Abstract
Background
We used the leptin-receptor (LPR)-deficient mice model (db/db), a spontaneous model of type 2 diabetes with early β cell dysfunction to determine whether a preventative sleeve gastrectomy (SG) is an effective technique for the treatment of β cell failure.
Methods
The animals operated at an early stage of life, prior to metabolic alterations, were used to study the molecular mechanisms of β cell function improvement after a SG.
Results
β cell function was significantly increased, and islet morphology remained normal, after the SG. The expression of Glut2, Pdx1, MafA, and Nkx6.1 were significantly increased after the SG. The expression of GLP-1 in the colonic tissue, as well as GLP-1R and PKC in islets, was significantly increased after the SG.
Conclusions
β cell dysfunction can be ameliorated by a preventative SG for db/db mice. Maintaining the GLP-1 pathway and key transcript factor (TF) activation contributes to the improvement of β cell function after a preventative SG.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bariatric surgery has been demonstrated to be an effective treatment for type 2 diabetes mellitus (T2DM) in patients with morbid obesity [1]. In general, prior to significant weight loss the anti-diabetic effect of surgery is observed, indicating that the anatomical manipulation is the underlying contributor to diabetes remission [2, 3]. β cell function is significantly improved after bariatric surgery [4, 5]. In recent years, the prevalence of the use of a sleeve gastrectomy (SG) has been increasing. SG can preserve total β cell mass in Goto-Kakizaki rats [6]. However, the success of T2DM treatment by SG was effected by many components including the patient’s age, body mass index, baseline functional status, comorbidities, C-peptide level, and duration of T2DM [7, 8]. Specially, recurrence of T2DM was associated with long duration of T2DM before the surgery [9–11]. Moreover, it is also reasonable that more complications, including organ failure, infection, and fistula, are feasible to observe in the patients with advanced stage T2DM after the surgery. So, the concept of “preventative” SG here is raised. Prior to metabolic alterations and at an early stage of life, SG was performed to prevent β cell failure, which was regarded as a “preventative” SG.
In this study, a preventative SG was performed on young leptin-receptor (LPR)-deficient (db/db) mice before evident metabolism abnormalities occurred. Our results demonstrate that the preventative SG resulted in very low mortality, significant weight loss, and maintenance of β cell function.
Materials and Methods
Animals
C57BLKS/J-Leprdb/m (db/m) heterozygotes for the diabetes spontaneous mutation (Leprdb) with normal in body weight, blood glucose, and plasma insulin, regarded as control in our study and C57BLKS/J-Leprdb/Leprdb (db/db) homozygous for Leprdb with elevation of blood glucose at 6 weeks of age were purchased from the Shanghai Laboratory Animal Center, Chinese Academy of Sciences (SLAC, CAS). All of the mice were housed in pathogen-free facilities with a 12-h light/dark cycle. Sleeve gastrectomy and sham operation were performed, respectively, on the db/db mice (db/db-S and db/db-Sham) at the age of 4 weeks under a microscope as previously described [12]. Briefly, under a microscope, laparotomy was followed by removal of ∼80 % of the stomach by cutting in near parallel to the greater curvature, 5 mm from gastroesophageal junction to 5 mm from the pylorus, leaving a narrow gastric tube in the lesser curvature approximately 5–6 mm wide. For sham operation, only retract the liver cranially and bluntly dissect the stomach from its surrounding ligaments. During the 7 days after the surgery, db/db-S and db/db-Sham were offered liquid diet and after that an ad libitum normal diet was resumed to be offered. All animals were killed at the age of 12 weeks. All of the animal experiments were conducted in accordance with the Guide for the Care and Use of Laboratory Animals published by the National Institutes of Health.
Glucose Tolerance Test and Metabolic Measurements
The mice were fasted for 12 h before the glucose tolerance test. The mice were injected intraperitoneally 1 g kg−1 glucose. The glucose measurements were taken up to 2 h post injection using One-Touch Ultra glucometers (LifeScan). The serum insulin levels were measured by a mouse insulin ELISA kit (Crystal Chem).
