Abstract
Nonspecific lipid transfer proteins (LTPs) are important allergens in fruits, vegetables, nuts, pollen, and latex. Despite their wide distribution throughout the plant kingdom, their clinical relevance is largely confined to the Mediterranean area. As they can sensitize via the gastrointestinal tract, LPTs are considered true food allergens, and IgE reactivity to LTPs is often associated with severe systemic symptoms. Although Pru p 3 represents the predominant LTP in terms of patients’ IgE recognition, the contribution of pollen LTPs in primary sensitization cannot be ruled out. Due to structural homology, LTPs from different allergen sources are generally IgE cross-reactive. However, sensitization profiles among allergic patients are extremely heterogeneous, and individual cross-reactivity patterns can be restricted to a single LTP or encompass many different LTPs. Molecule-based approaches in allergy research and diagnosis are important for better understanding of LTP allergy and could assist clinicians with providing adequate patient-tailored advice.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Based on structural and evolutionary relationships, seed storage proteins, inhibitors of α-amylase, and trypsin, as well as nonspecific lipid transfer proteins (LTPs) can be integrated into the huge protein superfamily of prolamins. Currently, this superfamily contains more than 3,000 proteins originating from more than 250 species mainly found in the plant kingdom [1]. Although individual members of this huge protein family display little sequence similarity, they share common structural features based on a conserved scaffold of eight cysteine residues. Given that almost 10% of currently known allergens feature this motif, the prolamin superfamily comprises the highest number of allergens [2]. Typically, members of the prolamin superfamily are important allergens in plant seeds. LTPs represent an exception, as they also have been isolated from nonseed plant tissues, such as fruits, leaves, roots, and pollen. Therefore, their impact on allergic disease goes far beyond plant food allergy [3]. Gene expression of LTPs is stimulated by biotic and abiotic plant stress, a typical trait of the diverse group of pathogenesis-related (PR) proteins. Interestingly, 50% of fourteen defined PR protein families contain allergens, among them nonspecific LTPs, also known as the PR-14 protein family [4].
To date, the International Union of Immunological Societies Allergen Nomenclature Subcommittee lists 39 allergenic LTPs originating from fruits (n = 18), pollen of trees and weeds (n = 9), vegetables (n = 7), nuts and seeds (n = 4), as well as latex (n = 1) (Table 1). The present article provides an overview and update on the physicochemical and immunologic properties of these molecules and discusses their impact on the allergic patient.
Structure and Biological Function
Plant LTPs were found to be evolutionary distinct from those identified in animals and can be further divided into those that are specific for certain classes of phospholipids and those that can bind several classes of lipids (termed nonspecific LTPs). Only the latter class was shown to contain allergens.
Structure and Lipid-binding Capacity
According to their molecular masses, nonspecific LTPs can be classified into the 9-kDa LTP1 and the 7-kDa LTP2 subfamilies. To date, several three-dimensional structures from members of both subfamilies have been solved by nuclear magnetic resonance and x-ray crystallography. Although they differ in their amino acid sequence, they display a similar secondary structure composed of four α-helices and share a basic isoelectric point as well as the typical prolamin cysteine signature (C-Xn-C-Xn-CC-Xn-CXC-Xn-C-Xn-C) (Fig. 1) [5•]. The large internal, tunnel-like cavity of both LTP subfamilies can accommodate a variety of lipids through interaction with their hydrophobic parts. It was further demonstrated that lipid-binding cavities exhibit high plasticity and flexibility and vary among individual members of the LTP family. Small hydrophobic amino acids (eg, Ile, Val, Leu, and Ala) appear throughout the LTP1 sequences. Some of these residues play an important role in defining the hydrophobic tunnel, showing affinity for a variety of lipids (eg, phospholipids, glycolipids, fatty acids, and acyl coenzyme A). Interestingly, three-dimensional structures of family 1 LTPs from rice and wheat revealed simultaneous interactions with two lipid molecules bound in a “tail-to-tail” conformation. Although smaller, the cavity of family 2 LTPs has been reported to be more flexible, resulting in binding of a wider variety of lipids, including sterols [6]. A recent study showed that lipid binding to Par j 1 and Par j 2 did not cause structural alterations but rather protected the disulfide bond-stabilized structure from reduction by dithiothreitol [7]. Thus, binding of naturally occurring ligands may stabilize the fold and therefore contribute to the allergenic potential of LTPs.
