Abstract
Diabetic pregnancy frequently results in macrosomia or fetal obesity. It seems that the anomalies in carbohydrate and lipid metabolism in macrosomic infants of diabetic mothers are due to maternal hyperglycemia, which leads to fetal hyperinsulinemia. We have developed a rat model of macrosomic offspring and assessed the onset of obesity in these animals. The macrosomic offspring born to diabetic mothers are prone to the development of glucose intolerance and obesity as a function of age. It seems that in utero programing during diabetic pregnancy creates a “metabolic memory” which is responsible for the development of obesity in macrosomic offspring. We have demonstrated that the metabolism of lipids, and altered anti-oxidant status and immune system are implicated in the etiopathology of obesity in these animals. We have reported beneficial effects of n-3 polyunsaturated fatty acids (PUFAs) in obese animals, born to diabetic dams.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Macrosomia has been defined as a birth weight greater than or equal to the 90th percentile birth weight for gestational age or infants who weigh >4,000 g at delivery, irrespective of gestational age or sex [1–4]. Macrosomic newborns incur a number of prenatal complications such as fetal distress, shoulder dystocia, and high incidence of caesarean delivery [2]. During the neonatal period, macrosomic infants are at increased risk for hypoglycemia, infant respiratory distress syndrome, hyperbilirubinemia, and hypertrophic cardiomyopathy [2]. Increased risks of maternal obstetrical complications and longer labor periods especially in primigravid women have been reported in mothers of macrosomic babies [5]. Consequently, fetal macrosomia is a risk factor for fetal injury and maternal morbidity in type I, type II, and gestational diabetic pregnancies [1, 4, 6–9].
The growth and development of the fetus depend not only upon nutrients, but also upon genetic makeup and feto-maternal endocrine status [10, 11]. Several alterations in the metabolism of carbohydrate and lipid, observed in infants of diabetic mothers at birth, also persist postnatally [12–20]. Here-below, we will try to shed light on the implication of in utero programing and some patho-physiological abnormalities in macrosomia.
In utero “metabolic memory” during diabetic pregnancy seems implicated in macrosomia
In 1995, David Barker [21] wrote: “The foetal origins hypothesis states that fetal undernutrition in middle to late gestation, which leads to disproportionate foetal growth, programes later coronay heart disease”. The process, whereby a stimulus or insult at a sensitive or critical period of development has long-term effects, is termed programing.
In fact, this in utero programing seems to create some kind of “metabolic memory” since the anomalies in the physiological system during gestational period are responsible, at adulthood, for the “onset” of the diseases like type II diabetes and obesity, associated to metabolic syndrome. Maternal hypercholesterolaemia during pregnancy is associated with greatly increased fatty streak formation in human fetal arteries and accelerated progression of atherosclerosis during childhood [22]. A good correlation exists between maternal and fetal plasma cholesterol levels in 5 to 6-month-old human fetuses [23, 24]. We would like to recall that some of the alterations such as increased triacylglycerol (TAG), apoB100, very low-density lipoprotein (VLDL), and low-density lipoprotein (LDL) levels in macrosomic newborns persist even after 1 month of life [13]. We have reported (see the next paragraph) that, in the macrosomic rats born to diabetic dams, most of the lipid parameters are normalized by the age of 2 months and later on, after 3 months, these offspring again develop these lipid anomalies. These observations suggest that there is some kind of in uetro “metabolic memory” which is dormant, to some extent, during childhood and may cause, in adulthood, an increase in glucose, insulin, and lipid levels in these animals [25]. Desai et al. [26] have demonstrated that adult glucose and lipid metabolism may be programed during fetal life. Insulin resistance, which we have noticed in our macrosomic adult rats, may be a programed response to fetal undernutrition as suggested elsewhere [27].
The in uetro metabolic modifications, responsible for the appearance of these physiological anomalies in adulthood, remain to be searched for. However, fetal hyperinsulinemia may, possibly, be an endogenous teratogen during critical periods of development, leading to permanent structural or functional organ changes and consequent programing of the “metabolic memory” [28]. It has been shown that maternal hyperglycemia leads to fetal hyperglycemia which stimulates pancreatic islet cells and, consequently, produces fetal hyperinsulinemia [17]. Maternal glucose levels and fetal macrosomia have been positive correlated [18, 19]. The fetal hyperinsulinemic state results in increased fat tissue, liver glycogen contents, and total body size [20]. Insulin receptors may also play a role in the increased insulin effects in infants. Several authors [16, 29] have provided evidence for the defective down-regulation of insulin receptors in hyperinsulinemic fetus, which may have increased insulin binding sites and, thus, its metabolic effects. The insulin concentrations in utero may also affect the induction and activity of various hepatic enzymes associated with fat and carbohydrate metabolism [20]. The role of sterol-regulatory-element-binding protein-1c (SREBP-1c) in the regulation of hepatic metabolism is now well established [30]. Indeed, insulin stimulates the synthesis of SREBP-1c [31]. SREBP-1c is a transcription factor that induces expression of genes involved in lipogenesis, especially fatty acid and TAG synthesis [32]. It has been shown [33] that this factor is active in fetal tissues and participates in the regulation of lipogenic genes during proliferation. Hence, it is possible that SREBP-1c levels are increased in macrosomic fetuses; however, the correlation between high expression of SREBP-1c and high lipid metabolism in macrosomic newborns remains to be established experimentally [13].
Experiments in animals have implicated the fetal hypothalamus as a key site that can be “programed” by transient changes in prenatal endocrine status [12]. Hence, we can cite a plausible study of Yura et al. [34] who have shown that in uetro undernutrition is closely associated with obesity related to detrimental metabolic sequelae in adulthood. They have demonstrated that the premature leptin surge in undernourished mice alters energy regulation by the hypothalamus and contributes to “developmental origins of obesity.” However, the implication of other factors in the in utero modifications remains to be investigated in future.
Lipid and lipoprotein metabolism is altered in newborn and adult macrosomic offspring
Most of the lipid abnormalities observed in macrosomic newborns are parallel with those found in their diabetic mothers [1]. Several investigators [13, 35, 36] have shown that, in macrosomic newborns of diabetic mothers, serum lipid, lipoprotein, and apo concentrations are higher than in normal newborns of healthy mothers [20, 37].
Macrosomic newborns possess high LDL levels as a result of high concentrations of VLDL, as most LDL particles are derived from VLDL by the action of lipoprotein lipase (LPL) [1, 13, 35]. High activities of LPL and hepatic TAG lipase (HTGL) have also been reported in infants of diabetic mothers [38, 39]. Macrosomic newborns possess high levels of high-density lipoprotein (HDL), which are accompanied by high HDL apoA-I and apoA-II concentrations, suggesting an increase in the number of HDL particles, probably as a result of their enhanced synthesis [13, 35]. These modifications in lipid metabolism of macrosomic infants can be seen in a recent review article [25].
