Abstract
Bipolar disorder (BD) is frequently misdiagnosed as major depressive disorder (MDD) in clinical practice, especially during depressive episodes. A unifying triple-network model, involving the default mode network (DMN), central executive network (CEN) and salience network (SN), has been proposed to explain the neural physiopathology of psychiatric and neurological disorders. Although several studies revealed shared and specific alterations between BD and MDD in key regions of DMN, CEN, and SN, and a few studies used different measures to detect detailed alterations in the triple networks in BD and MDD, their shared and specific patterns of altered functional connectivity (FC) in the triple networks has remained unclear. In this study, we acquired resting-state fMRI (R-fMRI) data from 38 unmedicated BD and 35 unmedicated MDD patients during depressive episodes along with 47 healthy controls. We first determined the spatially independent components of the DMN, SN, and CEN by using independent component analysis (ICA); then we estimated the inter-ROI and inter-network FC for each group. By comparing the differences between the three groups, we obtained the following results: (1) both the BD and MDD patients showed shared weaker intra-network FC in the left mPFC and right precuneus within the DMN as well as weaker inter-ROI FC between the left AI and right AI compared with the healthy controls; (2) the BD had weaker while the MDD had stronger intra-network FC in the right dlPFC within the rCEN as well as stronger inter-ROI FC between the right dlPFC and right ANG compared with the healthy controls; (3) the BD showed specific, stronger inter-ROI FC between the left PPC and right AI as well as stronger inter-network FC between the lCEN and SN compared with either the MDD or the control group. Our findings provide new information for understanding the neural physiopathology and clinical symptoms of depressed BD and MDD patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bipolar disorder (BD) and major depressive disorder (MDD) are two debilitating mood disorders that seriously affect the quality of life in patients, cause impaired social functioning, and increase mortality due to suicide (Grande et al. 2016; Judd et al. 2002). Clinically, BD is characterized by recurrent depressive and manic/hypomanic episodes, but the most common mood state is depression throughout the duration of the illness (Judd et al. 2002, 2003; de Almeida and Phillips 2013; Grande et al. 2016; Han et al. 2018). MDD, on the other hand, is only characterized by recurrent depressive episodes. It is difficult to distinguish between BD and MDD for the high prevalence of depressive episodes relative to manic/hypomanic episodes in the disease course of BD and the fact that the symptoms of mania are sometimes subthreshold (de Almeida and Phillips 2013). Unfortunately, this misdiagnosis has many potentially deleterious consequences, including inappropriate medication, which may lead to poor prognosis, higher suicide rates, switching to mania, and greater health care costs. Thus, it is necessary to understand the shared and specific neural physiopathology of BD and MDD patients during depressive episodes. These differences may help us to differentiate depressed BD from MDD.
The development of MRI has led to an accumulation of evidence about the shared and specific functional and structural alterations in BD and MDD. Previous reviews (Han et al. 2018; Gong and He 2015; Vargas et al. 2013) showed that BD and MDD patients have similar alterations in emotion- and cognition-processing neural circuits, involving brain regions in the default mode network (DMN), central executive network (CEN), salience network (SN), limbic, and attention networks, but have relatively few distinct neural correlates. As for the few specific alterations, Han et al. (2018) reviewed the results published on comparing alterations in BD and MDD patients. From the perspective of brain function, BD and MDD patients had different activation patterns in neural networks including the amygdala, anterior cingulate cortex (ACC), prefrontal cortex (PFC), and striatum. In addition, BD patients had much stronger functional connectivity (FC) pattern in the DMN, CEN, and brain regions including the PFC, ACC, parietal and temporal regions, and thalamus than MDD patients. From the perspective of brain structure, different gray matter volumes in the ACC, hippocampus, amygdala, and dorsolateral prefrontal cortex (dlPFC) were reported in BD and MDD patients, along with a thinner cortical thickness in dlPFC in BD compared with MDD patients. Additionally, BD patients showed reduced integrity in the anterior part of the corpus callosum and posterior cingulum. The goal of some of our previous work was also to reveal the shared and specific functional alterations between depressed BD and MDD patients by using the indices associated with graph theory and FC strength (Wang et al. 2017a, b). We found that the alterations in the depressed BD and MDD patients varied depending on the different indices and also found that the DMN and the limbic system were always involved. Taking the previous studies together, it seems that BD and MDD patients have more shared than specific alterations although BD patients have more pronounced alterations than MDD patients. At the network level, these alterations involve widespread brain regions, including key regions in the SN, DMN, and CEN. However, the findings across studies, even those based on the same indices, are sparse and inconsistent. One possible reason for this inconsistency is that the data in the studies were obtained when the patients were in different states, including depressed, euthymic, or remitted states. Previous studies found that the shared and specific neural alterations between BD and MDD patients are state dependent (Almeida et al. 2010; Rive et al. 2015, 2016). Other possible confounding factors include different durations of illness, number of episodes, levels of depressive symptoms, medications, or a mix of BD subtypes (Kempton et al. 2011).
In 2011, Menon proposed a unifying triple-network model to explain the neural physiopathology of psychiatric and neurological disorders because the dysfunctions of these disorders occur at a network-level rather than in an individual brain area (Menon 2011). This model examines ‘core’ brain networks that support cognitive, perceptual, affective, and social functions, including the SN, DMN, and CEN, which are thought to be abnormally organized in many psychiatric disorders (Menon 2011). So far, many studies have combined this model with resting-state functional MRI (R-fMRI) data to further understand the physiopathology of mental disorders, including BD and MDD (Wei et al. 2015; Goya-Maldonado et al. 2016; Zheng et al. 2015), schizophrenia (Manoliu et al. 2013, 2014b; Nekovarova et al. 2014; Lefebvre et al. 2016), Parkinson’s disease (Putcha et al. 2015), unconscious patients (Qin et al. 2015), and internet addiction (Wang et al. 2017). Based on the fact that BD and MDD patients showed widespread alterations in the triple networks (Mulders et al. 2015; Kaiser et al. 2015; Vargas et al. 2013), some studies have used different indices to detect detailed alterations in the triple networks with mixed results. Zheng et al. (2015) studied the interactions of the triple networks based on graph theory analysis and found that the connectivity strength of the right anterior insula (AI) was significantly higher, while the FC strength between the DMN and CEN was significantly lower in depressed MDD patients compared with healthy controls. Wei et al. (2015) compared the Hurst exponents of spontaneous brain activity between depressed MDD patients and healthy controls and revealed altered interactions of the DMN with the ventromedial PFC (vmPFC), SN, and CEN in MDD patients. De Kwaasteniet et al. (2014) compared the FC in the triple networks between patients with treatment resistant MDD (TRD) and non-treatment resistant MDD (non-TRD) as well as healthy controls and found weaker FC between the dlPFC and the angular gyrus (ANG), between the CEN and the DMN, as well as between the medial PFC and the precuneus in TRD patients compared with either non-TRD patients or healthy controls. In addition, only one study (Goya-Maldonado et al. 2016) has directly compared the FC alterations between depressed BD and MDD patients in core regions of the triple networks. They analyzed the FC in the fronto-parietal network (including core regions of the CEN), cingulo-opercular networks (including core regions of the SN) and the DMN based on R-fMRI data and found that depressed BD patients showed stronger FC in the fronto-parietal network whereas MDD patients presented stronger FC in the DMN, compared with healthy controls. This study provided information about the intra-network differences between depressed BD and MDD patients but no information about inter-network differences.
