Abstract
Purpose
To compare the pathologic effect of a mixture of n-butyl cyanoacrylate (NBCA), lipiodol, and ethanol (NLE) with a mixture of NBCA and lipiodol (NL) on the embolized vascular wall.
Materials and methods
Embolization was performed using four swine with NBCA and lipiodol in a volume ratio of 1:1 (NL11group) in the common hepatic artery (n = 1) and the internal iliac artery (n = 2); and with NBCA, lipiodol, and ethanol in a volume ratio of 1:1:2 (NLE112 group) in the common hepatic artery (n = 3) and the internal iliac artery (n = 6).
Results
NL11 casts had an intricate appearance in reticular configuration with red thrombus, while NLE112 casts presented in a single round configuration with surrounding ring-like red thrombus. Desquamation of endothelial cells and infiltration of neutrophils into the adventitial layer were found in all embolized vessels in both groups. Infiltration of neutrophils into the intermediate layer was found in the NL11 group but not in the NLE112 group.
Conclusion
The damage to the vascular wall caused by NLE112 was milder than that by NL11, implying the adverse effects of NLE112 are within tolerable limits.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
When a mixture of n-butyl cyanoacrylate (NBCA) and lipiodol is injected into blood or saline, the monomer NBCA becomes a polymer by anionic polymerization. The resulting solid is a potent material for vessel occlusion but also adheres to the devices used during embolization [1–5]. It is reported that the polymerization speed can be delayed by dilution with lipiodol [6–8]. When a mixture of NBCA, ethanol, and lipiodol was injected into saline, the resulting solid polymer was found to be minimally adhesive to the catheter, implying the feasibility of the embolic material for vessel occlusion [9]. However, NBCA is known to cause acute vasculitis [10–12], while ethanol causes cell damage by deprivation of intracellular fluid and coagulation necrosis of the vascular wall and organ parenchyma [13–15]. Based on these findings, the risk to the vascular wall of a mixture of NBCA and ethanol would appear to be greater than that of NBCA alone. It is crucial to investigate the effects on the vascular wall before this mixture can be used clinically.
The purpose of this study is to evaluate the pathologic effect on the embolized vascular wall of a mixture of NBCA, lipiodol, and ethanol (NLE) compared with that of a mixture of NBCA and lipiodol (NL), in transcatheter arterial embolization (TAE).
Materials and methods
The institutional committee on research animal care approved this study prior to its initiation.
Four female swine weighing 52–55 kg were used. To avoid the effect of inflammatory changes from organ infarction on the vessel wall, we selected the common hepatic artery and the right and left internal iliac arteries for proximal embolization because occlusion of these arteries causes minimal ischemic organ damage. Two embolic materials were used: a mixture of NBCA (Histoacryl: Aesculap, Tuttlingen, Germany) and lipiodol (iodinated ethyl esters of the fatty acid of poppy seed containing 40 % iodine) in a volume ratio of 1:1 (NL11); and a mixture of NBCA, lipiodol, and ethanol (99.5 %, Nakalai Tesque INC, Kyoto, Japan) in a volume ratio of 1:1:2 (NLE112) (Fig. 1). Embolization was performed in major arteries. We performed three embolizations with NL11 using one swine as control, in the common hepatic artery (n = 1) and the internal iliac artery (n = 2). We performed nine embolizations with NLE112 using three swine, in the common hepatic artery (n = 3) and in the internal iliac artery (n = 6). Pre-anesthesia was conducted with 5 mg/kg ketamine and 0.08 mg/kg atropine sulfate, and general anesthesia was maintained with isoflurane gas via tracheal intubation. Cardiac and pulmonary parameters were monitored throughout the procedures.
