Abstract
Purpose of Review
We reviewed recent literature on oxygen sensing in osteogenic cells and its contribution to development of a skeletal phenotype, the coupling of osteogenesis with angiogenesis and integration of hypoxia into canonical Wnt signaling, and opportunities to manipulate oxygen sensing to promote skeletal repair.
Recent Findings
Oxygen sensing in osteocytes can confer a high bone mass phenotype in murine models; common and unique targets of HIF-1α and HIF-2α and lineage-specific deletion of oxygen sensing machinery suggest differentia utilization and requirement of HIF-α proteins in the differentiation from mesenchymal stem cell to osteoblast to osteocyte; oxygen-dependent but HIF-α-independent signaling may contribute to observed skeletal phenotypes.
Summary
Manipulating oxygen sensing machinery in osteogenic cells influences skeletal phenotype through angiogenesis-dependent and angiogenesis-independent pathways and involves HIF-1α, HIF-2α, or both proteins. Clinically, an FDA-approved iron chelator promotes angiogenesis and osteogenesis, thereby enhancing the rate of fracture repair.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Oxygen bioavailability is a fundamental necessity for complex multicellular organisms; for growth beyond simple multicellular organisms to occur, it became necessary to develop internal transport and exchange mechanisms (e.g., the circulatory system) that enable the bulk flow of nutrients and waste to and from, respectively, cells in the larger body [1]. The fundamental necessity of O2 bioavailability is revealed in its absence: cellular metabolism favors anaerobic glycolysis before ultimately ceasing, thereafter by impairment of cell function and cell death, the tissue and organ death leading to death of an individual. To that end, the body has developed a variety of robust mechanisms to resolve reductions in tissue O2 availability (hypoxia), chiefly (1) increased cardiac output and ventilation; (2) improved vascularization; (3) enhanced blood O2-carrying capacity; and (4) a switch from aerobic to anaerobic respiration. At the cellular level, adaptation to hypoxia— whether acute or chronic— is driven by the energy/nutrient sensor mTOR, unfolded protein responses in the endoplasmic reticulum, NF-κB-mediated transcription, or the hypoxia-inducible factor (HIF) family of transcription factors [2].
HIFs are heterodimeric proteins composed of a HIF-α and HIF-β (or ARNT) subunit. Each subunit is constitutively expressed but has opposing stability: HIF-β/ARNT subunits remain stable, whereas HIF-α subunits are degraded under conditions of sufficient O2 bioavailability (normoxia). When cellular oxygen is sufficiently available (> ~ 5%), prolyl hydroxylase domain (Phd) proteins hydroxylate proline residues in HIF-α subunits (Fig. 1). Proline hydroxylation provides a binding site for von Hippel-Landau (Vhl) tumor suppressor protein, which subsequently recruits an ubiquitin E3 ligase complex that polyubiquitinates HIF-αs and targets them for proteasomal degradation. When oxygen levels are sufficiently low, HIF-α hydroxylation by PHDs is prevented, HIF-αs accumulate, associate with HIF-β, and induce gene expression via binding to HIF-responsive elements (HREs) in target gene promoters. Additional regulation of HIF-a-mediated signaling involves factor inhibiting HIF (FIH), which hydroxylates (N-terminal) asparaginyl residues, preventing association of HIF-α with transcriptional co-activators CBP/p300.
There are three HIF-α genes: HIF1A, HIF2A, and HIF3A. HIF-1α and HIF-2α directly induce gene transcription, whereas HIF-3α inhibits HIF-1α- or HIF-2α-mediated transcription by binding to ARNTs and sequestering their interaction with HIF-1α or HIF-2α, or preventing HIF-α and ARNT heterodimerization (reviewed in [2]). Structurally, HIF-1α and HIF-2α are composed of DNA binding and dimerization domains at their N termini, and transactivation domains at their C termini, and each gene reveals relatively high homology [3]. HIF-α/β heterodimers bind to HREs in target gene promoters, and there is evidence for both common and unique gene transcription in response to HIF-1α or HIF-2α. For example, HIF-1α induces transcription of genes involved in glycolysis (PGK, LDHA), apoptosis (BNIP3), and pH regulation (CAiX); HIF-2α induces cell proliferation (cyclin D1, TGF-alpha), de-differentiation (Oct4), and cell invasion (MMp2, Pai1), and both HIF-1α and HIF-2α induce genes involved in angiogenesis (VEGF) and glucose uptake (Glut1) [4]. Target gene specificity is not determined by specific binding of HIF-1α or HIF-2α to cognate HREs, but, rather, differences in the N-terminal transactivation domain (TAD), such that replacement of HIF-2α N-TAD with HIF-1α N-TAD is sufficient to confer HIF-1α-specific functionality to HIF-2α [3]. HIF-mediated gene transcription involves HIF-α/ARNT binding to the transcriptional co-activator CBP/p300, which provides another level of regulation of HIF-α-driven transcription. Additionally, HIF-2α is hydroxylated less efficiently by PHDs than is HIF-1α, indicating that more modest reductions in pericellular O2 are sufficient to promote HIF-2α stabilization than HIF-1α stabilization [5, 6]. Whereas HIF-1α requires very low O2 tension or even anoxia for its stabilization, HIF-2α is active under more physiological hypoxia (~ 5%), indicating differential involvement of HIF-α genes under acute vs. chronic hypoxia [7].
Hypoxia and the Skeletal System
Embryogenesis occurs in a hypoxic environment, such that HIF-α-directed signaling drives developmental morphogenesis [2]. Cells throughout the developing embryo are hypoxic and demonstrate stabilized HIF-α even after the development of a cardiovascular system. Within the skeletal system, hypoxia and HIF-α-driven signaling is involved in endochondral bone formation (see the recent review by Stegan and Carmeliet [8]).