Our goal was to use R-fMRI data to analyze the FC of the triple networks, including the intra-network, inter-ROI and inter-network FC, in unmedicated BD and MDD patients during depressive episodes. To reduce the confounding factors, such as the subtype-, medicine-, and states-related effects, we only included unmedicated BD-II (referred to as BD in the following) and MDD patients during depressive episodes, matching their number of episodes, age of onset, duration of illness, and clinical states. Based on the findings from previous studies, we hypothesized as follows: 1) the depressed BD and MDD patients had altered FC in the triple networks; 2) the depressed BD and MDD patients had more shared than specific FC alterations; 3) the depressed BD patients had more pronounced FC alterations than MDD patients. These combinations may help us understand the clinical symptoms of depressed BD and MDD patients.
Materials and methods
Subjects
A total of 73 patients, 38 currently depressed adults diagnosed with BD and 35 currently depressed adults diagnosed with MDD, were recruited from the Psychiatry Department of the First Affiliated Hospital of Jinan University (FAHJU), Guangzhou, China, from June 2014 to May 2017. The diagnoses of the BD and MDD patients were made according to the Structured Clinical Interview for DSM-IV (SCID) by two trained psychiatrists (Y.J. and S.Z.) independently. The clinical state of each patient was assessed using the 24-item Hamilton Depression Rating Scale (HDRS24) (Hamilton 1960) and the Young Mania Rating Scale (YMRS) (Young et al. 1978) during the 7-day period prior to the R-fMRI scanning. The inclusive criteria for each MDD patient were a HDRS24 total score > 21, while for each BD patient were a YMRS total score < 7 and a HDRS24 total score > 21 (Wang et al. 2015a). The exclusion criteria were patients with Axis-I psychiatric disorders other than MDD, BD and anxiety disorders, Axis-II psychiatric disorders, a history of organic brain disorder, neurological disorders, mental retardation, cardiovascular illness, alcohol/substance abuse, pregnancy, or any physical illness. At the time of scanning, all patients were either medication-naive or had been unmedicated for at least 5 months. None of the patients had ever received electroconvulsive therapy prior to participating in the study.
In addition, 47 age-, gender-, and education-matched healthy controls were recruited via local advertisements to be the healthy controls. They were carefully screened through a diagnostic interview, the Structured Clinical Interview for DSM-IV (non-patient edition), to rule out the presence of current or past psychiatric illness. The exclusion criteria for the healthy controls were similar to those of the patients; in addition, people with any history of psychiatric illness in first-degree relatives (determined by direct oral inquiry about any family history of mood or psychotic disorders in first-degree relatives), and any current or past mental disorders, neurological illness, or brain injuries were excluded from the healthy control group.
The present study was approved by the Ethics Committee of the First Affiliated Hospital of Jinan University, China. All subjects were right-handed according to their self-report and signed a written informed consent form after a full written and verbal explanation of the study.
Data acquisition
All the MRI data were obtained on a 3 T GE MR750 scanner with an 8-channel phased-array head coil in the Medical Center of the FAHJU. The R-fMRI data were acquired using a single-shot gradient-echo EPI sequence with the following parameters, volume repetition time (TR) = 2000 ms, echo time (TE) = 25 ms, flip angle (FA) = 90°, field of view (FOV) = 240 mm × 240 mm, data matrix = 64 × 64, thickness/gap = 3.0/1.0 mm, 35 axial interleaved slices covering the whole-brain, and 210 volumes acquired in 7 min. During the R-fMRI scanning, each subject was requested to keep their eyes closed but not to fall asleep and to relax their minds but not to think of anything particularly. After the scanning, we interviewed all the subjects, and no one reported that they had fallen asleep during the scanning. We also acquired high-resolution brain structural images (1mm3 isotropic) for each subject by using a T1-weighted three-dimensional brain volume imaging (3D-BRAVO) sequence (TR = 8.2 ms, TE = 3.2 ms, FA = 12°, FOV = 256 mm × 256 mm, data matrix = 256 × 256, slice thickness = 1.0 mm, and 136 axial slices covering the whole brain). For each subject, the R-fMRI data and 3D high-resolution brain structural images were acquired in the same session.
fMRI data processing
R-fMRI data were pre-processed on single-subject level using the FMRI Expert Analysis Tool from the FMRIB Software Library (FEAT/FSL) (Smith et al. 2004), including removal of first 10 time points, motion correction using FMRIB’s Linear Image Registration Tool (MCFLIRT), brain extraction (BET), spatial smoothing using a Gaussian kernel of 5 mm FWHM (full width at half maximum), high pass temporal filtering at 100 s, and resampling to 2 mm isotropic voxels. All of the subjects in this study satisfied our criteria for head motions, displacement <1.5 mm in any plane, and rotation <1.5° in any direction. Subsequently, we registered the processed functional images to the T1-weighted high-resolution structural images by using a boundary-based reconstruction (BBR) approach (Greve and Fischl 2009) and then normalized them into the standard space (MNI 152) by using a non-linear registration (FNIRT). Afterward, we performed a single-session independent component analysis (ICA) by using MELODIC/FSL to identify the independent components (ICs) and applied FIX to remove noise ICs (standard training set, threshold: 20) to yield a cleaned functional dataset for each subject (Feis et al. 2015; Salimi-Khorshidi et al. 2014).
Then the temporal concatenation approach in MELODIC was applied to the cleaned functional data from all the subjects to perform a group-level ICA with 30 spatial ICs (Shirer et al. 2012; Mingoia et al. 2012). For each IC, a group-level t-map was generated and was used to identify the brain regions involved. We first used the manual identification method of visual inspection to discard the ICs of the noise signals. Subsequently, we adopted the “discriminability index-based component identification (DICI)”, an automatic IC identification method. The DICI uses the “discriminability index (DI)” (DeCarlo 1998) to quantitatively evaluate the similarity of the spatial distribution of each IC to a predefined spatial template for resting-state networks (RSNs) identification (Zhang et al. 2013; Huang et al. 2018). In the current study, we selected the RSNs template provided by Shirer et al. (2012) as the reference template. Specifically, the t-maps for all the group-level ICs were first converted to binary maps (p < 0.01, FDR corrected), and then, the DICI value for each IC was calculated by comparing it with the RSNs template according to the following equation:
where the hit rate or sensitivity is the number of correctly identified voxels within a given IC versus the total number of voxels in the RSNs template, and the false alarm rate (1 - specificity) is the number of mistakenly identified voxels within a given IC versus the number of voxels outside the RSNs template. DICI is calculated as the z-transformed hit rate minus the z-transformed false alarm rate. The IC with the biggest DICI value was selected as the IC corresponding to the RSNs template.
By combining the results from the manual and automatic IC identification methods, we determined the group spatial maps included in the triple-network model and the ICs corresponding to the anterior DMN (aDMN), posterior DMN (pDMN), left CEN (lCEN), right CEN (rCEN), and SN (Menon 2011). Further, we used dual regression to estimate the individual spatial maps of the ICs and the corresponding time series for each subject. All these spatial maps of the ICs corresponded to the intra-network FC.
From the group spatial maps corresponding to the triple-network model, we identified the peak coordinates of the core regions of interest (ROIs) in each IC. Similarly to previous studies, we selected bilateral core ROIs in the precuneus, ventro-medial PFC (vmPFC), and angular gyrus (ANG) for the DMN (Buckner et al. 2008), the dlPFC and posterior parietal cortex (PPC) for the CEN (Seeley et al. 2007), and the ACC and anterior insula (AI) for the SN (Goulden et al. 2014). The coordinates of these ROIs were determined by the peak t-value in their spatial maps. Subsequently, we extracted the time course for each spherical ROI with the centroid at the peak voxel (radius = 6 mm) and then estimated the Pearson’s temporal correlation between any pair of ROIs (inter-ROI FC) or between any pair of networks (inter-network FC).