a Macroscopic view of a mixture of n-butyl cyanoacrylate and lipiodol in a volume ratio of 1:1, in saline (NL11 n-butyl-cyanoacrylate and lipiodol). b Macroscopic view of a mixture of n-butyl cyanoacrylate, lipiodol, and ethanol in a volume ratio of 1:1:2, in saline (NLE112 n-butyl-cyanoacrylate, lipiodol, and ethanol)
A 5 F sheath (Radifocus Introducer II H; Terumo Clinical Supply, Gifu, Japan) was inserted from the right femoral artery, and activated clotting time was maintained at more than 200 s (normal range: less than 120 s) during the procedure by heparin injection of 50 units/kg. A 5 F balloon catheter (Selecon MP 9 mm in diameter, 70 cm in length; Terumo Clinical Supply) was first advanced to the common hepatic artery, right internal iliac artery, or left internal iliac artery. A 2.2 F microcatheter was then advanced distally via the balloon catheter. Under interruption of arterial blood flow by balloon inflation, either NL11 or NLE112 was injected. Prior to injection, a 5 % glucose solution was infused into the microcatheter to prevent polymerization of the NBCA.
The syringe containing the NLE112 was thoroughly shaken by hand for several minutes to ensure homogeneous mixing. The injection was conducted slowly under radio-fluoroscopy. To avoid the embolic material adhering to the balloon catheter, the microcatheter was removed immediately after completion of the injection. The balloon catheter was deflated 10 min later, and an abdominal radiograph was taken to confirm the position of the embolic materials (Fig. 2). Two days after the procedure, another radiograph was taken to check whether the embolic material had migrated. The swine were then euthanized and necropsies were performed, and the common hepatic artery and the right and left internal iliac arteries were removed. To evaluate the histological effect of embolization on the vessel wall, the vessels were cut into 3-mm-thick sections and fixed in a 7.5 % neutral formaldehyde buffer. The vessel specimen for each group was stained with hematoxylin-eosin (HE) for microscopic examination. By macroscopic and microscopic examination, we investigated the presence of NL11 or NLE112 in the hepatic and iliac arteries in all specimens, and the extent of vessel wall damage in the specimen in each group that contained the largest amount of embolic material.
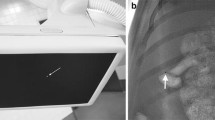
a Common hepatic arteriography depicts the gastroduodenal artery and three hepatic artery branches. b Radiograph taken after embolization of the common hepatic artery. The white arrow indicates the cast of the embolic material in the common hepatic artery. c Pelvic arteriography depicts the bilateral external and internal iliac arteries. d Radiograph taken after embolization of both internal iliac arteries. The white arrows indicate the cast of the embolic material in the internal iliac arteries
Results
Mobility of the embolic material
Abdominal radiographs obtained 10 min after injection and again after balloon deflation showed successful placement of the NL11 and NLE112 casts in the target arteries. Abdominal radiographs obtained 2 days later showed that none of the three NL11 casts had migrated, and the three NLE112 casts of the nine NLE112 casts, had migrated in the vessels (Fig. 3; Table 1).
Radiographs taken immediately after (a) and 2 days after (b) embolization of the bilateral internal iliac arteries with NLE112. In the right internal iliac artery, there was migration of the NLE112 cast to the peripheral branch at 2 days, while the NLE112 cast in the left internal iliac artery did not migrate. (White arrows indicate NLE112 casts.)
Macroscopic configuration of emboli in the vessels
In one vessel embolized with NLE112, the cast had migrated beyond the abdomen and could not be investigated. The remaining eleven vessels were evaluated for pathological change. There was no damage to the vessel wall in either group. NL11 casts and NLE112 casts were expanded and fully occluded the vessels. The NL11 casts had an intricate appearance, a reticular configuration with red thrombus (Fig. 4a), while the NLE112 casts were in a single round configuration and ringed by red thrombus (Fig. 5a).
