Abstract
To accomplish its multifunctional biological roles, zinc requires precise homeostatic mechanisms. There are efficient mechanisms that regulate zinc absorption from the alimentary tract and its excretion by the kidney depending on the organism demands. The regulatory mechanisms of cellular zinc inflow, distribution, and zinc outflow are so efficient that symptoms of zinc deficiency are rare, and symptoms connected with its massive accumulation are even more rare. The efficiency of homeostatic mechanisms that prevent zinc deficiency or excessive zinc accumulation in the organism is genetically conditioned. It seems that an essential element of zinc homeostasis is the efficiency of zinc transmembrane exchange mechanisms. Intracellular free zinc concentration is higher than in extracellular space. Physiologically, the active outflow of zinc ions from the cell depends on the increase of its concentration in extracellular space. The ion pumps activity depends on the efficiency by which the cell manages energy. Considering the fact that zinc deficiency accelerates apoptosis and that excessive zinc accumulation inside cells results in a toxic effect that forces its death brings about several questions: Is intensification and acceleration of changes in zinc metabolism with age meaningful? Is there a real zinc deficiency occurring with age or in connection with the aforementioned pathological processes, or is it just a case of tissue and cell redistribution? When discussing factors that influence zinc homeostasis, can we consider zinc supplementation or regulation of zinc balance in the area of its redistribution? To clarify these aspects, an essential element will also be the clear understanding of the nomenclature used to describe changes in zinc balance. Zinc homeostasis can be different in different age groups and depends on sex, thus zinc dyshomeostasisrefers to changes in its metabolism that deviate from the normal rates for a particular age group and sex. This concept is very ample and implies that zinc deficiency may result from a low-zinc diet, poor absorption, excessive loss of zinc, zinc redistribution in intra- and extracellular compartments, or a combination of these factors that is inadequate for the given age and sex group. Such factor or factors need to be considered for preventing particular homeostasis disorders (or dyshomeostasis). Regulation of zinc metabolism by influencing reversal of redistribution processes ought to be the main point of pharmacologic and nonpharmacologic actions to reestablish zinc homeostasis. Supplementation and chelation are of marginal importance and can be used to correct long-term dietary zinc deficiency or zinc poisoning or in some cases in therapeutic interventions. In view of its biological importance, the problem posed by the influence of zinc metabolism requires further investigation. To date, one cannot consider, for example, routine zinc supplementation in old age, because changes of metabolism with age are not necessarily a cause of zinc deficiency. Supplementation is warranted only in cases in which deficiency has been established unambiguously. An essential element is to prevent sudden changes in zinc metabolism, which lead to dyshomeostasis in the terms defined here. The primary prophylaxes, regular physical activity, efficient treatment of chronic diseases, are all elements of such prevention.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Zinc is currently considered one of the most important inorganic micronutrients. In spite of occupying the 27th place in abundance in the earth’s crust, it is without a doubt the most biologically important element in Group IIB of the periodic table [1].
It is found in nature mostly in the form of sulfides or oxides, and in foods the highest zinc content is found in oysters, saltwater fish, sunflower and pumpkin seeds, bran, wheat, some edible fungi, liver, egg yolks, onion, garlic, and tea [1, 2].
The human body contains 0.021–0.034 mol of zinc (1.4–2.3 g). It is concentrated mainly in the skin and its adnexa, bones, teeth, skeletal muscles, liver, prostate, testicles, and eye. There are areas of high concentration of zinc in the human brain, e.g., near hippocampus. In cells, zinc is mostly seated close to the cell membrane and in the nucleus [3].
Zinc is characterized by its multidirectional bioactivity. It is a component in more than 300 enzymes, fulfilling a variety of catalytic, co-catalytic and/or structural functions [1, 3, 4]. Among other things, zinc determines the activity of angiotensin-I converting enzyme (ACE), carbonic anhydrase, and the endothelin-converting enzyme (ECE). Its presence is essential for forming the quaternary structure of many regulatory proteins and hormonal receptors such as zinc fingers, zinc twists, and zinc clusters, which determine binding to DNA. Zinc is part of the nucleic acids structure and takes part in its metabolism. It stabilizes cell membranes and is a regulatory factor for their functions [1–7].
