Abstract
Objective
The purpose of this nonrandomized retrospective study was to report our new procedures using polyethylene glycolic acid (PGA) felt with fibrin sealant to prevent severe pancreatic fistula in patients undergoing pancreatic surgery.
Methods
From 2000 to 2008, 54 and 63 patients underwent pancreaticoduodenectomy (PD) and distal pancreatectomy (DP), respectively. Of those patients, we applied PGA felt with fibrin sealant to 18 PD patients and 26 DP patients. In PD patients, the PGA felt was wrapped around the pancreatic suture site, while in DP patients, the PGA felt was wrapped around the predictive division site. The pancreaticojejunostomy site in PD patients and the cut stump in DP patients were coated with fibrin sealant. We compared the occurrence rates for severe postoperative pancreatic fistula (POPF) that occurred after PD or DP both with and without our new procedures.
Results
Before introduction of our procedures, severe POPF developed in 14 of 36 PD patients (39%) and 10 of 37 DP patients (27%). In contrast, after introduction of our procedures, the incidence of POPF was only one in both of 18 PD (6%; P = 0.016) and 26 DP (4%; P = 0.017) patients.
Conclusion
In summary, our procedure using PGA felt with fibrin sealant may reduce the risk of severe POPF.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Postoperative pancreatic fistula (POPF) is the most frequent complication after pancreaticoduodenectomy (PD) and distal pancreatectomy (DP), occurring in 3–26%1–3 and 0–>60% of cases,3–5 respectively. POPF often develops into further complications such as fluid collection or intra-abdominal abscesses, wound infection, and sepsis. According to the 2005 International Study Group on Pancreatic Fistula classification,2 grade A pancreatic fistula have no clinical impact, whereas grade B and grade C pancreatic fistula require changes in clinical management or deviation from the normal clinical pathway. Thus, from a clinical perspective, it is important to reduce the risk of developing grade B or C POPF in patients undergoing pancreatectomy.
Herein, we describe our new surgical technique of applying polyethylene glycolic acid (PGA) felt with a fibrin sealant to reduce severe POPF of grade B or C, and evaluated the efficacy of these procedures in pancreaticojejunostomy and pancreatic transection patients receiving PD and DP for the prevention of grade B or C POPF.
Material and Methods
From May 2003 to April 2008, 54 and 63 patients underwent PD and DP, respectively, at the Department of Surgery, Kyoto Prefectural University of Medicine. Of these patients, the last 18 PD and 26 DP patients received a new surgical procedure involving application of PGA felt with fibrin sealant. POPFs were classified according to the internationally accepted definition of the International Study Group on Pancreatic Fistula.2 We retrospectively compared the perioperative morbidity rate of grade B or C POPF in the 36 PD and 37 DP cases without our new procedure (no-procedure group), and in the 18 PD and 25 DP cases with our new procedure (procedure group); in the no-procedure group, we never used PGA felt or fibrin sealant at the anastomotic site of pancreaticojejunostomy in the 36 PD cases, or both PGA felt and fibrin sealant at the same time in the 37 DP cases. We identified the pancreatic duct using a binocular loupe or an intraoperative ultrasonography and placed a pancreatic duct stent for external drainage in all PD cases. We used a stapler for 26 of the 37 DP cases in the no-procedure group after transection and closure of the pancreatic stump. The combined use of PGA felt and fibrin sealant cost approximately $170 in Japan.
New Surgical Procedure of Pancreaticojejunostomy
The child's reconstruction was performed in all 63 PD patients. The pancreas was transected with a knife or an ultrasonic dissector, followed by identification of the main pancreatic duct. A tube was transiently inserted into the pancreatic duct. The bleeding from the cut surface of the parenchyma was then closed using single stitches of 4-0 Polydioxanon monofilament absorbable sutures (PDS) (Ethicon Endosurgery; Johnson & Johnson, Cincinnati, OH, USA), and the suture site wrapped by laying PGA felt (Gunze Co., Kyoto, Japan). The pancreatic parenchyma was sutured penetratingly using straight needles with 4-0 monofilament nonabsorbable threads through the PGA felt and the seromuscular layer of the jejunum. After anastomosis between the pancreatic main duct and the jejunal wall using four to 12 stitches with 6-0 monofilament absorbable threads, the previous 4-0 threads were tied and the pancreaticojejunostomy finished (Fig. 1). The anastomotic site was reinforced by laying a fibrinogen/thrombin-coated collagen patch (Kaketsuken, Kumamoto, Japan; dose range 0.01–0.5 ml) onto the wrapped PGA felt.