Histological examination of an artery embolized with NL11. a NL with reticular configuration and red thrombus completely fills the vessel lumen. Hematoxylin-eosin (HE) stain: original magnification, ×20. b Desquamation of endothelial cells (asterisks) and infiltration of neutrophils (arrows) into the layers of intermediate membrane and adventitia. HE stain: original magnification, ×200. NL11 mixture of n-butyl cyanoacrylate and lipiodol in a volume ratio of 1:1
Histological examination of an artery embolized with NLE112. a NLE112 in a single round configuration with surrounding ring-like red thrombus is seen in the vessel lumen. Hematoxylin-eosin (HE) stain: original magnification, ×20. b Desquamation of endothelial cells (asterisk) was found with infiltration of neutrophils (arrows) into the adventitial layer but not into the intermediate layer. HE stain: original magnification, ×200. NLE mixture of n-butyl cyanoacrylate, lipiodol, and ethanol in a volume ratio of 1:1:2
Histological inflammatory response of the vessel wall
On microscopic examination, no necrosis was seen in the vessel wall of any specimen. In the three vessels embolized with NL11, desquamation of endothelial cells and infiltration of neutrophils into the intermediate membrane and adventitia was seen (Fig. 4b). Desquamation of endothelial cells and infiltration of neutrophils into the adventitial layer were also found in the eight vessels embolized with NLE112, but infiltration of neutrophils into the intermediate membrane layer was not observed (Fig. 5b; Table 2).
Discussion
Successful cast formation in the lumen was achieved in major vessels for both the NL11 and NLE112 groups. In comparing cast mobility between NL11 and NLE112, cast movement occurred in none of the NL11 group but in three of the nine casts of the NLE112 group. This finding indicates that NLE112 is less strongly adhesive to the vascular wall than is NL11. NBCA is reported to adhere to skin wounds and catheters. In the blood, it hardens by polymerization with hydroxyl anions [3–5, 16]. The addition of ethanol is reported to accelerate the polymerization process and to weaken the strength of adhesion to the catheter [1, 9]. The present results confirmed that the addition of ethanol decreases the strength with which NBCA adheres to the vascular wall.
Microscopic examination revealed that NL11 in the vessel had an intricate reticular configuration with red thrombus, whereas NLE112 presented as a single round droplet surrounded by a ring of red thrombus. In an in vitro study, NL11 injected into saline formed an accumulation of small oily droplets, while NLE112 injected into saline formed a single round droplet [9]. The present findings confirmed that NLE112 maintained similar configurations in vivo as that in vitro.
When NBCA creates a cast following polymerization, more resultant heat is generated as the water component increases [3, 16]. In previous histological studies of vessels occluded by NBCA embolization, it was suggested that vasculitis had probably occurred as a result of the heat generated by polymerization [17].
In the present study, microscopic examination revealed the desquamation of endothelial cells and infiltration of inflammatory cells into the adventitia in both the NL11 and NLE112 groups. However, infiltration of inflammatory cells into the intermediate membrane was found in the NL11 group but not in the NLE112 group, and the inflammatory cells appeared to have migrated from outside the vessel rather than from the vascular lumen. The vasa vasorum, a network of small arteries and veins, surrounds and penetrates the adventitia of large arteries [18–20]. The inflammatory cells could therefore have migrated from the small arteries of the vasa vasorum. We consider that the NLE112 group induced less disorder to the vascular wall compared with the NL11 group because polymerization was more instant in the NLE112 group.
A limitation of the present study is that the follow-up term of 2 days is rather short. Although inflammatory change to the vascular wall was mild, further investigation of NLE112 is warranted.
In conclusion, the damage to the vascular wall caused by NLE112 was milder than that by NL11. These findings indicate that the adverse effects caused by NLE112 as an embolic material are within tolerable limits.
References
Gad SC, editor. Pharmaceutical manufacturing handbook: production and processes. Hoboken (NJ): Wiley; 2008. p 364–367.
American Society for Gastrointestinal Endoscopy Assessment Committee. Technology status evaluation report: tissue adhesives and fibrin glues. Gastrointest Endosc. 2004;60:327–33.
Petkewich R. Liquid bandages. Chem Eng News. 2008;86:81.
Debrun GM, Aletich VA, Shownkeen H, Ausman J. Glued catheters during embolization of brain AVMs with acrylic glue. Interv Neuroradiol. 1997;30:13–9.
n-BCA Trial Investigators. N-Butyl cyanoacrylate embolization of cerebral arteriovenous malformations: results of a prospective, randomized, multi-center trial. AJNR Am J Neuroradiol. 2002;23:748–55.
