Abstract
Multi-drug resistance (MDR) can be explained by a drug handling-type activity. In this context it is also necessary to consider the multi-specificity between drugs and drug transporters in order to explain MDR. Accordingly, the efficiency of drug efflux in MDR has always been a conceptual problem in biochemistry. Indeed, how one protein can expel, from cells, hundreds of compounds with high specificity is still controversial today. To safeguard the notion of biochemical specificity, many studies have suggested alternative mechanisms to Pgp-mediated drug resistance, which do not involve the handling of drugs. However, none of these studies have definitively ruled out the possibility concept of drug handling. Thus, until now it was not possible to imagine MDR without drug-transporter affinity or specificity. However, drug-transporter affinity is not always needed to generate what appears to be a very efficient chemical reaction. Indeed, based on the fact that bi-dimensional diffusion properties (i.e. diffusion in the membrane) are paramount to explain drug pumping-mediated MDR, it is possible to suggest how specific mathematical properties of random motions can be used to construct a model of Pgp-MDR, providing that Pgp oscillates between open/drug-accepting and closed/drug-expelling conformations. This different viewpoint highlights the fact that the multi-specificity of drug transporters and the “vacuum cleaner” hypothesis may actually be two sides of the same coin, both explained by the diffusion properties of drugs in the membrane. After retrieving basic results, predictions will be highlighted. Finally, the coherence of this model in the context of cancer biology will be discussed further.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In 2007, the American Cancer Society report concluded that cancer kills ~7 m person a year worldwide (1 in 8 deaths). One of the major concerns in this field is that many cancers fail to respond to chemotherapy by acquiring multi-drug resistance (MDR), to which has been attributed the failure of treatment in over 90% of patients with metastatic cancer [25]. Furthermore, it is now recognized that cancer aggressiveness, i.e. the metastatic potential of tumours, is related to MDR [18, 44]. Although MDR can have several causes [40], one major form of resistance to chemotherapy has been correlated with the presence of membrane molecular “pumps” that actively transport drugs out of the cell. Historically, it was in 1973 that Dano Keld suggested that the mechanism of resistance was due to an outward efflux of drugs that “vacuum clean” drugs from cells [4]. This hypothesis gained credence 3 years later when P-glycoprotein (Pgp) was identified as the membrane protein over-expressed in MDR cancer cells that actively extrude membrane-embedded drugs [17]. Since then and further to an important body of works, a recent structural study has enabled the molecular basis of Pgp to be defined with remarkable precision [2]. This last study suggests that when ATP molecules bind to Pgp, slight conformational changes promote a “power stroke” leading to the passage of drugs from the inner leaflet to the outer one [2, 36].
Although the molecular model of Pgp has permitted a relatively simple representation of MDR in agreement with the usual concepts issued from the field of biochemistry, how a single protein can expel structurally different drugs is still poorly understood. Indeed, “controversy remains over how P-gp recognizes hundreds of different hydrophobic drugs and pump them out of the cell…” [15]. Beyond this last remark, there is something far more significant and important at stake: the Pgp-mediated MDR model does not conform to the fundamental notion of specificity and seems to challenge the roots of biochemistry. This conceptual issue was exposed early and very clearly by Paul Roepe: “…MDR cells are resistant to, and/or exhibit decreased retention of, literally hundreds of different hydrophobic compounds that are structurally divergent… Membrane transporters, like soluble enzymes, are exquisitely substrate-specific… If transporters were not specific, the cell would eventually become a high entropy chaotic mess…[as there are] no structural molecular motifs common to all the many different agents to which MDR cells are resistant…MDR protein is a very unusual enzyme with extraordinarily broad substrate recognition capabilities; that is, it violates the law of enzyme specificity” [33].
Given the paramount importance of the notion of “specificity” in classical biochemistry and cell biology, various models were put forward to explain MDR without absolutely requiring a drug-handling activity; by characterizing the interactions between the physico-chemical properties of drugs and biophysical changes recurrent in MDR cells, i.e. involving membrane potential [43], cytosolic pH [40, 43] and membrane recycling [29, 30].
Although conceptually satisfying and in accordance with the notion of specificity and, hence, basic Laws of biochemistry, it is worth noting that all these models have their own limits and that they cannot rule out completely the involvement of drug-handling by transporters. Indeed, the transport of drugs can coexist with the biophysical changes mentioned above. For example, it was demonstrated that changes in the cytosolic pH of MDR cells occurs in parallel to Pgp-mediated drug pumping, in a symport-like mechanism [12]. Given the paramount importance of cytosolic pH changes in the models that have tried to explain MDR without using a drug-handling-type activity, this study suggests that all the biophysical changes observed are parallels to Pgp-mediated drug extrusion [1, 13].
Thus, how Pgp functions is still an open and debated matter.
The central idea that leads to this conceptual issue is the fact that Pgp is considered as a transporter that must “handle” drugs to expel them. As a result, it is the “handling” of drugs that suggests the existence of some chemical reactions between Pgp and drugs. Naturally, if a chemical reaction is suggested, all the formalism from enzymology can then be used and thus the notions of affinity or specificity should apply.
To resolve the issue, i.e. to step away from the strict “handling” mechanism, one approach is to suggest that Pgp oscillates between two conformations: a drug-accepting/open conformation and a closed conformation (whereby a drug can be expelled via the power stroke suggested above). Hence, function of ATP concentration, the problem to resolve is to find out the probability that a drug diffusing in the membrane meets a Pgp in an open conformation. Posing the problem this way: (a) is coherent with most biological data concerning Pgp; (b) can explain the role of modulators (we shall develop this point later); and (c) calls in particular mathematical properties emerging from the “random walk” theory that are, sometimes, more informative than basic thermodynamics. In particular, an important result in this field is known as Polya’s theorem. This theorem demonstrates that over long enough periods of time, a diffusion in two dimensions (2D), or lower, will visit all the space; see [28] and references within. Translated in simple terms, this theorem affirms that drugs will meet Pgp if they stay long enough in the membrane.
