Abstract
We analyzed anatomic distribution of the radial nerve in the upper arms in Chinese-adult embalmed cadavers (120 nerves in 60 cadavers) and compared it with findings reported for Caucasian adults. The acromion, the medial epicondyle, and the lateral epicondyle were used as bony landmarks. We used previously described techniques to quantitatively describe the location of the radial nerve in relation to the surrounding skeleton. Courses of the radial nerve relative to the humeral shaft in Chinese subjects differed from those previously reported for Caucasian subjects. The parameters that differed from Caucasians were: the distances from the acromion to the upper margin (147 ± 21 mm versus 124 ± 12 mm), the acromion to the lower margin (195 ± 36 mm versus 176 ± 17 mm), and the medial epicondyle to the lower margin (111 ± 21 mm versus 131 ± 10 mm). Our study provides information to help identify the radial nerve during surgery and elucidates racial differences in the distribution of the radial nerve between Chinese and Caucasian populations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The radial nerve is one of the terminal branches of the posterior cord of the brachial plexus. It descends behind the third part of the axillary artery and the upper part of the brachial artery and passes in front of the subscapularis and the tendons of the latissimus dorsi and teres major. It is located between the deep brachial artery and the long head of the triceps. The nerve then courses inferiorly between the long and medial heads of the triceps entering the radial groove posterior aspect of the humerus. At this point, the radial nerve is vulnerable to injury if the humerus is fractured.
After coursing through the groove, the radial nerve enters the lateral intermuscular septum and is accompanied by the radial collateral branch of the deep brachial artery. It continues inferiorly between the brachialis and brachioradialis muscles and courses into the forearm crossing anterior to the capsule of the elbow. On reaching the front of the lateral epicondyle, it divides into branches, including the radial nerve proper and the muscular, cutaneous, articular, superficial, and deep terminal (posterior interosseous nerve) branches. The posterior interosseous nerve penetrates the supinator muscle (arcade of Frohse) [19] to innervate the extensor muscles of the brachium, forearm, and wrist [22].
The radial nerve crosses the posterior aspect of the humerus near its midpoint [13]. The site at which the nerve is most vulnerable to damage is near the junction of the middle and distal thirds of the humerus, as Holstein and Lewis [15], Bodner et al. [4], and Edwards and Kurth [11] have described. Rates of permanent radial nerve palsy after a posterior approach to the humerus are approximately 0% to 3% [2, 10, 15]. Surgeons must understand the anatomic relationships between the radial nerve and the bony landmarks of the humerus to avoid radial nerve injury during humeral shaft fracture internal fixation. However, two studies [8, 9] suggest some anatomic differences and variations among Chinese and Caucasian populations.
Therefore, we analyzed the anatomy of the radial nerve in the upper arms in Chinese adults (1) to define its position relative to the humerus to facilitate its identification during surgery and (2) to discover whether there are anatomic differences between Chinese and Caucasians regarding this nerve.
Materials and Methods
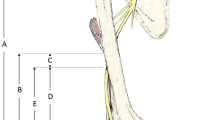
One of the authors (PHC) dissected 120 upper arms of 60 embalmed cadavers (8 women, 52 men) with 120 radial nerves. We chose this number arbitrarily without a prior power analysis. The arms of cadavers with identifiable scarring or trauma were excluded from our study. The middle points of the acromion, the medial epicondyle, and the lateral epicondyle were used as bony landmarks. In addition, the techniques described by Guse and Ostrum [13] were used as the basis for measurements of the radial nerve in relation to the surrounding skeleton (Fig. 1; Table 1): (1) Line A, from the acromion to the upper margin; (2) Line B, from the acromion to the lower margin; (3) Line C, from the medial epicondyle to the lower margin; (4) Line D, from the medial epicondyle to the upper margin; (5) Line E, from the lateral epicondyle to the lower margin; and (6) Line F, between the acromion and the lateral epicondyle (defined as humeral length).