Structural features of plant lipid transfer proteins (LTPs). Comparison of primary and tertiary structures of rice LTP1 and LTP2 reveals that LTP subfamilies display less than 30% sequence homology but share a similar α-helical fold (highlighted in yellow) that is stabilized by four disulfide bonds (depicted in red). Identical amino acids are indicated by asterisks, and cysteine residues showing the typical prolamin distribution pattern (C-Xn-C-Xn-CC-Xn-CXC-Xn-C-Xn-C) are numbered consecutively from 1 to 8. Linear IgE-binding epitopes of peach LTP are exposed to the allergen’s surface and illustrated in green (Pru p 311–20), blue (Pru p 331–40), and purple (Pru p 371–80), respectively. All models were obtained from the Protein Structure Database (http://www.pdb.org) and visualized using the program chimera (http://www.cgl.ucsf.edu/chimera)
Biological Function
LTPs mainly localize in epidermal plant tissues, and corresponding gene products are secreted and accumulate outside the cell walls of aerial organs (LTP1) or roots (LTP2). Because of their lipid-binding capacities, LTPs have been suggested to be involved in the transport of hydrophobic monomers that compose the waxy and polymeric cutin and suberin layers of plant tissues found above and below the ground, respectively [8]. However, their extracellular localization contradicts the originally proposed role in intracellular trafficking of lipids. Thus, the actual in vivo function of this plant protein family remains unclear. Based on the finding of their ability to inhibit microbial growth in vitro, LTPs are reported to be involved in the defense against bacterial and fungal pathogens. This function is supported by the fact that LTP expression is increased upon pathogen challenge. Although exact mechanisms have not been revealed, it was speculated that LTP toxicity results from interaction with biological membranes, possibly leading to permeabilization and loss of membrane integrity. For example, sunflower LTP was demonstrated to induce weak leakage of model membranes (liposomes) and is able to provoke permeabilization of intact spores of the pathogenic fungus Fusarium solani [9]. In addition to biotic factors, abiotic stressors such as drought, cold, and high salinity have been reported to upregulate LTP production in some plant species [5•]. Due to their role in plant defense, LTPs have been classified as PR-14 protein members [4].
Allergological Relevance and Distribution
Although the biological function of plant LTPs is not completely elucidated, their conservation during evolution and expansion throughout the plant kingdom indicates an involvement in vital processes. Allergens displaying such properties are frequently responsible for IgE cross-reactions, even between unrelated pollen and plant food allergen sources, and therefore were classified as “eurallergens,” emphasizing their wide distribution [3]. However, IgE sensitization to LTPs is strongly influenced by geographic aspects and may largely depend on differences in eating habits or patterns of pollen exposure.
Geographic Distribution
Plant Food Lipid Transfer Proteins
In the Mediterranean area, LTPs are major allergens from Rosaceae spp fruits, as well as different vegetables and nuts. Among food-related LTPs (n = 36), Pru p 3 represents the most studied in terms of epidemiology. Pru p 3-positive tests range between 4.6% and 100%, depending on selection criteria, geographic location, and number of participants (Table 2). Barber et al. [10] reported 13% positive Pru p 3 test results among 785 Spanish study participants. An epidemiologic study ranked Pru p 3 16th among 75 tested allergens on a microarray chip and first among all food-related allergens, with a sensitization prevalence of 9.8% [11]. Large screenings of Rosaceae fruit allergic patients from different countries showed that in Northern and Central Europe, where birch trees are abundant, allergy to apple and cherry seems to be linked to food homologues of Bet v 1, the birch pollen major allergen. By contrast, in the Mediterranean area, allergy to Rosaceae fruits is related to peach allergy and sensitization to LTPs [12]. Notably, LTPs essentially concentrate in the pericarp of fruits, whereas the pulp contains lower amounts [13]. This explains why some patients can more easily tolerate fruits after peeling. Protein levels of LTPs vary depending on maturity, storage conditions, and cultivar of the fruit [14]. However, studies that would determine a threshold level for LTP sensitization for triggering allergic reactions are still lacking.
Plant food LTPs are also present in cutin-free plant tissues (eg, roots), which primarily express members of the LTP2 subfamily. Although both LTP1 and LTP2 proteins can be found in plant seeds, thus far, only LTP1 proteins have been characterized as allergens. In fact, the official allergen list of the International Union of Immunological Societies currently contains no entries for allergens belonging to the LTP2 subfamily. Recently, Ara h 9 has been described as major allergen in peanut-allergic patients from the Mediterranean area [15].