Given the importance of drug–membrane interactions in MDR [9, 31] to favour the lateral diffusion of drugs in the membrane to meet transporters, this theorem is likely to be central in MDR. As previously discussed [28], to be extruded drugs must come in contact with transporters. If drug transporters oscillate between open (drug-accepting) and closed (drug-expelling) states and if the diffusion takes place in a space that permits the drug to visit the whole space many times, then the drug will inevitably meet a transporter, possibly more than once, until extrusion takes place. It follows that there is no need for high chemical affinity or specificity in this case. Thus, the apparent efficiency of Pgp-mediated multi-drug resistance would simply rely on the capability of the system to promote meetings between drugs and transporters. In this case, this would be driven by the dimensionality of the system in which MDR takes place.
After introducing the problem, a toy model based on random diffusion will be developed, that will allow us to make important predictions and to discuss the role of drugs and modulators in multi-drug resistance. We shall see that we can obtain Michaelis–Menten-like equations for Pgp function in which no affinity appears. The model will be discussed against data from the field of drug resistance. In addition, the model will be discussed and re-framed within the field of cancer biology to demonstrate its coherence and importance in the metastatic process.
Position of the Problem
This aim of this study is to understand and describe the relationships between spatial diffusion of chemicals in the membrane, the activation energy of their transverse movement across the membrane and, chance of meeting a transporter in an open configuration ready to expel them.
Pgp is an ABC transporter that needs ATP in order to expel drugs. In cells Pgp maximal velocity, measured via ATP conversion to ADP, is, in most of the cases (e.g. excluding cyclosporine A), relatively independent of the drugs themselves [21]. Given that the cytosolic concentration of ATP (3–5 mM) always exceeds the affinity of Pgp for ATP (K mATP ~ 0.3–1 mM) [6, 15], the drug transporter is very likely oscillating between two conformations: one accepting drugs (open) and the other one expelling drugs (closed). Therefore, one can legitimately suggest that the probability that a drug meets a Pgp in an open configuration is 1/2 due to the absence of correlation between the position of drugs and Pgp activity (Fig. 1a).
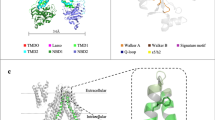
a One shall assume that drug transporters oscillate between open and closed states independently of drugs and that, only when a drug (plain circle) meets a transporter in the inner leaflet whilst the later is in the open configuration is the drug expelled by the transporter. b Representation of profiles of different energies involved when drugs cross the bilayer membrane. We shall take Kramer’s standpoint with only leading orders being involved [5]. The first term (left) of energy considered is the dehydration energy, noted: G. The second energy (centre) is mechanical and involves the difference in surface tensions between leaflets (\( \Updelta \sigma \)), noted: \( - \Updelta \sigma a \). In the previous relations, “a” is the cross-sectional area of drugs in the membrane. Finally, the last term of energy (right) is electrical and involves the interaction between the drug charge (Q) and the membrane potential (\( \Updelta V \)), noted: \( Q\Updelta V \). The latter interaction is modelled as a capacitor. Altogether these energies set up the pace at which drugs can cross the membrane. The sum of all these energies (\( E = G - a\Updelta \sigma + Q\Updelta V \)) shall be called activation energy and will be noted “E”. Finally and as demonstrated elsewhere using Boltzmann’s description of accessible states [31], the probability that a drug is in the inner leaflet is \( \exp ( - G/k_{\text{B}} T) \) where \( k_{\text{B}} \) and T are the Boltzmann’s constant and the absolute temperature, respectively. This means that once a drug has met a Pgp, the probability that the drug is expelled is \( \chi = e^{{ - G/k_{\text{B}} T}} /2 \). The factor 1/2 is for the fact that the transporter has to be in an open configuration. c Schematic representation of Polya’s theorem. This is certainly not a proof of Polya’s theorem but a good exercise to visualize how the spatial dimensions generate interesting properties regarding Brownian diffusion. Thus, this is a hand waiving explanation of Polya’s theorem. Let’s consider a Brownian diffusion in a space which dimension is “d”. After a sufficiently long time, the Brownian particle would have diffused within a volume \( V\sim R^{d} \). The volume of diffusion is necessarily related to time, and as far as Brownian diffusion are concerned, the radius of the volume of diffusion is expressed as \( R\sim t^{1/2} \). Thus, the volume is related to time by the following relation: \( V\sim t^{d/2} \). As seen in the figure, as time goes on the particle will visit more and more dots composing the volume. By dots one means the number of particles that can be inserted in the defined volume. In actual fact the number of dots (N) visited in the volume of diffusion is proportional to time: \( N\sim t \). Consequently, the density of dots visited in the volume of diffusion is: \( N/V\sim t^{1 - d/2} \). As a result, when d > 2 the “density of visitation” decreases with time, which means that many sites will be left unvisited. Conversely when d ≤ 2 it can be proven that the density of visitation is always one, which means that all the sites will be visited at least one time even so if, for this to happen, we have to wait long enough. All this formalism is further developed in [35]. d Representation of drug–transporter and drug–drug–transporter interactions. In the former case, the probability that a drug meets a transporter on its path is linked to the surface density of transporters and to the activation energy (seen in b above). When many drugs are present, competition over transporters can occur in which case, a drug (dark trace) can encounter a transporter that is extruding another drug (light trace). The dashed line in the figure represents what the path would have been without meeting a transporter
Upon incorporation into the membrane, drugs must diffuse in the membrane to interact with Pgp-like transporters. The diffusion time, or in other words residency time in the membrane, is related to the physical interaction between the drug and the membrane. One shall note “E” the activation energy needed to cross the membrane (Fig. 1b).