Approaches to measuring pO2 tensions (wherein 100% O2 = 760 mmHg) within bone have relied upon oxygen microelectrodes [9], bone marrow aspiration [10••], or chemical surrogates for hypoxia (pimonidazole) [11••]. Such approaches have established that disruption of blood vessels at a fracture site causes localized hypoxia (0.8–3% pO2) [9], that the pO2 of human bone marrow aspirates is 7.2% [10••], or that disuse increases osteocyte hypoxia in a reversible manner [11••]. Recent advances in microscopy and reporter mice have revealed two distinct types of bone capillaries—type H (high) and type L (low)—based on expression of the junctional protein CD31 (PECAM1) and the sialoglycoprotein endomucin [12•]. Arteries initially flow into type H capillaries, which are observed primarily in the growth plate, before transitioning into with type L capillaries, which branch from the metaphysis into the bone marrow within the diaphysis, prior to draining in the central vein [12•, 13••]. Thus, perhaps paradoxically, avascular cartilage receives the most oxygenated and nutrient-rich blood, in contrast to highly vascular bone and its marrow. Using two-photon phosphorescence lifetime microscopy, Spencer et al. demonstrated distinct spatial heterogeneities in local pO2 throughout bone and the bone marrow: pO2 was greatest in the periosteum and decreased in cortical bone [14]. Despite the high vascular network within bone marrow, observed pO2 was lower within bone marrow sinusoids compared to the endosteum, perhaps due to high metabolic demand of marrow stromal cells and hematopoietic stem cells. There is also suggestive evidence for intracortical heterogeneity in oxygen tension: osteocytes deep within cortical bone express markers of glycolysis and the oxygen-regulated protein ORP150, whereas osteocytes closer to the bone surface do not express these markers [15]. Functionally, both total and active mitochondria are greater in osteocytes near the endosteum or periosteum compared to osteocytes within cortical bone, and mid-cortical osteocytes are more resistant to ischemia-induced stress [16].
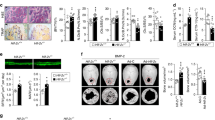
Tissue-specific deletion of Hif1a or Hif2a, or HIF-α-degrading machinery Phd2 or Vhl, reveals a variety of skeletal phenotypes that underscore the complexity of skeletal HIF-α signaling during development and disease. The tissue and developmental stage-specific cre drivers used to evaluate HIF-α signaling are shown in Table 1. Briefly, hypoxia and HIF-α promote skeletal mesenchyme condensation and limb development, promoting chondrogenesis by increasing Sox9 and reducing osteogenesis through Runx2 inhibition [17]. Skeletal malformations or low bone mass phenotypes are observed in Phd2-deficient preosteoblasts (Col1a2-cre; Phd2 cKO) [21••] or Hif1a-deficient mature osteoblasts (Bglap-cre; Hif1a cKO) [22••]. Certain models show no skeletal effect: Hif2a deletion in mature osteoblasts demonstrated no overt skeletal phenotype, despite reductions in vascular density [23•]; similarly, Hif1a deletion in osteocytes (Dmp1-cre; Hif1a cKO) produces mice that are phenotypically similar to wild-type controls [25••]. Other animal models of altered oxygen sensing demonstrate a high bone mass phenotype. In proliferating chondrocytes (Col2a1-ERT2-cre), deletion of either Phd2 [18] or Vhl [19] produces a high bone mass phenotype involving increased bone formation relative to resorption perhaps due to the transdifferentiation of hypertrophic chondrocytes into osteoblasts [18]. Individual deletion of Phd genes in osteoprogenitors (Osx-cre) failed to produce a skeletal phenotype, whereas combined deletion of each gene (Osx-cre; Phd1/2/3 cKO) increased HIF-α target gene expression, vascularization, and improved trabecular microarchitecture [20••]. Of note, deletion of Phd1/2 or Phd2/3 phenocopied improvements in trabecular microarchitecture without enhancing vascularity. Vhl deletion in mature osteoblasts (Bglap-cre; Vhl cKO) causes a high bone mass phenotype associated with increased vessel density, resulting from increased bone formation rate [22••]. Deletion of Phd2 or Vhl in osteocytes (Dmp1-cre; Phd2 or Dmp1-cre; Vhl cKO) also produces high bone mass in mice [24••, 25••].
Coupling Oxygen Sensing to Skeletal Phenotypes
HIFs and Vegf
A prevailing assumption, provided by the canonical pathway whereby PHD isoforms and Vhl regulate HIF-α stability, is that the skeletal effects observed from influencing PHD or Vhl are directly attributable to HIF-α stabilization and subsequent gene transcription, most generally Vegf. Indeed, Vegf and its various isoforms are necessary for endochondral bone formation (reviewed recently in [8]). Coupling angiogenesis to osteogenesis, and vice versa, involves reciprocal signaling between osteoblasts and endothelial cells: endothelial cells secrete BMP2 to promote bone formation [26], and osteoblasts secrete VEGF to enhance angiogenesis [27]. In vivo, manipulating Phd, Vhl, or HIFs in osteogenic cells can increase VEGF and angiogenesis [20••, 22••]. Similar coupling involves VEGF, Notch, and Noggin [28]. Nonetheless, there is sufficient evidence that angiogenesis is insufficient to promote osteogenesis. Osx-cre; Phd1/2 and Osx-cre; Phd2/3 cKO mice have a high bone mass without concordant changes in Vegf or vascularity [20••], deleting Hif1a or Hif2a in mature osteoblasts (Bglap-cre) reduces Vegf expression and vessel volume equivalently, yet Hif1a deletion influenced Tb.BV/TV moreso than Hif2a deletion [23•]. Further, stabilizing HIF-1α or HIF-2α comparably increases Vegf, but a skeletal phenotype was observed only in HIF-2α-stable mice [20••]. Related observations are found in mice lacking chondrocytic Hif1a, whose dwarfism and cartilage destruction is not rescued by VEGF164 overexpression [29].
Hypoxia and Wnt Signaling
The critical requirement of Wnt/Lrp5 signaling in skeletal biology is underscored by mutations in Lrp5 that produce reciprocal effects on the skeleton. Loss-of-function mutations in Lrp5 cause osteoporosis pseudoglioma (OPPG), characterized by low bone mass [30], whereas missense mutations in Lrp5 are observed in individuals with high bone mass [31]. Induction of Wnt signaling occurs during load-induced bone formation [32] and is required for new bone deposition in response to external loads [33, 34].
Regulation of Wnt signaling occurs via secreted decoy receptors (sFrps) or antagonists (Sost, Dkk isoforms) that bind to Lrp4-6 to prevent Wnt-Lrp interactions, and subsequent signal transduction [35]. Just as activating mutations in LRP4-6 promote HBM phenotypes [30, 31, 36, 37], complementary phenotypes emerge from deletion of Lrp4/5/6 antagonists [38,39,40,41,42,43,44]. Deletion of sFRPs increases trabecular bone [44] and bone mineral density [43], and loss of Dkk isoforms or Sost increases markers of bone formation and bone mass [39, 40]. In vivo and in vitro, evidence reveals functional interaction between HIF-α and Wnt signaling without consensus: Bglap-cre; Hif1a cKO mice display enhanced load-induced bone formation via β-catenin [45], osteocyte differentiation is attenuated in Bglap-cre; Vhl cKO mice, and both Osterix and HIF-α cooperatively reduce Wnt signaling [46]. Alternately, other reports indicate that hypoxia or hypoxia mimetics increase Wnt signaling in bone [47, 48]. In the cartilage, HIF-1a binds to β-catenin to prevent transcriptional induction of Wnt target genes [49].