In order to understand the role of lipid metabolism in the etiopathology of macrosomia, we have developed an animal model of macrosomia in our laboratory. The pregnant rat is a good experimental animal because it shows a rise in VLDL-TAG during pregnancy similar to that seen in humans [40]. Administration of streptozotocin (STZ) on day 5 of gestation exerts no effect on embryo development and, thus, avoids its lethal effects on the fetal pancreaticβ-cells [41, 42]. We have used this animal model to explore the association between birth weight and the predisposition of macrosomic pups of diabetic dams to the onset of adult obesity [14, 43–45]. Hence, we have noticed that at birth, macrosomic obese pups had higher serum glucose, insulin, saturated fatty acids, and lipoprotein (VLDL, LDL-HDL1, HDL2–3) levels, associated with increased serum lecithin cholesterol acyltransferase (LCAT) activity, than control pups. Most of these lipid anomalies become normal during first and second month of life of macrosomic rats.
Hereafter, we will describe the modifications which are apparent at 3 months of age, i.e., adulthood, of macrosomic animals in order to strengthen the notion that the fetal “metabolic memory” does have the consequences on the later life. First important observation is that these macrosomic rats gain weight progressively, as a function of age, till adulthood. Their weight gain is significantly higher than that in control rats [14, 43–45]. Besides, these adult macrosomic rats are hyperglycemic and hyperinsulinemic, with high lipid and lipoprotein concentrations. These obese rats also display significant increases in liver lipids, LCAT, LPL, HTGL, acyl Co-A cholesterol acyl transferase (ACAT), 3-hydroxy-3-methylglutaryl-CoA (HMG-CoA) reductase, and 7a-hydroxylase activities. Taken together, these results strongly suggest that the macrosomic rats developed insulin resistance at adulthood [41, 42, 46]. It is well known that the development of obesity is linked to insulin sensitivity, whereas weight maintenance in the obese state is associated with insulin resistance [45, 47, 48]. Adult obese macrosomic rats have high VLDL concentrations accompanied by a concomitant increase in all VLDL-apoprotein and lipid components, suggesting elevated VLDL particle number. Overproduction of VLDL, a common feature of human and various experimental obesities, is a direct consequence of hyperinsulinemia and hepatic hyperlipogenesis [49–52]. These adult obese rats also possess enhanced HDL2–3 levels. A positive correlation between adiposity and HDL levels is seen in several animal models of obesity [53, 54]. Adult obese offspring of diabetic dams also present compositional changes of HDL2–3 particles, including enrichment in cholesterol [43, 45]. Fatty acid composition of liver and VLDL-TAG lipids are also altered in 3-month-old obese rats [44]. One of the most interesting findings is a reduced arachidonic acid (C20:4n-6) level in the liver and VLDL-TAG and phospholipids. This phenomenon is important because it coincides with the development of insulin resistance. Similar changes in the fatty acid composition of plasma and liver lipids have been shown to occur in human diabetes and obesity [55, 56]. Indeed, it has been reported that the degree of complications in human diabetes is inversely correlated with arachidonic acid (C20:4n-6) levels [57, 58]. It is now known that decreased insulin sensitivity is associated with decreased arachidonic acid levels in humans [56]. Therefore, decreased arachidonic acid (C20:4n-6) amounts in liver and VLDL phospholipids of macrosomic rats might, in turn, impair insulin activity and aggravate insulin resistance at adulthood. Besides, adult macrosomic offspring display liver steatosis. Fatty acid composition of liver and VLDL lipids are also altered throughout adulthood, reflecting changes in insulin sensitivity in these obese offspring.
In conclusion, fetal macrosomia in the offspring of diabetic mothers influences lipid and lipoprotein metabolism at birth and adulthood. It is, therefore, apparent that macrosomia in diabetic pregnancy may be considered as an important risk factor for adult obesity, diabetes and other metabolic complications, including essential fatty acid metabolism abnormalities and dyslipoproteinemia.
Anti-oxidant status is diminished in adult macrosomic offspring
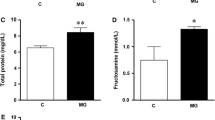
One of the earliest abnormalities observed in diabetic subjects is the involvement of oxidative stress [59]. High blood glucose levels in macrosomic newborns induce oxidative stress [60] which, in turn, induces the production of highly reactive oxygen radicals, being toxic to cells, particularly to the plasma membranes where these radicals interact with the lipid bilayer. Endogenous antioxidant enzymes, e.g., superoxide dismutase (SOD), catalase, glutathione peroxidase (GSH-Px), and reductase, and vitamins are responsible for the detoxification of deleterious oxygen radicals [61]. In diabetes as well as in macrosomia, protein glycation and glucose auto-oxidation may generate free radicals, which in turn catalyze lipid peroxidation [62]. Moreover, impaired glutathione metabolism [63] and decreased ascorbic acid levels [64] have been reported in diabetes and macrosomia. We have recently demonstrated that macrosomic obese pups exhibit a reduced anti-oxidant status, including increased plasma thiobarbituric acid reactive substances (TBARS), decreased oxygen radical absorbance capacity (ORAC) and vitamin C concentrations, SOD and GSH-Px activities [65]. Similar results have been obtained by Dincer et al. [66], who have shown a decrease in these enzyme activities in liver and lung of neonate of STZ-induced diabetic rats. Hence, treatment with antioxidants may prevent or reverse abnormalities associated with diabetes and its complications.
Cell-mediated immunity is altered in adult macrosomic offspring
It has been shown that the abnormalities in humoral and cell-mediated immunity in type I diabetic females may persist during pregnancy and, hence may complicate immune-fetal interaction [67]. As far as T-cell activation in diabetic pregnancy and their macrosomic offspring is concerned, only a few studies are available on the subject [67]. In fact, fully activated T-cells are detected in the cord blood of infants and mothers with type I diabetes but not in infants from normal mothers [67]. Moreover, from birth up to 15 years of age, the percentage of total T-cells was higher in children of type I diabetic mothers than in those of healthy mothers [68]. An increase in MHC class II positive lymphocytes has been observed in infants of type I diabetic mothers compared to controls [69]. Moreover, the newborns of type I diabetic mothers showed a significant reduction in natural killer (NK) lymphocytes, indicating a deficit in natural immunity at birth [70]. Newborn babies of type I diabetic mothers showed an increase in the number of CD4+ T-cells [71]. Furthermore, production of IL-1 and IL-2 in the culture supernatants of mitogen-stimulated lymphocytes of these newborns was higher than that in controls [72]. However, the role of pancreatic and splenic Th subsets in the modulation of these pathologies has not yet been explored. We have recently tried to establish a correlation between diabetic pregnancy/macrosomia and differentiation of T-cells into Th1 and Th2 subsets. We have demonstrated that diabetic pregnancy is associated with a decreased Th1 phenotype and IL-4 mRNA expression in the pancreas and spleen. In macrosomic offspring, high expression of IL-2 and IFN-γ mRNA, but not of Th2 cytokines, was observed, indicating that the Th1 phenotype is upregulated during macrosomia [73].