Whilst remaining in the membrane drugs diffuse. Diffusion properties are dependent on the number of spatial dimensions [28]. More precisely, diffusions taking place in 2D (or 1D) are necessarily recurring and will visit the whole space. In this context, there is a connection expected between the type of spatial diffusion (involving a dimensional aspect), the activation energy, and the chance of meeting a transporter in an open state (Fig. 1c). When the system involves one drug at low surface concentration, the problem can be solved relatively easily [31]. Problems arise, however, when the surface concentration of drug(s) increases or when they have long residency time in the membrane. In both cases, there will be competition between drugs over transporters that will be function of the pumping kinetics and ability of drugs to diffuse. Said differently, the probability that a drug meets a transporter involved in expelling another drug can be important. In the clinic, drug resistance modulators are used in conjunction with drugs to re-sensitize drug resistant tumour cells and reverse the effect of transporters. In this context it may well be that modulators need to have properties that will facilitate their interaction with transporters.
Table 1 lists the notations that will be used and give their definition.
Drugs Meeting Transporters: A Toy Model
Three time scales can be determined: (a) the transverse diffusion time across the membrane of thickness h, i.e. \( \sim h^{2} /D \) (the diffusion coefficient, D, shall be considered constant across the membrane); (b) the residency time of drugs in the membrane, T; and (c) the pumping kinetic, τ. (b) and (c) can be scaled by the transverse diffusion time. In which case, \( N^{*} = DT/h^{2} \), is the number of steps performed laterally by the drug in the membrane and, \( \delta n = D\tau /h^{2} \), is the equivalent number of lateral steps required to expel drugs. The overall problem can be reduced to a straightforward probability calculation if, instead of the number of lateral steps performed by the drug in the membrane, we focus solely on the non-recurring lateral steps. For \( N^{*} \) large enough the number of non-recurring steps, N, in 2D can be expressed as: \( N \cong \pi N^{*} /\ln \left( {N^{*} } \right) \) [35]. Let us note \( \rho = N_{\text{pgp}} S_{\text{pgp}} /S_{\text{cell}} \) the surface density of transporters where: \( N_{\text{pgp}} \), is the number of transporters; \( S_{\text{pgp}} \) the cross-section area of Pgp in the membrane (supposed constant) and; \( S_{\text{cell}} \) the cell surface area, respectively. One shall assume that each time a drug meets a transporter, its residency time in the membrane is reset to zero. In this context, given a random walk made of N non-recurring steps in total, there are “N” possibilities of placing a transporter on the random walk considered, “N − 1” other possibilities of placing a second transporter on the same random walk, and so on… Given that drug transporters have a similar effect on resetting the residency time of drugs in the membrane, the product of possibilities has to be divided by the number of possible permutations. Therefore, the probability that a drug meet “i” transporters on its N-step path is:
Let us note, χ: the probability that a drug is effectively expelled when it meets a transporter (Fig. 1a, d). Using basic cumulative probability rules, it follows that the probability that a drug meets “i” transporters on its N-step path and is expelled “k” times (k ≤ i) as a result is:
If we want to determine the probability of a drug being expelled, whatever the number of times the drug is expelled on its N-step path, summations over “k” in first and “i” in second must be performed. This leads to the following convolution product:
Using the binomial identity, Eq. 3 can be rewritten as:
Equation 4 demonstrates that the probability of not being pumped by a transporter decreases exponentially with the residency time in the membrane. Finally, using Eq. 3, it is possible to determine the average number of pumping, \( \left\langle n \right\rangle \), a drug will have to suffer during its journey in the membrane:
If we assume a high surface density of Pgp and low concentration of drugs in the membrane, so that the probability that two drugs meet the same Pgp over a time interval equivalent to the pumping time is negligible; the amount of drugs, N m, remaining in the membrane as a function of time can be written as:
In Eq. 6 the time has been normalized by the residency time of drugs in the membrane. Equation 6 demonstrates that the amount of drugs, N m, remaining in the membrane decreases exponentially (\( N_{\text{m}} \sim e^{ - t} \)). However, Eq. 6 is equivalent to the instance where the pumping time is supposed to be instantaneous. This is too simplistic a description needs to take into consideration the pumping kinetic.
Competition Between Identical Drugs Over Transporters
Once a drug meets a transporter, only immediate pumping and extrusion have been implicitly considered so far. However, drug extrusion via transporters is not instantaneous. Therefore, two drugs may meet the same transporter within a time interval corresponding to the pumping kinetic. This means, therefore, that a drug may meet a transporter without being expelled simply because the transporter is occupied with handling another drug. As a result Pgp-mediated drug resistance is expected to be re-sensitive to drugs in two conditions: (i) once a threshold concentration of drugs in the membrane has been attained and/or (ii), when the drug residency time in membrane is beyond a critical value to be determined. As a result, Eq. 6 has to be amended to take these facts into consideration.
The probability that two drugs meet the same transporter whatever the time considered is thus: \( \left( {p_{N} /N_{\text{Pgp}} } \right)^{2} \). Assuming that drug handling by a transporter takes a time equivalent to \( \delta n \) steps in total, competition between drugs will occur only if two drugs meet the same transporter within the time interval \( \delta n \). The probability attached to this event, \( \Omega_{N,\delta n} \), can be determined analytically.
Let us consider two drugs (denoted by “Drug 1” and “Drug 2” in Fig. 2) diffusing in a membrane over a time equivalent to N steps. We assume that these two drugs will meet the same Pgp (blue circle in Fig. 2) with a probability, \( \left( {p_{N} /N_{\text{Pgp}} } \right)^{2} \), and we want to determine whether this double hit will occur within a time interval \( \delta n \). Assuming that “Drug 1” has met Pgp in first after n 1 steps. This means that it remains N –n 1 possibilities for “Drug 2” to meet Pgp after “Drug 1”. As there is a total of N possibilities for “Drug 2” to meet Pgp, the probability that “Drug 2” meets Pgp after taking n 1 steps is: \( \left( {N - n_{1} } \right)/N \). Similarly, the probability that “Drug 2” meets Pgp before taking a total of n 2 steps is: \( n_{2} /N \). It follows that the probability that “Drug 2” meets Pgp after taking n 1 steps but before taking a total of n 2 steps is: \( \left( {N - n_{1} } \right)/N \times n_{2} /N \), with \( n_{2} - n_{1} = j \le \delta n \). Thus, the previous probability has to be summed over \( j = 0, \ldots ,\delta n \) and gives: \( \sum\limits_{j = 0}^{\delta n} {\left( {N - n_{1} } \right)/N \times \left( {n_{1} + j} \right)/N} \).