Totally, we derived three indices, the intra-network FC, inter-ROI FC and inter-network FC, to characterize the FC within the triple networks between the BD, MDD, and control groups. The intra-network FC characterizes the FC strength within a specific network. The inter-ROI FC refers to the FC between a pair of given core ROIs. If the ROIs belong to the same network, the inter-ROI FC gives us knowledge about the FC within the specific network. But if the ROIs belong to different networks, the inter-ROI FC gives us knowledge about the FC between networks, which is similar to the inter-network FC. Briefly, the intra-network FC and inter-network FC provide FC information within and between networks, respectively, from the macroscopical network perspective. And the inter-ROI FC emphasizes the FCs between core ROIs in the triple networks, adding supplementary information to the within and between network FC. Thus, the intra-network FC, inter-ROI FC, and inter-network FC provide information on the FC within the triple networks from different perspectives and are complementary to each other.
Structural MRI data processing
Because the structural properties of gray matter may affect the functional properties, we calculated the gray matter volume and took it as a covariate in the FC analysis in this study. Specifically, we conducted the FSL-VBM processing stream based on brain structural images (Smith et al. 2004). The steps of the VBM processing were as follows. First, the brain structural images for each subject were extracted using BET/FSL and GM-segmented before being registered to the MNI 152 standard space using FNIRT. Second, the resulting images were averaged across all subjects in this study and flipped along the x-axis to create a left-right symmetric study-specific GM template. Third, each native GM image was nonlinearly registered to this study-specific template and ‘modulated’ to correct for local expansion due to the nonlinear component of the spatial transformation. Each modulated GM image was then smoothed with a Gaussian kernel of 7 mm FWHM.
Statistics
Group effect
Considering that the data distribution may bias the statistical results in parametric tests, we used the non-parametric tests in our statistics. A permutation one-way analysis of variance (ANOVA) was used to detect differences in age and education level between the BD, MDD, and control groups. A Pearson’s χ2-test was used to detect difference in gender between the BD, MDD, and control groups. For clinical variables, a permutation two-sample t-test was used to detect the differences in the number of episodes, age of onset, duration of illness, HDRS24, and YMRS scores between the BD and MDD groups. A Pearson’s χ2-test was used to detect difference in comorbid anxiety between the BD and MDD groups.
The voxel-wise one-way analysis of covariance (ANCOVA) was conducted to detect the group effect on the intra-network FC in the triple networks. In the calculations, we compared the individual spatial map of each IC between the BD, MDD, and control groups by taking age, gender, years of education, and brain GM volume as covariates. The statistical threshold was set at p < 0.001 (Alphasim corrected) by combining a height threshold of p < 0.001 and an extent threshold of p < 0.001 determined by Monte Carlo simulations (Ledberg et al. 1998). Then a post-hoc analysis was performed for each of the detected clusters showing a significant group effect by extracting the mean value of a spherical ROI with the centroid at its corresponding peak voxel (radius = 6 mm).
The permutation ANCOVA was also conducted to detect the group effect on the inter-ROI and inter-network FC (p < 0.05, FDR corrected). In the calculations, we took age, gender, and years of education as covariates. A post hoc analysis was also carried out for the FCs that showed group effects.
Brain-behavior relationship
For the intra-network, inter-ROI, and inter-network FCs with a significant group effect, we performed a partial correlation analysis to describe their relationships with the clinical variables in the BD and MDD groups, separately (p < 0.05, FDR corrected). These clinical variables included the HDRS24 score, number of episodes, onset age, and total duration of illness. In the calculations, we took age, gender, and education as covariates.
Results
Demographic information
Table 1 lists the demographic and clinical characteristics of the three groups. No significant differences were detected in age, gender, or education level between the three groups. Additionally, no significant differences were found in the number of episodes, age of onset, duration of illness, HDRS24 score, YMRS score, and comorbid anxiety between the BD and MDD groups.
Spatial maps of the triple networks
Figure 1 shows the ICs corresponding to the aDMN, pDMN, lCEN, rCEN, and SN, which were selected from the 30 ICs (p < 0.001, FDR corrected). These selected ICs matched the ICs of the DMN, CEN, and SN reported in previous studies (Damoiseaux et al. 2006; Smith et al. 2009). Table 2 lists the peak coordinates of the core ROIs in each of the networks.
Group effect on intra-network FC
Figure 2a, b respectively show the group effects on the intra-network FC of the aDMN and pDMN, including clusters located in the left mPFC in the aDMN, and the right precuneus in the pDMN (p < 0.001, Alphasim corrected). The intra-network FC of both the left mPFC and right precuneus were weaker in both the BD and MDD groups compared with the control group. Figure 2c shows the group effect on the intra-network FC of the rCEN (p < 0.001, Alphasim corrected). The BD group showed a significantly weaker while the MDD group showed a significantly stronger intra-network FC in the right dlPFC compared with the control group. The detailed information about the statistical results is listed in Table 3.
The group effect on the intra-network FC of aDMN, pDMN, and rCEN in the patients with bipolar disorder (BD), patients with major depressive disorder (MDD), and healthy controls (p < 0.001 Alphasim corrected, ANCOVA). The post-hoc analysis was performed for the clusters showing significant group effect. Symbols of ◊, ∆, and ○ in the scatter plot indicate the mean intra-network FC value of a given cluster for a subject in the BD, MDD, and control groups, respectively. Red dots indicate outliers. The box plot shows the median (red line), interquartile range (blue lines), and sample minimum and maximum values (dark lines). The horizontal lines on top indicate pairwise comparisons that survived statistical thresholds: **, p < 0.01; *, p < 0.05. mPFC, medial prefrontal cortex; dlPFC, dorsolateral prefrontal cortex
Group effect on inter-ROI FC
Figure 3 reveals the three inter-ROI FCs showing significant group effects (Fig. 3, p < 0.05, FDR corrected). Both the BD and MDD groups showed weaker inter-ROI FC between the left AI and right AI compared with the control group. The inter-ROI FC between the right dlPFC and right ANG was weaker in the BD group but stronger in the MDD group compared with the control group. In addition, the inter-ROI FC between the left PPC and right AI was stronger in the BD group compared with either the MDD or control groups.
The group effect on the inter-ROI FC between core ROIs of the triple networks. A post-hoc analysis was performed for the FC showing significant group effect. a Inter-FC between different ROIs. The symbol of ‘+’ indicates p < 0.05 (FDR corrected, ANCOVA). b Post-hoc analysis. Symbols of ◊, ∆, and ○ in the scatter plot indicate the mean inter-FC value for a subject in the BD, MDD, and control groups, respectively. Red dots indicate outliers. The box plot shows the median (red line), interquartile range (blue lines), and sample minimum and maximum values (dark lines). The horizontal lines on top indicate pairwise comparisons that survived statistical thresholds: **, p < 0.01; *, p < 0.05. aDMN, anterior default mode network; pDMN, posterior default mode network; lCEN, left central executive network; rCEN, right central executive network; SN, salience network; L (R): left (right) hemisphere; vmPFC, ventromedial prefrontal cortex; ANG, angular gyrus; PPC, posterior parietal cortex; dlPFC, dorsolateral prefrontal cortex; ACC, anterior cingulate cortex; AI, anterior insula
Group effect on inter-network FC
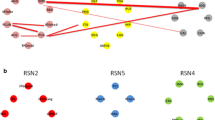
Figure 4 shows that only one inter-network FC had a significant group effect (p < 0.05, FDR corrected). A post hoc analysis revealed that the inter-network FC between the lCEN and SN was stronger in the BD group compared with either the MDD or control groups.