Although osteocytes do not directly contribute to bone formation, osteocytic β-catenin is required for the osteoanabolic effect of mechanical loading [50], and constitutively active β-catenin in osteocytes increases both cortical and trabecular bone mass through increasing both arms of remodeling [51]. Thus, regulation of β-catenin availability and transcription in osteocytes can exert profound effects on skeletal mass and microarchitecture. Two recent reports demonstrate an epistatic relationship between hypoxia and Wnt/β-catenin signaling in osteocytes to produce a high bone mass phenotype: osteocytic Vhl deletion decreases Sost and increases canonical Wnt signaling [25••]. Similarly, deleting Phd2 in osteocytes produced a high bone mass phenotype that correlated with decreased sclerostin expression and increased canonical Wnt signaling; in this model, osteocytic Phd2 deletion promoted sirtuin-1-mediated deacetylation of the Sost promoter [24••]. Whereas these reports identify an effect of hypoxia on Wnt signaling, the actual effect of hypoxia on Wnt signaling—stimulatory or inhibitory—is perhaps intrinsic to epigenetic modification or cellular bioenergetics in osteoblasts vs. osteocytes.
Canonical and non-canonical PHD/HIF/Vhl signaling. a Under conditions of sufficient pericellular oxygen, PHD proteins hydroxylate proline residues in HIF-1a or HIF-2a, Ndrg3, or IKK subunits. Vhl binds to hydroxylated HIF-α and Ndrg3 and are targeted for proteasomal degradation, whereas hydroxylated IKK subunits are catalytically incapable of phosphorylating IκBα, which results in NF-κB degradation and inhibition of NF-κB-mediated gene transcription. b Under conditions of reduced oxygen availability, there is insufficient oxygen available for PHD-regulated hydroxylation of HIF-α, Ndrg3, or IKK. Consequently, HIF-α binds to HIF-β to induce target gene transcription, such as lactate dehydrogenase (LDHA). LDHA subsequently converts pyruvate, generated during anaerobic glycolysis, into lactate, which binds to NDRG3 and prevents complex formation with Vhl; through currently unknown mechanisms, Ndrg3 can influence cell proliferation, autophagy, or apoptosis. In the absence of hydroxylation, IKK promotes phosphorylation and subsequent degradation of IκBα, enabling induction of NF-κB-dependent gene transcription
HIF-Independent Signaling by Phd and Vhl in the Skeleton
Both Phd genes and Vhl have cellular effects beyond oxygen sensing through HIFs. In addition to HIF-a subunits, PHDs hydroxylate other substrates including IKKβ [52] and NDRG3 [53], decreasing the activity or availability of each. Expressing dominant-negative IKKγ in preosteoblasts or mature osteoblasts increases bone formation [54], suggesting the skeletal phenotypes of the various Phd2 cKO mice may be secondary to PHD2/Ikkγ-mediated phenomena. Ndrg3 contributes to cell proliferation, differentiation, development, and response to stress including hypoxia [55]. Similar to HIF-α subunits, Ndrg3 is constitutively hydroxylated by Phd2 under normoxia prior to proteolytic degradation; under hypoxia, cellular metabolism switches from oxidative phosphorylation to anaerobic glycolysis as a source of ATP, thereby increasing lactate levels. Direct binding between lactate and Ndrg3 prevents NDRG3 association with VHL and thus its degradation. Once stabilized, NDRG3 promotes Raf/ERK signaling with resultant increases in proliferation and angiogenesis [53]. Additionally, the low bone mass phenotype of Col1a2-ER-cre; Phd2 cKO mice is attributed not to changes in HIF-a bioavailability and gene transcription, but instead to ascorbate-regulated Osx induction [56]. If so, and to what extent, these HIF-a-independent cascades influence skeletal development and homeostasis requires careful evaluation.
Osteogenic HIF Signaling in Skeletal Pathology and Pharmacology
Provided the functional and spatiotemporal linkage between angiogenesis and osteogenesis, and the uncoupling of the bone remodeling cycle favoring bone resorption with age, it is perhaps to be expected that changes in oxygen bioavailability are associated with post-menopausal and senile osteoporosis. Further, other skeletal or skeletal-associated pathologies—traumatic fracture and non-union, glucocorticoid or bisphosphonate-associated osteonecrosis, or renal phosphate wasting—implicate insufficient oxygen handling in osteogenic cells.
Osteoporosis and Oxygen
Bone marrow and bone perfusion are decreased in osteoporotic and aged individuals relative to estrogen complete or younger individuals [57, 58]. Aging causes endothelial dysfunction, which is exacerbated by ovariectomy and improved by supplemental estrogen. The vasoactive factors released from endothelial cells (e.g., NO and PGI2) have direct effects on both osteoblasts and osteoclasts and may influence interstitial fluid flow within osteocyte lacuna and canaliculi [59]. Serum VEGF levels positively correlate with BMD and are decreased in post-menopausal women [60]. Further, bone from ovariectomized rodents reveal increased staining for HIF-1a and HIF-2a [48, 61] suggesting that estrogen regulates HIF-α stability. This is not simply a correlative event, as pharmacologic manipulation of HIF-α isoforms, or genetic deletion of Phd2 or Vhl, protects against OVX-induced bone loss in rats and mice [14, 37, 49, 50].
Skeletal Fracture and Non-union
Disruption of blood vessels in response to bone fracture creates a hypoxic environment. Hematoma formation isolates the site of injury from perfusion, further augmenting localized hypoxia [9]. As fracture repair closely mimics stages of embryonic bone development—in which hypoxia and HIF-a signaling plays a crucial role—it is unsurprising that trauma-induced hypoxia promotes skeletal repair involving HIF-a signaling. A number of studies have confirmed the hypoxic environment around a fracture site [62••, 63], suggesting that pharmacologic, biologic, or genetic manipulation of neoangiogenesis may promote callus formation and bone repair. Deferoxamine (or desferrioxamine; DFO) is an FDA-approved iron chelator used in diseases associated with iron overload, such as thalassemia syndromes [64]. DFO promotes bone consolidation in tibial [65] or mandibular distraction osteogenesis [66], increases vascularity and callus size in femoral fractures [67], and hastens bone bridging and increased vascularity in femoral segmental defects [68]. Likewise, Bglap-cre; Vhl cKO mice demonstrate increased neoangiogenesis and skeletal repair compared to wild-type controls; conversely, osteoblastic deletion of Hif1a mitigates neoangiogenesis and bone repair [65]. Local injection of DFO is also effective in promoting bone repair after glucocorticoid-associated osteonecrosis.