As there are N possibilities for “Drug 1” to meet Pgp first, summation over n 1 needs to be performed. However, there are boundary conditions to consider as the summation over \( j = 0, \ldots ,\delta n \) works only if \( n_{1} \le N - \delta n \). Indeed let us assume that “Drug 1” meets Pgp after \( N - \left( {\delta n - l} \right) \) where \( l = 1, \ldots ,\delta n \). In this case, the summation j transforms to \( j = 0, \ldots ,\delta n - l \). Noting \( \Omega_{N,\delta n} \) the probability that “Drug 1” and “Drug 2” meet the same given Pgp, \( \Omega_{N,\delta n} \) is formally written as:
It is important to note that if \( \delta n \) is small compared to N, then the second term in the rhs of Eq. 7 can be omitted and we shall make this assumption. Furthermore, noting \( \varepsilon = \delta n/N \), using continuous integration \( \Omega_{N,\delta n} \) transforms to \( \Omega_{N,\delta n} \sim \int\limits_{0}^{1 - \varepsilon } {{\text{d}}x} \int\limits_{0}^{\varepsilon } {{\text{d}}y} \left( {1 - x} \right)\left( {x + y} \right) \). Where \( x = n_{1} /N \) and \( y = j/N \). Note that the leading order terms resulting from the continuous integration are: \( \Omega_{N,\delta n} \sim \left( {\delta n/N} \right)/6 - \left( {\delta n/N} \right)^{2} /4 \).
Assuming \( N > \delta n \) and using the leading order of \( \Omega_{N,\delta n} \) in \( \delta n/N \), the competition between two drugs over one single transporter can then be approached by:
Note that Eq. 8 is maximal for Nχρ ~ 1.2–1.3 (Fig. 3). The decrease that follows the maximal value is related to the fact that, two drugs meeting one given transporter over a time interval equivalent to \( \delta n \) steps in total is smaller as the residency time in the membrane increases. This is because there are more possibilities for two paths to cross one another without meeting the same transporter. If one considers that there are N m drugs in the membrane at any time, once one chosen drug is being potentially handled by a given Pgp, it remains \( N_{\text{m}}^{{}} - 1 \) other potential drugs to interfere with the drug that is being handled. Given that there are \( N_{\text{Pgp}} \) transporters in the membrane, the amount of drugs remaining in the membrane as a function of time becomes:
a Representation of the interaction between drugs as a function of non-recurring steps number, surface density of transporter and probability for a drug to be in the inner leaflet. Note that there is a maximal value for this interaction. b Plot of Eq. 10. The curve delineates two areas. In the area below the curve competition between drugs over transporters is not expected to occur. However, in the area above the curve, competition is expected to occur. As demonstrated by arrows I and II, there are two ways to move from the area below the curve to the one above it. The first way is to increase drug number and the second is to engineer drugs so that they stay for longer period of times in the membrane
In Eq. 9, the factor 1/2 is added to avoid counting twice pair-wise interactions between drugs and transporters. Equation 9 is a mean field approximation of the existing competition between drugs over transporters. Note that as the last rhs term brings a negative function, the competition between drugs over transporters is expected to trigger inward leak of drugs from the membrane into the cytosol. Indeed, let us assume that \( p_{N} = 1 \) (drugs meet transporters), for N m sufficiently large (i.e. \( N_{\text{m}} - 1\,\sim \,N_{\text{m}} \)) Eq. 9 transforms to: \( \partial_{t/T} N_{\text{m}} \sim - N_{\text{m}}^{2} \Omega_{N,\delta n} /2N_{\text{Pgp}} \) (with a solution as: \( N_{\text{m}} \,\sim \,1/t \)). Thus, it is not because drugs meet transporters with certainty that drugs will necessarily be expelled, on the contrary, this should sensitize cells.
To further comment on this point, a parameter, Λ, weighing the effect of single drug pumping (first term in the rhs of Eq. 9) against the competition between drugs over transporters (second term in the rhs of Eq. 9) can be obtained by dividing these two terms:
Naturally, from Eq. 10 it follows that if \( \Lambda > 1 \), the regime of competition between drugs over transporters dominates the system, whereas if \( \Lambda < 1 \), it is the regime defined by the “single pumping” that is predominant. Figure 3b summarizes these conclusions. Two arrows (I or II—see Fig. 3b) can then be defined suggesting that sensitization occurs when more drugs are added to cells (arrow I) and/or, the residency time of drugs in the membrane is increased (arrow II). The later result, in appearance counter-intuitive, can highlight why the lipophilic property of drugs seems so central to their cytotoxicity to MDR cells [3, 8, 41].
Last but not least, the later conclusion can also highlight how drug sensitizers (or drug resistance modulators) work to improve sensitivity to drugs without displaying a strong affinity to drug transporters.
Modulation of MDR with Modulators
Modulators are chemical entities that have a tendency to sensitize multi-drug resistant cells to drugs. As far as classic enzymology goes, we would expect the concentration of modulators required to reverse multi-drug resistance to be similar to the concentration of membrane transporters. However, albeit the explanation regarding the effects of modulators on drug resistance is discussed in terms of transporter inhibition, i.e. affinity to transporters, it remains unclear why, in some cases, 10–100 excess of modulators need to be used to reverse multi-drug resistance [22, 23]. For example, verapamil binds to Pgp but must be used at a concentration of ~10 μM to block the transport of chemotherapeutic agents at a concentration of 100 nM to 1 μM [40]. Further adding to a lack of clear understanding regarding the function of Pgp is the observation that the chemical affinity between drugs or modulators and Pgp is primarily dependent on the ability of a drug to partition in the bilayer lipid membrane [8, 10, 16, 26, 27, 37, 39].