The course of the radial nerve in relation to the humerus is viewed from the posterior aspect of the arm. Upper and lower margins are identified when the nerve pierces and leaves the posterior humerus, respectively. Line A = acromion to upper margin; Line B = acromion to lower margin; Line C = medial epicondyle to lower margin; Line D = medial epicondyle to upper margin; Line E = lateral epicondyle to lower margin; Line F = acromion to lateral epicondyle (defined as humeral length).
We considered data from the two radial nerves of one cadaver as independent sets of data. We then used an independent-samples t test to compare our mean data with those of Guse and Ostrum [13]. A p value less than 0.05 indicated a significant difference.
Results
We found differences (p < 0.05) in three of the six parameters defining distribution of the radial nerve around the humerus between Chinese and Caucasian subjects, especially in some parameters such as the distances from the acromion to the upper margin, from the acromion to the lower margin, and from the medial epicondyle to the lower margin (Table 1).
The mean humerus length was 287 mm, which was similar to the 302 mm reported by Guse and Ostrum [13]. The mean distance from the acromion to the upper margin was 147 mm and the mean distance to the lower margin was 195 mm (Line B). These findings differed from the 124 and 176 mm, respectively, reported by Guse and Ostrum [13]. The variation may be because the radial nerve traveled at a low position along the posterior aspect of the humerus. Mean distances from the medial epicondyle to the upper or lower margins were 161 mm (Line D) and 111 mm (Line C), respectively. Only the distance of Line C was different from the 131 mm reported by Guse and Ostrum [13]. The mean distance from the lateral epicondyle to the lower margin (104 mm, Line E) did not differ from the result of Guse and Ostrum [13] (126 mm).
The mean distance from the acromion to the upper margin was 147 mm (range, 114–204 mm). Therefore, the proximal safe zone was 11 cm, similar to the result of Guse and Ostrum [13] (10 cm). Distances from the lower margin to the medial and lateral epicondyles were 111 mm (range, 75–155 mm) and 104 mm (range, 60–156 mm), respectively. Therefore, the distal safe zone was 6 cm. This distance is less than the 10 cm reported by Guse and Ostrum [13].
Discussion
The radial nerve is at risk during surgical exposure. Therefore, comprehensive evaluation of the distribution of the radial nerve in the arm region is essential. The radial nerve may be at greatest risk with fractures of the middle [16, 17] or distal third of the humeral shaft [4, 15] owing to diminished mobility of the nerve where it pierces the lateral intermuscular septum [4, 5]. However, the incidence of iatrogenic injury to the radial nerve [7, 18] increases when the radial nerve runs along the posterior part of the humerus [4, 15]. We found its course along the humerus differs between Chinese and Western races.
Our study had some major limitations. First, although the same supine position is used for cadaveric dissections and for approaching humeral shaft fractures, extension or flexion of the elbow during surgery may allow better anatomic reduction or alignment when placing internal fixators. Therefore, changing positions for measurement might have introduced bias. Second, measurements were made in intact humeri. However, relationships to either or both margins change in fractured humeri that are surgically exposed, presumably because the radial nerve is tightly tethered to the lateral intermuscular septum [3, 13]. Third, we measured the nerve in embalmed cadavers, which may vary from the nerve live humans. Fourth, we considered the data from left and right arms as independent. Given normal symmetry, this assumption may be incorrect and thus overestimate the importance of the differences.
When treating humeral shaft fractures with internal or external fixators, reference points of the humeral head and the distal part of the olecranon fossa are not easy to identify even in open fractures because of the soft tissue covering around the shoulder or elbow. In clinical application, bony landmarks such as the tip of the acromion and the lateral epicondyle are easy to access and identify during surgery. Bono et al. [5] identified the length of the humerus as the true length from the head to the distal portion of the olecranon fossa. Guse and Ostrum [13], in contrast, defined the length of the entire humerus from the tip of the acromion to the lateral epicondyle.
