Abstract
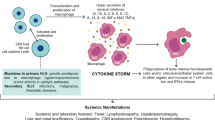
Macrophage activation syndrome (MAS), typically presenting beyond the first year of life, is an often lethal cousin of familial hemophagocytic lymphohistiocytosis (fHLH). Defects in natural killer (NK) cell and CD8 T cell cytotoxicity result in a pro-inflammatory cytokine storm, cytopenia, coagulopathy, and multi-organ system dysfunction. MAS can occur in association with infections (herpes viruses), cancer (leukemia), immune deficient states (post-transplantation), and in autoimmune (systemic lupus erythematosus) and autoinflammatory conditions (systemic juvenile idiopathic arthritis). The distinction between fHLH, the result of homozygous defects in cytolytic pathway genes, and MAS is becoming blurred with the identification of single or multiple mutations in the same cytolytic pathway genes in patients with later onset MAS. Here, we review the literature and present novel cytolytic pathway gene mutations identified in children with MAS. We study the inhibitory effect of one these novel mutations on NK cell function to suggest a direct link between fHLH and MAS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Macrophage activation syndrome (MAS) is quickly becoming a more recognized entity in both pediatric and adult hospital settings [1]. MAS is not a diagnosis of exclusion but can accompany infectious, oncologic, immunodeficiency, and rheumatic disorders [2•]. Among rheumatic diseases, MAS is most commonly seen in pediatrics in children with systemic juvenile idiopathic arthritis (sJIA), where it is believed by some to be inherent to the disease process in 40–50 % of cases, with approximately 10 % presenting clinically overtly [3, 4]. MAS is also seen in the related disorder, adult onset Still disease [5], but in adults it is more frequently seen in systemic lupus erythematosus (SLE) which is much more common [6•]. MAS also occurs in pediatric SLE [7•, 8] and in Kawasaki disease (KD) [9], along with a variety of other vaculitides and rheumatic disorders in children and adults [10•].
MAS is the terminology used by rheumatologists to refer to hemophagocytic lymphohistiocytosis (HLH) occurring in children and adults with rheumatic diseases. MAS, sometimes called reactive or secondary HLH, is likely similar to, if not the same disease process as, primary or familial HLH (fHLH), which typically occurs in the first year of life as a result of homozygous defects in cytolytic pathway genes [1, 2•]. As such, the diagnosis of fHLH can be made if there is a molecular diagnosis of homozygous or compound heterozygous mutations in the known associated HLH genes (Table 1), but usually the diagnosis is made by meeting 5 of 8 established criteria [11]. The HLH criteria reflect the clinical manifestations and associated laboratory abnormalities and include the following: fever, splenomegaly, peripheral cytopenia (2 or more lineages), hypertriglyceridemia or hypofibrinoginemia, hemophagocytosis on biopsy or in cerebrospinal fluid, low or absent natural killer (NK) cell activity, hyperferritinemia, and elevated soluble CD25 (interleukin-2 receptor alpha chain) [11]. In part, because MAS may not be initially as severe as fHLH in presentation, and since measurement of NK cell activity and soluble CD25 is frequently not readily available, criteria have been proposed to diagnosis MAS for rheumatic disorders.
For rheumatic diseases, preliminary diagnostic criteria have been put forth for establishing the diagnosis of MAS in the setting of sJIA [12]. These criteria overlap some of the HLH criteria (cytopenias and hypofibrinoginemia) but also include an elevated liver enzyme and 3 sets of clinical criteria (central nervous system dysfunction, hemorrhages, and hepatomegaly). Recently, an international effort is in the process of generating new MAS criteria for children with sJIA using a rigorous statistical modeling approach, including testing the criteria on large sets of real patient data [13•]. Related criteria efforts have also been attempted for pediatric lupus [14]. Whether or not a single scoring system for all forms of MAS/reactive HLH will be sensitive and specific enough is yet to be determined [15•].
Until recently, the restrictive nature of the HLH criteria for diagnosing non-fHLH forms of MAS has hindered the recognition and timely diagnosis of MAS in the hospital setting. While fHLH is rare occurring in approximately 1 in 50,000 live births [2•], MAS/reactive HLH is much more common as it can arise in the setting of infectious, oncologic, rheumatic, and immune deficient states [16, 17]. In fact, MAS is still likely vastly under-recognized, particularly in the intensive care unit (ICU) setting, where it may be labeled multiple organ dysfunction syndrome (MODS), systemic inflammatory response syndrome (SIRS), or culture negative sepsis [18]. The recognition of MAS in the ICU is particularly important, as treatment for MAS is often radically different (immunosuppression or chemotherapy) than broad spectrum antibiotic coverage, and mortality for these ICU syndromes is high [19]. Similarly, children with KD who share many features of MAS, have been labeled “shock syndrome” [20]. Again, it is important to realize that MAS in the setting of KD may require specific treatment such as interleukin-1 (IL-1) blockade [21•]. Until a more global set of diagnostic criteria for all forms of MAS are validated, in the setting of a febrile, ill-appearing patient, a very sensitive, inexpensive, and simple screening tool remains an elevated serum ferritin level [22, 23].
