Abstract
Background
Impaction bone grafting has been used for acetabular reconstruction in revision surgery. However, most series do not establish differences in survival in revisions with differing severity of bone loss.
Questions/purposes
We therefore determined (1) the survival rate for rerevision associated with varying degrees of bone loss; (2) the frequency with which bone graft resorption occurred; and (3) whether the reconstruction restored the anatomic center of rotation of the hip.
Methods
We retrospectively reviewed 165 patients (181 hips) who underwent rerevision for major bone loss. Using the classification of Paprosky et al. 98 hips had a Grade 3A defect and 83 a Grade 3B. We determined survival rates for revision and graft resorption. Cup position was determined measuring vertical and horizontal positions and the distance from the center of the prosthetic femoral head to the normal center of rotation of the hip in both groups according to Ranawat. The minimum followup until rerevision or the latest evaluation was 0.3 years months (mean, 7.5 years; range, 0.3–17.7 years).
Results
The survival rate for revision at 8 years was 84% (95% confidence interval: 61–100) for Grade 3A and 82% (95% confidence interval: 68–100) for Grade 3B. Twelve hips were rerevised. Seventeen grafts showed bone resorption. Acetabular cup position was anatomically restored in both Grades 3A and 3B.
Conclusions
The midterm results for impacted bone allograft and cemented all-polyethylene cups were similar in both Grade 3A and Grade 3B hips. Acetabular reconstruction allows anatomic positioning of the cups and is associated with a low rate of rerevision.
Level of Evidence
Level IV, therapeutic study. See Guidelines for Authors for a complete description of levels of evidence.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The use of a cementless cup in acetabular revision surgery has low rates of loosening [35, 37, 38, 51], especially in hips with a minor defect affecting less than 30–50% of the host-bone bed. However, biologic fixation of a cementless porous-coated component is unlikely when over 50% of the host bone-bed has been lost [17, 23, 32]; the amount of porous coating in contact with living host-bone then is often limited and bone ingrowth fixation is not obtained [23]. Other surgical techniques include structural allograft with either cementless or cemented cups, implantation of nonhemispheric cementless cups (triflanged, oblong cups), new biomaterials such as tantalum cups and devices, or antiprotrusio cages. Midterm results of these different techniques vary [2, 12, 16, 28, 32].
Impacted morselized bone allograft and cement in the acetabulum have been used in revision surgery [13, 18, 45, 48] and bone graft incorporation has been reported in histologic studies [5, 41, 44, 47]. In a goat model of impacted allografts, Schimmel et al. [41] showed complete incorporation of the allograft by 48 weeks. Studying 24 human acetabular biopsies after reconstruction, Van der Donk et al. report similar findings [53]. However, most series regarding impaction bone grafting in acetabular revision surgery do not consider differences between bone defects of differing severity.
We therefore determined (1) the survival rate for rerevision associated with varying degrees of bone loss; (2) the frequency with which bone graft resorption occurred; (3) whether the reconstruction restored the anatomic center of rotation of the hip; and (4) the functional scores and complications related to this technique.
Patients and Methods
We retrospectively reviewed all 188 patients (208 hips) revised for aseptic loosening of a cemented or uncemented cup with a large defect without pelvic discontinuity between 1992 and 2003 with followup until rerevision or a minimum of 5 years. The average time between the initial total hip replacement (THA) and the revision acetabular surgery was 76 months (range, 38–194 months). Twenty-three patients (27 hips) were excluded: nine patients died for reasons unrelated to the revision surgery, 13 (17 hips) were lost to followup, and one had a deep infection (0.5%) although he was included in the rerevision survivorship analysis. These exclusions left 165 patients (181 hips). Acetabular bone status was classified during the operation according to the criteria of Paprosky et al. [38] as Grade 3A (98 hips) and Grade 3B (83 hips). A first revision surgery was more frequent in hips with Type 3A bone defects, whereas metallic meshes were more frequently used in bone Type 3B defects (Table 1). Minimum followup for the 181 hips until rerevision or the latest evaluation was 0.3 years (mean, 7.5 years; range, 0.3–17.7 years).
