Abstract
Background
This study was planned to compare the traditional method of laparoscopic cholecystectomy (LC) versus LC using harmonic as regard the safety and efficacy.
Material and methods
This study included group A (70 patients) in whom LC was conducted using the traditional method (TM) by clipping both cystic duct and artery and dissection of gallbladder from liver bed by diathermy, and group B (70 patients) LC was conducted using harmonic scalpel (HS) closure and division of both cystic duct and artery and dissection of gallbladder from liver bed by HS. The intraoperative and postoperative parameters were collected including duration of operation, postoperative pain, and complications.
Results
HS provides a shorter operative duration than TM (33.21 + 9.6 vs. 51.7 + 13.79, respectively, p = 0.001), with a significant less incidence of gallbladder peroration (7.1% vs. 18.6, p = 0.04) and less rate of conversion to open cholecystectomy but not reach a statistical significance. The amount of postoperative drainage is significantly less in HS (29 + 30 vs. 47.7 + 31, p = 0.001). No postoperative bile leak was encountered in HS, but it occurred in 2.9% of patients in TM. VAS in HS at 12 h postoperative was 3.25 + 1.84 vs 5.01 + 1.2 (p = 0.001) and at 24 h postoperative was 3.12 + 1.64 vs. 4.48 + 1.89 (p = 0.001).
Conclusion
HS provides a complete hemobiliary stasis and is a safe alternative to stander clip of cystic duct and artery. It provides a shorter operative duration, less incidence of gallbladder perforation, less postoperative pain, and less rate of conversion to open cholecystectomy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The advantages of laparoscopic cholecystectomy (LC) have been published extensively, and LC has become the gold standard in treating benign gallbladder diseases.1–3 LC has largely replaced conventional open cholecystectomy.4–6
The traditional LC is commonly performed by means of dissector, the electrosurgical hook, spatula, and/or scissors, and this method has been used in most centers. Simple metal clips are frequently used to achieve cystic duct and artery closure.7–8 Alternative technique using sutures for cystic duct closure is infrequently used.9
Various energy sources are routinely used as cutting and coagulating aids in laparoscopic surgery. Risks involved with the use of monopolar electrosurgery are significantly greater.10 Nonetheless, monopolar electrosurgery is the preferred method in more than 85% of surgeons.11 Bipolar electrosurgery, being as effective as monopolar electrosurgery, has not been widely used in the LC procedure.12
The majority of electrosurgical injuries manifests late or goes unrecognized. The incidence of accidental burns caused by unintentional energy transmission during a LC ranges between 0.06% and 0.3%. However, only one or two patients in 1,000 are recognized.13
Several studies have described the use of ultrasound dissection technology in the LC, which concluded that ultrasonic dissection was safe and easy to use.14–16 Few studies reported the harmonic scalpel, though superior, is not immune from causing undesirable biological effects on the body.14–17 However, current available studies on LC using harmonic ultrasonic dissector are too small to determine any statistically significant difference in outcomes between traditional LC and LC with harmonic.
This study planned to compare traditional method of LC versus LC using harmonic as regard the safety and efficacy.
Material and Methods
This study was carried out from January 2008 to December 2008. Patients with gallbladder stone were treated by LC at the Gastroententerology Surgical Center and Mansoura University General Hospital and were included in this prospective randomized trial. The exclusion criteria included patients above 80 years old, patients with history of upper laparotomy, patients with common bile duct stones, and pregnant women.
All patients were subjected to thorough history and clinical examination focused on manifestation of gallstone disease and chronic liver disease. The following investigations were performed [whole blood picture, liver function tests (serum albumin, ALT, AST, and prothrombine time “INR”), HCV and HBV markers, and abdominal ultrasound] to show the state of the liver, portal vein, gallbladder, and CBD.
Informed consent was obtained from all patients to be included in the study, after explaining the nature of the disease and operative steps and possible complications. This study was approved by the local ethical committee.
The patients were randomized into two groups using enclosed envelope. The envelopes were drawn and opened by a nurse not otherwise engaged in the study before operation. Group A LC was done using traditional method, which included 70 patients, and group (B) LC was done using harmonic scalpel, which included 70 patients.
Under general anesthesia and the same antibiotics (third generation cephalosporin), surgery was performed using conventional four ports umbilical port, port below xiphoid, and two ports below right costal margin. Pneumoperitoneum at pressure 12 mmHg was used.
In group A, LC was done using traditional method by dissection of Calot’s triangle and clipping of both cystic duct and artery by metal clips. After that, dissecting the gallbladder from its bed by hook using electrocautery technique was performed. Finally, we insert abdominal drain in Morrison pouch.