Cell growth and cytokinesis depend on the intracellular zinc content and its transport [1, 3, 4, 8, 15]. Also, zinc translocates calcium from one site to another, modifying calcium-dependent processes [7, 16].
For accomplishing its multifunctional roles, zinc requires precise homeostatic mechanisms. There are efficient mechanisms that regulate zinc absorption from alimentary tract as well as its excretion by the kidney depending on the organism demands. The regulatory mechanisms of cellular zinc inflow, distribution, and zinc outflow are so efficient that symptoms of zinc deficiency are rare, and symptoms connected with its massive accumulation are even rarer [1, 17, 18].
Zinc Homeostasis
It is known that the basic mechanism of zinc homeostasis maintenance involves changes in zinc absorption and secretion to and from the alimentary tract. It also involves regulation of zinc urinary excretion and its tissue and cell redistribution [19].
The intracellular content of zinc is genetically conditioned. It shows relatively small intra-individual variations in comparison to inter-individual variations, and shows different values in different organs [20–25]. There are two pools of intracellular zinc: slow-acting, associated to protein synthesis or to cell membrane (structural zinc), and fast-acting (also called free zinc), as in catalytic centers and signal transmitters [1, 17].
Practically all of the zinc, approximately 98%, is located in intracellular space. The small amount of extracellular zinc changes in response to different factors, regardless of its consumption and total content in the human body [1, 6].
The serum zinc concentration is tied to circadian rhythm, undergoing a gradual reduction from early morning to late afternoon [26], but remains relatively constant, except during long-lasting periods of dietary zinc deficiency, severe stress response, such as in cases of cardiac infarction, infection, or inflammation, which cause the serum zinc concentration to decrease [1, 6].
Emotional stress or short-term physical exertion does not bring changes in zinc concentration in blood serum, but chronic emotional stress or frequent, nonphysiological effort causes its decrease [1, 6, 18].
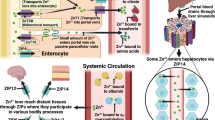
The concentration of free zinc inside the cell is lower than in extracellular space, e.g., in blood serum [27, 28], an electrochemical gradient is created causing zinc to flow across the membrane. In bipolar cells such as enterocytes, hepatocytes, or endothelial cells zinc inflow (influx) is driven by the concentration gradient through the top surface without energy expenditure. Under conditions of high extracellular zinc, transport also occurs by passive diffusion. Transmembrane zinc transport through the basic part of the cell takes place by both passive diffusion and active transport mechanisms. It is likely that there exists a potassium–zinc anti-transport (2K+/Zn++). Zinc inflow is also connected with anionic chloride–bicarbonate exchange (Cl−/HCO3 −). In unipolar cells, zinc ions inflow takes place in similar fashion [28–31].
Zinc outflow (efflux) takes place against the electrochemical gradient on an active transport basis, a calcium–zinc anti-transport (Ca++/Zn++), and by the ionic transport mechanisms previously described.
The efficiency of homeostatic mechanisms that prevent zinc deficiency or excessive zinc accumulation in the organism is genetically conditioned [21–25, 32–36]. The genetic diversity of the population and zinc content in the diet may be determinants in the evolution of arterial hypertension or arteriosclerosis. Accelerated arteriosclerosis evolution, ischemic disease, and diabetes with zinc excess in the diet [37–42], deficiency [43–46], or no association [47] were determined in different population samples.
With age, there is a decrease of gastrointestinal (GI) absorption of zinc concomitant with increases in red blood cell concentration and urinary excretion [48, 49]. It suggests that the change in zinc metabolism is an element of the aging process. The efficiency of ionic pumps decreases with age, affecting the regulatory mechanisms of intra- and extracellular zinc balance. This results in increases of zinc content in frontal lobe and hippocampus neurocytes and a decrease of its content in lymphocytes. These changes suggest a growing redistribution of zinc ions in organism following deficiency of the total pool of zinc with age [50–54].
Similar changes are observed during chronic pathological processes such as arterial hypertension, type 2 diabetes, or obesity [55–58]. Age-matched subjects suffering from such conditions show lower serum zinc concentration and increased urinary excretion when compared to healthy individuals. These processes are statistically tied to a shorter lifetime span.
