Abstract
Background
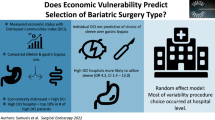
Patients with Medicaid are much less likely to undergo bariatric surgery compared to those with commercial insurance. The aims of this study were to compare outcomes after laparoscopic Roux-en-Y gastric bypass (LRYGB) for patients covered by Medicaid, other (non-Medicaid) government insurance, and commercial insurance.
Methods
This was a retrospective cohort study of all eligible patients who underwent LRYGB between July 2004 and October 2011 at a single university hospital (n = 450). Multivariable regression analysis was used to compare percent weight loss (PWL), absolute weight loss (AWL), hospital length of stay (LOS) ≥3 days, and 30-day readmission rates. Analyses were adjusted for appropriate covariates.
Results
There was a nonsignificant increase in PWL in Medicaid patients at 2 months (p = 0.08), 6 months (p = 0.09), and 12 months (p = 0.17) compared to commercial insurance patients. Similarly, there was a nonsignificant increase in AWL in Medicaid patients at 2 months (p = 0.054), 6 months (p = 0.08), and 12 months (p = 0.14) compared to commercial insurance patients. Medicaid patients had similar PWL and AWL compared to those with other government insurance (p ≥ 0.29 at all time points). Medicaid patients were more likely to have a hospital LOS ≥ 3 days (OR 2.03; 95 % confidence interval (CI) 1.09–3.77) and a hospital readmission within 30 days of discharge (odds ratio (OR) 2.84; 95 % CI 1.15–6.96) compared to commercial insurance patients.
Conclusions
These data should be considered as states expand Medicaid and make decisions regarding treatment of severe obesity. Interventions to decrease hospital LOS and the 30-day readmission rate, particularly in Medicaid patients, should be explored.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The prevalence of severe obesity, defined as a body mass index (BMI) ≥40 kg/m2, has increased from 1 % in 1990 to more than 6 % among adults in the USA (1). Severe obesity is strongly associated with chronic medical conditions, and it is a major contributor to disability and healthcare expenditures (2). There is a clear relationship between socioeconomic status (SES) and obesity, and prior studies have shown a more than threefold increase in severe obesity among those in the lowest SES quartile compared to those in the highest SES quartile (3).
Those who are severely obese are at high risk for morbidity and mortality (4). Medical, pharmaceutical, and behavioral therapy has short-term effectiveness of 5–10 % weight loss, but the recidivism rate is high (5). The effectiveness and safety of bariatric surgery in the laparoscopic and accredited programs has increased utilization of bariatric surgery as a management option. Among the bariatric surgery options, laparoscopic Roux-en-Y gastric bypass (LRYGB) has been the most frequently performed and shown in high quality data to be effective and durable (6–8).
Despite significantly higher rates of severe obesity and, therefore, eligibility for bariatric surgery, patients of lower SES groups who have Medicaid insurance are much less likely to undergo bariatric surgery compared to those with commercial insurance (9, 10). The underlying reason that fewer Medicaid patients undergo bariatric surgery compared to those with commercial insurance is somewhat unclear, but poorer access may be a critical factor, as many bariatric surgery centers do not accept Medicaid insurance and not all state Medicaid programs cover bariatric surgery (11). In addition, surgeons may be biased against operating on patients with Medicaid as a national survey of bariatric surgeons showed that public insurance significantly and independently decreased the odds that a surgeon would decide to perform bariatric surgery on a severely obese patient (12). Surgeons may be reluctant to operate on patients with Medicaid because prior data had suggested that patients with Medicaid have worse outcomes, including poorer postoperative weight loss, longer hospital stays, increased complications, and higher rates or readmission, although this is controversial (13–16).
Given the relationship between lower SES and severe obesity, the efficacy and safety of bariatric surgery in this population is an important area of investigation. The purpose of this study was to assess the relationship of Medicaid status with weight loss outcomes, hospital length of stay, and 30-day hospital readmissions after LRYGB surgery. We hypothesized that Medicaid patients would have similar weight loss but longer hospital stays and higher readmission rates compared to non-Medicaid populations.
Methods
This is a retrospective cohort study of consecutive patients who underwent laparoscopic Roux-en-Y gastric bypass (LRYGB) surgery between July 2004 and October 2011 at the University of Colorado Hospital (UCH). This study was approved by the Colorado Multiple Institutional Review Board.
