Abstract
Autoimmune diseases (ADs) are a spectrum of diseases originating from loss of immunologic self-tolerance and T cell abnormal autoreactivity, causing organ damage and death. However, the pathogenic mechanism of ADs remains unclear. The current treatments of ADs include nonsteroidal anti-inflammatory drugs (NSAIDS), antimalarials, corticosteroids, immunosuppressive drugs, and biological therapies. With the need to prevent side effects resulting from current treatments and acquire better clinical remission, developing a novel pharmaceutical treatment is extremely urgent. The concept of T cell vaccination (TCV) has been raised as the finding that immunization with attenuated autoreactive T cells is capable of inducing T cell-dependent inhibition of autoimmune responses. TCV may act as an approach to control unwanted adaptive immune response through eliminating the autoreactive T cells. Over the past decades, the effect of TCV has been justified in several animal models of autoimmune diseases including experimental autoimmune encephalomyelitis (EAE), murine autoimmune diabetes in nonobese diabetic (NOD) mice, collagen-induced arthritis (CIA), and so on. Meanwhile, clinical trials of TCV have confirmed the safety and efficacy in corresponding autoimmune diseases ranging from multiple sclerosis (MS) to systemic lupus erythematosus (SLE). This review aims to summarize the ongoing experimental and clinical trials and elucidate possible molecule mechanisms of TCV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Autoimmune diseases (ADs) are a spectrum of diseases characterized by self-immune regulation disorders and accumulation of autoantibodies after environmental triggering of genetically susceptible individuals. ADs can be generally divided into two categories: systemic autoimmune diseases such as systemic lupus erythematosus (SLE) and organ- or tissue-specific autoimmune diseases, both of which involve chronic inflammation, causing multiple major organ damage and organ failure [1]. The overall objective of disease management in autoimmune diseases is to suppress chronic inflammation and prevent organ damage. Therapies revolve around five drug classes: nonsteroidal anti-inflammatory drugs (NSAIDS), antimalarials, steroids, immunosuppressive drugs, and biological therapies [2]. The first four kinds of drug strategies are most widely used worldwide. However, the general immunosuppression and steroid-related side effects, such as osteoporosis, diabetes mellitus, and cataract, undermine the long-term administration and limit the use on patients with multiple organ complications. In some autoimmune diseases such as rheumatoid arthritis (RA), relatively well-established protein-based treatments (biological drugs or biologics) have been developed. One of the most effective biologics is monoclone antibody targeting tumor necrosis factor (TNF), and the subsequent biologics researches continue to focus on some surface molecules of immune cells like CD20, CD3, CD22, CD52, complements, and additional members of the TNF superfamily [3, 4]. However, the biologics require high production cost and commonly large dose, thus partially limiting patient accessibility and clinical applications [5]. For example, belimumab, the first and only disease-modifying biologics for SLE, was approved in 2011. It costs approximately $45,000 annually in the USA [2, 6]. Worse still, a large number of ADs still lack effective and successful specific therapy. Significant need in novel therapeutic strategy of ADs remains unmet.
Though the precise cellular and molecular mechanisms leading to AD have remained clouded in uncertainty, there is growing evidence that the compromise of tolerance and onset of ADs are closely related to the activated autoreactive T cells [1]. Autoimmunity is clearly based on the interaction of genetics and environment, and while there is little that can be done to alter genetic predisposition [7–11], there is considerable effort on dissecting T cell subpopulations and developing unique vaccination protocols to circumvent effector pathways [12–19]. The degeneration or inactivation of activated autoreactive T cells may provide an approach toward controlling autoimmune response and regulating pathogenic trigger of autoimmune reaction. In this review, we summarized the ongoing experimental and clinical trials and illustrated possible molecule mechanisms of a novel therapy that targets autoreactive T cells in ADs, termed “T cell vaccination” (TCV), therefore hoping to provide new insight into the understanding of autoimmunity and develop more effective T cell vaccine.
The Concept of T Cell Vaccination
The concept of TCV was first raised by Ben-Nun et al. in 1981, based on the finding that attenuated T lymphocyte cells reactive against myelin basic protein (MBP) can induce vaccination against autoimmune encephalomyelitis in rats models [20]. To some extent, the effect of TCV is similar to conventional vaccination against etiological agents from infectious diseases. During the conventional process, individuals are purposely exposed to attenuate microbial pathogens, which then instruct the immune system to recognize and neutralize them in their virulent form. However, instead of using foreign microbial agents, TCV uses neutralized pathogenic autoreactivce T cells or their T cell receptor (TCR) peptides.
The pathogenicity of autoreactive T cells has been investigated in various animal models and clinical trials of autoimmune diseases like SLE, RA, type 1 diabetes (T1D), multiple sclerosis (MS), myasthenia gravis, inflammatory bowel disease [21–23], and so on. Experimental autoimmune encephalomyelitis (EAE), the animal model of MS, is caused by immune response to self-antigens, mainly the MBP of the central nervous system, and can be induced by adaptive transfer of MBP-reactive T cells [20, 24]. In addition, previous research has observed that autoreactive T lymphocytes selected and isolated from rats administered an arthritogenic dose of Mycobacterium tuberculosis can reduce autoimmune arthritis [25]. Furthermore, adoptive transfer of autoreactive CD4+ T cells specific to 70 k (subunit of the U1 small nuclear ribonucleoprotein (snRNP), which is one of the pathogenic self-antigens of SLE) could develop a diffuse proliferative glomerulonephritis in C57BL/6 (B6) mice expressing HLA-DR4 [26]. Such evidence indicates that accidentally stimulated autoreactive T cells are sufficient to induce the imbalance of regulatory network and, therefore, lead to autoimmunity. Novel treatments that specifically target at self-reactive pathogenic T cells could therefore regulate the autoimmune system and result in improvement in both clinical manifestation and laboratory parameters of ADs.
The immune regulation effects of TCV have been supported by a number of animal models of ADs, using TCR peptide protocol or whole attenuated pathogenic T cells as vaccine. These models have achieved a positive outcome in reducing circling autoreactive T cells after vaccination and ameliorating disease activity [25, 27–30]. Subsequent research on the mechanism of TCV has elucidated a complicated anti-idiotypic and anti-ergotypic network to be responsible for the pathogenic procedure [24, 31–35]. Clinical trials of TCV in ADs have emerged after the optimistic result from animal models. In these experimental and clinical trials, selected autologous T cell lines that recognize candidate self-antigens or artificial TCR peptide of autoimmune T cells induce regulatory immune response for clinical benefit. Using TCV to deplete autoreactive T cells in human autoimmune circumstance has started to reveal the pathologic relevance of various autoimmune T cell populations in the disease processes and provide a unique opportunity to test the autoimmune theories in a clinical setting [22, 36–38].
T Cell Vaccination for Multiple Sclerosis
Myelin-Reactive T Cells in MS
MS is a chronic, debilitating neurologic autoimmune disease characterized by central nervous system (CNS) white matter inflammation, demyelination and, in cases of chronic disease, astroglial scarring. The formation of demyelinated lesions leads to axonal injury and neurological deficit [39]. While the precise mode of disease etiology remains elusive, it is widely believed that the CNS-specific myelin protein plays a vital role in stabilizing the myelin sheath in the CNS and has been implicated in the pathogenesis of MS. It has been demonstrated that the destructive autoimmune mechanisms in MS are presumably initiated by abnormal activation of potentially pathogenic autoimmune T cells, which recognize CNS components (CNS-specific myelin protein) [40]. The EAE, an umbrella term referring to multiple different models of CNS autoimmunity in vertebrate animals, has been widely used in the study of CNS autoimmunity, especially in MS animal models [40]. As the first and most widely studied model, the great progress made in the application of TCV in EAE is attributed to the well-established understanding of autoantigens and corresponding immune abnormalities in MS. The target antigens, which have been found to cause clinical EAE in animal models, include MBP [38, 41–43], proteolipid protein (PLP) [44, 45], and myelin oligodendrocyte glycoprotein (MOG) [46], which are widely studied. Some latest proven candidate target antigens such as myelin-associated oligodendrocytic basic protein (MOBP) [47] and associated oligodendrocyte-specific protein (OSP) [48] are also believed to be responsible for the pathogenesis of MS. Other myelin proteins, such as myelin-associated glycoprotein (MAG) and Nogo-A, have been demonstrated with encephalitogenic potential [49–51].
Encephalitogenic Potential of T Cells and Application of TCV in Animal Models of MS
Studies performed to characterize myelin-reactive T cells in cerebrospinal fluid (CSF) and peripheral blood in murine models suggested that MBP is the most relevant and core source of encephalitogenic immune response in the CNS, according to previous studies of EAE. Using both MBP-derived peptides and MBP-reactive T cell clones could lead to the onset of EAE in murine models. Zamvil et al. were able to induce EAE in SJL/J mice with the C-terminal peptide (89–169) and in PL/J mice with MBP (1–37). Later, they demonstrated that an acetylated N-terminal-derived peptide from MBP was also sufficient to induce EAE in PL/J mice [42, 43]. Moreover, immunization of SJL/J mice with the immune-dominant epitope of PLP (139–151) or passive transfer of PLP (139–151)-reactive T cell lines and clones to naive hosts brought about a relapsing-remitting disease course of EAE [45], suggesting that PLP was the immune-dominant epitope for the induction of EAE in the SJL strain. Sun and his colleagues reported in their study that pMOG (35–55) consistently activated a high proportion of CD8+ TCRαβ + T cells that were encephalitogenic in C57BL/6 (B6) mice [52]. But MOG was leading a less virulent response in EAE as disease induced by the immune-dominant MOG (35–55) peptide in C57BL6/J (B6) mice tended to be chronic in nature [44, 52]. Similar research has been carried out on RAG-1−/−mice [52].
