Abstract
Klotho is a senescence suppressor protein that, when overexpressed, extends the lifespan of mice. Klotho-disrupted mice exhibit atherosclerosis and endothelial dysfunction, which led us to investigate the effect of the Klotho protein on vascular inflammation, particularly adhesion molecule expression. In this study, human umbilical vein endothelial cells (HUVECs) were preincubated with Klotho protein and then exposed to tumor necrosis factor-α (TNF-α) or vehicle. Reverse transcription-PCR and Western blot analyses revealed that Klotho suppressed TNF-α-induced expression of intracellular adhesion molecule-1 (ICAM-1) and vascular cell adhesion molecule-1 (VCAM-1). NF-κB activation, IκB phosphorylation induced by TNF-α were also attenuated by Klotho protein administration. The inhibition of eNOS phosphorylation by TNF-α was reversed by Klotho. Furthermore, Klotho inhibited TNF-α-induced monocyte adhesion to HUVECs and suppressed adhesion molecule expression in an organ culture of the rat aorta. These results suggest that Klotho suppresses TNF-α-induced expression of adhesion molecules and NF-κB activation. Klotho may have a role in the modulation of endothelial inflammation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mice with homozygous disruption of the Klotho gene exhibit multiple age-related disorders that are observed in humans, including skin atrophy, ectopic calcification, osteoporosis, and atherosclerosis [1, 2]. On the other hand, overexpression of Klotho in mice extends the lifespan independent of food intake and growth [3]. The Klotho gene is expressed primarily in the distal tubules of the kidney, the choroid plexus in the brain, the parathyroid, the testis, and the ovary [1, 4–6].
The functions of Klotho have been investigated in several reports. Klotho inhibits insulin/IGF-1 signaling and increases resistance to oxidative stress [7, 8]. We have shown that Klotho reduces oxidative stress-induced apoptosis and cellular senescence in vascular cells [9]. Moreover, recent reports have revealed that Klotho functions as an essential cofactor in the activation of FGF signaling by FGF23 and regulates calcium and phosphate homeostasis [10, 11]. It was suggested that abnormal phosphate homeostasis in Klotho-disrupted mice may be the causative factor for the shortened lifespan of these mice.
Atherosclerosis and emphysema are observed in Klotho-disrupted mice [1]. Inflammation is an essential component of atherosclerosis in the vascular cells and of emphysema in the pulmonary cells [12, 13]. However, the association between Klotho and inflammation has not been investigated. Klotho-disrupted mice exhibit endothelial dysfunction, which can be rescued by the administration of Klotho protein [14, 15]. Endothelial function is subject to nitric oxide-mediated regulation and is impaired by inflammatory processes [12, 16]. Thus, Klotho may prevent endothelial cell inflammation and suppress the development of atherosclerosis in the vasculature.
In the present study, we investigated the effects of Klotho on the expression of TNF-α-induced cell adhesion molecules and on NF-κB activation, which are essential components of endothelial inflammation.
Results
Klotho protein inhibits TNF-α-induced expression of adhesion molecules on HUVECs
We investigated the effects of Klotho protein on the expression of adhesion molecules on HUVECs. Inflammation was induced by TNF-α administration. TNF-α strongly increased ICAM-1 and VCAM-1 expression (Figs. 1 and 2). When HUVECs were incubated with both TNF-α and Klotho, ICAM-1 and VCAM-1 expression was significantly suppressed compared with TNF-α treatment alone (Figs. 1 and 2). Klotho protein in the absence of TNF-α did not lead to any significant changes in the expression of these adhesion molecules (Figs. 1 and 2).