In group B, LC was done using harmonic ACE (Ethicon Endo-Surgery) by dissection of Calot’s and then occlusion of both cystic duct and artery using harmonic ACE. For closure and division of cystic pedicle, we set the instrument at power 2, i.e., more coagulation, and do it at two levels and separate the duct at the proximal level toward the gallbladder. When dissecting the gallbladder from its bed, we set it to level 5, i.e., more cutting power, and control of any bleeding from the bed using the active blade of harmonic ACE. Finally, we insert abdominal drain in Morrison pouch.
The intraoperative parameter observed included duration of the operation, amount of CO2 used in the operation, bile escape, saline irrigation during operation, and volume of blood loss were all recorded.
The patients started oral feeding 8 h postoperatively; abdominal ultrasound was done for all patients in both groups on day of discharge to show any collection or free fluid in the abdomen. The patients were usually discharged after removal of drain and when the patient is surgically free.
Postoperative pain (PP) was evaluated at 12 h, 24 h, 48 h, and 1 week after operation using a visual analog scale (VAS)18 (with which each patients noted the severity of pain at each evaluated time using a linear between 0 (no pain) and 10 (severe pain). Postoperative analgesia in the form of nonsteroidal anti-inflammatory drug was administered intramuscularly when required. If the patients still complained of pain, strong analgesic (1 mg/kg pethidine intramuscularly) was administered. The total dose of these medications was recorded.
Postoperative maximum body temperatures were recorded at (24 and 48 h) for all patients.
Postoperative nausea and vomiting “PONV” were assessed after 24 and 48 h. Metoclopramide was given if the patients required reduction of nausea, and the total doses of this medication were recorded. The frequency of vomiting was recorded.
At the end of the first postoperative week, first month, and sixth postoperative month, patients underwent a clinical examination and an abdominal ultrasonography. In addition, blood sample was taken to show follow up of liver function.
The statistical analysis of the data in this study was preferred using the SPSS version 10. Analysis of data was by intension to treat. For continuous variables, descriptive statistics were calculated and reported as mean + SD. Categorical variables were described using frequency distributions. The Student’s t test for paired samples was used to detect differences in the means of continuous variables, and chi-square test was used in cases with low expected frequencies (p < 0.05 was considered to be significant).
Results
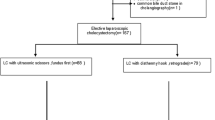
This study was carried out from January 2008 to December 2008. One hundred fifty patients with gallbladder stone were treated by LC at the Gastroenterology Surgical Center and Mansoura University Hospital, and ten patients were excluded due to different reasons: three patients had common bile duct stones, three patients had previous history of laparotomy, two patients were above 80 years, and two patients refused to join in this study.
One hundred forty patients were included in this prospective randomized trial. They were randomly divided into two groups: group A, LC with conventional method that included 70 patients with a mean age of 41.38 + 11.91 and group B, LC using harmonic that included 70 patients with a mean age of 40.97 + 11.56. Demographic data of the patients on both groups are shown in Table 1.
Intraoperative and postoperative findings of both groups are shown in Table 2. The incidence of gallbladder perforation was significantly higher in the traditional group than in the harmonic group (18.6% vs. 7.1%, respectively; p = 0.04). The mean operative time was significantly shorter in the harmonic group than in the traditional group (33.21 + 9.62 min vs. 51.7 + 13.79 vs. respectively; p = 0.0001). Intraoperative blood loss was significantly more in the traditional group than in the HS group (83.31 + 46.23 vs. 43.28 + 31.27; p = 0.0001). In the traditional group, two cases (2.9%) were converted to open surgery (one due to unclear anatomy and one due to bleeding), but in the HS group, all cases were completed laparoscopically. The mean amount of postoperative drainage was significantly more in the traditional group than in the HS group (47.78 + 31.54 vs. 29 + 30.79 ml, p = 0.001. The hospital stay was shorter in harmonic group (23.44 + 2.29 vs. 26.95 + 8.94 h, p = 0.002).
The overall morbidity rate was 15.71% (11/70) in the traditional group versus 4.2% (3/70) in the HS group, with the difference being statistically insignificant. The rate of pulmonary and port site infection was higher in traditional group than HS group, but it did not reach statistical significance. There was bile leak encountered in two patients (2.9%) in the traditional group (one from accessory duct and the other from cystic duct), but no postoperative bile leak occurred in HS group. No bile duct injuries were encountered in the present study (Table 3).