Chronic Kidney Disease-Mineral Bone Disorder
CKD-MBD is a systemic disorder of calcium and phosphate balance secondary to kidney dysfunction; the inability of the kidneys to adequately filter phosphate leads to secretion of the phosphaturic hormone FGF23 from bone, specifically osteocytes, to reduce expression of renal phosphate cotransporters in the renal proximal tubule and decrease circulating (1α,25)-(OH)2-vitamin D3. Emerging evidence indicate that FGF23 synthesis and secretion is induced by HIF-α-induced erythropoietin (EPO) produced by bone marrow cells [69,70,71,72] or osteoprogenitors/osteoblasts [69, 72]; this regulation is apparent in development [69] and disease [73••], but may be absent in adulthood [69]. In osteoprogenitors, a PHD-Vhl-HIF-2α axis drives EPO expression and erythropoiesis and unexpectedly decreases renal EPO expression [69]. Provided the complex interaction between FGF23, PTH, and vitamin D3 in calcium and phosphate homeostasis in health and disease [74], oxygen sensing in osteogenic cells must be carefully considered as part of multi-tissue interactions and feedback mechanisms governing serum calcium and phosphate levels.
Osteonecrosis
Osteonecrosis, or avascular necrosis, results from disrupted blood supply to bone [75]. Ischemic cell death in bone marrow and trabeculae then contributes to subchondral bone collapse and joint arthrosis. Osteonecrosis is observed in individuals sustaining traumatic injury, or is associated with sustained or high-dose corticoid or antiresorptive therapy, but is also observed in individuals with autoimmune diseases or high alcohol consumption. Provided clinical evidence for tissue ischemia, it is not surprising that bone cell hypoxia contributes to the causation and potential resolution of osteonecrosis. Polymorphisms in Hif1a [76] or Vegfc [77] are associated with idiopathic osteonecrosis of the femoral head in Korean men, and greater VEGF-C expression is observed in the actively repairing edematous zone immediately adjacent to necrotic tissue in the femoral head [78]. Glucocorticoid-induced osteonecrosis of the femoral head in a murine model demonstrated rapid reduction in Hif1a and Vegf expression in the femoral head, but not the distal femur, and vascular conversion to pools of edema prior to any observable effect on bone mineral density or osteocyte apoptosis [79]; in vitro, glucocorticoids also rapidly reduce Hif1a and Vegf expression. A small molecule PHD inhibitor, EDHB, reduced the incidence of steroid-associated osteonecrosis in rabbits and promoted HIF-α/VEGF signaling [80]. Glucocorticoids also reduce regional matrix remodeling by osteocytes (perilacunar remodeling) which contributes to osteonecrosis and subchondral bone degeneration [81], although this study did not directly evaluate interactions between vascularity, oxygen sensing, and perilacunar remodeling.
Antiresorptive bisphosphonate therapy is also associated with osteonecrosis of the jaw and ear canal [82, 83]. Anti-angiogenic effects of aminobisphosphonates [84] are suggested as part of the multifactorial pathophysiology of bisphosphonate-related osteonecrosis of the jaw (BRONJ), though certain studies in rodents fail to support the hypothesis that bisphosphonates suppress angiogenesis [85, 86]. Decreased angiogenesis in bone would also suggest potential osteoblast- or osteocyte-intrinsic regulation of angiogenesis under disease states, yet, to date, studies designed to interrogate the connection between oxygen sensing in osteoblasts and BRONJ are lacking; similarly, there is no current evidence of hypoxia or aberrant vascular density in another complication from prolonged bisphosphonate use, atypical femur fracture.
Osteoanabolic Therapies PTH and PTHrP Directly and Indirectly Induce Neoangiogenesis
Teriparatide™ (recombinant PTH(1–34)) and abaloparatide™ (recombinant parathyroid receptor-related protein(1–34)) represent the only currently available FDA-approved osteoanabolic agents. That these agents are osteoanabolic, in the context of angiogenesis-osteogenesis coupling suggests that PTH may influence angiogenesis in development and repair. PTH-induced acceleration of cranial repair associates with angiopoietin-1 levels and angiogenesis and decreased arteriogenesis [87]; continuous PTH induces bone marrow vascularity independent of osteoclastogenesis [88]; PTH-related peptide (PTHrP) associates with osteolytic metastasis and VEGF expression by breast cancer cells [89]. PTH(1–84)-induced increases in trabecular bone volume fraction and Vegf expression in the murine tibial metaphysis are blocked by anti-VEGF antibody co-treatment [90]; similarly, angiogenesis is required for PTH(1–84)-induced increases in BMD and toughness in rats [91]. Yet, the influence of PTH on skeletal vascularization requires more thorough elucidation, as Prisby et al. found that PTH(1–84) reduced the number of bone marrow blood vessels, instead redistributing them closer to sites of bone formation [90]. Yet, HIF-1α may restrain osteoanabolism in response to PTH, as mice lacking Hif1a in mature osteoblasts reveal enhanced bone formation compared to wild type [92].
Conclusions
The works reviewed above demonstrate that oxygen sensing in bone is fundamentally necessary for skeletal development and repair, is altered in disease states, and can be pharmacologically manipulated to hasten bone repair. These works, and others, have identified causal interactions between angiogenesis and osteogenesis, as well as osteogenesis in the absence of vascular changes; in doing so, they have fundamentally established a role for oxygen sensing in osteogenic cells as a means of driving bone formation. Yet, there are many questions left to be answered, and many more that are not yet considered. Among these are:
-
1.
Which HIF-α genes are necessary throughout cellular lifespan and differentiation from a mesenchymal stem cell to osteoblast to osteocyte? Whereas Bglap-cre; Hif1a cKO mice have a low bone mass phenotype [19], osteocytic Dmp1-cre; Hif1a cKO mice do not [25••], suggesting lineage-specific necessity for a particular HIF-α gene. Such lineage-specific requirements for Hif1a vs. Hif2a are also suggested by the work of Wu et al., wherein deletion of both Hif1a and Hif2a was necessary to produce a skeletal phenotype [20••].
-
2.