Besides, the T-cells of gestational diabetic rats and their macrosomic offspring seem to present a defect in signal transduction. Indeed, we have shown that the recruitment of free intracellular calcium concentrations from intracellular pool is altered in these animals [74]. Hence, it appears clear that the T-cells in diabetic pregnancy and macrosomic obese offspring are in vivo activated and hence, whenever one will talk of the preventive strategies, one should think of using agents which exert immunomodulatory effects.
PPAR-α is critical for diabetic pregnancy
Peroxisome proliferator-activated receptors (PPARs) are ligand-activated transcriptional factors that regulate a large number of genes by transcriptional activation and repression [75]. The three isotypes have been identified in lower vertebrates and mammals [76]. PPARα, PPARβ (δ), and PPARγ exhibit different tissue distribution as well as different ligand specificities and functions [77]. PPARα is highly expressed in the liver and brown adipose tissue and regulates lipid homeostasis. It controls positively the fatty acid transport and oxidation in the liver [76]. Thus, this receptor may play a non-negligible role in the regulation of chronic diseases such as diabetes, obesity, and atherosclerosis.
Our initial interest, in this study, was to examine the implication of PPARα in the induction of macrosomia in diabetic pregnancy in mice. To our surprise, we observed that 50% of PPARα-null mice with diabetic pregnancy aborted while the abortion was only 8.3% in wild type mice. We also observed high level of mortality (nearly 79%) in PPARα-null diabetic mice without any sign of macrosomia in both strains of mice, though the remaining offspring at adulthood developed insulin resistance. These observations indicate that the expression of PPARα is necessary for a successful diabetic pregnancy (unpublished results).
n-3 PUFAs exert beneficial effects in macrosomia
Polyunsaturated fatty acids (PUFAs) are known to modulate the metabolism of lipids and lipoproteins [78–81]. Dietary PUFAs have been classified into two categories, belonging to n-6 and n-3 families. The n-6 PUFAs, synthesized from linoleic acid (18:2n-6), are abundantly present in meat and vegetable oils. The most biologically active n-6 PUFA is arachidonic acid (C20:4n-6), which is implicated in most of the cellular functions. Arachidonic acid (C20:4n-6) gives rise to physiologically active eicosanoids (prostaglandins, thromboxanes, leucotrienes, and lipoxins). High contents of n-3 PUFAs, specifically docosahexaenoic acid (DHA; C22:6n-3) and eicosapentaenoic acid (EPA; C20:5n-3), are found in fish oil and marine algae. DHA is a significant structural component of membrane phospholipids whereas EPA gives rise, similar to arachidonic acid, to different biologically active metabolites via cyclo-oxygenase and lipoxygenase pathways [82].
Fish intake delays development of diabetes in glucose-intolerant individuals [83]. Studies in rats have shown [84] that fish oil exerts beneficial effects on insulin resistance, since it completely prevents the development of insulin resistance induced by a diet rich in fat. Insulin resistance in rats is inversely and significantly correlated with the n-3 PUFAs content of their skeletal muscles [85]. n-3 PUFAs enhance peripheral glucose utilization in rats [86].
In the rat model, we have noticed that feeding an n-3 PUFAs diet to diabetic pregnant rats decreased the incidence of macrosomia (64% in standard diet fed dams versus 48% in n-3 PUFAs diet fed dams). Besides, macrosomic rats of n-3 PUFAs diet fed group showed lower weight gain than those fed the standard diet, at each age [87]. n-3 PUFAs diet significantly decreased adipose tissue weight and lipid contents in macrosomic rats. At the age of 3 months, liver lipid levels were significantly enhanced in macrosomic rats compared to control animals in standard diet fed group. This elevation was not noticed in macrosomic rats fed an n-3 PUFAs diet. The elevation in the concentrations of serum and liver total cholesterol and TAG induced by diabetic pregnancy and macrosomia was significantly reduced by feeding an n-3 PUFAs diet [87]. Diabetes and macrosomia induced-elevation in serum and liver saturated fatty acids, 18:1 and 18:2(n-6), and a reduction in 20:4n-6, 20:5n-3, and 22:6n-3 levels was corrected by feeding an n-3 PUFAs diet to these animals [87]. The n-3 PUFAs diet in macrosomic pups increased serum and liver levels of eicospentaenoic acid (EPA) and docosahexaenoic acid (DHA). The n-3 PUFAs diet induces a significant diminution in liver and serum triglyceride and cholesterol concentrations in macrosomic pups during adulthood. The hypocholesterolemic effect of n-3 PUFAs was apparent in VLDL and LDL-HDL1, and was accompanied by an increase in cholesterol levels in HDL2–3 fraction.
The n-3 PUFAs exert their mechanisms of action at different lipid parameters. Several studies have suggested that the hypotriglyceridemic effect of n-3 fatty acids is due to reduced hepatic TAG output [88] or accelerated clearance of VLDL-TAGs [89]. In fact, n-3 PUFAs supplementation increases the endogenous activities of LPL and HTGL [90]. However, the effects of n-3 PUFAs on lipolytic activities are divergent, with sometimes decreased or no effects [91]. Several mechanisms have also been proposed for the TAG lowering associated with n-3 PUFAs. These mechanisms include decreased delivery of fatty acids to the liver, accompanied by increased fatty acid oxidation and decreased fatty acid synthesis, resulting in decreased fatty acid availability for TAG synthesis [91]. Moreover, LDL levels are decreased, unchanged or increased with n-3 PUFAs [91, 92]. Dietary supplementation with n-3 PUFAs induces the presence of large LDL particles, which might be expected to reduce atherogenic risk [92]. In addition, large amounts of EPA are found in LDL-esterified cholesterol, which leads to a marked disordering of lipid core and lowering of the LDL transition temperature [91]. Greater fluidity of the LDL core has been associated with reduced atherogenicity of the particle. In view of the well-known inverse relationship between plasma TAG levels and HDL-cholesterol (HDL-C), it is not surprising that fish oil treatment might increase HDL-C and HDL2 levels [90, 91]. It is important to note that HDL2 levels are known to be antiatherogenic, as they protect LDL against oxidative modifications.
