Abstract
Background
The objective of this study was to evaluate whether preoperative CA19-9 levels and the platelet–lymphocyte ratio (PLR) might reflect prognostic indices for resected ampullary adenocarcinoma.
Materials and Methods
Data were collected prospectively over a 10-year period for consecutive patients undergoing pancreatoduodenectomy for malignancy.
Results
Both preoperative PLR and CA19-9 results were available in 52 cases of resected ampullary adenocarcinoma. Preoperative CA19-9 levels of ≤150 kU/l (or ≤300 kU/l in the presence of bilirubin levels >35 µmol/l) and a PLR of ≤160 were found to represent the optimal cut-off values to risk stratify patients. If both levels were elevated (n = 8), patients had a median overall survival of 10.1 months. If either CA19-9 or PLR were elevated individually (n = 23), patients had a median survival of 25.2 months. For cases where both levels were less than the cut-off values (n = 21), the median overall survival time was not reached but was greater than 60 months (log rank, p < 0.001). This preoperative risk stratification was found to remain a significant independent predictor of survival on multivariate analysis (Cox, p = 0.001) alongside resection margin status (p = 0.002) and tumor size (p = 0.051).
Conclusions
Preoperative CA19-9 and PLR both merit further evaluation as prognostic indices in resected ampullary adenocarcinoma.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Serum levels of the sialyated Lewis blood group antigen CA19-9 are commonly measured during the initial investigation of patients with suspected pancreatic malignancy1 and have been demonstrated to have comparable sensitivity for ampullary adenocarcinoma when compared with pancreatic adenocarcinoma.2 CA19-9 is synthesized by the gallbladder and biliary mucosa and excreted in bile and is therefore commonly elevated in benign conditions associated with cholestasis.3–5 Approximately 5% of the population have undetectable serum CA19-9 levels due to an inability to synthesize the Lewis antigen glycosyl transferase enzyme.6
Preoperative CA19-9 levels have been used as a predictor of resectability for pancreatic malignancy to guide decision making regarding optimum use of staging laparoscopy.7 Levels of >150 kU/l (or >300 kU/l in the presence of cholestasis) have been shown to identify a patient group with periampullary malignancy at greater risk of unresectability for whom the diagnostic yield from staging laparoscopy is maximized.8,9 It is well recognized that normalization of serum CA19-9 after resection for pancreatic cancer is associated with a more favorable survival outcome10–12, but only a small number of studies have investigated whether elevated preoperative CA19-9 levels in isolation may also confer significant prognostic information in periampullary cancer.2,13,14
Previous studies have suggested that elevated preoperative C-reactive protein (CRP) levels15, thrombocytosis16,17 and lymphocytopenia18,19 may also represent potential prognostic markers in resected pancreatic cancer. We have recently reported that a combination of preoperative hematological indices, the platelet–lymphocyte ratio, represents a significant prognostic index in resected pancreatic cancer.20 However, no previous studies have investigated whether this marker of systemic inflammation might provide any prognostic information in resected ampullary cancer. Similarly, the prognostic value of preoperative CA19-9 levels adjusted for cholestasis in the same patient group has not previously been investigated. The objective of this study was to determine whether preoperative CA19-9 levels and the platelet–lymphocyte ratio might represent significant prognostic indices in patients undergoing resection for ampullary adenocarcinoma and to determine whether a combination of these parameters might provide superior prognostic information.
Materials and Methods
Prospective data were collected for all patients undergoing pylorus-preserving pancreatoduodenectomy or classical Kausch–Whipple resection between January 1997 and September 2007 at the Royal Liverpool University Hospital. Patient demographics, operative details, and the histological characteristics of the resected specimen were recorded. Processing and reporting of the pathology specimens were undertaken according to the Royal College of Pathologists’ Guidelines21 using the fifth edition of the UICC TNM Classification System.22 A positive resection margin (R1) was defined as tumor involvement within 1 mm of one or more resection margins on microscopic examination. No R2 resections were identified. Details of preoperative intervention for biliary drainage and adjuvant therapy were also recorded, and survival data were obtained from hospital computer records.
