Abstract
The knowledge of ethnic-specific health needs is now essential to design effective health services and population-based prevention strategies. However, data on migrant populations living in Southern Europe are limited. The study is designed to investigate ethnic inequalities in hospitalization for acute myocardial infarction (AMI) in the Veneto region (Italy). Hospital admissions for AMI in Veneto for the whole resident population aged 20–59 years during 2008–2013 were studied. Age and gender-specific AMI hospitalization rates for immigrant groups (classified by country of origin according to the United Nations geoscheme) and Italians were calculated. The indirect standardization method was used to estimate standardized hospitalization ratios (SHR) for each immigrant group, with rates of Italian residents as a reference. Overall, 8200 AMI events were retrieved, 648 among immigrants. The highest risk of AMI is seen in South Asians males (SHR 4.2, 95% CI 3.6–4.9) and females (SHR 2.5, 95% CI 1.4–4.5). AMI rates in South Asian males sharply increase in the 30–39 years age class. Other immigrant subgroups (Eastern Europe, North Africa, Sub-Saharan Africa, other Asian countries, Central-South America, high-income countries) displayed age- and gender-adjusted hospitalization rates similar to the native population. Present findings stress the urgent need for implementation of ethnic-specific health policies in Italy. The awareness about the high cardiovascular risk in subjects from South Asia must be increased among general practitioners and immigrant communities.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The high rate of influx and settlement of migrant populations into Europe may pose important challenges for public health and clinical care [1]. The design of health services and implementation of population-based cardiovascular prevention (CV) strategies must now recognize the important ethnic inequalities in the incidence of CV diseases. Cultural factors may indeed limit the ability of interventions addressed at the native population to reach minority groups, and ethnic-specific data at the regional level are essential [2].
Immigrants from South Asia (Indian sub-continent) living in England were identified as a population at highly increased risk for acute myocardial infarction (AMI) early in the 1970s and 1980s, with rates between 1.4 and 5.0 greater than in the native population [3]. Increased AMI rates are observed in all South Asians with different religions, dietary habits and socioeconomic status, and are even more evident among subjects younger than 40 years [3]. Moreoever, the high incidence of AMI among South Asians is observed in different countries of Northern Europe such as Scotland [4], Sweden [5], Denmark [6], Norway [7], and the Netherlands [8]. Due to changes in diet and other lifestyles both among immigrants to Europe and North America, and within the Indian sub-continent, South Asians are expected to contribute 40% of the global cardiovascular diseases burden by 2020 [9]. In case–control studies carried out in Asian countries, a high prevalence of metabolic risk factors such as diabetes, high waist-to-hip ratio, and high apolipoprotein B100 to apolipoprotein A-I ratio is observed in young South Asians, possibly accounting for high AMI rates at earlier ages than in other ethnic groups [10]. Conversely, the situation is currently unknown in most countries in the South of Europe that have experienced a net increase in immigration during the last two decades [1]. In particular, during the 1990s and 2000s, the Veneto Region (Northeastern Italy, about 4,900,000 inhabitants) has been a destination area for economic migrants mainly from Eastern Europe, Africa, and Asia. The adult immigrant population is now mostly represented by first generation immigrants, and a high prevalence of diabetes is recently reported among South Asians [11, 12]. The aim of the study is to investigate variations in hospital admission rates for AMI across different immigrant groups in Veneto compared to the Italian population.
Methods
Population data by country of citizenship, gender, and age were available from the 2011 Italian official census (http://dati.istat.it/); the immigrant population was defined by a foreign (non-Italian) citizenship. To deal with larger numbers, countries were grouped by area of provenance based on a simplified version of macro-geographical regions and sub-regions defined by the United Nation Organization [13], already adopted in previous studies on the regional immigrant population [14]. Analyses were restricted to legal residents: irregular immigrants (illegal entry or legal entry followed by overstay), as well as subjects with a short-term stay in the region for tourism, study, or work were not included due to the lack of population data. All analyses excluded elderly subjects, and were limited to the 20–59 age band.