The group effect on the inter-network FC between different networks. A post hoc analysis was performed for the inter-FC showing significant group effect. a Correlations between different networks. The symbol of ‘+’ indicates p < 0.05 (FDR corrected, ANCOVA). b Post-hoc analysis. Symbols of ◊, ∆, and ○ in the scatter plot indicate the mean inter-FC value for a subject in the BD, MDD, and control groups, respectively. Red dots indicate outliers. The box plot shows the median (red line), interquartile range (blue lines), and sample minimum and maximum values (dark lines). The horizontal lines on top indicate pairwise comparisons that survived statistical thresholds: **, p < 0.01; *, p < 0.05. aDMN, anterior default mode network; pDMN, posterior default mode network; lCEN, left central executive network; rCEN, right central executive network; SN, salience network
Brain-behavior correlations
For the brain-behavior correlation analysis, we found a significant negative correlation between the intra-network FC of the pDMN in the right precuneus and the number of depressive episodes (r = −0.495, p = 0.004), as well as between the intra-network FC of the aDMN in the left mPFC, and the HDRS24 score (r = −0.362, p = 0.033) in the MDD group. However, no significant correlation was detected between the FCs with significant group effect and any of the clinical variables in the BD group (p < 0.05). All these results are displayed in Fig. S1 in the Supplementary materials.
Discussion
In this study, we compared group differences in the intra-network, inter-ROI, and inter-network FCs based on the triple-network model. The shared and specific FC alteration patterns in the depressed BD and MDD groups were as follows: 1) Both the BD and MDD patients showed weaker intra-network FC in the left mPFC and right precuneus within the DMN as well as weaker inter-ROI FC between the left AI and right AI within the SN. 2) The BD group had weaker, whereas the MDD group had stronger, intra-network FC in the right dlPFC and inter-ROI FC between the right dlPFC and right ANG. 3) The BD group showed specific, stronger inter-ROI FC between the left PPC and right AI and stronger inter-network FC between the lCEN and SN compared with either the MDD or control group. These findings confirmed that there were a greater number of shared than specific alterations in the triple networks connectivity patterns of BD and MDD patients, but the differences were more pronounced in BD than in MDD patients. These findings may provide new insights into the neural physiopathology of depressed BD and MDD patients.
Shared FC alterations in both BD and MDD
This study detected a shared, weaker intra-network FC within the DMN, including the left mPFC of the aDMN and the right precuneus of the pDMN (Fig. 2) in both the BD and MDD patients. This finding is consistent with previous studies that reported a weaker DMN FC in BD (Khadka et al. 2013; Sole et al. 2017) and MDD (Yang et al. 2016; Zhu et al. 2017) patients. In fact, previous studies also reported a stronger DMN FC in BD (Khadka et al. 2013; Sole et al. 2017) and MDD (Zhu et al. 2017; Straub et al. 2017) patients. Although there is inconsistency in the alteration direction in DMN FC across studies, the specific alterations but not alteration direction were always used to account for the depressive symptomatology (Broyd et al. 2009; Murrough et al. 2011). The DMN is believed to be responsible for self-referential processing (Menon 2011), and it has been suggested as a potential neural substrate for ruminative thoughts and introspective cognitive patterns (Liu et al. 2017). As a result, the aberrant DMN activity could lead to dysfunctional self-referential processing in the form of an excessively negative self-focus (Ho et al. 2015; Whitfield-Gabrieli and Ford 2012), which is a typical symptom of depressed patients. In addition, this study detected that the intra-network FC in the left mPFC was significantly negatively correlated with the HDRS24 score, and the intra-network FC in the right precuneus was significantly negatively correlated with the number of episodes (Fig. S1 in the Supplementary materials) in the MDD patients. Previous studies also have reported associations between less activity in the precuneus and depressive severity (Rzepa and McCabe 2016; Liu et al. 2017; Peng et al. 2015), as well as between altered activity in the mPFC and depressive severity (Yoshimura et al. 2010; Kaiser et al. 2016). These significant correlation results indicated that, as the depression accumulate, deficits in the mPFC and precuneus become increasingly severe. Taken together, our finding of weaker intra-network FC in the DMN for both depressed BD and MDD patients may account for their similarities in the expression of depression clinically, especially in maladaptive self-referential processing.
Within the SN, we detected weaker inter-ROI FC between the bilateral AI in both the BD and MDD groups (Fig. 3). This finding indicated the impaired inter-hemisphere communication in the AI in BD and MDD patients. The AI is involved in a diverse functions related to emotion or regulation of the body’s homeostasi (Craig 2009; Menon and Uddin 2010). It has been validated that the AI showed weaker activity in emotional information’s processing, attention, and cognitive control in depressed patients; and altered AI activity may be related to altered salience processing of emotional stimuli, mirroring anhedonic aspects of depressed patients (Diener et al. 2012). Further, the inter-hemisphere communication plays an important role in the integrated brain function underlying coherent cognition and behavior (Kelly et al. 2011; Wang et al. 2015b), and it has been reported altered in BD (Zhao et al. 2017; Wang et al. 2015a) and MDD (Guo et al. 2013) patients. Thus, the impaired inter-hemisphere communication in the AI detected in our study may reflect the impaired brain integration in salience processing of emotional information, manifested by the clinical symptom of emotional dysregulation in both depressed BD and MDD patients.
Shared but opposite FC alteration directions between BD and MDD
Our study detected that the BD group had weaker, but the MDD had stronger, intra-network FC of the CEN in the right dlPFC (Fig. 2) as well as inter-ROI FC between the right dlPFC and right ANG compared with the control group (Fig. 3). The dlPFC, a core region of the CEN, is believed to be involved in control processes during goal-directed/externally oriented tasks (Fox and Raichle 2007) and in the regulation of emotional processing (Phillips et al. 2008). Aberrant activity in the right dlPFC has been reported in BD (Chai et al. 2011; Chen et al. 2011) and MDD (Diener et al. 2012; Fitzgerald et al. 2008; Grimm et al. 2008) patients during rest or multiple tasks. The ANG, a core region of the DMN, plays an important role in self-referential processing (Menon 2011). The inter-ROI FC between the right dlPFC and right ANG corresponds to the FC between the CEN and DMN. Previous studies have also reported altered FC between the CEN and DMN in MDD patients (Manoliu et al. 2014a; Ye et al. 2012; de Kwaasteniet et al. 2014; Sheline et al. 2010). Nolen-Hoeksema et al. (1993) proposed that, during depressive episodes, the altered DMN dominance over the task positive network (TPN, mainly involves the CEN) is associated with higher levels of depressive rumination in MDD patients. The insula has been implicated casually in switching between modes of relative DMN and CEN dominance (Sridharan et al. 2008). Hamilton et al. (2013) proposed that, in depressive episodes, the DMN supports the representation of negative self-referential information and that the insula, when promoted by heightened levels of DMN activity, initiates a potentially adaptive engagement of the CEN. This formulation can help to explain the association between the FC between DMN and CEN and depressive rumination. Thus, our findings of altered intra-network FC in the right dlPFC, as well as altered inter-ROI FC between the right dlPFC and the right ANG, may provide an additional evidence for the assumption of aberrant executive control, especially emotional control, and hence depressive rumination in BD and MDD patients during depressive episodes (Fales et al. 2008; Joormann and Siemer 2011).
