Abstract
The protective effects of TGF-β have been documented in various autoimmune diseases, mostly in organ-specific autoimmunity including type 1 diabetes mellitus (T1DM). However, TGF-β also plays a role as a pro-inflammatory mediator by induction of Th17 cytokine production. IL-23 also plays a key role in differentiation of Th17 cells, which are implicated in pathogenesis of autoimmune conditions including T1DM. The aim of this study was to investigate and compare the difference in the level of TGF-β1 and IL-23 gene expression in unstimulated peripheral blood mononuclear cells (PBMCs) of patients with different forms of diabetes compared with normal healthy controls subjects. Patients with T1DM were grouped as early-onset T1DM (N = 20) with age at diagnosis <18 years and late-onset T1DM (N = 20) with the age at onset >18 years. Patients with T2DM (N = 20) and normal healthy controls (N = 20) were recruited from the same area. TGF-β1 and IL-23 gene expression in fresh unstimulated PBMCs was determined in each group using quantitative real-time PCR. The results confirmed that a significant difference in TGF-β1 and IL-23 gene expression was observed in both forms of juvenile-onset T1DM and adult-onset T1DM compared to the controls and T2DM patients. There was no significant difference for TGF-β gene expression in patients with T2DM and controls. We therefore conclude that our results support the previous data on TGF-β gene down-regulation in T1DM. Also up-regulation of IL-23 has been observed in T1DM whilst it was down-regulated in T2DM. We also found no significant difference between juvenile-onset and adult-onset T1DM indicating same mechanism might be involved in the pathogenesis of both types. More studies on different cytokines in Th17 pathways are required to further confirm our finding.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Inflammatory cytokines play central role in pathogenesis of autoimmune diseases including type 1 diabetes mellitus (T1DM). TGF-β is a multifunctional cytokine acting on a variety of cell types in a wide range of biological processes like immune regulation (via increasing of adhesion molecules and providing chemotactic gradients), tissue repair (modulation of ECM, extra-cellular matrix, turn over) and tumourigenesis [1].
The protective effects of TGF-β have been documented in different autoimmune diseases, mostly in organ-specific autoimmunity including T1DM. Intramuscular injection of plasmid DNA, which encodes latent TGF-β (pCMV-TGF-β1), decrease the incidence of diabetes in both cyclophosphamide (CYP)-treated (accelerated) and non-CYP treated (natural course) diabetes in NOD mice [2, 3]. A similar protective role for TGF-β against diabetes has been observed in islet-specific expression of TGF-β in NOD mice [4, 5] or by injection of TGF-β-producing T cell clones [6]. Neutralization of TGF-β with anti-TGF-β accelerates the onset of diabetes [7, 8]. TGF-β gene expression has been observed in Treg cells in peripheral blood of children with T1DM [9]. Reduced TGF-β expression has been previously reported in peripheral blood mononuclear cells (PBMCs) in children with T1DM [10].
Although Th1 immune response is the most recognized mechanism in development of autoimmune conditions, new data point towards the implication of Th17 pathway in autoimmunity [11, 12]. Recent evidence indicates a central role of Th17 response in T1DM [12]. IL-23 is a proinflammatory, heterodimeric cytokine involved in differentiation of Th17 cells [13] playing pivotal role in regulation of Th17 cell expansion rather than their development [13, 14]. TGF-β also acts together with IL-23 operating as a pro-inflammatory mediator by induction of Th17 pathway [8]. However at the ultimate phase of the immune response, TGF-β suppresses the inflammatory pathways [15]. The effect of TGF-β on naïve compared with antigen-experienced/memory CD8+ T cells seems to be different depending on their differentiation status and activation history indicating dual role of TGF-β in autoimmunity [16].
The aim of this study was to investigate and compare the difference in the level of TGF-β1 and IL-23 gene expression in unstimulated PBMCs of patients with different forms of diabetes compared with controls subject.
Materials and methods
Patients groups
Patients with diabetes were recruited from diabetes clinic in Shariati hospital, Tehran University of medical sciences. Patients were diagnosed according to American Diabetes Association (ADA) Criteria. The cases fulfilled at least one of the triple criteria recommended by ADA were included in the study. Diabetes was regarded as T1DM if it was diagnosed before the age of 30 years and accompanied with acute onset and presence of ketonemia and treatment with insulin began within the first year of diagnosis and continued thereafter. In most patients diagnosed with T1DM in our study DKA was the first symptom and treatment with insulin began at the time of diagnosis. Normal healthy controls subjects were recruited from the same area.