Klotho suppressed TNF-α-induced ICAM-1 expression in HUVECs. a Relative levels of ICAM-1 mRNA. Data are normalized to the average value of the control and expressed as mean ± SEM. *P < 0.05 vs. control. **P < 0.05 vs. treatment with TNF-α alone. b Western blot of ICAM-1 and α-tubulin expression. Three separate experiments were performed using different cell preparations. Representative images are shown
Klotho suppressed TNF-α-induced VCAM-1 expression in HUVECs. a Relative levels of VCAM-1 mRNA. Data are normalized to the average value of the control and expressed as mean ± SEM. *P < 0.05 vs. control. **P < 0.05 vs. treatment with TNF-α alone. b Western blot of VCAM-1 and α-tubulin expression. Three separate experiments were performed using different cell preparations. Representative images are shown
Klotho protein inhibits TNF-α-induced NF-κB activation in HUVECs
Both ICAM-1 and VCAM-1 expression is usually regulated by the transcription factor NF-κB. A luciferase assay was used to investigate whether Klotho protein affects NF-κB activity. TNF-α increased NF-κB activity in HUVECs. When cells were incubated with both TNF-α and Klotho protein, NF-κB activation was suppressed compared with TNF-α treatment alone (Fig. 3a). Klotho protein treatment alone did not change the NF-κB activity relative to control (Fig. 3a). These results indicate that Klotho protein suppresses ICAM-1 and VCAM-1 expression by inhibiting NF-κB activity.
Effect of Klotho on TNF-α-induced NF-κB activation and IκB phosphorylation in HUVECs. a NF-κB activation was evaluated by luciferase assay. Data are normalized to the average value of the control and expressed as mean ± SEM. *P < 0.05 vs. control. **P < 0.05 vs. treatment with TNF-α alone. b IκB phosphorylation was evaluated by phospho-IκB expression. Expression was determined by Western blotting. Representative images are shown. Three separate experiments were performed using different cell preparations
Klotho protein inhibits TNF-α-induced IκB phosphorylation in HUVECs
NF-κB activation is preceded by IκB phosphorylation. To determine whether Klotho protein inhibits IκB phosphorylation in HUVECs, IκB phosphorylation was examined by Western blot analysis. TNF-α increased IκB phosphorylation in HUVECs. When cells were incubated with both TNF-α and Klotho protein, IκB phosphorylation was inhibited compared with TNF-α treatment alone (Fig. 3b). Klotho protein in the absence of TNF-α treatment did not change IκB phosphorylation relative to the control (Fig. 3b). These results indicate that the Klotho protein inhibits TNF-α-induced IκB phosphorylation in HUVECs.
Klotho protein recovers the eNOS phosphorylation reduced by TNF-α in HUVECs
We investigated the effects of Klotho protein on the phosphorylation of eNOS in HUVECs. Inflammation was induced by TNF-α administration. Treatment with TNF-α significantly suppressed eNOS phosphorylation (Fig. 4). When HUVECs were incubated with both Klotho protein and TNF-α, eNOS phosphorylation was similar to that of the control (Fig. 4). Klotho protein treatment in the absence of TNF-α did not lead to any significant changes in the expression of eNOS phosphorylation (Fig. 4).
Klotho protein inhibits TNF-α-induced monocyte adhesion to HUVECs
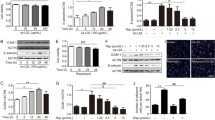
Next, the effects of Klotho protein on monocyte adhesion to HUVECs were investigated. Klotho protein treatment alone had no significant effect on the adhesion of THP-1 human monocytic cells to HUVECs (Fig. 5). TNF-α treatment enhanced by three-fold the adhesion of THP-1 cells to HUVECs (Fig. 5). When HUVECs were incubated with Klotho protein prior to TNF-α treatment, THP-1 cell adhesion was significantly suppressed compared with TNF-α treatment alone (Fig. 5). These results indicate that Klotho protein inhibits TNF-α-induced monocyte adhesion to HUVECs.
Klotho protein suppresses adhesion molecule expression in an organ culture of rat aorta
The effect of Klotho protein on the expression of adhesion molecules in vessels was investigated in an organ culture of rat aorta. Incubation with TNF-α induced the expression of ICAM-1 and VCAM-1 in the endothelium of rat aorta (Fig. 6). Consistent with observations in cultured cells, the TNF-α-induced expression of the adhesion molecules was suppressed by concurrent treatment with Klotho protein (Fig. 6).
Discussion
The present study revealed that the Klotho protein suppressed TNF-α-induced ICAM-1 and VCAM-1 expression in endothelial cells. Specifically, Klotho attenuated TNF-α-induced NF-κB activity and phosphorylated eNOS repression. These results suggest that Klotho might directly attenuate atherosclerosis, leading to a reduction in ischemic vascular disease. To determine the effect of Klotho on inflammation in endothelial cells, we focused on the adhesion molecules ICAM-1 and VCAM-1. When endothelial cells are exposed to pro-inflammatory molecules such as TNF-α, IL-1β, PDGF, and VEGF, adhesion molecules are prominently up-regulated on the cell surface [12, 17]. Furthermore, increased expression of ICAM-1 and VCAM-1 has been shown in animals with inflammation and in human atherosclerotic plaques.