Admissions for AMI were retrieved from the regional archive of hospital discharge records for the period 2008–2013 (roughly centered around 2011 census data). The archive includes all hospitalizations in public and private hospitals, as well as admissions of residents to facilities outside the study area. The principal and up to five secondary discharge diagnoses are coded according to the International Classification of Diseases, 9th Revision, Clinical Modification (ICD9-CM). According to previous analyses on regional discharge records, an AMI was identified by a ICD-9-CM code 410.x1 in any diagnostic position (the fifth digit was restricted to 1, “the first episode of care” for AMI according to ICD9-CM); thereafter, a distinction was applied between non-ST-elevation myocardial infarction (NSTEMI, ICD-9-CM 410.71) and ST-elevation myocardial infarction (STEMI, fourth digit ≠ 7) [15]. To avoid double counting of the same AMI event, transfers between hospitals (e.g., from a facility without to a facility with cardiac surgery) were accounted for. All analyses were carried out on discharge records previously anonymized with a unique identification key, without any possibility of identification of individuals.
Age–gender-specific hospitalization rates were computed for the Italian and the immigrant population. To properly compare populations with huge differences in age structure, standardized hospitalization ratios (SHR) were computed as the ratios between admissions observed for each immigrant group, and those expected according to age- and gender-specific rates registered among Italian citizens. SHR were computed also separately for STEMI and NSTEMI. Finally, for Italians, South Asians, and all other immigrant groups combined, age-standardized rates were computed by the direct method; the new World standard population for the 20–59 years age interval was taken as a reference, with the following standardization weights applied across 5-year age classes: 0.154, 0.148, 0.142, 0.134, 0.123, 0.113, 0.101, 0.085. Hospitalization rates possibly include multiple events for the same subject through the study period; therefore, a sensitivity analysis was carried out restricted to the first hospitalization for each subject in 2008–2013.
Results
Out of 2,643,907 subjects aged 20–59 years resident in the Veneto region at the 2011 census, 315,080 (11.9%) have a foreign citizenship. The most represented immigrant groups are from Eastern Europe (56% of the overall immigrant population), North Africa (12%), Sub-Saharan Africa (9%), South Asia (9%), other Asian countries (7%), Central, and South America (4%), with only 3% being from EU15 and other high-income countries. Within South Asian immigrants, the most represented country is Bangladesh (37%), followed by India (33%), Sri-Lanka (23%), and Pakistan (6%). Table 1 shows that males prevail among immigrants from Africa and South Asia, and females among immigrants from South America and Eastern Europe. All immigrant sub-populations (except for subjects from high-income countries) are shifted toward younger ages with respect to Italians, especially those from South Asia.
Overall, 8200 AMI events were retrieved from hospitalization records in the study period; 648 involve residents with foreign citizenship. After adjustment for age, all immigrant subgroups display rates similar or lower than the native population, except for subjects from South-Asian countries, with a four-fold increased risk among males (Table 2). It is worth noting that South Asians, despite accounting for only 9% of all immigrants, represent 26% of all admissions for AMI among foreign citizens. Findings remain unchanged in analyses restricted to the first AMI experienced by each subject through the study period (n = 7895, data not shown).
AMI rates in South Asian males sharply increase as well in the 30–39 years age class, remaining much higher than those registered among Italians across older ages (Table 3). By contrast, in all the other immigrant subgroups combined, age-specific rates and age-standardized rates are close to those observed in the native population. A similar tendency, although based on small numbers, is observed among females.
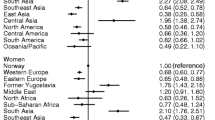
Figure 1 shows rate ratios broken down by type of AMI for the two immigrant groups with the largest numbers. Among subjects from Eastern Europe, figures are similar to the Italian population for both genders and AMI type. Among South Asians, estimates among females lack precision, whereas a greatly increased risk for both STEMI and NSTEMI can be confirmed for males.
Discussion
Our study shows that ethnic groups vary in risk of AMI, and identifies immigrants from South Asian countries as the subgroup with the highest SHR for AMI in both men and women.