Considering the fact that zinc deficiency accelerates apoptosis [59] and that excessive zinc accumulation inside cells results in a toxic effect that forces its death [60, 61] brings about several questions: Is intensification and acceleration of changes in zinc metabolism with age meaningful? Is there a real zinc deficiency occurring with age or in connection with the aforementioned pathological processes, or is it just a case of tissue and cell redistribution? When discussing factors that influence zinc homeostasis, can we consider zinc supplementation or regulation of zinc balance in the area of its redistribution?
To clarify these aspects, an essential element will also be the clear understanding of the nomenclature used to describe changes in zinc balance. Zinc homeostasis can be different in different age groups and depends on sex, thus, zinc dyshomeostasis refers to changes in its metabolism that deviate from the normal rates for a particular age group and sex. This concept is very ample and implies that zinc dyshomeostasis includes zinc deficiency (resulting from a low-zinc diet, poor absorption, or excessive loss of zinc), zinc redistribution in intra- and extracellular compartments with local deficiency or excess and zinc excess (resulting from a high-zinc diet) or a combination of these factors that is inadequate for the given age and sex group. Such factor or factors need to be considered for preventing particular homeostasis disorders (or dyshomeostasis).
Aging and progressive organ changes, for example in arterial hypertension, have a definite influence on the function of the organism. Both processes greatly decrease zinc, thus, it would be of value to include zinc supplementation in these subjects to improve immune function, among other things. In spontaneously hypertensive rats, a frequent cause of death (in addition to vascular changes) is pneumonia resulting from weakened immunity [42, 62–64].
Similar changes in zinc metabolism occur in diabetes and obesity [55–58]. These can explain faster dynamics of organ changes with coexisting arterial hypertension, diabetes, and overweight. Normalization of zinc balance parameters after normalization of body weight as well as improvement of the glucose tolerance after zinc substitution has been demonstrated [65–67].
Likewise, chronic inflammatory diseases of the GI tract, respiratory system, circulatory failure, neoplastic diseases, chronic psychical stress or excessive, chronic physical effort load are proven causes of zinc dyshomeostasis [1, 6, 18].
The redistribution connected with intracellular zinc accumulation and disrupted balance of free zinc ions in neurons and extracellular space of the central nervous system can be related to neurodegenerative processes [61]. Free intracellular zinc is a potentially toxic cation that takes part in impairing of neurons in the course of ischemia, trauma, or epilepsy [60].
It seems that an essential element of zinc homeostasis is the efficiency of zinc transmembrane exchange mechanisms. Physiologically, the activity of zinc ions’ outflow from the cell depends on the increase of its concentration in extracellular space. The ion pumps activity is dependent on the efficiency of cell energetic status. The exchange of zinc across the membrane is affected, among other things, by aldosterone, other steroid hormones, including sex hormones and endogenous ouabain [55, 68, 69].
To answer the raised questions, the parameters describing zinc homeostasis and the level of its dyshomeostasis, deficiency, excess, and degree of its redistribution need to be taken into account. It is also essential to determine rates for specific age and sex groups, probably also with reference to particular populations with regard to race or geographical distribution.
Measuring the necessary parameters should be reliable, relatively simple, and accessible. To date, the methods employed to determine zinc metabolism include direct measurement of zinc levels and indirect techniques such as quantifying transporting proteins, determining the activity of zinc-dependent enzymes. The direct methods include determining serum zinc concentrations, measuring the zinc concentration in serum-basal and after intravenous or oral zinc supply, known as zinc tolerance tests [70–72], the degree of absorption and redistribution with use of zinc isotopes [17, 19, 55], excretion with urine [17–19, 71], zinc content in erythrocytes and leukocytes [12, 20–22, 48, 55], inflow and outflow rates [27, 30, 31, 55, 73], free zinc content in cells and serum [28, 59, 60, 73]. The other methods of zinc metabolism estimation include zinc content in cell membranes of erythrocytes and thrombocytes, in hair, biopsy material, or by determining albumin, ceruloplasmin, and copper concentrations in blood plasma, calcium serum concentration (in zinc excess), or by measuring, i.e., the alkaline phosphatase and 5prime-nucleotidase activities [2, 3, 5, 8–12, 15, 18, 19, 73–76].
