Abstract
Polycystic ovary syndrome (PCOS) is characterized by the presence of hyperandrogenism and an increased follicular mass probably determined by deregulation of locally produced factors. Anti-Müllerian hormone (AMH) is a glycoprotein that inhibits follicular recruitment and determines the size of the follicular pool. To evaluate the role of androgens in the regulation of AMH expression in bovine granulosa cells from small follicles, granulosa cells from 3 to 4 mm follicles were isolated and incubated in basal culture media, or in media containing testosterone (T) at 10−5M, T 10−8M, or estradiol (E2) at 150 ng/ml for 48 h. AMH mRNA levels of these cells were determined using real-time PCR (RT PCR). AMH protein levels and E2 were determined in cell-conditioned media. A 3.4-fold decrease in AMH mRNA levels was observed in granulosa cells exposed to T 10−5M (P = 0.03, n = 5), but not in cells exposed to T 10−8M. AMH protein levels showed a 1.8-fold reduction in cell-conditioned media from cells exposed to T 10−5M (P = 0.01, n = 5), without significant changes in the group exposed to T 10−8M. Cells treated with E2 150 ng/ml showed no change in AMH protein levels. We propose that AMH expression is modulated by androgens in bovine granulosa cells from small follicles. Thus, it is possible to speculate that androgens, by inhibiting AMH expression, may promote follicle recruitment, increasing the early growing follicular pool. This new mechanism may have implications for the understanding of PCOS pathophysiology.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Polycystic ovary syndrome (PCOS) is a highly prevalent (5–10%) endocrine-metabolic dysfunction in premenopausal women and is the most frequent cause of anovulatory infertility and hyperandrogenism in women. Ovarian morphology assessed by ultrasound and by histological examination has shown that polycystic ovaries are characterized by an excessive number of growing follicles compared with normal ovaries [1, 2], suggesting an altered folliculogenesis in this syndrome.
In previous studies we have found that daughters of women with PCOS exhibit higher levels of AMH, a marker of growing follicles, compared with control girls [3, 4]. This suggests that the follicular alterations described in adult PCOS women may appear early during development. Nevertheless, the origin of this higher follicular mass is still unknown.
To have a better comprehension of this phenomenon, it is important to understand the mechanisms involved in follicular recruitment dynamics.
During normal folliculogenesis a cohort of follicles grow from the primary stage to the size at which they become visible at ultrasonography (2 mm diameter). This initial stage is independent of gonadotropins. It proceeds further to the selection of the dominant follicle and culminates with ovulation, which are gonadotropin-dependent processes.
Two kinds of derangement in folliculogenesis have been described in PCOS: excessive early follicular growth and impaired selection and ovulation due to follicular arrest [5]. It has been hypothesized that the increased number of small follicles present in PCOS is due to the trophic effects of androgens, whether increased locally in the ovary, or systemically, as has been observed in prenatal androgenization experimental models [6, 7]. This increased follicular mass, through the secretion of locally produced factors, could interfere with the normal process of follicular selection and ovulation [5]. One of the factors that has been proposed as possible mediators of these follicular derangements is the anti-Müllerian hormone.
Anti-Müllerian hormone (AMH), also called Müllerian inhibiting substance (MIS), is a dimeric glycoprotein member of the TGFβ superfamily [8]. AMH is produced exclusively in the gonads [9] and its sexually dimorphic expression in the ovary and testis is crucial for the normal differentiation of reproductive structures.
In the ovary, the expression of AMH starts in the columnar granulosa cells of primary follicles [10]. Its expression increases until the follicle reaches a diameter of 4 mm and diminishes progressively during the subsequent stages of development [10].
Experimental studies performed in rodents have shown that AMH has an inhibitory effect on primordial follicle recruitment [11]. In addition, other studies have demonstrated that AMH affects FSH sensitivity of growing follicles during the selection process [12, 13]. Therefore AMH seems to be an important regulatory factor involved both in the determination of the size of the follicular mass and the process of selection and subsequent ovulation. Thus, to understand the pathophysiology of this increased follicular mass in PCOS, it becomes very important to identify factors that may regulate AMH expression in the ovary, which are, to our knowledge, currently unknown.