This corresponds well with previous data collected in the same area, showing an unfavorable metabolic profile in this population group with a high prevalence of non-insulin-treated diabetes among South Asians aged 20–39 years [11]. Furthermore, immigrants in Italy with diabetes have a lower probability to undergo annual controls for glycated hemoglobin and renal function, [16] to be treated with glucose lowering drugs [17], and have poorer glycemic control with respect to the native population [18]. Study results are also concordant with the high risk of AMI observed among immigrants from South Asia living in different countries of Northern Europe compared to the native populations [4, 7, 8, 19]. In spite of all the above evidence, only few countries specifically consider ethnic minorities in their national health plans for metabolic and cardiovascular prevention. Furthermore, the main scientific societies in Europe still give limited attention to specific metabolic risk profiles in selected immigrant populations [20].
The present analyses reduce an informative gap already underlined in 2014 by a multidisciplinary task force calling for improving collection of data about immigrants’ health in Italy, aimed at supporting specific prevention policies to contrast cardiovascular diseases [21]. According to the present findings, the potential gains from controlling major established risk factors might be substantial in South Asians, and greater than in Italians. Except for diabetes, sparse data are available on cardiovascular risk factors among immigrants in Italy, and further observational research and intervention studies, especially among populations with South Asian ethnicity, are warranted. A recent meta-analysis of randomized controlled trials has shown that lifestyle interventions are highly effective within Asian populations [22]. However, it is also now evident that health services and prevention strategies have to be culturally tailored. Experience collected in old destination countries of immigration such as the Netherlands show that within overall declining of AMI rates, ethnic inequalities tend to persist, underlying the need of primary preventive strategies targeted at migrant groups with persistent higher incidence [23]. Among preventive measures, education needs to be reinforced, and subjects from South Asia need to be informed of their propensity to develop premature diabetes and coronary artery disease, to adopt appropriate dietary and lifestyle changes; health care personnel should be aware of ethnic-specific metabolic risks to appropriately screen immigrants from South Asia; finally, once high-risk patients are identified intensive cardiovascular risk reduction measures should be implemented [24]. In particular, in a high-risk group such as South Asians, screening and prevention strategies might effectively be addressed to the whole community to support a cultural change and an active participation in prevention programs [22].
The present study has a number of limitations. Rates were truncated at 59 years for two main reasons: elderly subjects are scarcely represented among the immigrant population, and an underestimation of rates among immigrants has been reported to be more probable in older age classes, mainly due to unregistered remigration to the country of origin [14, 25]. Based on available population data, population groups were defined by citizenship. Immigrants can obtain the Italian citizenship by marriage or—on demand—after a minimum of 10 consecutive years of legal residence; therefore, subjects born abroad who acquired the Italian citizenship are excluded from immigrant groups and included in the Italian population. However, since immigration in Italy is a relatively recent phenomenon, this limit does not have an impact on main study findings. As the census takes place only every 10 years, to deal with reliable denominators for hospitalization rates, we restricted the analyses to years close to the census, which was assumed to provide the average population for the study period. This approach is commonly adopted in studies both on mortality among immigrant populations [14, 26], and on disease incidence, including AMI hospitalization rates across different ethnic groups [27]. The use of census data could have introduced a numerator/denominator bias; however, this bias should be of limited size in analyses by large area of provenence, and not by single country of citizenship. As a drawback, this choice excludes potentially useful analyses by single country within the Indian sub-continent; South Asian subgroups have been demonstrated to differ in terms of coronary heart disease rates and related risk factors [28]. Identification of hospitalizations for AMI and distinction between STEMI and NSTEMI are consistent with previously published findings [15] and with routinely adopted algorithms in our Region; however, we lack clinical validation studies on ICD9-CM codes for AMI. Since among South Asians, rates are increased both for STEMI and NSTEMI, it is unlikely that a differential misclassification of discharge codes (e.g., between unstable angina/other acute coronary diseases and NSTEMI) could explain study findings. The prevalence of risk factors and comorbidities might be assessed in subjects hospitalized for AMI, although underestimated based on secondary discharge diagnoses, but is unknown in the source population. Finally, information on time since arrival in Italy and on socio-economic status (education level, income) was not available.
Notwithstanding the above limitations, this report shows huge health inequalities across subpopulations of migrants living in Italy. The Italian health-care system is a comprehensive service with universal coverage and high ranks of attainment and performance [29]. However, the still unaddressed high cardiovascular risk in subjects from South Asia underlines the urgent need for health policies tailored to specific immigrant groups.