Based on literature and own observations in the field of screening tests to determine zinc metabolism by means that permit to “pre-evaluate” zinc excess or deficiency and redistribution occurrence, the zinc concentration in blood serum and lymphocytes are adequate parameters, provided that the differences caused by age, sex, and population are taken into account.
Serum zinc values range from 12.2 μM/l to 21.4 μM/l (80–140 μg%) [2]. Deficiency is manifest if serum zinc levels are ≤9.9 μM/l [75]. The decrease of lymphocyte zinc levels is a measure of the redistribution process, which, jointly with serum zinc, are good indicators of zinc deficiency in the organism.
In a previous study on healthy individuals of both sexes, aged 33.22 ± 9.15 years, the zinc content in lymphocytes was 0.59 ± 0.56 μg/mg protein. When classified by sex, the value for women was 0.69 ± 0.70 and 0.45 ± 0.27 for men [77].
The following tests seem to be essential to better estimate zinc homeostasis: zinc tolerance tests, zinc content in erythrocytes, rate of zinc outflow from lymphocytes, and zinc distribution using 65Zn or 70Zn isotopic tracing.
Changes in the parameters of zinc balance provide evidence for its tissue- and cell distribution, which is not an unambiguous sign of deficiency or excess. Supplementation will help in cases of deficiency. In cases of zinc excess, treatment will involve suitable chelating agents, whereas dyshomeostasis without zinc excess or deficiency will require metabolism regulation to attenuate the condition. There are reports of a possible therapeutic modulation of zinc metabolism [78, 79].
Zinc Deficiency
Decreased concentrations of zinc in serum, lymphocytes, and erythrocytes together with clinical symptoms would be considered valid proofs of zinc deficiency [1]. Confirmation of deficiency comes from zinc tolerance tests (increased absorption from the alimentary tract or accelerated decrease of serum concentration after intravenous administration) and, in questionable situations, isotopic research. Once deficiency has been proven, a supplementation program may be established. The efficiency of supplementation will be evidenced by improvement of the aforementioned indicators and remission of symptoms.
There are no univocal studies to favor routine zinc supplementation in diseases such as arterial hypertension, diabetes, or obesity accompanied by zinc deficiency [33–40, 44, 47, 51, 52–54, 56, 61). This is also the case for supplementing older adults. Because the serum zinc level decreases with age, the apparent deficiency may be part of a physiological phenomenon [48, 49].
Zinc Excess
High serum zinc accompanied by deficiencies of calcium, copper, iron and by anemia and diminished osmotic resistance of red blood cells are evidence of excess zinc in the organism.
The confirmed examinations may be zinc tolerance tests (decreased absorption from the alimentary tract or delay decrease of serum concentration after i.v. administration) and, in questionable situations, isotopic research. Treatment may require use of suitable chelators to avoid the possibility of intracellular toxicity of zinc [60, 61].
There are reports of a possible therapeutic modulation of zinc metabolism (diminish influx to cell). Zinc chelation therapy is used to lower cardiotoxicity of cytostatics [78]. Also, for example, intraventricular injections of calcium ethylenediaminetetraacetic acid (EDTA) have been shown to reduce neuronal death after an episode of cerebral ischemia [79].
Estimating the Degree of Zinc Redistribution
The evidence of redistribution will be mutual relationships between the zinc concentration in blood serum and its content in lymphocytes and erythrocytes. Zinc tolerance tests and isotopic tracing with 65Zn or 70Zn can be used to verify and determine the course of redistribution leading to either deficiency or accumulation.
Summary
Regulation of zinc metabolism to diminish the degree of dyshomeostasis will be possible depending on the primary cause. It can be accomplished by administering drugs that indirectly or directly affect zinc metabolism. Considering the toxic activity of intracellular zinc excess, an essential element of the treatment will be the improvement of cell membrane function and, as a consequence, the increase of zinc flow out to extracellular space. Because excessive intracellular zinc disrupts the mechanisms of oxygen metabolism, it consequently diminishes the activity of zinc outflow from the cell. This constitutes a “vicious circle” mechanism that needs to be broken. Means of affecting intracellular oxygen metabolism, such as pyruvates, help to bring down the accumulation of zinc and improves the cell survival rate [80].