In studies by Chao et al. [6] and Chapman et al. [7], the anterolateral approach was applied in the upper thirds of the humeral shaft and the posterior approach was used in fractures of the middle and distal thirds of the humerus [1, 12, 14, 20, 21]. The danger zone for plate fixation of fractures of the middle to distal thirds of the humerus, especially via the posterior approach, is where the nerve runs along the posterior aspect of the humerus.
We found the upper margin was located approximately in the middle of the humerus in reference to bony landmarks such as the acromion or the medial epicondyle. In contrast, the mean lower margin was never within 60 mm proximal to the lateral epicondyle. The mean pathway of the nerve along the posterior portion of the humerus was 50 mm (range, 22–120 mm). Therefore, surgeons can identify the distal margin in two ways. First, they can identify the middle point of the humerus and then extend approximately 5 cm distally. Second, they can identify the lateral epicondyle and then extend 6 cm proximally. Both ways allow clinicians to easily locate the distal margin when placing a dynamic compression plate to treat a humeral shaft fracture.
Six-, seven-, and eight-hole broad dynamic compression plates of the AO system (4.5-mm broad compression plate; Smith and Nephew, Memphis, TN) are commonly used to treat humeral shaft fractures [6, 7, 14, 18]; the lengths of these plates are 10.4, 11.9, and 13.5 cm, respectively. Each size of these plates is longer than the course along the posterior humerus. During internal fixation of a dynamic compression plate, the course of the radial nerve is easily encountered. By measuring the bony landmarks mentioned previously, surgeons can predict preoperatively if placement of the plate will interfere with the course of the radial nerve. Careful dissection with clear observation from the lateral intermuscular septum [3] from the proximal and distal aspects allows for displacement of the radial nerve and facilitates safe placement of the dynamic compression plate deep to it.
Intramedullary nailing and external fixation provide the advantages of preserving soft tissue around the fracture site [3, 6, 7, 18]. Although these techniques often involve closed reduction and percutaneous fixation, iatrogenic injury of the radial nerve still can result from insertion of a blind locking screw or external full or half pin.
After entering the lateral intermuscular septum, the radial nerve takes a superficial course and runs from the lateral to the anterior aspect of the humerus. The lower margin where the nerve pierces the lateral intermuscular septum is approximately from the middle to the distal fifth of the humerus. Placement of a locking screw or pin of the external fixator can directly injure the nerve. Owing to variability in the location of the lower margin (60–156 mm from either epicondyle), use of a small open incision for observation and protection with a sleeve are recommended when placing distal locking screws or fixator pins. The safe zone for placing a distal locking screw or external pin from lateral to medial is 60 mm within the lateral epicondyle, according to our results.
Owing to individualized variability, surgeons must carefully place any internal or external fixators used to treat different fractures of the humeral shaft. Our data illustrate variability of the course of the radial nerve and differences in the course of the nerve between Chinese and Caucasian adults. The information should help the clinician avoid iatrogenic injury during surgical procedures.
References
Archdeacon MT. Combined olecranon osteotomy and posterior triceps splitting approach for complex fractures of the distal humerus. J Orthop Trauma. 2003;17:368–373.
Bell MJ, Beauchamp CG, Kellam JK, McMurtry RY. The results of plating humeral shaft fractures in patients with multiple injuries: the Sunnybrook experience. J Bone Joint Surg Br. 1985;67:293–296.
Bodner G, Buchberger W, Schocke M, Bale R, Huber B, Harpf C, Gassner E, Jaschke W. Radial nerve palsy associated with humeral shaft fracture: evaluation with US: initial experience. Radiology. 2001;219:811–816.
Bodner G, Huber B, Schwabegger A, Lutz M, Waldenberger P. Sonographic detection of radial nerve entrapment within a humerus fracture. J Ultrasound Med. 1999;18:703–706.
Bono CM, Grossman MG, Hochmald N, Tornetta P 3rd. Radial and axillary nerves: anatomic considerations for humeral fixation. Clin Orthop Relat Res. 2000;373:259–264.