Other studies have found evidence of epitope spreading in the relapsing EAE (R-EAE) model. Mice immunized with PLP (139–151) developed splenic lymphocyte responses to PLP (178–191), and these PLP (178–191)-reactive T cells could induce EAE upon adoptive transfer. It means that myelin-reactive T cells with encephalitogenic epitopes themselves maybe, to some extent, independent of producing MS-like inflammation and demyelination [53].
Unlike MBP, PLP, and MOG, the role of MOBP in MS immunization remains unclear. In order to characterize the T cell autoimmunity against MOBP, Nathali Kaushansky delineated the major encephalitogenic epitope of MOBP and dissected the epitope at the residue level. Analysis of the T cell response to MOBP in SJL/J mice showed that MOBP-reactive T cells predominantly responded against one dominant and major encephalitogenic epitope, the MOBP (15–36) [47], whereas other studies indicated MOBP (37–60) to be the main encephalitogenic reaction producer [54]. Considering the clinical manifestation and histology appearance observed in MOBP (15–36), immunized models were much more severe than that of MOBP (37–60), and the discrepancy might result from the difference in immunization protocols or because MOBP (37–60) was carrying a minor or cryptic encephalitogenic epitope [47, 54]. Results from TCV with the tracking technique utilizing encephalitogenic T cells expressing GFP showed an evident decrease of encephalitogenic T cells in the CNS and lymphoid organs, a reduction in the Th1 cytokine producing cells in the CNS, and the appearance of T cells responsive to the anti-MBP effector T cells [55].
Administration of TCV in MS Patients
The successful application of TCV in animal models of MS encouraged subsequent research in clinical trials. Zhang et al. conducted a study with six MS patients with T cell clones against MBP peptides (1–37, 45–89, and 90–170). Administration of the vaccines induced an anti-idiotypic T cell response, specifically recognizing the vaccine clones, which was accompanied by a progressive depletion of circulating MBP-reactive T cells in all the patients [30] (Table 1). In another 16 patient pilot trial, five relapsing-remitting MS (RRMS) and three chronic-progressive MS (CPMS) patients were treated with three subcutaneous injections of two to four vaccine clones. Over half of the treated patients had decreases in relapse rates. Magnetic resonance imaging also showed mitigation of brain lesion compared with the controls [29]. With the support of TCV effectiveness in these pilot studies, a preliminary clinical trial involving a larger number of patients (RRMS (n = 28) or secondary progressive MS (SPMS) (n = 26)) was launched by Zhang and co-workers. Fifty-four patients were immunized with irradiated autologous MBP-reactive T cells (both whole MBP and MBP peptides 83–99 and 151–170 reactive T cell lines). A correlation between depletion of MBP-reactive T cells and a reduction by 40 % in the rate of relapses in RRMS patients were observed, compared with the pretreatment rate in the same cohort. However, the reduction in expanded disability scale score (EDSS) was minimal in RRMS patients, while the EDSS slightly increased in SPMS patients over a period of 2 years [56].
Besides, attempts with the bovine blood-derived myelin-reactive T cell line as vaccines were made in a few experiments. In a TCV pilot trial involving four SPMS patients, modest effectiveness was reflected by a progressive decline of circulating whole myelin-reactive T cells after vaccination, and cytotoxic T cells recognizing the inoculates were isolated from the peripheral blood of two MS patients [57]. But no further study with bovine myelin-reactive TCV protocol ensues in consideration of the potential problem of heterogenicity.
The ability of interleukin (IL)-2 to expand CD4+ T lymphocytes reactive to myelin from CSF as vaccine has been verified by earlier research [57]. Based on the presumption that CSF lymphocytes can better reflect the repertoire of inflammatory cells infiltrating the parenchyma and they may contain infiltrating pathogenic cells relevant to the disease process because of its proximity to the target organ in MS, two pieces of preliminary research with CSF-delivered vaccine were undertaken [58, 59] (Table 1). One of them was conducted by Van der Aa et al. [59], which vaccinated five MS patients (four RRMS, one CPMS) with activated CD4+ T cells derived from CSF. The vaccinations were well tolerated and no toxicity or adverse effects were reported. Proliferative responses and anti-ergotypic responses against the CSF vaccine were observed in three to five patients. After that, a double-blind placebo-controlled trial with MS patients (n = 60) was conducted to study the effects of TCV with CSF-derived vaccines in early RRMS patients (unpublished results, Table 1).
In general, it is widely accepted that multiple autoreactive T cell lines of myelin protein or peptides are responsible for the pathogenesis of MS. Therefore, incorporating T cell populations specific for these autoantigens in the vaccine may improve the effectiveness of previous TCV protocol [37, 60, 61]. To probe whether the multivalent TCV protocol could gain more effective clinical remission from MS patients, Achrion et al. undertook a divalent TCV trial in 20 RRMS patients with T cell lines (TCL) prepared using immune-dominant epitope sequences of MBP (83–99, 87–110, 151–170) and MOG (6–26, 34–56) at a dose of up to 1.5E7 cells per peptide of attenuated myelin-reactive T cells (MRTC). Deletion of MBP and MOG-reactive T cells was found to be correlated with a reduction by 55 % in the rate of relapses. Neurological disability stabilized when compared with the 2- and 1-year pretreatment progression rates. Significant reduction in the number and volume of active lesions was revealed by quantitative MRI analysis [62] (Table 1). Another major step toward the practical use of TCV in treating MS patients is the exploitation of “Tovaxin,” a trivalent formulation of attenuated myelin peptide-reactive T cells (sponsored by Opexa Pharmaceuticals Inc) [63]. To assess the safety and tolerability of Tovaxin therapy, an open-label dose escalation study of TCV in MS patients was conducted in 2009, using attenuated MRTC selected with six myelin peptides [61]. In this study, the mid-dose (30–45E6 dose) proved to be the most effective with reductions in MRTC ranging from 92.4 % at week 5 to 64.8 % at week 52. A rapid depletion of circulating MRTC and improvement trends in clinical outcomes were reported. However, a slight rebound in MRTC was observed by week 52 for all doses, which was speculated to be a patient-specific response linked with a post-vaccination episode of clinical relapse and/or worsening disease. Several reasons may account for the rebound in MRTC, such as continued exposure to the myelin antigens, a shifting profile due to the polyspecificity of the TCR of MRTCs, lack of the induction of a sustained immune response, or an inadequate vaccination schedule. Overall, the study demonstrated favorable effects of Tovaxin on clinical and immunological parameters according to a press release, and Tovaxin (licensed by Merck Serono) has been granted Fast Track designation by the US Food and Drug Administration (FDA) for SPMS [61] (Table 1). Further phase IIb placebo-controlled study with Tovaxin was conducted in 150 subjects. The results showed that subjects with higher disease activity favored Tovaxin in terms of annualized relapse rate (ARR) and disability progression. Prior disease-modifying treatment (DMT) exposure might undermine effect size and the validity of the study. As a result, limiting subject selection to DMT treatment-naive individuals might be a reasonable approach to phase 2 or proof-of-concept studies of limited duration [36].
More recently, the first double-blind, controlled clinical trial of 30 patients with RPMS was organized by Dimitrios Karussis. During the trial, 30 patients were prescreened and tested for their peripheral blood lymphocyte reactivities against multiple autologous T cell vaccinations with a mixture of attenuated T cell lines reactive to three or more, among nine different peptides from the sequences of the three major myelin proteins implicated as autoantigens in MS: MBP, PLP, and MOG. The MBP peptides include M1 (84–102) and M2 (143–168); the MOG peptides: MO1 (1–22), MO2 (34–56), MO3 (64–86), and MO4 (74–96); and the PLP peptides: P1 (41–58), P2 (184–199), and P3 (190–209). It found a remarkable clinical effect on relapses and a beneficial effect on disability, buttressed by the follow-up EDSS scores and the performance in the timed 10-m walking test, while the MRI result remained the same [60] (Table 1). The failure to detect a positive effect on MRI parameters may be explained by the small size and short clinical course of the study. Interestingly, additional TCV studies failed to show significant MRI effects as well [27, 56, 62]. Whether the transmission method of TCV affects MRI parameters necessitates further investigation, because intravenous injection appears to have a better clinical remission and associated serologic improvement in patients with CPMS, when being compared with subcutaneous immunization [64].
To sum up, promising results from different clinical trials at various stages of MS provide justification for TCV as an alternative in MS treatment. Despite their limitations in some trials due to the relatively small number of participants and the lack of significant MRI data, both the vaccination with T cell clones and multiple anti-myelin cell lines (polyclonal vaccine) show feasibility and safety of the procedure and indicate clinical efficacy of TCV in MS. But further studies with a larger group of patients and longer follow-up periods are needed.