Drugs that produce a favorable effect on zinc metabolism are, among others, those inhibiting angiotensin-converting enzyme activity, spironolactone, substances that rise sensibility of tissues to insulin and insulin itself. Non-pharmacological actions such as weight reduction also profitably influence zinc metabolism [65].
Regulation of zinc metabolism by influencing reversal of redistribution processes ought to be the main point of pharmacologic and nonpharmacologic actions to reestablish zinc homeostasis. Supplementation and chelation are of marginal importance and can be used to correct long-term dietary zinc deficiency or zinc poisoning, or in some cases in therapeutic interventions.
In view of its biological importance, the problem posed by the influence of zinc metabolism requires further investigation. To date, one cannot consider, for example, routine zinc supplementation in old age, because changes of metabolism with age are not necessarily a cause of zinc deficiency. Supplementation is warranted only in cases in which deficiency has been established unambiguously. An essential element is to prevent changes in zinc metabolism, which leads to dyshomeostasis in the terms defined here. The primary prophylaxes, regular physical activity, efficient treatment of chronic diseases, are all elements of such prevention.
References
Vallee BL, Falchuk KH (1993) The biochemical basis of zinc physiology. Physiol Rev 73:79–94
Kokot F, Tatoń J (1991) Zaburzenia przemiany materii w Chorobach Wewnêtrznych pod red. F. Kokota, PZWL Warszawa 670
Holtmeier HJ, Kuhn M, Rummel K (1976) Zink ein lebenswichtiges Mineral, Wissenschaftliche Verlagsgeselschaft MbH. Stuttgart 13
Turner AJ, Brown CD, Carson JA, Barens K (2000) The neprilysin family in health and disease. Adv Exp Med Biol 477:229–240
Lopez-Ongil S, Senchak V, Saura M, Zaragoza C, Ames M, Ballerman BJ, Rodriguez-Puyol M, Rodroguez-Puyol D, Lowenstein CJ (2000) Superoxide regulation of endothelin converting enzyme. J Biol Chem 275:26423–26429
Cousins RJ (1986) Toward a molecular understanding of zinc metabolism. Clin Physiol Biochem 4:20–30
Csermely P, Somogyi J (1989) Zinc as a possible mediator of signal transduction in T lymphocytes. Acta Physiol Hung 74:195–197
Avery RA, Bettger WJ (1992) Zinc deficiency alters the protein composition of the membrane skeleton but not the extractability or oligomeric form of spectrin in rat erythrocyte membranes. J Nutr 122:428–434
Bettger WJ, O’Dell BL (1981) A critical physiological role of zinc in the structure and function of biomembranes. Life Sci 28:1425–1438
Carvalho A (1972) Binding and release of cations by sarcoplasmic reticulum before and after removal of lipids. Eur J Biochem 27:491–502
Dorup I, Clausen T (1991). Effects of magnesium and zinc deficiencies on growth and protein synthesis in skeletal muscle and the heart. Br J Nutr 66:493–504
Driscoll ER, Bettger WJ (1992) Zinc deficiency in the rat alters the lipid composition of the erythrocyte membrane Triton shell. Lipids 27:972–977
Evans RM (1988) The steroid and thyroid hormone receptor superfamily. Science 240:889–895
Harrison NL, Radke HK, Tamkun MM, Lovinger DM (1993) Modulation of gating of cloned rat and human K+ channels by micromolar Zn+2. Mol Pharmacol 43:482–486
Maccara IG (1985) Oncogenesis, ions and phospholipids. Am J Physiol 248:C3–C11
Csermely P, Sandor P, Radics L, Somogyi J (1989) Zinc forms complexes with higher kinetical stability than calcium, 5-F-BAPTA as a good example. Biochem Biophys Res Commun 165:838–844
Lowe NM, Green A, Rhodes JM, Lombard M, Jalan R, Jackson MJ (1993) Studies of human zinc kinetics using the stable isotope 70Zn. Clin Sci 84:113–117
Girchev R, Tzachev K (1988) Metabolism and homeostasis of zinc and copper. Acta Physiol Pol 39(Suppl 32):103–118