Studies on hazelnut allergy scored Cor a 8 between 0% and 71%, and among 4,297 Italian study participants, 5.7% tested positive for Cor a 8 in a microarray system (Table 2). Although most data on LTPs were gathered from the Mediterranean area, scattered reports show LTP reactivity worldwide, although at a very low prevalence [16]. For example, a study evaluating sensitization to LTPs in Dutch children concluded that sensitization to Cor a 8 is a risk factor for severe symptoms in response to ingestion of hazelnut not only in the Mediterranean but also in birch-endemic areas [17].
Pollen Lipid Transfer Proteins
In addition to plant-derived foods, LTPs also constitute important pollen allergens of plant species native to the Mediterranean basin (eg, pellitory [18], olive [10], plane [19], and mugwort [20]). Among inhaled LTPs causing respiratory symptoms, the highest prevalence has been reported for Par j 1 and Par j 2 from Parietaria spp, ranging from 0% to 85%, depending on patient selection criteria and countries (Table 2). A large study using simplex IgE testing in a Spanish population (n = 786) reported a prevalence rate of 8.3% for Par j 2 [10]. According to Scala et al. [11], the frequency of IgE reactivity to Par j 2 and Par j 1 measured by the Immuno Solid-phase Allergen Chip in a very large Italian cohort of unselected allergic participants (n = 16,408) is 25.7% and 22.2%, respectively, ranking these molecules sixth and ninth among 75 tested allergens. Prevalence of Art v 3 sensitization was reported to range from 0% to 88.9%. A recent study reported a sensitization rate of 7.7% to Art v 3 in an unselected cohort of 4,297 allergic patients [21]. Concerning Ole e 7, Barber et al. [10] reported a prevalence rate of almost 15% among 786 participants. Pollen LTPs from ragweed and plane tree have been reported positive from 11% to 41% and 51.7%, respectively (Table 2). However, as only a few studies on a limited number of selected patients are available for these pollen LTPs, the prevalence is thought to be lower. Interestingly, LTPs also have been detected in the pollen of Rosaceae trees, thus constituting an additional source of exposure [22••].
The Sensitizer Question
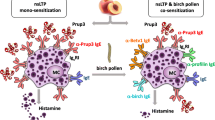
Ever since LTPs were identified as important allergens, a longstanding debate about the sensitizing molecule began, emphasizing a predominant role for peach LTP. In fact, IgE reactivity to any LTP under investigation is largely accompanied by Pru p 3 sensitization. Although some cases of IgE reactivity to pollen without concomitant Pru p 3 recognition have been described [19], the high frequency of sensitization and allergenicity renders Pru p 3 a marker molecule for LTP allergy. LTPs are generally considered true or class 1 food allergens that are able to sensitize via the gastrointestinal tract but also have been discussed in the context of class 2 food allergies due to IgE cross-reactivity between homologous pollen and food allergens. Typically, pollen allergens act as primary sensitizers in class 2 food allergies. However, in the case of LTPs, this picture is rather ambiguous. For example, in mugwort peach allergy, both Pru p 3 and Art v 3 have been suggested as the primary sensitizer, depending on selection of the study population [20, 23]. According to current knowledge, no evidence suggests a clinical association between sensitization to LTP from food and pollen. Still, it has been suggested that exposure to olive, pellitory, plane tree, and mugwort in the absence of birch pollen, as well as fruit consumption at a young age might facilitate the development of and in parallel explain the geographic restriction of LTP allergy [12, 24]. This suggestion is supported by the observation that the risk of sensitization to apple LTP seems to be decreased in patients suffering from birch pollinosis, whereas it is increased in patients with mugwort or plane pollen allergy [12]. In addition to ingestion and inhalation, skin contact has been proposed as a third route of LTP exposure. For example, the high allergen content in peels and cutin layers of fresh fruits has been proposed to be responsible for transdermal sensitization and peach-induced urticaria [25]. However, sensitization to Hev b 12 was shown to have no clinical relevance in contact allergy to natural rubber latex [26].
In summary, LTPs can be considered as widely distributed and cross-reactive “eurallergens” capable of sensitizing via the gastrointestinal and respiratory tracts as well as potentially across the skin. The clinical significance of LTPs is mainly confined to the Mediterranean area, where they represent major allergens and are particularly responsible for allergies to plant-derived foods.
Antigenic and Allergenic Determinants
T-cell Epitopes
Recently, two independent studies identified T-cell epitopes of Pru p 3 using T-cell lines from Spanish and Italian patients [27•, 28]. Despite some slightly controversial results, residues 61 to 80 were identified in both studies. In contrast to other plant food and pollen allergens, Pru p 3-specific T-cell clones demonstrated low production of interleukin-10 and a high expression of integrin β7, indicating that those cells were presumably primed in the gut [27•]. Although data on T-cell cross-reactivity are still missing, one could speculate that homologous LTPs present in various foodstuffs might be able to stimulate preexisting T cells, as was shown for Bet v 1-related food allergens [29].