In PD patients, the suture site was wrapped by laying PGA felt. The pancreatic parenchyma was sutured penetratingly using straight needles with 4-0 monofilament nonabsorbable threads through the PGA felt and the seromuscular layer of the jejunum. After anastomosis between the pancreatic main duct and the jejunal wall using four to 12 stitches with 6-0 monofilament absorbable threads, the former 4-0 threads were tied and the pancreaticojejunostomy finished
New Surgical Procedure of Pancreatic Transaction in DP
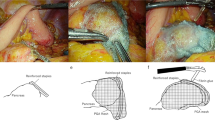
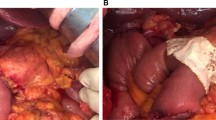
A stapling device is useful for pancreatic transection. In the staple method, we used devices that gave a staple line consisting of a triple row of closely placed staples. Before stapling, PGA felt was wrapped around the predictive staple line. The staple line was reinforced by laying a fibrinogen/thrombin-coated collagen patch onto the transected stump (Fig. 2a, b). In some cases, transection was also performed using the Echelon 60 with PGA felt (Gunze Co.) stocking type (Fig. 3a, b). The closure jaw of the staple was clamped carefully and slowly at a fixed speed, taking more than approximately 5 min. This procedure reduced the thickness of the pancreatic parenchyma at the site of planned resection and facilitated the subsequent application of the linear stapler across the pancreas. To ensure hemostasis from the pancreatic stump, the stapler was not released immediately after firing, and the jaws of the stapler were held shut for approximately 2 min. A ligation of the main pancreatic duct was unnecessary, and minor bleeding from the stump could be easily controlled by either compression or coagulation using electrocautery. This staple procedure with the above-described techniques provides a secure staple line without any tissue damage. Routine postoperative prophylactic octreotide was not used.
Postoperative Follow-up
Postoperative assessment included repeated measurement (days 1, 3, 4, and 5) of the amylase concentration in serum and drainage fluid while the drain was in place. Computed tomography was performed if the patient had any symptoms suggestive of abdominal collection (pain, fever, vomiting) or if major hyperleukocytosis was present. Oral feeding was allowed after the return of bowel function, usually before complete drain removal, except in cases of suspected or confirmed POPF. Conservative management of POPF was attempted whenever possible as initial treatment, and included total parenteral nutrition, percutaneous drainage of intra-abdominal fluid collection, antibiotics, and octreotide administration.
Statistical Methods
The perioperative morbidity rates were compared using the Mann–Whitney U test. Statistical significance was defined as P < 0.05. All statistical analyses were performed using statistical software (StatView 5.0; SAS Institute, Cary, NC, USA).
Results
Tumor pathology and morbidity in all 117 cases are shown in Tables 1 and 2. The clinicopathologic features of the 36 PD and 37 DP cases in the no-procedure group and of the 18 PD and 26 DP in the procedure group are shown in Tables 3 and 4. There were no significant differences in morbidity rates and patterns between cases in the two groups, except for grade B and C POPF.
There were four cases of postoperative mortality in the 36 no-procedure group PD cases (11.1%), but none in the 18 procedure group PD cases. Among all perioperative morbidities, POPF was the most frequent complication, occurring in 21 (58.3%) of the 36 no-procedure group PD cases and in ten (55.6%) of the 18 procedure group PD cases (Table 3). However, grade B and C POPF occurred in 14 (38.9%) of the 36 no-procedure group PD cases and in one (5.6%) of the 18 procedure group PD cases (Table 3). The occurrence rate of severe POPF in PD cases with PGA felt with fibrin sealant was significantly lower than in PD cases without PGA felt (P = 0.016). Four patients with grade C in the no-procedure group PD cases also had sepsis with postoperative intra-abdominal abscess; one of those patients unsuccessfully treated by percutaneous drainage required an operative drainage.