King JC, Shames DM, Woodhouse LR (2000) Zinc homeostasis in humans. J Nutr 130:1360S–1366S
Darlu P, Lalouel JM, Henrotte JG, Rao DC (1983) A genetic study of red blood zinc concentration in man. Hum Hered 33:311–318
Henrotte JG, Santarromana M, Pia M (1987) Genetic factors regulating zinc concentrations in mics spleen and liver: relationship with the H-2 complex. Immunogenetics 25:408–410
Henrotte JG, Santarromana M, Franck G, Bourdon R (1990) Blood and tissue zinc levels in spontaneously hypertensive rats. J Am Coll Nutr 9:340–344
Henrotte JG, Santarromana M, Franck G, Guicheney P, Boulu R, Bourdon R (1992) High cardiac zinc levels in spontaneously hypertensive rats. J Hypertens 10:553–559
Olholm-Larsen P (1979) Serum zinc levels in heterozygous carriers of the gene for acrodermatitis enteropathica. Hum Genet 46:65–74
Smith JC, Zeller JA, Brown ED, Ong SC (1976) Elevated Plasma zinc: a heritable anomaly. Science 193:496–498
McMaster D, McCrum E, Patterson CC, Kerr MM, O’Reilly D, Evans AE, Love AH (1992) Serum copper and zinc in random samples of the population of Northen Ireland. Am J Clin Nutr 56:440–446
Simons TJB (1991) Intracellular free zinc and zinc buffering in human red blood cells. J Membr Biol 123:63–71
Simson TJB (1991) Calcium-dependent zinc efflux in human red blood cells. J Membr Biol 123:73–80
Bobilya DJ, Briske-Anderson M, Reeves PG (1992) Zinc transport into endothelial cell is a facilitated process. J Cell Physiol 151:1–7
Raffaniello RD, Shih-Yu L, Teichberg S, Wapnir RA (1992) Distinct mechanisms of zinc uptake at the apical and basolateral membranes of caco-2 cells. J Cell Physiol 152:356–361
Tacnet F, Lauthier F, Ripoche P (1993) Mechanisms of zinc transport into pig small intestine brush-border membrane vesicles. J Physiol 465:57–72
Gracia CE, Kdcoyne CM, Cardillo C, Cannon RO 3, Quyyumi AA, Panza JA (1995) Effect of copper-zinc superoxide dismutase on endothelium-dependent vasodilation in patients with essential hypertension. Hypertension 26:863–868
Sato M, Yanagisawa H, Nojima Y, Tamura J, Wada O (2002) Zn deficiency aggravates hypertension in spontaneously hypertensive rats: possible role of Cu/Zn-superoxide dismutase. Clin Exp Hypertens 24:355–370
Cebeci SA, Kocaturk PA, Kavas GO (2002) Hypertension: does impaired endothelium-dependent relaxation affect superoxide scavenging? Biol Trace Elem Res 90:239–249
Sato M, Kurihara N, Moridaira K, Sakamoto H, Tamura J, Wada O, Yanagisawa H (2003) Dietary Zn deficiency does not influence systemic blood pressure and vascular nitric oxide signaling in normotensive rats. Biol Trace Elem Res 91:157–172
Yanagisawa H, Sato M, Nodera M, Wada O (2004). Excessive zinc intake elevates systemic blood pressure levels in normotensive rats—potential role of superoxide-induced oxidative stress. J Hypertens 22:543–550
Davydenko NV, Smirnova IP, Kvasha EA, Gorbas EAIM, Koblianskaia AV (1995) Interrelatioship between dietary intake of minerals and prevalence of hypertension. Vopr Pitan 6:17–19
Davydenko NV, Smirnova IP, Kvasha EA, Gorbas EAIM (1995) The relationship between the copper and zinc intake with food and the prevalence of ischaemic heart disease and its risk factors. Lik Sprava 5-6:73–77
Anonymous (1985) Megadose zinc intakes impairs immune responses. Nutr Rev 43:141–143
Chandra RK (1984) Excessive intake of zinc impairs immune response. JAMA 252:1443–1445
Ripa S, Ripa R (1994) Zinc and atherosclerosis. Minerva Med 85:647–654
Ripa S, Ripa R (1994) Zinc and arterial pressure. Minerva Med 85:455–459
Singh RB, Niaz MA, Rastogi SS, Bajaj S, Gaoli Z, Shoumin Z (1998) Current zinc intake and diabetes and coronary artery disease and factors associated with insulin resistance in rural and urban populations of North India. J Am Coll Nutr 17:564–570
