Abstract
Background
Laparoscopic sleeve gastrectomy (LSG) is a surgical procedure which reduces the gastric volume causing a feeling of early fullness while decreasing hunger due to a reduced secretion of ghrelin. This leads to a considerable loss of body weight. The purpose of this study was to assess the usefulness of early x-ray examination and subsequent x-ray follow-up in the detection of postoperative complications and long-term functional recovery.
Methods
From March 2010 to April 2011, 101 consecutive patients underwent LSG for morbid obesity and were subsequently included in this retrospective study. All patients were submitted to early x-ray examination 1–3 days after surgery and x-ray follow-up 3–6 months after surgery to detect the presence and persistence of surgical and functional complications.
Results
Early postoperative x-ray examination detected one case of suture leakage 1 day after surgery as well as one abscess and one gastric fistula in two patients who had become symptomatic 9 and 10 days after surgery.
Conclusions
Early x-ray examination showed that complications were mainly functional and rarely surgical. Subsequent follow-up showed that functional disturbances were significantly reduced over time. X-ray is an easy and reliable method for detecting complications and side effects of LSG. However, in view of the extremely low incidence of surgical complications revealed at the early x-ray examination, this procedure may not be required as a routine examination in all operated patients and should be performed only in patients who become symptomatic and those considered at risk of developing more serious complications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Laparoscopic sleeve gastrectomy (LSG) is a surgical procedure which reduces gastric volume causing a feeling of early fullness while decreasing hunger due to a reduced secretion of ghrelin, a hormone released by the cells in the fundus of the stomach [1]. This leads to a considerable loss of body weight which is usually maintained over time [2, 3]. Recently, thanks to the excellent results obtained in terms of excess weight loss (EWL) and safe postoperative outcome [4, 5], LSG has been proposed as a sole bariatric procedure [2].
Indications for LSG were initially restricted to super-obese patients (BMI >50 kg/m2) [6]. These indications have gradually been extended, and the guidelines of the American Society for Metabolic and Bariatric Surgery currently set forth the following indications: BMI >40 or >35 associated with comorbidities. Candidates for LSG must have a long clinical history of morbid obesity, unsuccessful dietary therapy, and be between the ages 18 and 65 years [7–9].
Also, in revision surgery, LSG is a valid solution in patients who experience insufficient EWL or weight regain after gastric banding or gastrointestinal bypass [10]. The most frequent complications after LSG are leaks, hemorrhage, gastric stricture, abscess, wound complications, and gastric dilatation. Diagnostic methods used to detect, diagnose, and confirm such complications are contrast swallow (Gastrografin) in the early follow-up study and multislice CT which is performed only in cases which are ambiguous [11–13].
The purpose of this retrospective study was to assess the usefulness of early x-ray examination and subsequent x-ray follow-up in the detection of postoperative complications and side effects and in the study of short- and long-term functional recovery.
Materials and Methods
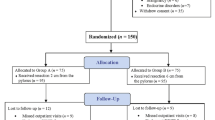
From March 2010 to April 2011, 148 consecutive patients underwent LSG in the department of laparoscopic surgery of the authors' university hospital. Of these patients, 101 were selected for this retrospective study as they could present reports from early postoperative x-ray examination and subsequent follow-up: 67 females (mean age, 49 years) and 34 males (mean age, 52.5 years); preoperative mean body mass index (BMI) was 45.36 and 47.15, respectively. Informed consent was obtained from all patients for the publication of this paper and related images.
LSG was performed according to the classical technique involving a longitudinal resection of the stomach on the greater curvature thereby reducing the stomach volume to 80–120 ml in order to avoid failure in treatment or early weight regain [14].
All patients underwent early x-ray examination 1–3 days after surgery and x-ray follow-up 3–6 months after surgery. Early postoperative morphological and functional x-ray examination was carried out after oral administration of water-soluble iodinated contrast medium (Gastrografin). The patient, in the standing position, swallowed the contrast medium (about 60 ml of Gastrografin dilution) under video-fluoroscopic observation which allowed evaluation of the staple line and functionality of the gastroesophageal tract and gastric tube. Late x-ray follow-up was performed using a radiopaque contrast medium consisting of barium sulfate suspension which was orally administered; this contrast medium was considered safe as the patients were already following a regular diet including solid and liquid food at the time of the follow-up, and they were all asymptomatic. Late follow-up permitted evaluation of the gastric function in the new anatomical condition.
Statistical analysis of the functional variation occurring between the early x-ray examination and the follow-up was carried out using the chi-square test (IBM SPSS Statistics).