One suitable candidate regulator for AMH is testosterone. Androgens reduce the expression of AMH in Sertoli cells [14]. This is based on the fact that there is an inverse correlation between AMH and testosterone systemic levels during male development, with increasing levels of testosterone and decreasing levels of AMH. This relationship is more accurately seen when intra-testicular testosterone concentrations are compared with systemic AMH levels [14, 15]. The mechanisms involved in this regulation are not clear.
It is known that the intra-ovarian androgen concentrations are higher in PCOS, which could be associated with the increased size of the follicular pool characteristically seen in these women [16]. If androgens are capable of regulating AMH expression, in vitro, in granulosa cells, this may constitute a possible mechanism for androgens to regulate the size of the follicular pool.
The aim of the present study is to determine if androgens are able to regulate AMH expression, in vitro, in bovine granulosa cells from small antral follicles placed in culture. The bovine ovary is morphologically and physiologically very similar to its human homolog, so it constitutes a good model for the study of the regulation of AMH [17, 18].
Results
There was a significant reduction in AMH mRNA levels in granulosa cells exposed to T 10−5M, with a 3.4-fold decrease compared to AMH mRNA levels in granulosa cells incubated in basal media (ratio: 0.29 ± 0.04, mean ± SEM; Kruskal–Wallis; P = 0.03; Dunn’s test Basal versus T 10−5M P < 0.05; n = 5) (Fig. 1). Cells exposed to T 10−8M showed no significant difference with the basal sample.
AMH mRNA levels normalized for 18s mRNA and calibrated by the basal sample, in cultured granulosa cells from 3 to 4 mm bovine follicles exposed to testosterone (T)10−5M and 10−8M for 48 h. Each measurement corresponds to RNA extracted from two independent equivalent experiments. * Significant difference between basal and T 10−5M (Kruskal Wallis, P = 0.03). Basal AMH/18s ratio: 0.016 ± 0.009 (mean ± SEM)
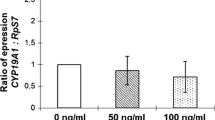
AMH protein secretion measured in cell-conditioned media from the same experiments showed a 1.8-fold reduction in media from cells exposed to T 10−5M (ratio = 0.55 ± 0.03; Kruskal–Wallis; P = 0.01, n = 5), without significant changes in the group exposed to T 10−8M (Fig. 2).
AMH protein levels normalized by the basal sample, measured in cell-conditioned media from cultured granulosa cells from 3 to 4 mm bovine follicles exposed to testosterone (T)10−5M and 10−8M for 48 h. * Significant difference between basal and T 10−5M (Kruskal Wallis, P = 0.01). Basal AMH (ng/ml):0.24 ± 0.03 (mean ± SEM)
To determine if E2 locally produced from T by granulosa cells was responsible for the changes observed in the expression of AMH, the amount of E2 produced in cell-conditioned media from cells exposed to T 10−5M was determined. The amount of E2 measured was very low, showing little aromatase activity in these cells, but was significantly higher than the amount measured in the basal sample (basal: 35.7 ± 9.3 pg/ml vs. T 10−5M: 130 ± 15.3 pg/ml, Mann–Whitney, P = 0.028; n = 5) (Fig. 3).
To determine if this amount of E2 was able to decrease AMH production, granulosa cells from 3 to 4 mm follicles were incubated for 48 h with the highest concentration of E2 measured in the previous experiments (150 pg/ml) or with basal media. AMH was measured by ELISA in cell-conditioned media from these experiments, showing no significant differences between basal and stimulated cells (basal: 0.62 ± 0.18 vs. estradiol: 0.77 ± 0.23 ng/ml, mean ± SEM, Mann–Whitney, P = 0.169; n = 6) (Fig. 4).
Discussion
In the present study, using a technique previously described for human ovaries [19, 20], we were able to isolate small follicles and granulosa cells from bovine tissue, and to demonstrate for the first time a direct regulatory effect of testosterone on AMH expression in the mammal ovary.