Study Population
A database of patients who underwent bariatric surgery at UCH was reviewed to determine eligibility. Patients who underwent LRYGB met the standard eligibility criteria with a preoperative body mass index (BMI) of ≥40 kg/m2 (or ≥35 kg/m2 with one or more obesity-related complications). All patients had similar medical and psychiatric screening preoperatively, as well as nutritional and exercise counseling. Patients were excluded if they had an open RYGB or a prior history of any other weight loss surgery.
Data Collection
The bariatric surgery patient database includes type of bariatric surgery, date of surgery, age at surgery, gender, race, insurance provider at the time of surgery, preoperative weight, and obesity-related medical complications. The database also includes information on the indication for surgery and whether the patient has had any prior weight loss surgery. We then used the UCH electronic medical record system (Epic; Verona, WI) to extract additional clinical information for eligible patients, including weight at the standard 2-, 6-, and 12-month follow-up clinic visits. Discharge summaries were reviewed to determine hospital length of stay (LOS) following LRYGB. Patient records were reviewed to identify any hospitalizations that occurred within 30 days after discharge following LRYGB, including admissions to hospitals other than UCH as documented in clinic/telephone notes. All included patients had a documented phone encounter and/or clinic visit at least 30 days following discharge. In addition to reviewing the EMR, we separately queried our endoscopy reporting database (Provation; Minneapolis, MN) to identify all patients who had undergone an upper endoscopy within 12 months post-LRYGB and recorded whether a gastrojejunal (GJ) anastomotic ulcer or stricture occurred.
In total, 450 eligible patients underwent LRYGB during the study period. The main exposure of interest was the insurance status at the time of LRYGB. Insurance status was divided into three categories: (1) Medicaid (n = 183); (2) other (non-Medicaid) government insurance (n = 174), which was almost exclusively Tricare (government insurance for military personnel and their dependents; n = 165) with a few covered by Medicare (n = 9); and (3) commercial insurance (e.g., Cigna, United, etc.; n = 93). There were four primary outcomes: percent weight loss (PWL), absolute weight loss (AWL), hospital LOS ≥3 days after LRYGB, and hospital readmission within 30 days following discharge after LRYGB. PWL was calculated as [weight loss (in kg)/initial weight (in kg)] × 100. Absolute weight loss (AWL, in kg) was calculated as initial weight − weight (at specified time points). Due to patients being lost to follow-up, the patient population available for analyses for weight loss outcomes at 2 months (n = 399), 6 months (n = 318), and 12 months (n = 224) was reduced from the overall population (n = 450).
Statistical Analysis
Demographic and baseline characteristics of the three different groups (Medicaid, other government insurance, and commercial insurance) were compared using ANOVA and chi-square tests to describe the patient population. Multivariable analyses for PWL and AWL were performed using linear regression. Age, gender, pre-LRYGB BMI, and pre-LRYGB diagnoses of diabetes, obstructive sleep apnea, hypertension, and osteoarthritis were included as covariates for the PWL outcomes at 2, 6, and 12 months after LRYGB. Age, gender, pre-LRYGB body weight, and pre-LRYGB diagnoses of diabetes, obstructive sleep apnea, hypertension, and osteoarthritis were included for the AWL outcomes at 2, 6, and 12 months after LRYGB. Because hospital LOS was not distributed normally, the hospital LOS outcome was dichotomized into <3 and ≥3 days. Models for hospital LOS and the 30-day readmission outcomes were adjusted for age, gender, pre-LRYGB BMI, and pre-LRYGB diagnoses of diabetes, obstructive sleep apnea, hypertension, and osteoarthritis. All data were entered into and analyzed using STATA 10.0 statistical software (StataCorp, College Station, TX). The “predxcat” command was used in Stata to calculate means and proportions from the regression models for the PWL, AWL, hospital LOS, and 30-day readmission that were adjusted for the above covariates.
Results
Demographics
Baseline demographics and clinical characteristics were different across the three groups (Table 1). Overall, Medicaid patients were younger and had a higher proportion of women compared to the other two groups. Those with other government insurance had a lower preoperative body weight and BMI. With the exception of a lower prevalence of hypertension in the Medicaid group, the prevalence of obesity-related medical comorbidities preoperatively was similar across the three groups.