As MAS is more frequently being recognized and diagnosed, the question arises as to why some individuals with certain infections, malignancies, immunodeficiencies, and rheumatic disorders are prone to develop MAS and others are not. This selectivity implies that not only is the particular condition (e.g., H1N1 influenza) [24, 25] a risk factor for MAS but the individual’s genetically susceptible host immune response may also play an important role in the development of MAS. Most of the understanding of the pathophysiology of MAS has come from the study of animals spontaneously or genetically engineered to be deficient in the same cytolytic pathway genes as found in fHLH (Table 1) [2•, 26••, 27••, 28]. Although there are most likely multiple pathophysiologic pathways capable of leading to the end common pathway of MAS that do not require defects in lymphocyte cytolysis [29••], there are emerging data that subsets of MAS patients have partial defects in the same genes which are homozygous deficient in fHLH infants [27••]. An exploration of genetic defects in cytolytic pathway proteins in patients with MAS/secondary HLH is the focus of this review [30].
Cytolysis and MAS Pathophysiology
A current hypothesis as to the pathophysiology of HLH proposes that the inability of NK or CD8 T cells to lyse infected antigen-presenting cells (APC) leads to ongoing infection as well as an amplifying crosstalk of pro-inflammatory cytokines elicited by the APC and the lymphocyte ineffective in cytolysis [2•, 26••, 27••, 31]. The resultant “cytokine storm” contributes to hemophagocytosis by activated macrophages/histiocytes, multi-organ dysfunction, pancytopenia, coagulopathy, and eventual host demise. This has perhaps been best explored experimentally in an animal model of perforin deficiency [32]. These mice deficient in perforin-dependent target cell cytotoxicity are perfectly healthy until exposed to a particular virus, LCMV, and then they develop a rapidly fatal condition similar to HLH. Elimination of CD8 T cells prior to infection rescues the mice from death, as does blockade of the pro-inflammatory cytokine, interferon-gamma (IFN-γ) [32]. Interestingly, as little as 20 % wild-type (WT) perforin-expressing CD8 T cell chimerism is also able to ameliorate the HLH picture in these animals [33•]. As APCs are also critically important to the process of HLH [34], elimination of antigen-presenting dendritic cells (DC) can also protect against the HLH picture in perforin-deficient mice [35••]. It has recently been proposed that the severity of the lymphocyte killing defect in different mouse strains positively correlates with the severity of the HLH phenotype [26••]; it is therefore intriguing to speculate that a subset of human MAS presenting later in life than fHLH (infancy) may result from more subtle genetic defects in lymphocyte cytolysis.
Cytolysis and Genetics of MAS in sJIA
In humans, non-familial MAS has been most rigorously studied in children with sJIA. It has been known for some time that children with HLH and their first degree relatives have defects in NK cell function [36], but not long after it was also recognized that children with sJIA and MAS had similar NK cell dysfunction [37]. This is in part why it has been proposed that MAS not be considered a complication but rather an inherent aspect of disease in a substantial proportion of children with sJIA [3]. In studying one of the known HLH-associated genes, Grom and colleagues identified a haplotype of polymorphisms across the UNC13D gene (Table 1) which encodes for Munc13-4, a protein critical for getting the cytolytic perforin-containing vesicles to the NK cell immunologic synapse. This particular haplotype was notably over-represented in sJIA patients with MAS compared to controls, implying a genetic link of an established lymphocyte cytolytic pathway gene and MAS [38]. Moreover, a known fHLH causative mutation in UNC13D was identified in a patient with sJIA, suggesting a particular risk for MAS development [39].
Another HLH gene critical to lymphocyte cytolytic activity, PRF1, encoding the perforin protein (Table 1), was found to be mutated resulting in an amino acid change (A91V) in 20 % of a European population of sJIA patients with MAS; it was also present in 10 % of sJIA patients without known MAS versus approximately 3 % of the general population [40]. Because this mutation is so common in the overall population, some have suggested it is strictly a polymorphism [41]; however, more recent functional analyses of this mutation have shown perforin A91V to impair NK cell lytic activity (Cron et al., in preparation) [42•, 43–45]. Interestingly, at Children’s of Alabama (CoA), we have identified this same perforin A91V mutation in one of our MAS patients of unknown etiology (Table 2, patient #4) and in 2 of our immunodeficiency patients (Table 2, patients #9 and #10), both of whom had decreased NK cell function. Most recently, we identified the common perforin A91V mutation (Cron et al., in preparation) among the first 4 sequenced of a small cohort of fatal H1N1 influenza-infected adults with hemophagocytosis on autopsy [25]. Thus, single copy HLH gene mutations for both PRF1 and UNC13D are associated with, and may be capable of contributing to, MAS development in children with sJIA and children and adults with other unrelated disorders or infections.