The preoperative full blood count, CA19-9, and concurrent bilirubin levels were recorded where available. The normal diagnostic reference interval for serum CA19-9 used in our laboratory is <35 kU/l. Univariate survival analysis was conducted using a CA19-9 cut-off value of 150 kU/l in non-jaundiced patients and 300 kU/l in patients with CA190-9 levels recorded in the presence of cholestasis (bilirubin >35 μmol/l). These values were selected on the basis of the previously published literature investigating the role of CA19-9 in the assessment of periampullary tumor resectability.7,8 Using a number of different cut-off points, a platelet–lymphocyte ratio of 160 was found to represent the optimum stratification point at which the survival difference between two groups was maximized.
Statistical Analysis
Continuous data were described using median, inter-quartile range (IQR) and 95% confidence intervals (CI). χ 2 or Fisher’s exact tests were used for comparative analysis of categorical data. Relationships between two continuous variables were analyzed using Spearman’s rank correlation. Survival data were analyzed using log rank testing for univariate analysis and Cox proportional hazards with forward-stepwise regression for multivariate analysis (‘NR’ signifies that the upper limit of the confidence interval for median survival was not reached). Corrected log rank p values were quoted for univariate survival where continuous prognostic data were dichotomized.23 All patients who died within 30 days of surgery were excluded from survival analysis and a p value of ≤0.05 was taken to reflect significance. Statistical analysis was performed using Statview version 5 (ISAS Institute, Cary, NC, USA) and Microsoft Excel (Microsoft Office 2007).
Results
Three hundred fifty-one consecutive patients underwent pancreatoduodenectomy for pancreatic or periampullary tumors during the study period. Seventy-seven cases had histologically confirmed adenocarcinoma arising from the ampulla of Vater. Two patients (2.6%) who died within 30 days of surgery were excluded from subsequent survival analyses. There were 37 censored cases with a median follow-up time of 22.5 months. Table 1 demonstrates the demographics of the study group along with the preoperative CA19-9 and full blood count results.
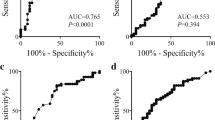
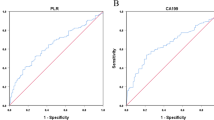
Median overall survival of the study group was 34.9 (95% CI = 25.2 to 63.8) months. The median survival times according to preoperative CA19-9 levels (using a cut-off value of ≤150 or ≤300 kU/l in jaundiced cases) and platelet–lymphocyte ratio ≤160 together with the median survival recorded for the various histological subgroups are shown in Table 2. The corresponding survival curves when stratifying by preoperative CA19-9 and platelet–lymphocyte ratio are shown in Figs. 1 and 2, respectively. No significant correlation between CA19-9 and platelet–lymphocyte ratio was identified (Spearman, rho = 0.022, p = 0.875).
Kaplan–Meier cumulative survival curves for ampullary adenocarcinoma patients stratified by preoperative CA19-9 ≤150 kU/l (or ≤300 kU/l in jaundiced cases). † A cut-off value of >150 kU/l was used to define the high-risk group for CA19-9 when recorded in the absence of concurrent cholestasis (i.e., bilirubin ≤35 µmol/l) and a cut-off value of >300 kU/l was used in the presence of cholestasis (i.e., bilirubin >35 µmol/l).
A further stratification index was generated for those patients where both preoperative CA19-9 and platelet–lymphocyte ratio were recorded (n = 52). If both levels were above the selected threshold values (n = 8), patients were classified as ‘high risk’ with an associated median overall survival of 10.1 (95% CI = 7.5 to 32.4) months. If either CA19-9 or PLR were elevated individually (n = 23), patients were classified as ‘intermediate risk’ with a median survival of 25.2 (95% CI = 14.1 to 47.8) months. For the remaining cases where both levels were less than the cut-off values (n = 21), patients were classified as ‘low risk’. The median overall survival time for this group was not reached but was found to be in excess of 60 months on Kaplan–Meier analysis (Fig. 3). When comparing the survival between these groups a log rank p value of less than 0.001 was obtained.