Percent Weight Loss
For all patients, the mean PWL (±SD) at 2 months post-LRYGB was 18.3 ± 5.2; the mean PWL (±SD) at 6 months post-LRYGB was 31.4 ± 5.9; and the mean PWL (±SD) at 12 months post-LRYGB was 38.7 ± 7.8. Preoperative BMI was positively associated with PWL at 2 months (p = 0.03) and 12 months (p = 0.003) after LRYGB. Age was negatively associated with PWL at 6 months (p = 0.05). A preoperative diagnosis of diabetes was associated with reductions in PWL at 6 months (p = 0.001) and 12 months (p < 0.001).
There was a nonsignificant increase in PWL for Medicaid patients compared to those with commercial insurance (Fig. 1) at 2 months (p = 0.08), 6 months (p = 0.09), and 12 months (p = 0.17). Medicaid patients had similar PWL compared to those with other government insurance at each of the three time points (all p ≥ 0.48). Patients with other government insurance had greater PWL at 6 months (by 2.1 ± 0.8 percentage points; p = 0.01) compared to those with commercial insurance.
Adjusted mean percent weight loss at 2 months (a), at 6 months (b), and at 12 months (c) after laparoscopic Roux-en-Y gastric bypass, by an insurance provider. Means calculated from the regression model adjusted for age, gender, pre-LRYGB body mass index, and pre-LRYGB diagnoses of diabetes, obstructive sleep apnea, hypertension, and osteoarthritis
Absolute Weight Loss
For all patients, the mean AWL (±SD) at 2 months post-LRYGB was 24.4 ± 9.4 kg; the mean AWL (±SD) at 6 months post-LRYGB was 41.2 ± 12.3 kg; and the mean AWL (±SD) at 12 months post-LRYGB was 50.5 ± 15.7 kg. Preoperative body weight was associated with AWL at 2, 6, and 12 months after LRYGB (all p < 0.001). Age was associated with AWL at 6 months (p = 0.03). A preoperative diagnosis of diabetes was associated with reductions in AWL at 6 months (p = 0.001) and 12 months (p < 0.001).
The results for AWL were similar to the PWL outcomes. There was a nonsignificant increase in AWL for Medicaid patients compared to those with commercial insurance (Fig. 2) at 2 months (p = 0.054), 6 months (p = 0.08), and 12 months (p = 0.14). Medicaid patients had similar AWL compared to those with other government insurance at each of the three time points (all p ≥ 0.29). Patients with other government insurance had greater AWL at 6 months (by 2.5 ± 1.2 kg; p = 0.03) compared to those with commercial insurance.
Adjusted mean absolute weight loss at 2 months (a), at 6 months (b), and at 12 months (c) after laparoscopic Roux-en-Y gastric bypass, by an insurance provider. Means calculated from the regression model adjusted for age, gender, pre-LRYGB body mass index, and pre-LRYGB diagnoses of diabetes, obstructive sleep apnea, hypertension, and osteoarthritis
Hospital Length of Stay After LRYGB
Overall, the mean hospital LOS (±SD) following LRYGB was 2.5 ± 1.2 days and was not statistically different among the three groups. However, because hospital LOS was not distributed normally, the hospital LOS outcome was dichotomized into <3 days and ≥3 days. A hospital LOS ≥3 days occurred in 130 patients (28.9 %), with the vast majority of those patients having a hospital LOS of either 3 days (n = 77) or 4 days (n = 26). Increasing age (p = 0.01), increasing preoperative BMI (p = 0.02), and a preoperative diagnosis of diabetes (p = 0.05) were associated with a hospital LOS ≥3 days. After adjusting for all covariates, patients with Medicaid were more likely to have a hospital LOS ≥3 days (odds ratio (OR) 2.03; 95 % confidence interval (CI) 1.09–3.77) compared to those with commercial insurance (Fig. 3). There was not a significant difference in the likelihood of having a hospital LOS ≥3 days for those with other government insurance compared to those with commercial insurance (OR 1.47; 95 % CI 0.80–2.71) and those with Medicaid (OR 0.72; 95 % CI 0.43–1.22).