B-cell Epitopes
Determination of linear IgE-binding epitopes using overlapping synthetic peptides yielded valuable information primarily for Pru p 3. As depicted in Fig. 1, three major epitopes were localized at residues 11 to 25, 31 to 45, and 71 to 80, which mainly corresponded to positively charged regions on the molecule’s surface [30]. In addition, residues R39, T40, and R44 were found to be critical for IgE recognition, as a Pru p 3 triple mutant displayed decreased antibody reactivity. A later study showed that LTPs of apple, apricot, and plum share consensus epitopes, which presumably accounts for pronounced IgE cross-reactivity between these molecules [31]. Interestingly, the sequence within residues 16 to 24 was found to be highly conserved among certain LTPs and seems to represent a Rosaceae-specific epitope. A consensual IgE-binding epitope (residues 39–44) in LTPs from various sources was predicted using a computational algorithm [32]. To determine conformational epitopes, mimotope mapping using a phage display library was applied for Pru p 3. The resulting mimotope recognized by patients with oral allergy syndrome was composed of L37R39T40P42D43R44A46P70S76Y79, whereas the mimotope for systemic patients consisted of N35N36L37R39T40D43A46S76P78 [33]. Apart from the fact that LTP symptom severity obviously cannot be fully explained by recognition of different epitopes, identified residues are also involved in the formation of linear allergenic determinants. As another example, allergenic epitopes of the wheat flour LTP were mapped presenting similar epitopes as described for Pru p 3 mimotopes [34]. However, two different sequential epitopes were identified pointing at a specific sensitization toward the allergen source. In addition, the major Parietaria allergens Par j 1 and Par j 2 were shown to contain five and eight IgE epitopes, respectively, three of which were similar on both molecules [18]. Taken together, clear evidence indicates that LTPs contain both linear and conformational IgE epitopes. Although LTPs are extremely heat stable, the allergenicity of those molecules can be reduced or abolished upon excessive heat treatment [35]. Particularly at neutral buffer conditions, the fold of Pru p 3 was shown to be irreversibly denatured [36]. In addition, the allergological relevance of the disulfide bond-stabilized structure was demonstrated with cysteine mutants of Par j 1 [37].
IgE Cross-reactivity
Prediction of antibody cross-reactivity relies on simple comparison of linear sequence stretches or on the three-dimensional structure. Allergenic members of the LTP family usually demonstrate moderate primary sequence identities ranging from 45% to 65% but are well above the currently defined cross-reactivity threshold of 35%. However, the highly conserved three-dimensional structure gives rise to additional epitopes involved in IgE cross-reactivity. Because sensitization and thus cross-reactivity show an extremely complex pattern, some examples of IgE cross-reactivity demonstrated for LTPs from plant foods and pollen are presented in the following sections.
Cross-reactivity Between Foods
A high degree of IgE cross-reactivity has been observed for allergenic LTPs within the Rosaceae family [38], including the potent sensitizer molecule Pru p 3. In fact, most of the known LTPs to date are members of this botanical family showing high sequence identity. Recently identified allergenic LTPs from various sources (eg, mulberry [21], peanut [15], mustard [39], lettuce [40], green bean [41], or cabbage [42]) all demonstrated in vitro cross-reactivity with Pru p 3. Although some variability exists among patients and in the degree of cross-reactivity, most previous studies showed that Pru p 3 is the most potent inhibitory molecule, while inhibition to Pru p 3 by other LTPs can only be partially achieved. In general, it seems that this molecule possesses more epitopes and/or epitopes with higher IgE-binding affinity compared with other LTPs [43]. Moreover, Pru p 3 also demonstrates a higher mediator release capacity in biological assays for most investigated patients’ sera. However, a weaker potency was found in a subgroup of lettuce allergic patients, suggesting a different source of sensitization [40].