The human aging process is associated with vascular endothelial dysfunction. Klotho-deleted mice exhibit endothelial dysfunction and reduced NO production [14]. Furthermore, parabiosis with wild-type mice or Klotho gene delivery reversed these changes [15]. Endothelial function is well known to be affected by vascular inflammation; in particular, the loss of NO is a key mechanism underlying endothelial dysfunction [12]. These facts are consistent with the anti-inflammatory effects of Klotho that were observed in the present study.
Klotho is expressed mainly in the kidney, brain, adipose tissue, and testis and is rarely expressed in endothelial cells. Reduced Klotho gene expression in the kidney has been shown in animal models of hypertension, renal failure, and hyperlipidemia [18]. In these diseases, reduced Klotho expression might lead to enhanced endothelial inflammation and atherosclerosis. Atherosclerosis observed in the Klotho-deleted mouse may be caused not only by the effects of calcium and phosphate metabolic abnormalities on the artery, but also by endothelial dysfunction arising from vascular inflammation.
Klotho, which is closely related to the FGF23 protein, regulates bone metabolism via calcium and phosphate handling. Actually, Klotho-deleted mice exhibit osteoporosis. It is well known that NF-κB activation leads to osteoclast differentiation and development, which results in osteoporosis [19]. Osteoporosis in Klotho-deleted mice may be caused partly by the suppression of Klotho anti-inflammatory function via NF-κB inhibition. Further study of the association between inflammation and Klotho in bone is warranted.
Jace et al. [20] reported that Klotho expression in human CD4+ lymphocytes of rheumatoid arthritis (RA) patients is significantly reduced. Furthermore, Klotho expression was correlated with CD28 expression, which is dependent on increased levels of TNF-α [20]. This study suggested that Klotho down-regulation may underlie both physiological and RA-related T-cell aging. In RA patients, enhanced NF-κB activation can be observed in the synovium and lymphocytes [21], and NF-κB inhibition is considered to be an attractive strategy for the treatment of chronic arthritis. Considering the inhibition of NF-κB expression by Klotho that was observed in the present study, reduced Klotho expression may have a role in the development of RA.
This study did not reveal the pathway by which Klotho inhibited adhesion molecules and NF-κB. However, it is consistent with the results to assume that Klotho inhibited ICAM-1 and VCAM-1 via NF-κB activity. The inhibition of NF-κB activity may be related to nitric oxide expression. Further studies are needed to elucidate the detailed pathway by which Klotho inhibits endothelial inflammation.
In conclusion, this study demonstrated that the Klotho protein attenuated the expression of adhesion molecules and NF-κB in endothelial cells in vitro and ex vivo. Klotho might be closely associated with the endothelial inflammatory process.
Materials and methods
Purification of soluble recombinant human Klotho
The plasmid pCAGGS-Klotho was constructed by inserting a complete mouse membrane form Klotho cDNA into the pCAGGS expression vector [9]. A 6xHis tag was inserted into the pCAGGS-Klotho plasmid (at a site at the 3′ end of the Klotho cDNA) for construction of the 6xHis-pCAGGS-Klotho plasmid. The plasmid was transfected into COS-1 cells (Sanko Junyaku, Tokyo, Japan) using Lipofectamine Plus 2000, and cells were grown for 48 h. The 6xHis-Klotho protein was purified from cell lysates by affinity chromatography on nickel-nitrilotriacetic acid agarose gel (QIAGEN). Immunoblotting of the anti-6xHis-tagged protein with an anti-Klotho antibody (KM2076, generous gift from Kyowa Hakko Kogyo Co. Ltd., Tokyo, Japan) [22] demonstrated that the recombinant purified protein was coincident with the Klotho protein.
Cell culture
We cultured sub-confluent HUVECs (Sanko Junyaku, Tokyo, Japan) for 4 h with Klotho protein (200 pM), followed by administration of TNF-α (10 pg/μl) for 4 h, and then used for mRNA quantification, Western blot analysis, NF-κB activity assay and adhesion assay. HUVECs were cultured in CC-3156 EBM-2 (Sanko Junyaku, Tokyo, Japan) supplemented with 2% FBS and antibiotics without corticosteroid.