HLH Gene Mutations in a Pediatric MAS Cohort
From February 2008 to February 2012, 28 individuals with MAS, plus 2 children with immunodeficiency and decreased NK cell function, were identified at CoA. Ten of these children were tested for NK cell dysfunction, and 8 of them (Table 2, patients #1, 3, 5, 6, 9, 10, 11, 12) had decreased cytolytic activity (patients #4, 7, 8 were not studied). Seventeen of these patients were screened at the discretion of the treating physician at the time of hospitalization for MAS (or in clinic for the 2 immunodeficiency patients) for 5 of the HLH associated genes (PRF1, UNC13D, STX11, STXBP2, RAB27A) (Table 1). A rather surprisingly high percentage (13/17 or 76 %) of these children was found to have at least one mutation among these 5 selected genes (Table 2). Among the 11 kids with MAS, 9 met ≥5 or more HLH criteria, one met 4 criteria (Table 2, patient #13), and one had mild MAS as part of sJIA (Table 2, patient #8). Of the entire cohort of 28 MAS patients (not including 2 immunodeficiency patients with HLH gene mutations, but including 15 who were not sequenced for HLH genes), 39 % had at least on HLH gene mutation. It is possible that this percentage would be higher if the entire cohort (15 more of the 28) were sequenced, but it is likely that the sickest kids were sequenced as 4 of those with HLH gene mutations died from MAS, whereas 24 others, including all those not sequenced, all survived (Table 2). Thus, confounding by indication may have identified the bulk of those with HLH gene mutations. Nevertheless, comparable numbers have recently been observed in Cincinnati (Grom et al., submitted) implying that many children with MAS may care a risk allele with a mutation of at least one of the classic HLH genes (Table 1). Similar reports of HLH gene mutations in 14 % of 175 adults with MAS/secondary HLH have also been reported, with almost half having the perforin A91V mutation [46••]. Thus, the distinction between primary/fHLH and secondary or reactive HLH/MAS is becoming genetically blurred.
In the cohort reported here (Table 2), as might be predicted, 3 of the 13 patients (23 %) possessed the relatively common (3 % of the North American general population) perforin A91V mutation (Table 2, patients # 4, 9, 10). However, the HLH genes most commonly mutated in this cohort were UNC13D and STXBP2 with 5 patients each (Table 2). Several of these mutations had not been previously described in the medical literature, including one Munc13-4 mutation (R966W) that was identified in two of the children, one with leukemia-associated MAS and the other with sJIA-associated MAS (Table 2, patients #1 and #6, respectively). Another mutation, Munc13-4 I283V (Table 2, patient #2), has previously been considered a benign polymorphism as it is present in 4 % of African-Americans, but it was recently reported as a cause of late onset fHLH in another cohort [47•]. The patient with the Munc13-4 I283V amino acid change in our cohort developed uveitis and spondyloarthritis after the MAS was clinically controlled. Intriguingly, a previously well 18-year-old female in our cohort (Table 2, patient #3) with a Rab27a A87P mutation also developed uveitis and spondyloarthritis after MAS resolution. This particular RAB27A mutation is a known cause of Griscelli-2 fHLH when present on both chromosomes [48]. We have recently found that over-expression of this RAB27A mutation in the NK-92 NK cell line [49] delays cytotoxic granule polarization to the immunologic synapse and dramatically lowers NK cell cytotoxicity (Zhang et al., in preparation). Thus, single copy variants of HLH genes (Table 1) likely contribute to late onset HLH/MAS via partial dominant negative or hypomorphic effects [46••] resulting in decreased lymphocyte cytolytic activity.
A Novel STXBP2 Mutation Decreases NK Cell Lytic Function
Intriguingly, 5 of the 13 patients in this cohort (Table 2) had mutations in STXBP2, the cause of fHLH5 (Table 1) [50]. A similar relative abundance of STXBP2 and UNC13D mutations was also recently noted in a group of 14 sJIA patients with MAS (Grom et al., submitted). In the current cohort (Table 2), many of the STXBP2 mutations were novel or had rarely been reported in association with HLH. Several of these mutations were present in non-coding regions, including 5’ and 3’ untranslated regions and RNA splice sites. It is possible that these non-coding mutations may alter Munc18-2 levels and thus diminish lymphocyte cytolytic function, as recent reports have demonstrated that mutations in intronic and transcriptional regulatory regions of HLH genes can contribute to HLH and immunodeficiency [51••, 52•]. Furthermore, a sizeable cohort of fHLH5 patients was reported with splice-site mutations in STXBP2 resulting in later onset HLH [53•]. Thus, it is believable that the STXBP2 splice-site mutations in the cohort reported here likely contributed to MAS, in particular for two of the patients with multiple STXBP2 mutations, one associated with the death of the child (Table 2, patients #12 and #13).