Although both the BD and MDD groups showed altered intra-network FC in the right dlPFC and altered inter-ROI FC between the right dlPFC and right ANG, we found that they altered in opposite directions. The two alteration directions, corresponding to weaker and stronger FCs, all show abnormalities. Compared with control groups, weaker or stronger FCs related to the dlPFC have been reported in MDD (Diener et al. 2012; Grimm et al. 2008; Fitzgerald et al. 2008) and in BD groups (Chai et al. 2011; Chen et al. 2011). Also, weaker (Manoliu et al. 2014a; Ye et al. 2012; de Kwaasteniet et al. 2014) or stronger (Sheline et al. 2010) FCs between the DMN and CEN have been detected in MDD groups, but no studies directly compared this FC in a BD group with that in a control group. Actually, these studies above paid more attention to the specific abnormality but not the direction. Thus, it is hard to infer which alteration direction lead to BD or MDD. As we have discussed above, the altered intra-network FC in the right dlPFC and stronger inter-network FC between DMN and CEN in BD and MDD patients may account for the depressive rumination clinically. While the weaker intra-network FC in the right dlPFC and stronger inter-network FC between DMN and CEN in BD patients may be related to the stronger inter-network FC between SN and CEN, which may account for their recurrent depressive and manic episodes. The specific stronger FC between SN and CEN in BD patients is discussed in next part. Taken together, the different directions of FC alteration may reflect different pathological mechanisms in executive control, especially in emotional control, between BD and MDD patients during depressive episodes.
Specific FC alterations to BD
Our study found that the BD group had specific, stronger inter-ROI FC between the left PPC and the right AI (Fig. 3) and stronger inter-network FC between the lCEN and SN compared with either the MDD or the control group. This result is consistent with previous studies that reported the FC between PPC and AI was a key indicator of dysfunction in BD patients and could be a biomarker to distinguish BD from MDD patients (Liu et al. 2015; Ellard et al. 2018). The CEN is associated with externally-oriented and cognitively demanding mental activity (Dosenbach et al. 2007), and the SN plays a role in the identification of internal and external stimuli and in the shifting of brain function from DMN to CEN activities (Sridharan et al. 2008; Palaniyappan and Liddle 2012). The stronger FC between the SN and CEN may reflect a greater assignment of saliency to external stimuli (Menon 2011). Thus, the specific, stronger inter-ROI FC between the left PPC and the right AI and stronger inter-network FC between the CEN and SN in BD patients can account for the vulnerability to hypomanic occurrence or residual effects of previous hypomanic episodes in BD patients, even though they are currently in a depressive episode. But it is worth to mention that this specific alteration detected in depressed BD patients should be considered in their depressed state but not in their euthymic or remitted state. When comparing our results with a recent study, in which Syan et al. (2018) reviewed the resting-state FC in BD patients during an euthymic or remitted state compared with healthy controls, we found that our results have no overlapping with their findings.
Limitations
This study has several limitations. First, although the shared and specific FC alterations in the triple networks were detected in depressed BD and MDD patients, we cannot infer whether these alterations would have persisted once the patients were in other states and whether the findings represented state or trait effects of the respective illnesses. Previous studies indicated that the shared and specific neural alterations between BD and MDD are state dependent (Almeida et al. 2010; Rive et al. 2015; Rive et al. 2016). Second, selecting young patients with a clear BD-II diagnosis was difficult because of the low number of episodes for BD patients and because of the uncertainty as to whether some of the MDD patients might later switch to a BD diagnosis in the absence of longitudinal data is unclear. However, we tried our best to reduce the possibility of misdiagnosis. Two experienced, senior psychiatrists carried out the diagnosis. We also tracked the MDD patients after we acquired the data and found that none of the patients had switched to another diagnosis type by the time of the submission of this manuscript. Third, we did not distinguish the number of depressive episodes from the number of manic episodes in the BD group. This may have caused some confusion and affected the analysis of the correlation between the FC and the number of episodes. Future studies should record the number of depressive and manic episodes separately. Fourth, although the patients were unmedicated for at least 5 months prior to the scan, the subjects in each group may have had different exposures to medication, an issue which could have biased the results. Thus, it is difficult to estimate the potential contribution of lifetime exposure to medication in relation to the results. Fifth, we used the Alphasim correction for the multiple comparisons of the intra-network FC, which may increase the false positive rate (FPR) (Eklund et al. 2016). However, in this study, we set the statistical threshold at p < 0.001 by combining a height threshold of p < 0.001 and an extent threshold of p < 0.001, which can minimize the FPR (Cox et al. 2017; Woo et al. 2014). Sixth, because the functional components identified by ICA depend on the number of meaningful components predetermined to exist in the datasets (Abou-Elseoud et al. 2010), the derived results may be affected by the number of input model order values. In this study, we set the component number to 30, which is consistent with many previous studies (Damoiseaux et al. 2006; Smith et al. 2009). As an exploratory measure, we also tried other model order values, but they all had a suboptimal decomposition in which the components of interest either merged commonly recognized RSNs or split the RSNs into multiple subcomponents. More accurate dimension estimation methods are urgently needed to address this issue in order to support reliable decompositions across studies. Finally, we did not make any physiological measurements so we could not exclude their effects on our analysis. Future studies should be careful to collect and analyze this type of data.
Conclusion
In conclusion, this study revealed the altered FC in the triple networks in depressed BD and MDD patients, manifested by more shared than specific alterations in BD and MDD patients but more pronounced alterations in BD than MDD patients. The shared alterations in the FCs within DMN and SN may reflect the similarity in the expressions of depression in both BD and MDD patients. The shared but opposite alterations in the FCs within CEN and between CEN and DMN may indicate the different pathological mechanisms in executive control, especially in emotional control, between BD and MDD patients. Additionally, the specific altered FC between CEN and SN in BD may reflect either a pathway involved in the vulnerability for hypomanic occurrence or the residual effects of previous hypomanic episodes in BD patients. Thus, our findings provide new information for further understanding the physiopathology of depressed BD and MDD patients.
References
Abou-Elseoud, A., Starck, T., Remes, J., Nikkinen, J., Tervonen, O., & Kiviniemi, V. (2010). The effect of model order selection in group PICA. Human Brain Mapping, 31(8), 1207–1216.
Almeida, J. R. C., Versace, A., Hassel, S., Kupfer, D. J., & Phillips, M. L. (2010). Elevated amygdala activity to sad facial expressions: A state marker of bipolar but not unipolar depression. Biological Psychiatry, 67(5), 414–421.
Broyd, S. J., Demanuele, C., Debener, S., Helps, S. K., James, C. J., & Sonuga-Barke, E. J. S. (2009). Default-mode brain dysfunction in mental disorders: A systematic review. Neuroscience and Biobehavioral Reviews, 33(3), 279–296.
Buckner, R. L., Andrews-Hanna, J. R., & Schacter, D. L. (2008). The brain's default network: Anatomy, function, and relevance to disease. Annals of the New York Academy of Sciences, 1124, 1–38.
Chai, X. J., Whitfield-Gabrieli, S., Shinn, A. K., Gabrieli, J. D., Nieto Castanon, A., McCarthy, J. M., et al. (2011). Abnormal medial prefrontal cortex resting-state connectivity in bipolar disorder and schizophrenia. Neuropsychopharmacology, 36(10), 2009–2017.
Chen, C. H., Suckling, J., Lennox, B. R., Ooi, C., & Bullmore, E. T. (2011). A quantitative meta-analysis of fMRI studies in bipolar disorder. Bipolar Disorders, 13(1), 1–15.
Cox, R. W., Chen, G., Glen, D. R., Reynolds, R. C., & Taylor, P. A. (2017). FMRI clustering in AFNI: False-positive rates redux. Brain Connectivity, 7(3), 152–171.
Craig, A. D. (2009). How do you feel - now? The anterior insula and human awareness. Nature Reviews Neuroscience, 10(1), 59–70.