Adjusted percentage of patients with a hospital length of stay (LOS) ≥3 days after laparoscopic Roux-en-Y gastric bypass, by an insurance provider. Percentages calculated from the regression model adjusted for age, gender, pre-LRYGB body mass index, and pre-LRYGB diagnoses of diabetes, obstructive sleep apnea, hypertension, and osteoarthritis
30-Day Hospital Readmission
Readmission to the hospital within 30 days of discharge after LRYGB occurred in 61 patients (13.6 %). The most common indications for readmission were nausea, vomiting, and/or dehydration (n = 21) and abdominal pain (n = 19). The other indications for readmission occurred with a frequency of ≤1 %, and included cardiovascular events (n = 1), thromboembolic complications (n = 2), wound infections (n = 2), gastrointestinal bleeding (n = 5), chest pain (n = 1), small bowel obstruction/ileus (n = 4), anastomotic leak/perforation (n = 2), and other (n = 4). A preoperative diagnosis of diabetes was associated with an increase in the odds of being readmitted to the hospital (p = 0.01). After adjusting for all covariates, patients with Medicaid were more likely to have a 30-day hospital readmission (OR 2.84; 95 % CI 1.15–6.96) compared to those with commercial insurance (Fig. 4). There was not a significant difference in the likelihood of a 30-day hospital readmission for those with other government insurance compared to those with commercial insurance (OR 1.64; 95 % CI 0.65–4.15) and those with Medicaid (OR 0.58; 95 % CI 0.30–1.13).
Adjusted percentage of patients readmitted within 30 days of discharge after laparoscopic Roux-en-Y gastric bypass, by an insurance provider. Percentages calculated from the regression model adjusted for age, gender, pre-LRYGB body mass index, and pre-LRYGB diagnoses of diabetes, obstructive sleep apnea, hypertension, and osteoarthritis
Anastomotic Complications
In total, 39 patients underwent an upper endoscopy within 1 year (8.7 %); 10 patients had a GJ anastomotic ulcer (2.2 %), and 9 patients had a GJ anastomotic stricture (2.0 %). Overall, there was no significant difference in the rates of the three groups undergoing an upper endoscopy (p = 0.41), having a GJ ulcer (p = 0.13), or having a GJ stricture (p = 0.30). The number of these events was too small to conduct multivariable analyses.
Discussion
Medicaid patients had similar weight loss at 2, 6, and 12 months post-LRYGB when compared to patients with other government insurance and those with commercial insurance. These observations are remarkable, as they do not demonstrate the usual disparity in health outcomes that is consistently seen with Medicaid patients (17–19). There is mixed prior data regarding the effect of insurance status on weight loss outcomes after bariatric surgery. Early studies reported that patients with Medicaid had poorer weight loss postoperatively, but more recent studies have shown that patients with Medicaid had similar weight loss outcomes (after adjusting for potential confounders) after both RYGB as well as sleeve gastrectomy(13, 15, 20). Our data support the conclusion that patients with Medicaid have effective weight loss following LRYGB.
Our study also showed that the mean hospital LOS was not significantly different among the three groups. However, Medicaid patients were more likely than those with commercial insurance to have a hospital LOS ≥3 days. The explanation for these somewhat contradictory results is not related to any increase in major postoperative complications. Instead, there was simply a higher percentage of Medicaid patients who were discharged on the third postoperative day compared to those with commercial insurance. Unfortunately, the retrospective nature of this study could not address the reasons behind this small delay in discharge. The finding of Medicaid patients having a hospital LOS ≥3 days was not related to associated comorbidities, as these were adjusted for in multivariable analysis. Furthermore, any residual confounding would likely have biased the results in favor of a lower rate of having a hospital LOS ≥3 days in the Medicaid group given that they were younger and had a slightly better comorbidity profile.
Previous studies are inconclusive with regards to whether patients with Medicaid have prolonged postoperative hospital stays following bariatric surgery. Using data from the National Hospital Discharge Survey, Dallal et al. showed that patients with Medicaid were more likely to have a prolonged hospital LOS (defined as at least 7 days) following bariatric surgery (21). Conversely, Akkray et al. did not demonstrate that patients with Medicaid were more likely to have a hospital LOS ≥3 days compared to those with private insurance, though the number of patients with Medicaid was relatively small (22). The definition of a prolonged hospital LOS is certainly a critical factor. Our results indicate that 10 % of Medicaid patients could be discharged 1 day sooner (based on the absolute difference in hospital LOS ≥3 days) compared to commercial insurance patients, but further understanding of the delay in discharge is necessary to inform what interventions might be necessary to achieve this outcome.
