammatory cytokine (IL-1β, IL-6, and TNF-α) levels in an astrocyte culture medium were determined by ELISA. OGD significantly increased the release of IL-1β in astrocytes (243.59 ± 15.73 pg/mL), and this was significantly attenuated in MANF (50 ng/mL) pretreated astrocytes (190.28 ± 15.83 pg/mL) (P < 0.05 vs. OGD group) and MANF (100 ng/mL) pretreated astrocytes (110.99 ± 12.17) (P < 0.01 vs. OGD group). The secretion of IL-6 was also stimulated by OGD in astrocytes (361.97 ± 46.75 pg/mL), and this was significantly attenuated in MANF (50 ng/mL) pretreatment astrocytes (274.21 ± 18.23 pg/mL) (P < 0.05 vs. OGD group) and MANF (100 ng/mL) pretreatment astrocytes (191.74 ± 15.16 pg/mL) (P < 0.01 vs. OGD group). The secretion of TNF-α was increased in OGD-induced astrocytes (1,476.55 ± 138.63 pg/mL), which was significantly reduced in MANF (50 and 100 ng/mL) pretreatment astrocytes (1,193.54 ± 79.42 and, 1,078.56 ± 84.68 pg/mL, respectively; P < 0.05 vs. OGD group) (Fig. 3).
Secretion of inflammatory cytokines in astrocytes detected by ELISA. a The treatment of OGD for 2 h significantly increased the release of IL-1β in astrocytes, and this was significantly attenuated in MANF (50 or 100 ng/mL) pretreated astrocytes. b The secretion of IL-6 stimulated by OGD was also significantly attenuated by the pretreatment of MANF (50 or 100 ng/mL). c The secretion of TNF-α induced by OGD was significantly reduced by MANF (50 or 100 ng/mL) pretreatment astrocytes (*P < 0.05, **P < 0.01 vs. OGD group)
MANF Suppresses the mRNA Expression of Proinflammatory Cytokines in Astrocytes Induced by OGD
It is well established that astrocytes participate in normal and abnormal processes of the CNS through the release of cytokines (Ridet et al. 1997; Lau and Yu 2001). We therefore evaluated the expression of proinflammatory cytokines following OGD with or without preincubation of MANF (50 and 100 ng/mL). Real-time RT-PCR results showed that OGD treatment increased the mRNA expression levels of proinflammatory cytokines including IL-1β, IL-6, and TNF-α (18.22 ± 2.83, 15.13 ± 2.25, and 10.13 ± 0.65, respectively. The relative expression was standardized on the basis of β-actin). The preincubation of MANF attenuated OGD-induced upregulation of mRNA expression of the three cytokines (Fig. 4).
The mRNA expression of proinflammatory cytokines in astrocytes induced by OGD for 2 h with or without MANF preincubation. The relative expression was standardized on the basis of β-actin. The treatment of OGD for 2 h increased the mRNA expression levels of proinflammatory cytokines including IL-1β (a), IL-6 (b), and TNF-α (c), and the preincubation of MANF (50 or 100 ng/mL) attenuated the upregulation of mRNA expression of the three cytokines induced by OGD (*P < 0.05, **P < 0.01 vs. OGD group)
Discussion
In ischemic injury of the brain and spinal cord, astrocytes play an important role in the protection of neurons, neurogenesis, and neuron repair (Song et al. 2002; Emsley et al. 2004). Astrocytes are crucial to providing protection and repair of the neurons insulted by ischemic injury in the CNS. Furthermore, they secrete an array of proinflammatory and anti-inflammatory cytokines to modify the microenvironment. Therefore, astrocyte damage and inflammation induced by OGD lead to the deterioration of neurons after ischemic injury. Previous evidence has also implicated the negative influence of neuroinflammation in a number of conditions of CNS ischemic injury. Inflammatory processes in CNS are mediated by the activation of glial cells capable of producing immunomodulatory molecules, phagocytosing cellular debris, and recruiting immune cells from the periphery. Although activation of the glia is essential for the maintenance of neuronal function following stress or insult, an uncontrolled response causes glial cell damage and is highly undesirable given the lack of regenerative capacity of the injured brain and spinal cord. Astrocytes, as the resident cells, play a crucial role in both physiological and pathological processes in the CNS by taking part in the maintenance of homeostasis, cell defense, and repair. Astrocytes provide structural, metabolic, and trophic support for neurons, yet they are also immunocompetent cells capable of secreting inflammatory mediators (Benarroch 2005). The damage of astrocytes leads to excessive secretion of proinflammatory molecules such as IL-1β, IL-6, and TNF-α, which may have a deleterious impact on neuronal viability.