T Cell Vaccination for Rheumatoid Arthritis
Autoreactive T Cells with Common TCR V Gene Sequence in RA
RA is an autoimmune disease with unknown etiology, characterized by persistent synovitis, destruction of joint cartilage, systemic inflammation, and autoantibodies (particularly to rheumatoid factor and citrullinated peptide) presence [65]. In contrast to comparatively well-defined autoantigens in MS, autoantigens of RA are much more complicated, though there is a consensus of the role of some autoantibodies and inflammatory cytokines involved in the hierarchy of the RA processes [66]. Collagen-induced arthritis (CIA) represents an animal model of autoimmune poly-arthritis with significant similarities to human rheumatoid arthritis that can be induced upon immunization with native type II collagen (CII) [67].
The specific recognition of peptide derived from TCRs of autoreactive T cells is the trigger of protective regulation induced by TCV. Various attempts have been made to analyze TCR variable region (TCR V) gene usage and third complementarity-determining region (CDR3) sequence motifs. These studies have revealed some interesting findings suggestive of a restricted TCR V gene usage and limited clonality among lesion-derived T cells in RA [68–70]. Although the peripheral blood TCR beta chain variable region (Vβ) expression was heterogeneous [69], the T lymphocytes with common TCR Vβ clonotypes, infiltrating in the articulars of RA patients, appeared to cause arthritogenic effects in substantial researches [71–74].
The restricted TCR Vβ clonotypes vary among animal models and human individuals and fluctuate between different organs and tissue, making a consensus of TCR Vβ restriction less likely to be achieved [69, 70, 74–77]. Decades ago, increased expression of TCR V beta gene 14 (Vβ 14) was discovered in juvenile RA patients [68]. Later, TCR V beta 3 (Vβ 3) and V beta 17 (Vβ 17) have also been found to be overrepresented among IL-2 receptor (IL-2R)-positive T cells in RA patients [75]. However, in the course of CIA progression in Lewis rats, T cells with high expression of TCR V beta 5.2 (Vβ 5.2) and TCR V beta 8.2 (Vβ 8.2) are the main pathogenic T cell clonotypes, which is similar to TCR Vβ gene expression pattern in lupus-prone mice and EAE murine model [78, 79]. Besides, increased expression of TCR V beta 15 (Vβ 15) and TCR V beta 19 (Vβ 19) in CIA rats was confirmed in a recent study, which investigated the effect of immunomodulator triptolide on TCR Vβ gene expression [73]. In spite of the discrepancy in restricted TCR Vβ gene distribution, the broad scope of regulations triggered by V gene determinants has been widely acknowledged, and some immune suppressors like cyclosporin A and triptolide can reverse such kind of overexpression in patients with early RA [73, 77].
TCR Peptide Vaccination in RA
The certain families of V genes have been implicated to utilize more often than others in T cell responses. Conceptually, this characteristic could allow targeting of a limited set of V genes that would be represented in the autoreactive T cell pool in most patients. Although these widely shared sets of V genes have not yet been fully defined for the key autoimmune diseases, vaccinations with peptides derived from restricted overrepresented TCRs are proven to be, to some extent, effective for autoimmune disorders in RA [68–70, 76]. Ge et al. constructed recombinant DNA vaccines encoding TCR Vβ 5.2 and TCR Vβ 8.2, which are main pathogenic T cell clonotypes in CIA. Both vaccines inhibited CIA by alleviating the arthritis index score and histological change and lowering the level of IFN-gamma (IFN-γ), the ratio of CD4+/CD8+ lymphocytes, and the anti-CII antibody in serum [79].
Subsequent clinical trials were conducted with a single or multivalent peptide vaccination of TCR Vβ 3, Vβ 14, and Vβ 17, which is correlated with the restricted TCR Vβ gene distribution. An initial study measured the safety and immunogenicity of different doses of Vβ 17 (97) CDR2 peptide vaccine (Table 2). It demonstrated that about 35 % of immunized patients had measurable T cell proliferation responses to injected peptides after immunization, together with decreased (20 %) circulating levels of activated Vβ 17 T cells. Clinically, the TCR treatment resulted in falling pain and swollen joint scores and an improvement of total joint scores at all follow-up visits [80]. In a murine model, the group injected with a combination of the two vaccines (pTCR Vβ 5.2 and pTCR Vβ 8.2) showed stronger inhibitive effects on CIA than either individual vaccine [79]. Therefore, in order to decide whether a cocktail of TCR V region peptides will obtain a wider base of immunization in regulating pathogenic T cell clones than a single TCR Vβ 17 CDR2 peptide vaccination in larger number of RA patients, a phase II clinical trial was developed, using a combination of three peptides derived from Vβ 3, Vβ 14, and Vβ 17, respectively [75, 81] (Table 2). It yielded promising improvement in joint manifestation, while the laboratory parameters like ESR and CRP remained unchanged [76]. One possible explanation of the incomplete remission of laboratory parameters in this study and other clinical trials in RA may relate to the biased Vβ gene utilization of peripheral blood and synovial fluid among different patients, observed in unselected T cell populations and the CD4+ T cells in RA patients [76].
Whole Autoreactive T Cell Vaccination in RA
With the successful application of TCR peptide vaccination in RA and the understanding of pathogenic T cells in RA etiology, an alternative approach to identify pathogenic T cells as TCV without knowing the pathogenic autoantigens has been considered: to directly isolate infiltrating T cells from synovial lesions with characterized pathologic relevance. Parallel efforts have already been made with efficacy in MS and other ADs [60].
In fact, in 1993, there was a phase I study of TCV conducted with 13 RA patients (Table 2). All patients received a subcutaneous injection of attenuated autologous T lymphocytes from a CD4+ clone (n = 4) or line (n = 9) isolated from synovial tissue (n = 3) or synovial fluid (n = 10). Treated patients showed a slight decrease in disease activity, which was most noticeable at 8 weeks after the injection [82]. Chen and colleagues described an approach for T cell vaccination quite similar to the aforementioned one to bypass the need for defined TCR peptides from autoimmune T cell clones. In the pilot clinical study, they used autologous irradiated synovial T cells selected for pathologic relevance for vaccination in human. Fifteen patients received this TCV via six subcutaneous inoculations over a period of 12 months. A substantial response, defined as meeting the American College of Rheumatology’s 50 % improvement criteria, was witnessed in 10 of the 15 patients (66.7 %) and was accompanied by a marked improvement in RA-related laboratory parameters including standard hematologic, liver, and renal function tests and blood chemistry [71]. In mechanism, there was a reduction of CD4+ Tregs and CD8+ cytotoxic T cells specific for T cell vaccine accompanied with a characteristic shift in the Vβ gene distribution pattern of peripheral T cells. However, the overall outcome from TCV in RA is not as optimistic as that in MS. Opexa previously investigated “Tovaxin” for the potential treatment of RA. But no further development has been reported since December 2002 [63].
T Cell Vaccination for SLE
Anti-RNP Immunity and TCV
SLE is a kind of autoimmunity disease which is caused by accumulation of autoimmune antibody against constituents of the nucleus, in particular chromatin and RNA-binding proteins [83]. The major targets of anti-nuclear antibodies (ANAs) in SLE include the nucleosome (the fundamental unit of chromatin) and its individual components (double-stranded DNA (dsDNA) and histones). They also include snRNPs, in particular Sm and U1A-RNP [84–86]. In the 1980s, the antibodies to snRNPs were regarded as more closely related to mixed connective tissue disease (MCTD) because the titer of which in sera was much higher than the titer in SLE patients. But data from lupus-prone mice and human clinical trials in recent years has seen snRNP antibodies being detected at the early stage of disease preceding the appearance of anti-dsDNA and anti-histone antibodies [84, 86]. These findings suggest that the appearance of these antibodies can serve as a trigger for autoimmune response, giving anti-RNP antibodies a new identity in SLE diagnosis. Clinically, anti-dsDNA and chromatin Abs are serological hallmarks of SLE and their presence is used to define some particular clinical manifestations of SLE such as lupus nephritis (LN) [87, 88]. Nonetheless, a recent single center cohort study of male pediatric SLE in Texas Children’s Hospital showed that a significantly higher proportion of boys with LN had anti-RNP antibodies. It means that the strength of the correlation between renal disease and anti-RNP antibodies may be higher than previously expected [89].
The critical role of T cells in anti-RNP lupus has been sustained by the strong pathogenic potential of anti-RNP pathogenic T cell in inducing anti-RNP-associated nephritis. Such autoreactive CD4+ T cells can help B cell produce anti-dsDNA antibodies and limit the number of T cell epitopes defined on the autoantigens. The proliferation of autoreactive T cells in vivo is attributed to complicated mechanisms including defects in activation-induced cell death, uncontrolled elimination of regulatory T cells, and abnormal activation of antigen presenting cells (APCs) such as dendritic cells [90]. TCV, targeting at those pathogenic T cells (mostly CD4+ effector T cells), can stimulate Foxp3+ CD4+ Tregs and CD8+ Tregs to block anti-RNP response and protect against autoimmune kidney disease [91]. Such kind of CD8+ Tregs, identified by a number of markers including CD44, inducible T cell costimulator ligand, CXCR5, very late antigen-4, and CD122 may mediate the immune response by targeting T follicular helper (Tfh) cells in a Qa-1-restricted manner [92–94].