Different cemented (104 hips) and cementless (77 hips) THAs were revised in this series. Each revised cup was individually assessed; 70 (39%) only underwent acetabular revision, whereas 111 (61%) underwent revision of both components. Cemented stems (Exeter; Stryker, Howmedica International, Newbury, UK) were used with bone impaction grafting in 68 hips; cementless stems used were: Solution (Johnson & Johnson, DePuy, Warsaw, IN) in 31, Wagner (Zimmer, Warsaw, IN) in four, and others in eight hips.
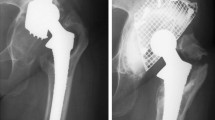
We used a posterolateral approach in all hips. Acetabular cup and cement were removed and the membrane excised and sent for histologic and bacteriologic study. The acetabular margins were defined and the cup always positioned as close to the center of hip rotation as possible. In revision surgery with large bone defects, use of the transverse acetabular ligament is not practical, and the obturator foramen is always a good reference for positioning the cup inferiorly and medially. Before impacting the morselized bone allograft and cement, segmental acetabular defects were reconstructed with metallic meshes screwed to the bone bed (Fig. 1). Until 1997, we implanted thin Vitallium meshes using ASIF miniscrews. Afterwards, we used special meshes designed for this technique (X-change; Stryker, Howmedica International, Staines, Middlesex, UK). Fresh-frozen femoral head allograft from the bone bank was used in all hips. Allograft bone chips were morselized with a bone mill (Lere Bone Mill; Johnson & Johnson, DePuy) or manually using a rongeur with a size of 0.7 to 1 cm2 and impacted with a trial prosthesis socket from X-Change instruments (Stryker, Howmedica International) according to the Nijmegen technique [26, 48]. The acetabulum was cleaned and filled with a substantial layer of bone graft to a thickness of at least 5 mm [50]. An all-polyethylene cup was cemented using antibiotic-loaded bone cement (Palacos with gentamicin; Merck, Darmstadt, Germany). The standard low-profile socket was used in almost all cases (Stryker, Howmedica International). In cases in which a well-fixed Charnley stem was associated with a loosened 22.25-mm Charnley cup, a Charnley cemented cup (Johnson & Johnson, DePuy) was used (25 hips).
Postoperative radiograph of the hip of a 57-year-old woman taken at the seventh year followup examination shows a segmental acetabular defect treated with impacted bone graft and cement. A metallic mesh with screws was used to reconstruct the acetabulum. The cup is stable, the bone graft is incorporated, and the patient has a good clinical result.
The postoperative management in our early patients included bed rest for 14 days. Beginning in 1997, patients spent 5 days in bed with the leg in abduction, and then, depending on intraoperative bone quality and the resulting reconstruction of the acetabulum (and frequently the femur), they were allowed to walk with partial weightbearing using crutches or a walker at 6 weeks with full weightbearing after 3 months. Antibiotic prophylaxis (1 g cefazolin every 6 hours) was discontinued at 48 hours. Subcutaneous heparin was used as a routine preventive measure for thromboembolic problems until the patients were fully mobile.
Clinical evaluation assessed pain, function, and motion following the Merle D’Aubigné and Postel scale (range 1–6) [31] at every followup examination: 6 weeks, 12 weeks, 6 months, 1 year, and annually thereafter. Levels 5 and 6 are considered a good clinical result and levels 4 and lower, a poor result [31]. Clinical failure was defined as rerevision or removal of the cup, pain (level 4 or worse), or both. Thigh pain was not considered evidence of clinical acetabular failure, although groin and buttock pain were recorded as signs of clinical failure resulting from acetabular loosening [39].