Results
The x-ray pattern of the gastric tube of the 101 patients enrolled in this study was classified according to Werquin et al. [5]: tubular (53 %), superior pouch (28 %), and inferior pouch (19 %). Early x-ray examination revealed only one case of suture leakage (Fig. 1) occurring in a gastric tube classified as an inferior pouch pattern. In two patients, a small superior pouch was suspected, but x-ray revealed no suture leakage, and subsequent CT scan was negative. Nine days after surgery, an additional x-ray examination with oral administration of Gastrografin revealed gastric fistula in a patient who had developed fever and high white blood cell count. There were also six cases of clinical complications which were not detectable at x-ray examination: one case of peptic ulcer bleeding, one case of subhepatic abscess, three cases of suture infection, and one case of trocar site hernia (Table 1).
Patients who presented surgical complications did not undergo reoperation. Radiologically guided percutaneous drainage was placed in the patient with a subhepatic abscess; in the patients with leakage and gastric fistula, the treatment was conservative and consisted of jejunal enteral feeding and total parenteral nutrition; late follow-up revealed no anomaly in any of these patients.
As to gastroesophageal function after surgery (Table 2), early x-ray examination showed gastroesophageal reflux in 32 patients (27 females and 5 males), delayed gastroesophageal transit in 16 patients (12 females and 4 males), and delayed gastric emptying in 13 patients (10 females and 3 males). Late x-ray follow-up revealed persistent gastroesophageal reflux in 12 of the initial 32 patients (seven females and five males), delayed gastroesophageal transit in 3 of the initial 16 patients (three females), and disappearance of delayed gastric emptying in all 13 patients.
The data were submitted to the chi-square test with the following result: gastroesophageal reflux χ 2 = 10.489 (p = 0.0012), delayed gastroesophageal transit χ 2 = 8.366 (p = 0.0038), delayed gastric emptying χ 2 8.52 (p = 0.0035). LSG resulted in a reduction of mean BMI over 6–8 months from 45.36 before surgery to 41.6 after surgery (−9.1 %) in the female group and from 47.15 to 42.8 (−9 %) in the male group.
Discussion
Early x-ray examination and subsequent follow-up were easy to perform and well tolerated by all the patients despite two cases of transient nausea (1.98 %). LSG resulted in all patients in an EWL over 6–8 months of 17.7 % in the female group and of 15.9 % in the male group.
Early x-ray examination revealed only one case of surgical complication 1 day after surgery. Nine days after surgery, x-ray detected one case of gastric fistula in a patient who had developed fever and high white blood cell count. This fistula was probably missed at the early x-ray examination due to the smallness of the lumen or possibly due to increased pressure in the gastric stump occurring after the examination.
Another patient developed fever and strong pain in the upper right abdominal quadrant and was submitted to an additional x-ray examination which was negative for suture leakage and/or fistula; in this patient a subhepatic abscess was diagnosed by abdominal ultrasound and CT 10 days after surgery. The relatively late onset of these two complications (gastric fistula and presumably occult gastric fistula also in the patient with subhepatic abscess) appears consistent with ischemic injury and subsequent wall laceration [15].
As LSG preserves the integrity of the pyloric antrum and vagal innervation, the physiological functions of the stomach are maintained and digestion can occur naturally [16]. Few studies have addressed the effects of LSG on esophagogastric motility; two studies reported accelerated gastric emptying [5, 17] while another reported symptoms of gastroesophageal reflux.
The data related to the gastroesophageal function were submitted to the χ 2 test to evaluate the variation between early x-ray examination and follow-up. The test revealed a high statistical significance of the variation in gastroesophageal reflux (p = 0.0012), whereas variations in delayed gastroesophageal transit and delayed gastric emptying were less significant (p = 0.0038 and p = 0.0035, respectively).
The authors therefore believe that early x-ray examination is useful particularly for detecting gastroesophageal reflux in order to intervene with targeted therapies, if required, while early x-ray seems to be less useful with regard to the other two functional parameters considered.
The prevalence of early functional disorders in the female subgroup (gastroesophageal reflux, 84.4 % females vs 15.6 % males; delayed gastroesophageal transit, 75 % females vs 25 % males; delayed gastric emptying, 76.9 % females vs 23.1 % males, respectively) might be due to the fact that the study group counted more women than men (67 women vs 34 men).
As to the radiological patterns, it was observed that gastroesophageal reflux and delayed gastroesophageal transit exclusively affected the “tubular” pattern, while delayed gastric emptying was equally distributed among the three patterns. The high incidence of gastroesophageal reflux seen at the early x-ray examination (31 %) was probably due to the fact that the staple line, which is often long in the “tubular pattern,” involved the angle of His. Late x-ray follow-up showed a good function of the gastroesophageal junction and the gastric tube with a reduction of gastroesophageal reflux from 31 to 11 %, delayed gastroesophageal transit from 16 to 2 %, and total disappearance of delayed gastric emptying. This suggests that the observed early functional disturbances are of a transient character and may be related to edema and reflex spasms of the tissues affected by the surgery.