Damoiseaux, J. S., Rombouts, S. A., Barkhof, F., Scheltens, P., Stam, C. J., Smith, S. M., et al. (2006). Consistent resting-state networks across healthy subjects. Proceedings of the National Academy of Sciences of the United States of America, 103(37), 13848–13853.
de Almeida, J. R. C., & Phillips, M. L. (2013). Distinguishing between unipolar depression and bipolar depression: Current and future clinical and neuroimaging perspectives. Biological Psychiatry, 73(2), 111–118.
de Kwaasteniet, B. P., Rive, M. M., Ruhé, H. G., Schene, A. H., Veltman, D. J., Fellinger, L., et al. (2014). Decreased resting-state connectivity between neurocognitive networks in treatment resistant depression. Frontiers in Psychiatry, 6, 28–28.
DeCarlo, L. T. (1998). Signal detection theory and generalized linear models. Psychological Methods, 3(2), 186–205.
Diener, C., Kuehner, C., Brusniak, W., Ubl, B., Wessa, M., & Flor, H. (2012). A meta-analysis of neurofunctional imaging studies of emotion and cognition in major depression. Neuroimage, 61(3), 677–685.
Dosenbach, N. U., Fair, D. A., Miezin, F. M., Cohen, A. L., Wenger, K. K., Dosenbach, R. A., et al. (2007). Distinct brain networks for adaptive and stable task control in humans. Proceedings of the National Academy of Sciences of the United States of America, 104(26), 11073–11078.
Eklund, A., Nichols, T. E., & Knutsson, H. (2016). Cluster failure: Why fMRI inferences for spatial extent have inflated false-positive rates (vol 113, pg 7900, 2016). Proceedings of the National Academy of Sciences of the United States of America, 113(33), E4929–E4929.
Ellard, K. K., Zimmerman, J. P., Kaur, N., Van Dijk, K. R. A., Roffman, J. L., Nierenberg, A. A., et al. (2018). Functional connectivity between anterior insula and key nodes of Frontoparietal executive control and salience networks distinguish bipolar depression from unipolar depression and healthy control subjects. Biological Psychiatry: Cognitive Neuroscience and Neuroimaging, 3(5), 473–484.
Fales, C. L., Barch, D. M., Rundle, M. M., Mintun, M. A., Snyder, A. Z., Cohen, J. D., Mathews, J., & Sheline, Y. I. (2008). Altered emotional interference processing in affective and cognitive-control brain circuitry in major depression. Biological Psychiatry, 63(4), 377–384.
Feis, R. A., Smith, S. M., Filippini, N., Douaud, G., Dopper, E. G., Heise, V., et al. (2015). ICA-based artifact removal diminishes scan site differences in multi-center resting-state fMRI. Frontiers in Neuroscience, 9, 395.
Fitzgerald, P. B., Srithiran, A., Benitez, J., Daskalakis, Z. Z., Oxley, T. J., Kulkarni, J., & Egan, G. F. (2008). An fMRI study of prefrontal brain activation during multiple tasks in patients with major depressive disorder. Human Brain Mapping, 29(4), 490–501.
Fox, M. D., & Raichle, M. E. (2007). Spontaneous fluctuations in brain activity observed with functional magnetic resonance imaging. Nature Reviews Neuroscience, 8(9), 700–711.
Gong, Q., & He, Y. (2015). Depression, neuroimaging and connectomics: A selective overview. Biological Psychiatry, 77(3), 223–235.
Goulden, N., Khusnulina, A., Davis, N. J., Bracewell, R. M., Bokde, A. L., McNulty, J. P., & Mullins, P. G. (2014). The salience network is responsible for switching between the default mode network and the central executive network: Replication from DCM. Neuroimage, 99, 180–190.
Goya-Maldonado, R., Brodmann, K., Keil, M., Trost, S., Dechent, P., & Gruber, O. (2016). Differentiating unipolar and bipolar depression by alterations in large-scale brain networks. Human Brain Mapping, 37(2), 808–818.
Grande, I., Berk, M., Birmaher, B., & Vieta, E. (2016). Bipolar disorder. Lancet, 387(10027), 1561–1572.
Greve, D. N., & Fischl, B. (2009). Accurate and robust brain image alignment using boundary-based registration. Neuroimage, 48(1), 63–72.
Grimm, S., Beck, J., Schuepbach, D., Hell, D., Boesiger, P., Bermpohl, F., Niehaus, L., Boeker, H., & Northoff, G. (2008). Imbalance between left and right dorsolateral prefrontal cortex in major depression is linked to negative emotional judgment: An fMRI study in severe major depressive disorder. Biological Psychiatry, 63(4), 369–376.
Guo, W., Liu, F., Dai, Y., Jiang, M., Zhang, J., Yu, L., Long, L., Chen, H., Gao, Q., & Xiao, C. (2013). Decreased interhemispheric resting-state functional connectivity in first-episode, drug-naive major depressive disorder. Progress in Neuropsychopharmacology and Biological Psychiatry, 41, 24–29.
Hamilton, M. (1960). A rating scale for depression. J Neurol Neurosurg Psychiatry, 23(1), 56–62.
Hamilton, J. P., Chen, M. C., & Gotlib, I. H. (2013). Neural systems approaches to understanding major depressive disorder: An intrinsic functional organization perspective. Neurobiology of Disease, 52, 4–11.
Han, K.-M., De Berardis, D., Fornaro, M., & Kim, Y.-K. (2018). Differentiating between bipolar and unipolar depression in functional and structural MRI studies. Progress in Neuropsychopharmacology & Biological Psychiatry.
Ho, T. C., Connolly, C. G., Henje Blom, E., LeWinn, K. Z., Strigo, I. A., Paulus, M. P., Frank, G., Max, J. E., Wu, J., Chan, M., Tapert, S. F., Simmons, A. N., & Yang, T. T. (2015). Emotion-dependent functional connectivity of the default mode network in adolescent depression. Biological Psychiatry, 78(9), 635–646.
Huang, H., Wang, J., Seger, C., Lu, M., Deng, F., Wu, X., He, Y., Niu, C., Wang, J., & Huang, R. (2018). Long-term intensive gymnastic training induced changes in intra- and inter-network functional connectivity: An independent component analysis. Brain Structrue and Function, 223(1), 131–144.
Joormann, J., & Siemer, M. (2011). Affective processing and emotion regulation in dysphoria and depression: Cognitive biases and deficits in cognitive control. Social and Personality Psychology Compass, 5(1), 13–28.
Judd, L. L., Akiskal, H. S., Schettler, P. J., Endicott, J., Maser, J., Solomon, D. A., Leon, A. C., Rice, J. A., & Keller, M. B. (2002). The long-term natural history of the weekly symptomatic status of bipolar I disorder. Archives of General Psychiatry, 59(6), 530–537.
Judd, L. L., Akiskal, H. S., Schettler, P. J., Coryell, W., Endicott, J., Maser, J. D., Solomon, D. A., Leon, A. C., & Keller, M. B. (2003). A prospective investigation of the natural history of the long-term weekly symptomatic status of bipolar II disorder. Archives of General Psychiatry, 60(3), 261–269.
Kaiser, R. H., Andrews-Hanna, J. R., Wager, T. D., & Pizzagalli, D. A. (2015). Large-scale network dysfunction in major depressive disorder: A meta-analysis of resting-state functional connectivity. JAMA Psychiatry, 72(6), 603–611.
Kaiser, R. H., Whitfield-Gabrieli, S., Dillon, D. G., Goer, F., Beltzer, M., Minkel, J., Smoski, M., Dichter, G., & Pizzagalli, D. A. (2016). Dynamic resting-state functional connectivity in major depression. Neuropsychopharmacology, 41(7), 1822–1830.
Kelly, C., Zuo, X. N., Gotimer, K., Cox, C. L., Lynch, L., Brock, D., Imperati, D., Garavan, H., Rotrosen, J., Castellanos, F. X., & Milham, M. P. (2011). Reduced interhemispheric resting state functional connectivity in cocaine addiction. Biological Psychiatry, 69(7), 684–692.