Chiplonkar SA, Agte VV, Tarwadi KV, Paknikar KM, Diwate UP (2004) Micronutrient deficiencies as predisposing factors for hypertension in lacto-vegetarian Indian adults. J Am Coll Nutr 23:239–247
Schutte AE, Van Rooyen JM, Huisman HW, Kruger HS, Malan NT, De Didder JH (2003) Dietary risk markers that contribute to the aetiology of hypertension in black South African children: the THUSA BANA study. J Hum Hypertens 17:29–35
Fodor JG, Rusted IE (1987) Electrolyte profiles in a hypertensive population: The Newfoundland Study. Clin Invest Med 10:586–591
Hajjar I, Kotchen T (2003) Regional variations of blood pressure in the United States are associated with regional variation in dietary intakes: the NHANES-II data. J Nutr 133:211–214
Lindeman RD, Clark ML, Colmore JP (1971) Influence of age and sex on plasma and red-cell zinc concentration. J Gerontol 26:358–363
Wastney ME, Ahmed S, Henkin RI (1992) Changes in regulation of human zinc metabolism with age. Am J Physiol 263(5 Pt 2):R1162–R1168
Donahue AN, Aschner M, Lash LH, Syversen T, Sonntag WE (2006) Growth hormone administration to aged animals reduces disulfide glutathione levels in hippocampus. Mech Ageing Dev 127:57–63
Hodkinson CF, Kelly M, Coudray C, Gilmore WS, Hannigan BM, O’Connor JM, Strain JJ, Wallace JM (2005) Zinc status and age-related changes in peripheral blood leucocyte subpopupations in healthy men and women aged 55–70 y: the ZENITH study. Eur J Clin Nutr 59(Suppl 2):S63–S67
Ravaglia G, Forti P, Maioli F, Bastagli L, Facchini A, Mariani E, Savarino L, Sassi S, Cucinotta D, Lenaz G (2000) Effect of micronutrient on natural killer cell immune function in healthy free-living subjects aged ≥90 y. Am J Clin Nutr 71:590–598
Mocchegiani E, Malavolta M, Marcellini F, Pawelec G (2006) Zinc, oxidative stress, genetic background and immunosenescence: implications for healthy ageing. Immunity and Ageing 3:6
Mocchegiani E, Costarelli L, Giacconi R, Cipriano C, Muti E, Rink L, Malavolta M (2006) Zinc homeostasis in aging: two elusive faces of the same metal. Rejuvenation Res 9:351–354
Tubek S (2005) The zinc content in lymphocytes and the activity of zinc ions efflux from lymphocytes in primary arterial hypertension. Biol Trace Elem Res 107:89–99
Sprietsma JE (1999) Modern diets and diseases: NO-zinc balance. Under Th1, zinc and nitrogen monoxide (NO) collectively protect against viruses, AIDS, autoimmunity, diabetes, allergies, asthma, infectious diseases, atherosclerosis and cancer. Med Hypotheses 53:6–16
Chandra RK (1981) Immune response in overnutrition. Cancer Res 41:3795–3796
Takakura M (1998) Analysis of zinc concentrations in leucocytes and its application to patients with non-insulin-dependent diabetes mellitus. Hokkaido Igaku Zasshi 73:571–580
Treves S, Trentini PL, Ascanelli M, Bucci G, Di Vrigilio F (1994) Apoptosis is dependent on intracellular zinc and independent of intracellular calcium in lymphocytes. Exp Cell Res 211:339–343
Malaiyandi LM, Honick AS, Rintoul GL, Wang QJ, Reynolds IJ (2005) Zn2+ inhibits mitochondrial movement in neurons by phosphatidylinositol 3-kinase activation. J Neurosci 25:9507–9514
Capasso M, Jeng JM, Malavolta M, Mocchegiani E, Sensi SL (2005) Zinc dyshomeostasis: a key modulator of neuronal injury. J Alzheimers Dis 8:93–108
Kromhout D, Wibowo AA, Herber i wsp RF (1985) Trace metals and coronary heart disease risk indicators in 152 elderly men (The Zutphen Study). Am J Epidemiol 122:378–385
Ripa S, Ripa R (1995) Zinc and immune function. Minerva Med 86:315–318
Przybylski J (1991) The role of arterial chemoreceptors and tissue oxygen supply in primary arterial hypertension pathogenesis, based upon investigations carried out on animal model (SAH). Qualifying thesis. Medical University of Warsaw, Warsaw, pp 24–42, 85–167 (in Polish).