Standard AP and lateral radiographs of the pelvis were made for all patients immediately after the operation and every followup examination. All postoperative and followup radiographs were made at our institution following the same protocol [24]. Measurements were made by a single author (EGR) who had not been involved in the surgery. The locations of radiolucent lines around the cup were recorded using the DeLee and Charnley zones [11]. The preoperative and postoperative positions of the cup were assessed by determining the acetabular inclination of the cup. The center of rotation of the hip was defined using the center of the femoral head and the interteardrop line or obturator foramina. The true acetabular region (TAR) was defined as a right-angled triangle whose height and width are equal to 20% of the height of the pelvis according to Ranawat et al. [40]. The hypotenuse of the triangle is the diameter of the mouth of the acetabulum and its midpoint coincides with the approximate femoral head center (AFHC), the center of rotation of the hip. The AFHC was used as the reference point to measure distances between the center of rotation of the patient’s normal hip and the center of the prosthetic femoral head (CPFH). These distances were recorded for each hip (Fig. 2). If the CPFH was initially superior or lateral to the TAR, the cup was defined as being outside the TAR and changes of over 5 mm in cup position in followup radiographs were compared with the immediate postoperative images. To facilitate the assessment of the radiolucent lines, regardless of their thickness, we used Hodgkinson et al. criteria [22]. Radiographic cup loosening was difficult to evaluate because of the frequent use of metallic meshes. However, cup migration was defined as change of more than 5º in the abduction acetabular angle or 5 mm in either in the height or lateral position of the cup. Radiographic cup loosening was defined based on Schmalzried and Harris criteria [42] and classified as definite loosening, probable loosening, and possible loosening. Although bone graft density, appearance of the graft-host junction, and trabecular continuity between bone graft and acetabular bone could be assessed by radiographs, these parameters are of limited usefulness in evaluating bone graft remodeling [21, 46]. The anatomic center of the hip was considered as reconstructed when the AFHC-CPFH distance was less than 5 mm.
Diagram showing the method for preoperative and postoperative measurements of the cup. The true acetabular region (TAR) is measured as the area enclosed by a right-angled triangle with the height and width (B) equal to 20% of the height of the pelvis (A). The midpoint of the hypotenuse of the triangle is defined as the approximate center of the femoral head (AFHC) and represents the normal center of rotation of the hip. CPFH indicates the center of the prosthetic femoral head and KK′ the Köhler line, which is drawn from the medial border of the ilium to the medial border of the ischium.
We used Kaplan-Meier survivorship analysis [25], with 95% confidence intervals to estimate the cumulative probability of not having a cup revision as well as the cumulative probability of not having cup loosening. All patients including lost hips were assessed. The “best-case” scenario curve was compared with the “worst-case” scenario curve [15, 33]. The former included patients who had been lost to followup but whose available data indicated a good result as success. The latter curve considered the patients who had been lost to followup as failures. Differences in survival were determined using the log-rank test. Analysis of the reconstruction of the anatomic center of the hips considered the inclination acetabular angle, height, and horizontal location of the center of the hip, as well as the AFHC-CPFH distance within each group and then between groups. Pre- and postoperative changes in the inclination angle, the height and location of the center of the hip, and/or the AFHC-CPHF distance between the two groups were compared using two-way analysis of variance of repeated measures factoring for Grade 3A and 3B hips. Statistical analysis was performed by statistical package SAS 9.1 (SAS Institute Inc, Cary, NC).
Results
The cumulative probability of not having a rerevision for any cause at 8 years was similar (p = 0.1143) in Grade 3A and Grade 3B (Fig. 3). If the patients excluded from the followup study were included (208 hips), the cumulative probability of not having a revision of any prosthetic component for any cause was 83.9% (95% confidence interval, 61.5%–100%) for 3A and 81.6% (95% confidence interval, 67.5%–95.6%) for 3B in the “best-case” scenario and 72.3% (95% confidence interval, 52.1%–92.6%) for 3A and 75.6% (95% confidence interval, 61.6%–89.6%) for 3B in the “worst-case” scenario at the same interval. There were 12 cup rerevisions, 11 for loosening and one for infection. Rerevised cups were less frequent in Grade 3A (four hips) than in Grade 3B (eight hips).The hip that failed because of septic loosening and another hip with severe dysplasia that failed because of aseptic loosening and major bone graft resorption were not reconstructed and were converted to permanent resection arthroplasties. In the other rerevised cups, a new reconstruction using impaction bone allografting was performed (Table 2).