Histologic and Immunostaining Analyses
Pancreata were harvested and fixed in 4 % buffered formaldehyde. The immunohistologic analyses were performed on paraffin serial sections, as described previously [13]. The antibodies used for the immunochemistry and immunofluorescence assays are the following: polyclonal rabbit anti-Pdx1 antibody (1:3000, Abcam), polyclonal rabbit anti-MafA antibody (1:2000, Abcam), polyclonal rabbit anti-MafB antibody (1:100, Novus Biologicals), polyclonal rabbit anti-Nkx6.1 antibody (1:200, Novus Biologicals), polyclonal rabbit anti-Glut2 (1:400, Abcam), monoclonal mouse anti-insulin antibody (1:1000, Sigma), polyclonal rabbit anti-glucagon antibody (1:200, Cell Signaling Technology), polyclonal rabbit anti-Foxo1 antibody (1:100, Cell Signaling Technology). The images were acquired using a Zeiss confocal microscope or an Olympus system.
Isolation of Mouse Pancreatic Islets and Glucose-Stimulated Insulin Secretion (GSIS)
Pancreatic islets were isolated as previously described [13]. Briefly, the pancreases were digested with collagenase and dissociated vigorously by mechanical pipetting. The islets were “hand-picked” from dark-field dishes under a dissecting microscope and pooled for further analysis.
The islets were incubated over a period of 60 min in 1 ml Krebs–Ringer bicarbonate Hepes buffer (KRBH, 140 mM NaCl, 3.6 mM KCl, 0.5 mM NaH2PO4, 0.5 mM MgSO4, 1.5 mM CaCl2, 2 mM NaHCO3, 10 mM Hepes (pH 7.4), 0.25 % BSA) containing 2.8 mM/l glucose or 16.7 mM/l glucose. Experiments were conducted with three to five tubes for each condition. The insulin levels in the supernatant were measured by a mouse insulin ELISA kit (Crystal Chem).
Quantitative PCR Analysis
The total RNA extraction was performed on hand-picked islets using an RNeasy kit (Qiagen) according to the manufacturer’s instructions. Quantitative real-time polymerase chain reactions (PCRs) were performed as previously described [13]. The following primer pairs were used in this study:
MafA-fw, 5′-AGGAGGAGGTCATCCGACTG-3′;
MafA-rev, 5′-CTTCTCGCTCTCCAGAATGTG-3′;
Nkx6.1-fw, 5′-CTGCACAGTATGGCCGAGATG-3′;
Nkx6.1-rev, 5′-CCGGGTTATGTGAGCCCAA-3′;
Pdx1-fw, 5′-CCCCAGTTTACAAGCTCGCT-3′;
Pdx1-rev, 5′-CTCGGTTCCATTCGGGAAAGG-3′;
GLP-1-fw, 5′-TTACTTTGTGGCTGGATTGCTT-3′;
GLP-1-rev, 5′-AGTGGCGTTTGTCTTCATTCA-3′;
GLP-1R-fw, 5′-ACGGTGTCCCTCTCAGAGAC-3′;
GLP-1R-rev, 5′- ATCAAAGGTCCGGTTGCAGAA-3′;
Glut2-fw, 5′-TCAGAAGACAAGATCACCGGA-3′;
Glut2-rev, 5′-GCTGGTGTGACTGTAAGTGGG-3′;
Statistical Analysis
All of the results are reported as the means ± standard errors of the mean. Differences for continuous variables were assessed by performing t test, ANOVA or, ANCOVA as appropriate. Bonferroni’s correction was used for the post hoc analyses, P values less than 0.05 were considered significant. All of the analyses were performed using the GraphPad Prism software (GraphPad Software Inc.).
Results
Mortality
Of the 18 db/db mice that underwent surgery at 4-week-old, two mice deceased post-operation (1-month survival rate 88.9 %). One mouse died within 72 h post-operation from acute intraperitoneal inflammation; the other mouse died 7 days post-operation with continuous weight loss. However, if the surgery was performed at 8-week-old mice, the 1-month survival rate dropped to 50 %; for 12-week-old mice, the rate dropped to 22 % (Fig. 1a).