Informed consent was obtained from all participants. After collection of heparinized venous blood, lymphocyte separation was performed using density gradient ficoll (1.077) and total RNA was extracted from fresh unstimulated PBMCs using TriPure Isolation Reagent (Roche Applied Science), according to the manufacturer’s protocol. One μg aliquot of total RNA from each sample was reverse transcribed into single-stranded cDNA using random hexanucleotides primers and expand reverse transcriptase (Roche Applied Science). cDNA for each sample was subjected to quantitative real-time PCR using the following primers for HPRT internal quantitative control forward 5′-CCTGGCGTCGTGATTAGTGAT-3′, reverse 5′-AGACGTTCAGTCCTGTCCATAA-3′ and TGF-β, forward 5′-CGACTACTACGCCAAGGA-3′ and reverse 5′-GAGAGCAACACGGGTTCA-3′ primers and IL-23, forward 5′-GGACAACAGTCAGTTCTGCTT-3′ and reverse 5′-CACAGGGCTATCAGGGAGC-3′.
Quantitative PCR
All quantitative PCR reactions were performed in 20 μl reaction mixtures containing 250 ng cDNA, 10 ml Takara Real-Time™ SYBR Green/ROX PCR Master, primer pairs and nuclease-free water to 20 ml. Each biological replicate was run in duplicate on an ABI Step One quantitative PCR system. Thermocycling conditions consisted of an initial polymerase activation step at 95°C for 10 min, followed by 40 cycles at 95°C for 5 s and 60°C for 30 s. Afterwards, melting curves were generated to confirm a single gene-specific peak and to detect primer dimmer formation.
Statistical analysis
Gene expression data were normalized against HPRT as reference gene. Data analysis was performed using the 2−ΔΔCT method. The significance of differences between control and test groups was established by t-test using SPSS software. The significance level was set at P < 0.05.
Results
Patients with T1DM were grouped as juvenile-onset T1DM (N = 20) with age at diagnosis <18 years and adult-onset T1DM (N = 20) with the age at onset >18 years. Duration of diabetes was 1.4 ± 1.6 years in juvenile-onset T1DM and 1.9 ± 1.7 in adult-onset T1DM. The characteristics of patients are given in Table 1.
TGF-β gene expression in different groups of patients with diabetes compared to the controls
A significant decrease in TGF-β gene expression was observed in T1DM compared to the controls (P = 0.02; 95% CI: 0.4–5.9). There was no significant difference in TGF-β gene expression between T2DM and controls (Fig. 1).
TGF-β gene expression in PBMCs of patients with diabetes. a There was a significant decrease in TGF-β expression in T1DM compared to the controls (P = 0.02) and compared to T2DM (P < 0001). b There were significant decreases for TGF-β expression in both types of early-onset T1DM and late-onset T1DM compared to the controls and T2DM. There were no significant differences between early-onset T1DM late-onset T1DM
TGF-β gene expression in patients with adult-onset T1DM was lower than patients with juvenile-onset T1DM, however, this did not reach significance level (P = 0.1). TGF-β gene expression was significantly decreased in patients with T1DM compared to patients with T2DM (P < 0.001; 95% CI: 0.6–2.1) (Fig. 1).
IL-23 gene expression in different groups of patients with diabetes compared to the controls
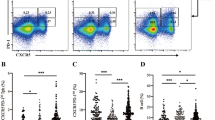
There was a significant decrease in IL-23 gene expression in patients with T2DM compared to the controls (P = 0.004). IL-23 gene expression was significantly increased in patients with T1DM compared to patients with T2DM (P = 0.02) but not compared to the controls (P = 0.1). The difference for IL-23 gene expression between early-onset T1DM and T2DM was significant (P = 0.004), whilst the difference between late-onset T1DM and T2DM was less significant (P = 0.05). There was no significant difference for IL-23 gene expression in patients with adult-onset T1DM and juvenile-onset T1DM (P = 0.4) (Fig. 2).