Bone allograft resorption was difficult to evaluate when metallic mesh was used, but most hips had not migrated and showed uniform graft and host bone density. We observed possible loosening in six hips, probable loosening in two, and definite loosening in 12. All hips revised because of aseptic loosening presented major bone resorption. Three loosened hips were not revised because the symptoms were only mild. Bone resorption was more severe in Grade 3B hips (Table 2). Radiolucent lines were uncommon. Progression of radiolucent lines was infrequent (cup migration was seen in the rerevised cup). Demarcation was categorized as Type 0 when there were no radiolucent lines around the cup, as Type 1 when the line was in zone 1 of DeLee and Charnley [11], as Type 2 when it was in zones 1 and 2, as Type 3 when it was in all three zones, and as Type 4 when the acetabular cup had migrated (Table 3). The cumulative probability of not having probable or definite radiographic loosening at 8 years was greater (p = 0.0453) with Grade 3A than grade 3B (Fig. 4).
The horizontal and vertical distances from the center of the femoral head to the reference points and acetabular inclination angle improved after surgery in both grades. The surgery also improved distances between CPHF and the AFHC in both groups (Table 4; Fig. 5). The preoperative radiographs showed that only five hips (all with a 3A defect) had a AFHC-CPFH distance equal to or lower than 5 mm. Radiographic accurate reconstruction was more frequent (p = 0.004) in Grade 3A (40 hips) than in Grade 3B defect (17 hips). Although the postoperative AFHC-CPFH distance was less in the 3A hips than the other group, the change in distance was greater (p < 0.001) for the 3B hips, which also had the greater AFHC-CPFH preoperative distance (Fig. 6). Surgery was able to place most of the outside-the-TAR CPHF hips in both groups inside the TAR (Table 5).
(A) Preoperative radiograph in a 68-year-old woman showing the distance from the approximate femoral head center (AFHC) to the center of the prosthetic femoral head (CPFH). (B) Postoperative radiograph of the same patient showing the distance from the approximate femoral head center AFHC to the center of the prosthetic femoral head (CPFH).
Graph showing distances from the approximate femoral head center (AFHC) to the center of the prosthetic femoral head (CPFH) pre- and postoperatively in both Grade 3A and 3B. The postoperative AFHC-CPFH distance is less in the 3A hips than the other group. However, the change in distance is greater for the 3B hips, which also had the greater AFHC-CPFH preoperative distance.
There was an improvement in the functional score from a mean of 7.8 to 16.5 points. Mild pain (Level 4) was only present in rerevised hips. Postoperative complications included four dislocations, which were treated nonoperatively. A woman with rheumatoid arthritis had a deep infection and was included in the survival rerevision analysis.
Discussion
The use of a cementless cup used in acetabular revision surgery has low rates of loosening [35, 37, 51], especially in hips with a defect that affected less than 30% of the host-bone bed. Impacted morselized bone allograft and cement in the acetabulum have been used in revision surgery [13, 18, 37, 48] and bone graft incorporation has been reported in histologic studies [5, 41, 44, 47]. However, most series reporting impaction bone grafting in acetabular revision surgery do not establish differences between different defects of differing severities. We therefore determined (1) the survival rate for rerevision associated with varying degrees of bone loss; (2) the frequency with which bone graft resorption occurred; and (3) whether the reconstruction restored the anatomic center of rotation of the hip.
Our study has some limitations. First, although we have routinely used CT for preplanning since November 2003 [20], most of the hips in this study were operated on before then, so CT is not included in this series. Given radiographs can underestimate bone defects, we cannot ensure the severity of the defects was accurately ascertained, although they can be compared to bone loss in other studies using only radiographs. Second, we have only used conventional radiographs and they are inadequate for detecting migration of less than 4 to 6 mm [34]. Radiostereometric analysis (RSA) could have detected migration and rotation of the cup at an early stage and over time [34]. Third, we lacked a control group of patients of similar age and acetabular defects who were operated on with other techniques with which to compare our observations. Fourth, we lacked biopsies and autopsy retrieval of acetabula reconstructed with this technique to confirm the bone graft remodeling and new bone formation.