Mortality of db/db mice operated at different ages. a For the db/db mice that underwent surgery at 4-week-old (n = 18), 1-month survival rate is 88.9 %. However, if the surgery was performed at 8-week-old mice (n = 10), the 1-month survival rate dropped to 50 %; for 12-week-old mice, the rate dropped to 22 % (n = 9)
β Cell Function Is Maintained After the SG
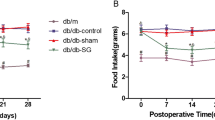
At 4 weeks of age, the body weight of the db/db mice was significantly increased compared with the db/m mice (Fig. 2a). An intraperitoneal glucose tolerance test (IPGTT) demonstrated that blood glucose levels in the db/db mice were similar with the db/m mice at 4 weeks of age (Fig. 2b). The IPGTT revealed a significant increase in plasma insulin levels at 15 and 30 min after glucose loading in the db/db mice compared with the db/m mice (Fig. 2c), suggesting that β cells could compensate to meet metabolic demand at this age. At 12 weeks, the body weight was significantly reduced in the db/db-S mice compared with the db/db-Sham mice (Fig. 2d). In addition, dynamic glucose monitoring showed that the random blood glucose was significantly reduced in the db/db-S mice compared with the db/db-Sham mice (Fig. 2e). The IPGTT revealed a significant reduction in blood glucose levels in the db/db-S mice compared with the db/db-Sham mice (Fig. 2f). A glucose-stimulated insulin secretion (GSIS) test showed insulin secretion from isolated islets from the db/db-S was significantly increased at both low and high glucose concentrations compared with the db/db-Sham mice (Fig. 2g). The general characteristics of three groups 8 weeks after the surgery were listed in Table 1.
Improvement of β cell function after the SG. a The body weight of the db/db mice (n = 9) was significantly increased compared with the control mice (n = 9) at 4 weeks of age. b The intraperitoneal glucose tolerance test (IPGTT) showed no significant difference in the blood glucose levels between the db/db (n = 6) and control (n = 6) mice at 4 weeks of age. c The plasma insulin levels at 15 and 30 min after the IPGTT were significantly increased in the db/db mice (n = 6) compared with the control mice (n = 6) at 4 weeks of age. d After the SG, the body weight of the db/db-S mice (n = 9) was significantly reduced compared with the db/db-Sham mice (n = 8) at 12 weeks of age. e The 24-h dynamic blood glucose monitoring showed that the random blood glucose levels were significantly reduced in the db/db-S mice (n = 7) compared with the db/db-Sham mice (n = 6) at 12 weeks of age. f The blood glucose levels at 0, 15, 30, 60, 90, and 120 min after the IPGTT were significantly reduced in the db/db-S mice (n = 6) compared with the db/db-Sham mice (n = 6) at 12 weeks of age. g The insulin secretion from the isolated islets was significantly increased after the glucose-stimulated insulin secretion (GSIS) test in the db/db-S mice (n = 12) compared with the db/db-Sham (n = 12) mice at 12 weeks of age. *P < 0.05, **P < 0.01, ***P < 0.001
The Change in Islet Morphology After the SG
To examine the effects of the SG on β cells, pancreatic sections were analyzed using hematoxylin-eosin (HE) staining and immunohistochemistry. The HE staining showed that the morphology of the islets in the db/db-S mice was similar with the controls, while the islets in the db/db-Sham mice were “disintegrated” (Fig. 3a). Insulin immunoreactivity in the β cells was reduced in combination with a relative increase in the number of intra-islet α cells in the db/db-Sham mice. In the db/db-S mice, insulin immunoreactivity was significantly increased, and the intra-islet α cells were significantly reduced compared with the db/db-Sham mice (Fig. 3b).
Maintaining the islet morphology after the SG. a The HE staining showed that the morphology of the islets in the db/db-Sham mice (n = 4), rather than the db/db-S mice (n = 4) was “disintegrated”. b A representative islet of the control (n = 4), db/db-Sham (n = 4), and db/db-S (n = 4) mice stained for insulin (red) and glucagon (Gcg; green). Increased intra-islet α cells were observed in the db/db-Sham mice, while most of the α cells located in the mantle of the islets were observed in the control and db/db-S mice. b The proportions of the Gcg positive cells observed in the islets in the control, db/db-Sham, and db/db-S mice. *P < 0.05
The Expression of Glut2 After the SG
Glut2 is the β cell’s principal glucose transporter and is essential for maintaining insulin secretion function [14]. Immunofluorescence staining showed a near complete loss of Glut2 expression in the db/db-Sham mice at 12 weeks of age. The expression of Glut2 was partly maintained in the db/db-S mice, although still significantly reduced compared with the control mice (Fig. 4a). The mRNA levels of Glut2 were also significantly increased in the islets of the db/db-S mice compared with the db/db-Sham mice (Fig. 4b).