We have here-before mentioned that macrosomia is associated with altered anti-oxidant enzyme activities and vitamin concentrations. As far as the effects of n-3 PUFAs on anti-oxidant status are concerned, contradictory results have been reported. In fact, some authors [93, 94] have reported increased levels of TBARS in human plasma after consumption of n-3 fatty acids, while other investigators [95, 96] could not find any significant differences in TBARS levels in their studies. However, several reports have shown the beneficial effects of fish oils containing n-3 PUFAs like EPA and DHA in the protection against lipid peroxidation in rat and human beings with diabetes [97, 98]. Kesavulu et al. [99] have demonstrated that the treatment of diabetic patients with n-3 fatty acids improved their anti-oxidant status. We observed that feeding an n-3 PUFAs diet restored antioxidant status in diabetic dams and macrosomic offspring [65]. Hence, n-3 PUFAs diet reduced increased plasma TBARS and corrected the decreased ORAC values in diabetic rats and their macrosomic offspring. Furthermore, n-3 PUFAs diet increased the diminished vitamin A levels in diabetic mothers and vitamin C concentrations in macrosomic pups. Besides, this diet improved the decreased erythrocyte SOD and GSH-Px activities in diabetic and macrosomic animals [65].
As far as the immune system is concerned, n-3 PUFAs have been considered as immunosuppressors and, therefore, they have been used in the management of a number of inflammatory and autoimmune diseases, including rheumatoid arthritis and multiple sclerosis [100, 101] as these pathologies are characterized by the presence of activated T-cells and cytokines either at the site of tissue injury [102, 103] or in the circulation [104, 105]. n-3 PUFAs have been shown to suppress mitogen-stimulated proliferation of lymphocytes isolated from lymph nodes [106], spleen [107], and lymphatic duct [108], in mice and human beings [107, 109, 110]. Feeding the n-3 PUFAs diet corrected intracellular calcium homeostasis in T-cells of diabetic pregnant dams and their macrosomic obese rats [74].
Feeding the n-3 PUFAs diet induces a shift in Th1/Th2 ratio to Th2 phenotype in rats with diabetic pregnancy [73]. Indeed, the n-3 PUFAs diet diminished Th1 mRNA quantities in macrosomic offspring. Besides, n-3 PUFAs diet upregulates Th2 profile in diabetic pregnant rats, associated with a decreased Th1 phenotype. Wallace et al. [111] have also observed that feeding fish oil to mice induced a shift in IFN-γ/IL-4 ratio by a factor of four as compared to animals fed the low fat diets. As far as the molecular mechanism of action of n-3 PUFAs is concerned, not much is known on this subject. We have previously shown that dietary n-3 PUFAs are incorporated into cell phospholipids [112]. Hence, we can propose that dietary n-3 PUFAs may exert their action by modulating cell signaling. We have recently shown that T-cell activation and T-cell calcium signaling are altered in diabetic pregnancy and macrosomia, and dietary fish oils, particularly EPA and DHA, restore these T-cell abnormalities [113]. Furthermore, DHA and EPA have been shown to induce increases in free intracellular calcium concentrations, by opening CRAC channels, in Jurkat T-cells [114]. During cell activation, a modification in intracellular pH also plays an important role in cell cycle progression and, hence, DHA and EPA have been shown to modulate this phenomenon in Jurkat T-cells [115]. Denys et al. [116, 117] have also demonstrated that DHA inhibits the phosphorylation of ERK1/ERK2 in Jurkat T-cells. Dietary n-3 PUFAs, incorporated into plasma membrane, may also give rise to diacylglycerols which, in turn, may modulate cell activation. It has been shown that diacylglycerols, containing EPA and DHA, modulate not only PKC activation [118] and calcium signaling [119], but also ERK1/ERK2 phosphorylation by acting on rasGRP [120].
To sum up, we can state that n-3 PUFAs, modulate lipid/lipoprotein metabolism, anti-oxidant status and, T-cell activation and differentiation and, consequently, exert their beneficial effects in diabetic pregnancy and macrosomia.
Conclusion
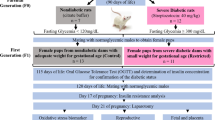
Fetal macrosomia is a risk factor for later obesity, diabetes, and dyslipoproteinemia. Macrosomia is a pathology where in utero development, in hyperglycemic and hyperlipidemic situations, plays an important role in the programing of the “metabolic memory” (Fig. 1). Maternal diabetes should be carefully considered and appropriate management of hyperglycemia should be sought. Macrosomia is a multifactorial pathology, involving anomalies in lipids, lipoproteins, anti-oxidants status, and activation of immune system (Th1-biased). Hence, dietary n-3 PUFAs exert beneficial effects by counteracting these physiological parameters both at maternal and macrosomic levels. Nonetheless, further detailed investigations are required to explore the role of these fatty acids in insulin resistance in obesity related to macrosomia.
Important physiological modifications in the diabetic pregnancy, leading to the in utero programing, implicated in macrosomia. Beside other unknown factors, insulin and leptin seem to play a key role in in utero programing, leading to creation of the “metabolic memory”, also responsible for the patho-physiological abnormalities at adulthood. The figure also shows the patho-physiological modifications observed in adult macrosomic offspring
References
Merzouk, H., Bouchenak, M., Loukidi, B., Prost, J., & Belleville, J. (2000). Fetal macrosomia related to maternal poorly controlled type 1 diabetes strongly impairs serum lipoprotein concentrations and composition. Journal of Clinical Pathology, 53, 917–923.
Meshari, A. A., De Silva, S., & Rahman, I. (1990). Fetal macrosomia-maternal risks and fetal outcome. International Journal of Gynaecology and Obstetrics, 32, 215–222.
Miller, J. M., Brown, H. L., Pastorek, J. G., & Gabert, H. A. (1988). Fetal overgrowth. Diabetic versus non diabetic. Journal of Ultrasound in Medicine, 7, 577–579.
Sacks, D. A., Chen, W., Greespoon, J. S., & Wolde-Tsadik, G. (1997). Should the same glucose values be targeted for type 1 as for type 2 diabetics in pregnancy? American Journal of Obstetrics and Gynecology, 177, 1113–1119.
Adesina, O. A., & Olayemi, O. (2003). Fetal macrosomia at the university college hospital, Ibadan: a 3-year review. Journal of Obstetrics and Gynaecology, 23, 30–33.
Sacks, D. A. (1993). Fetal macrosomia, and gestational diabetes: What’s the problem? Obstetrics and Gynecology, 81, 775–781.
Nassar, A. H., Usta, I. M., Khalil, A. M., Melhem, Z. I., Nakad, T. I., & Abu Musa, A. A. (2003). Fetal macrosomia (≥4500 g): Perinatal outcome of 231 cases according to the mode of delivery. Journal of Perinatology, 23, 136–141.
Conway, D. L. (2002). Delivery of the macrosomic infant: Cesarean section versus vaginal delivery. Seminars in Perinatology, 26, 225–231.
Taylor, R., Lee, C., Kyne-Grzebalski, D., Marshall, S. M., & Davison, J. M. (2002). Clinical outcomes of pregnancy in women with type 1 diabetes. Obstetrics and Gynecology, 99, 537–541.