The present model emphasizes the ability of chemicals to interact based on their ability to meet up. Accordingly, the model agrees with the fact that if modulators work this may be because they reach Pgp first, thereby placing the transporter into an “occupied” state. As a result, it is statistically more difficult for a “true” drug to encounter any non-occupied Pgp. This will result in more drugs traversing the membrane and hence increasing the cellular chemo-sensitivity. It follows here that, if drugs are outnumbered by modulators and/or modulators stay in the membrane for longer and diffuse more rapidly in the membrane than drugs, possibly linked to their smaller sizes [45], then modulation of multidrug resistance is very likely. This can be modelled.
Let us denote by a tilde all the variables that are connected to modulators. \( \tilde{N}_{\text{m}} \) is the number of modulators in the membrane, \( \tilde{N} \) their time of residency in the membrane (converted in steps number), and \( p_{{\tilde{N}}} \) the probability that modulators meet transporters. The probability that a drug (not a modulator) meets a Pgp is given by Eq. 9 minus the fact that the Pgp may be occupied handling a modulator (not a drug). Accordingly, it follows:
The last rhs term of Eq. 11 corresponds to the competition between drugs and modulators over transporters. More specifically, \( \Omega_{{\tilde{N},N,\delta \tilde{n}}} \)is the probability that a modulator meets a transporter first, followed by a drug meeting the same transporter within a time interval corresponding to the pumping time of modulators (i.e. \( \delta \tilde{n} \)). \( \Omega_{{\tilde{N},N,\delta \tilde{n}}} \) can be determined analytically using the same formalism as for Eq. 7 and it follows:
To determine the effect of modulators on drug resistance, let us now assume that drugs and modulators meet transporters with a probability equal to unity (i.e. \( p_{N} \sim p_{{\tilde{N}}} \sim 1 \)) and that the pumping kinetic of drugs or modulators are similar (i.e. \( \delta n\sim \delta \tilde{n} \)). Using the property, \( \Omega_{{\tilde{N},N,\delta \tilde{n}}} = \Omega_{{\tilde{N},\delta \tilde{n}}} \tilde{N}/N \) (Eq. 12), and considering only the first-order development in \( \delta n/N \); it follows, \( \Omega_{{\tilde{N},N,\delta \tilde{n}}} = \Omega_{{\tilde{N},\delta \tilde{n}}} \tilde{N}/N\sim \Omega_{N,\delta n} \). As a result, Eq. 11 can be rewritten as: \( \partial_{t/T} N_{\text{m}} \,\sim \, - N_{\text{m}}^{2} \Omega_{N,\delta n} \left( {1 + 2\tilde{N}_{\text{m}} /N_{\text{m}} } \right)/2N_{\text{Pgp}} \). Now, if modulators outnumber drugs (\( \tilde{N}_{\text{m}} \gg N_{\text{m}} \)) then Eq. 11 transforms to \( \partial_{t/T} N_{\text{m}} \sim - N_{\text{m}} \). The latter relation shows that modulators can “hide” drug transporters to re-sensitize cells to drugs. However, the latter relation assumes that a modulator will remain in the membrane for a time much longer than the residency time of drugs in the membrane. This point is not totally justified. Indeed, given that the system including drugs and modulators is dynamic, in that modulators do cross the membrane, a similar equation as to Eq. 11 has to apply to modulators. To determine how drugs and modulators are related to one another dynamically, one needs to focus first on the number of modulators remaining in the membrane over a time similar to their residency time in the membrane. We shall note “\( \tilde{T} \)” as this variable. It follows in this case that:
In Eq. 13, \( \Omega_{{N,\tilde{N},\delta n}} \) is the probability that a drug meets a transporter first followed by a modulator meeting the same transporter within a time interval corresponding to the pumping time of drugs (i.e. \( \delta n \)). In this case, it is the drug that is the modulator of “true” modulators. Equations 11 and 13 form a system of non-linear equations which are difficult to solve directly. However, further reasonable hypotheses can be made for these equations to be amenable. The first hypothesis is that drugs and modulators meet transporters with a probability equal to unity (i.e. \( p_{N} \,\sim \,p_{{\tilde{N}}} \,\sim \,1 \)). The second hypothesis is that the power stroke of Pgp is independent of the chemical considered and solely dependent on ATP molecules binding to the transporter [2, 21, 36]. It follows: \( \delta n \cong \delta \tilde{n} \) that, in turn, implies: \( \Omega_{{\tilde{N},N,\delta \tilde{n}}} = \Omega_{{\tilde{N},\delta \tilde{n}}} {\frac{{\tilde{N}}}{N}} \) and \( \Omega_{{N,\tilde{N},\delta n}} = \Omega_{N,\delta n} {\frac{N}{{\tilde{N}}}} \). Assuming that drugs and modulators have similar transmembrane diffusion coefficient—i.e. that they have similar MW—as \( \tilde{T}/T\,\sim \,\tilde{N}/N \) at the first order,Footnote 1 Eqs. 11 and 13 can be rewritten as:
Note that in Eqs. 14a and 14b the time is a dimensionless variable. Finally, Eq. 14b shows that the ratio between the residency times of modulators and drugs (\( N/\tilde{N} \)) in the membrane is the fundamental variable to consider when using modulators. Indeed, as represented in Fig. 4 it is this parameter that sets up the sensitization to drugs. The ability of a modulator to reverse drug resistance has been extensively documented and the interaction between the membrane and the modulator seems central to this [10, 14, 16, 45]. Equations 14a and 14b agree with this assumption and suggests a power law, i.e. \( \left( {N/\tilde{N}} \right)^{2} \), explaining the sensitivity.