IL-23 gene expression in PBMCs of patients with diabetes. a There was a significant increase in IL-23 gene expression in patients with T1DM compared to T2DM (P = 0.01). IL-23 was significantly decreased in patients with T2DM compared to the controls (P = 0.004). b IL-23 gene expression was higher in patients with early-onset T1DM than late-onset T1DM but there were no significant differences
Discussion
We observed that TGF-β gene expression is significantly lower in fresh PBMCs derived from both adult-onset and juvenile-onset T1DM compared to patients with T2DM and normal healthy controls. Whilst IL-23 gene expression was significantly increased in T1DM compared to T2DM. Therefore, IL-23 and TGF-β seems to have contradictory role in pathogenesis of diabetes.
Activated monocytes play an important role in the pathogenesis of type 1 diabetes. Inflammatory monocytes are also involved in the pathogenesis of type 2 diabetes [17, 18]. Recently, the interests have risen for immunotherapy of T1DM and suppression of immune reaction by targeting autoreactive T cells and T regulatory cells (Tregs). Expressions of several pro- and anti-inflammatory cytokines including TGF-β have been observed in Tregs of patients with type 1 diabetes [9].
An imbalance between Th1/Th2 immune response has been known as the underlying mechanism in development of autoimmune disorders. However, recent evidence suggests the involvement of Th17 CD4+ T cells subtype differentiated from naïve T cells as a result of signals from combination of TGF-β1, IL-6, IL-21, IL-1beta and IL-23 [13]. IL-17-producing T cells are responsible for many of the inflammatory and autoimmune responses [11]. Recently it has been observed that IL-23 induces pathogenic IL-17 producing CD8+ T cells in autoimmune diabetes (Tc17) [11]. Our data emphasize the role of Th17 pathway involved in both type of diabetes, which requires further assessment. Analysis of T cell subsets in various groups of diabetes might be helpful to identify mechanisms involved in disease pathogenesis.
Previous reports indicate the existence of heterogeneity in the genetic, immune and metabolic characteristics of adult and juvenile forms of type 1 diabetes [17, 19]. Recent studies have observed distinct pattern of inflammatory gene expression in peripheral monocytes of diabetes patients depending on clinical manifestations and age at diagnosis [17, 20]. Low concordance rate in twin studies for adult-onset T1DM indicates small impact of genetic risk in susceptibility to adult-onset T1DM and latent autoimmune diabetes of adults (LADA) which is primarily presenting with non-insulin requiring diabetes. However, beside the low twin concordance rate both types show association with HLA genes [19] indicating the high impact of immune system deregulation in susceptibility to T1DM in adults. It is necessary to examine Th17 cytokines expression profile and T cell subsets in patients with different types of diabetes to find out the exact role of Th17 pathway in susceptibility to T2DM and T1DM diabetes at different age. It will be also interesting to examine the association between Th17 cytokines expression and diabetes associated auto-antibodies in adult-onset and juvenile-onset T1DM and also in patients with LADA. Cytokines produced in Th17 pathways might be implicated in clinical manifestation of diabetes and could be identified as a marker to distinguish between various forms of diabetes at different age at onset. More studies are required to further confirm the data we have observed in this study.