Similarly, how does oxygen sensing in osteoblasts vs. osteocytes influence skeletal phenotype, and how does this relate to cellular bioenergetics? Two recent reports using osteocytic Dmp1-cre mice reveal equivocal increases in skeletal phenotype compared to mature osteoblastic Bglap-cre mice [24••, 25••], demonstrating that oxygen handling by osteocytes can have pronounced skeletal effects, but also that persistence of gene deletion, as osteoblasts differentiate into osteocytes, must be considered. Osteogenic cells are capable of both oxidative and glycolytic metabolism, using glycolysis primarily in undifferentiated mesenchymal stem cells then switching to oxidative phosphorylation in osteoblasts (reviewed in Riddle and Clemens [93]) as functional demand on osteoblasts to synthesize and secrete matrix increases. To date, evaluation of osteocyte bioenergetics is absent, but it is intriguing to consider the disparate skeletal phenotypes observed with osteoblast vs. osteocyte deletion of oxygen sensing machinery as a consequence of cell-intrinsic metabolic profile.
-
3.
To what extent do observed phenotypes in Vhl or Phd cKO animals require HIF-α signaling? Based solely on the canonical HIF signaling pathway, it is facile to assume that effects produced in such murine models are due to stabilization of HIF-1α or HIF-2α. Yet, Col1a2; Phd2 cKO mice resemble a spontaneous fracture mouse (sfx) whose phenotype results from inability to correctly synthesize vitamin C [21••]. Similarly, Vhl targets proteins beyond HIF-1α or HIF-2α for proteolytic degradation: hypoxia-induced lactate levels (themselves due to HIF-α-induced LDHA expression) bind to NDRG3 and prevent its Vhl-mediated degradation. How these HIF-independent signals contribute to skeletal development, coupling, and cellular bioenergetics is insufficiently interrogated.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Monahan-Earley R, Dvorak AM, Aird WC. Evolutionary origins of the blood vascular system and endothelium. J Thromb Haemost. Wiley/Blackwell (10.1111); 2013;11 Suppl 1:46–66.
Dunwoodie SL. The role of hypoxia in development of the Mammalian embryo. Dev Cell. 2009;17:755–73.
Hu C-J, Sataur A, Wang L, Chen H, Simon MC. The N-terminal transactivation domain confers target gene specificity of hypoxia-inducible factors HIF-1alpha and HIF-2alpha. Tansey W, editor. Mol Biol Cell. 2007;18:4528–42.
Pawlus MR, Hu C-J. Enhanceosomes as integrators of hypoxia inducible factor (HIF) and other transcription factors in the hypoxic transcriptional response. Cell Signal. 2013;25:1895–903.
Koivunen P, Hirsila M, Gunzler V, Kivirikko KI, Myllyharju J. Catalytic properties of the asparaginyl hydroxylase (FIH) in the oxygen sensing pathway are distinct from those of its prolyl 4-hydroxylases. J Biol Chem. American Society for Biochemistry and Molecular Biology. 2004;279:9899–904.
Koh MY, Powis G. Passing the baton: the HIF switch. Trends Biochem Sci. 2012;37:364–72.
Lin Q, Cong X, Yun Z. Differential Hypoxic Regulation of Hypoxia-Inducible Factors 1α and 2α. Mol Cancer Res. American Association for Cancer Research. 2011;9:757–65.
Stegen S, Carmeliet G. The skeletal vascular system – Breathing life into bone tissue. Bone. Elsevier. 2018;115:50–8.
Brighton CT, Krebs AG. Oxygen tension of healing fractures in the rabbit. J Bone Joint Surg Am. 1972;54:323–32.
Harrison JS, Rameshwar P, Chang V, Bandari P. Oxygen saturation in the bone marrow of healthy volunteers. Blood. American Society of Hematology. 2002;99:394–4.
Dodd JS, Raleigh JA, Gross TS. Osteocyte hypoxia: a novel mechanotransduction pathway. Am J Physiol. 1999;277:C598–602.
Kusumbe AP, Ramasamy SK, Adams RH. Coupling of angiogenesis and osteogenesis by a specific vessel subtype in bone. Nature. 2014;507:323–8.
Sivaraj KK, Adams RH. Blood vessel formation and function in bone. Development. Oxford University Press for The Company of Biologists Limited; 2016;143:2706–2715.
Spencer JA, Ferraro F, Roussakis E, Klein A, Wu J, Runnels JM, et al. Direct measurement of local oxygen concentration in the bone marrow of live animals. Nature. Nature Publishing Group. 2014;508:269–73.
Guo D, Keightley A, Guthrie J, Veno PA, Harris SE, Bonewald LF. Identification of osteocyte-selective proteins. Huber C, Huber L, editors. Proteomics. Wiley-Blackwell; 2010;10:3688–3698.
Frikha-Benayed D, Basta Pljakic J, Majeska RJ, Schaffler MB. Regional differences in oxidative metabolism and mitochondrial activity among cortical bone osteocytes. Bone. Elsevier Inc. 2016;90:15–22.
Mangiavini L, Merceron C, Araldi E, Khatri R, Gerard-O'Riley R, Wilson TL, et al. Loss of VHL in mesenchymal progenitors of the limb bud alters multiple steps of endochondral bone development. Dev Biol. 2014;393:124–36.
Cheng S, Aghajanian P, Pourteymoor S, Alarcon C, Mohan S. Prolyl Hydroxylase Domain-Containing Protein 2 (Phd2) Regulates Chondrocyte Differentiation and Secondary Ossification in Mice. Sci Rep. 2016;6:35748.
Weng T, Xie Y, Huang J, Luo F, Yi L, He Q, et al. Inactivation of Vhl in osteochondral progenitor cells causes high bone mass phenotype and protects against age-related bone loss in adult mice. J Bone Miner Res. 2014;29:820–9.
Wu C, Rankin EB, Castellini L, Alcudia JF, Fernandez-Alcudia J, LaGory EL, et al. Oxygen-sensing PHDs regulate bone homeostasis through the modulation of osteoprotegerin. Genes Dev. Cold Spring Harbor Lab; 2015;29:817–31. Deletion of individual PHD proteins in osteoprogenitors is insufficient to produce a high bone mass phenotype; high bone mass phenotypes can occur independent of changes in bone vascularity.
Cheng S, Xing W, Pourteymoor S, Mohan S. Conditional disruption of the prolyl hydroxylase domain-containing protein 2 (Phd2) gene defines its key role in skeletal development. J Bone Miner Res. 2014;29:2276–86 Phd2 deletion in pre-osteoblasts decreases bone mass and microarchitecture, possibly through HIF-a-independent mechanisms that involve citamin C-induced osterix expression.