There was no postoperative mortality in DP cases. POPF occurred in 21 (56.8%) of the 37 no-procedure group DP cases and in 11 (42.3%) of the 26 procedure group DP cases (Table 4). However, grade B and C POPF occurred in ten (27.0%) of the no-procedure group DP cases and in only one (3.8%) of the procedure group DP cases. The occurrence rate of severe POPF in cases with PGA felt with fibrin sealant was significantly lower than in cases without (P = 0.017). Severe POPF occurred in 11 of the 63 DP patients (Table 4); nine of the fistulas (14%) were classified as grade B. Both patients with grade C POPF also had sepsis with postoperative intra-abdominal abscess. No patients required operative drainage.
Discussion
Pancreatic fistula remains a problem after PD and DP, with several technical variations failing to reduce its incidence.3 Most patients with this complication are treated conservatively or by interventional radiology, and if treated in a timely fashion, pancreatic fistula does not lead to mortality. Nevertheless, pancreatic fistula formation is a major source of subsequent morbidity and associated complications including abscess pseudo aneurysm, hemorrhage, and sepsis, with considerable health-care expenditure.6,7
We have previously examined the efficacy of various procedures to prevent severe POPF in both PD and DP patients. In pancreaticojejunostomy of PD, we first tried suturing between the seromuscular layer of the jejunum and the anterior–posterior faces of the remnant pancreas. We also started a modified Kakita's procedure8 or duct-to-mucosa pancreaticojejunostomy. However, there were no significant differences in the occurrence rates of severe POPF using the different of anastomotic procedures. Reported risk factors of POPF in PD in patients older than 60 years of age include nondilated duct size, longer operative time, greater intraoperative red blood cell transfusions, lower surgical volume, and soft texture.9–11 With regard to the anastomotic procedure, duct-to-mucosa pancreaticojejunostomy and external drainage of the pancreatic duct with a stent have been recommended;12 the efficacy of those procedures, however, remains controversial. In DP, we previously cut the stump of the remnant pancreas using a knife, then subsequently ligated the main pancreatic duct and sutured the tissue of the pancreas to close. A recently published systematic review appraised the available surgical alternatives for the management of the pancreatic stump after DP, which included duct ligation, ultrasonic dissection, the use of fibrin sealant, patches and meshes, pancreaticoenteric anastomosis, and hand-sewn and stapler closure,4 reflecting the clinical heterogeneity in this field. The benefits of staple transection for the pancreas as a simple, quick, and secure method for closing the proximal pancreas have been well described.13,14 However, only the randomized clinical trial of stapling vs. hand sewing showed no significant advantage of stapling (incidence of pancreatic fistula: 14% vs. 33%, respectively).4,15 For POPF, an occurrence rate of 23% for stapled closure after DP was observed in a meta-analysis, which was slightly lower than for hand-sewn closure.15 Furthermore, a significant reduction in the fistula rate after staple closure (using the Powered Multifire Endo GIA 60) compared with suture closure was reported (pancreatic fistula: stapler, 0% vs. suture, 35%),14 although the opposite pattern was also demonstrated (pancreatic fistula: stapler, 25% vs. suture, 14%).6
Fibrin sealant is used clinically to prevent the leakage of gastrointestinal anastomoses and hemorrhages in parenchymal organs.16–18 Suzuki et al.19 reported that intraoperative fibrin sealant of the pancreatic stump prevented POPF in patients who underwent pancreatic surgery. A randomized clinical trial showed that POPF occurred in 15% of patients in the fibrin sealant group and in 40% of the control group.19 Ohwada et al.20 recommended a fibrin sealant sandwich technique for preventing POPF. This unique technique sandwiches fibrin sealant between the dorsal and ventral edges of the remnant pancreas. The incidence of POPF in that study was 9% in the sandwich technique group vs. 27% in the simple sealing group. Fibrin sealant is a biologic adhesive that can be used conveniently by spraying onto the cut surface of the pancreas.19 However, fibrin sealant may not sufficiently block openings of small branches of the pancreatic duct that are not ligated. Therefore, in some cases, continuous exocrine pancreatic secretion from these small pancreatic ducts could lead to POPF after DP, despite the use of fibrin glue. On the other hand, Reuben et al.21 recommended a PGA felt of a stapled pancreatic transaction line for preventing pancreatic fistulas (pancreatic fistula: PGA felt, 3.5% vs. no PGA felt, 27.5%).