Another important finding in this study was that Medicaid patients were almost three times more likely to be readmitted within 30 days of hospital discharge compared to patients with commercial insurance. This data supports some previous published reports that suggested a higher readmission rate in patients with Medicaid following bariatric surgery (13, 23, 24). The large majority of these readmissions were for nonspecific abdominal pain and nausea and not for serious complications (bleeding, anastomotic leak/perforation, or wound infection). Similar to the finding for a hospital LOS ≥3 days, the higher rate of readmission in this study was not related to obesity-related comorbidities, as these were adjusted for in multivariable analysis. Again, any residual confounding would likely have biased the results in favor of a lower readmission rate within the Medicaid group given that they were younger and had a slightly better comorbidity profile. Medicaid patients tend to have higher rates of hospital readmission for all diagnoses, not just after bariatric surgery (25). This increased rate of hospital readmission provides an opportunity to develop interventions and/or protocols to decrease the 30-day readmission rate in Medicaid patients. This could include better postdischarge instructions and access to outpatient services that might prevent some of these readmissions.
The strengths of this study include that there was a large proportion of Medicaid patients compared to previous studies that had a small minority of Medicaid patients. In addition, because this was a single institution study, all patients received similar preoperative and postoperative care as per our institutional protocol. Another strength is the inclusion of a group with other (non-Medicaid) government insurance. The most pertinent limitation for the weight loss outcomes of the study was the number of patients lost to follow-up at 6 and 12 months post-LRYGB. However, the demographic and preoperative clinical characteristics of the Medicaid patients who were lost to follow-up at both time points were similar to both the Medicaid and non-Medicaid patients who did follow-up at 6 and 12 months. Previously reported studies (26) and data from this study confirm that early weight loss is the strongest predictor of long-term weight loss following bariatric surgery. Medicaid patients who were lost to follow-up at 6 months had similar weight loss outcomes at 2 months compared to Medicaid and non-Medicaid patients who returned at 6 months. Similarly, Medicaid patients who were lost to follow-up at 12 months had similar weight loss outcomes at 2 and 6 months compared to Medicaid and non-Medicaid patients who returned at 12 months. These data suggest the overall weight loss outcomes would likely not have been significantly altered with higher rates of follow-up.
Conclusion
Given similar weight loss and a significantly higher rate of severe obesity in the Medicaid population, eliminating barriers to increase utilization of bariatric surgery by Medicaid patients should be strongly considered as Medicaid eligibility expands. While patients with Medicaid had similar postoperative weight loss, they were more likely to have a hospital LOS of at least 3 days and were more likely to be readmitted to the hospital within 30 days of discharge. The LOS and readmission outcomes were not related to an increase in serious postoperative complications or to differences in underlying comorbidities. A deeper understanding of why these patients are being readmitted is necessary in order to design appropriate interventions to reduce hospital LOS and the readmission rate in the Medicaid population.
Abbreviations
- BMI:
-
Body mass index
- LRYGB:
-
Laparoscopic Roux-en-Y gastric bypass
- PWL:
-
Percent weight loss
- AWL:
-
Absolute weight loss
- SES:
-
Socioeconomic status
- LOS:
-
Length of stay
References
Flegal KM, Carroll MD, Kit BK, et al. Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999-2010. JAMA. 2012;307(5):491–7.
Finkelstein EA, Khavjou OA, Thompson H, et al. Obesity and severe obesity forecasts through 2030. Am J Prev Med. 2012;42(6):563–70. doi:10.1016/j.amepre.2011.10.026.
Baum 2nd CL, Ruhm CJ. Age, socioeconomic status and obesity growth. J Health Econ. 2009;28(3):635–48. doi:10.1016/j.jhealeco.2009.01.004. Epub Feb 5.
Whitlock G, Lewington S, Sherliker P, et al. Body-mass index and cause-specific mortality in 900 000 adults: collaborative analyses of 57 prospective studies. Lancet. 2009;373(9669):1083–96. doi:10.1016/S0140-6736(09)60318-4.
Johansson K, Neovius M, Hemmingsson E. Effects of anti-obesity drugs, diet, and exercise on weight-loss maintenance after a very-low-calorie diet or low-calorie diet: a systematic review and meta-analysis of randomized controlled trials. Am J Clin Nutr. 2014;99(1):14–23. doi:10.3945/ajcn.113.070052. Epub 2013 Oct 30.
Adams TD, Gress RE, Smith SC, et al. Long-term mortality after gastric bypass surgery. N Engl J Med. 2007;357(8):753–61.
Courcoulas AP, Christian NJ, Belle SH, et al. Weight change and health outcomes at 3 years after bariatric surgery among individuals with severe obesity. JAMA. 2013;310(22):2416–25. doi:10.1001/jama.2013.280928.
Sjostrom L, Narbro K, Sjostrom CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52.