One of the novel STXBP2 mutations identified led to an amino acid change, Munc18-2 A433V, and was associated with decreased NK cell activity and the death of a child with MAS/secondary HLH (Table 2, patient #5). To test the plausibility that this single copy mutation contributed to MAS development, we first cloned the wild-type (WT) STXBP2 mutation into a lentiviral expression vector [54] that co-expressed a green fluorescent protein (GFP) for tracking transduced cells. Using site directed mutagenesis [54], we further generated a lentiviral construct expressing the novel Munc18-2 A433V patient mutation. The STXBP2 WT, mutant, or an empty lentiviral expression vector were independently transduced into the human NK cell line, NK-92 [49], and cells were sorted for GFP expression. These cells were co-cultured with fluorochrome-labeled K562 target cells [55] at increasing effector (NK-92) to target (K562) cell ratios, and cell lysis was determined using 7AAD staining by flow cytometry [56]. We repeatedly found that over-expression of WT Munc18-2 augmented NK cell lysis of K562 target cells compared to empty vector control, but over-expression of the Munc18-2 A433V mutant consistently and statistically significantly reduced NK cell lytic function (Fig. 1). These results confirmed the concept that a single copy HLH mutation may contribute to decreased NK cell function and serve as a risk for development of later age onset HLH or MAS.
Decreased cytolysis in NK cells overexpressing a novel MUNC18-2 mutation. NK-92 human NK cells (49) were transduced with a green fluorescent protein-expressing (GFP) lentiviral vector (z-368-ΔNP) co-expressing wild-type MUNC18-2 (squares), mutant MUNC18-2 (A433V) (triangles), or GFP alone (circles) under the control of the immediate–early cytomegalovirus transcriptional promoter. GFP + flow cytometry (FCM) sorted NK-92 cells were cultured with eFluor450-labeled K562 target cells at graded effector to target (E:T) cell ratios, and cell death was measured by 7AAD staining at 4 h post-incubation using FCM. Summary data (n = 3) are presented as means ± SEM percent cell lysis (cytotoxicity) along the Y-axis and increasing E:T ratio on the X-axis. All 3 conditions were statistically significantly different from one another (2-way ANOVA, p = 0.0005)
Conclusions
MAS belongs on the spectrum of fHLH and secondary or reactive HLH sharing many clinical, laboratory, and pathologic features. MAS is a consequence of a pro-inflammatory cytokine storm that results from a dysregulated immune response which can occur associated with a variety of infectious, oncologic, rheumatic, and immune deficient conditions. The frequently fatal condition of MAS/secondary HLH is still widely under-recognized and therefore undertreated in children and adults, particularly in the setting of the hospital ICU in patients with MODS. It is important to understand that MAS is an end common pathway from many disease states and not a diagnosis of exclusion. Until improved and timely diagnostic aids are developed, it is likely worth screening for MAS by serum ferritin levels in febrile acutely ill individuals.
In both children and adults, there is mounting evidence that genes associated with fHLH (Table 1) are found to be mutated in late onset HLH and MAS. Even single copy mutations have been shown to decrease NK cell cytolytic activity and thus likely directly contribute to the pathophysiology of MAS/secondary HLH. From the data presented in this present pediatric MAS cohort (Table 2), both the large number and varied HLH genes and individual mutations identified suggest causality rather than a simple association with MAS and decreased NK cell function. Moreover, the demonstration that over-expression of one of the novel STXBP2 mutations found in this MAS cohort experimentally decreased NK cell cytolytic function (Fig. 1) further strengthens this argument.
It is somewhat sobering to consider the fact that some of the identified MAS patient mutations are relatively frequent in the general population (up to 3–4 %) and likely contribute to MAS in a large variety of settings (intracellular infections, rheumatic conditions, leukemia, immune deficiency states). The association of the perforin A91V mutation with H1N1 influenza is a prime example of this discomforting concept. A large percentage of the general public is exposed to various infections, H1N1 influenza, for example. Many in the population will contract the infection, but only a subset of individuals will require hospitalization or die from the infection. In these cases, it is not only the infection that is a trigger, but it is the individual’s genetically determined immune response to the infection that can be lethal as a result of developing MAS. It is therefore not all that surprising that fHLH genes are found mutated in a substantial percentage of individuals identified with MAS and secondary HLH. In addition to the genetic risk, there may also be a second “hit” contributed by the infection, or, in the case of rheumatic diseases, a hyper-inflammatory state that results in MAS. Increased awareness of MAS, and knowledge of the genetic susceptibility for the development of MAS, are both likely to help combat the fatal nature of this more common than previously considered hyper-inflammatory disorder.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Filipovich AH. The expanding spectrum of hemophagocytic lymphohistiocytosis. Curr Opin Allergy Clin Immunol. 2011;11(6):512–6.
Janka GE. Familial and acquired hemophagocytic lymphohistiocytosis. Annu Rev Med. 2012;63:233–46. An up-to-date, thorough, and well written review on the topic of HLH.