Cross-reactivity Between Pollen and Food
The first evidence that LTPs from pollen and food sources demonstrate in vitro cross-reactivity came from studies that enrolled peach and mugwort LTP sensitized individuals. However, depending on different study populations, Pru p 3 [23] or Art v 3 [20] was considered the primary sensitizing molecule. A correlation between Art v 3 and Cas s 8 was found, as a positive skin prick test to chestnut LTP was only observed in Art v 3 sensitized patients [38]. The cabbage allergen, Bra o 3, was also found to cross-react with Art v 3 in inhibition experiments [42]. A study by Lauer et al. [19] showed that plane pollen LTP may also elicit allergic symptoms independent of preexisting Pru p 3 sensitization and may represent the sensitizing molecule in at least a subgroup of plane pollen allergic individuals [19]. Although Par j 1 and Par j 2 are considered members of the LTP family, they seem to play a unique role within this allergen group, with an evident restriction to Parietaria pollen allergy. In inhibition studies, Par j 2 demonstrates rather low or absent cross-reactivity with other allergenic LTPs [21, 44]. This may result from their low sequence identity (<35%) as well as structural differences due to longer protein sequences.
Clinical Picture of Lipid Transfer Protein Allergy
A broad spectrum of symptoms can be caused by ingestion or inhalation of LTPs, with severity ranging from rather mild to anaphylactic reactions. However, LTP sensitization without clinical translation also has been observed.
Symptoms Upon Ingestion
In most cases, the ingestion of plant food LTPs causes symptoms in the oral cavity. However, it became evident from very early reports on these allergens that they are also capable of eliciting severe generalized reactions. Unlike other allergen groups (eg. Bet v 1-related food allergens or profilins), LTPs can be responsible for severe reactions upon the ingestion of fresh as well as processed foods. In fact, it was shown that LTPs retain their allergenic activity during processing; thus, even cooked food, fruit juices, jams, and fermented drinks still display IgE-binding activity [22••]. It is noteworthy that LTPs were the only detectable allergens in different commercial tomato products [45]. In addition, several studies have demonstrated the resistance of LTPs to proteolysis by pepsin [22••], while gastric and duodenal digestion was assessed in detail for Vit v 1 [46]. Stability under such conditions is an important feature for class 1 food allergens, which can elicit systemic reactions and sensitize via the gastrointestinal tract. The remarkable physicochemical properties of LTPs render them potent elicitors of allergic reactions, including anaphylaxis. However, individuals do not necessarily react to all LTPs to which they are exposed. In the Italian population, most patients sensitized to Pru p 3 show clinical reactivity solely upon peach ingestion, whereas other fruits do not cause symptoms. In contrast, some Pru p 3-positive patients do react to a broad number of LTP-containing food sources. In between these two conditions is a wide range of clinical manifestations rendering the prediction of symptoms and diet recommendation difficult.
Symptoms Upon Inhalation
Individuals monosensitized to Parietaria pollen extract are now recognized to have IgE toward the two major allergens, Par j 1 and Par j 2. Due to the long-lasting pollen season causing the highest level of allergen exposure among allergenic pollen, up to 60% of the sensitized patients are affected by asthma symptoms associated with rhinoconjunctivitis [47]. Little is known about the relevance of other pollen LTPs (eg, Art v 3 or Pla a 3) in causing respiratory symptoms because patients often also display IgE antibodies against other allergens (eg, Art v 1, Pla a 1, and Pla a 2) from the same plants. To define the clinical profile of inhalant LTPs, the strategy could be to select sensitized patients who do not react to different and concurrent allergens.
Diagnostic Options and Treatment of Lipid Transfer Protein Allergic Patients
Diagnosis
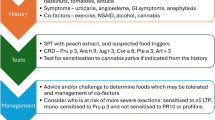
Routine clinical allergy diagnosis using commercially available extracts is hampered by the fact that products are not routinely standardized on LTPs. Thus, those molecules may be present at different amounts or totally absent as a consequence of extraction procedures, leading to false-negative results. The currently most reliable way to diagnose sensitization to LTP is based on purified molecules using, for example, microarray systems. At present, several LTPs have been successfully produced in Escherichia coli and Pichia pastoris. Recombinant allergens resembling the natural molecule have the advantage of being free of contaminating allergens from the same source. In general, molecule-based approaches result in the best patient profiles and help to decide whether to exclude/include certain plant-derived foods to prevent unnecessary diet restrictions.
Therapeutic Approach
Allergen avoidance and pharmacologic therapy remain the pillars to prevent allergic reactions to food LTPs. However, two studies using extracts with quantified LTPs have been published dealing with immunotherapy of hazelnut and peach LTP allergic patients [48, 49••]. Such preliminary studies pave the way to food allergy treatment. In this context, a European Union-funded project assessing the safety and efficacy of Pru p 3-based immunotherapy is currently in its second year. Three centers in Greece, Italy, and Spain are enrolling patients under very stringent selection criteria to determine the feasibility of a treatment for these highly affected patients. In general, consumption of carrots, potatoes, bananas, and melons was found to be safe for LTP allergic individuals [50]. Regarding the treatment of patients allergic to pollen LTPs, specific immunotherapy is performed with extracts and was shown to be clinically efficient.