Martin M, Beekley A, Kjorstad R, et al. Socioeconomic disparities in eligibility and access to bariatric surgery: a national population-based analysis. Surg Obes Relat Dis. 2010;6(1):8–15. doi:10.1016/j.soard.2009.07.003.
Birkmeyer NJ, Gu N. Race, socioeconomic status, and the use of bariatric surgery in Michigan. Obes Surg. 2012;22(2):259–65. doi:10.1007/s11695-010-0210-3.
Lee JS, Sheer JL, Lopez N, Rosenbaum S. Coverage of obesity treatment: a state-by-state analysis of Medicaid and state insurance laws. Public Health Rep. 2010;125(4):596-604.
Santry HP, Lauderdale DS, Cagney KA, et al. Predictors of patient selection in bariatric surgery. Ann Surg. 2007;245(1):59–67.
Alexander JW, Goodman HR, Martin Hawver LR, et al. The impact of medicaid status on outcome after gastric bypass. Obes Surg. 2008;18(10):1241–5.
Funk LM, Suzo A, Mikami DJ, et al. Two-Year outcomes for medicaid patients undergoing laparoscopic Roux-en-Y Gastric bypass: a case-control study. Obes Surg. 2014;26:26.
Melton GB, Steele KE, Schweitzer MA, et al. Suboptimal weight loss after gastric bypass surgery: correlation of demographics, comorbidities, and insurance status with outcomes. J Gastrointest Surg. 2008;12(2):250–5.
Nguyen GC, Patel AM. Racial disparities in mortality in patients undergoing bariatric surgery in the U.S.A. Obes Surg. 2013;23:1508–14. doi:10.1007/s11695-013-0957-4.
Ortega E, Morinigo R, Flores L, et al. Predictive factors of excess body weight loss 1 year after laparoscopic bariatric surgery. Surg Endosc. 2012;26(6):1744–50.
Kapoor JR, Kapoor R, Hellkamp AS, et al. Payment source, quality of care, and outcomes in patients hospitalized with heart failure. J Am Coll Cardiol. 2011;58(14):465–71. doi:10.1016/j.jacc.2011.06.034.
Banta JE, Joshi KP, Beeson L, et al. Patient and hospital characteristics associated with inpatient severe sepsis mortality in California, 2005-2010. Crit Care Med. 2012;40(11):2960–6. doi:10.1097/CCM.0b013e31825bc92f.
Madan AK, Tichansky DS, Ternovits CA, et al. Establishing a laparoscopic bariatric program in a safety net hospital. Surg Endosc. 2007;21(5):801–4.
Dallal RM, Datta T, Braitman LE. Medicare and Medicaid status predicts prolonged length of stay after bariatric surgery. Surg Obes Relat Dis. 2007;3(6):592–6.
Akkary E, Nerlinger A, Yu S, et al. Socioeconomic predictors of weight loss after laparoscopic Roux-Y gastric bypass. Surg Endosc. 2009;23(6):1246–51. doi:10.1007/s00464-008-0138-z.
Dallal RM, Bailey L, Guenther L, et al. Comparative analysis of short-term outcomes after bariatric surgery between two disparate populations. Surg Obes Relat Dis. 2008;4(2):110–4.
Hong B, Stanley E, Reinhardt S, et al. Factors associated with readmission after laparoscopic gastric bypass surgery. Surg Obes Relat Dis. 2012;8(6):691–5.
Fuller RL, Atkinson G, McCullough EC, et al. Hospital readmission rates: the impacts of age, payer, and mental health diagnoses. J Ambul Care Manag. 2013;36(2):147–55. doi:10.1097/JAC.0b013e3182866c1c.
Mor A, Sharp L, Portenier D, et al. Weight loss at first postoperative visit predicts long-term outcome of Roux-en-Y gastric bypass using Duke weight loss surgery chart. Surg Obes Relat Dis. 2012;8(5):556–60. doi:10.1016/j.soard.2012.06.014. Epub Jul 16.
Conflict of Interest
No conflicts of interest exist for any of the authors of this manuscript. No funding was obtained for this study.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Jensen-Otsu, E., Ward, E.K., Mitchell, B. et al. The Effect of Medicaid Status on Weight Loss, Hospital Length of Stay, and 30-Day Readmission After Laparoscopic Roux-en-Y Gastric Bypass Surgery. OBES SURG 25, 295–301 (2015). https://doi.org/10.1007/s11695-014-1367-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-014-1367-y