References
Rechel B, Mladovsky P, Ingleby D, Mackenbach JP, McKee M (2013) Migration and health in an increasingly diverse Europe. Lancet 381:1235–1245
Modesti PA, Perticone F, Parati G, Agabiti Rosei E, Prisco D (2016) Chronic disease in the ethnic minority and migrant groups: time for a paradigm shift in Europe. Intern Emerg Med 11:295–297
Hughes LO, Raval U, Raftery EB (1989) First myocardial infarctions in Asian and white men. BMJ 298:1345–1350
Fischbacher CM, Bhopal R, Povey C, Steiner M, Chalmers J, Mueller G, Jamieson J, Knowles D (2007) Record linked retrospective cohort study of 4.6 million people exploring ethnic variations in disease: myocardial infarction in South Asians. BMC Publ Health 7:142
Hedlund E, Lange A, Hammar N (2007) Acute myocardial infarction incidence in immigrants to Sweden. Country of birth, time since immigration, and time trends over 20 years. Eur J Epidemiol 22:493–503
Hempler NF, Larsen FB, Nielsen SS, Diderichsen F, Andreasen AH, Jørgensen T (2011) A registry-based follow-up study, comparing the incidence of cardiovascular disease in native Danes and immigrants born in Turkey, Pakistan and the former Yugoslavia: do social inequalities play a role? BMC Publ Health 11:662
Rabanal KS, Selmer RM, Igland J, Tell GS, Meyer HE (2015) Ethnic inequalities in acute myocardial infarction and stroke rates in Norway 1994–2009: a nationwide cohort study (CVDNOR). BMC Public Health 15:1073
van Oeffelen AA, Vaartjes I, Stronks K, Bots ML, Agyemang C (2013) Incidence of acute myocardial infarction in first and second generation minority groups: does the second generation converge towards the majority population? Int J Cardiol 168:5422–5429
Gholap N, Davies M, Patel K, Sattar N, Khunti K (2011) Type 2 diabetes and cardiovascular disease in South Asians. Prim Care Diabetes 5:45–56
Joshi P, Islam S, Pais P, Reddy S, Dorairaj P, Kazmi K, Pandey MR, Haque S, Mendis S, Rangarajan S, Yusuf S (2007) Risk factors for early myocardial infarction in South Asians compared with individuals in other countries. JAMA 297:286–294
Fedeli U, Casotto V, Ferroni E, Saugo M, Targher G, Zoppini G (2015) Prevalence of diabetes across different immigrant groups in North-eastern Italy. Nutr Metab Cardiovasc Dis 25:924–930
Testa R, Bonfigli AR, Genovese S, Ceriello A (2016) Focus on migrants with type 2 diabetes mellitus in European Countries. Intern Emerg Med 11:319–326
United Nations Statistic Division. Composition of macro geographical (continental) regions, geographical sub-regions, and selected economic and other groupings. http://unstats.un.org/unsd/methods/m49/m49regin.htm. Accessed 30 Sept 2016
Fedeli U, Ferroni E, Pigato M, Avossa F, Saugo M (2015) Causes of mortality across different immigrant groups in Northeastern Italy. PeerJ 3:e975
Brocco S, Fedeli U, Schievano E, Milan G, Avossa F, Visentin C, Alba N, Olivari Z, Di Pede F, Spolaore P (2006) Effect of the new diagnostic criteria for ST-elevation and non-ST-elevation acute myocardial infarction on 4-year hospitalization: an analysis of hospital discharge records in the Veneto Region. J Cardiovasc Med 7:45–50
Buja A, Gini R, Visca M, Damiani G, Federico B, Francesconi P, Donato D, Marini A, Donatini A, Brugaletta S, Baldo V, Bellentani M; Valore Project (2013) Prevalence of chronic diseases by immigrant status and disparities in chronic disease management in immigrants: a population-based cohort study. Valore Project. BMC Public Health 13:504
Modesti PA, Calabrese M, Malandrino D, Colella A, Galanti G, Zhao D (2016) New findings on type 2 diabetes in first-generation Chinese migrants settled in Italy: Chinese in Prato (CHIP) cross-sectional survey. Diabetes Metab Res Rev. doi:10.1002/dmrr.2835