The Expression of Specific β Cell Transcription Factors
Several transcription factors, such as Nkx6.1, MafA, and Pdx1, have been identified as playing important roles in β cell differentiation, maturation, and function maintenance [15, 16]. Immunofluorescence staining showed that the inactivation of Nkx6.1, MafA, and Pdx1 were observed in the islets of the db/db-Sham mice, while their expression levels were significantly increased in the db/db-S mice (Fig. 5a). The transcription factor Foxo1 integrates signals enforcing β cell fate under metabolic stress [17]. Immunostaining results showed that Foxo1 nuclear translocation was significantly increased in the islets of the db/db-Sham mice. However, similar to the control mice, the transcription factors were significantly reduced in the db/db-S mice (Fig. 5a). Moreover, the mRNA levels of Nkx6.1, Pdx1, and MafA were significantly higher in the islets of the db/db-S mice compared with the db/db-Sham mice (Fig. 5b).
The expression levels of the specific β cell transcription factors in the β cells in the control (n = 6), db/db-Sham (n = 6), and db/db-S (n = 6) mice. a The immunofluorescence analysis of Pdx1, MafA, Nkx6.1, and Foxo1 expression levels in the islets from the control, db/db-Sham, and db/db-S mice. The quantification of the percentage of β cells containing these transcription factors is shown. b The real-time PCR analysis of Pdx1, MafA, and Nkx6.1 expression in the islets i\n the control, db/db-Sham, and db/db-S mice. *P < 0.05, ***P < 0.001
The Expression of GLP-1-Pathway Associated Proteins
The expression of GLP-1 in colonic tissue was significantly reduced in the db/db-Sham mice, while its expression was maintained in the db/db-S mice (Fig. 6a). Moreover, the mRNA levels of GLP-1R and PKC in the islets were maintained in the db/db-S mice and significantly reduced in the db/db-Sham mice (Fig. 6b).
Discussion
In contrast to the high-fat-diet (HFD) mouse model, rapid progression of T2DM along with severe β cell dysfunction can be observed in db/db mice [18]. Both genetic (LPR defect) and environmental (excess food intake) effects contribute to the phenotypes. Our results demonstrate that a preventative SG significantly improved β cell function in db/db mice, indicating the importance of environmental components in maintaining β cell function. In fact, β cell dysfunction could present in individuals who are at high risk of developing T2DM even when their glucose levels are still normal [19], suggesting that therapeutic strategies to maintain β cell function at the early stage might benefit for pre-T2DM and T2DM population. Previous studies have shown that markedly reduced preoperative β cell function decreased the chances of T2DM remission in SG and other bariatric surgical procedures [20–22]. Therefore, for the subpopulation of the obesity-associated diabetes patients whose β cell function are easily impaired, an active or preventative SG could be encouraged for their diabetes care, which is supported by our results that a preventative SG led to lower mortality and satisfied outcomes in db/db mice.
However, although significantly effective, a preventative SG cannot maintain random blood glucose levels in a normal range as in the control in our study. It is well-known that a LPR defect results in neuroendocrine control impairment and hyperphagia [23]. Because after the SG the mice have free access to an ad libitum diet, it is supposed that combining a SG with caloric restriction would further benefit diabetes therapy.
Recent studies have identified transcription factors (TFs) that are critical for maintaining a mature β cell phenotype. The inactivation of specific β cell transcription factors results in β cells dysfunction [18]. Glut2 and Pdx1 are regarded as functional markers of mature β cells [24]. Loss of cytoplasmic expression of Glut2 and nuclear expression of Pdx1 are associated with early-onset islet dysfunction [25]. In fact, Glut2 expression in islets is known to be regulated by Pdx1. Therefore, the impaired expression of these two factors might have a common mechanism [26]. MafA is a master glucose-regulated TF that contributes to the maintenance of β cell differentiation and interacts with Pdx1 [27, 28]. After a preventative SG, the expression of these β cell specific TFs are maintained and constitute an interactive pathway that contributes to β cell function improvement.