Vector field representing the variation of drugs (y axis) and modulators (x axis) as a function of the ratio (\( \tilde{N}/N \)) between the numbers of steps performed by drugs and modulators in the membrane (i.e. the residency time). The initial state is provided by the condition \( N_{\text{m}} = \tilde{N}_{\text{m}} = 1 \) namely equal amount of drug and modulator (upper right corner). Three cases are represented depending on the residency time of the modulator in the membrane: similar (\( \tilde{N}/N = 1 \); left), twice as long (\( \tilde{N}/N = 2 \); centre) or three times longer (\( \tilde{N}/N = 3 \); right) than the residency time of the drug in the membrane. If one imagines a dot staying on the curve and travelling downward from the upper right corner (i.e. following the sense of vector field), then N m decreases more rapidly than \( \tilde{N}_{\text{m}} \) as \( \tilde{N}/N \) increases. This demonstrates that an important property of modulators to consider is their ability of remaining in membrane for longer periods than drugs
Discussion
The “vacuum cleaner” hypothesis and the multi-specificity that exists between chemicals and transporters have always been conceptually problematic in the field of MDR. A solution to the “vacuum cleaner” hypothesis, based on the ability of drugs to diffuse in the membrane, was suggested a few years ago [31]. However, this latter study assumed that upon meeting a transporter, a drug would be expelled because of its interaction with a transporter. Therefore, this assumption implicitly suggested the existence of an affinity between drugs and transporters. Thus, even so the “vacuum cleaner” hypothesis was explained, the multi-specificity was still lingering.
This article corrects and prolongs the previous theory making full use of results known in the field of random walks. For a comprehensive review on this point see [28]. The main conclusion is that the multi-specificity is not necessarily a problem in the field of MDR, if the drug transporters oscillate between open and closed states. In this case, what is significant is the ability of chemicals to meet a transporter.
Naturally, if one wants oscillating transporters, one suggests that MDR induced by Pgp will rely on ATP synthesis and consumption. This seems to be the case as:
-
(a)
The ATP concentration in cells (3–5 mM) always exceeds the affinity of Pgp for ATP (K mATP ~ 0.3–1 mM) [6, 15], that, in turn, suggests that the transporter is always “active”.
-
(b)
Pgp ATPase activity is relatively independent of the presence of drugs [36], and the affinity of drugs towards transporters is chiefly dependent on their affinity towards the membrane [7].
-
(c)
The apparent stoichiometry of the hypothesized ATP-coupled active drug transport, i.e. the number of ATP molecules hydrolysed per drug transported, can be enormous (calculated to be up to ~36,000 ATP/drug in reconstituted proteo-liposomes) [6, 33]. This suggests that whilst consuming ATP, Pgp does not necessarily lead to drug extrusion.
Altogether, these data strongly suggest that Pgp is very likely continuously recycling between “open” and “closed” states by over-consuming ATP. This may explain why Pgp is so sensitive to the cellular metabolism [12]. It is interesting to note that Pgp activity leads to a parallel acidification of the extracellular medium [20] that, in turn, is thought to be related to initial metastatic steps [42]. Given that the vast majority of metastatic tumours are also MDR in nature [25], the recycling between open and closed conformations, so important for the multi of drug resistance, is likely to be paramount also for the metastatic process. Thus, in the future, it will be central to drug-target the membrane of MDR cancer cells, as it is the membrane that makes the application of Polya’s theorem (i.e. dimensionality) possible in these cells, see [28].
Defining Pseudo Affinity and Velocity Constants
In general, when the transport of drugs by Pgp is studied in the field of enzymology, the notion of affinity is traditionally called upon to explain experimental observations. In our model, even so we show that the drug–Pgp interaction is possible; the chemical affinity between drug and transporter is never mentioned. This raises the question as to whether we can define an affinity-like constant between drugs and transporters?
It is possible (see supplementary material) to rewrite the set of equations suggested in this article to lead to Michaelis–Menten-like equations, whereby defining pseudo velocity and affinity constants. However, contrary to the “true” ones that are chiefly independent to one another, the “pseudo” ones (as the pseudo maximal velocity and the pseudo affinity) are related to one another. Of course the model does not rule out the notion of affinity in the field of MDR, it simply suggests possible alternatives. Again, as seen, this way of envisaging Pgp-mediated MDR leads to results that are coherent with data from this field including: (i) a drug pumping chiefly independent of drug chirality [24]; (ii) a modulation of MDR based on drugs [11, 19] or modulators [45] lipophilicity; and (iii) a mechanism of drug resistance fundamentally sensitive to drug physico-chemical properties [11, 19, 29, 32, 38, 45].
Although our deductions agree in principle with results obtained in the field of MDR, it is important to recognize that more needs to be done experimentally to ascertain the full validation of the theory.
On the Importance of Considering Systems Dimensionality in Basic Biology
In good faith with basic biochemistry that discards the concept of multi-specificity, alternative hypotheses about MDR have been developed more or less successfully to explain the “multi” of MDR, see for example [31, 34]. It seems, however, that all the models cannot exclude active drug pumping (developed in introduction). As underlined by Paul Roepe, the problem that has given rise to this controversy relies in the notion of specificity and affinity. MDR does not conform to the Law of enzyme specificity that, in turn, is supposed to promote a type of order in biological systems. The model we suggest is an alternative to this controversy.