Conclusions
The prevalence of allergic disease has been drastically increasing during recent decades in industrialized countries. This has been paralleled by fundamental environmental changes, such as increased pollution, reduced microbial burden, or altered socioeconomics. Many of those environmental changes may constitute abiotic stressors for plants and therefore influence expression and allergenicity of PR proteins. As a consequence, augmented exposure to LTPs could directly influence the frequency of sensitizations. However, this cannot explain the restriction of clinically relevant LTP allergy to the Mediterranean basin. Evidently, pollen of the predominant allergenic plants native to this area contains LTPs, whereas such pollen is rarely found in other geographic regions. In addition to Pru p 3, pollen LTPs should be considered more seriously with regard to the question of the primary sensitizer. Due to complex and individual sensitization patterns of LTP allergic patients, studies clearly addressing this topic are still missing. Although sensitization to LTPs displays a broad range of clinical manifestations, it is linked to severe anaphylactic symptoms in the Mediterranean population. In contrast to conventional allergy tests using extracts, molecule-based diagnosis allows the simultaneous testing of many allergenic LTPs, revealing patient-specific sensitization profiles. Such profiles would be useful for the clinician in providing adequate dietary advice and provide the basis for future therapeutic approaches.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Finn RD, Tate J, Mistry J, et al.: The Pfam protein families database. Nucleic Acids Res 2008, 36:D281–D288.
Radauer C, Bublin M, Wagner S, et al.: Allergens are distributed into few protein families and possess a restricted number of biochemical functions. J Allergy Clin Immunol 2008, 121:847.e7–852.e7.
Hauser M, Roulias A, Ferreira F, et al.: Panallergens and their impact on the allergic patient. Allergy Asthma Clin Immunol 2010, 6:1.
Hoffmann-Sommergruber K: Pathogenesis-related (PR)-proteins identified as allergens. Biochem Soc Trans 2002, 30:930–935.
• Salcedo G, Sanchez-Monge R, Barber D, et al.: Plant non-specific lipid transfer proteins: an interface between plant defence and human allergy. Biochim Biophys Acta 2007, 1771:781–791. This review article provides detailed information on structural features and biological function of plant-nonspecific LTPs.
Yeats TH, Rose JK: The biochemistry and biology of extracellular plant lipid-transfer proteins (LTPs). Protein Sci 2008, 17:191–198.
Gonzalez-Rioja R, Asturias JA, Martinez A, et al.: Par j 1 and Par j 2, the two major allergens in Parietaria judaica, bind preferentially to monoacylated negative lipids. FEBS J 2009, 276:1762–1775.
Douliez J, Michon T, Elmorjani K, et al.: Structure, biological and technological functions of lipid transfer proteins and indolines, the major lipid binding proteins from cereal kernels. J Cereal Sci 2000, 32:1–20.
Regente MC, Giudici AM, Villalain J, et al.: The cytotoxic properties of a plant lipid transfer protein involve membrane permeabilization of target cells. Lett Appl Microbiol 2005, 40:183–189.
Barber D, de la Torre F, Feo F, et al.: Understanding patient sensitization profiles in complex pollen areas: a molecular epidemiological study. Allergy 2008, 63:1550–1558.
Scala E, Alessandri C, Bernardi ML, et al.: Cross-sectional survey on immunoglobulin E reactivity in 23 077 subjects using an allergenic molecule-based microarray detection system. Clin Exp Allergy 2010, 40:911–921.
Fernandez-Rivas M, Bolhaar S, Gonzalez-Mancebo E, et al.: Apple allergy across Europe: how allergen sensitization profiles determine the clinical expression of allergies to plant foods. J Allergy Clin Immunol 2006, 118:481–488.
Borges JP, Jauneau A, Brule C, et al.: The lipid transfer proteins (LTP) essentially concentrate in the skin of Rosaceae fruits as cell surface exposed allergens. Plant Physiol Biochem 2006, 44:535–542.
Sancho AI, van Ree R, van Leeuwen A, et al.: Measurement of lipid transfer protein in 88 apple cultivars. Int Arch Allergy Immunol 2008, 146:19–26.
Lauer I, Dueringer N, Pokoj S, et al.: The non-specific lipid transfer protein, Ara h 9, is an important allergen in peanut. Clin Exp Allergy 2009, 39:1427–1437.