References
W.A. Border, N.A. Noble, Targeting TGF-beta for treatment of disease. Nat. Med. 1, 1000–1001 (1995)
D. Fujii, J.E. Brissenden, R. Derynck, U. Francke, Transforming growth factor beta gene maps to human chromosome 19 long arm and to mouse chromosome 7. Somat. Cell Mol. Genet. 12, 281–288 (1986)
C.A. Piccirillo, Y. Chang, G.J. Prud’homme, TGF-beta1 somatic gene therapy prevents autoimmune disease in nonobese diabetic mice. J. Immunol. 161, 3950–3956 (1998)
C. King, J. Davies, R. Mueller, M.S. Lee, T. Krahl, B. Yeung, E. O’Connor, N. Sarvetnick, TGF-beta1 alters APC preference, polarizing islet antigen responses toward a Th2 phenotype. Immunity 8, 601–613 (1998)
M. Moritani, K. Yoshimoto, S.F. Wong, C. Tanaka, T. Yamaoka, T. Sano, Y. Komagata, J. Miyazaki, H. Kikutani, M. Itakura, Abrogation of autoimmune diabetes in nonobese diabetic mice and protection against effector lymphocytes by transgenic paracrine TGF-beta1. J. Clin. Invest. 102, 499–506 (1998)
H.S. Han, H.S. Jun, T. Utsugi, J.W. Yoon, A new type of CD4+ suppressor T cell completely prevents spontaneous autoimmune diabetes and recurrent diabetes in syngeneic islet-transplanted NOD mice. J. Autoimmun. 9, 331–339 (1996)
S. You, M. Alyanakian, B. Segovia, D. Damotte, J. Bluestone, J. Bach, L. Chatenoud, Immunoregulatory pathways controlling progression of autoimmunity in NOD mice. Ann. N. Y. Acad. Sci. 1150, 300–310 (2008)
P.Y. Mantel, C.B. Schmidt-Weber, Transforming growth factor-beta: recent advances on its role in immune tolerance. Methods Mol. Biol. 677, 303–338 (2011)
W. Łuczyński, A. Stasiak-Barmuta, A. Juchniewicz, N. Wawrusiewicz-Kurylonek, E. Iłendo, J. Kos, A. Kretowski, M. Górska, L. Chyczewski, A. Bossowski, The mRNA expression of pro- and anti-inflammatory cytokines in T regulatory cells in children with type 1 diabetes. Folia Histochem. Cytobiol. 1(48), 93–100 (2010)
M. Halminen, O. Simell, M. Knip, J. Ilonen, Cytokine expression in unstimulated PBMC of children with type 1 diabetes and subjects positive for diabetes-associated autoantibodies. Scand. J. Immunol. 53, 510–513 (2001)
M. Kunz, S.M. Ibrahim, Cytokines and cytokine profiles in human autoimmune diseases and animal models of autoimmunity. Mediat. Inflamm. 97, 92–98 (2009)
X. Gao, G. Ding, Z. Wang, H. Fu, Z. Ni, J. Ma, S. Song, F. Liu, Z. Fu, Adjuvant treatment suppresses IL-17 production by T cell-independent myeloid sources in nonobese diabetic mice. Mol. Immunol. 47(14), 2397–2404 (2010)
V.S. Costa, T.C. Mattana, M.E. da Silva, Unregulated IL-23/IL-17 immune response in autoimmune diseases. Diabetes Res. Clin. Pract. 88, 222–226 (2010)
B. Ciric, M. El-behi, R. Cabrera, G.X. Zhang, A. Rostami, IL-23 drives pathogenic IL-17-producing CD8+ T cells. J. Immunol. 182(9), 5296–5305 (2009)
S.M. Wahl, Transforming growth factor beta: the good, the bad, and the ugly. J. Exp. Med. 180, 1587–1590 (1994)
C.M. Filippi, A.E. Juedes, J.E. Oldham, E. Ling, L. Togher, Y. Peng, R.A. Flavell, M.G. von Herrath, Transforming growth factor-beta suppresses the activation of CD8+ T-cells when naive but promotes their survival and function once antigen experienced: a two-faced impact on autoimmunity. Diabetes 57(10), 2684–2692 (2008)
R.C. Padmos, N.C. Schloot, H. Beyan, C. Ruwhof, F.J. Staal, D. de Ridder, H.J. Aanstoot, W.K. Lam-Tse, H. de Wit, C. de Herder, R.C. Drexhage, B. Menart, R.D. Leslie, H.A. Drexhage, LADA Consortium, Distinct monocyte gene-expression profiles in autoimmune diabetes. Diabetes 57, 2768–2773 (2008)
J.C. Pickup, Inflammation and activated innate immunity in the pathogenesis of type 2 diabetes. Diabetes Care 27, 813–823 (2004)
R.D. Leslie, M. Delli Castelli, Age-dependent influences on the origins of autoimmune diabetes: evidence and implications. Diabetes 53, 3033–3040 (2004)
E. Korpinen, P.H. Groop, J.A. Fagerudd, A.M. Teppo, H.K. Akerblom, O. Vaarala, Increased secretion of TGF-beta1 by peripheral blood mononuclear cells from patients with Type 1 diabetes mellitus with diabetic nephropathy. Diabet. Med. 18(2), 121–125 (2001)
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Abbasi, F., Amiri, P., Sayahpour, F.A. et al. TGF-β and IL-23 gene expression in unstimulated PBMCs of patients with diabetes. Endocrine 41, 430–434 (2012). https://doi.org/10.1007/s12020-011-9578-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-011-9578-7