Rerevision rates in this series are similar to those obtained in other series using this technique (Table 6). Van Haaren et al. [54] report a high rate of failure by impaction bone grafting in large acetabular defects, including pelvic discontinuities. Our series excluded cases with pelvic discontinuity because major bone defects associated with pelvic discontinuity usually require complex acetabular reconstructive techniques using cages or plates, which effectively excluded them from this series [1]. Buttaro et al. [6] suggested metal mesh, impaction bone grafting, and a cemented acetabular component can be considered when reconstructing acetabular defects of medium severity, but severe combined deficiencies would be treated with an acetabular ring. Impaction bone allografting was used for reconstruction in most of the revised cups (10 of 12 cups). Like in other series [45], the impression at rerevision was that the original bone grafting had been incorporated, and a new bone impacting grafting was performed because part of the existing graft looked viable and well healed to the host-bone. Unfortunately, we did not make core biopsies in any case to confirm whether the bone was viable on the periphery of the graft.
Radiological assessment of bone graft resorption is difficult after the use of the impacted bone allograft with cement in an acetabular revision, but the cup and graft remodeling is clearly stable. Most hips presented uniform graft and host bone radiodensity. Histologic studies of cup loosening in humans report bone substitution, but at a slower rate than in animal models [5, 41, 44, 47]. Although bone graft resorption has been described in areas of substantial weightbearing [21], it is not common with this technique. Somers et al. [49] recommended using bulk allograft in very large defects. However, two other studies suggest bulk allografts are at risk for mechanical weakening during the process of creeping substitution whereas a strong buttress is needed [27, 30]. The open structure of the cancellous bone graft, associated with cement, permits good vascularization, and thus bone substitution takes place without mechanical loosening [48]. In an in vitro study Board et al. [3] found BNP-7 was released from the graft in proportion to the strain imposed, and suggested strain from vigorous graft impaction and postoperative load transformed bone allograft from osteoconductive to osteoinductive. Clinical studies using PET for evaluation of the spatial and temporal development of bone formation report that the impacted bone allograft had transformed to living bone in acetabular revision surgery [52]. Like in other series, radiolucent lines were quite infrequent in this series [46, 48].
Placing the acetabulum in the anatomic position is important for good long-term results [9, 19, 36, 40]. Theoretically, the location of the center of rotation of the hip affects the load and a higher and more medial position will result in greater loads than a lower position [56]. In this series, all the parameters for defining the reconstruction of the anatomic center of the hip showed improvement in both groups. These distances decreased in both groups after surgery, although the postoperative AFHC-CPFH distance is less in the 3A hips, the change in distance is greater for the 3B hips, which also had the greater AFHC-CPFH preoperative distance.
The midterm results for impacted bone allografts and cemented all-polyethylene cups were similar in both Grades 3A and 3B hips. Acetabular reconstruction allows us anatomic positioning of the cup and is associated with a low rate of rerevision due to graft resorption and cup loosening. We believe it reasonable to reconstruct the acetabulum using morselized bone allografts and cement when hips have an acetabular defect greater than 30% (Grades 3A and 3B), especially in young patients who will probably require a new cup revision at some time in their future. Continued followup will be required to determine if this technique results in less rerevision and loosening.
References
Berry DJ, Lewallen DG, Hanssen AD, Cabanela ME. Pelvic discontinuity in revision total hip arthroplasty. J Bone Joint Surg Am. 1999;81:1692–1702.
Berry DJ, Müller ME. Revision arthroplasty using an anti-protrusio cage for massive acetabular bone deficiency. J Bone Joint Surg Br. 1992;74:711–715.
Board TN, Rooney P, Kay PR. Strain imparted during impaction grafting may contribute to bony incorporation; An in vitro study of the release of BMP-7 from allograft. J Bone Joint Surg Br. 2008;90:821–824.
Buckley SC, Stockley I, Hamer AJ, Kerry RM. Irradiated allograft for acetabular revision surgery: results at a mean of five years. J Bone Joint Surg Br. 2005;87:310–313.