Behrens EM, Beukelman T, Paessler M, Cron RQ. Occult macrophage activation syndrome in patients with systemic juvenile idiopathic arthritis. J Rheumatol. 2007;34(5):1133–8.
Bleesing J, Prada A, Siegel DM, Villanueva J, Olson J, Ilowite NT, et al. The diagnostic significance of soluble CD163 and soluble interleukin-2 receptor alpha-chain in macrophage activation syndrome and untreated new-onset systemic juvenile idiopathic arthritis. Arthritis Rheum. 2007;56(3):965–71.
Singh S, Samant R, Joshi VR. Adult onset Still's disease: a study of 14 cases. Clin Rheumatol. 2008;27(1):35–9.
Kumakura S, Murakawa Y. Clinical characteristics and treatment outcomes of autoimmune-associated hemophagocytic syndrome in adults. Arthritis Rheumatol. 2014. A large number (n = 116) of secondary HLH patients with underlying autoimmune diseases was used to identify risk factors (male sex, dermatomyositis, and anemia) associated with mortality.
Bennett TD, Fluchel M, Hersh AO, Hayward KN, Hersh AL, Brogan TV, et al. Macrophage activation syndrome in children with systemic lupus erythematosus and children with juvenile idiopathic arthritis. Arthritis Rheum. 2012;64(12):4135–42. Data from a large number of pediatric JIA (n = 102) and SLE (n = 19) patients with MAS suggested similar mortality rates in the two populations (6 and 11 %, respectively).
Pringe A, Trail L, Ruperto N, Buoncompagni A, Loy A, Breda L, et al. Macrophage activation syndrome in juvenile systemic lupus erythematosus: an under-recognized complication? Lupus. 2007;16(8):587–92.
Latino GA, Manlhiot C, Yeung RS, Chahal N, McCrindle BW. Macrophage activation syndrome in the acute phase of Kawasaki disease. J Pediatr Hematol Oncol. 2010;32(7):527–31.
Atteritano M, David A, Bagnato G, Beninati C, Frisina A, Iaria C, et al. Haemophagocytic syndrome in rheumatic patients. A systematic review. Eur Rev Med Pharmacol Sci. 2012;16(10):1414–24. Through a PUBMED literature search, 421 patients with HLH associated with rheumatic diseases were identified with most patients represented by sJIA and SLE.
Henter JI, Horne A, Arico M, Egeler RM, Filipovich AH, Imashuku S, et al. HLH-2004: Diagnostic and therapeutic guidelines for hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer. 2007;48(2):124–31.
Ravelli A, Magni-Manzoni S, Pistorio A, Besana C, Foti T, Ruperto N, et al. Preliminary diagnostic guidelines for macrophage activation syndrome complicating systemic juvenile idiopathic arthritis. J Pediatr. 2005;146(5):598–604.
Davi S, Consolaro A, Guseinova D, Pistorio A, Ruperto N, Martini A, et al. An international consensus survey of diagnostic criteria for macrophage activation syndrome in systemic juvenile idiopathic arthritis. J Rheumatol. 2011;38(4):764–8. Expert opinion from 232 physicians worldwide was used to identify the most useful clinical and laboratory criteria (hyperferritinemia, falling platelet count, hemophagocytosis in bone marrow) to develop improved diagnostic criteria for MAS in the setting of sJIA.
Parodi A, Davi S, Pringe AB, Pistorio A, Ruperto N, Magni-Manzoni S, et al. Macrophage activation syndrome in juvenile systemic lupus erythematosus: a multinational multicenter study of thirty-eight patients. Arthritis Rheum. 2009;60(11):3388–99.
Fardet L, Galicier L, Lambotte O, Marzac C, Aumont C, Chahwan D, et al. Development and validation of a score for the diagnosis of reactive hemophagocytic syndrome (HScore). Arthritis Rheumatol. 2014. Reactive HLH patient and control data were used to develop a numerical score (HScore) based on the presence of clinical, biological, and cytological variables in order estimate the risk of developing HLH.
Gupta S, Weitzman S. Primary and secondary hemophagocytic lymphohistiocytosis: clinical features, pathogenesis and therapy. Expert Rev Clin Immunol. 2010;6(1):137–54.
Park HS, Kim DY, Lee JH, Kim SD, Park YH, Lee JS, et al. Clinical features of adult patients with secondary hemophagocytic lymphohistiocytosis from causes other than lymphoma: an analysis of treatment outcome and prognostic factors. Ann Hematol. 2012;91(6):897–904.
Castillo L, Carcillo J. Secondary hemophagocytic lymphohistiocytosis and severe sepsis/ systemic inflammatory response syndrome/multiorgan dysfunction syndrome/macrophage activation syndrome share common intermediate phenotypes on a spectrum of inflammation. Pediatr Crit Care Med. 2009;10(3):387–92.
Typpo KV, Petersen NJ, Hallman DM, Markovitz BP, Mariscalco MM. Day 1 multiple organ dysfunction syndrome is associated with poor functional outcome and mortality in the pediatric intensive care unit. Pediatr Crit Care Med. 2009;10(5):562–70.