Edelman, R. (1981). Obesity: Does it modulate infectious disease and immunity. Progress in Clinical and Biological Research, 67, 327–337.
Herrera, E., & Amusquivar, E. (2000). Lipid metabolism in the fetus and the newborn. Diabetes/Metabolism Research and Reviews, 16, 202–210.
Pribylova, H., & Dvorakova, L. (1996). Long-term prognosis of infants of diabetic mothers. Relationship between metabolic disorders in newborns and adult offspring. Acta Diabetologica, 33, 30–34.
Merzouk, H., Madani, S., Prost, J., Loukidi, B., Meghilli-Bouchenak, M., & Belleville, J. (1999). Changes in serum lipid and lipoprotein concentrations and compositions at birth and after one month of life in macrosomic infants of insulin-dependent diabetic mothers. European Journal of Paediatrics, 158, 750–756.
Merzouk, H., Madani, S., Chabane Sari, D., Prost, J., Bouchenak, M., & Belleville, J. (2000). The time course of changes in serum glucose, insulin, lipids and tissue lipase activities in macrosomic offspring of streptozotocin-induced mild diabetic rats. Clinical Science, 98, 21–30.
Cordero, L., & Landon, M. (1993). Infant of the diabetic mother. Clinics in Perinatology, 20, 635–648.
Plagemann, A., Harder, T., Kohlhoff, R., Rohde, W., & Dorner, G. (1997). Glucose tolerance and insulin secretion in children of mothers with pregestational IDDM or gestational diabetes. Diabetologia, 40, 1094–1100.
Schwartz, R., & Teramo, K. A. (2000). Effects of diabetic pregnancy on the fetus, and newborn. Seminars in Perinatology, 24, 120–135.
Sameshima, H., Kamitomo, M., Kajiya, S., Kai, M., Furukawa, S., & Ikenoue, S. (2000). Early glycemic control reduces large-for-gestational-age infants in 250 Japanese gestational diabetes pregnancies. American Journal of Perinatology, 17, 371–376.
Jimenez-Moleon, J. J., Bueno-Cavanillas, A., Luna-del-Castillo, J., Garcia-Martin, M., Lardelli-Claret, P., & Galvez-Gargas, R. (2002). Impact of different levels of carbohydrate intolerance on neonatal outcomes classically associated with gestational diabetes mellitus. European Journal of Obstetrics, Gynecology, and Reproductive Biology, 102, 36–41.
Fowden, A. L. (1989). The role of insulin in prenatal growth. Journal of Developmental Physiology, 12, 173–182.
Barker, D. J. (1995). Fetal origins of coronary heart disease. British Medical Journal, 311, 171–174.
Palinski, W., & Napoli, G. (2002). The fetal origins of atherosclerosis: maternal hypercholesterolemia, and cholesterol-lowering or antioxidant treatment during pregnancy influence in utero programming and postnatal susceptibility to atherogenesis. The FASEB Journal, 16, 1348–1360.
Napoli, C., D’Armiento, F. P., Mancini, F. P., Witztum, J. L., Palumbo, G., & Palinski, W. (1997). Fatty streak formation occurs in human fetal aortas and is greatly enhanced by maternal hypercholesterolemia: intimal accumulation of LDL and its oxidation precede monocyte recruitment into early atherosclerotic lesions. The Journal of Clinical Investigation, 100, 2680–2690.
Vogel, R. A., Coretti, M. C., & Plotnick, G. D. (1997). Effect of a single high-fat meal on endothelial function in healthy subjects. The American Journal of Cardiology, 79, 350–354.
Merzouk, H., & Khan N. A. (2003). Implication of lipids in macrosomia of diabetic pregnancy: Can n-3 polyunsaturated fatty acids exert beneficial effects? Clinical Science (London), 105, 519–529.
Desai, M., Crowther, N., Ozanne, S. E., Lucas, A., & Hales, C. N. (1995). Adult glucose and lipid metabolism may be programmed during fetal life. Biochemical Society Transactions, 23, 331–335.
Phillips, D. I. W. (1996). Insulin resistance as a programmed response to fetal undernutrition. Diabetologia, 39, 1119–1122.
Dorner, G., & Plagemann, A. (1994). Perinatal hyperinsulinism as possible predisposing factor for diabetes mellitus, obesity and enhanced cardiovascular risk in later life. Hormone and Metabolic Research, 26, 213–221.
Lautala, P., Puukka, R., Knip, M., & Perkkila, L. (1988). Postnatal decrease in insulin binding to erythrocytes in infants of diabetic mothers. The Journal of Clinical Endocrinology and Metabolism, 66, 696–701.
Foufelle, F., & Ferre, P. (2002). New perspectives in the regulation of hepatic glycolytic and lipogenic genes by insulin and glucose: A role for the transcription factor sterol regulatory-element-binding protein-1c. Biochemical Engineering Journal, 366, 377–391.
Azzout-Marniche, D., Becard, D., Guichard, C., Foretz, P., & Foufelle, F. (2000). Insulin effects on sterol regulatory-element-binding protein-1c (SREBP-1c). transcriptional activity in rat hepatocytes. Biochemical Engineering Journal, 350, 389–393.
Edwards, P. A., Tabor, D., Kast, H. R., & Venkateswaran, A. (2000). Regulation of gene expression by SREBP and SCAP. Biochimica et Biophysica Acta, 1529, 103–113.
Wilentz, R. E., Witters, L. A., & Pizer, E. S. (2000). Lipogenic enzymes fatty acid synthase and acetyl-coenzyme A carboxylase are coexpressed with sterol regulatory element binding protein and Ki-67 fetal tissues. Pediatric and Developmental Pathology, 3, 525–531.
Yura, S., Itoh, H., Sagawa, N., Yamamoto, H., Masuzaki, H., Nakao, K., Kawamura, M., Takemura, M., Kakui, K., Ogawa, Y., & Fujii S. (2005). Role of premature leptin surge in obesity resulting from intrauterine undernutrition. Cell Metabolism, 1, 371–378.
Merzouk, H., Madani, S., Korso, N., Bouchenak, M., Prost, J., & Belleville, J. (2000). Maternal and fetal serum lipid and lipoprotein concentrations and compositions in type 1 diabetic pregnancy: relationship with maternal glycemic control. The Journal of Laboratory and Clinical Medicine, 136, 441–448.
Cowett, R. M., & Schartz, R. (1982). The infant of diabetic mother. Pediatric Clinics of North America, 29, 1213–1231.
Kalkhoff, R. K. (1991). Impact of maternal fuels and nutritional state on fetal growth. Diabetes, 40, 61–65.
Raivio, K. O. (1985). Carbohydrate and lipid abnormalities in infants of diabetic mothers. Clinical Pediatrics, 197, 159–162.