In CNS ischemic injury, astrocyte damage and inflammatory responses are induced by ERS caused by hypoxia–ischemia, glucose starvation, ATP depletion, oxidative stress, and disturbance of Ca2+ homeostasis. Neurons insulted cannot be mediated by the protection from astrocytes, and CNS injury may be exacerbated due to the proinflammatory cytokines secreted by damaged astrocytes. Normal functioning of astrocytes requires the trafficking of large amounts of proteins through the ER, which makes them highly sensitive to perturbations in ER homeostasis. Any changes in this trafficking can lead to severe and chronic activation of the UPR, which might cause ERS-based inflammation and cell death in the long run. Prior studies have revealed that pathways activated by the ERS induce sterile inflammation. The ER is a multifunctional organelle involved in protein-folding and processing, intracellular Ca2+ homeostasis, and cell death signal activation (Baumann and Walz 2001). The ERS have been shown to mediate cell-autonomous proinflammatory transcriptional programs, which are mainly governed by transcription factors such as NF-κB, which is one of the central mediators of proinflammatory pathways. Genes transcribed by NF-κB include those encoding crucial proinflammatory cytokines such as IL-1β, IL-6, and TNF-α (Hotamisligil and Erbay 2008; Zhang and Kaufman 2008; Verfaillie et al. 2013). Furthermore, acute-phase response (APR) is also induced by the UPR in ERS. APR commences in the early phases of the innate immune response mainly due to the activity of proinflammatory factors such as IL-1β, IL-6, and TNF-α (Cray et al. 2009). One of the diagnostic signatures of the APR is activation of the production of various cytokines (e.g., IL-1β and IL-6), which can aggravate tissue damage and cause more severe sterile immunopathological conditions (Korbelik et al. 2008). In the present study, OGD is used to induce the ERS, inflammation and cell death in astrocytes, imitating the process of astrocyte damage induced by hypoxia–ischemia in vitro.
Previous studies demonstrate that there is no efficient method to treat the astrocyte damage and inflammation caused by ischemic injury in the CNS; however, MANF demonstrates a promising potential to protect astrocytes and neurons by resisting ERS in the CNS. MANF consists of two domains: an amino-terminal saposin-like domain that may interact with lipids or membranes and a presumably unfolded carboxy-terminal domain that may protect cells against endoplasmic reticulum stress. Growing evidence suggests that MANF is an ER stress response protein and is able to protect cells against ER stress-induced cell death in vitro (Apostolou et al. 2008). In this line, the crystal structure suggests that MANF may help protein folding in the ER. In the MANF C-terminal domain, the two cysteines in the 127CKGC130 motif (132CRAC135 in CDNF) form a C-terminal disulphide bridge that may facilitate the formation of cysteine bridges and protein folding in the ER, thus reducing the ER stress caused by unfolded or incorrectly folded proteins (Lindholm et al. 2007).
Therefore, in our study, we focused on the role of MANF on OGD-induced cell damage and inflammation in astrocytes. Our results show that the cell viability of astrocytes with MANF preincubation was promoted compared with the astrocytes induced by OGD without MANF, and the percentage of LDH released in the MANF pretreated astrocytes induced by OGD was significantly lower than the OGD groups without MANF pretreatment, indicating that MANF alleviates OGD-induced astrocyte damage. In addition, Western blot showed that the increase of the ER-stress marker GRP78 induced by OGD was significantly reduced by MANF preincubation, as well as the p65 subunit of NF-κB in the nucleus, indicating that MANF alleviates the activation of NF-κB pathway by suppressing the ER stress in astrocytes. Meanwhile, the secretion and mRNA expression levels of the proinflammatory cytokines IL-1β, IL-6, and TNF-α in astrocytes were increased by OGD, and this upregulation was significantly suppressed by preincubation of MANF, demonstrating that MANF plays an important role in astrocyte inflammation and functioning by resisting ER stress. Thus, MANF may represent a promising strategy for neuroprotection in the CNS.
In summary, we have shown that pretreatment of MANF in astrocytes give cells the potential to alleviate the inflammatory responses and secretion of proinflammatory cytokine by suppressing ER stress. Whether MANF provides the same protection from cell damage and an inflammatory response induced by ischemia injury to astrocytes in vivo remains to be seen. Future studies will explore the function of MANF to astrocytes in vivo to advance research in animal models of neurologic disease.