Buma P, Lamerigts N, Schreurs BW, Gardeniers J, Verslayen D, Slooff TJJH. Impacted graft incorporation after cemented acetabular revision. Histological evaluation in 8 patients. Acta Orthop Scand. 1996;67:536–540.
Buttaro MA, Comba F, Pusso R, Piccaluga F. Acetabular revision with metal mesh, impaction grafting, and a cemented cup. Clin Orthop Relat Res. 2008;466:2482–2490.
Comba F, Buttaro M, Pusso R, Piccaluga F. Acetabular reconstruction with impacted bone allografts and cemented acetabular components: a 2- to 13-year follow-up study of 142 aseptic revisions. J Bone Joint Surg Br. 2006;88:865–869.
Comba F, Buttaro M, Pusso R, Piccaluga F. Acetabular revisión surgery with impacted bone allograft and cemented cups in patients younger than 55 years. Inter Orthop (SICOT). 2009;33:611–616.
Crowninshield RD, Brand RA, Pedersen DR. A stress analysis of acetabular reconstruction in protrusion acetabuli. J Bone Joint Surg Am. 1983;65:495–499.
Deakin DE, Bannister G. Graft incorporation after acetabular and femoral impaction grafting with washed irradiated allograft and autologous marrow. J Arthroplasty. 2007;22:89–94.
DeLee JG, Charnley J. Radiological demarcation of cemented sockets in total hip arthroplasty. Clin Orthop Relat Res. 1976;121:20–32.
Dennis DA. Management of massive acetabular defects in revision total hip arthroplasty. J Arthroplasty. 2003;18(Suppl 1):121–125.
El-Kawy S, Hay D, Drabu K. Clinical and radiological bone allograft technique results of impaction in acetabular revisions associated with massive bone stock deficiencies: four to seven years follow-up study. Hip Int. 2005;15:46–51.
Emms NW, Buckley SC, Stockley I, Hamer AJ, Kerry RM. Mid- to long-trem results of irradiated allograft in acetabular reconstruction. A follow-up report. J Bone Joint Surg Br. 2009; 91:1419–1423.
Font-Rodriguez DE, Scuderi GR, Insall JN. Survivorship of cemented total knee arthroplasty. Clin Orthop Relat Res. 1997;345:79–86.
Garbuz D, Morsi E, Gross AE. Revision of the acetabular component of a total hip arthroplasty with a massive structural allograft: study with a minimum five-year follow-up. J Bone Joint Surg Am. 1996;78:693–697.
Garcia-Cimbrelo E. Porous-coated cementless acetabular cups in revision surgery. A 6- to 11-year follow-up study. J Arthroplasty. 1999;14:397–406.
Garcia-Cimbrelo E, Cordero J. Impacted morsellised allograft and cemented cup in acetabular revision surgery. A five to nine year follow-up study. Hip Int. 2002;12:281–288.
Garcia-Cimbrelo E, Diaz-Martin A, Madero R, Munuera L. Loosening of the cup after low-friction arthroplasty in patients with acetabular protrusion. The importance of the position of the cup. J Bone Joint Surg Br. 2000;82:108–115.
Garcia-Cimbrelo E, Tapia M, Martín-Hervás C. Multislice computed tomography for evaluating acetabular defects in revision THA. Clin Orthop Relat Res. 2007;463:138–143.
Gerber SD, Harris WH. Femoral head autografting to augment acetabular deficiency in patients requiring total hip replacement: a minimum five-year and an average seven-year follow-up study. J Bone Joint Surg Am. 1986;68:1241–1248.
Hodgkinson JP, Shelley P, Wroblewsky BM. The correlation between the roentgenographic appearance and operative findings at the bone-cement junction of the socket in Charnley low-friction arthroplasties. Clin Orthop Relat Res. 1988;228:105–109.
Hooten JP Jr, Engh CA Jr, Engh CA. Failure of structural acetabular allografts in cementless revision hip arthroplasty. J Bone Joint Surg Br. 1994;76:419–422.
