Abstract
Purpose
Dysphagia is a symptom of different pathological conditions characterised by alteration of the swallowing mechanism, which may manifest at different levels. We report our experience in the evaluation of the swallowing mechanism with combined videofluoroscopy and manometric recordings.
Materials and methods
For the combined study, we used a Dyno Compact computerised system (Menfis Biomedical s.r.l., Bologna, Italy) equipped with: (1) graphics card for the management of ultrasonographic or radiological images; (2) A.VI.U.S. dedicated software package, which enables digital-quality recording (PAL/NTSC, composite video or S-Video) of the videofluoroscopy study in AVI format with 320×240 resolution and 25 Hz acquisition frequency. The delay introduced by the process of image digitalisation is in the order of 200 ms, so for analysis purposes, the images can be considered synchronised with the manometric recordings. The videomanometry study was performed with the administration of contrast material either in bolus form or diluted. Data were collected on a specifically designed grid for the evaluation of 46 videofluoroscopic items, of which 34 are derived from the laterolateral view (seven in the oral preparatory phase, 15 in the oral transport phase and 12 in the pharyngeal phase) and 12 in the anteroposterior view (six in the oral preparatory phase and six in the oropharyngeal phase). A positive finding for the individual parameters is expressed in a binary fashion. Manometric evaluation was based on 11 items divided into four major and seven minor criteria.
Results
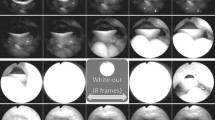
Dynamic videofluoroscopy swallow study combined with concurrent manometry enabled the simultaneous recording of anatomical alterations and the functional data of oropharyngeal pressure, thus providing a picture of the anatomical, biomechanical and physiological conditions of swallowing and the manner of bolus propulsion and transit.
Conclusions
An early and effective diagnosis of oropharyngeal dysphagia means being able to effectively implement appropriate rehabilitation techniques, improve the patient’s quality of life, and minimise the complications associated with swallowing disorders (choking, aspiration pneumonia, malnourishment). Distinction of the anatomical level of dysphagia is not a matter of simple classification; rather, it is essential in that different clinical presentations require different diagnostic strategies, and a precise definition of the anatomical-functional substrate is required to implement the correct therapeutic approach. This study presents the authors’ experience with the use of combined videofluoroscopy and manometry with particular emphasis on the examination technique.
Riassunto
Obiettivo
La disfagia è un sintomo sotteso da differenti quadri patologici, in cui si verifica un’alterazione del meccanismo deglutitorio, che può estrinsecarsi a vari livelli. Gli autori riportano la loro esperienza nella valutazione del meccanismo della deglutizione mediante l’integrazione diagnostica combinata manometrica e videofluoroscopica.
Materiali e metodi
Per lo studio combinato è stato impiegato il sistema computerizzato “Dyno Compact” (Menfis Biomedical s.r.l., Bologna, Italia) dotato di: 1) scheda grafica per la gestione di immagini ecografiche o radiografiche; 2) A.VI.U.S. software dedicato, attraverso il quale è possibile registrare in qualità digitale (PAL/NTSC, video composito o S-Video) la videofluoroscopia, in filmati AVI con risoluzione 320×240 e con frequenza di acquisizione di 25 Hz; il ritardo introdotto dal processo di digitalizzazione dell’immagine è dell’ordine dei 200 ms, quindi, ai fini dell’analisi, l’immagine si può considerare sincronizzata con i tracciati pressori. Lo studio VFS è stato effettuato mediante somministrazione di boli adeguati di mezzo di contrasto opportunamente diluito. I dati vengono raccolti su una griglia precostituita per la valutazione di 46 items videofluoroscopici, di cui 34 derivano dallo studio in proiezione latero-laterale (7 in fase buccale, 15 in fase orale e 12 in fase faringea) e 12 dallo studio in proiezione antero-posteriore (6 in fase buccale e 6 in fase orofaringea); la positività ai singoli parametri è espressa in maniera binaria. La valutazione pressoria si basa su 11 sialoritems manometrici, a loro volta divisi in 4 criteri maggiori e 7 minori
Risultati
La valutazione fluoroscopica dinamica della deglutizione con registrazione video abbinata alla manometria simultanea, ha permesso di registrare contemporaneamente le alterazioni anatomiche correlandole al dato funzionale della pressione orofaringea, consentendo durante la medesima registrazione di valutare la situazione anatomica, biomeccanica e fisiologica della deglutizione e le modalità di propulsione e transito del bolo.