The use of Hill–Langmuir or Michaelis–Menten equations to determine the experimental affinity between two substrates is fully justified ex vivo, i.e. in a beaker. Their applications using true biological systems can be limited. One reason for this is that these Laws take for granted the bulk homogenous isotropic diffusion (as in our beaker) for substrates to collide and react in biological systems. However, this extrapolation is likely to be of limited use in heterogeneous biological complex systems. In particular, one could easily imagine that two substrates with low affinity to each other [to react] will always react successfully, because the space in which these two substrates diffuse allows them to repeatedly collide. Thus, in theory, many “hits” can compensate for low affinities between chemicals. This means that the notion of chemical affinity has to include also the notion of physical affinity, which involves a study of the surrounding space (including dimensionality) where diffusions take place. Seen this way, all the objections made on the “multi” of drug resistance and essentially based on biochemical rules are not entirely justified. The model exposed in this article suggests how two compounds without significant affinity towards one another, e.g. a drug and a transporter, can nonetheless react very efficiently, hence defining “multi”-drug resistance.
Conclusion
In this study I have demonstrated that MDR can be explained using basic physical notions. This has the potential to solve long-standing paradoxes in this field and to redefine parameters involved in drug resistance. Thus, this study suggests that MDR may be the result of both drug pumping and physical affinity.
Notes
As explained in the paragraph “drug meeting transporters: a toy model”: \( N\,\sim \,\left( {DT/h^{2} } \right)/\ln \left( {DT/h^{2} } \right) \), which implies that \( \tilde{N}/N\,\sim \,\left( {\tilde{T}/T} \right) \times \left[ {\ln \left( {D\tilde{T}/h^{2} } \right)/\ln \left( {DT/h^{2} } \right)} \right] \). The first-order development of the latter relation provides the result expected.
References
Aanismaa, P., & Seelig, A. (2007). P-Glycoprotein kinetics measured in plasma membrane vesicles and living cells. Biochemistry, 46, 3394–3404.
Aller, S. G., Yu, J., Ward, A., Weng, Y., Chittaboina, S., Zhuo, R., et al. (2009). Structure of P-glycoprotein reveals a molecular basis for poly-specific drug binding. Science, 323, 1718–1722.
Bennis, S., Faure, P., Chapey, C., Hu, Y. P., Fourche, J., El Yamani, J., et al. (1997). Cellular pharmacology of lipophilic anthracyclines in human tumor cells in culture selected for resistance to doxorubicin. Anticancer Drugs, 8, 610–617.
Dano, K. (1973). Active outward transport of daunomycin in resistant Ehrlich ascites tumor cells. Biochimica et Biophysica Acta, 323, 466–483.
Daune, M. (1993). Biophysique moleculaire. Paris: InterEditions.
Doige, C. A., Yu, X., & Sharom, F. J. (1993). The effects of lipids and detergents on ATPase-active P-glycoprotein. Biochimica et Biophysica Acta, 1146, 65–72.
Eytan, G. D. (2005). Mechanism of multidrug resistance in relation to passive membrane permeation. Biomedicine and Pharmacotherapy, 59, 90–97.
Facchetti, I., Grandi, M., Cucchi, P., Geroni, C., Penco, S., & Vigevani, A. (1991). Influence of lipophilicity on cytotoxicity of anthracyclines in LoVo and LoVo/Dx human cell lines. Anticancer Drug Des, 6, 385–397.
Ferte, J. (2000). Analysis of the tangled relationships between P-glycoprotein-mediated multidrug resistance and the lipid phase of the cell membrane. European Journal of Biochemistry, 267, 277–294.
Friche, E., Jensen, P. B., Roed, H., Skovsgaard, T., & Nissen, N. I. (1990). In vitro circumvention of anthracycline–resistance in Ehrlich ascites tumour by anthracycline analogues. Biochemical Pharmacology, 39, 1721–1726.
Friche, E., Demant, E. J., Sehested, M., & Nissen, N. I. (1993). Effect of anthracycline analogs on photolabelling of p-glycoprotein by [125I]iodomycin and [3H]azidopine: Relation to lipophilicity and inhibition of daunorubicin transport in multidrug resistant cells. British Journal of Cancer, 67, 226–231.
Gatlik-Landwojtowicz, E., Aanismaa, P., & Seelig, A. (2004). The rate of P-glycoprotein activation depends on the metabolic state of the cell. Biochemistry, 43, 14840–14851.
Gatlik-Landwojtowicz, E., Aanismaa, P., & Seelig, A. (2006). Quantification and characterization of P-glycoprotein–substrate interactions. Biochemistry, 45, 3020–3032.
Gosland, M. P., Lum, B. L., & Sikic, B. I. (1989). Reversal by cefoperazone of resistance to etoposide, doxorubicin, and vinblastine in multidrug resistant human sarcoma cells. Cancer Research, 49, 6901–6905.
Gottesman, M. M., Ambudkar, S. V., & Xia, D. (2009). Structure of a multidrug transporter. Nature Biotechnology, 27, 546–547.
Hofsli, E., & Nissen-Meyer, J. (1990). Reversal of multidrug resistance by lipophilic drugs. Cancer Research, 50, 3997–4002.
Juliano, R. L., & Ling, V. (1976). A surface glycoprotein modulating drug permeability in Chinese hamster ovary cell mutants. Biochimica et Biophysica Acta, 455, 152–162.
Kaplan, O., Jaroszewski, J. W., Clarke, R., Fairchild, C. R., Schoenlein, P., Goldenberg, S., et al. (1991). The multidrug resistance phenotype: 31P nuclear magnetic resonance characterization and 2-deoxyglucose toxicity. Cancer Research, 51, 1638–1644.
Lampidis, T. J., Kolonias, D., Podona, T., Israel, M., Safa, A. R., Lothstein, L., et al. (1997). Circumvention of P-GP MDR as a function of anthracycline lipophilicity and charge. Biochemistry, 36, 2679–2685.
Landwojtowicz, E., Nervi, P., & Seelig, A. (2002). Real-time monitoring of P-glycoprotein activation in living cells. Biochemistry, 41, 8050–8057.