In conclusion, considering the extremely low incidence (0.99 %) of surgical complications revealed at the early x-ray examination and detection of two cases of complications in patients who subsequently developed symptoms, it is our opinion that early x-ray examination is not required as a routine procedure in all operated patients. It should be performed only in patients considered at high risk or in patients who develop symptoms of complications or possibly in patients in whom the surgeon encountered problems during the surgical procedure.
Our data also suggest only a modest and temporary impact of LSG on the gastroesophageal motility and function, and it is not correlated with the anatomic subtype of the gastric tube (as defined by the x-ray patterns described by Werquin [5]). However, gastroesophageal function after LSG should be investigated further in a prospective study using specific clinical questionnaires and a study of pH-metric parameters before and after surgery.
References
Melissas J, Daskalakis M, Koukouraki S, et al. Sleeve gastrectomy—a “food limiting” operation. Obes Surg. 2008;18:1251–6.
Jacobs M, Bisland W, Gomez E, et al. Laparoscopic sleeve gastrectomy: a retrospective review of 1- and 2-year results. Surg Endosc. 2010;24(4):781–5.
Langer FB, Reza Hoda MA, Bohdjalian A. Sleeve gastrectomy and gastric banding: effects on plasma ghrelin levels. Obes Surg. 2005;15:1024–9.
Lewis CE, Dhanasopon A, Dutson EP, et al. Early experience with laparoscopic sleeve gastrectomy as a single-stage bariatric procedure. Am Surg. 2009;75(10):945–9.
Werquin C, Caudron J, Mezghani J, et al. Early imaging features after sleeve gastrectomy. J Radiol. 2008;89:1721–8.
Braghetto I, Korn O, Valladares H, et al. Laparoscopic sleeve gastrectomy: surgical technique, indications and clinical results. Obes Surg. 2007;17(11):1442–50.
Akkary E, Duffy A, Bell R. Deciphering the sleeve: technique, indications, efficacy, and safety of sleeve gastrectomy. Obes Surg. 2008;18:1323–9.
Mognol P, Chosidow D, Marmuse JP. Laparoscopic sleeve gastrectomy (LSG): review of a new bariatric procedure and initial results. Surg Technol Int. 2006;15:47–52.
Menenakos E, Stamou KM, Albanopoulos K, et al. Laparoscopic sleeve gastrectomy performed with intent to treat morbid obesity: a prospective single-center study of 261 patients with a median follow-up of 1 year. Obes Surg. 2010;20:276–82.
Sánchez-Santos R, Masdevall C, Baltasar A, et al. Short- and mid-term outcomes of sleeve gastrectomy for morbid obesity: the experience of the Spanish National Registry. Obes Surg. 2009;19(9):1203–10.
Tan JT, Kariyawasam S, Wijeratne T, et al. Diagnosis and management of gastric leaks after laparoscopic sleeve gastrectomy for morbid obesity. Obes Surg. 2010;20(4):403–9.
Baumann T, Grueneberger J, Pache G, et al. Three-dimensional stomach analysis with computed tomography after laparoscopic sleeve gastrectomy: sleeve dilation and thoracic migration. Surg Endosc. 2011;25(7):2323–9.
Triantafyllidis G, Lazoura O, Sioka E, et al. Anatomy and complications following laparoscopic sleeve gastrectomy: radiological evaluation and imaging pitfalls. Obes Surg. 2011;21(4):473–8.
Weiner RA, Weiner S, Pomhoff I, et al. Laparoscopic sleeve gastrectomy—influence of sleeve size and resected gastric volume. Obes Surg. 2007;17(10):1297–305.
Frezza EE, Reddy S, Gee LL, et al. Complications after sleeve gastrectomy for morbid obesity. Obes Surg. 2009;19(6):684–7.
Lee CM, Cirangle PT, Jossart GH. Vertical gastrectomy for morbid obesity in 216 patients: report of two-year results. Surg Endosc. 2007;21(10):1810–6.
Melissas J, Koukouraki S, Askoxylakis J, et al. Sleeve gastrectomy—a restrictive procedure? Obes Surg. 2007;17:57–62.
Conflict of interest
M. Gnecchi, G. Bella, A.R. Pino, I. Staltari, N. Di Leo, N.A. Polli, and F. M. Drudi declare no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gnecchi, M., Bella, G., Pino, A.R. et al. Usefulness of X-Ray in the Detection of Complications and Side Effects After Laparoscopic Sleeve Gastrectomy. OBES SURG 23, 456–459 (2013). https://doi.org/10.1007/s11695-012-0799-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-012-0799-5