Table 3 demonstrates that the only significant difference between the three risk groups in terms of tumor histology was resection margin status with a trend toward an increased likelihood of margin involvement in the intermediate and high-risk groups compared with the low-risk group (Fisher’s exact, p = 0.046). There was no significant difference in the proportion of patients undergoing preoperative biliary drainage when comparing the three risk groups (p = 0.674). There was no difference in survival when comparing cases who did (n = 60) or did not require preoperative biliary drainage (n = 15) in the overall patient group [median survival = 34.9 (95% CI = 19.6 to 63.8) months and 32.7 (95% CI = 12.4 to NR) months, respectively—log rank, p = 0.988]. Similarly, there was no significant difference in the proportion of patients who went on to receive adjuvant therapy (p = 0.885).
The results of a multivariate survival analysis using Cox proportional hazards with forward stepwise regression are shown in Table 4. Resection margin status, tumor size, and nodal status were included alongside the preoperative CA19-9/platelet–lymphocyte ratio risk stratification. Nodal status failed to emerge as a significant variable on forward stepwise regression (p = 0.336) and was therefore omitted from the final multivariate model. Although an association between the preoperative risk stratification and likelihood of resection margin involvement was demonstrated (Table 3), the Cox analysis suggests that both were independent prognostic variables in this patient group. Tumor differentiation was not included as an additional covariate in the multivariate model due to the lack of statistical significance on univariate analysis (Table 2, p = 0.157) and the limited number of deaths that were seen (24 out of 52) in the patient group analyzed.24
Discussion
CA19–9 is widely used as a diagnostic tool in the preliminary investigation of suspected periampullary malignancy.25 As a prognostic tool, failure of normalization of CA19-9 levels post-resection is strongly associated with disease recurrence and poorer survival rates.10–12 Evidence also exists to suggest that pre-resection CA19-9 levels in isolation might act as a significant predictor of survival for periampullary cancer patients,2,13,14, but the prognostic value of preoperative CA19-9 levels in resected ampullary adenocarcinomas has not previously been independently investigated. Other studies have also suggested that various preoperative inflammatory and hematological parameters such as CRP15 along with the circulating platelet16,17 and lymphocyte counts18,19 confer significant prognostic information in resected pancreatic cancer. However, no studies to date have investigated whether any markers of systemic inflammation might also represent significant independent prognostic factors in resected ampullary cancer.
Chronic inflammation is both an etiological factor and physiological consequence of pancreatic carcinogenesis.26 The proinflammatory phase associated with systemic inflammation results in release of various immunological mediators such as interleukin (IL)-1, IL-3, and IL-6, which increase circulating platelet counts as a result of megakaryocyte proliferation.27,28 Preoperative thrombocytosis is commonly associated with a number of different malignancies and has been widely reported as an adverse prognostic marker in several cancers29,30 including pancreatic adenocarcinoma.16,17 Release of inhibitory mediators such as IL-10 and transforming growth factor beta 2 as part of the inflammatory response can result in reduced circulating and tumor-infiltrating lymphocyte counts.31 Pancreatic cancer has been shown to be associated with lower preoperative lymphocyte counts when compared with other gastrointestinal cancers.32 No previous studies have been published, which have sought to investigate the immunological interaction between tumor and host in the specific context of ampullary cancer.
The results from the present study indicate that an elevated preoperative CA19-9 level and platelet–lymphocyte ratio are both associated with poorer survival in patients undergoing resection for ampullary adenocarcinoma. The lack of any correlation between these two indices suggests that both markers are influenced by different aspects of ampullary tumor biology. The Kaplan–Meier analyses for each parameter (Figs. 1 and 2) demonstrate similar survival curves. However, use of a combined index incorporating both CA19-9 and platelet–lymphocyte ratio enables a low-risk patient group to be identified with a highly favorable survival outcome (>60 months), while a high-risk group can also be predicted for whom a median survival of less than 12 months is observed. This prognostic stratification was found to remain statistically significant when analyzed alongside the important histopathological tumor characteristics. Larger tumors, poor differentiation, nodal metastases, and R1 resections all exhibited the expected trend toward poorer survival on univariate analysis in keeping with previous studies.33–35
This finding has potential clinical relevance when considering which patients with resected ampullary cancer might benefit from adjuvant therapy. Although no definitive evidence exists to advocate adjuvant therapy as an optimum treatment strategy in resected ampullary cancer,36,37 the available evidence suggests that patients with less favorable histological tumor characteristics (e.g., T3/T4 tumors) tend to see more benefit from adjuvant treatment.38–41 The preoperative risk stratification described in the present study represents a potential prognostic tool that may be of use alongside tumor histology in selecting a patient group at high risk of early recurrence and poorer overall survival for whom adjuvant therapy may be of most benefit.