Kanegaye JT, Wilder MS, Molkara D, Frazer JR, Pancheri J, Tremoulet AH, et al. Recognition of a Kawasaki disease shock syndrome. Pediatrics. 2009;123(5):e783–9.
Miettunen PM, Narendran A, Jayanthan A, Behrens EM, Cron RQ. Successful treatment of severe paediatric rheumatic disease-associated macrophage activation syndrome with interleukin-1 inhibition following conventional immunosuppressive therapy: case series with 12 patients. Rheumatology (Oxford). 2011;50(2):417–9. The use of an IL-1 blocker was used to successfully treat 12 children with rheumatic disease and refractory MAS.
Allen CE, Yu X, Kozinetz CA, McClain KL. Highly elevated ferritin levels and the diagnosis of hemophagocytic lymphohistiocytosis. Pediatr Blood Cancer. 2008;50(6):1227–35.
Rosario C, Zandman-Goddard G, Meyron-Holtz EG, D'Cruz DP, Shoenfeld Y. The hyperferritinemic syndrome: macrophage activation syndrome, Still's disease, septic shock and catastrophic antiphospholipid syndrome. BMC Med. 2013;11:185.
Beutel G, Wiesner O, Eder M, Hafer C, Schneider AS, Kielstein JT, et al. Virus-associated hemophagocytic syndrome as a major contributor to death in patients with 2009 influenza A (H1N1) infection. Crit Care. 2011;15(2):R80.
Harms PW, Schmidt LA, Smith LB, Newton DW, Pletneva MA, Walters LL, et al. Autopsy findings in eight patients with fatal H1N1 influenza. Am J Clin Pathol. 2010;134(1):27–35.
Jessen B, Kogl T, Sepulveda FE, de Saint Basile G, Aichele P, Ehl S. Graded defects in cytotoxicity determine severity of hemophagocytic lymphohistiocytosis in humans and mice. Front Immunol. 2013;4:448. This study positively correlates the degree of HLH with the degree of defect in lymphocyte-mediated cytolysis in 6 different HLH prone mouse strains. Humans with biallelic defects in corresponding HLH genes revealed a similar severity gradient in HLH manifested by age of disease onset.
Ravelli A, Grom AA, Behrens EM, Cron RQ. Macrophage activation syndrome as part of systemic juvenile idiopathic arthritis: diagnosis, genetics, pathophysiology and treatment. Genes Immun. 2012;13(4):289–98. This timely review article thoughtfully covers the diagnostic criteria, genetic predisposition, the cell type and cytokine pathophysiology, and effective cytokine blockade treatment of MAS in the setting of children with sJIA.
Verbsky JW, Grossman WJ. Hemophagocytic lymphohistiocytosis: diagnosis, pathophysiology, treatment, and future perspectives. Ann Med. 2006;38(1):20–31.
Behrens EM, Canna SW, Slade K, Rao S, Kreiger PA, Paessler M, et al. Repeated TLR9 stimulation results in macrophage activation syndrome-like disease in mice. J Clin Invest. 2011;121(6):2264–77. A novel mouse model of MAS on a genetically normal background and not requiring infection was developed and used to study the pathophysiology of MAS.
Risma K, Jordan MB. Hemophagocytic lymphohistiocytosis: updates and evolving concepts. Curr Opin Pediatr. 2012;24(1):9–15.
Usmani GN, Woda BA, Newburger PE. Advances in understanding the pathogenesis of HLH. Br J Haematol. 2013;161(5):609–22.
Jordan MB, Hildeman D, Kappler J, Marrack P. An animal model of hemophagocytic lymphohistiocytosis (HLH): CD8+ T cells and interferon gamma are essential for the disorder. Blood. 2004;104(3):735–43.
Terrell CE, Jordan MB. Mixed hematopoietic or T-cell chimerism above a minimal threshold restores perforin-dependent immune regulation in perforin-deficient mice. Blood. 2013;122(15):2618–21. Using the perforin-deficient murine model of HLH, the authors show that only 10–20 % chimeric WT perforin-sufficient T cells are required to reduce HLH and prolong survival.
Behrens EM. Macrophage activation syndrome in rheumatic disease: what is the role of the antigen presenting cell? Autoimmun Rev. 2008;7(4):305–8.
Terrell CE, Jordan MB. Perforin deficiency impairs a critical immunoregulatory loop involving murine CD8(+) T cells and dendritic cells. Blood. 2013;121(26):5184–91. Perforin-dependent lysis of antigen presenting dendritic cells by cytotoxic CD8 T cells is critical for maintaining immune regulation in an animal model of HLH.
Sullivan KE, Delaat CA, Douglas SD, Filipovich AH. Defective natural killer cell function in patients with hemophagocytic lymphohistiocytosis and in first degree relatives. Pediatr Res. 1998;44(4):465–8.