Quantification of Klotho, ICAM-1 and VCAM-1 mRNA
Klotho, ICAM-1 and VCAM-1 mRNA were extracted from cells with the SV Total RNA Isolation kit (Promega, Madison, WI). To quantify the expression of Klotho, ICAM-1 and VCAM-1 mRNAs, the TaqMan-PCR (Applied Biosystems, Foster City, CA) method was used with a PRISM 7900 HT (Applied Biosystems), which can detect RNA amounts in real time with a fluorescent probe complementary to the RNA sequence. Expression levels of each gene were normalized to control gene expression (18SrRNA gene).
Western blot analysis
Cells were washed twice with PBS and harvested in a lysis buffer [1% SDS, 100 mM NaCl, 50 mM Tris–HCl (pH 8.0), and 20 mM EDTA]. The harvested cells were sonicated. After centrifugation, samples were boiled for 10 min, electrophoresed in a 12.5% SDS-PAGE gel, and electroblotted onto nitrocellulose filters. Blots were blocked in 5% nonfat milk in PBS for 1 h; incubated with rat monoclonal anti-Klotho (KM2076), anti-ICAM-1 (Cell Signaling), anti-VCAM-1 (R&D systems), anti-phospho eNOS (Cell signaling), or anti-phospho IκB (Cell Signaling) antibodies for over night; and incubated with peroxidase-conjugated secondary antibodies for 1 h. To monitor equal loading of proteins, membranes were incubated with anti-α-tubulin antibody (Calbiochem, La Jolla, CA). Immunoblots were developed with an ECL plus Western blotting detection system (GE Healthcare, Little Chalfont, Buckinghamshire, UK), as described previously [23, 24].
NF-κB activity assay
NF-κB activity was assessed with the Dual-Luciferase Reporter Assay System (Promega, Madison, WI). Briefly, HUVECs were seeded into 6-well plates and transfected with 1 μg NF-κB reporter plasmid and 100 ng control Renilla luciferase vector pRL-TK using Lipofectamine reagent (Invitrogen, Carlsbad, CA) according to the manufacturer’s instructions, and then incubated for 6 h in 2 ml culture medium. After removal of Lipofectamine in the medium, TNF-α was added, and cells were harvested 1 h later. The Luciferase activity was measured with the Dual-Luciferase Reporter Assay System (Promega) and a luminometer (Wallac 1420 ARVOMX/Light; Perkin–Elmer). The firefly luciferase activity of NF-κB was normalized to Renilla luciferase activity and expressed as the -fold induction compared with the control value.
Adhesion assay
The human monocytic THP-1 cell line was purchased from DSMZ (Deutsche Sammlung von Mikroorganismen und Zellkulturen, Germany) and cultivated in RPMI 1640 (10% FCS, 2 mmol/L L-glutamine, 100 U/ml penicillin, and 100 μg/ml streptomycin; MP Biomedicals).
The adhesion of THP-1 human monocytic cells (Deutsche Sammlung von Mikroorganismen und Zellkulturen, Germany) to HUVECs was determined as previously described [25]. FITC-labeled THP-1 cells were incubated with HUVECs in 6-well plates for 10 min at 37°C. The cells were washed three times with PBS to remove nonadherent monocytes. Adherent cells were lysed with 50 mmol/l Tris (pH 8.4)/0.1% SDS, and the fluorescence was measured. Statistical significance was determined by a paired t test.
Organ culture
Thoracic aortas were collected from rat and were cultured in EBM-2 (Sanko Junyaku, Tokyo, Japan) supplemented with 2% FBS in the presence or absence of Klotho protein for 4 h at 37°C, 5% CO2, followed by TNF-α incubation for 4 h. The aortas were then washed in PBS and snap-frozen in OTC compound (Sakura, Tokyo). Serial 10-μm-thick cryostat sections were collected on poly-d-lysine-coated slides and fixed in acetone. Sections were immunostained using anti-F8 antibody for endothelial cell marker (BD Pharmingen) [26], anti-ICAM-1 antibody (BD Pharmingen) and anti-VCAM-1 antibody (BD Pharmingen).
Statistical analysis
Comparisons of data from various time points were performed by one-way ANOVA followed by Duncan’s multiple range tests, using StatView software (Abacus Concepts Inc., Berkeley, CA). All data are expressed as mean ± SEM. P < 0.05 was considered statistically significant.