Animal Experiments and Clinical Trials of TCV in SLE
The analogous TCV protocol was first adopted in 1992 with MRL-MP/lpr-lpr mice (MRL/lpr mice), which can develop SLE spontaneously (Table 3). After the vaccination, a selective depletion of autoreactive T cells expressing products of the Vβ 8.2 subfamily was observed, which is homologous with the anti-MBP T cells in EAE [78]. To further identify suitable T cell clones for TCV, Takao Fujii firstly used different anti-dsDNA Ab-stimulating clones of irradiated CD4+ Vβ 8.3 Th1 as vaccine to test the effect of TCV in MRL/lpr mice (Table 3) [95]Table 3. Compared with the results in PBS-treated MRL/lpr mice, both anti-dsDNA antibody titers and the activity index for LN decreased in MRL/lpr mice vaccinated with irradiated (i-) dna51 cells, whereas MRL/lpr mice vaccinated with i-rnp2, i-dna5, and stimulated (s-) dna51-specific autoreactive T cell clones failed to show any clinical improvement and antibody reduction. Therefore, un-irradiated clone dna51, or clone rnp2 with or without irradiation, was generally ineffective for TCV in MRL/lpr mice. In addition, the survival rate was not improved in any group, indicating that the influence of a single clone vaccine to the immune system was inadequate to maintain a consistent clinical remission. Taken together the reports from preliminary studies of TCV in MRL/lpr mice, which have confirmed the efficiency of TCV using whole pathogenic cells (either autoreactive T cells or unselected lymphocytes) [78, 96], it is reasonable to regard polyclone autoreactive T cells or multivalue TCR peptide as being a more effective TCV protocol. Recently, the first exploration of whole autologous T cell protocol in a clinic has been tested in Chinese patients with SLE (Table 3). Purified CD4+ T cells from PBMC were injected after 25 Gy irradiation. The results have seen clinical improvements together with decreased titers of antinuclear Abs in most patients. Efficacy in that study was shown only for mild lupus manifestations, which can be easily treated with low-dose corticosteroid and/or conventional immunosuppressants. TCV with unselected T cells offers, therefore, a questionable therapeutic approach in intractable lupus manifestations, such as LN [97].
Based on the findings that B6 mice could develop a diffuse proliferative glomerulonephritis after immunization with 70 kD subunit of the U1 snRNP (70 k) or 70 k-specific CD + T cells [26], and the acknowledged close relationship between HLA-DR4 and anti-Sm or anti-RNP Abs in SLE patients [98], Trivedi et al. optimized the TCV therapy using irradiated anti-70 k T cells in HLA-DR4tg mice with anti-RNP-associated glomerulonephritis. It found an antigen-specific reduction in T cell proliferation and was associated with a high rate of clinical improvement in established nephritis in this model [99]. The analysis of pathogenic T cell clones showed that the anti-RNP mice with interstitial pneumonitis also had T cell infiltrated with the same oligoclonal T cell subset, suggesting that T cell vaccination could be effective for this spectrum of disease as well (Table 3). Further study showed efficacy, even in a donor/recipient MHC class II mismatch setting, with induced remission of anti-RNP-associated nephritis in over 80 % of treated mice, which have developed either induced or spontaneous autoimmunity (Trex1 deficiency model) [100]. Inhibited anti-70 k T cell proliferation and bound hybridomas expressing the conserved CDR3 motifs were observed in vaccine responder sera (Table 3). The 70 k-selected T cells from 70 k-immunized B6 and HLA-DR4 mice had a high prevalence of TCR Vβ CDR3 regions that were similar to anti-70 k T cells. The latter have been previously identified from the spleen, lymph nodes, and lesional tissues of HLA-DR4tg mice and from the circulation of human patients with anti-70 k autoimmunity (most notably in the presence of MS, RA, and T1D). The predilection for T cells expressing such TCRs in the peripheral circulation or tissue may be one factor for predisposition to autoimmune response. This may allow for further practical development of a standardized anti-RNP T cell vaccine preparation useful for multiple patients.
T Cell Vaccination for Type 1 Diabetes
β Cell Autoantigens and Autoreactive T Cells in T1D
T1D refers to a chronic autoimmune disease with a subclinical prodromal period featured by selective loss of insulin-producing β cells in the pancreatic islets and leukocyte invasion of the islets in genetically susceptible subjects [101]. A series of autoantigens targeting β cells have been identified in T1D, including insulin, glutamic acid decarboxylase (GAD), the protein tyrosine phosphatase-related islet antigen 2 (IA-2) and, most recently, the zinc transporter Slc30A8 residing in the insulin secretory granule of the β cell. The issue whether there is any primary autoantigen in T1D has remained controversial [102, 103]. Autoreactive T cells, both CD4+ and CD8+ cells, have been implicated as active players in β cell destruction. CD4+ T cells are attracted to islets by β cell antigens which include insulin, chromogranin A, and islet amyloid polypeptide. Adaptive transfer of pathogenic, polyclonal CD4+ T cells isolated from the spleen of nonobese diabetic (NOD) mice have been reported to accelerate the diabetogenic autoimmune process in un-irradiated postnatal NOD female mice [103]. CD4+ Th1 and Th17 T cells have important roles in the pathogenesis of T1D [104]. While the effector function of Th1 cells has been well established, that of Th17 cells appears to be questionable because of their inherent plasticity. Th17 cells are believed to contribute to pathogenicity, but several studies indicate that Th17 cells also transfer disease through conversion to Th1 cells in vivo [105]. Another important cell clone of CD4+ T cells is Foxp3+ Tregs, which promote the maintenance of peripheral tolerance, but they ultimately fail in autoimmune diseases. The trajectory that leads to Treg failure in controlling autoreactive effector T cells during autoimmunity is not well understood. Recent studies emphasized the role of inflammatory cytokines, such as IL-6, in inhibiting or subverting Treg function, underscored the issue of Treg plasticity, and examined the possible resistance of autoimmune T cells to Treg-mediated control and Treg-associated inhibitory cytokines transformation growth factor beta (TGF-β), IL-10, and IL-35 in facilitating Treg suppressive activity and promoting Treg generation [106].
Administration of TCV in Animal Models in T1D
The NOD mouse strain provides an excellent model of autoimmune disease and an important tool for dissecting tolerance mechanisms. The NOD mouse develops spontaneous autoimmune diabetes, which shares considerable similarities with autoimmune or T1D in human subjects, including the presence of pancreas-specific autoantibodies and autoreactive CD4+ and CD8+ T cells. In this sense, it is generally regarded as a valid model for the human insulin-dependent disease [107].
Elias et al. discovered a functionally important peptide that has been spotted within the sequence of the human variant of the 65-kDa heat shock protein (HSP-65) molecule. The pathogenesis of diabetes in NOD strain mice was associated with T cell reactivity to an antigen cross-reactive with HSP-65. To identify peptide epitopes that were critical to the insulin-dependent diabetes mellitus of NOD mice, they studied the specificities of Th cells capable of causing hyperglycemia and diabetes. Alternatively, both attenuated pathogenic T cells and peptide itself can downregulate immunity to HSP-65 and be used as therapeutic T cell vaccines to abort the diabetogenic process. As a result, T cell vaccination and specific peptide therapy are feasible in dealing with spontaneous autoimmune diabetes [108]. Methods to attenuate autoreactive T cells that would be subsequently used as a T cell vaccine vary. Initial studies in autoimmune disease used ultraviolet light and 8-methoxypsoralen, while succeeding research turned to some cytoxic drugs such as deoxycoformycin and deoxyadenosine (dCF/dAdo) [108, 109].
On this score, Wang et al. conducted a piece of research that used T cell clones reactive to GAD65 p206-220, which is a strong trigger of β cell-specific autoimmunity in multiple low doses (MLD) of streptozotocin (STZ)-induced T1D models. Blood glucose level and body weight improved in the TCV-treated group, accompanied by decreased production of both IL-17 and IL-23 in intrapancreatic infiltrating lymphocytes (IPL). This observation may indicate suppressed function of intrapancreatic Th17 cells. The effect was produced by signal transducer and activator of transcription 3 (Stat3) phosphorylation-mediated retinoic acid-related orphan receptor γt (RORγt) inhibition [110].
Mechanisms of T Cell Vaccination
Anti-idiotypic Network
Anti-idiotypic or anti-clonotypic response is a specific immune response of TCV that relies on the presence of a T cell population that is poised to respond to peptide derived from TCRs of autoreactive T cells. As members of the immunoglobulin superfamily, TCRs are heterodimers composed of two chains (α and β or γ and δ). Most T cells express αβ TCRs, which are generated by a series of gene rearrangements resembling that of immunoglobulin gene segments in B cells. As is the case with immunoglobulins, each TCR α/β and γ/δ chain consists of structural framework regions (FRs) and complementarity-determining regions (CDRs) 1, 2, and 3 that form the binding site for conventional antigens. The specific recognition of antigen (in the case of TCV, TCR peptide from autoreactive T cells) is predominantly contingent on the contact with TCR determinants within the hypervariable CDR3 regions or less variable CDR2 regions [111].
Anti-idiotypic T cells, which consist of both CD4+ and CD8+ T cells, provoke the anti-idiotypic T cell and humoral response against the autoreactive CD4+ or CD8+ T cell lines after TCV, as predicted by characteristic sequence diversity within these regions [31, 34, 35, 112]. Studies performed in a variety of autoimmune models have suggested that the CDR3 region from autoreactive T cells exhibits sequence homology to those in humans with autoimmunity. This finding highlights the role of the CDR3 region in promoting the interaction between autoreactive T cells and anti-idiotypic T cells [95].