The bovine ovary is, in many aspects, very similar to the human. Both species are monovulatory and have an initial non-gonadotropin-dependent stage of development for follicles <2–5 mm in humans and <3–4 mm in cattle [18]. During this period, the peak in AMH expression is reached in both species [10, 21]. When the follicle reaches this size, cyclic FSH recruitment is necessary to continue growth. In humans, a single rise in FSH levels selects the dominant follicle. In cattle for each cycle there may be 2–3 FSH surges, each one determining the recruitment of 8–41 small follicles, but only the one that coincides with the onset of luteolysis (LH surge) determines ovulation of the dominant follicle [18]. In both species, as follicles enter the gonadotropin-dependent stage of growth, they significantly decrease their AMH expression [10, 21].
Our study focuses in the non-gonadotropin stage of development which operates in a very similar manner in both species. Nonetheless, there may be many interspecies differences in AMH regulation and one has to be careful in extrapolating this data directly to the human.
As follicles of different sizes differ in their level of expression of the androgen receptor [22, 23] and of AMH [10, 21], in the present study we chose a narrow range of follicle sizes using only follicles between 3 and 4 mm which, as described in the literature, express the highest amount of AMH compared to follicles in other stages [21], and are big enough to be dissected and provide a proper amount of granulosa cells for culture. T concentrations used in this study were chosen based on studies performed in human ovarian tissue, in which intra-follicular T concentrations in normal 2–5 mm follicles are around 10−8M and in PCOS follicles are around 10−5M [16].We have found that using a concentration of T similar to that described in small follicles from PCOS ovaries, granulosa cells respond with a lower production of AMH, while when we use a “physiologic” androgen concentration there is no significant change. This could mean that when follicles are exposed to a high androgen concentration, AMH is, at least locally, downregulated.
E2 production in this system is very low. Nevertheless it rises significantly when T is added. To rule out the fact that the effect observed was due to E2, we incubated granulosa cells with the highest concentration measured in cell-conditioned media from cells exposed to T 10−5M, which was 150 ng/ml. Media from cells exposed to E2 150 ng/ml showed no significant change in AMH protein levels. Thus, the effect observed with T was most probably an androgenic effect and not a secondary estrogenic effect. Although a possible synergistic effect of E2 with T cannot be ruled out as aromatase inhibitor studies were not performed.
It has been shown that T promotes the growth of bovine follicles in vitro [23]. On the other hand, AMH has been shown to decrease follicular recruitment [24]. Our data suggest that a possible mechanism by which androgens may promote follicular development in mammals is by decreasing AMH expression in granulosa cells.
It would be possible to suggest that androgens synthesized in the ovary are able to produce a gentle decrease in the local production of AMH by granulosa cells from follicles at the initial stages of development, lowering the threshold for follicular recruitment and therefore allowing more follicles to enter the non-gonadotropin-dependent stage of growth.
As mentioned previously, there are two types of derangement in PCOS folliculogenesis: excessive early follicular growth and impaired selection and ovulation due to follicular arrest. It has been hypothesized that the increased number of small follicles in these patients is due to the trophic effects of androgens locally increased in the ovary [5]. Modulation of AMH by androgens may be one of the mechanisms involved in the generation of an increased follicular mass in these patients. Further studies in human tissue from control and PCOS patients may clarify this issue.
Recently Pellat et al. [20], using the same technique of the present study, found an increased basal AMH in vitro production in granulosa cells from PCOS patients. As in PCOS the local ovarian androgen production is increased, there seems to be apparent discrepancy with our results. Nevertheless, our study shows an in vitro response in the expression of AMH in granulosa cells from normal mammal ovaries. The ovarian physiology in PCOS patients differs in many aspects from normal ovarian physiology. PCOS preantral follicles show a prolonged survival [25], granulosa cells respond prematurely to LH [26] and display increased aromatase activity [27]. Moreover, the chronic exposure to androgens may have long-term effects that have not been addressed in our study. Further investigation regarding the response of PCOS granulosa cells to androgens may clarify this issue.
In summary, using a bovine model we have found that androgens downregulate AMH expression in granulosa cells from small antral follicles. These data may suggest new mechanisms for follicular recruitment in mammals which may contribute to the understanding of PCOS pathophysiology.