The time course of changes in maximum body temperature from preoperative (baseline) values is shown in Table 3. There was no observed significant change in temperatures in both groups.
Although the total incidence of nausea and vomiting were higher in the traditional group, the number of patients who expressed suffering from nausea or vomiting did not differ significantly at different time points (Table 3).
The incidence of pain is significantly more in the traditional group at 12 h postoperatively (68.6% vs. 51.4%, p = 0.03), but the incidence of PP at different postoperative time points (24 h, 48 h, and 1 week) differs but not did not reach a significance between both groups (Table 3). VAS in HS group was lower than in the traditional group; the difference is significant at 12 h postoperative (3.25 + 1.84 vs. 5.01 + 1.2, p = 0.0001) and at 24 h postoperative (3.12 + 1.64 vs. 4.48 + 1.89, p = 0.0001), but the difference was insignificant at 48 h and 1 week postoperative (Table 4).
Discussion
LC is the gold standard treatment of gall stones. The ultrasonically activated (harmonic) scalpel has been proven to be an effective and safe instrument for dissection and hemostasis in both open and laparoscopic surgical procedures. To date, the primary use of the harmonic scalpel in LC has been for the division of cystic artery and liver bed dissection. Advancements in the harmonic scalpel blade tip now provide for the reliable ultrasonic division and closure of cystic duct.19
Ultrasonic scalpel causing three effects that act synergically: cavitation, coaptation/coagulation, and cutting. The lateral energy spread is minimal, and the risk of distant tissue damage is lower than that of electrosurgery.20,21
In our study, the mean operative time was significantly shorter in the harmonic group than in the traditional group (33.21 + 9.62 min vs. 51.7 + 13.79, respectively, p = 0.0001). Samer et al. reported that statistically significant shorter mean operative time in the HS group can be attributed to several factors; the harmonic ACE is a multifunctional instrument. It replaces four instruments routinely used in the LC, namely, the dissector, clip applier, scissors, and electrosurgical hook or spatula. Finally, the activation of the harmonic ACE does not form smoke, therefore allowing the surgeon to work in a clear operative field throughout the operation.
In our study, intraoperative blood loss was significantly more in the traditional group than isn the HS group (83.31 + 46.23 vs. 43.28 + 31.27; p = 0.0001). Westervalt19 and Huscher et al.22 reported that harmonic scalpel has been proven to be an effective and safe instrument for dissection and hemostasis.
The main finding of the present study is the absence of either minor or major bile leaks from the cystic-duct stump in the HS group, denoting that the harmonic shears are as safe and efficient as simple metal clips in achieving the closure of the cystic-duct stump in the LC. Samer et al. reported the same result about the absence of either minor or major bile leaks from the cystic-duct stump. Westervalt19 found that no bile leaks from the cystic-duct stump in his 100 patients in whom the closure and division of the cystic duct was achieved solely by the harmonic shears. Huscher et al.22 found that bile leaks were encountered in seven of the 331 patients (2.1%), in whom the closure and division of the cystic duct was achieved by the harmonic shears alone. This 2.1% cystic-duct leakage rate is comparable to the 2% rate reported in the literature when using other cystic-duct closure techniques.22–24
Huscher et al.22 stated that the blades were first applied more proximally for a few seconds to achieve a simple sealing of the lumen, then they were applied a few millimeters distal to the previous application site, holding the grasp until the division of the duct was accomplished.
Various examples of cystic-duct leakage are due to inadequate closure of the duct caused by mismatch of the clip arms, necrosis of the duct at the site of clipping, or slippage of the clips off the end of the duct and migration into the biliary tract.25–30 The above-mentioned hazards inherent in the use of metallic clips were not encountered when closure and division of the cystic duct was achieved with the harmonic shears.
The use of ultracision was associated with a statistically significant lower incidence of gallbladder perforation compared to electrocautery (7.1% vs. 18.6%, respectively; p = 0.04).14 Samer et al. reported that the use of the harmonic ACE was associated with a statistically significant lower incidence of gallbladder perforation, compared to electrocautery (10% vs. 30%, respectively; p = 0.002).