Wang Y, Wan C, Deng L, Liu X, Cao X, Gilbert SR, et al. The hypoxia-inducible factor alpha pathway couples angiogenesis to osteogenesis during skeletal development. J Clin Invest. 2007;117:1616–26 The first study to directly demonstrate genetic manipulation of oxygen-sensing in bone influences skeletal phenotype.
Shomento SH, Wan C, Cao X, Faugere M-C, Bouxsein ML, Clemens TL, et al. Hypoxia-inducible factors 1alpha and 2alpha exert both distinct and overlapping functions in long bone development. J Cell Biochem. 2010;109:196–204 Demonstration that HIF-1a and HIF-2a in mature osteoblasts have common and unique influence on bone microarchitecture and vascularization.
Stegen S, Stockmans I, Moermans K, Thienpont B, Maxwell PH, Carmeliet P, et al. Osteocytic oxygen sensing controls bone mass through epigenetic regulation of sclerostin. Nat Comms. Nature Publishing Group; 2018;9:2557. Osteocytic oxygen-sensing exerts profound effects on bone via epistatic inhibition of Sost expression.
Loots GG, Robling AG, Chang JC, Murugesh DK, Bajwa J, Carlisle C, et al. Vhl deficiency in osteocytes produces high bone mass and hematopoietic defects. Bone. 2018;116:307–14 Using an osteocytic cre driver, osteocytic deletion of Vhl influences bone mass through Wnt-dependent and -independent mechanisms.
Street J, Bao M, deGuzman L, Bunting S, Peale FV, Ferrara N, et al. Vascular endothelial growth factor stimulates bone repair by promoting angiogenesis and bone turnover. Proc Natl Acad Sci USA. 2002;99:9656–61.
Deckers MML, van Bezooijen RL, van der Horst G, Hoogendam J, Van Der Bent C, Papapoulos SE, et al. Bone morphogenetic proteins stimulate angiogenesis through osteoblast-derived vascular endothelial growth factor A. Endocrinology. 2002;143:1545–53.
Ramasamy SK, Kusumbe AP, Wang L, Adams RH. Endothelial Notch activity promotes angiogenesis and osteogenesis in bone. Nature. Nature Publishing Group. 2014;507:376–80.
Maes C, Araldi E, Haigh K, Khatri R, Van Looveren R, Giaccia AJ, et al. VEGF-independent cellautonomous functions of HIF-1α regulating oxygen consumption in fetal cartilage are critical for chondrocyte survival. J Bone Miner Res. Wiley-Blackwell. 2012;27:596–609.
Gong Y, Slee RB, Fukai N, Rawadi G, Roman-Roman S, Reginato AM, et al. LDL receptor-related protein 5 (LRP5) affects bone accrual and eye development. Cell. 2001;107:513–23.
Little R, Carulli J, Del Mastro R, Dupuis J, Osborne M, Folz C, et al. A mutation in the LDL receptor-related protein 5 gene results in the autosomal dominant high-bone-mass trait. Am J Hum Genet. 2002;70:11–9.
Armstrong VJ, Muzylak M, Sunters A, Zaman G, Saxon LK, Price JS, et al. Wnt/beta-catenin signaling is a component of osteoblastic bone cell early responses to load-bearing and requires estrogen receptor alpha. J Biol Chem. 2007;282:20715–27.
Tu X, Rhee Y, Condon K, Bivi N, Allen MR, Dwyer D, et al. Sost downregulation and local Wnt signaling are required for the osteogenic response to mechanical loading. Bone. 2011.
Sawakami K, Robling AG, Ai M, Pitner ND, Liu D, Warden SJ, et al. The Wnt co-receptor LRP5 is essential for skeletal mechanotransduction but not for the anabolic bone response to parathyroid hormone treatment. J Biol Chem. 2006;281:23698–711.
Williams BO, Insogna KL. Where Wnts went: the exploding field of Lrp5 and Lrp6 signaling in bone. J Bone Miner Res. 2009;24:171–8.
Kato M, Patel M, Levasseur R, Lobov I, Chang B, Glass D, et al. Cbfa1-independent decrease in osteoblast proliferation, osteopenia, and persistent embryonic eye vascularization in mice deficient in Lrp5, a Wnt coreceptor. J Cell Biol. 2002;157:303–14.
Leupin O, Piters E, Halleux C, Hu S, Kramer I, Morvan F, et al. Bone overgrowth-associated mutations in the LRP4 gene impair sclerostin facilitator function. J Biol Chem. 2011;286:19489–500.
Loots GG, Kneissel M, Keller H, Baptist M, Chang J, Collette NM, et al. Genomic deletion of a long-range bone enhancer misregulates sclerostin in Van Buchem disease. Genome Research. 2005;15:928–35.
Balemans W, Ebeling M, Patel N, Van Hul E, Olson P, Dioszegi M, et al. Increased bone density in sclerosteosis is due to the deficiency of a novel secreted protein (SOST). Hum Mol Genet. 2001;10:537–43.
Brunkow ME, Gardner JC, Van Ness J, Paeper BW, Kovacevich BR, Proll S, et al. Bone dysplasia sclerosteosis results from loss of the SOST gene product, a novel cystine knot-containing protein. Am J Hum Genet. 2001;68:577–89.
Balemans W, Patel N, Ebeling M, Van Hul E, Wuyts W, Lacza C, et al. Identification of a 52 kb deletion downstream of the SOST gene in patients with van Buchem disease. J Med Genet. 2002;39:91–7.
Kusu N, Laurikkala J, Imanishi M, Usui H, Konishi M, Miyake A, et al. Sclerostin is a novel secreted osteoclast-derived bone morphogenetic protein antagonist with unique ligand specificity. J Biol Chem. 2003;278:24113–7.
Nakanishi R, Shimizu M, Mori M, Akiyama H, Okudaira S, Otsuki B, et al. Secreted frizzled-related protein 4 is a negative regulator of peak BMD in SAMP6 mice. J Bone Miner Res. 2006;21:1713–21.
Bodine PVN, Zhao W, Kharode YP, Bex FJ, Lambert A-J, Goad MB, et al. The Wnt antagonist secreted frizzled-related protein-1 is a negative regulator of trabecular bone formation in adult mice. Mol Endocrinol. 2004;18:1222–37.
Riddle RC, Leslie JM, Gross TS, Clemens TL. Hypoxia-inducible factor-1α protein negatively regulates load-induced bone formation. J Biol Chem. 2011;286:44449–56.