We recently started applying PGA felt with fibrin sealant at the pancreaticojejunostomy and pancreatic stump for reinforcement. In PD or DP, the PGA felt worked as a cushion for a thread knot or a stapler to prevent tissue damage. If a pancreatic tissue tearing occurs, it is thought to be repaired by the fibrin sealant. The PGA felt can be easily hydrolyzed in wet conditions by fibrin glue, and the PGA felt is absorbed within 3 months.22 In addition, because the rate of water absorption is high in the PGA felt, the fibrin glue is thought to attach firmly to the cut surface of the pancreas compared with the application of the fibrin sealant or PGA felt only. The PGA felt may focus the fibrin sealant to the cut surface of the pancreas to prevent early detachment of the fibrin sealant from the pancreas, enhancing the effects of the fibrin sealant. In the present study, the combination of the PGA felt and fibrin sealant was a significant independent factor for the prevention of severe POPF, despite the use of various procedures such as stapling or suturing with or without this combination (data not shown). The combined use of fibrin sealant and a polyethylene glycolic acid mesh patch is common for the prevention of air leakage from the lung during thoracic surgery,23 while a PGA felt with fibrin sealant was used for hepatectomy to prevent bile leakage, although there are no reports for pancreatectomy. This is the first report of combined use of fibrin sealant and a PGA mesh patch in pancreatic surgery. In future, a prospective randomized control study is necessary to confirm the efficacy of this procedure.
In conclusion, the application of this procedure using fibrin sealant and a PGA mesh patch to the pancreaticojejunostomy and pancreatic stump could reduce severe POPF after pancreatic surgery.
References
Bilimoria MM, Cormier JN, Mun Y, Lee JE, Evans DB, Pisters PW. Pancreatic leak after pancreatectomy is reduced following main pancreatic duct ligation. Br J Surg 2003;90:190–196.
Bassi C, Dervenis C, Butturini G, Fingerhut A, Yeo C, Izbicki J, Neoptolemos J, Sarr M, Traverso W, Buchler M. International Study Group on Pancreatic Fistula Definition: postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery 2005;138:8–13
Balzano G, Zerbi A, Cristallo M, Di Carlo V. The unsolved problem of fistula after left pancreatectomy: the benefit of cautious drain management. J Gastrointest Surg 2005;9:837–842.
Knaebel HP, Diener MK, Wente MN, Büchler MW, Seiler CM. Systematic review and meta-analysis of technique for closure of the pancreatic remnant after distal pancreatectomy. Br J Surg 2005;92:539–546.
Kuroki T, Tajima Y, Kanematsu T. Surgical management for the prevention of pancreatic fistula following distal pancreatectomy. J Hepatobiliary Pancreat Surg 2005;12:283–285.
Sheehan MK, Beck K, Creech S, Pickleman J, Aranha GV. Distal pancreatectomy: does the method of closure influence fistula formation? Am Surg 2002;68:264–268.
Rodriguez JR, Germes SS, Pandharipande PV, Gazelle GS, Thayer SP, Warshaw AL, Fernández-del Castillo C. Implications and cost of pancreatic leak following distal pancreatic resection. Arch Surg 2006;141:361–366.
Kakita A, Yoshida M, Takahashi T. History of pancreaticojejunostomy in pancreaticoduodenectomy: development of a more reliable anastomosis technique. J Hepatobiliary Pancreat Surg 2001;8:230–237.