Methods
Ovarian dissection
Ovaries were obtained at a local abattoir after approval from the local livestock authority (SAG). Immediately after killing, ovaries from 1–2-year-old cows were washed and placed in Medium 199 (M199, Hyclone, Logan, UT), previously prewarmed at 39°C, and transported to the laboratory. To isolate follicles and granulosa cells, we adapted a previously described procedure for human ovaries [19, 20]. Follicles were isolated from the surrounding stroma under sterile conditions using binocular microscopy. Follicle diameters were measured with calipers before the follicular fluid was aspirated. Only 3–4 mm follicles from the same ovary were used for the rest of the study. Follicular fluid was aspirated with a 26-gauge needle and stored. A crosswise incision into the follicle was then made to expose the granulosa cell layer, which was flushed away from the theca with a stream of M 199 and collected (Fig. 5). All the granulosa cells from 3 to 4 mm follicles of the same ovary were pooled together and centrifuged for 10 min at 1500 rpm. The supernatant was discarded and the cells were resuspended in fresh prewarmed media.
Sixteen ovaries were dissected. An average of 12.3 follicles of 3–4 mm was obtained from each ovary, which yielded approximately 300,000 total granulosa cells per ovary. As 100,000 cells were required for each well, one basal and one or two experimental wells were incubated in each experiment.
Granulosa cell cultures
Resuspended cells were counted using Tripan blue exclusion and plated out at a density of 1 × 105 viable cells/well in 96-well plates with 300 µl of M199 supplemented with penicillin/streptomycin (Hyclone, Logan, UT) and amphotericin (Hyclone, Logan, UT). Cells were incubated at 39°C (normal body temperature for cows) in 95% air–5% CO2 in a humidified incubator for 24 h. After the first 24 h, media was changed and cells were incubated for 48 h in basal media or in the presence of either 10−8M or 10−5M testosterone (Merck Darmstadt, Germany). To differentiate the potential effect of E2 produced by aromatization of T, we determined the exact amount of E2 produced by the cells incubated with T 10−5M, and we incubated cells in the presence of the determined amount of estradiol (Sigma, St Louis, MO). After the incubation period, media was collected and stored at −20°C. Cells were collected with a 4 M guanidinium thiocyanate (Sigma, St Louis, MO) denaturing solution containing 0.1 M 2-mercaptoethanol (Merck, Darmstadt, Germany), homogenized by pipetting, and stored at −80°C. Cells collected from two equivalent wells from two different experiments were pooled together for RNA extraction, in order to obtain enough material for real-time PCR (RT PCR) amplification.
RNA extraction and RT PCR
The amount of total RNA obtained from two wells ranged from 1 to 3 µg, which was enough to produce a good amplification in RT PCR reactions for both amplicons.
Homogenates were defrosted on ice, RNA was extracted using the Chomczynski and Sacchi method and stored at −80°C [28]. To remove DNA contamination, RNA was treated with 1 µ/µg of RNA RQ1 RNAse-free DNAse (Promega, Madison, WI) following manufacturer’s instructions. This reaction mixture was incubated at 37°C for 30 min, heated for 5 min at 75°C to inactivate the DNase, and placed immediately on ice for 5 min. For reverse transcription, the total amount of RNA (1–3 µg) from each sample was heated for 5 min at 75°C, placed on ice, and then incubated for 10 min at 25°C with 1.6 mM deoxynucleotide triphosphate, 10 mM dithiothreitol, 176 nM random hexamers (Invitrogen Corp, Carlsbad, CA), and 25 U RNaseOUT (Invitrogen Corp, Carlsbad, CA).Temperature was raised to 42°C and 125 U of Superscript II Reverse Transcriptase (Invitrogen Corp, Carlsbad, CA) was added to each tube. After 1 h of incubation, the reaction was terminated by heating the samples at 75°C for 10 min. cDNA samples were stored at −20°C. Samples were used for RT PCR reactions for AMH mRNA and 18s mRNA as a housekeeping gene. The following primers were used for bovine AMH: forward: 5′-TCA-TCC-CCG-AGA-CAT-ACC-3′; reverse: 5′-ACC-ATG-TTT-GGG-ACG-TGG-3′; and 18s mRNA: forward: 5′-TCA-AGA-ACG-AAA-GTC-GGA-GG-3′; reverse 5′-GGA-CAT-CTA-AGG-GCA-TCA-CA-3′. Amounts of 18s mRNA were determined using a commercially available RT primer pair (Ambion, Austin, TX). Samples of cDNA were subjected to amplification using 2× Brilliant II Sybr green mastermix (Stratagene, La Jolla, CA), 0.1 µM each 18s mRNA primer or 0.16 µM each AMH primer in a total volume of 25 µl. The reactions were carried out in a Stratagene Mx3000P QPCR System (Stratagene, La Jolla, CA) using the following protocol: a denaturation step at 95°C for 10 min; 40 cycles of a three step amplification, including denaturation at 95°C for 30 s, annealing at 60°C for 30 s, and extension at 72°C for 30 s; a melting curve program (72–95°C) with continuous fluorescence measurement; and a final cooling step to 25°C. Data acquisition was carried out at the end of the extension step.