The majority of patients analyzed (80%) underwent intervention for biliary drainage before resection. Instrumentation of the biliary tree represents a potential source of preoperative sepsis42 and, as such, may act as a confounding factor in interpreting the survival data. Although previous studies have suggested that biliary drainage in the preoperative setting may increase the risk of early postoperative morbidity such as wound infection,43 no evidence exists to suggest that preoperative biliary stenting has any influence on operative mortality or subsequent survival after pancreatoduodenectomy. The results from the current study confirmed that the requirement for preoperative biliary drainage had no effect on postoperative survival after resection for ampullary cancer. Furthermore, when stratifying patients into the three risk groups, there was no significant difference in the proportion of cases in each group who underwent preoperative biliary stenting. This suggests that intervention for biliary drainage is unlikely to be a significant confounding factor in explaining the marked survival differences observed when comparing the three risk-stratified groups. Similarly, there was no significant difference in the proportion of patients in each risk group who went on to receive adjuvant treatment. Hence, adjuvant therapy is also unlikely to reflect a significant confounding factor when interpreting the survival data.
Conclusion
The results of the present study suggest that significant prognostic information can be obtained from routine blood results before resection for ampullary cancer. Stratification of ampullary adenocarcinoma patients according to both preoperative CA19-9 levels and platelet–lymphocyte ratio should be considered in the survival analyses of future adjuvant and neoadjuvant trials to validate these findings.
References
Goonetilleke KS, Siriwardena AK. Systematic review of carbohydrate antigen (CA19-9) as a biochemical marker in the diagnosis of pancreatic cancer. Eur J Surg Oncol 2007;33:266–270.
Kau SY, Shyr YM, Su CH, Wu CW, Lui WY. Diagnostic and prognostic values of CA19-9 and CEA in periampullary cancers. J Am Coll Surg 1999;188:415–420.
Ker CG, Chen JS, Lee KT, Sheen PC, Wu CC. Assessment of serum and bile level of CA19-9 and CA125 in cholangitis and bile duct carcinoma. J Gastroenterol Hepatol 1991;6:505–508.
von Ritter C, Eder MI, Stieber P, Lamerz R, Jungst D, Strigl M, Meyer G, Reuter C, Paumgartner G. Biliary mucin secreted by cultured human gallbladder epithelial cells carries the epitope of CA19-9. Anticancer Res 1997;17:2931–2934.
Brockmann J, Emparan C, Hernandez CA, Sulkowski U, Dietl KH, Menzel J, Wolters H, Glodny B, Senninger N. Gallbladder bile tumor marker quantification for detection of pancreato-biliary malignancies. Anticancer Res 2000;20:4941–4947.
Itzjowitz S, Kim Y. New carbohydrate tumour markers. Gastroenterology 1986;90:491–494.
Schlieman MG, Ho HS, Bold RJ. Utility of tumour markers in determining resectability of pancreatic cancer. Arch Surg 2003;138:951–956.
Connor S, Bosonnet L, Alexakis N, Raraty M, Ghaneh P, Sutton R, Neoptolemos JP. Serum CA19-9 measurement increases the effectiveness of staging laparoscopy in patients with suspected pancreatic malignancy. Dig Surg 2005;22:80–85.
Halloran CM, Ghaneh P, Connor S, Sutton R, Neoptolemos JP, Raraty MG. Carbohydrate antigen 19.9 accurately selects patients for laparoscopic assessment to determine resectability of pancreatic malignancy. Br J Surg 2008;95:453–459.
Sperti C, Pasquali C, Catalini S, Cappellazzo F, Bonadimani B, Behboo R, Pedrazzoli S. CA19-9 as a prognostic index after resection for pancreatic cancer. J Surg Oncol 1993;52:137–141.
Montgomery RC, Hoffman JP, Riley LB, Rogatko A, Ridge JA, Eisenberg BL. Prediction of recurrence and survival by post-resection CA19-9 values in patients with adenocarcinoma of the pancreas. Ann Surg Oncol 1997;4:551–556.