LC has become the standard treatment for gallbladder disease. However, despite its low degree of invasiveness, many patients complain of PP and PONV due to residual pneumoperitoneum.31,32
Many factors attributed to PP may be due to residual pneumoperitoneum, diaphragmatic stretch during laparoscopy, or duration of the operation with using large volume of gases.32–34 The use of lower insufflations pressure (7.5 mmHg) has considerably decreased PP.35 In our study, the incidence of pain is significantly more in the traditional group at 12 h postoperatively (68.6% vs. 51.4%, p = 0.03), and VAS in HS group was lower than in traditional group; the difference is significant at 12 h postoperative (3.25 + 1.84 vs. 5.01 + 1.2, p = 0.0001) and at 24 h postoperative (3.12 + 1.64 vs. 4.48 + 1.89, p = 0.0001). This statistical difference may be attributed to several factors such as shorter duration of operation, so we use less amount of gasses, and less incidence of perforation of gallbladder in harmonic group so less escape of bile in the peritoneum.
The mean amount of postoperative drainage was significantly more in the traditional group than in the HS group (47.78 + 31.54 vs. 29 + 30.79 ml, p = 0.001. The hospital stay was shorter in the harmonic group (23.44 + 2.29 vs. 26.95 + 8.94 h, p = 0.002) as reported by Huscher et al.22
Conclusion
The harmonic scalpel provides complete hemobiliary stasis for all patients and is a safe alternative to stander clip of cystic duct and artery. It provides a shorter operative duration, less incidence of gallbladder perforation, less PP, and less rate of conversion to open cholecystectomy.
References
Fullarton GM, Bell G. A prospective audit of the introduction of laparoscopic cholecystectomy in west of Scotland. west of Scotland laparoscopic cholecystectomy audit group. Gut 1994;35(8):1121–1126.
Uchiyama K, Onishi H, Tani M, Kinoshita H, Ueno MYmanue H. Timing of laparoscopic cholecystectomy for acute cholecystitis with cholecysteolithiasis. Hepatogastroenterology 2004;51:346–348.
Toyama Y, Milyake R, Son K, Yoshida S, Usuba T. Three port laproscopic paritial hepatectomy using an ultrasonically activated devices (USAD). J Hepatobiliary Pancreat Surg 2006;13:317–322.
Cunniffe MG, Mc Anena OJ, Dar MA, Calleary J, Flynn N. A prospective randomized trial of intraoperative bupivacaine irrigation for management of shoulder tip pain following laparoscopy. Am J Surg 1998;176:258–261.
Hardacre JM, Tallmini MA. Pulmonary and haemodynaemic changes during laparoscopy—are they important? Surgery 2000;17:241–244.
Wills VL, Hunt DR. Pain after laparoscopic cholecystectomy. Br J Surg 2000;87:273–284.
Rohatgi A, Widdison A. An audit of cystic duct closure in laparoscopic cholecystectomies. Surg Endosc 2006;20:875–877.
Yano H, Okada K, Kinuta M, Nakano Y, Tono T, Matsui S, Iwazawa T, Kanoh T, Monden T. Efficacy of absorbable clips compared with metal clips for cystic duct ligation in laparoscopic cholecystectomy. Surg Today 2003;33:18–23.
Nathanson LK, Easter DW, Cuschieri A. Ligation of the structures of the cystic pedicle during laparoscopic cholecystectomy. Am J Surg 1991;161:350–354.
Tang B, Hanna GB, Joice P, Cuschieri A. Identification and categorization of technical errors by Observational Clinical Human Reliability Assessment (OCHRA) during laparoscopic cholecystectomy. Arch Surg 2004;139:1215–1220.
Tucker RD. Laparoscopic electrosurgical injuries: survey results and their implications. Surg Laparosc Endosc 1995;5(4):311–317.
Edelman DS, Unger SW. Bipolar versus monopolar cautery scissors for laparoscopic cholecystectomy: a randomized, prospective study. Surg Laparosc Endosc 1995;5(6):459–462.
Nduka CC, Super PA, Monson JR, Darzi AW. Cause and prevention of electrosurgical injuries in laparoscopy. J Am Coll Surg 1994;179:161–170.
Janssen IMC, Swank DJ, Boonstra O, Knipscheer BC, Klinkenbijil JH, Goor HV. Randomized, clinical trial of ultrasonic versus electrocautery dissection of the gallbladder in laparoscopic cholecystectomy. Br J Surg 2003;90:799–803.
Wetter LA, Payne JH, Kirshenbaum G, Podoll EF, Bachinsky T, Way LW. The ultrasonic dissector facilitates laparoscopic cholecystectomy. Arch Surg. 1992;127:1195–1199.
Tebala GD. Three-port laparoscopic cholecystectomy by harmonic dissection without cystic duct and artery clipping. Am J Surg 2006;9:718–720.
Sietses C, Eijsbouts QAJ, Blomberg BME, Cuesta MA. Ultrasonic energy versus monopolar electrosurgery in laparoscopic cholecystectomy. Surg Endosc 2001;15:69–71.