Litman, T., Nielsen, D., Skovsgaard, T., Zeuthen, T., & Stein, W. D. (1997). ATPase activity of P-glycoprotein related to emergence of drug resistance in Ehrlich ascites tumor cell lines. Biochimica et Biophysica Acta, 1361, 147–158.
Litman, T., Zeuthen, T., Skovsgaard, T., & Stein, W. D. (1997). Competitive, non-competitive and cooperative interactions between substrates of P-glycoprotein as measured by its ATPase activity. Biochimica et Biophysica Acta, 1361, 169–176.
Litman, T., Zeuthen, T., Skovsgaard, T., & Stein, W. D. (1997). Structure–activity relationships of P-glycoprotein interacting drugs: Kinetic characterization of their effects on ATPase activity. Biochimica et Biophysica Acta, 1361, 159–168.
Loetchutinat, C., Heywang, C., Priebe, W., & Garnier-Suillerot, A. (2001). The absence of stereoselective P-glycoprotein- and multidrug resistance-associated protein-mediated transport of daunorubicin. Biochemical Pharmacology, 62, 561–567.
Longley, D. B., & Johnston, P. G. (2005). Molecular mechanisms of drug resistance. Journal of Pathology, 205, 275–292.
Mankhetkorn, S., & Garnier-Suillerot, A. (1998). The ability of verapamil to restore intracellular accumulation of anthracyclines in multidrug resistant cells depends on the kinetics of their uptake. European Journal of Pharmacology, 343, 313–321.
Mankhetkorn, S., Dubru, F., Hesschenbrouck, J., Fiallo, M., & Garnier-Suillerot, A. (1996). Relation among the resistance factor, kinetics of uptake, and kinetics of the P-glycoprotein-mediated efflux of doxorubicin, daunorubicin, 8-(S)-fluoroidarubicin, and idarubicin in multidrug-resistant K562 cells. Molecular Pharmacology, 49, 532–539.
Panagiotopoulou, V., Richardson, G., Jensen, O. E., & Rauch, C. (2010). On a biophysical and mathematical model of Pgp-mediated multidrug resistance: Understanding the “space-time” dimension of MDR. European Biophysics Journal with Biophysics Letters, 39, 201–211.
Rauch, C. (2009). On the relationship between drug’s size, cell membrane mechanical properties and high levels of multi drug resistance: A comparison to published data. European Biophysics Journal, 38, 537–546.
Rauch, C. (2009). Toward a mechanical control of drug delivery. On the relationship between Lipinski’s 2nd rule and cytosolic pH changes in doxorubicin resistance levels in cancer cells: A comparison to published data. European Biophysics Journal, 38, 829–846.
Rauch, C., & Pluen, A. (2007). Multidrug resistance-dependent “vacuum cleaner” functionality potentially driven by the interactions between endocytosis, drug size and Pgp-like transporters surface density. European Biophysics Journal, 36, 121–131.
Roepe, P. D. (1992). Analysis of the steady-state and initial rate of doxorubicin efflux from a series of multidrug-resistant cells expressing different levels of P-glycoprotein. Biochemistry, 31, 12555–12564.
Roepe, P. D. (2000). What is the precise role of human MDR 1 protein in chemotherapeutic drug resistance? Current Pharmaceutical Design, 6, 241–260.
Roepe, P. D. (2001). pH and multidrug resistance. Novartis Foundation Symposium, 240, 232–47; discussion 247–250, 265–268.
Rudnick, J., & Gaspari, G. (2004). Elements of random walk, 2004 edn. Cambridge, MA: Cambridge University Press.
Sauna, Z. E., & Ambudkar, S. V. (2007). About a switch: how P-glycoprotein (ABCB1) harnesses the energy of ATP binding and hydrolysis to do mechanical work. Molecular Cancer Therapeutics, 6, 13–23.
Schott, B., & Robert, J. (1989). Comparative activity of anthracycline 13-dihydrometabolites against rat glioblastoma cells in culture. Biochemical Pharmacology, 38, 4069–4074.
Seelig, A. (2007). The role of size and charge for blood–brain barrier permeation of drugs and fatty acids. Journal of Molecular Neuroscience, 33, 32–41.
Seelig, A., & Landwojtowicz, E. (2000). Structure–activity relationship of P-glycoprotein substrates and modifiers. The European Journal of Pharmaceutical Sciences, 12, 31–40.
Simon, S. M., & Schindler, M. (1994). Cell biological mechanisms of multidrug resistance in tumors. Proceedings of the National Academy of Sciences of USA, 91, 3497–3504.
Skovsgaard, T. (1980). Circumvention of resistance to daunorubicin by N-acetyldaunorubicin in Ehrlich ascites tumor. Cancer Research, 40, 1077–1083.
Stock, C., Cardone, R. A., Busco, G., Krahling, H., Schwab, A., & Reshkin, S. J. (2008). Protons extruded by NHE1: Digestive or glue? European Journal of Cell Biology, 87, 591–599.
Wadkins, R. M., & Roepe, P. D. (1997). Biophysical aspects of P-glycoprotein-mediated multidrug resistance. International Review of Cytology, 171, 121–165.
Yin, L., Castagnino, P., & Assoian, R. K. (2008). ABCG2 expression and side population abundance regulated by a transforming growth factor beta-directed epithelial-mesenchymal transition. Cancer Research, 68, 800–807.
Zamora, J. M., Pearce, H. L., & Beck, W. T. (1988). Physical-chemical properties shared by compounds that modulate multidrug resistance in human leukemic cells. Molecular Pharmacology, 33, 454–462.
Acknowledgments
This study has been supported by the University of Nottingham (NRF4305).
Author information
Authors and Affiliations
Corresponding author
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Rauch, C. The “Multi” of Drug Resistance Explained by Oscillating Drug Transporters, Drug–Membrane Physical Interactions and Spatial Dimensionality. Cell Biochem Biophys 61, 103–113 (2011). https://doi.org/10.1007/s12013-011-9166-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-011-9166-8