The size of the amplicons obtained was verified by using a 2% agarose electrophoresis in which a 489 bp band and a 212 bp band were obtained for the 18s mRNA and AMH amplicons, respectively. Reactions containing no template or no reverse transcriptase showed no amplification ruling out DNA contamination.
In the melting curve program a single amplicon was obtained at 84°C for 18s mRNA and at 90°C for AMH in all samples. Dilutions of cDNA amplified for AMH and 18s mRNA from bovine testicle samples were used to produce standard curves for 18s mRNA and AMH. These curves were used to calculate the efficiency of the RT PCR reaction for each amplicon. The MxPro Program was used to analyze the data. Efficiencies from the standard curves and Cts for AMH and 18s mRNA from basal and experimental (stimulated with testosterone) samples were used for the calculation of the AMH/18s mRNA ratio, calibrated by the basal sample using the following formula:
where E AMH is the efficiency of amplification for AMH, E 18s mRNA is the efficiency of amplification for 18s mRNA, Ct basal is the Ct for the corresponding amplicon in the basal condition, and Ct exp is the Ct for the corresponding amplicon in the experimental condition. Standard curves for both genes were used to calculate efficiencies. The efficiency was 94.7% for AMH and 94.2% for 18s mRNA.
Measurement of AMH and estradiol in cell-conditioned media
Cell-conditioned media from the same experiments described above was used for the determination of AMH concentration using a serum-based enzyme-linked immunosorbent (ELISA) kit (Diagnostic Systems Laboratories, Texas, USA). This ELISA was validated for the measurement of bovine AMH using culture media mixed with cow follicular fluid samples (which was the best available source of bovine AMH protein) from 3 to 4 mm follicles which were diluted in parallel with serum-based standards (r 2 = 0.989). The assay sensitivity was 0.006 ng/ml and the intra- and inter-assay coefficients of variation were 4.6 and 8.0%, respectively. This kit has been previously used for the measurement of bovine AMH in other studies [21].
The protein levels were measured by method of Bradford [29] and each experiment was normalized for the basal sample to calculate the fold increase or decrease for each case.
Cell-conditioned media from cells stimulated with T 10−5M or basal media was used for the determination of E2 by electrochemiluminiscence, using an automatic analyzer Roche Elecsys 1010 (Roche, Basel, Switzerland). The assay sensitivity was 5.0 pg/ml and the intra- and inter-assay coefficients of variation were 2.7 and 5.0%, respectively.
Statistical analysis
Data were analyzed using the Graph Pad Prism 5 package. For comparisons between 3 or more groups, Kruskal–Wallis statistics with Dunn’s post-test was used. Mann–Whitney test was used for comparisons between two groups. A P value <0.05 was considered significant.