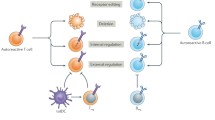
The CD8+ anti-idiotypic T cells presented by class I MHC (HLA-E in human, Qa-1 in mice, which are nonclassic MHC-I molecules that bind hydrophobic peptides, including the leader sequences of class I HLA molecules and components of TCR) [71, 113] may be cytotoxic against TCR determinants and are inhibitory for CD4+ effector T cells, thus causing deletion or inhibition of pathogenic T cell clones present in the vaccinating lines [71] (Fig. 1). In EAE, CD8+ T cell-mediated cytotoxicity appears to be more important than Abs against the MBP-specific T cells [114]. The CD4+ T cells are the major cytokine producers and are capable of inhibiting proliferation of autoreactive T cells by recognition of idiotypic T cell determinants in the context of MHC II molecules. They secrete a variety of cytokines, including IL-4 and IL-10 (Th2 cell phenotype) [21, 114], which may exert regulatory effects on the potentially pathogenic Th1 cells selected for the TCV. TCV induces not only T cell but also B cell reactivity and namely production of anti-idiotypic antibodies capable of binding and inhibiting autoreactive T cell clones. Anti-idiotypic antibodies belong to IgG isotype recognizing TCR determinants irrespective of MHC molecules. The mechanism of action of these antibodies could be related to shielding and functional TCR blockade. In lupus-prone MRL/lpr mice, anti-idiotypic antibodies recognizing a 12 amino acid sequence of clone dna51 TCR Vβ 8.3 CDR 3 were detected and suppressed pathogenic dna51 cell proliferation. However, compared to anti-idiotypic T cell response, the humoral effect is less important in regulating the abnormal immune system in ADs, because in some human trials of MS, no major antibody responses were observed toward the vaccine clones in vaccinated patients, and vaccination with Vβ 17 CDR2 peptides vaccine in RA showed similar results [81, 114]. The reactivity and regulatory properties of anti-idiotypic antibodies induced by T cell vaccination need further explanation (Fig. 1).
Complex anti-idiotypic network induced by TCV: the CD8+ anti-idiotypic T cells mediate a cytotoxic effect while CD4+ anti-idiotypic T cells are the main cytokine provider (IL-4 and IL-10), and comparative minial humoral response also takes part in the process of specific anti-reactive T cells regulation. See text for detailed information on the different components of the anti-idiotypic network
Anti-ergotypic Network
The term “ergotopes” came from the Greek ergon, meaning “work” or “activity.” It is used to define the TCR nonspecific response to autoreactive pathogenic T cells in autoimmune diseases. Regulation of anti-ergotypic network originates from the finding that only activated anti-MBP T cells could cause EAE, and the surprising observation that activated T cells whose TCR was not specific for MBP, the target antigen in EAE could also act as a T cell vaccine to protect rats against EAE [24, 115]. These findings remind us that the anti-idiotypic mechanism, which is specific for the autoreactive T cells, does not account for all the effects of TCV observed in animal models, because the inactive T cells that share the same TCR peptide as the activated T cells cannot function well as the activated cells.
The anti-ergotypic response is generally composed of three major components: (1) the target T cells: they can be CD8+ or CD4+ T cells that lead to the imbalance of immunity in vivo. (2) The ergotope: They are constituted by a T cell-restricted ergotope not expressed by other cell types, such as TCR and the alpha chain of the IL-2 receptor (CD25), or a widely expressed, shared ergotope such as HSP 60 [116–118]. (3) The anti-ergotypic T cells: They are detectable in the naive immune system, but their quantity can be expanded during the induction of an immune response against autoreactive T cells, or as a result of TCV or specific, anti-ergotypic vaccination [119].
The anti-ergotypic T cells include both TCRαβ + and TCRγδ + T cells. The response of TCRαβ + CD8+ anti-ergotypic T cells occurs at the early phase of the immune response after TCV, which is restricted by classical MHC class I and dependent on B7 and CD28 molecules. The CD4+ subset of anti-ergotypic TCRαβ + T cells has been detected after the priming in vivo to anti-ergotope and is restricted to classical MHC class II molecules [116]. By contrast, the response of naive TCRγδ + anti-ergotypic T cells is not inhibited by antibodies to classical MHC class I or MHC class II molecules (manuscript submitted for publication). But it also depends on B7 and CD28 molecules [115] (Fig. 2). These TCRγδ + anti-ergotypic T cells are believed to be associated with human organ-specific autoimmune diseases. In response to ergotope of activated T cells, the TCRγδ + T cells secrete several cytokines including IFN-γ and TNF-α and have the capacity to reduce autoantibody production like anti-dsDNA Ab, in a contact-dependent manner [120]. However, the cytokine secretion profile of TCRαβ + T remains controversial, as some research reported TCRαβ + T cell proliferation without any detectable cytokines, while other studies showed that the CD8+ subset of TCRαβ + T cells did secrete IFN-γ, TNF-α/β, and TGF-β [34, 115] (reviewed by Avishai Mimran and Irun R. Cohen, Fig. 2).
Complex anti-ergotypic network induced by TCV: a subset of effector T cells are activated by markers only commonly expressed on the surface of activated T cells, termed “ergotope.” Through the presentation of ergotope peptide by professional APC (macrophage/dendritic cell) and activated autoreactive T cells, anti-ergotypic T cells proliferate and secrete multiple cytokines to downregulate the abnormal immune response. See text for detailed information on the different components of the anti-ergotypic network
The continual battle between self-reactive T cells and suppressive Tregs is critical in determining whether autoimmunity commences. Scientific and medical interest in tolerance mechanisms have brought about the discovery of a whole array of immune-regulatory T cells. These different suppressor subsets are individually able to downregulate, in their own way, the activity of pathogenic autoreactive T cells. Among them, Foxp3+ regulatory T cells (Foxp3+ Tregs) have emerged as the primary mediator in the peripheral tolerance mechanisms and the control of self-reactive T cells, thus safeguarding the tolerance barrier [106]. These Tregs can selectively expand after vaccination, which is corresponding with certain characteristic shift in the Vβ gene distribution pattern of peripheral T cells. Through producing IL-10 or TGF-β and expressing a high level of transcription factor Foxp3 in treated patients, anti-ergotypic Tregs exhibit increased inhibitory activity and adaptively transfer resistance to adjuvant arthritis in naive rats [71]. Improvement of disease severity and mortality has been witnessed when Tregs were depleted by treatment with anti-CD25 antibodies, following PLP (139–151) immunization to induce EAE [121]. These attempts indicate a leading role of anti-ergotypic Tregs in the process of anti-ergotypic response induced by TCV [27, 33].
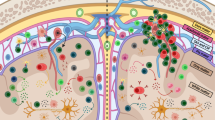
There are two pathways in which anti-ergotypic T cells respond to ergotopes, either by whole, activated T cells directly or professional APCs indirectly. But the responses to these two forms of specific activation differ [117, 122]. The difference is critical in the life history of the anti-ergotypic regulation network. In the first pathway, the stimulated anti-ergotypic T cells are activated by whole activated stimulator T cells and secrete their cytokines (IL-10 or TGF-β) to downregulate their activated target T cells. But in the process of this regulation, anti-ergotypic T cells themselves become anergic and cannot be reactivated by a second contact with activated effector T cell. In other words, they are extinguished by the effector cells they downregulate (Fig. 3). Over the years, this irreversible poor growth behavior has effectively prevented researchers from raising lines of anti-ergotypic T cells in vitro and characterizing anti-ergotypic T cells. Downregulation of anti-ergotypic T cells by activated effector T cells might also explain how the induction of a disease such as adjuvant arthritis might downregulate naive anti-ergotypic T cells [116]. Other professional APCs, such as macrophages and dendritic cells, can present ergotope peptides to anti-ergotypic T cells, but the response of anti-ergotypic T cells to APC/peptide stimulation is not the same as the response to whole, activated T cells. In this regard, Cohen et al. discovered that “cross-presentation” of ergotope peptides by APCs stimulates the anti-erg T cells without making them anergic and dead. Therefore, anti-ergotypic activation by professional APCs (non-T cell) allows cyclical self-renewal of anti-ergotypic T cells (Fig. 3).
The two pathways that anti-ergotypic T cells respond to ergotopes lead to opposite outcome of Treg cycling. Some professional APCs, such as macrophages and dendric cells, can present ergotope peptides to anti-ergotypic T cells, and this kind of “cross-presentation” of ergotope peptides by APCs stimulates the anti-ergotypic T cells without causing them to become anergic and dead. Thus, anti-ergotypic activation by professional APCs allows the cyclical Treg self-renewal (Treg renewal, blue arrows). Resting Tregs can also be activated by ergotope from whole activated autoreactive T cells and downregulate the activated target autoreactive T cells by secreting cytokines (IL-10 or TGF-β, figure not shown). After that, the activated anti-erg T cells themselves become anergic (Treg loss, red arrows). See text for detailed information on Treg cycling
Conclusion
In conclusion, TCV has already been proven to be tolerable and safe to ADs in various animal models and human trials [27, 35, 36, 60, 62, 123]. A complicated anti-idiotypic and anti-ergotypic network is involved in the immune regulation of TCV, and several mainstream cytokines and lymphocyte phenotype transfer also take part in the process of depleting autoreactive T cells and reversing abnormal autoimmune responses. However, undefined humoral response and ambiguous roles of some uncommon lymphocyte populations including Tfh cells and TCRγδ + T cells necessitate further studies. Clinically, the protocol of TCV varies from a single selected autoreactive T cell clones to multi-epitope TCR peptides. These strategies do not meet with uniform success in the pool of ADs due to difficulties in selecting appropriate clinical end points and background treatments, or as a result of the high degree of heterogeneity among patients with ADs. We believe the promising findings from TCV in MS will serve as the pioneer of a wider application of TCV in ADs. A more specific and precise designation is of great importance in its future administration.