Rovamo, L. M., Taskinen, M. R., Kuusi, J., & Raivio, K. O. (1986). Postheparin plasma lipoprotein and hepatic lipase activities in hyperinsulinemic infants of diabetic mothers and in large for date infants at birth. Pediatric Research, 20, 623–626.
Knopp, R. H., Warth, M. R., Charles, D., Childs, M., Li, J. R., & Mabuchi, H. Van (1986). Lipoprotein metabolism in pregnancy, fat transport to the fetus, and the effects of diabetes. Biology of the Neonate, 50, 297–317.
Oh, W., Gelardi, N. L., & Cha, C. J. (1988). Maternal hyperglycemia in pregnant rats: Its effects on growth and carbohydrate metabolism in the offspring. Metabolism: Clinical and Experimental, 37, 1146–1151.
Gelardi, N. L., Cha, C. J., & Oh, W. (1990). Glucose metabolism in adipocytes of obese offspring of mild hyperglycemic rats. Pediatric Research, 28, 641–645.
Merzouk, H., Madani, S., Boualga, A., Prost, J., Bouchenak, M., & Belleville, J. (2001). Age-related changes in cholesterol metabolism in macrosomic offspring of rats with streptozotocin-induced diabetes. Journal of Lipid Research, 42, 1152–1159.
Merzouk, H., Madani, S., Hichami, A., Prost, J., Belleville, J., & Khan, N. A. (2002). Age-related changes in fatty-acid composition of liver and serum very-low-density lipoprotein lipids in obese offspring of streptozotocin-induced diabetes rats. Obesity Research, 10, 703–714.
Merzouk, H., Madani, S., Hichami, A., Prost, J., Moutairou, K., Belleville, J., & Khan, N. A. (2002). Impaired lipoprotein metabolism in obese offspring of streptozotocin-induced diabetic rats. Lipids, 37, 773–781.
Gelardi, N. L., Cha, C. J., & Oh, W. (1991). Evaluation of insulin sensitivity in obese offspring of diabetic rats by hyperinsulinemic-euglycemic clamp technique. Pediatric Research, 30, 40–44.
Kissebah, A. H., Freedman, D. S., & Peiris, A. N. (1989). Health risks of obesity. The Medical Clinics of North America, 73, 111–138.
Del Prato, S., Enzi, G., Vigili de Kreutzenberg, S., Lisato, G., Riccio, A., Maifreni, L., Iori, E., Zurlo, F., Sergi, G., & Tiengo, A. (1990). Insulin regulation of glucose and lipid metabolism in massive obesity. Diabetologia, 33, 228–236.
Verges, B. L. (1999). Dyslipidaemia in diabetes mellitus. Review of the main lipoprotein abnormalities and their consequences on the development of atherogenesis. Diabetes & Metabolism, 25(Suppl 3), 32–40.
Suckling, K. E., & Jackson, B. (1993). Animal models of human lipid metabolism. Progress in Lipid Research, 32, 1–2.
Boulange, A., Planche, E., & Gasquet, P. (1981). Onset and development of hypertriglyceridemia in the Zucker rat (fa/fa). Metabolism: Clinical and Experimental, 30, 1045–1052.
Bioletto, S., Golay, A., Munger, R., Kalix, B., & James, R. W. (2000). Acute hyperinsulinemia and very-low-density and low-density lipoprotein subfractions in obese subjects. The American Journal of Clinical Nutrition, 71, 443–449.
Cohn, J. S., Nestel, P. J., & Turley, S. D. (1987). Metabolism of high-density lipoprotein in the hyperlipidemic, diabetic SHR/N-corpulent rat. Metabolism, 36, 230–236.
Mela, D. J., Cohen, R. S., & Kris-Etherton, P. M. (1987). Lipoprotein metabolism in a rat model of diet-induced adiposity. The Journal of Nutrition, 117, 1655–1662.
Simopoulos, A. P. (1999). Essential fatty acids in health and chronic disease. The American Journal of Clinical Nutrition, 70, 560S-569S.
Storlien, L. H., Hulbert, A. J. & Else, P. L. (1998). Polyunsaturated fatty acids, membrane function and metabolic diseases such as diabetes and obesity. Current Opinion in Clinical Nutrition and Metabolic Care, 1, 559–563.
Rabini, R. A., Tesei, M., Galeazzi, T., Dousset, N., Ferretti, G., & Mazzanti, L. (1999). Increased susceptibility to peroxidation of VLDL from non-insulin-dependent diabetic patients: A possible correlation with fatty acid composition. Molecular and Cellular Biochemistry, 199, 63–67.
Jones, D. B., Carter, R. D., Haitas, B., & Mann, J. I. (1983). Low phospholipid arachidonic acid values in diabetic platelets. British Medical Journal, 286, 173–175.
Yessoufou, A., Moutairou, K., Girard, A., Fatoke, M., Prost, J., Ahissou, H., Djrolo, F., Avode, G., Amoussou-Guenou, D., Hichami, A., & Khan, N. A. (2005). Antioxidant status in alcohol-related diabetes mellitus in Beninese subjects. Cellular and Molecular Biology, 51, 849–858.
Kamath, U., Rao, G., Raghothama, C., Rai, L., & Rao P. (1998). Erythrocyte indicators of oxidative stress in gestational diabetes. Acta Paediatrica, 87, 676–679.
Merzouk, S., Hichami, A., Madani, S., Merzouk, H., Berrouiguet, A.Y., Prost, J., Moutairou, K., Chabane-Sari, N., & Khan, N. A. (2003). Antioxidant status and levels of different vitamins determined by high performance liquid chromatography in diabetic subjects with multiple complications. General Physiology and Biophysics, 22, 15–27.
Hunt, J. V., Smith, C. C. T., & Wolf, S. P. (1990). Autoxidative glycosylation and possible involvment of peroxides and free radicals in LDL modification by glucose. Diabetes, 39, 1420–1424.
McLennan, S. V., Heffernan, S., Wright, L., Rae, C., Fisher, E., Yue, D. K., & Turtle, J. R. (1991). Changes in hepatic glutathione metabolism in diabetes. Diabetes, 40, 344–348.
Young, I. S., Torney, J. J., & Trimble, E. R. (1992). The effects of ascorbate supplementation on oxidative stress in the streptozotocin diabetic rat. Free Radical Biology & Medicine, 8, 752–758.
Yessoufou, A., Soulaimann, N., Merzouk, S. A., Moutairou, K., Ahissou, H., Prost, J., Simonin, A. M., Merzouk, H., Hichami, A., & Khan, N. A. (2006). N-3 Fatty acids modulate antioxidant status in diabetic rats and their macrosomic offspring. International Journal of Obesity (Lond), 30, 739–750.
Dincer, Y., Alademir, Z., Ilkova, H., & Akcay, T. (2002). Susceptibility of glutatione and glutathione-related antioxidant activity to hydrogen peroxide in patients with type 2 diabetes: Effect of glycemic control. Clinical Biochemistry, 35, 297–301.