References
M. Kuro-o, Y. Matsumura, H. Aizawa, H. Kawaguchi, T. Suga, T. Utsugi, Y. Ohyama, M. Kurabayashi, T. Kaname, E. Kume, H. Iwasaki, A. Iida, T. Shiraki-Iida, S. Nishikawa, R. Nagai, Y.I. Nabeshima, Mutation of the mouse klotho gene leads to a syndrome resembling ageing. Nature 390, 45–51 (1997)
Y. Nabeshima, Klotho: a fundamental regulator of aging. Ageing Res. Rev. 1, 627–638 (2002)
H. Kurosu, M. Yamamoto, J.D. Clark, J.V. Pastor, A. Nandi, P. Gurnani, O.P. McGuinness, H. Chikuda, M. Yamaguchi, H. Kawaguchi, I. Shimomura, Y. Takayama, J. Herz, C.R. Kahn, K.P. Rosenblatt, M. Kuro-o, Suppression of aging in mice by the hormone Klotho. Science 309, 1829–1833 (2005)
N. Koh, T. Fujimori, S. Nishiguchi, A. Tamori, S. Shiomi, T. Nakatani, K. Sugimura, T. Kishimoto, S. Kinoshita, T. Kuroki, Y. Nabeshima, Severely reduced production of klotho in human chronic renal failure kidney. Biochem. Biophys. Res. Commun. 280, 1015–1020 (2001)
A. Kamitani, H. Yamada, M. Kinuta, M. Watanabe, S.A. Li, T. Matsukawa, M. McNiven, H. Kumon, K. Takei, Distribution of dynamins in testis and their possible relation to spermatogenesis. Biochem. Biophys. Res. Commun. 294, 261–267 (2002)
K. Miyamoto, M. Ito, H. Segawa, M. Kuwahata, Molecular targets of hyperphosphataemia in chronic renal failure. Nephrol Dial Transplant 18(Suppl 3), iii79–iii80 (2003)
M. Yamamoto, J.D. Clark, J.V. Pastor, P. Gurnani, A. Nandi, H. Kurosu, M. Miyoshi, Y. Ogawa, D.H. Castrillon, K.P. Rosenblatt, M. Kuro-o, Regulation of oxidative stress by the anti-aging hormone klotho. J. Biol. Chem. 280, 38029–38034 (2005)
H. Rakugi, N. Matsukawa, K. Ishikawa, J. Yang, M. Imai, M. Ikushima, Y. Maekawa, I. Kida, J. Miyazaki, T. Ogihara, Anti-oxidative effect of Klotho on endothelial cells through cAMP activation. Endocrine 31, 82–87 (2007)
M. Ikushima, H. Rakugi, K. Ishikawa, Y. Maekawa, K. Yamamoto, J. Ohta, Y. Chihara, I. Kida, T. Ogihara, Anti-apoptotic and anti-senescence effects of Klotho on vascular endothelial cells. Biochem. Biophys. Res. Commun. 339, 827–832 (2006)
H. Kurosu, Y. Ogawa, M. Miyoshi, M. Yamamoto, A. Nandi, K.P. Rosenblatt, M.G. Baum, S. Schiavi, M.C. Hu, O.W. Moe, M. Kuro-o, Regulation of fibroblast growth factor-23 signaling by klotho. J. Biol. Chem. 281, 6120–6123 (2006)
I. Urakawa, Y. Yamazaki, T. Shimada, K. Iijima, H. Hasegawa, K. Okawa, T. Fujita, S. Fukumoto, T. Yamashita, Klotho converts canonical FGF receptor into a specific receptor for FGF23. Nature 444, 770–774 (2006)
T. Trepels, A.M. Zeiher, S. Fichtlscherer, The endothelium and inflammation. Endothelium 13, 423–429 (2006)
K. Larsson, Aspects on pathophysiological mechanisms in COPD. J. Intern. Med. 262, 311–340 (2007)
Y. Saito, T. Yamagishi, T. Nakamura, Y. Ohyama, H. Aizawa, T. Suga, Y. Matsumura, H. Masuda, M. Kurabayashi, M. Kuro-o, Y. Nabeshima, R. Nagai, Klotho protein protects against endothelial dysfunction. Biochem. Biophys. Res. Commun. 248, 324–329 (1998)
Y. Saito, T. Nakamura, Y. Ohyama, T. Suzuki, A. Iida, T. Shiraki-Iida, M. Kuro-o, Y. Nabeshima, M. Kurabayashi, R. Nagai, In vivo klotho gene delivery protects against endothelial dysfunction in multiple risk factor syndrome. Biochem. Biophys. Res. Commun. 276, 767–772 (2000)