References
Wahren-Herlenius M, Dorner T (2013) Immunopathogenic mechanisms of systemic autoimmune disease. Lancet 382:819–831
Koutsokeras T, Healy T (2014) Systemic lupus erythematosus and lupus nephritis. Nat Rev Drug Discov 13:173–174
Chan AC, Carter PJ (2010) Therapeutic antibodies for autoimmunity and inflammation. Nat Rev Immunol 10:301–316
Croft M, Benedict CA, Ware CF (2013) Clinical targeting of the TNF and TNFR superfamilies. Nat Rev Drug Discov 12:147–168
Sathish JG, Sethu S, Bielsky MC, de Haan L, French NS, Govindappa K et al (2013) Challenges and approaches for the development of safer immunomodulatory biologics. Nat Rev Drug Discov 12:306–324
Murphy G, Lisnevskaia L, Isenberg D (2013) Systemic lupus erythematosus and other autoimmune rheumatic diseases: challenges to treatment. Lancet 382:809–818
Selmi C, Lu Q, Humble MC (2012) Heritability versus the role of the environment in autoimmunity. J Autoimmun 39:249–252
Smyk D, Rigopoulou EI, Baum H, Burroughs AK, Vergani D, Bogdanos DP (2012) Autoimmunity and environment: am I at risk? Clin Rev Allergy Immunol 42:199–212
McNally RJ (2010) Are transient environmental agents involved in the aetiology of primary biliary cirrhosis? Dis Markers 29:275–276
Bogdanos DP, Smyk DS, Rigopoulou EI, Mytilinaiou MG, Heneghan MA, Selmi C et al (2012) Twin studies in autoimmune disease: genetics, gender and environment. J Autoimmun 38:J156–J169
Chen RC, Naiyanetr P, Shu SA, Wang J, Yang GX, Kenny TP et al (2013) Antimitochondrial antibody heterogeneity and the xenobiotic etiology of primary biliary cirrhosis. Hepatology 57:1498–1508
Sthoeger Z, Sharabi A, Mozes E (2014) Novel approaches to the development of targeted therapeutic agents for systemic lupus erythematosus. J Autoimmun. pii: S0896-8411(14)00099-7. doi:10.1016/j.jaut.2014.06.002
Keijzer C, van der Zee R, van Eden W, Broere F (2013) Treg inducing adjuvants for therapeutic vaccination against chronic inflammatory diseases. Front Immunol 4:245
Serr I, Weigmann B, Franke RK, Daniel C (2014) Treg vaccination in autoimmune type 1 diabetes. BioDrugs Clin Immunotherapeut Biopharm Gene Ther 28:7–16
Valaperti A, Nishii M, Germano D, Liu PP, Eriksson U (2013) Vaccination with Flt3L-induced CD8alpha+ dendritic cells prevents CD4+ T helper cell-mediated experimental autoimmune myocarditis. Vaccine 31:4802–4811
Harrison LC, Wentworth JM, Zhang Y, Bandala-Sanchez E, Bohmer RM, Neale AM et al (2013) Antigen-based vaccination and prevention of type 1 diabetes. Curr Diabetes Rep 13:616–623
Cohen IR (2014) Activation of benign autoimmunity as both tumor and autoimmune disease immunotherapy: a comprehensive review. J Autoimmun. pii: S0896-8411(14)00091-2. doi:10.1016/j.jaut.2014.05.002
Maueroder C, Munoz LE, Chaurio RA, Herrmann M, Schett G, Berens C (2014) Tumor immunotherapy: lessons from autoimmunity. Front Immunol 5:212
Tian Z, Gershwin ME, Zhang C (2012) Regulatory NK cells in autoimmune disease. J Autoimmun 39:206–215
Ben-Nun A, Wekerle H, Cohen IR (1981) Vaccination against autoimmune encephalomyelitis with T-lymphocyte line cells reactive against myelin basic protein. Nature 292:60–61
Rangachari M, Kuchroo VK (2013) Using EAE to better understand principles of immune function and autoimmune pathology. J Autoimmun 45:31–39
Rivera VM (2011) Tovaxin for multiple sclerosis. Expert Opin Biol Ther 11:961–967
Yao Y, Han W, Liang J, Ji J, Wang J, Cantor H et al (2013) Glatiramer acetate ameliorates inflammatory bowel disease in mice through the induction of Qa-1-restricted CD8(+) regulatory cells. Eur J Immunol 43:125–136
Lohse AW, Mor F, Karin N, Cohen IR (1989) Control of experimental autoimmune encephalomyelitis by T cells responding to activated T cells. Science 244:820–822
Holoshitz J, Naparstek Y, Ben-Nun A, Cohen IR (1983) Lines of T lymphocytes induce or vaccinate against autoimmune arthritis. Science 219:56–58
Greidinger EL, Zang Y, Fernandez I, Berho M, Nassiri M, Martinez L et al (2009) Tissue targeting of anti-RNP autoimmunity: effects of T cells and myeloid dendritic cells in a murine model. Arthritis Rheum 60:534–542
Hermans G, Medaer R, Raus J, Stinissen P (2000) Myelin reactive T cells after T cell vaccination in multiple sclerosis: cytokine profile and depletion by additional immunizations. J Neuroimmunol 102:79–84
Kaushansky N, Kerlerzzde Rosbo N, Zilkha-Falb R, Yosef-Hemo R, Cohen L, Ben-Nun A (2011) Multi-epitope-targeted’ immune-specific therapy for a multiple sclerosis-like disease via engineered multi-epitope protein is superior to peptides. PLoS One 6:e27860
Medaer R, Stinissen P, Truyen L, Raus J, Zhang J (1995) Depletion of myelin-basic-protein autoreactive T cells by T-cell vaccination: pilot trial in multiple sclerosis. Lancet 346:807–808
Zhang J, Medaer R, Stinissen P, Hafler D, Raus J (1993) MHC-restricted depletion of human myelin basic protein-reactive T cells by T cell vaccination. Science 261:1451–1454
Hong J, Zang YC, Tejada-Simon MV, Li S, Rivera VM, Killian J et al (2000) Reactivity and regulatory properties of human anti-idiotypic antibodies induced by T cell vaccination. J Immunol 165:6858–6864
Lider O, Beraud E, Reshef T, Friedman A, Cohen IR (1989) Vaccination against experimental autoimmune encephalomyelitis using a subencephalitogenic dose of autoimmune effector T cells. (2). Induction of a protective anti-idiotypic response. J Autoimmun 2:87–99
Lider O, Reshef T, Beraud E, Ben-Nun A, Cohen IR (1988) Anti-idiotypic network induced by T cell vaccination against experimental autoimmune encephalomyelitis. Science 239:181–183
Mimran A, Cohen IR (2005) Regulatory T cells in autoimmune diseases: anti-ergotypic T cells. Int Rev Immunol 24:159–179
Zang YC, Hong J, Rivera VM, Killian J, Zhang JZ (2000) Preferential recognition of TCR hypervariable regions by human anti-idiotypic T cells induced by T cell vaccination. J Immunol 164:4011–4017
Fox E, Wynn D, Cohan S, Rill D, McGuire D, Markowitz C (2012) A randomized clinical trial of autologous T-cell therapy in multiple sclerosis: subset analysis and implications for trial design. Mult Scler 18:843–852
Zhang J (2004) T cell vaccination as an immunotherapy for autoimmune diseases. Cell Mol Immunol 1:321–327
Zhang J, Stinissen P, Medaer R, Raus J (1996) T cell vaccination: clinical application in autoimmune diseases. J Mol Med (Berl) 74:653–662
Martin R, McFarland HF, McFarlin DE (1992) Immunological aspects of demyelinating diseases. Annu Rev Immunol 10:153–187
Frohman EM, Racke MK, Raine CS (2006) Multiple sclerosis—the plaque and its pathogenesis. N Engl J Med 354:942–955
Mekala DJ, Geiger TL (2005) Immunotherapy of autoimmune encephalomyelitis with redirected CD4+CD25+ T lymphocytes. Blood 105:2090–2092
Zamvil S, Nelson P, Trotter J, Mitchell D, Knobler R, Fritz R et al (1985) T-cell clones specific for myelin basic protein induce chronic relapsing paralysis and demyelination. Nature 317:355–358
Zamvil SS, Mitchell DJ, Moore AC, Kitamura K, Steinman L, Rothbard JB (1986) T-cell epitope of the autoantigen myelin basic protein that induces encephalomyelitis. Nature 324:258–260
Tompkins SM, Padilla J, Dal Canto MC, Ting JP, Van Kaer L, Miller SD (2002) De novo central nervous system processing of myelin antigen is required for the initiation of experimental autoimmune encephalomyelitis. J Immunol 168:4173–4183
Tuohy VK, Lu Z, Sobel RA, Laursen RA, Lees MB (1989) Identification of an encephalitogenic determinant of myelin proteolipid protein for SJL mice. J Immunol 142:1523–1527