Grom AA, Villanueva J, Lee S, Goldmuntz EA, Passo MH, Filipovich A. Natural killer cell dysfunction in patients with systemic-onset juvenile rheumatoid arthritis and macrophage activation syndrome. J Pediatr. 2003;142(3):292–6.
Zhang K, Biroschak J, Glass DN, Thompson SD, Finkel T, Passo MH, et al. Macrophage activation syndrome in patients with systemic juvenile idiopathic arthritis is associated with MUNC13-4 polymorphisms. Arthritis Rheum. 2008;58(9):2892–6.
Hazen MM, Woodward AL, Hofmann I, Degar BA, Grom A, Filipovich AH, et al. Mutations of the hemophagocytic lymphohistiocytosis-associated gene UNC13D in a patient with systemic juvenile idiopathic arthritis. Arthritis Rheum. 2008;58(2):567–70.
Vastert SJ, van Wijk R, D'Urbano LE, de Vooght KM, de Jager W, Ravelli A, et al. Mutations in the perforin gene can be linked to macrophage activation syndrome in patients with systemic onset juvenile idiopathic arthritis. Rheumatology (Oxford). 2010;49(3):441–9.
Zur Stadt U, Beutel K, Weber B, Kabisch H, Schneppenheim R, Janka G. A91V is a polymorphism in the perforin gene not causative of an FHLH phenotype. Blood. 2004;104(6):1909. author reply 1910.
Martinez-Pomar N, Lanio N, Romo N, Lopez-Botet M, Matamoros N. Functional impact of A91V mutation of the PRF1 perforin gene. Hum Immunol. 2013;74(1):14–7. The most recent report supporting decreased cytolytic activity of NK cells expressing the common perforin A91V mutation.
Trambas C, Gallo F, Pende D, Marcenaro S, Moretta L, De Fusco C, et al. A single amino acid change, A91V, leads to conformational changes that can impair processing to the active form of perforin. Blood. 2005;106(3):932–7.
Voskoboinik I, Sutton VR, Ciccone A, House CM, Chia J, Darcy PK, et al. Perforin activity and immune homeostasis: the common A91V polymorphism in perforin results in both presynaptic and postsynaptic defects in function. Blood. 2007;110(4):1184–90.
Voskoboinik I, Thia MC, Trapani JA. A functional analysis of the putative polymorphisms A91V and N252S and 22 missense perforin mutations associated with familial hemophagocytic lymphohistiocytosis. Blood. 2005;105(12):4700–6.
Zhang K, Jordan MB, Marsh RA, Johnson JA, Kissell D, Meller J, et al. Hypomorphic mutations in PRF1, MUNC13-4, and STXBP2 are associated with adult-onset familial hemophagocytic lymphohistiocytosis. Blood. 2011;118(22):5794–8. A significant percentage (14 %) of adult patients from a large cohort with HLH (n = 175) were found to have mutations in 3 of the fHLH genes leading to the credence that these genes contribute to late onset HLH.
Sumegi J, Barnes MG, Nestheide SV, Molleran-Lee S, Villanueva J, Zhang K, et al. Gene expression profiling of peripheral blood mononuclear cells from children with active hemophagocytic lymphohistiocytosis. Blood. 2011;117(15):e151–60. Gene expression profiling from 11 children with untreated HLH revealed decreased expression of NK cell function while showing increased expression of some of the pro-inflammatory cytokines (IL-1, IL-6).
Menasche G, Pastural E, Feldmann J, Certain S, Ersoy F, Dupuis S, et al. Mutations in RAB27A cause Griscelli syndrome associated with haemophagocytic syndrome. Nat Genet. 2000;25(2):173–6.
Gong JH, Maki G, Klingemann HG. Characterization of a human cell line (NK-92) with phenotypical and functional characteristics of activated natural killer cells. Leukemia. 1994;8(4):652–8.
Cote M, Menager MM, Burgess A, Mahlaoui N, Picard C, Schaffner C, et al. Munc18-2 deficiency causes familial hemophagocytic lymphohistiocytosis type 5 and impairs cytotoxic granule exocytosis in patient NK cells. J Clin Invest. 2009;119(12):3765–73.
Cichocki F, Schlums H, Li H, Stache V, Holmes T, Lenvik TR, et al. Transcriptional regulation of Munc13-4 expression in cytotoxic lymphocytes is disrupted by an intronic mutation associated with a primary immunodeficiency. J Exp Med. 2014. Demonstration that a fHLH mutation that disrupts transcription factor engagement of a UNC13D transcriptional enhancer in intron 1 results in decreased NK cell cytolytic activity and shows that mutations outside the coding sequence of fHLH genes can alter lymphocyte killing function and contribute to HLH pathogenesis.