References
L.J. Webber, S. Stubbs, J. Stark, G.H. Trew, R. Margara, K. Hardy, S. Franks, Formation and early development of follicles in the polycystic ovary. Lancet 362, 1017–1021 (2003)
S. Jonard, Y. Robert, C. Cortet-Rudelli, P. Pigny, C. Decanter, D. Dewailly, Ultrasound examination of polycystic ovaries: is it worth counting the follicles? Hum. Reprod. 18, 598–603 (2003)
T. Sir-Petermann, E. Codner, M. Maliqueo, B. Echiburu, C. Hitschfeld, N. Crisosto, F. Perez-Bravo, S.E. Recabarren, F. Cassorla, Increased anti-Mullerian hormone serum concentrations in prepubertal daughters of women with polycystic ovary syndrome. J. Clin. Endocrinol. Metab. 91, 3105–3109 (2006)
N. Crisosto, E. Codner, M. Maliqueo, B. Echiburu, F. Sanchez, F. Cassorla, T. Sir-Petermann, Anti-Mullerian hormone levels in peripubertal daughters of women with polycystic ovary syndrome. J. Clin. Endocrinol. Metab. 92, 2739–2743 (2007)
S. Jonard, D. Dewailly, The follicular excess in polycystic ovaries, due to intra-ovarian hyperandrogenism, may be the main culprit for the follicular arrest. Hum. Reprod. Update 10, 107–117 (2004)
A. Gougeon, Regulation of ovarian follicular development in primates: facts and hypotheses. Endocr. Rev. 17, 121–155 (1996)
D.H. Abbott, D.K. Barnett, C.M. Bruns, D.A. Dumesic, Androgen excess fetal programming of female reproduction: a developmental aetiology for polycystic ovary syndrome? Hum. Reprod. Update 11, 357–374 (2005)
N. Josso, N. di Clemente, TGF-beta family members and gonadal development. Trends Endocrinol. Metab. 10, 216–222 (1999)
M.M. Lee, P.K. Donahoe, Mullerian inhibiting substance: a gonadal hormone with multiple functions. Endocr. Rev. 14, 152–164 (1993)
C. Weenen, J.S. Laven, A.R. Von Bergh, M. Cranfield, N.P. Groome, J.A. Visser, P. Kramer, B.C. Fauser, A.P. Themmen, Anti-Mullerian hormone expression pattern in the human ovary: potential implications for initial and cyclic follicle recruitment. Mol. Hum. Reprod. 10, 77–83 (2004)
A.L. Durlinger, M.J. Gruijters, P. Kramer, B. Karels, H.A. Ingraham, M.W. Nachtigal, J.T. Uilenbroek, J.A. Grootegoed, A.P. Themmen, Anti-Mullerian hormone inhibits initiation of primordial follicle growth in the mouse ovary. Endocrinology 143, 1076–1084 (2002)
A.L. Durlinger, M.J. Gruijters, P. Kramer, B. Karels, T.R. Kumar, M.M. Matzuk, U.M. Rose, F.H. de Jong, J.T. Uilenbroek, J.A. Grootegoed, A.P. Themmen, Anti-Mullerian hormone attenuates the effects of FSH on follicle development in the mouse ovary. Endocrinology 142, 4891–4899 (2001)
N. di Clemente, B. Goxe, J.J. Remy, R.L. Cate, N. Josso, B. Vigier, R. Salesse, Inhibitory effect of AMH upon aromatase activity and LH receptors of granulosa cells of rat and porcine immature ovaries. Endocrine 2, 553–558 (1994)
L. Al-Attar, K. Noel, M. Dutertre, C. Belville, M.G. Forest, P.S. Burgoyne, N. Josso, R. Rey, Hormonal and cellular regulation of Sertoli cell anti-Mullerian hormone production in the postnatal mouse. J. Clin. Invest. 100, 1335–1343 (1997)
R. Rey, I. Lordereau-Richard, J.C. Carel, P. Barbet, R.L. Cate, M. Roger, J.L. Chaussain, N. Josso, Anti-mullerian hormone and testosterone serum levels are inversely during normal and precocious pubertal development. J. Clin. Endocrinol. Metab. 77, 1220–1226 (1993)
K.P. McNatty, D.M. Smith, A. Makris, C. DeGrazia, D. Tulchinsky, R. Osathanondh, I. Schiff, K.J. Ryan, The intraovarian sites of androgen and estrogen formation in women with normal and hyperandrogenic ovaries as judged by in vitro experiments. J. Clin. Endocrinol. Metab. 50, 755–763 (1980)