Chen D, Li Y, Zhou Z, Xing Y, Zhong Y, Zou X, et al. Synergistic inhibition of Wnt pathway by HIF-1α and osteoblast-specific transcription factor osterix (Osx) in osteoblasts. Samant R, editor. PLoS ONE. Public Library of Science; 2012;7:e52948.
Genetos DC, Toupadakis CA, Raheja LF, Wong A, Papanicolaou SE, Fyhrie DP, et al. Hypoxia decreases sclerostin expression and increases Wnt signaling in osteoblasts. J Cell Biochem. 2010;110:457–67.
Peng J, Lai ZG, Fang ZL, Xing S, Hui K, Hao C, et al. Dimethyloxalylglycine prevents bone loss in ovariectomized C57BL/6J mice through enhanced angiogenesis and osteogenesis. Samant R, editor. PLoS ONE. Public Library of Science; 2014;9:e112744.
Bouaziz W, Sigaux J, Modrowski D, Devignes C-S, Funck-Brentano T, Richette P, et al. Interaction of HIF1α and β-catenin inhibits matrix metalloproteinase 13 expression and prevents cartilage damage in mice. Proc Natl Acad Sci USA. National Academy of Sciences. 2016;113:5453–8.
Javaheri B, Stern AR, Lara N, Dallas M, Zhao H, Liu Y, et al. Deletion of a single β-catenin allele in osteocytes abolishes the bone anabolic response to loading. J Bone Miner Res. 2014;29:705–15.
Tu X, Delgado-Calle J, Condon KW, Maycas M, Zhang H, Carlesso N, et al. Osteocytes mediate the anabolic actions of canonical Wnt/β-catenin signaling in bone. Proc Natl Acad Sci USA. National Acad Sciences; 2015 :201409857.
Cummins EP, Berra E, Comerford KM, Ginouves A, Fitzgerald KT, Seeballuck F, et al. Prolyl hydroxylase-1 negatively regulates IkappaB kinase-beta, giving insight into hypoxia-induced NFkappaB activity. Proc Natl Acad Sci USA. National Academy of Sciences; 2006;103:18154–9.
Lee DC, Sohn HA, Park Z-Y, Oh S, Kang YK, Lee K-M, et al. A lactate-induced response to hypoxia. Cell. 2015;161:595–609.
Chang J, Wang Z, Tang E, Fan Z, McCauley L, Franceschi R, et al. Inhibition of osteoblastic bone formation by nuclear factor-kappaB. Nat Med. 2009;15:682–9.
Melotte V, Qu X, Ongenaert M, van Criekinge W, de Bruine AP, Baldwin HS, et al. The N-myc downstream regulated gene (NDRG) family: diverse functions, multiple applications. FASEB J. Federation of American Societies for Experimental Biology; 2010;24:4153–66.
Xing W, Pourteymoor S, Mohan S. Ascorbic acid regulates osterix expression in osteoblasts by activation of prolyl hydroxylase and ubiquitination-mediated proteosomal degradation pathway. Physiological Genomics. American Physiological Society Bethesda, MD; 2011;43:749–57.
Lahtinen T, Alhava EM, Karjalainen P, Romppanen T. The effect of age on blood flow in the proximal femur in man. Journal of Nuclear Medicine. 1981;22:966–72.
Burkhardt R, Kettner G, Bohm W, Schmidmeier M, Schlag R, Frisch B, et al. Changes in trabecular bone, hematopoiesis and bone marrow vessels in aplastic anemia, primary osteoporosis, and old age: a comparative histomorphometric study. Bone. 1987;8:157–64.
Prisby RD, Dominguez JM, Muller-Delp J, Allen MR, Delp MD. Aging and estrogen status: a possible endothelium-dependent vascular coupling mechanism in bone remodeling. Malaval L, editor. PLoS ONE. Public Library of Science; 2012;7:e48564.
Senel K, Baykal T, Seferoglu B, Altas EU, Baygutalp F, Ugur M, et al. Circulating vascular endothelial growth factor concentrations in patients with postmenopausal osteoporosis. Arch Med Sci. Termedia. 2013;9:709–12.
Zhao Q, Shen X, Zhang W, Zhu G, Qi J, Deng L. Mice with increased angiogenesis and osteogenesis due to conditional activation of HIF pathway in osteoblasts are protected from ovariectomy induced bone loss. Bone. Elsevier Inc. 2012;50:763–70.
Komatsu D, Hadjiargyrou M. Activation of the transcription factor HIF-1 and its target genes, VEGF, HO-1, iNOS, during fracture repair. Bone. 2004;34:680–8.
Toupadakis CA, Wong A, Genetos DC, Chung D-J, Murugesh D, Anderson MJ, et al. Long-term administration of AMD3100, an antagonist of SDF-1/CXCR4 signaling, alters fracture repair. J Orthop Res. 2012.
Ward R. An update on disordered iron metabolism and iron overload. Hematology. 2010;15:311–7.
Wan C, Gilbert SR, Wang Y, Cao X, Shen X, Ramaswamy G, et al. Activation of the hypoxiainducible factor-1alpha pathway accelerates bone regeneration. Proc Natl Acad Sci USA. 2008;105:686–91.
Donneys A, Deshpande SS, Tchanque-Fossuo CN, Johnson KL, Blough JT, Perosky JE, et al. Deferoxamine expedites consolidation during mandibular distraction osteogenesis. Bone. 2013;55:384–90.
Shen X, Wan C, Ramaswamy G, Mavalli M, Wang Y, Duvall CL, et al. Prolyl hydroxylase inhibitors increase neoangiogenesis and callus formation following femur fracture in mice. J Orthop Res. 2009;27:1298–305.
Stewart R, Goldstein J, Eberhardt A, Chu GT-MG, Gilbert S. Increasing vascularity to improve healing of a segmental defect of the rat femur. J Orthop Trauma. 2011;25:472–6.
Fan L, Li J, Yu Z, Dang X, Wang K. Hypoxia-inducible factor prolyl hydroxylase inhibitor prevents steroid-associated osteonecrosis of the femoral head in rabbits by promoting angiogenesis and inhibiting apoptosis. PLoS ONE. Public Library of Science; 2014;9:e107774. Pre-clinical evidence that small molecule PHD antagonists can mitigate avascular necrosis.
Rankin EB, Wu C, Khatri R, Wilson TLS, Andersen R, Araldi E, et al. The HIF signaling pathway in osteoblasts directly modulates erythropoiesis through the production of EPO. Cell. 2012;149:63–74 Vhl deletion in osteoprogenitors causes a high bone mass and HIF-dependent polycythemia.