Giordano, C. (1990). Immunobiology of normal and diabetic pregnancy. Immunology Today, 11, 301–303.
Roll, U., Scheeser, J., Standl, E., & Ziegler A. G. (1994). Alterations of lymphocytes subsets in children of diabetic mothers. Diabetologia, 37, 1132–1141.
Di Mario, U., Dotta, F., Garguilo, P., Sutherland, J., Adreani, D., Guy, K., Pachi, A., & Fallacca, F. (1987). Immunology in diabetic pregnacy: Activated T-cells in diabetic mothers and neonates. Diabetologia, 30, 66–71.
Lapolla, A., Sanzari, M. C., Znacanaro, F., Masin, M., Guerriero, A., Piva, I., Toniato, R., Erle, G., Plebani, M., & Fedele, D. (1999). Study on lymphocyte subpopulation in diabetic mothers at delivery and in their newborns. Diabetes, Nutrition & Metabolism, 12, 394–399.
Giordano, C., De Maria, R., Mattina, A., Stassi, G., Todaro, M., Pugliese, A., Galluzzo, G., Botta, R. M., & Galluzzo, A. (1982). Analysis of T-lymphocytte subsets after phyhemagglutinin stimulation in normal and type 1 diabetic mothers and their infants. American Journal of Reproductive Immunology, 28, 65–70.
El Mohandes, A., Touraine, J. L., Shurky, A. S., & Salle, B. (1982). Lymphocyte populations and reponses to mitogens in infants of diabetic mothers. Journal of Clinical & Laboratory Immunology, 8, 25–29.
Khan, N. A., Yessoufou, A., Minji, K., & Hichami, A. (2006). N-3 fatty acids modulate TH1 and TH2 dichotomy in diabetic pregnancy and macrosomia. Journal of Autoimmunity, 26, 268–277.
Guermouche, B., Yessoufou, A., Soulimane, N., Merzouk, H., Moutairou, K., Hichami, A., & Khan, N. A. (2004). N-3 fatty acids modulate T-cell calcium signaling in obese macrosomic rats. Obesity Research, 12, 1744–1753.
Issemann, I., & Green, S. (1990). Activation of a member of the steroid hormone receptor superfamily by peroxisome proliferators. Nature, 347, 645–650.
Wahli, W. (2002). Peroxisome proliferator-activated receptors (PPARs): from metabolic control to epidermal wound healing. Swiss Medical Weekly, 132, 83–91.
Braissant, O., Foufelle, F., Scotto, C., Dauca, M., & Wahli, W. (1996). Differential expression of peroxisome proliferator-activated receptors (PPARs): Tissue distribution of PPAR-alpha, -beta, and -gamma in the adult rat. Endocrinology, 137, 354–366.
Lichtenstein, A. H., Kennedy, E., Barrier, P., Danford, D., Ernst, N. D., Grundy, S. M., Leveille, G. A., Van Horn, L., Williams, C. L., & Booth, S. L. (1998). Dietary fat consumption and health. Nutrition Reviews, 56, 3–19.
Horrocks, L. A., & Yeo, Y. K. (1999). Health benefits of docosahexaenoic acid (DHA). Pharmacological Research, 40, 211–225.
Sundram, K. (1997). Modulation of human lipids and lipoproteins by dietary palm oil and palm olein: A review. Asia Pacific Journal of Clinical Nutrition, 6, 12–16.
Norum, K. R. (1992). Dietary fat and blood lipids. Nutrition Reviews 50, 30–37.
Lewis, R. A., Austen, K. F., & Soberman, R. J. (1990). Leukotrienes and other products of the 5-lipoxygenase pathway. Biochemistry and relation to pathobiology in human diseases. The New England Journal of Medicine, 323, 645–655.
Feskens, E. J., Bowles, C. H., & Kromhout, D. (1991). Inverse association between fish intake and risk of glucose intolerance in normoglycemic elderly men and women. Diabetes Care, 14, 935–941.
Storlien, L. H., Kraegen, E. W., Chisholm, D. J., Ford, G. L., Bruce, D. G., & Pascoe, W. S. (1987). Fish oil prevents insulin resistance induced by high-fat feeding in rats. Science (Washington, D.C.)., 237, 885–888.
Storlien, L. H., Jenkins, A. B., Chrisholm, D. J., Pascoe, W. S., Jhouri, S., & Kraegen, E. W. (1991). Influence of dietary fat composition on development of insulin resistance in rats. Diabetes, 40, 280–289.
Lardinois, C. K., & Starich, G. H. (1991). Polyunsaturated fats enhance peripheral glucose utilization in rats. Journal of the American College of Nutrition, 10, 340–345.
Soulimane-Mokhtari, N. A., Guermouche, B., Yessoufou, A., Saker, M., Moutairou, K., Hichami, A., Merzouk, H., & Khan, N. A. (2005). Modulation of lipid metabolism by n-3 polyunsaturated fatty acids in gestational diabetic rats and their macrosomic offspring. Clinical Science (Lond)., 09, 287–95.
Harris, W. S., Connor, W. E., Illingworth, D. R., Rothrock, D. W., & Foster, D. M. (1990). Effects of fish oil on VLDL triglyceride kinetics in humans. Journal of Lipid Research, 31, 1549–1558.
Harris, W. S., Lu, G., Rambjor, G. S., Walen, A. I., Ontko, J. A., Cheng, Q., & Windsor, S. L. (1997). Influence of n-3 fatty acid supplementation on the endogenous activities of plasma lipases. The American Journal of Clinical Nutrition, 66, 254–260.
Demke, D. M., Peters, G. R., Linet, O. I., Metzler, C. M., & Klott, K. A. (1988). Effects of a fish oil concentrate in patients with hypercholesterolemia. Atherosclerosis, 70, 73–80.
Harris, W. S. (1989). Fish oils and plasma lipid and lipoprotein metabolism in humans: a critical review. Journal of Lipid Research, 30, 785–807.
Sanchez-Muniz, F. J., Bastida, S., Viejo, J. M., & Terpstra, A. H. (1999). Small supplements of n-3 fatty acids change serum low density lipoprotein composition by decreasing phospholipid and apolipoprotein B concentrations in young adult women. European Journal of Clinical Nutrition, 38, 20–27.
Wander, R. C., & Shi-Hua, Du. (2000). Oxidation of plasma proteins is not increased after supplementation with eicosapentaenoic and docosahexaenoic acids. The American Journal of Clinical Nutrition, 72, 731–737.
Allard, J. P., Kurian, R., Aghdassi, E., Muggli, R., & Royall, D. (1997). Lipid peroxidation during n-3 fatty acid and vitamin E supplementation in humans. Lipids, 32, 535–541.