After the SG, activation of the GLP-1 pathway was observed in our study, including increased expression of GLP-1 in the colonic tissue and GLP-1R and PKC in the islets. GLP-1 binds to GLP-1R and then regulates Pdx1 expression by PKC [29]. However, the role enhanced GLP-1 secretion after a SG plays roles in maintaining β cell function is controversial [30, 31]. The upregulation of GLP-1 and GLP-1R could be the result of chronic euglycemia [32]. A study of double mutant LPR−/−; GLP-1R−/− mice model may unveil the roles that GLP-1R signaling plays on β cell function improvement after a SG.
In conclusion, β cell dysfunction can be ameliorated by a preventative SG for db/db mice. Maintaining key transcript factor (TF) activation contributes to the improvement of β cell function after a preventative SG. Moreover, functional enteroinsular axis maintaining also benefits blood glucose control and β cell function improvement during this course. Therefore, our results shed light on the underlying molecular mechanisms for β cell function improvement after a preventative SG.
References
Tham JC, Howes N, le Roux CW. The role of bariatric surgery in the treatment of diabetes. Ther Adv Chronicle Dis. 2014;5(3):149–57.
Rubino F, Gagner M, Gentileschi P, et al. The early effect of the Roux-en-Y gastric bypass on hormones involved in body weight regulation and glucose metabolism. Ann Surg. 2004;240:236–42.
Basso N, Capoccia D, Rizzello M, et al. First-phase insulin secretion, insulin sensitivity, ghrelin, GLP-1, and PYY changes 72 h after sleeve gastrectomy in obese diabetic patients: the gastric hypothesis. Surg Endosc. 2011;25:3540–50.
Kashyap SR, Daud S, Kelly KR, et al. Acute effects of gastric bypass versus gastric restrictive surgery on beta-cell function and insulinotropic hormones in severely obese patients with type 2 diabetes. Int J Obes (Lond). 2010;34:462–71.
Nannipieri M, Mari A, Anselmino M, et al. The role of beta-cell function and insulin sensitivity in the remission of type 2 diabetes after gastric bypass surgery. J Clin Endocrinol Metab. 2011;96:E1372–9.
Grong E, Kulseng B, Arbo IB, Nord C, Eriksson M, Ahlgren U, Mårvik R. Sleeve gastrectomy, but not duodenojejunostomy, preserves total beta-cell mass in Goto-Kakizaki rats evaluated by three-dimensional optical projection tomography. Surg Endosc. 2015 Jun 12.
Lee WJ, Almulaifi A, Tsou JJ, Ser KH, Lee YC, Chen SC. Laparoscopic sleeve gastrectomy for type 2 diabetes mellitus: predicting the success by ABCD score. Surg Obes Relat Dis. 2014 Dec 31.
Khorgami Z, Andalib A, Aminian A, Kroh MD, Schauer PR, Brethauer SA. Predictors of readmission after laparoscopic gastric bypass and sleeve gastrectomy: a comparative analysis of ACS-NSQIP database. Surg Endosc. 2015 Aug 26. [Epub ahead of print].
Brethauer SA, Aminian A, Romero-Talamás H, et al. Can diabetes be surgically cured? Long-term metabolic effects of bariatric surgery in obese patients with type 2 diabetes mellitus. Ann Surg. 2013;258(4):628–36. discussion 636–7.
Runkel M, Müller S, Brydniak R, et al. Downgrading of type 2 diabetes mellitus (T2DM) after obesity surgery: duration and severity matter. Obes Surg. 2015;25(3):494–9.
Casella G, Abbatini F, Calì B, et al. Ten-year duration of type 2 diabetes as prognostic factor for remission after sleeve gastrectomy. Surg Obes Relat Dis. 2011;7(6):697–702.
Bruinsma BG, Uygun K, Yarmush ML, et al. Surgical models of Roux-en-Y gastric bypass surgery and sleeve gastrectomy in rats and mice. Nat Protoc. 2015;10(3):495–507.
Li F, Su Y, Cheng Y, et al. Conditional deletion of Men1 in the pancreatic β-cell leads to glucagon-expressing tumor development. Endocrinology. 2015;156(1):48–57.
Guillam MT, Hümmler E, Schaerer E, et al. Early diabetes and abnormal postnatal pancreatic islet development in mice lacking Glut-2. Nat Genet. 1997;17(3):327–30.
Pan FC, Wright C. Pancreas organogenesis: from bud to plexus to gland. Dev Dyn. 2011;240(3):530–65.
Wang H, Brun T, Kataoka K, et al. MAFA controls genes implicated in insulin biosynthesis and secretion. Diabetologia. 2007;50(2):348–58.