Kempton, M. J., Salvador, Z., Munafo, M. R., Geddes, J. R., Simmons, A., Frangou, S., et al. (2011). Structural neuroimaging studies in major depressive disorder. Meta-analysis and comparison with bipolar disorder. Archives of General Psychiatry, 68(7), 675–690.
Khadka, S., Meda, S. A., Stevens, M. C., Glahn, D. C., Calhoun, V. D., Sweeney, J. A., Tamminga, C. A., Keshavan, M. S., O’Neil, K., Schretlen, D., & Pearlson, G. D. (2013). Is aberrant functional connectivity a psychosis Endophenotype? A resting state functional magnetic resonance imaging study. Biological Psychiatry, 74(6), 458–466.
Ledberg, A., Akerman, S., & Roland, P. E. (1998). Estimation of the probabilities of 3D clusters in functional brain images. Neuroimage, 8(2), 113–128.
Lefebvre, S., Demeulemeester, M., Leroy, A., Delmaire, C., Lopes, R., Pins, D., Thomas, P., & Jardri, R. (2016). Network dynamics during the different stages of hallucinations in schizophrenia. Human Brain Mapping, 37(7), 2571–2586.
Liu, Y. T., Wu, X., Zhang, J. C., Guo, X. J., Long, Z. Y., & Yao, L. (2015). Altered effective connectivity model in the default mode network between bipolar and unipolar depression based on resting-state fMRI. Journal of Affective Disorders, 182, 8–17.
Liu, C., Ma, X., Yuan, Z., Song, L., Jing, B., Lu, H., et al. (2017). Decreased resting-state activity in the Precuneus is associated with depressive episodes in recurrent depression. The Journal of Clinical Psychiatry, 78(4), e372–e382.
Manoliu, A., Riedl, V., Doll, A., Bauml, J. G., Muhlau, M., Schwerthoffer, D., et al. (2013). Insular dysfunction reflects altered between-network connectivity and severity of negative symptoms in schizophrenia during psychotic remission. Frontiers in Human Neuroscience, 7, 216.
Manoliu, A., Meng, C., Brandl, F., Doll, A., Tahmasian, M., Scherr, M., et al. (2014a). Insular dysfunction within the salience network is associated with severity of symptoms and aberrant inter-network connectivity in major depressive disorder. Frontiers in Human Neuroscience, 7.
Manoliu, A., Riedl, V., Zherdin, A., Muhlau, M., Schwerthoffer, D., Scherr, M., et al. (2014b). Aberrant dependence of default mode/central executive network interactions on anterior insular salience network activity in schizophrenia. Schizophrenia Bulletin, 40(2), 428–437.
Menon, V. (2011). Large-scale brain networks and psychopathology: A unifying triple network model. Trends in Cognitive Sciences, 15(10), 483–506.
Menon, V., & Uddin, L. Q. (2010). Saliency, switching, attention and control: A network model of insula function. Brain Structure and Function, 214(5–6), 655–667.
Mingoia, G., Wagner, G., Langbein, K., Maitra, R., Smesny, S., Dietzek, M., Burmeister, H. P., Reichenbach, J. R., Schlösser, R. G. M., Gaser, C., Sauer, H., & Nenadic, I. (2012). Default mode network activity in schizophrenia studied at resting state using probabilistic ICA. Schizophrenia Research, 138(2–3), 143–149.
Mulders, P. C., van Eijndhoven, P. F., Schene, A. H., Beckmann, C. F., & Tendolkar, I. (2015). Resting-state functional connectivity in major depressive disorder: A review. Neuroscience & Biobehavioral Reviews, 56, 330–344.
Murrough, J. W., Iacoviello, B., Neumeister, A., Charney, D. S., & Iosifescu, D. V. (2011). Cognitive dysfunction in depression: Neurocircuitry and new therapeutic strategies. Neurobiology of Learning and Memory, 96(4), 553–563.
Nekovarova, T., Fajnerova, I., Horacek, J., & Spaniel, F. (2014). Bridging disparate symptoms of schizophrenia: A triple network dysfunction theory. Frontiers in Behavioral Neuroscience, 8, 171.
Nolen-Hoeksema, S., Morrow, J., & Fredrickson, B. L. (1993). Response styles and the duration of episodes of depressed mood. Journal of Abnormal Psychology, 102(1), 20–28.
Palaniyappan, L., & Liddle, P. F. (2012). Does the salience network play a cardinal role in psychosis? An emerging hypothesis of insular dysfunction. Journal of psychiatry & neuroscience: JPN, 37(1), 17–27.
Peng, D. H., Liddle, E. B., Iwabuchi, S. J., Zhang, C., Wu, Z. G., Liu, J., et al. (2015). Dissociated large-scale functional connectivity networks of the precuneus in medication-naive first-episode depression. Psychiatry Research: Neuroimaging, 232(3), 250–256.
Phillips, M. L., Ladouceur, C. D., & Drevets, W. C. (2008). A neural model of voluntary and automatic emotion regulation: Implications for understanding the pathophysiology and neurodevelopment of bipolar disorder. Molocular Psychiatry, 13(9), 829–833.
Putcha, D., Ross, R. S., Cronin-Golomb, A., Janes, A. C., & Stern, C. E. (2015). Altered intrinsic functional coupling between core neurocognitive networks in Parkinson's disease. Neuroimage Clinical, 7, 449–455.
Qin, P. M., Wu, X. H., Huang, Z. R., Duncan, N. W., Tang, W. J., Wolff, A., et al. (2015). How are different neural networks related to consciousness? Annals of Neurology, 78(4), 594–605.
Rive, M. M., Mocking, R. J., Koeter, M. W., van Wingen, G., de Wit, S. J., van den Heuvel, O. A., et al. (2015). State-dependent differences in emotion regulation between Unmedicated bipolar disorder and major depressive disorder. JAMA Psychiatry, 72(7), 687–696.
Rive, M. M., Redlich, R., Schmaal, L., Marquand, A. F., Dannlowski, U., Grotegerd, D., Veltman, D. J., Schene, A. H., & Ruhé, H. G. (2016). Distinguishing medication-free subjects with unipolar disorder from subjects with bipolar disorder: State matters. Bipolar Disorders, 18(7), 612–623.
Rzepa, E., & McCabe, C. (2016). Decreased anticipated pleasure correlates with increased salience network resting state functional connectivity in adolescents with depressive symptomatology. Journal of Psychiatric Research, 82, 40–47.
Salimi-Khorshidi, G., Douaud, G., Beckmann, C. F., Glasser, M. F., Griffanti, L., & Smith, S. M. (2014). Automatic denoising of functional MRI data: Combining independent component analysis and hierarchical fusion of classifiers. Neuroimage, 90, 449–468.
Seeley, W. W., Menon, V., Schatzberg, A. F., Keller, J., Glover, G. H., Kenna, H., Reiss, A. L., & Greicius, M. D. (2007). Dissociable intrinsic connectivity networks for salience processing and executive control. Journal of Neuroscience, 27(9), 2349–2356.
Sheline, Y. I., Price, J. L., Yan, Z. Z., & Mintun, M. A. (2010). Resting-state functional MRI in depression unmasks increased connectivity between networks via the dorsal nexus. Proceedings of the National Academy of Sciences of the United States of America, 107(24), 11020–11025.
Shirer, W. R., Ryali, S., Rykhlevskaia, E., Menon, V., & Greicius, M. D. (2012). Decoding subject-driven cognitive states with whole-brain connectivity patterns. Cerebral Cortex, 22(1), 158–165.