Safi F, Schlosser W, Falkenreck S, Beger HG. Prognostic value of CA19-9 serum course in pancreatic cancer. Hepatogastroenterology 1998;45:253–259.
Lundin J, Roberts PJ, Kuusela P, Roberts PJ. The prognostic value of preoperative serum levels of CA19-9 and CEA in patients with pancreatic cancer. Br J Cancer 1994;69:515–519.
Ferrone CR, Finkelstein DM, Thayer SP, Muzikansky A, Fernandez-delCastillo C, Warshaw AL. Perioperative CA19-9 levels can predict stage and survival in patients with pancreatic ductal adenocarcinoma. J Clin Oncol 2006;24:2897–2902.
Jamieson NB, Glen P, McMillan DC, McKay CJ, Foulis AK, Carter R, Imrie CW. Systemic inflammatory response predicts outcome in patients undergoing resection for ductal adenocarcinoma head of pancreas. Br J Cancer 2005;92:21–23.
Suzuki K, Aiura K, Kitagou M, Hoshimoto S, Takahashi S, Ueda M, Kitajima M. Platelet counts closely correlate with the disease-free survival interval of pancreatic cancer patients. Hepatogastroenterology 2004;51:847–853.
Brown KM, Domin C, Aranha GV, Yong S, Shoup M. Increased preoperative platelet count is associated with decreased survival after resection for adenocarcinoma of the pancreas. Am J Surg 2005;189:278–282.
Yamaguchi K, Noshiro H, Shimizu S, Morisaki T, Chijiiwa K, Tanaka M. Long-term and short-term survivors after pancreatectomy for pancreatic cancer. Int Surg 2000;85:71–76.
Fogar P, Sperti C, Basso D, Sanzari MC, Greco E, Davoli C, Navaglia F, Zambon CF, Pasquali C, Venza E, Pedrazzoli S, Plebani M. Decreased total lymphocyte counts in pancreatic cancer: an index of adverse outcome. Pancreas 2006;32:22–28.
Smith RA, Bosonnet L, Raraty M, Sutton R, Neoptolemos JP, Ghaneh P. Preoperative platelet-lymphocyte ratio is an independent significant prognostic marker in resected pancreatic ductal adenocarcinoma. Am J Surg 2008; in press.
Campbell F, Bennett M, Foulis AJ. Minimum dataset for histopathological reporting of pancreatic, ampulla of Vater and bile duct carcinoma. Royal College of Pathologists; 2002. http://www.rcpath.org.
Sobin LH, Wittekind CH. TNM classification of malignant tumours. 5th ed. New York: Wiley, 1997.
Altman DG, Lausen B, Sauerbrei W, Schumacher M. Dangers of using optimal cutpoints in the evaluation of prognostic factors. J Nat Cancer Inst 1994;86:829–835.
Vittinghoff E, McCulloch CE. Relaxing the rule of ten events per variable in logistic and Cox regression. Am J Epidemiol 2006;165:710–718.
Koprowski H, Steplewski Z, Mitchell K, Herlyn M, Herlyn D, Fuhrer P. Colorectal carcinoma antigens detected by hybridoma antibodies. Somat Cell Genet 1979;5:957–972.
McKay CJ, Glen P, McMillan DC. Chronic inflammation and pancreatic cancer. Best Prac Res Clin Gastroent 2008;22:65–73.
Klinger MH, Jelkmann W. Role of blood platelets in infection and inflammation. J Interferon Cytokine Res 2002;22:913–922.
Alexandrakis MG, Passam FH, Moschandrea IA, Christophoridou AV, Pappa CA, Coulocheri SA, Kyriakou DS. Levels of serum cytokines and acute phase proteins in patients with essential and cancer-related thrombocytosis. Am J Clin Oncol 2003;26:135–140.
Monreal M, Fernandez-Llamazares J, Pinol M, Julian JF, Broggi M, Escola D, Abad A. Platelet count and survival in colorectal cancer—a preliminary study. Thromb Haemost 1998;79:916–918.
Ikeda M, Furukawa H, Imamura H, Shimizu J, Ishida H, Masutani S, Tatsuta M, Satomi T. Poor prognosis associated with thrombocytosis in patients with gastric cancer. Ann Surg Oncol 2002;9:287–291.