Ben-Nun A, deRosbo Kerlero N, Kaushansky N, Eisenstein M, Cohen L, Kaye JF et al (2006) Anatomy of T cell autoimmunity to myelin oligodendrocyte glycoprotein (MOG): prime role of MOG44F in selection and control of MOG-reactive T cells in H-2b mice. Eur J Immunol 36:478–493
Kaushansky N, Eisenstein M, Zilkha-Falb R, Ben-Nun A (2010) The myelin-associated oligodendrocytic basic protein (MOBP) as a relevant primary target autoantigen in multiple sclerosis. Autoimmun Rev 9:233–236
Kaushansky N, Hemo R, Eisenstein M, Ben-Nun A (2007) OSP/claudin-11-induced EAE in mice is mediated by pathogenic T cells primarily governed by OSP192Y residue of major encephalitogenic region OSP179-207. Eur J Immunol 37:2018–2031
Davalos D, Baeten KM, Whitney MA, Mullins ES, Friedman B, Olson ES et al (2014) Early detection of thrombin activity in neuroinflammatory disease. Ann Neurol 75:303–308
Reindl M, Di Pauli F, Rostasy K, Berger T (2013) The spectrum of MOG autoantibody-associated demyelinating diseases. Nat Rev Neurol 9:455–461
Yang Y, Liu Y, Wei P, Peng H, Winger R, Hussain RZ et al (2010) Silencing Nogo-A promotes functional recovery in demyelinating disease. Ann Neurol 67:498–507
Sun D, Whitaker JN, Huang Z, Liu D, Coleclough C, Wekerle H et al (2001) Myelin antigen-specific CD8+ T cells are encephalitogenic and produce severe disease in C57BL/6 mice. J Immunol 166:7579–7587
McMahon EJ, Bailey SL, Castenada CV, Waldner H, Miller SD (2005) Epitope spreading initiates in the CNS in two mouse models of multiple sclerosis. Nat Med 11:335–339
Holz A, Bielekova B, Martin R, Oldstone MB (2000) Myelin-associated oligodendrocytic basic protein: identification of an encephalitogenic epitope and association with multiple sclerosis. J Immunol 164:1103–1109
Volovitz I, Marmor Y, Mor F, Flugel A, Odoardi F, Eisenbach L et al (2010) T cell vaccination induces the elimination of EAE effector T cells: analysis using GFP-transduced, encephalitogenic T cells. J Autoimmun 35:135–144
Zhang JZ, Rivera VM, Tejada-Simon MV, Yang D, Hong J, Li S et al (2002) T cell vaccination in multiple sclerosis: results of a preliminary study. J Neurol 249:212–218
Correale J, Lund B, McMillan M, Ko DY, McCarthy K, Weiner LP (2000) T cell vaccination in secondary progressive multiple sclerosis. J Neuroimmunol 107:130–139
Hafler DA, Cohen I, Benjamin DS, Weiner HL (1992) T cell vaccination in multiple sclerosis: a preliminary report. Clin Immunol Immunopathol 62:307–313
Van der Aa A, Hellings N, Medaer R, Gelin G, Palmers Y, Raus J et al (2003) T cell vaccination in multiple sclerosis patients with autologous CSF-derived activated T cells: results from a pilot study. Clin Exp Immunol 131:155–168
Karussis D, Shor H, Yachnin J, Lanxner N, Amiel M, Baruch K et al (2012) T cell vaccination benefits relapsing progressive multiple sclerosis patients: a randomized, double-blind clinical trial. PLoS One 7:e50478
Loftus B, Newsom B, Montgomery M, Von Gynz-Rekowski K, Riser M, Inman S et al (2009) Autologous attenuated T-cell vaccine (Tovaxin) dose escalation in multiple sclerosis relapsing-remitting and secondary progressive patients nonresponsive to approved immunomodulatory therapies. Clin Immunol 131:202–215
Achiron A, Lavie G, Kishner I, Stern Y, Sarova-Pinhas I, Ben-Aharon T et al (2004) T cell vaccination in multiple sclerosis relapsing-remitting nonresponders patients. Clin Immunol 113:155–160
Hellings N, Stinissen P (2008) Tovaxin, radiation-attenuated, patient-specific T-cells for the therapeutic vaccination of multiple sclerosis. Curr Opin Investig Drugs 9:534–540
Achiron A, Mandel M (2004) T-cell vaccination in multiple sclerosis. Autoimmun Rev 3:25–32
Scott DL, Wolfe F, Huizinga TW (2010) Rheumatoid arthritis. Lancet 376:1094–1108
Boissier MC, Semerano L, Challal S, Saidenberg-Kermanac’h N, Falgarone G (2012) Rheumatoid arthritis: from autoimmunity to synovitis and joint destruction. J Autoimmun 39:222–228
Backlund J, Li C, Jansson E, Carlsen S, Merky P, Nandakumar KS et al (2013) C57BL/6 mice need MHC class II Aq to develop collagen-induced arthritis dependent on autoreactive T cells. Ann Rheum Dis 72:1225–1232
Grom AA, Thompson SD, Luyrink L, Passo M, Choi E, Glass DN (1993) Dominant T-cell-receptor beta chain variable region V beta 14+ clones in juvenile rheumatoid arthritis. Proc Natl Acad Sci U S A 90:11104–11108
Li Y, Sun GR, Tumang JR, Crow MK, Friedman SM (1994) CDR3 sequence motifs shared by oligoclonal rheumatoid arthritis synovial T cells. Evidence for an antigen-driven response. J Clin Invest 94:2525–2531
Ostenstad B, Dybwad A, Lea T, Forre O, Vinje O, Sioud M (1995) Evidence for monoclonal expansion of synovial T cells bearing V alpha 2.1/V beta 5.5 gene segments and recognizing a synthetic peptide that shares homology with a number of putative autoantigens. Immunology 86:168–175
Chen G, Li N, Zang YC, Zhang D, He D, Feng G et al (2007) Vaccination with selected synovial T cells in rheumatoid arthritis. Arthritis Rheum 56:453–463
Pierer M, Rossol M, Kaltenhauser S, Arnold S, Hantzschel H, Baerwald C et al (2011) Clonal expansions in selected TCR BV families of rheumatoid arthritis patients are reduced by treatment with the TNFalpha inhibitors etanercept and infliximab. Rheumatol Int 31:1023–1029
Wang J, Wang A, Zeng H, Liu L, Jiang W, Zhu Y et al (2012) Effect of triptolide on T-cell receptor beta variable gene mRNA expression in rats with collagen-induced arthritis. Anat Rec (Hoboken) 295:922–927
Xiao J, Li S, Wang W, Li Y, Zhao W (2007) Protective effects of overexpression TCR Vbeta5.2-HSP70 and TCR Vbeta8.2-HSP70 against collagen-induced arthritis in rats. Cell Mol Immunol 4:439–445
Bridges SL Jr, Moreland LW (1998) T-cell receptor peptide vaccination in the treatment of rheumatoid arthritis. Rheum Dis Clin N Am 24:641–650
Jenkins RN, McGinnis DE (1995) T-cell receptor V beta gene utilization in rheumatoid arthritis. Ann N Y Acad Sci 756:159–172
VanderBorght A, De Keyser F, Geusens P, De Backer M, Malaise M, Baeten D et al (2002) Dynamic T cell receptor clonotype changes in synovial tissue of patients with early rheumatoid arthritis: effects of treatment with cyclosporin A (Neoral). Jo Rheumatol 29:416–426
De Alboran IM, Gutierrez JC, Gonzalo JA, Andreu JL, Marcos MA, Kroemer G et al (1992) lpr T cells vaccinate against lupus in MRL/lpr mice. Eur J Immunol 22:1089–1093
Ge PL, Ma LP, Wang W, Li Y, Zhao WM (2009) Inhibition of collagen-induced arthritis by DNA vaccines encoding TCR Vbeta5.2 and TCR Vbeta8.2. Chin Med J 122:1039–1048
Moreland LW, Heck LW Jr, Koopman WJ, Saway PA, Adamson TC, Fronek Z et al (1996) V beta 17 T cell receptor peptide vaccination in rheumatoid arthritis: results of phase I dose escalation study. J Rheumatol 23:1353–1362
Moreland LW, Morgan EE, Adamson TC 3rd, Fronek Z, Calabrese LH, Cash JM et al (1998) T cell receptor peptide vaccination in rheumatoid arthritis: a placebo-controlled trial using a combination of Vbeta3, Vbeta14, and Vbeta17 peptides. Arthritis Rheum 41:1919–1929
van Laar JM, Miltenburg AM, Verdonk MJ, Leow A, Elferink BG, Daha MR et al (1993) Effects of inoculation with attenuated autologous T cells in patients with rheumatoid arthritis. J Autoimmun 6:159–167
Janko C, Schorn C, Grossmayer GE, Frey B, Herrmann M, Gaipl US et al (2008) Inflammatory clearance of apoptotic remnants in systemic lupus erythematosus (SLE). Autoimmun Rev 8:9–12
Ippolito A, Wallace DJ, Gladman D, Fortin PR, Urowitz M, Werth V et al (2011) Autoantibodies in systemic lupus erythematosus: comparison of historical and current assessment of seropositivity. Lupus 20:250–255