Conclusioni
Fare precocemente una buona diagnosi di disfagia orofaringea significa poter intervenire efficacemente con tecniche riabilitative logopediche, migliorare la qualità di vita del paziente, nonché ridurre al minimo le complicanze che questa comporta (soffocamento, polmonite ab ingestis, malnutrizione). La differenziazione del livello anatomico della disfagia non riveste una semplice categorizzazione, ma è indispensabile in quanto alla diversità di presentazione clinica corrisponde un differente approccio metodologico diagnostico, ed a una precisa definizione del substrato anatomo-funzionale responsabile del sintomo, corrisponde un diverso approccio terapeutico. Gli autori con il presente contributo presentano la loro esperienza nell’impiego della videofluoromanometria ed in particolare la metodologia di conduzione dell’esame.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Miller AJ (2002) Oral and pharyngeal reflexes in the mammalian nervous system. Crit Rev Oral Biol Med 13:409–425
Donner MW, Bosma JF, Robertson DL (1985) Anatomy and physiology of the pharynx. Gastrointest Radiol 10:196–212
Bosma JF (1957) Deglutition Pharyngeal state. Physiol Rev 37:275–300
Miller AJ (1982) Deglutition. Physiol Rev 62:129–184
Dodds WJ, Stewart ET, Longeman JA (1990) Physiology and radiology of the normal oral and pharyngeal phases of swallowing. AJR Am J Roentgenol 154:953–963
Logeman JA (1995) Dysphagia: evaluation and treatment. Folia Phoniatr Logop47:140–164
College of Audiologists and Speech Language Pathologists of Ontario (CASPO) (2000) Preferred practice guideline for dysphagia
American Speech Language Hearing Association (ASHA) (2001) Clinical indicators for instrumental assessment of dysphagia. ASHA Special interest report 2001. Available from url: http://dysphagia.com/asha_SID_12.htm
Reilly S, Douglas J, Oates J (2001) Evidence-based practice in speech pathology. Whurr Publishers, London and Philadelphia
Logemann JA (1983) Evaluation and treatment of swallowing disorders. College Hill Press, San Diego, CA
Arvedson J, Rogers B, Buck G et al(1994) Silent aspiration prominent in children with dysphagia (1994). Int J Ped Othorhinolaryng 28:173–181
Aviv JE (2000) Prospective, randomized outcome of endoscopy versus modified barium swallow on patients with dysphagia. Laryngoscope 110:563–574
Ali GN, Fallace KL, Schwartz R et al (1996) Mechanism of oral-pharyngeal dysphagia in patients with parkinson’s disease. Gastroenterology 110:383–392
Barbiera F, Condello S, De Palo A er al (2006) Role of videofluorography swallow study in management of dysphagia in neurologically compromised patients. Radiol Med 111:818–827
Gates J, Hartnell GG, Gramigna GD (2006) Videofluoroscopy and swallowing studies for neurologic disease: a primer. RadioGraphics 26:e22
Kahrilas PJ, Dodds WJ, Dent J et al (1998) Upper esophageal sphincter function during deglutition. Gastroenterology 95:52–62
Kahrilas PJ (1994) Anathomy, physiology and pathophysiology of dysphagia. Acta Otorhinolaryngol Belg 48:97–117
Kelly J (1997) Use of manometry in the evaluation of dysphagia. Otolaryngol Head Neck Surg 116:355–357
Sokol EM, Heitmann P, Wolf BS, Cohen BR (1966) Simultaneous cineradiographic-manometric study of the distal esophagus: small hiatal hernias and rings. Gastroenterology 50:737–753
Mcconnel FMS, Cerenko D, Hersh T, Weil LJ (1988) Evaluation of pharyngeal dysphagia with manofluorography. Dysphagia 2:187–195
Castell JA, Dalton CB, Castell DO (1990) Pharyngeal and upper esophageal sphincter manometry in humans. Am J Physiol 258:G173–G178
Olsson R, Castell JA, Castell DO, Ekberg O (1995) Solid-state computerized manometry improves diagnostic yield in pharyngeal dysphagia: simultaneous videoradiography and manometry in dispagia patients with normal barium swallows. Abdom Imaging 20:230–235
Goeleyen A, Robberecht W, Carbonez A, Dejaeger E (2006) Manofluorographic evaluation of swallowing in amyotrophic lateral sclerosis and its relationship with clinical evaluation of swallowing. Amyotroph Lateral Scler 7:235–240
Lang IM, Shaker R (1997) Aatomy and physiology of tha upper esophageal sphincter. Am J Med 103:50S–55S
De Caluwe D, Nassogne MC, Reding R et al (1999) Cricopharyngeal achalasia: case report and review of the literature. Eur J Pediatr Surg 9:109–112
Williams RBH, Wallace KL, Ali GN, Cook IJ (2002) Biomechanics of failed deglutitive upper esophageal sphincter relaxation in neurogenic dysphagia. Am J Physiol Gastrointest Liver Physiol 283:G16–G26
Buchholz DW (1994) Neurogenic dysphagia: what is the cause when the cause is not obvious? Dysphagia 9:245–255
Cook IJ, Kharilas PJ (1999) American Gastroenterological Association Technical review on management of oropharyngeal dysphagia. Gastroenterology 116:455–478
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Cappabianca, S., Reginelli, A., Monaco, L. et al. Combined videofluoroscopy and manometry in the diagnosis of oropharyngeal dysphagia: examination technique and preliminary experience. Radiol med 113, 923–940 (2008). https://doi.org/10.1007/s11547-008-0290-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-008-0290-5