Ishikawa Y, Kudo H, Kagawa Y, Sakamoto S (2005) Increased plasma of zinc in obese adult females on a weight-loss program based on a hypocaloric balanced diet in vivo 19:1035–1037
Simon SF, Taylor CG (2001) Dietary zinc supplementation attenuates hyperglycemia in db/db mice. Exp Biol Med (Maywood) 226:43–51
Raz I, Karsai D, Katz M (1989) The influence of zinc supplementation on glucose homeostasis in NIDDM. Diabetes Res 11:73–79
Schoner W, Scheiner-Bobis G (2005) Endogenous cardiac glycosides: hormones using the sodium pump as signal transducer. Semin Nephrol 25:343–351
Schoner W, Bauer N, Muller-Ehmsen J, Kramer U, Hambarchian N, Schwinger R, Moeller H, Kost H, Weitkamp C, Schweitzer T, Kirch U, Neu H, Grunbaum EG (2003) Ouabain as a mammalian hormone. Ann NY Acad Sci 986:678–684
Tubek S (2001) Increased absorption of zinc from alimentary tract in the primary arterial hypertension. Biol Trace Elem Res 83:31–38
Henderson LM, Brewer GJ, Dressman JB, Swidan SZ, DuRoss DJ, Adair CH, Barnett JL, Berardi RR (1996) Use of zinc tolerance test and 24-hour urinary zinc content to assess oral zinc absorption. J Am Coll Nutr 15:79–83
Neve J, Hanocq M, Peretz A, Abi Khalil F, Pelen F, Famaey JP, Fontaine J (1991) Pharmacokinetic study of orally administered zinc in humans: evidence for an enteral recirculation. Eur J Drug Metab Pharmacokinet 16:315–323
Balesaria S, Hogstrand Ch (2006) Identification, cloning and characterization of a plasma membrane zinc efflux transporter, TrZnT-1, from fugu pufferfish (Takifugu rubripes). Biochem J 394:485–493
Agte VV, Chiplonkar SA, Tarwadi KV (2005) Factors influencing zinc status of apparently healthy Indians. J Am Coll Nutr 24:334–341
Vivoli G, Bergomi M, Rovesti S et al (1995) Zinc, copper and zinc- or copper-dependent enzymes in human hypertension. Biol Trace Elem Res 49:97–106
Kok J, Van der Schoot C, Veldhuizen M, Wolterbeek HT (1993) The uptake of zinc by erythrocytes under near-physiological conditions. Biol Trace Elem Res 38:13–26
Tubek S (2006) Selected zinc metabolism parameters in relation to insulin, renin–angiotensin–aldosterone system and blood pressure in healthy subjects—gender differences. Biol Trace Elem Res 114:65–72
Tetef ML, Synold TW, Chow W, Leong L, Margolin K, Morgan R, Raschko J, Shibata S, Somlo G, Yen Y, Groshen S, Johnson K, Lenz HJ, Gandara D, Doroshow JH (2001) Phase I trial of 96-hour continuous infusion of dexrazoxane in patients with advanced malignancies. Clin Cancer Res 7:1569–1576
Cuajungco MP, Lees GJ (1997) Zinc metabolism in the brain: relevance to human neurodegenerative disorders. Neurobiol Dis 4:137–169
Yoo MH, Lee JY, Lee SE, Koh JY, Yoon YH (2004) Protection by pyruvate of rat retinal cells against zinc toxicity in vitro, and pressure-induced ischemia in vivo. Invest Ophthalmol Vis Sci 45:1523–1530
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Tubek, S. Zinc Supplementation or Regulation of its Homeostasis: Advantages and Threats. Biol Trace Elem Res 119, 1–9 (2007). https://doi.org/10.1007/s12011-007-0043-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12011-007-0043-7