Smith, S. M., Jenkinson, M., Woolrich, M. W., Beckmann, C. F., Behrens, T. E., Johansen-Berg, H., et al. (2004). Advances in functional and structural MR image analysis and implementation as FSL. Neuroimage, 23 Suppl, 1, S208–S219.
Smith, S. M., Fox, P. T., Miller, K. L., Glahn, D. C., Fox, P. M., Mackay, C. E., Filippini, N., Watkins, K. E., Toro, R., Laird, A. R., & Beckmann, C. F. (2009). Correspondence of the brain's functional architecture during activation and rest. Proceedings of the National Academy of Sciences of the United States of America, 106(31), 13040–13045.
Sole, B., Jimenez, E., Torrent, C., Reinares, M., Bonnin, C. D. M., Torres, I., et al. (2017). Cognitive impairment in bipolar disorder: Treatment and prevention strategies. International Journal of Neuropsychopharmacology, 20(8), 670–680.
Sridharan, D., Levitin, D. J., & Menon, V. (2008). A critical role for the right fronto-insular cortex in switching between central-executive and default-mode networks. Proceedings of the National Academy of Sciences, 105(34), 12569–12574.
Straub, J., Metzger, C. D., Plener, P. L., Koelch, M. G., Groen, G., & Abler, B. (2017). Successful group psychotherapy of depression in adolescents alters fronto-limbic resting-state connectivity. Joural of Affective Disorders, 209, 135–139.
Syan, S. K., Smith, M., Frey, B. N., Remtulla, R., Kapczinski, F., Hall, G. B. C., et al. (2018). Resting-state functional connectivity in individuals with bipolar disorder during clinical remission: A systematic review. Joural of Psychiatry & Neuroscience, 43(5), 170175.
Vargas, C., Lopez-Jaramillo, C., & Vieta, E. (2013). A systematic literature review of resting state network--functional MRI in bipolar disorder. Joural of Affective Disorders, 150(3), 727–735.
Wang, Y., Zhong, S., Jia, Y., Zhou, Z., Wang, B., Pan, J., & Huang, L. (2015a). Interhemispheric resting state functional connectivity abnormalities in unipolar depression and bipolar depression. Bipolar Disorders, 17(5), 486–495.
Wang, Y., Zhong, S., Jia, Y., Zhou, Z., Zhou, Q., & Huang, L. (2015b). Reduced interhemispheric resting-state functional connectivity in unmedicated bipolar II disorder. Acta Psychiatrica Scandinavica, 132(5), 400–407.
Wang, L., Shen, H., Lei, Y., Zeng, L. L., Cao, F., Su, L., Yang, Z., Yao, S., & Hu, D. (2017). Altered default mode, fronto-parietal and salience networks in adolescents with internet addiction. Addictive Behaviors, 70, 1–6.
Wang, Y., Wang, J., Jia, Y., Zhong, S., Niu, M., Sun, Y., Qi, Z., Zhao, L., Huang, L., & Huang, R. (2017a). Shared and specific intrinsic functional connectivity patterns in Unmedicated bipolar disorder and major depressive disorder. Scientific Reports, 7(1), 3570.
Wang, Y., Wang, J., Jia, Y., Zhong, S., Zhong, M., Sun, Y., Niu, M., Zhao, L., Zhao, L., Pan, J., Huang, L., & Huang, R. (2017b). Topologically convergent and divergent functional connectivity patterns in unmedicated unipolar depression and bipolar disorder. Translational Psychiatry, 7(7), e1165.
Wei, M., Qin, J., Yan, R., Bi, K., Liu, C., Yao, Z., & Lu, Q. (2015). Association of resting-state network dysfunction with their dynamics of inter-network interactions in depression. Journal of Affective Disorders, 174, 527–534.
Whitfield-Gabrieli, S., & Ford, J. M. (2012). Default mode network activity and connectivity in psychopathology. Annual Review of Clinical Psychology, 8, 49–76.
Woo, C. W., Krishnan, A., & Wager, T. D. (2014). Cluster-extent based thresholding in fMRI analyses: Pitfalls and recommendations. Neuroimage, 91, 412–419.
Yang, R., Gao, C., Wu, X., Yang, J., Li, S., & Cheng, H. (2016). Decreased functional connectivity to posterior cingulate cortex in major depressive disorder. Psychiatry Research: Neuroimaging, 255, 15–23.
Ye, T., Peng, J., Nie, B., Gao, J., Liu, J., Li, Y., Wang, G., Ma, X., Li, K., & Shan, B. (2012). Altered functional connectivity of the dorsolateral prefrontal cortex in first-episode patients with major depressive disorder. European Journal of Radiology, 81(12), 4035–4040.
Yoshimura, S., Okamoto, Y., Onoda, K., Matsunaga, M., Ueda, K., Suzuki, S., & ShigetoYamawaki. (2010). Rostral anterior cingulate cortex activity mediates the relationship between the depressive symptoms and the medial prefrontal cortex activity. Journal of Affective Disorders, 122(1–2), 76–85.
Young, R. C., Biggs, J. T., Ziegler, V. E., & Meyer, D. A. (1978). A rating scale for mania: Reliability, validity and sensitivity. British Journal of Psychiatry, 133, 429–435.
Zhang, H., Jia, W., Liao, W., & Zang, Y. (2013). Automatic component identification method based on normalized sensitivity/specificity measurement. Paper presented at the Oraganization ofHum brain Mapp (OHBM), Seattle, USA.
Zhao, L., Wang, Y., Jia, Y., Zhong, S., Sun, Y., Qi, Z., Zhang, Z., & Huang, L. (2017). Altered interhemispheric functional connectivity in remitted bipolar disorder: A resting state fMRI study. Scientific Reports, 7(1), 4698.
Zheng, H., Xu, L., Xie, F., Guo, X., Zhang, J., Yao, L., & Wu, X. (2015). The altered triple networks interaction in depression under resting state based on graph theory. BioMed Research International, 2015(386326), 1–8.
Zhu, X., Zhu, Q., Shen, H., Liao, W., & Yuan, F. (2017). Rumination and default mode network subsystems connectivity in first-episode, drug-naive young patients with major depressive disorder. Scientific Reports, 7, 43105.
Funding
This study was funded by the National Natural Science Foundation of China (81801685, 81871338, 81671670, 81501456, 81471650, 81428013, 81471654, 81371535, and 61571047); National Natural Science Foundation of Guangdong Province, China (2018A030310003); Planned Science and Technology Project of Guangdong Province, China (2014B020212022); and Planned Science and Technology Project of Guangzhou, China (201508020004, 20160402007, 201604020184). The funding organizations played no further role in the study design, data collection, analysis, interpretation, or paper writing. The authors appreciate the editing assistance of Drs. Rhoda E. and Edmund F. Perozzi.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human subjects were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all the individual subjects included in the study.
Additional information
Highlights
1) The BD and MDD groups had a shared weaker FC in the left mPFC and right precuneus within the DMN, and between the left AI and right AI within the SN.
2) The BD group had weaker, but the MDD group had stronger, FC in the right dlPFC within the rCEN, and between the right dlPFC and right ANG compared with the control group.
3) The BD group showed specific, stronger FC between the left PPC and right AI and between the lCEN and SN compared with either the MDD or the control group.
Electronic supplementary material
ESM 1
(DOCX 1569 kb)
Rights and permissions
About this article
Cite this article
Wang, J., Wang, Y., Wu, X. et al. Shared and specific functional connectivity alterations in unmedicated bipolar and major depressive disorders based on the triple-network model. Brain Imaging and Behavior 14, 186–199 (2020). https://doi.org/10.1007/s11682-018-9978-x
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-018-9978-x