Johnston RC, Fitzgerald RH Jr, Harris WH, Poss R, Müller ME, Sledge CB. Clinical and radiographic evaluation of total hip replacement: a standard system of terminology for reporting results. J Bone Joint Surg Am. 1990;72:161–168.
Kaplan EL, Meier P. Nonparametric estimation from incomplete observations. J Am Stat Assoc. 1958;53:457–481.
Kinzinger PJ, Karthaus RP, Slooff TJ. Bone grafting for acetabular protrusion in hip arthroplasty. 27 cases of rheumatoid arthritis followed for 2 to 8 years. Acta Orthop Scand. 1991;62:110–112.
Knight J, Fujii K, Atwater R, Grothaus L. Bone-grafting for acetabular deficiency during primary and revision total hip arthroplasty: a radiographic and clinical analysis. J Arthroplasty. 1993;8:371–382.
Lakstein D, Backstein D, Safir O, Kosashvili Y, Gross AE. Trabecular MetalTM cups for acetabular defects with 50% or less host bone contact. Clin Orthop Relat Res. 2009;467:2318–2324.
Mehendele S, Learmonth ID, Smith EJ, Nedungayil S, Maheshwarf R, Hassaballa MA. Use of irradiate bone graft for impaction grafting in acetabular revision surgery: a review of fifty consecutive cases. Hip Int. 2009; 9:114–119.
Mendes DG, Roffman M, Silbermann M. Reconstruction of the acetabular wall with bone graft in arthroplasty of the hip. Clin Orthop Relat Res. 1984;186:29–37.
Merle D’Aubigné R, Postel M. Functional results of hip arthroplasty with acrylic prosthesis. J Bone Joint Surg Am. 1954;36:451–475.
Morsi E, Garbuz D, Gross AE. Total hip arthroplasty with shelf grafts using cemented cups. A long-term follow-up study. J Arthroplasty. 1996;11:81–85.
Murray DW, Britton AR, Bulstrode CJK. Loss to follow-up matters. J Bone Joint Surg Br. 1997;79:254–257.
Ornstein E, Franzén H, Johnsson R, Stefánsdóttir A, Sundberg M, Tägil M. Five-year follow-up of socket movements and loosening after revision with impacted morselized allograft bone and cement. A radiostereometric and radiographic analysis. J Arthroplasty. 2006;21:975–984.
Padgett DE, Kull L, Rosenberg A, Sumner DR, Galante JO. Revision of the acetabular component without cement after total hip arthroplasty. Three to six-year follow-up. J Bone Joint Surg Am. 1993;75:663–673.
Pagnano MW, Hanssen AD, Lewallen DG, Shaughnessy WJ. The effect of superior placement of the acetabular component on the rate of loosening after total hip arthroplasty: long-term results in patients who have Crowe type-II congenital dysplasia of the hip. J Bone Joint Surg Am. 1996;78:1004–1014.
Paprosky WG, Magnus RE. Principles of bone grafting in revision total hip arthroplasty: acetabular technique. Clin Orthop Relat Res. 1994;298:147–155.
Paprosky WG, Perona PG, Lawrence JM. Acetabular defect classification and surgical reconstruction in revision arthroplasty: a 6-year follow-up evaluation. J Arthroplasty. 1994;9:33–44.
Pupparo F, Engh CA. Comparison of porous-threaded and smooth-threaded acetabular components of identical design. Two- to four-year results. Clin Orthop Relat Res. 1991;271:201–206.
Ranawat CS, Dorr LD, Inglis AE. Total hip arthroplasty in protrusio acetabuli of rheumatoid arthritis. J Bone Joint Surg Am. 1980;62:1059–1065.
Schimmel JW, Buma P, Versleyen D, Huiskes R, Slooff TJJH. Acetabular reconstruction with impacted morcellized cancellous allografts in cemented hip arthroplasty: a histologic and biomechanical study on the goat. J Arthroplasty. 1998;13:438–448.
Schmalzried TP, Harris WH. The Harris-Galante porous-coated acetabular component with screw fixation: radiographic analysis of eighty-three primary hip replacement at a minimum of five years. J Bone Joint Surg Am. 1992;74:1130–1139.