Huskisson EC. Measurement of pain. Lancet 1974:1127–1131.
Westervalt J. Clipless cholecystectomy: broadening the role of the harmonic scalpel. JSLS 2004;8:283–285.
Amaral JF, Chrosteek CA. Experimental comparison of the ultrasonically activated scalpel to electrosurgery and laser surgery for laparoscopic use. Min Invasive Ther Allied Technol 1997;6:324–331.
Gossot D, Buess G, Cuschieri A, Leporte E, Lirici M, Marvik R, Meijer D, Melzer A, Schurr MO. Ultrasonic dissection for endoscopic surgery. Surg Endosc 1999;13:412–417.
Huscher CGS, Lirici MM, Di Paola M, Crafa F, Napolitano C, Mereu A, Recher A, Corradi A, Amini M. laparoscopic cholecystectomy by ultrasonic dissection without cystic duct and artery ligature. Surg Endosc 2003;17:442–451.
Miroshnik M, Saafan A, Koh S, Farlow J, Neophyton J, Lizzio, Yee F, Ethell T, Bean A, Fenton-Lee D. Biliary tract injury in laparoscopic cholecystectomy: results of a single unit. ANZ J Surg 2002;72:867–870.
Wise US, Glick GL, Landeros M. Cystic duct leak after laparoscopic cholecystectomy: a multiinstitutional study. Surg Endosc 1996;10:1189–1193.
Hanazaki K, Igarashi J, Sodeyama H, Matsuda Y. Bile leakage resulting from clip displacement of the cystic duct stump: a potential pitfall of laparoscopic cholecystectomy. Surg Endosc 1999;13:168–171.
Nelson TM, Nakashima M, Mulvihill SJ. How secure are laparoscopically placed clips? Arch Surg 1992;127:718–720.
McMahon AJ, Fullarton G, Baxter JN, O’Dwyer PJ. Bile duct injury and bile leakage in laparoscopic cholecystectomy. Br J Surg 1995;82:307–313.
Reis LD. Surgical clips incorporated into a duodenal ulcer: a rare complication after elective laparoscopic cholecystectomy. Endoscopy 2000;32:S3.
Labuski MR, Wise SW. Recurrent abdominal abscess secondary to a dropped laparoscopic clip: CT imaging. Abdom Imaging 1999;24:191–192.
Jorgensen J, Gillies RB, Hunt DR, Caplehorn JR, Lumely T. A simple and effective way to reduce postoperative pain after laparoscopic cholecystectomy. Aust NZJ 1995;65:466–469.
Libermann MA, Howe S, Lane M. Ondansetron versus placebo for prophylaxis of nausea and vomiting in patients undergoing ambulatory laparoscopic cholecystectomy. Am J Surg 2000;179:60–62.
Fredman B, Jedeikin R, Olsfanger D, Flor P, Gruzman A. Residual pneumoperitoneum: a cause of postoperative pain after laparoscopic cholecystectomy. Anesth Analg 1994;79:152–154.
Sharma RR, Axelsson H, Oberg A, Jansson E, Clergue F. Diaphragmatic activity after laparoscopic cholecystectomy. Anesthesiology 1999;91:406–413.
Windberge UB, Auer R, Keplinnger F, Langle F, Heinze G, Losert UM. The role of intraabdominal pressure on splanchnic and pulmonary haemodynaemic and metabolic changes during CO2 pneumoperitoneum. Gastrointest Endosc 1999;49:84–91.
Wallace DH, Serpell MG, Baxter JN, O’Dwyer PJ. Randomized trial of different insufflations pressure for laparoscopic cholecystectomy. Br J Surg 1997;84:455–458.
Author information
Authors and Affiliations
Corresponding author
Additional information
Tharwat Kandil, Ayman M El Nakeeb, and Emad El Hefnawy wrote the paper. Tharwat Kandil, Ayman M El Nakeeb, and Emad El Hefnawy designed research. Tharwat Kandil, Ayman M El Nakeeb, and Emad El Hefnawy performed research. Tharwat Kandil, Ayman M El Nakeeb, and Emad El Hefnawy analyzed data.
Rights and permissions
About this article
Cite this article
Kandil, T., El Nakeeb, A. & El Hefnawy, E. Comparative Study between Clipless Laparoscopic Cholecystectomy by Harmonic Scalpel Versus Conventional Method: A Prospective Randomized Study. J Gastrointest Surg 14, 323–328 (2010). https://doi.org/10.1007/s11605-009-1039-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-009-1039-8