Choe YM, Lee KY, Oh CA, Lee JB, Choi SK, Hur YS, Kim SJ, Cho YU, Ahn SI, Hong KC, Shin SH, Kim KR. Risk factors affecting pancreatic fistula after pancreaticoduodenectomy. World J Gastroenterol 2008;14:6970–6974.
Yeo CJ, Cameron JL, Maher MM, Sauter PK, Zahurak ML, Talamini MA, Lillemoe KD, Pitt HA. A prospective randomized trial of pancreaticogastrostomy versus pancreaticojejunostomy after pancreaticoduodenectomy. Ann Surg 1995;222:580–592.
Yang YM, Tian XD, Zhuang Y, Wang WM, Wan YL, Huang YT. Risk factors of pancreatic leakage after pancreaticoduodenectomy. World J Gastroenterol 2005;11:2456–2461.
Poon RT, Fan ST, Lo CM, Ng KK, Yuen WK, Yeung C, Wong J. External drainage of pancreatic duct with a stent to reduce leakage rate of pancreaticojejunostomy after pancreaticoduodenectomy. Ann Surg 2007;246:425–435.
Kajiyama Y, Tsurumaru M, Udagawa H, Tsutsumi K, Kinoshita Y, Akiyama H. Quick and simple distal pancreatectomy using the GIA stapler: report of 35 cases. Br J Surg 1996;83:1711.
Takeuchi K, Tsuzuki Y, Ando T, Sekihara M, Hara T, Kori T, Nakajima H, Kuwano H. Distal pancreatectomy: is staple closure beneficial? ANZ J Surg 2003;73:922–925.
Bassi C, Butturini G, Molinari E, Mascetta G, Salvia R, Falconi M, Gumbs A, Pederzoli P. Pancreatic fistula rate after pancreatic resection: the importance of definitions. Dig Surg 2004;21:54–59.
Kram HB, Garces MA, Klein SR, Shoemaker WC. Common bile duct anastomosis using fibrin glue. Arch Surg 1985;120:1250–1256.
Kram HB, Clark SR, Ocampo HP, Yamaguchi MA, Shoemaker WC. Fibrin glue sealing of pancreatic injuries, resections and anastomoses. Am J Surg 1991;161:479–482.
Noun R, Elias D, Balladur P, Bismuth H, Parc R, Lasser P, Belghiti J. Fibrin glue effectiveness and tolerance after elective liver resection: a randomized trial. Hepatogastroenterology 1996;43:221–224.
Suzuki Y, Kuroda Y, Morita A, Fujino Y, Tanioka Y, Kawamura T, Saitoh Y. Fibrin glue sealing for the prevention of pancreatic fistulas following distal pancreatectomy. Arch Surg 1995;130:952–955.
Ohwada S, Ogawa T, Tanahashi Y, Nakamura S, Takeyoshi I, Ohya T, Ikeya T, Kawashima K, Kawashima Y, Morishita Y. Fibrin glue sandwich prevents pancreatic fistula following distal pancreatectomy. World J Surg 1998;22:494–498.
Thaker RI, Matthews BD, Linehan DC, Strasberg SM, Eagon JC, Hawkins WG. Absorbable mesh reinforcement of a stapled pancreatic transection line reduces the leak rate with distal pancreatectomy. J Gastrointest Surg 2007;11:59–65.
Nakamura T, Shimizu Y, Watanabe S, Hitomi S, Kitano M, Tamada J, Matsunobe S. New bioabsorbable pledgets and non-woven fabrics made from polyglycolide (PGA) for pulmonary surgery: clinical experience. Thorac Cardiovasc Surg 1990;38:81–85.
Kaseda S, Aoki T, Hangai N, Omoto T, Yamamoto S, Sugiura H. Treating bullous lung disease with Holmium YAG laser in conjunction with fibrin glue and DEXON mesh. Lasers Surg Med 1998;22:219–222.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Ochiai, T., Sonoyama, T., Soga, K. et al. Application of Polyethylene Glycolic Acid Felt with Fibrin Sealant to Prevent Postoperative Pancreatic Fistula in Pancreatic Surgery. J Gastrointest Surg 14, 884–890 (2010). https://doi.org/10.1007/s11605-009-1149-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-009-1149-3