Schreurs BW, Bolder SBT, Gardeniers JWM, Verdonschot N, Slooff TJJH, Veth RPH. Acetabular revision with impacted moresllised cancellous bone grafting and a cemented cup. A 15- to 20-year follow-up. J Bone Joint Surg Br. 2004;86:492–497.
Schreurs BW, Buma P, Huiskes R, Slagter JL, Slooff TJ. Morselized allografts for fixation of the hip prosthesis femoral component: a mechanical and histological study in the goat. Acta Orthop Scand. 1994;65:267–275.
Schreurs BW, Keurentjes JC, Gardeniers JWM, Verdonschot N, Slooff TJJH, Veth RPH. Acetabular revision with impacted morsellised cancellous bone grafting and a cemented acetabular component. A 20- to 25-year follow-up. J Bone Joint Surg Br. 2009;91:1148–1153.
Schreurs BW, Slooff TJJH, Buma P, Gardeniers JWM, Huiskes R. Acetabular reconstruction with impacted morselized cancellous bone graft and cement. A 10- to 15-year follow-up of 60 revision arthroplasties. J Bone Joint Surg Br. 1998;80:391–395.
Singer GC, Muirhead-Allwood SK. The histology of impacted cancellous allograft in acetabular reconstruction. Hip Int. 1999;9:20–24.
Slooff TJJH, Schimmel JW, Buma P. Cemented fixation with bone grafts. Orthop Clin North Am. 1993;24:667–677.
Somers JFA, Timperley AJ, Norton M, Taylor R, Gie GA. Block allografts in revision total hip arthroplasty. J Arthroplasty. 2002;17:562–568.
Somford MP, Bolder SBT, Gardeniers JWM, Slooff TJJH, Schreurs BW. Favorable survival of acetabular reconstruction with bone impaction grafting in dysplastic hips. Clin Orthop Relat Res. 2008;466:359–365.
Tanzer M, Drucker D, Jasty M, McDonald M, Harris WH. Revision of the acetabular component with an uncemented Harris-Galante porous-coated prosthesis. J Bone Joint Surg Am. 1992;74:987–994.
Ullmark G, Sörensen J, Nilsson O. Bone healing of severe acetabular defects after revision arthroplasty. A clinical positron emission tomography study of 7 cases. Acta Orthop. 2009;80:179–183.
Van der Donk S, Buma P, Slooff TJJH, Gardeniers JWM, Schreurs BW. Incorporation of moreselized bone grafts: a study of 24 acetabular biopsy specimens. Clin Orthop Relat Res. 2002;396:131–141.
Van Haaren EH, Heyligers IC, Alexander FGM, Wuisman PIJM. High rate of failure of impaction grafting in large acetabular defects. J Bone Joint Surg Br. 2007;89:296–300.
Wang J-W, Fong C-Y, Su Y-S, Yu H-N. Acetabular revisión with morsellised allogenic bone graft and a cemented metal-backed component. J Bone Joint Surg Br. 2005;88-B:586–591.
Yoder SA, Brand RA, Pedersen DR, O’Gorman TW. Total hip acetabular component position affects component loosening rates. Clin Orthop Relat Res. 1984;186;29–37.
Acknowledgments
We thank Rosario Madero-Jarabo, PhD, Mth Statistic, for the statistical analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
Each author certifies that he or she has no commercial associations (eg, consultancies, stock ownership, equity interest, patent/licensing arrangements, etc) that might pose a conflict of interest in connection with the submitted article.
Each author certifies that his or her institution has approved the human protocol for this investigation, that all investigations were conducted in conformity with ethical principles of research, and that informed consent was obtained.
This work was performed at Hospital La Paz, Madrid, Spain.
About this article
Cite this article
Garcia-Cimbrelo, E., Cruz-Pardos, A., Garcia-Rey, E. et al. The Survival and Fate of Acetabular Reconstruction With Impaction Grafting for Large Defects. Clin Orthop Relat Res 468, 3304–3313 (2010). https://doi.org/10.1007/s11999-010-1395-4
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-010-1395-4