Rabadi S, Udo I, Leaf DE, Waikar SS, Christov M. Acute blood loss stimulates fibroblast growth factor 23 production. Am J Physiol Renal Physiol. 2018;314:F132–9.
Flamme I, Ellinghaus P, Urrego D, Kruger T. FGF23 expression in rodents is directly induced via erythropoietin after inhibition of hypoxia inducible factor proline hydroxylase. Jelkmann WEB, editor. PLoS ONE. Public Library of Science; 2017;12:e0186979.
Clinkenbeard EL, Hanudel MR, Stayrook KR, Appaiah HN, Farrow EG, Cass TA, et al. Erythropoietin stimulates murine and human fibroblast growth factor-23, revealing novel roles for bone and bone marrow. Haematologica. Haematologica. 2017;102:e427–30.
Zhang Q, Doucet M, Tomlinson RE, Han X, Quarles LD, Collins MT, et al. The hypoxia-inducible factor-1α activates ectopic production of fibroblast growth factor 23 in tumor-induced osteomalacia. Bone Res. 2016;4:175–6.
Blau JE, Collins MT. The PTH-Vitamin D-FGF23 axis. Rev Endocr Metab Disord. Springer US. 2015;16:165–74.
Johnson EO, Soultanis K, Soucacos PN. Vascular anatomy and microcirculation of skeletal zones vulnerable to osteonecrosis: vascularization of the femoral head. Orthop Clin North Am. 2004;35:285–91–viii.
Hong JM, Kim T-H, Chae S-C, Koo K-H, Lee YJ, Park EK, et al. Association study of hypoxia inducible factor 1alpha (HIF1alpha) with osteonecrosis of femoral head in a Korean population. Osteoarthr Cartil. 2007;15:688–94.
Hong JM, Kim TH, Kim HJ, Park EK, Yang EK, Kim SY. Genetic association of angiogenesis- and hypoxia-related gene polymorphisms with osteonecrosis of the femoral head. Exp Mol Med. Nature Publishing Group. 2010;42:376–85.
Radke S, Battmann A, Jatzke S, Eulert J, Jakob F, Schutze N. Expression of the angiomatrix and angiogenic proteins CYR61, CTGF, and VEGF in osteonecrosis of the femoral head. J Orthop Res. Wiley-Blackwell. 2006;24:945–52.
Weinstein RS, Hogan EA, Borrelli MJ, Liachenko S, O'Brien CA, Manolagas SC. The Pathophysiological Sequence of Glucocorticoid-Induced Osteonecrosis of the Femoral Head in Male Mice. Endocrinology. 2017;158:3817–31.
Fowler TW, Acevedo C, Mazur CM, Hall-Glenn F, Fields AJ, Bale HA, et al. Glucocorticoid suppression of osteocyte perilacunar remodeling is associated with subchondral bone degeneration in osteonecrosis. Sci Rep. 2017;7:44618.
Wickham N, Crawford A, Carney AS, Goss AN. Bisphosphonate-associated osteonecrosis of the external auditory canal. J Laryngol Otol. Cambridge University Press; 2013;127 Suppl 2:S51–3.
McCadden L, Leonard CG, Primrose WJ. Bisphosphonate-induced osteonecrosis of the ear canal: our experience and a review of the literature. J Laryngol Otol. Cambridge University Press. 2018;132:372–4.
Santini D, Vincenzi B, Dicuonzo G, Avvisati G, Massacesi C, Battistoni F, et al. Zoledronic acid induces significant and long-lasting modifications of circulating angiogenic factors in cancer patients. Clin Cancer Res. 2003;9:2893–7.
Xiong H, Wei L, Hu Y, Zhang C, Peng B. Effect of alendronate on alveolar bone resorption and angiogenesis in rats with experimental periapical lesions. Int Endod J. Wiley/Blackwell (10.1111); 2010;43:485–91.
Soki FN, Li X, Berry J, Koh A, Sinder BP, Qian X, et al. The effects of zoledronic acid in the bone and vasculature support of hematopoietic stem cell niches. J Cell Biochem. Wiley-Blackwell. 2013;114:67–78.
Zhang L, Wang T, Chang M, Kaiser C, Kim JD, Wu T, et al. Teriparatide Treatment Improves Bone Defect Healing Via Anabolic Effects on New Bone Formation and Non-Anabolic Effects on Inhibition of Mast Cells in a Murine Cranial Window Model. J Bone Miner Res. Wiley-Blackwell. 2017;32:1870–83.
Jilka RL, O'Brien CA, Bartell SM, Weinstein RS, Manolagas SC. Continuous elevation of PTH increases the number of osteoblasts via both osteoclast-dependent and -independent mechanisms. J Bone Miner Res. Wiley-Blackwell. 2010;25:2427–37.
Isowa S, Shimo T, Ibaragi S, Kurio N, Okui T, Matsubara K, et al. PTHrP regulates angiogenesis and bone resorption via VEGF expression. Anticancer Res. 2010;30:2755–67.
Prisby R, Guignandon A, Vanden-Bossche A, Mac-Way F, Linossier M-T, Thomas M, et al. Intermittent PTH(1-84) is osteoanabolic but not osteoangiogenic and relocates bone marrow blood vessels closer to bone-forming sites. J Bone Miner Res. 2011;26:2583–96.
Rhee Y, Park S-Y, Kim YM, Lee S, Lim SK. Angiogenesis inhibitor attenuates parathyroid hormone-induced anabolic effect. Biomed. Pharmacother. 2009;63:63–8.
Frey JL, Stonko DP, Faugere M-C, Riddle RC. Hypoxia-inducible factor-1α restricts the anabolic actions of parathyroid hormone. Bone Res. 2014;2:14005.
Riddle RC, Clemens TL. Bone Cell Bioenergetics and Skeletal Energy Homeostasis. Physiological Reviews. 2017;97:667–98.
Acknowledgements
We are grateful to those whose work was cited within and to those whose work was not due to space limitations. Research reported in this publication was supported by the National Institute of Arthritis and Musculoskeletal and Skin Diseases of the National Institutes of Health under award R01AR064255 (DCG).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Clare Yellowley and Damian Genetos declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Disclaimer
The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Skeletal Biology and Regulation
Rights and permissions
About this article
Cite this article
Yellowley, C.E., Genetos, D.C. Hypoxia Signaling in the Skeleton: Implications for Bone Health. Curr Osteoporos Rep 17, 26–35 (2019). https://doi.org/10.1007/s11914-019-00500-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-019-00500-6