Gaier S, Oberhuber C, Hemmer W, et al.: Pru p 3 as a marker for symptom severity for patients with peach allergy in a birch pollen environment. J Allergy Clin Immunol 2009, 124:166–167.
Flinterman AE, Akkerdaas JH, den Hartog Jager CF, et al.: Lipid transfer protein-linked hazelnut allergy in children from a non-Mediterranean birch-endemic area. J Allergy Clin Immunol 2008, 121:423.e2–428.e2.
Asturias JA, Gomez-Bayon N, Eseverri JL, et al.: Par j 1 and Par j 2, the major allergens from Parietaria judaica pollen, have similar immunoglobulin E epitopes. Clin Exp Allergy 2003, 33:518–524.
Lauer I, Miguel-Moncin MS, Abel T, et al.: Identification of a plane pollen lipid transfer protein (Pla a 3) and its immunological relation to the peach lipid-transfer protein, Pru p 3. Clin Exp Allergy 2007, 37:261–269.
Lombardero M, Garcia-Selles FJ, Polo F, et al.: Prevalence of sensitization to Artemisia allergens Art v 1, Art v 3 and Art v 60 kDa. Cross-reactivity among Art v 3 and other relevant lipid-transfer protein allergens. Clin Exp Allergy 2004, 34:1415–1421.
Ciardiello MA, Palazzo P, Bernardi ML, et al.: Biochemical, immunological and clinical characterization of a cross-reactive nonspecific lipid transfer protein 1 from mulberry. Allergy 2010, 65:597–605.
•• Zuidmeer L, van Ree R: Lipid transfer protein allergy: primary food allergy or pollen/food syndrome in some cases. Curr Opin Allergy Clin Immunol 2007, 7:269–273. This review gives an excellent overview on the impact of protein stability and localization of LTPs related to sensitization and allergic reactions.
Pastorello EA, Pravettoni V, Farioli L, et al.: Hypersensitivity to mugwort (Artemisia vulgaris) in patients with peach allergy is due to a common lipid transfer protein allergen and is often without clinical expression. J Allergy Clin Immunol 2002, 110:310–317.
Reuter A, Lidholm J, Andersson K, et al.: A critical assessment of allergen component-based in vitro diagnosis in cherry allergy across Europe. Clin Exp Allergy 2006, 36:815–823.
Asero R, Mistrello G, Amato S, et al.: Peach fuzz contains large amounts of lipid transfer protein: is this the cause of the high prevalence of sensitization to LTP in Mediterranean countries? Eur Ann Allergy Clin Immunol 2006, 38:118–121.
Rihs HP, Rueff F, Lundberg M, et al.: Relevance of the recombinant lipid transfer protein of Hevea brasiliensis: IgE-binding reactivity in fruit-allergic adults. Ann Allergy Asthma Immunol 2006, 97:643–649.
• Schulten V, Radakovics A, Hartz C, et al.: Characterization of the allergic T-cell response to Pru p 3, the nonspecific lipid transfer protein in peach. J Allergy Clin Immunol 2009, 124:100–107. Within this study, T-cell epitopes of Pru p 3 were mapped, and it was further shown that the T-cell response is dominated by T-helper type 2 cells, which are presumably primed in the gut.
Tordesillas L, Cuesta-Herranz J, Gonzalez-Munoz M, et al.: T-cell epitopes of the major peach allergen, Pru p 3: identification and differential T-cell response of peach-allergic and non-allergic subjects. Mol Immunol 2009, 46:722–728.
Bohle B, Zwolfer B, Heratizadeh A, et al.: Cooking birch pollen-related food: divergent consequences for IgE- and T cell-mediated reactivity in vitro and in vivo. J Allergy Clin Immunol 2006, 118:242–249.
Garcia-Casado G, Pacios LF, Diaz-Perales A, et al.: Identification of IgE-binding epitopes of the major peach allergen Pru p 3. J Allergy Clin Immunol 2003, 112:599–605.
Borges JP, Barre A, Culerrier R, et al.: Lipid transfer proteins from Rosaceae fruits share consensus epitopes responsible for their IgE-binding cross-reactivity. Biochem Biophys Res Commun 2008, 365:685–690.
Borges JP, Barre A, Culerrier R, et al.: How reliable is the structural prediction of IgE-binding epitopes of allergens? The case study of plant lipid transfer proteins. Biochimie 2007, 89:83–91.
Pacios LF, Tordesillas L, Cuesta-Herranz J, et al.: Mimotope mapping as a complementary strategy to define allergen IgE-epitopes: peach Pru p 3 allergen as a model. Mol Immunol 2008, 45:2269–2276.