Homo-Delarche F, Calderari S, Irminger JC, et al. Islet inflammation and fibrosis in a spontaneous model of type 2 diabetes, the GK rat. Diabetes. 2006;55(6):1625–33.
Baetens D, Stefan Y, Ravazzola M, et al. Alteration of islet cell populations in spontaneously diabetic mice. Diabetes. 1978;27:1–7.
Kahn SE. Clinical review 135: the importance of beta-cell failure in the development and progression of type 2 diabetes. J Clin Endocrinol Metab. 2001;86(9):4047–58.
Eickhoff H, Guimarães A, Louro TM, et al. Insulin resistance and beta cell function before and after sleeve gastrectomy in obese patients with impaired fasting glucose or type 2 diabetes. Surg Endosc. 2015;29(2):438–43.
Mallipedhi A, Min T, Prior SL, et al. Association between the preoperative fasting and postprandial C-peptide AUC with resolution of type 2 diabetes 6 months following bariatric surgery. Metabolism. 2015;64(11):1556–63.
Ramos-Leví AM, Matía P, Cabrerizo L, et al. C-peptide levels predict type 2 diabetes remission after bariatric surgery. Nutr Hosp. 2013;28(5):1599–603.
Zhang Y, Proenca R, Maffei M, et al. Positional cloning of the mouse obese gene and its human homologue. Nature. 1994;372:425–32.
Ahlgren U, Jonsson J, Jonsson L, et al. Specific inactivation of the mouse Ipf1/Pdx1 gene results in loss of the β-cell phenotype and maturity onset diabetes. Genes Dev. 1998;12(12):1763–8.
Reimer MK, Ahrén B. Altered beta-cell distribution of pdx1 and GLUT-2 after a short-term challenge with a high-fat diet in C57BL/6J mice. Diabetes. 2002;51 Suppl 1:S138–43.
Waeber G, Thompson N, Nicod P, et al. Transcriptional activation of the GLUT2 gene by the IPF-1/STF-1/IDX-1 homeobox factor. Mol Endocrinol. 1996;19:1327–34.
Aramata S, Han SI, Kataoka K. Roles and regulation of transcription factor MafA in islet B-cells. Endocr J. 2007;54:659–66.
Raum JC, Gerrish K, Artner I, et al. FoxA2, Nkx2.2, and PDX-1 regulate islet beta-cell-specific mafA expression through conserved sequences located between base pairs −8118 and −7750 upstream from the transcription start site. Mol Cell Biol. 2006;26(15):5735–43.
Wang X, Cahill CM, Piñeyro MA, et al. Glucagon-like peptide-1 regulates the beta cell transcription factor, PDX-1, in insulinoma cells. Endocrinology. 1999;140(10):4904–7.
Jiménez A, Mari A, Casamitjana R, et al. GLP-1 and glucose tolerance after sleeve gastrectomy in morbidly obese subjects with type 2 diabetes. Diabetes. 2014;63(10):3372–7.
Wilson-Pérez HE, Chambers AP, Ryan KK, et al. Vertical sleeve gastrectomy is effective in two genetic mouse models of glucagon-like Peptide 1 receptor deficiency. Diabetes. 2013;62(7):2380–5.
Xu G, Kaneto H, Laybutt DR, et al. Downregulation of GLP-1 and GIP receptor expression by hyperglycemia: possible contribution to impaired incretin effects in diabetes. Diabetes. 2007;56(6):1551–8.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
All of the animal experiments were conducted in accordance with the Guide for the Care and Use of Laboratory Animals published by the National Institutes of Health.
Conflict of Interest
The authors declare no conflict of interest.
Statement of Animal Rights
All applicable institutional and/or national guidelines for the care and use of animals were followed.
Funding
This research is supported by grants from Shanghai Natural Science Foundation (14ZR1436600).
Disclosure Statement
The authors have nothing to disclose.
Additional information
Feng Li, Chunjun Sheng and Kexiu Song contributed equally to this work.
Rights and permissions
About this article
Cite this article
Li, F., Sheng, C., Song, K. et al. Preventative Sleeve Gastrectomy Contributes to Maintaining β Cell Function in db/db Diabetic Mouse. OBES SURG 26, 2402–2410 (2016). https://doi.org/10.1007/s11695-016-2112-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-016-2112-5