References
Apostolou A, Shen Y et al (2008) Armet, a UPR-upregulated protein, inhibits cell proliferation and ER stress-induced cell death. Exp Cell Res 314(13):2454–2467
Aronica E, Ravizza T et al (2012) Astrocyte immune responses in epilepsy. Glia 60(8):1258–1268
Baumann O, Walz B (2001) Endoplasmic reticulum of animal cells and its organization into structural and functional domains. Int Rev Cytol 205:149–214
Begum G, Kintner D et al (2012) DHA inhibits ER Ca2+ release and ER stress in astrocytes following in vitro ischemia. J Neurochem 120(4):622–630
Benarroch EE (2005) Neuron-astrocyte interactions: partnership for normal function and disease in the central nervous system. Mayo Clin Proc 80(10):1326–1338
Cray C, Zaias J et al (2009) Acute phase response in animals: a review. Comp Med 59(6):517–526
Dong Y, Benveniste EN (2001) Immune function of astrocytes. Glia 36(2):180–190
Emsley JG, Arlotta P et al (2004) Star-cross’d neurons: astroglial effects on neural repair in the adult mammalian CNS. Trends Neurosci 27(5):238–240
Hosoi T, Ozawa K (2010) Endoplasmic reticulum stress in disease: mechanisms and therapeutic opportunities. Clin Sci (Lond) 118(1):19–29
Hotamisligil GS (2010) Endoplasmic reticulum stress and the inflammatory basis of metabolic disease. Cell 140(6):900–917
Hotamisligil GS, Erbay E (2008) Nutrient sensing and inflammation in metabolic diseases. Nat Rev Immunol 8(12):923–934
Kintner DB, Luo J et al (2007) Role of Na+-K+-Cl– cotransport and Na+/Ca2+ exchange in mitochondrial dysfunction in astrocytes following in vitro ischemia. Am J Physiol Cell Physiol 292(3):C1113–C1122
Korbelik M, Cecic I et al (2008) Acute phase response induction by cancer treatment with photodynamic therapy. Int J Cancer 122(6):1411–1417
Lau LT, Yu AC (2001) Astrocytes produce and release interleukin-1, interleukin-6, tumor necrosis factor alpha and interferon-gamma following traumatic and metabolic injury. J Neurotrauma 18(3):351–359
Lee KS, Kim SR et al (2006) Peroxisome proliferator activated receptor-gamma modulates reactive oxygen species generation and activation of nuclear factor-kappaB and hypoxia-inducible factor 1alpha in allergic airway disease of mice. J Allergy Clin Immunol 118(1):120–127
Li J, Wang JJ et al (2009) Endoplasmic reticulum stress is implicated in retinal inflammation and diabetic retinopathy. FEBS Lett 583(9):1521–1527
Lindholm P, Saarma M (2010) Novel CDNF/MANF family of neurotrophic factors. Dev Neurobiol 70(5):360–371
Lindholm P, Voutilainen MH et al (2007) Novel neurotrophic factor CDNF protects and rescues midbrain dopamine neurons in vivo. Nature 448(7149):73–77
Ridet JL, Malhotra SK et al (1997) Reactive astrocytes: cellular and molecular cues to biological function. Trends Neurosci 20(12):570–577
Ron D, Walter P (2007) Signal integration in the endoplasmic reticulum unfolded protein response. Nat Rev Mol Cell Biol 8(7):519–529
Song H, Stevens CF et al (2002) Astroglia induce neurogenesis from adult neural stem cells. Nature 417(6884):39–44
Verfaillie T, Garg AD et al (2013) Targeting ER stress induced apoptosis and inflammation in cancer. Cancer Lett 332(2):249–264
Wang J, Li G et al (2012) High glucose-induced expression of inflammatory cytokines and reactive oxygen species in cultured astrocytes. Neuroscience 202:58–68
Zhang K, Kaufman RJ (2008) From endoplasmic-reticulum stress to the inflammatory response. Nature 454(7203):455–462
Acknowledgments
The authors are grateful to Prof. Chen ZY (Department of Neurobiology, Shandong University) and Prof. Tang DQ, Wang XL, Cui TX, Cui ZQ (Research Center for Cell Therapy, Qilu Hospital of Shandong University), for their kind advice and help with this research. The study was supported by a grant from Ph.D. Programs Foundation of Ministry of Education of China (20110131120079).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhao, H., Liu, Y., Cheng, L. et al. Mesencephalic Astrocyte-Derived Neurotrophic Factor Inhibits Oxygen–Glucose Deprivation-Induced Cell Damage and Inflammation by Suppressing Endoplasmic Reticulum Stress in Rat Primary Astrocytes. J Mol Neurosci 51, 671–678 (2013). https://doi.org/10.1007/s12031-013-0042-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-013-0042-4