M. Mihm, A.C. Evans, Mechanisms for dominant follicle selection in monovulatory species: a comparison of morphological, endocrine and intraovarian events in cows, mares and women. Reprod. Domest. Anim. 43(Suppl 2), 48–56 (2008)
G.P. Adams, R. Jaiswal, J. Singh, P. Malhi, Progress in understanding ovarian follicular dynamics in cattle. Theriogenology 69, 72–80 (2008)
H.D. Mason, R. Margara, R.M. Winston, R.W. Beard, M.J. Reed, S. Franks, Inhibition of oestradiol production by epidermal growth factor in human granulosa cells of normal and polycystic ovaries. Clin. Endocrinol. (Oxf) 33, 511–517 (1990)
L. Pellatt, L. Hanna, M. Brincat, R. Galea, H. Brain, S. Whitehead, H. Mason, Granulosa cell production of anti-Mullerian hormone is increased in polycystic ovaries. J. Clin. Endocrinol. Metab. 92, 240–245 (2007)
D. Monniaux, N. Clemente, J.L. Touze, C. Belville, C. Rico, M. Bontoux, J.Y. Picard, S. Fabre, Intrafollicular steroids and anti-mullerian hormone during normal and cystic ovarian follicular development in the cow. Biol. Reprod. 79, 387–396 (2008)
S.G. Hillier, M. Tetsuka, H.M. Fraser, Location and developmental regulation of androgen receptor in primate ovary. Hum. Reprod. 12, 107–111 (1997)
M.Y. Yang, J.E. Fortune, Testosterone stimulates the primary to secondary follicle transition in bovine follicles in vitro. Biol. Reprod. 75, 924–932 (2006)
A.L. Durlinger, P. Kramer, B. Karels, F.H. de Jong, J.T. Uilenbroek, J.A. Grootegoed, A.P. Themmen, Control of primordial follicle recruitment by anti-Mullerian hormone in the mouse ovary. Endocrinology 140, 5789–5796 (1999)
L.J. Webber, S.A. Stubbs, J. Stark, R.A. Margara, G.H. Trew, S.A. Lavery, K. Hardy, S. Franks, Prolonged survival in culture of preantral follicles from polycystic ovaries. J. Clin. Endocrinol. Metab. 92, 1975–1978 (2007)
D.S. Willis, H. Watson, H.D. Mason, R. Galea, M. Brincat, S. Franks, Premature response to luteinizing hormone of granulosa cells from anovulatory women with polycystic ovary syndrome: relevance to mechanism of anovulation. J. Clin. Endocrinol. Metab. 83, 3984–3991 (1998)
H.D. Mason, D.S. Willis, R.W. Beard, R.M. Winston, R. Margara, S. Franks, Estradiol production by granulosa cells of normal and polycystic ovaries: relationship to menstrual cycle history and concentrations of gonadotropins and sex steroids in follicular fluid. J. Clin. Endocrinol. Metab. 79, 1355–1360 (1994)
P. Chomczynski, N. Sacchi, Single-step method of RNA isolation by acid guanidinium thiocyanate-phenol-chloroform extraction. Anal. Biochem. 162, 156–159 (1987)
M.M. Bradford, A rapid and sensitive method for the quantitation of microgram quantities of protein utilizing the principle of protein-dye binding. Anal. Biochem. 72, 248–254 (1976)
Acknowledgments
We would like to thank Dr. Helen Mason and her colleagues at St. Georges University of London, for their instruction regarding follicle dissection and granulosa cell culture techniques. We would also like to thank Mr. Herman Rodriguez at the local abattoir for his help with the extraction of bovine ovaries. This work was supported by grants from: CONICYT 23070163 to partially support the Ph.D. thesis (to NC), FONDECYT: 1071007 (to TS-P), and 1090036 (to HL). NC is recipient of a Ph.D. MD fellowship from the Faculty of Medicine of the University of Chile.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Crisosto, N., Sir-Petermann, T., Greiner, M. et al. Testosterone-induced downregulation of anti-Müllerian hormone expression in granulosa cells from small bovine follicles. Endocr 36, 339–345 (2009). https://doi.org/10.1007/s12020-009-9227-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-009-9227-6