D.G. Harrison, Cellular and molecular mechanisms of endothelial cell dysfunction. J. Clin. Invest. 100, 2153–2157 (1997)
E. Galkina, K. Ley, Vascular adhesion molecules in atherosclerosis. Arterioscler. Thromb. Vasc. Biol. 27, 2292–2301 (2007)
R. Nagai, Y. Saito, Y. Ohyama, H. Aizawa, T. Suga, T. Nakamura, M. Kurabayashi, M. Kuroo, Endothelial dysfunction in the klotho mouse and downregulation of klotho gene expression in various animal models of vascular and metabolic diseases. Cell. Mol. Life Sci. 57, 738–746 (2000)
E. Jimi, S. Ghosh, Role of nuclear factor-kappaB in the immune system and bone. Immunol. Rev. 208, 80–87 (2005)
J.M. Witkowski, M. Soroczynska-Cybula, E. Bryl, Z. Smolenska, A. Jozwik, Klotho—a common link in physiological and rheumatoid arthritis-related aging of human CD4+ lymphocytes. J. Immunol. 178, 771–777 (2007)
M.L. Handel, L.B. McMorrow, E.M. Gravallese, Nuclear factor-kappa B in rheumatoid synovium. Localization of p50 and p65. Arthritis Rheum. 38, 1762–1770 (1995)
Y. Kato, E. Arakawa, S. Kinoshita, A. Shirai, A. Furuya, K. Yamano, K. Nakamura, A. Iida, H. Anazawa, N. Koh, A. Iwano, A. Imura, T. Fujimori, M. Kuro-o, N. Hanai, K. Takeshige, Y. Nabeshima, Establishment of the anti-Klotho monoclonal antibodies and detection of Klotho protein in kidneys. Biochem. Biophys. Res. Commun. 267, 597–602 (2000)
J. Yang, N. Matsukawa, H. Rakugi, M. Imai, I. Kida, M. Nagai, J. Ohta, K. Fukuo, Y. Nabeshima, T. Ogihara, Upregulation of cAMP is a new functional signal pathway of Klotho in endothelial cells. Biochem. Biophys. Res. Commun. 301, 424–429 (2003)
M. Imai, K. Ishikawa, N. Matsukawa, I. Kida, J. Ohta, M. Ikushima, Y. Chihara, X. Rui, H. Rakugi, T. Ogihara, Klotho protein activates the PKC pathway in the kidney and testis and suppresses 25-hydroxyvitamin D3 1alpha-hydroxylase gene expression. Endocrine 25, 229–234 (2004)
M.I. Cybulsky, M.A. Gimbrone Jr., Endothelial expression of a mononuclear leukocyte adhesion molecule during atherogenesis. Science 251, 788–791 (1991)
A. Giatromanolaki, M.I. Koukourakis, D. Theodossiou, K. Barbatis, K. O’Byrne, A.L. Harris, K.C. Gatter, Comparative evaluation of angiogenesis assessment with anti-factor-VIII and anti-CD31 immunostaining in non-small cell lung cancer. Clin. Cancer Res. 3, 2485–2492 (1997)
Acknowledgements
We would like to express gratitude Ms. Kazuko Iwasa and Ms. Eriko Nagata for their continuous support of our investigations. This work was supported by the Osaka-Medical Research Foundation for Incurable Diseases, research grants from Takeda Science Foundation, the Japan Research Foundation for Clinical Pharmacology, and Grants-in-Aid for scientific research from the Ministry of Education, Science, Sports, Culture, and Technology of Japan (18590265, 18590811, 19650188).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Maekawa, Y., Ishikawa, K., Yasuda, O. et al. Klotho suppresses TNF-α-induced expression of adhesion molecules in the endothelium and attenuates NF-κB activation. Endocr 35, 341–346 (2009). https://doi.org/10.1007/s12020-009-9181-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12020-009-9181-3