Nordoy, A., Bonaa, K. H., Nilsen, H., Berge, R. K., & Hansen, J. B. (1998). Ingerbresten OC. Effects of Simvastatin and omega-3 fatty acids on plasma lipoproteins and lipid peroxidation in patients with combined hyperlipidaemia. Journal of Internal Medicine, 243, 163–170.
Ando, K., Nagata, K., Beppu, M., Kikugawa, K., Kawabata, T., Hasegawa, K., & Suzuki, M. (1998). Effect of n-3 fatty acid supplementation on lipid peroxidation and protein aggregation in rat erythrocyte membranes. Lipids, 33, 505–512.
Hunkar, T, Aktan, F, Ceylan, A, & Karasu, C. (2002). Antioxidants in Diabetes-Induced Complications (ADIC). Study Group. Effects of cod liver oil on tissue antioxidant pathways in normal and streptozotocin-diabetic rats. Cell Biochemistry and Function, 20, 297–302.
Gunes, A., Ceylan, A., Sarioglu, Y., Stefek, M., Bauer, V., & Karasu C. (2005). The Antioxidants in Diabetes-induced Complications (ADIC). Study Group. Reactive oxygen species mediate abnormal contractile response to sympathetic nerve stimulation and noradrenaline in the vas deferens of chronically diabetic rats: effects of in vivo treatment with antioxidants. Fundamental & Clinical Pharmacology, 19, 73–79.
Kesavulu, M. M., Kameswararao, B., Apparao, Ch, Kumar, E. G., & Harinarayan, C. V. (2002). Effect of omega-3 fatty acids on lipid peroxidation and antioxidant enzyme status in type 2 diabetic patients. Diabetes & Metabolism, 28, 20–26.
Bittiner, S. B., Tucker, W. F. G., Cartwright, I., & Bleehen S. S. (1988). A Double-Blind randomised, placebo-controlled trial of fish oil in psoriasis. Lancet, 1, 378–380.
Kremer, J. M., Jubiz, W, Michalek, A, Rynes, R. I., Bartholonew, L. E., Bigaouette, J, Timchalck, M., Beeler, D., & Lininger, L. (1987). Fish oil fatty acid supplementation in active rheumatoid Arthrisis. Annals of Internal Medicine, 106, 479–503.
Konttinen, Y. T., Bergroth, V., Kinnunen, E., Nordstorm, D., & Kouri, T. (1987). Activated T-lymphocytes in patients with multiple sclerosis in clinical remission. Journal of the Neurological Sciences, 81, 133–139.
Barker, J. N. (1991). The patophysiology of psoriasis. Lancet, 338, 227–230.
Merrill, J. E., Mohlstorm, C., Uittenbogaart, C., Kermani-Arab V, Elisson, G. W., & Myers, L. W. (1984). Reponse and production of interleukin-2 by peripheral blood and cerebrospinal fluid lymphocytes of patients with multiple sclerosis. Journal of Immunology, 133, 1931–1937.
Wolf, R. E., & Brelsford W.G. (1988). Soluble Interleukin-2 receptors in systemic lupus erythematosus. Arthritis and Rheumatism, 31, 729–735.
Calder, P. C., Bevan, S. J., Hunt, S. V., & Newshlome E. A. (1991). Effect of fatty acids on the proliferation of concavaline A-stimulated rat lymphnode lymphocytes. The International Journal of Biochemistry, 23, 579–588.
Tsang, W. M., Weyman, C., & Smith, A. D. (1977). Effect of fatty acids mixtures phyto haemmaglutinin-stimulated lymphocytes from different species. Biochemical Society Transactions, 15, 153–154.
Calder, P. C., Bevan S. J., & Newsholme E. A. (1992). The inhibition of T- lymphocyte proliferation by fatty acids is an eicosanoid-indepedant mechanism. Immunology, 75, 108–115.
Buttke, T. M. (1984). Inhibition of lymphocyte proliferation by free fatty acids—I. Immunology, 53, 507–514.
Soyland, E., Nenseter, M. S., Braathhen L., & Drevon, C. A. (1993). Very long chain n-3 and n-6 polyunsaturated fatty acids inhibit proliferation in human T lymphoctes in vitro. European Journal of Clinical Investigation, 23, 112–121.
Wallace, A., Miles, E. A., Evans, C., Stock T. E., Yaqoob P., & Calder P. C. (2001). Dietary fatty acids influence the production of Th1- but not Th2-type cytokines. Journal of Leukocyte Biology, 69, 449–457.
Triboulot, C., Hichami, A., Denys, A., & Khan N. A. (2001). Dietary (n-3). polyunsaturated fatty acids exert antihypertensive effects by modulating calcium signaling in T cells of rats. The Journal of Nutrition, 131, 2364–2369.
Khan, N. A., & Hichami, A. (2002). Role of n-3 polyunsaturated fatty acids in T-cell signalling. In G. Pandalai (Ed.), Recent advances in research in lipids (Vol. 6). Transworld Publications, Trivendrum, Kerala, India, pp. 65–78.
Bonin, A., & Khan N. A. (2000). Regulation of calcium signalling by docosahexaenoic acid in human T-cells. Implication of CRAC channels. Journal of Lipid Research, 41, 277–284.
Aires, V., Hichami, A., Moutairou, K., & Khan, N. A. (2003). Docosahexaenoic acid and other fatty acids induce a decrease in pHi in Jurkat T-cells. British Journal of Pharmacology, 140, 1217–1226.
Denys, A., Hichami, A., & Khan N. A. (2001). Eicosapentaenoic acid and docosahexaenoic acid modulate MAP kinase (ERK1/ERK2) signaling in human T cells. Journal of Lipid Research, 42, 2015–2020.
Denys, A., Hichami, A., & Khan N. A. (2002). Eicosapentaenoic acid and docosahexaenoic acid modulate MAP kinase enzyme activity in human T-cells. Molecular and Cellular Biochemistry, 232, 143–148.
Madani, S., Hichami, A., Legrand, A., Belleville, J., & Khan, N. A. (2001). Implication of acyl chain ofdiacylglycerols in activation of different isoforms of protein kinase C. The FASEB Journal, 15, 2595–2601.
Hichami, A., Morin, C., Rousseau, E., & Khan, N. A. (2005). Diacylglycerol-containing docosahexaenoic acid in acyl chain modulates airway smooth muscle tone. American Journal of Respiratory Cell and Molecular Biology, 33, 378–386.
Madani, S., Hichami, A., Charkaoui-Malki, M., & Khan, N. A. (2004). Diacylglycerols containing Omega 3 and Omega 6 fatty acids bind to RasGRP and modulate MAP kinase activation. The Journal of Biological Chemistry, 279, 1176–1183.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Khan, N.A. Role of lipids and fatty acids in macrosomic offspring of diabetic pregnancy. Cell Biochem Biophys 48, 79–88 (2007). https://doi.org/10.1007/s12013-007-0019-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12013-007-0019-4