Salazar-Onfray F, Lopez MN, Mendoza-Naranjo A. Paradoxical effects of cytokines in tumor immune surveillance and tumor escape. Cytokine Growth Factor Rev 2007;18:171–182.
Romano F, Uggeri F, Crippa S, Di Stefano G, Scotti M, Scaini A, Caprotti R, Uggeri F. Immunodeficiency in different histotypes of radically operable gastrointestinal cancers. J Exp Clin Cancer Res 2004;23:195–200.
Beger HG, Treitschke F, Gansauge F, Harada N, Hiki N, Mattfeldt T. Tumor of the ampulla of Vater: Experience with local or radical resection in 171 consecutively treated patients. Arch Surg 1999;134:526–532.
Brown KM, Tompkins AJ, Yong S, Aranha GV, Shoup M. Pancreaticoduodenectomy is curative in the majority of patients with node negative ampullary cancer. Arch Surg 2005;140:529–533.
Riall TS, Cameron JL, Lillemoe KD, Winter KD, Campbell KA, Hruban RH, Chang D, Yeo CJ. Resected periampullary adenocarcinoma: 5-year survivors and their 6- to 10-year follow-up. Surgery 2006;140:764–772.
Klinkenbijl JH, Jeekel J, Sahmoud T, van Pel R, Couvreur ML, Veenhof CH, Arnaud JP, Gonzalez DG, de Wit LT, Hennipman A, Wils J. Adjuvant radiotherapy and 5-fluorouracil after curative resection of cancer of the pancreas and periampullary region: phase III trial of the EORTC gastrointestinal tract cancer cooperative group. Ann Surg 1999;230:776–782.
Takada T, Amano H, Yasuda H, Nimura Y, Matsushiro T, Kato H, Nagakawa T, Nakayama T, Study Group of Surgical Adjuvant Therapy for Carcinomas of the Pancreas and Biliary Tract. Is postoperative adjuvant chemotherapy useful for gallbladder carcinoma? A phase III mulitcenter prospective randomized controlled trial in patients with resected pancreaticobiliary carcinoma. Cancer 2002;95:1685–1695.
Lee JH, Whittington R, Williams NN, Berry MF, Vaughn DJ, Haller DG, Rosato EF. Outcome of pancreaticoduodenectomy and impact of adjuvant therapy for ampullary carcinomas. Int J Radiat Oncol Biol Phys 2000;47:945–953.
Mehta VK, Fisher GA, Ford JM, Poen JC, Vierra MA, Oberhelman HA, Bastidas AJ. Adjuvant chemoradiotherapy for “unfavorable” carcinoma of the ampulla of Vater: preliminary report. Arch Surg 2001;136:65–69.
Sikora SS, Balachandran P, Dimri K, Rastoqi N, Kumar A, Saxena R, Kapoor VK. Adjuvant chemoradiotherapy in ampullary cancers. Eur J Surg Oncol 2005;31:158–163.
Krishnan S, Rana V, Evans DB, Varadhachary G, Das P, Bhatia S, Delclos ME, Janjan NA, Wolff RA, Crane CH, Pisters PW. Role of adjuvant chemoradiation therapy in adenocarcinomas of the ampulla of Vater. Int J Radiat Oncol Biol Phys 2008;70:735–743.
Jagannath P, Dhir V, Shrikhande S, Shah RC, Mulllerpatan P, Mohandas KM. Effect of preoperative biliary stenting on immediate outcome after pancreaticoduodenectomy. Br J Surg 2005;92:356–361.
Sewnath ME, Karsten TM, Prins MH, Rauws EJ, Obertop H, Gouma DJ. A meta-analysis on the efficacy of preoperative biliary drainage for tumors causing obstructive jaundice. Ann Surg 2002;236:17–27.
Acknowledgment
Financial support from the Cancer Research UK is acknowledged.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Smith, R.A., Ghaneh, P., Sutton, R. et al. Prognosis of Resected Ampullary Adenocarcinoma by Preoperative Serum CA19-9 Levels and Platelet-Lymphocyte Ratio. J Gastrointest Surg 12, 1422–1428 (2008). https://doi.org/10.1007/s11605-008-0554-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-008-0554-3