Tordesillas L, Pacios LF, Palacin A, et al.: Molecular basis of allergen cross-reactivity: non-specific lipid transfer proteins from wheat flour and peach fruit as models. Mol Immunol 2009, 47:534–540.
Sancho AI, Rigby NM, Zuidmeer L, et al.: The effect of thermal processing on the IgE reactivity of the non-specific lipid transfer protein from apple, Mal d 3. Allergy 2005, 60:1262–1268.
Gaier S, Marsh J, Oberhuber C, et al.: Purification and structural stability of the peach allergens Pru p 1 and Pru p 3. Mol Nutr Food Res 2008, 52(Suppl 2):S220–S229.
Bonura A, Amoroso S, Locorotondo G, et al.: Hypoallergenic variants of the Parietaria judaica major allergen Par j 1: a member of the non-specific lipid transfer protein plant family. Int Arch Allergy Immunol 2001, 126:32–40.
Garcia-Selles FJ, Diaz-Perales A, Sanchez-Monge R, et al.: Patterns of reactivity to lipid transfer proteins of plant foods and Artemisia pollen: an in vivo study. Int Arch Allergy Immunol 2002, 128:115–122.
Sirvent S, Palomares O, Vereda A, et al.: nsLTP and profilin are allergens in mustard seeds: cloning, sequencing and recombinant production of Sin a 3 and Sin a 4. Clin Exp Allergy 2009, 39:1929–1936.
Hartz C, San Miguel-Moncin Mdel M, Cistero-Bahima A, et al.: Molecular characterisation of Lac s 1, the major allergen from lettuce (Lactuca sativa). Mol Immunol 2007, 44:2820–2830.
Zoccatelli G, Pokoj S, Foetisch K, et al.: Identification and characterization of the major allergen of green bean (Phaseolus vulgaris) as a non-specific lipid transfer protein (Pha v 3). Mol Immunol 2010, 47:1561–1568.
Palacin A, Cumplido J, Figueroa J, et al.: Cabbage lipid transfer protein Bra o 3 is a major allergen responsible for cross-reactivity between plant foods and pollens. J Allergy Clin Immunol 2006, 117:1423–1429.
Zuidmeer L, Salentijn E, Rivas MF, et al.: The role of profilin and lipid transfer protein in strawberry allergy in the Mediterranean area. Clin Exp Allergy 2006, 36:666–675.
Gadermaier G, Harrer A, Girbl T, et al.: Isoform identification and characterization of Art v 3, the lipid-transfer protein of mugwort pollen. Mol Immunol 2009, 46:1919–1924.
Pravettoni V, Primavesi L, Farioli L, et al.: Tomato allergy: detection of IgE-binding lipid transfer proteins in tomato derivatives and in fresh tomato peel, pulp, and seeds. J Agric Food Chem 2009, 57:10749–10754.
Vassilopoulou E, Rigby N, Moreno FJ, et al.: Effect of in vitro gastric and duodenal digestion on the allergenicity of grape lipid transfer protein. J Allergy Clin Immunol 2006, 118:473–480.
D’Amato G, Ruffilli A, Sacerdoti G, et al.: Parietaria pollinosis: a review. Allergy 1992, 47:443–449.
Enrique E, Pineda F, Malek T, et al.: Sublingual immunotherapy for hazelnut food allergy: a randomized, double-blind, placebo-controlled study with a standardized hazelnut extract. J Allergy Clin Immunol 2005, 116:1073–1079.
•• Fernandez-Rivas M, Garrido Fernandez S, Nadal JA, et al.: Randomized double-blind, placebo-controlled trial of sublingual immunotherapy with a Pru p 3 quantified peach extract. Allergy 2009, 64:876–883. This article describes the first exploratory clinical trial for sublingual immunotherapy using a peach extract standardized on Pru p 3, providing promising therapeutic options for the treatment of food allergy.
Asero R, Mistrello G, Roncarolo D, et al.: Detection of some safe plant-derived foods for LTP-allergic patients. Int Arch Allergy Immunol 2007, 144:57–63.
Acknowledgment
The authors contributing to this work were supported by the Christian Doppler Research Association and Biomay AG, Vienna, Austria.
Disclosure
Dr. Ferreira has served as a consultant for Biomay AG. No other potential conflicts of interest relevant to this article were reported.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Egger, M., Hauser, M., Mari, A. et al. The Role of Lipid Transfer Proteins in Allergic Diseases. Curr Allergy Asthma Rep 10, 326–335 (2010). https://doi.org/10.1007/s11882-010-0128-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11882-010-0128-9