Laderach D, Koutouzov S, Bach JF, Yamamoto AM (2003) Concomitant early appearance of anti-ribonucleoprotein and anti-nucleosome antibodies in lupus prone mice. J Autoimmun 20:161–170
Olsen NJ, Karp DR (2014) Autoantibodies and SLE—the threshold for disease. Nat Rev Rheumatol 10:181–186
Alba P, Bento L, Cuadrado MJ, Karim Y, Tungekar MF, Abbs I et al (2003) Anti-dsDNA, anti-Sm antibodies, and the lupus anticoagulant: significant factors associated with lupus nephritis. Ann Rheum Dis 62:556–560
Kirou KA, Lee C, George S, Louca K, Peterson MG, Crow MK (2005) Activation of the interferon-alpha pathway identifies a subgroup of systemic lupus erythematosus patients with distinct serologic features and active disease. Arthritis Rheum 52:1491–1503
Wenderfer SE, Canter D, Deguzman M, Muscal E (2014) A69: Lupus nephritis and autoantibody characteristics of a single center cohort of male pediatric SLE patients. Arthritis Rheumatol 66(Suppl 11):S101
Attridge K, Walker LS (2014)Homeostasis and function of regulatory T cells(Tregs)in vivo: lessons from TCR-transgenic Tregs. Immunol Rev 259:23–39
Wang YM, Zhang GY, Hu M, Polhill T, Sawyer A, Zhou JJ et al (2012) CD8+ regulatory T cells induced by T cell vaccination protect against autoimmune nephritis. J Am Soc Nephroly : JASN 23:1058–1067
Kim HJ, Verbinnen B, Tang X, Lu L, Cantor H (2010) Inhibition of follicular T-helper cells by CD8(+) regulatory T cells is essential for self tolerance. Nature 467:328–332
Madakamutil LT, Maricic I, Sercarz E, Kumar V (2003) Regulatory T cells control autoimmunity in vivo by inducing apoptotic depletion of activated pathogenic lymphocytes. J Immunol 170:2985–2992
Smith TR, Kumar V (2008) Revival of CD8+ Treg-mediated suppression. Trends Immunol 29:337–342
Fujii T, Okada M, Fujita Y, Sato T, Tanaka M, Usui T et al (2009) Vaccination with autoreactive CD4(+)Th1 clones in lupus-prone MRL/Mp-Fas(lpr/lpr) mice. J Autoimmun 33:125–134
Ben-Yehuda A, Bar-Tana R, Livoff A, Ron N, Cohen IR, Naparstek Y (1996) Lymph node cell vaccination against the lupus syndrome of MRL/lpr/lpr mice. Lupus 5:232–236
Li ZG, Mu R, Dai ZP, Gao XM (2005) T cell vaccination in systemic lupus erythematosus with autologous activated T cells. Lupus 14:884–889
Smolen JS, Klippel JH, Penner E, Reichlin M, Steinberg AD, Chused TM et al (1987) HLA-DR antigens in systemic lupus erythematosus: association with specificity of autoantibody responses to nuclear antigens. Ann Rheum Dis 46:457–462
Trivedi S, Zang Y, Culpepper S, Rosenbaum E, Fernandez I, Martinez L et al (2010) T cell vaccination therapy in an induced model of anti-RNP autoimmune glomerulonephritis. Clin Immunol 137:281–287
Zang Y, Martinez L, Fernandez I, Pignac-Kobinger J, Greidinger EL (2014) Conservation of pathogenic TCR homology across class II restrictions in anti-ribonucleoprotein autoimmunity: extended efficacy of T cell vaccine therapy. J Immunol 192:4093–4102
Mathis D, Vence L, Benoist C (2001) Beta-Cell death during progression to diabetes. Nature 414:792–798
Formby B, Shao T (1993) T cell vaccination against autoimmune diabetes in nonobese diabetic mice. Ann Clin Lab Sci 23:137–147
Knip M, Siljander H (2008) Autoimmune mechanisms in type 1 diabetes. Autoimmun Rev 7:550–557
Panoutsakopoulou V, Huster KM, McCarty N, Feinberg E, Wang R, Wucherpfennig KW et al (2004) Suppression of autoimmune disease after vaccination with autoreactive T cells that express Qa-1 peptide complexes. J Clin Invest 113:1218–1224
Haskins K, Cooke A (2011) CD4 T cells and their antigens in the pathogenesis of autoimmune diabetes. Curr Opin Immunol 23:739–745
Bettini M, Vignali DA (2009) Regulatory T cells and inhibitory cytokines in autoimmunity. Curr Opin Immunol 21:612–618
Anderson MS, Bluestone JA (2005) The NOD mouse: a model of immune dysregulation. Annu Rev Immunol 23:447–485
Elias D, Reshef T, Birk OS, van der Zee R, Walker MD, Cohen IR (1991) Vaccination against autoimmune mouse diabetes with a T-cell epitope of the human 65-kDa heat shock protein. Proc Natl Acad Sci U S A 88:3088–3091
Marks DI, Iannoni B, Coote MA, Mandel TE, Fox RM (1991) Prevention of cyclophosphamide-induced and spontaneous diabetes in NOD mice by syngeneic splenocytes treated with cytotoxic drugs. Autoimmunity 11:73–79
Wang M, Yang L, Sheng X, Chen W, Tang H, Sheng H et al (2011) T-cell vaccination leads to suppression of intrapancreatic Th17 cells through Stat3-mediated RORgammat inhibition in autoimmune diabetes. Cell Res 21:1358–1369
Nikolich-Zugich J, Slifka MK, Messaoudi I (2004) The many important facets of T-cell repertoire diversity. Nat Rev Immunol 4:123–132
Lal G, Shaila MS, Nayak R (2006) Activated mouse T cells downregulate, process and present their surface TCR to cognate anti-idiotypic CD4+ T cells. Immunol Cell Biol 84:145–153
Lu L, Werneck MB, Cantor H (2006) The immunoregulatory effects of Qa-1. Immunol Rev 212:51–59
Hermans G, Denzer U, Lohse A, Raus J, Stinissen P (1999) Cellular and humoral immune responses against autoreactive T cells in multiple sclerosis patients after T cell vaccination. J Autoimmun 13:233–246
Correale J, Rojany M, Weiner LP (1997) Human CD8+ TCR-alpha beta(+) and TCR-gamma delta(+) cells modulate autologous autoreactive neuroantigen-specific CD4+ T-cells by different mechanisms. J Neuroimmunol 80:47–64
Mimran A, Mor F, Carmi P, Quintana FJ, Rotter V, Cohen IR (2004) DNA vaccination with CD25 protects rats from adjuvant arthritis and induces an antiergotypic response. J Clin Invest 113:924–932
Mimran A, Mor F, Quintana FJ, Cohen IR (2005) Anti-ergotypic T cells in naive rats. J Autoimmun 24:191–201
Quintana FJ, Mimran A, Carmi P, Mor F, Cohen IR (2008) HSP60 as a target of anti-ergotypic regulatory T cells. PLoS One 3:e4026
Hellings N, Raus J, Stinissen P (2006) T-cell-based immunotherapy in multiple sclerosis: induction of regulatory immune networks by T-cell vaccination. Expert Rev Clin Immunol 2:705–716
Fujii T, Okada M, Craft J (2002) Regulation of T cell-dependent autoantibody production by a gammadelta T cell line derived from lupus-prone mice. Cell Immunol 217:23–35
Zhang X, Koldzic DN, Izikson L, Reddy J, Nazareno RF, Sakaguchi S et al (2004) IL-10 is involved in the suppression of experimental autoimmune encephalomyelitis by CD25+CD4+ regulatory T cells. Int Immunol 16:249–256
Vandenbark AA, Chou YK, Whitham R, Mass M, Buenafe A, Liefeld D et al (1996) Treatment of multiple sclerosis with T-cell receptor peptides: results of a double-blind pilot trial. Nat Med 2:1109–1115
Leuenberger T, Paterka M, Reuter E, Herz J, Niesner RA, Radbruch H et al (2013) The role of CD8+ T cells and their local interaction with CD4+ T cells in myelin oligodendrocyte glycoprotein35-55-induced experimental autoimmune encephalomyelitis. J Immunol 191:4960–4968
Acknowledgments
This work was supported by the National Natural Science Foundation of China (No. 81210308042, No. 81220108017, and No. 30972745), the National Basic Research Program of China (973 Plan) (2009CB825605), the programs of the Science-Technology Commission of Hunan Province (2011FJ2007, 2011TP4019-7, 2012WK3046, and 2012TT2015), the Fundamental Research Funds for the Central Universities, and the National Key Clinical Speciality Construction Project of National Health and Family Planning Commission of the People’s Republic of China.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Huang, X., Wu, H. & Lu, Q. The Mechanisms and Applications of T Cell Vaccination for Autoimmune Diseases: a Comprehensive Review. Clinic Rev Allerg Immunol 47, 219–233 (2014). https://doi.org/10.1007/s12016-014-8439-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12016-014-8439-6