Ballotari P, Caroli S, Ferrari F, Romani G, Marina G, Chiarenza A, Manicardi V, Giorgi Rossi P (2015) Differences in diabetes prevalence and inequalities in disease management and glycaemic control by immigrant status: a population-based study (Italy). BMC Public Health 15:87
Hammar N, Alfredsson L, Rosén M, Spetz CL, Kahan T, Ysberg AS (2001) A national record linkage to study acute myocardial infarction incidence and case fatality in Sweden. Int J Epidemiol 30(Suppl 1):S30–S34
Modesti PA (2015) Ethnicity: new challenge for cardiovascular prevention in Europe. Hypertension 66:464–465
Modesti PA, Bianchi S, Borghi C, Cameli M, Capasso G, Ceriello A, Ciccone MM, Germanò G, Maiello M, Muiesan ML, Novo S, Padeletti L, Palmiero P, Pillon S, Rotella CM, Saba PS, Scicchitano P, Trimarco B, Volpe M, Pedrinelli R, Di Biase M, Italiana Societa’, di Cardiologia (SIC); Societa’ Italiana dell’Ipertensione Arteriosa (SIIA); Societa’ Italiana di Medicina Interna (SIMI); Societa’ Italiana di Nefrologia (SIN); Associazione Medici Diabetologi (AMD); Associazione Italiana Aritmia e Cardiostimolazione (AIAC); Società Italiana dell’Obesità (SIO); Societa’ Italiana di Prevenzione Cardiovascolare (SIPREC); Osservatorio Nazionale della Sanità Elettronica e Telemedicina (ONSET) (2014) Cardiovascular health in migrants: current status and issues for prevention. A collaborative multidisciplinary task force report. J Cardiovasc Med 15:683–692
Modesti PA, Galanti G, Cala’ P, Calabrese M (2016) Lifestyle interventions in preventing new type 2 diabetes in Asian populations. Intern Emerg Med 11:375–384
van Oeffelen A, Agyemang C, Koopman C, Stronks K, Bots M, Vaartjes I (2014) Downward trends in acute myocardial infarction incidence: how do migrants fare with the majority population? Results from a nationwide study. Eur J Prev Cardiol 21:1493–1500
Bainey KR, Jugdutt BI (2009) Increased burden of coronary artery disease in South-Asians living in North America. Need for an aggressive management algorithm. Atherosclerosis 204:1–10
Spallek J, Arnold M, Razum O, Juel K, Rey G, Deboosere P, Mackenbach JP, Kunst AE (2012) Cancer mortality patterns among Turkish immigrants in four European countries and in Turkey. Eur J Epidemiol 27:915–921
Wild SH, Fischbacher C, Brock A, Griffiths C, Bhopal R (2007) Mortality from all causes and circulatory disease by country of birth in England and Wales 2001–2003. J Public Health 29:191–198
Nijjar AP, Wang H, Quan H, Khan NA (2010) Ethnic and sex differences in the incidence of hospitalized acute myocardial infarction: British Columbia, Canada 1995–2002. BMC Cardiovasc Disord 10:38
Williams ED, Nazroo JY, Kooner JS, Steptoe A (2010) Subgroup differences in psychosocial factors relating to coronary heart disease in the UK South Asian population. J Psychosom Res 69:379–387
World Health Organization (2000) The World health report 2000: health systems: improving performance. http://www.who.int/whr/2000/en/whr00_en.pdf?ua=1. Accessed 26 August 2016
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Statement of human and animal rights
In this retrospective study, all analyses were carried out on anonymized records, without any possibility of identification of individuals.
Informed consent
All analyses were carried out on anonymized records routinely collected during the delivery of health care. For this type of study, informed consent is not required.
Rights and permissions
About this article
Cite this article
Fedeli, U., Cestari, L., Ferroni, E. et al. Ethnic inequalities in acute myocardial infarction hospitalization rates among young and middle-aged adults in Northern Italy: high risk for South Asians. Intern Emerg Med 13, 177–182 (2018). https://doi.org/10.1007/s11739-017-1631-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11739-017-1631-y