Qian Y, Johnson JA, Connor JA, Valencia CA, Barasa N, Schubert J, et al. The 253-kb inversion and deep intronic mutations in UNC13D are present in North American patients with familial hemophagocytic lymphohistiocytosis 3. Pediatr Blood Cancer. 2014;61(6):1034–40. Two specific deep intronic mutations, including the one studied in Cichocki et al. above, and one large 253 kilobase inversion in the UNC13D gene were found to be present in total in about 17 % of a large (n = 1,709) cohort of North Americans with a suspected diagnosis of HLH.
Pagel J, Beutel K, Lehmberg K, Koch F, Maul-Pavicic A, Rohlfs AK, et al. Distinct mutations in STXBP2 are associated with variable clinical presentations in patients with familial hemophagocytic lymphohistiocytosis type 5 (FHL5). Blood. 2012;119(25):6016–24. Among a large cohort of STXPB2 mutant HLH patients, clinical differences in disease expression were correlated with specific types of STXBP2 mutations such that patients with exon 15 splice-site mutations presented later in life and had less severe NK cell defects.
Selliah N, Zhang M, White S, Zoltick P, Sawaya BE, Finkel TH, et al. FOXP3 inhibits HIV-1 infection of CD4 T-cells via inhibition of LTR transcriptional activity. Virology. 2008;381(2):161–7.
Klein E, Ben-Bassat H, Neumann H, Ralph P, Zeuthen J, Polliack A, et al. Properties of the K562 cell line, derived from a patient with chronic myeloid leukemia. Int J Cancer. 1976;18(4):421–31.
Cao LF, Krymskaya L, Tran V, Mi S, Jensen MC, Blanchard S, et al. Development and application of a multiplexable flow cytometry-based assay to quantify cell-mediated cytolysis. Cytometry A. 2010;77(6):534–45.
Ohadi M, Lalloz MR, Sham P, Zhao J, Dearlove AM, Shiach C, et al. Localization of a gene for familial hemophagocytic lymphohistiocytosis at chromosome 9q21.3-22 by homozygosity mapping. Am J Hum Genet. 1999;64(1):165–71.
Stepp SE, Dufourcq-Lagelouse R, Le Deist F, Bhawan S, Certain S, Mathew PA, et al. Perforin gene defects in familial hemophagocytic lymphohistiocytosis. Science. 1999;286(5446):1957–9.
Feldmann J, Callebaut I, Raposo G, Certain S, Bacq D, Dumont C, et al. Munc13-4 is essential for cytolytic granules fusion and is mutated in a form of familial hemophagocytic lymphohistiocytosis (FHL3). Cell. 2003;115(4):461–73.
zur Stadt U, Schmidt S, Kasper B, Beutel K, Diler AS, Henter JI, et al. Linkage of familial hemophagocytic lymphohistiocytosis (FHL) type-4 to chromosome 6q24 and identification of mutations in syntaxin 11. Hum Mol Genet. 2005;14(6):827–34.
Rubin CM, Burke BA, McKenna RW, McClain KL, White JG, Nesbit Jr ME, et al. The accelerated phase of Chediak-Higashi syndrome. An expression of the virus-associated hemophagocytic syndrome? Cancer. 1985;56(3):524–30.
Enders A, Zieger B, Schwarz K, Yoshimi A, Speckmann C, Knoepfle EM, et al. Lethal hemophagocytic lymphohistiocytosis in Hermansky-Pudlak syndrome type II. Blood. 2006;108(1):81–7.
Arico M, Imashuku S, Clementi R, Hibi S, Teramura T, Danesino C, et al. Hemophagocytic lymphohistiocytosis due to germline mutations in SH2D1A, the X-linked lymphoproliferative disease gene. Blood. 2001;97(4):1131–3.
Rigaud S, Fondaneche MC, Lambert N, Pasquier B, Mateo V, Soulas P, et al. XIAP deficiency in humans causes an X-linked lymphoproliferative syndrome. Nature. 2006;444(7115):110–4.
Compliance with Ethics Guidelines
Conflict of Interest
Randy Q. Cron has received < $5,000 each as consulting fees from Genentech, Novartis, and Swedish Orphan Biovitrum. Alexei A. Grom has received < $5,000 each as consulting fees from Novartis and Roche. Mingce Zhang, Edward M. Behrens, T. Prescott Atkinson, and Bita Shakoory declare that they have no conflict of interest. The work used to generate the data in Fig. 1 was supported by a grant from the Kaul Pediatric Research Institute to Randy Q. Cron.
Human and Animal Rights and Informed Consent
This article does not contain any studies with animals. Institutional Review Board approval was obtained for human subjects studies.
Author information
Authors and Affiliations
Corresponding author
Additional information
This article is part of the Topical Collection on Pediatric Rheumatology
Rights and permissions
About this article
Cite this article
Zhang, M., Behrens, E.M., Atkinson, T.P. et al. Genetic Defects in Cytolysis in Macrophage Activation Syndrome. Curr Rheumatol Rep 16, 439 (2014). https://doi.org/10.1007/s11926-014-0439-2
Published:
DOI: https://doi.org/10.1007/s11926-014-0439-2