Stoesslein F, Ditscherlein G, Romaniuk PA. Experimental studies on new liquid embolization mixtures (histoacryl-lipiodol, histoacryl-panthopaque). Cardiovasc Intervent Radiol. 1982;5:264–7.
Spiegel SM, Vinuela F, Goldwasser JM, Fox AJ, Pelz DM. Adjusting the polymerization time of isobutyl-2 cyanoacrylate. AJNR Am J Neuroradiol. 1986;7:109–12.
Gounis MJ, Lieber BB, Wakhloo AK, Siekmann R, Hopkins LN. Effect of glacial acetic acid and ethiodized oil concentration on embolization with N-butyl 2-cyanoacrylate: an in vivo investigation. AJNR Am J Neuroradiol. 2002;23:938–44.
Kawai N, Sato M, Minamiguchi H, et al. Basic study of a mixture of n-butyl cyanoacrylate, ethanol, and lipiodol as a new embolic material. J Vasc Radiol. 2012;23:1516–21.
Brothers MF, Kaufmann JCE, Fox AJ, Deveikis JP. n-Butyl 2-cyanoacrylate—substitute for IBCA in interventional neuroradiology: histopathologic and polymerization time studies. AJNR Am J Neuroradiol. 1989;10:777–86.
Cylwik B, Darewicz J, Karasewicz B. Morphometric and histological examinations of dog kidneys after embolization of the renal artery with the cyanoacrylic glue “Chirurcoll-Polfa”. Int Urol Nephrol. 1985;17:303–9.
Tanaka T, Kawai N, Sato M, et al. Safety of bronchial arterial embolization with n-butyl cyanoacrylate in a swine model. World J Radiol. 2012;28:455–61.
Shiina S, Tasuda H, Muto H, et al. Percutaneous ethanol injection in the treatment of liver neoplasms. AJR Am J Roentgenol. 1987;149:949–52.
Kawano M. An experimental study of percutaneous absolute ethanol injection therapy for small hepatocellular carcinoma: effects of absolute ethanol on the healthy canine liver. Gastroenterol Jpn. 1989;24:663–9.
Ivanick MJ, Thorwarth W, Donohue J, Mandell V, Delany D, Jaques PF. Infarction of the left main-stem bronchus: a complication of bronchial artery embolization. AJR Am J Roentgenol. 1983;141:535–7.
Qureshi A, Roberts AC, Drew PJ, Monson JRT, Duthie GS. n-Butyl cyanoacrylate adhesive for skin closure of abdominal wounds: preliminary results. Am R Coll Surg Engl. 1997;79:414–5.
Matsuo T, Yanai H, Sugiu K, Tominaga S, Kimata Y. Orbital exenteration after transarterial embolization in a patient with Wyburn-Mason syndrome: pathologic findings. Jpn J Ophthalmol. 2008;52:308–13.
Woerner CA. Vasa vasorum of arteries, their demonstration and distribution. In: Lansing AI, editor. The arterial wall. Baltimore: Williams and Wilkins; 1959. p 1–14.
O’Neill JF. The effects on venous endothelium of alterations in blood flow through the vessels in the vein walls and the possible relation to thrombosis. Ann Surg. 1947;126:270–88.
Scotland RS, Vallance PJT, Ahluwalia A. Endogeneous factors involved in regulation of tone of arterial vasa vasorum: implications for conduit vessel physiology. Cardiovasc Res. 2000;46:403–11.
Conflict of interest
All authors have no conflict of interest to declare. The authors have no personal, financial or institutional interest in any of the drugs, materials, or devices documented in this manuscript.
Author information
Authors and Affiliations
Corresponding author
About this article
Cite this article
Tanaka, F., Kawai, N., Sato, M. et al. Effect of transcatheter arterial embolization with a mixture of n-butyl cyanoacrylate, lipiodol, and ethanol on the vascular wall: macroscopic and microscopic studies. Jpn J Radiol 33, 404–409 (2015). https://doi.org/10.1007/s11604-015-0432-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11604-015-0432-3