Chao TC, Chou WY, Chung JC, Hsu CJ. Humeral shaft fractures treated by dynamic compression plates, Ender nails and interlocking nails. Int Orthop. 2005;29:88–91.
Chapman JR, Henley MB, Agel J, Benca PJ. Randomized prospective study of humeral shaft fracture fixation: intramedullary nails versus plates. J Orthop Trauma. 2000;14:162–166.
Chen TH, Chen CH, Shyu JF, Wu CW, Lui WY, Liu JC. Distribution of the superficial temporal artery in the Chinese adult. Plast Reconstr Surg. 1999;104:1276–1279.
Chen TH, Shyu JF, Chen CH, Ma KH, Wu CW, Lui WY, Liu JC. Variations of the cystic artery in Chinese adults. Surg Laparosc Endosc Percutan Tech. 2000;10:154–157.
Dabezies EJ, Banta CJ 2nd, Murphy CP, d’Ambrosia RD. Plate fixation of the humeral shaft for acute fractures, with or without radial nerve injuries. J Orthop Trauma. 1992;6:10–13.
Edwards P, Kurth L. Postoperative radial nerve paralysis caused by fracture callus. J Orthop Trauma. 1992;6:234–236.
Gerwin M, Hotchkiss RN, Weiland AJ. Alternative operative exposures of the posterior aspect of the humeral diaphysis with reference to the radial nerve. J Bone Joint Surg Am. 1996;78:1690–1695.
Guse TR, Ostrum RF. The surgical anatomy of the radial nerve around the humerus. Clin Orthop Relat Res. 1995;320:149–153.
Hausman M, Panozzo A. Treatment of distal humerus fractures in the elderly. Clin Orthop Relat Res. 2004;425:55–63.
Holstein A, Lewis GM. Fractures of the humerus with radial-nerve paralysis. J Bone Joint Surg Am. 1963;45:1382–1388.
Kettelkamp DB, Alexander H. Clinical review of radial nerve injury. J Trauma. 1967;7:424–432.
Mast JW, Spiegel PG, Harvey JP Jr, Harrison C. Fractures of the humeral shaft: a retrospective study of 240 adult fractures. Clin Orthop Relat Res. 1975;112:254–262.
McCormack RG, Brien D, Buckley RE, McKee MD, Powell J, Schemitsch EH. Fixation of fractures of the shaft of the humerus by dynamic compression plate or intramedullary nail: a prospective, randomised trial. J Bone Joint Surg Br. 2000;82:336–339.
Ozturk A, Kutlu C, Taskara N, Kale AC, Bayraktar B, Cecen A. Anatomic and morphometric study of the arcade of Frohse in cadavers. Surg Radiol Anat. 2005;27:171–175.
Russell GV Jr, Jarrett CA, Jones CB, Cole PA, Gates J. Management of distal humerus fractures with minifragment fixation. J Orthop Trauma. 2005;19:474–479.
Uhl RL, Larosa JM, Sibeni T, Martino LJ. Posterior approaches to the humerus: when should you worry about the radial nerve? J Orthop Trauma. 1996;10:338–340.
Williams PL, Warwick R, Dyson M, Bannister LH (eds). Gray’s Anatomy. 37th ed. London, UK: Churchill Livingstone; 1989:1135–1136.
Author information
Authors and Affiliations
Corresponding author
Additional information
One or more of the authors (THC) have received funding from Taipei Veterans General Hospital, Taiwan, ROC (Grant V96-A-054).
Each author certifies that his or her institution has approved or waived approval for the reporting of this case and that all investigations were conducted in conformity with ethical principles of research.
About this article
Cite this article
Chou, PH., Shyu, JF., Ma, HL. et al. Courses of the Radial Nerve Differ Between Chinese and Caucasians. Clin Orthop Relat Res 466, 135–138 (2008). https://doi.org/10.1007/s11999-007-0019-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11999-007-0019-0