Abstract
Purpose
This study was performed to clarify the role of perfusion-weighted imaging (PWI) at 3 Tesla in the characterisation of haemodynamic heterogeneity within gliomas and surrounding tissues and in the differentiation of high-grade from low-grade gliomas.
Materials and methods
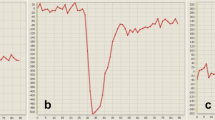
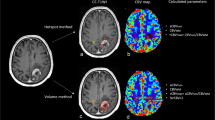
We examined 36 patients with histologically verified gliomas (25 with high-grade and 11 with low-grade gliomas). PWI was performed by first-pass gadopentetate dimeglumine T2*-weighted echo-planar images, and cerebral blood volume (CBV) maps were computed with a nondiffusible tracer model. Relative CBV (rCBV) was calculated by dividing CBV in pathological areas by that in contralateral white matter.
Results
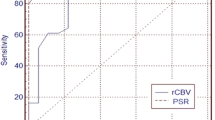
In high-grade gliomas, rCBV were markedly increased in mass [mean±standard deviation (SD), 4.3±1.2] and margins (4.0±1.1) and reduced in necrotic areas (0.3±0.3). Oedematous-appearing areas were divided in two groups according to signal intensity on T2-weighted images: tumour with lower (nearly isointense to grey matter) and oedema with higher (scarcely isointense to cerebrospinal fluid) signal intensity. Tumour showed significantly higher rCBV than did oedema (1.8±0.5 vs. 0.5±0.2; p<0.001) areas. In low-grade gliomas, mass (2.0±1.5) and margin (2.2±1.2) rCBV were significantly lower than in high-grade gliomas (p<0.001).
Conclusions
Three-Tesla PWI helps to distinguish necrosis from tumour mass, infiltrating tumour from oedema and high-grade from low-grade gliomas. It enhances the magnetic resonance (MR) assessment of cerebral gliomas and provides useful information for planning surgical and radiation treatment.
Riassunto
Obiettivo
Chiarire il ruolo dell’imaging pesato in perfusione (PWI) a 3 Tesla nella caratterizzazione dell’eterogeneità emodinamica dei gliomi cerebrali e dei tessuti circostanti, e nella differenziazione dei gliomi di alto grado da quelli di basso grado.
Materiali e metodi
Abbiamo esaminato 36 pazienti con gliomi verificati istologicamente (25 con alto ed 11 con basso grado). Il PWI è stato ottenuto mediante immagini eco-planari T2*-pesate con primo passaggio di gadopentetato di dimeglumina, e le mappe di volume ematico cerebrale (CBV) sono state elaborate con il modello del tracciante non diffusibile. Il volume ematico cerebrale relativo (rCBV) è stato calcolato dividendo il CBV nelle aree patologiche per quello nella sostanza bianca controlaterale.
Risultati
Nei gliomi di alto grado, l’rCBV appariva marcatamente incrementato nella massa (media±SD, 4,3±1,2) ed ai margini (4,0±1,1), e ridotto nelle aree necrotiche (0,3±0,3). Le regioni apparentemente edematose sono state divise in due gruppi sulla base dell’intensità di segnale nelle immagini pesate in T2: “tumore” con più basso segnale (quasi isointenso alla sostanza grigia) ed “edema” con segnale più elevato (quasi isointenso al liquido cefalorachidiano). Le aree “tumore” presentavano rCBV significativamente più elevato rispetto a quelle “edema” (1,8±0,5 vs 0,5±0,2; p<0,001). Nei gliomi di basso grado, l’rCBV nella massa (2,0±1,5) e nel margine (2,2±1,2) erano significativamente più bassi che nei gliomi di alto grado (p<0,001).
Conclusioni
Il PWI a 3T aiuta a differenziare la necrosi dalla massa tumorale, il tumore infiltrante dall’edema, e i gliomi di alto grado da quelli di basso grado. Esso facilita la caratterizzazione in RM dei gliomi cerebrali e fornisce utili informazioni per la pianificazione del trattamento chirurgico e radiante.
Article PDF
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
References/Bibliografia
Hess KR, Broglio KR, Bondy ML (2004) Adult glioma incidence trends in the United States, 1977–2000. Cancer 101:2293–2299
Cha S (2006) Update on brain tumor imaging: from anatomy to physiology. AJNR Am J Neuroradiol 27:475–487
Ginsberg LE, Fuller GN, Hashmi M et al (1998) The significance of lack of MR contrast enhancement of supratentorial brain tumors in adults: histopathological evaluation of a series. Surg Neurol 49:436–440
Cha S, Knopp EA, Johnson G et al (2002) Intracranial mass lesions: dynamic contrast-enhanced susceptibility-weighted echo-planar perfusion MR imaging. Radiology 223:11–29
Covarrubias DJ, Rosen BR, Lev MH (2004) Dynamic magnetic resonance perfusion imaging of brain tumors. Oncologist 9:528–537
Barbier E, Lamalle L, Decorps M (2001) Methodology of brain perfusion imaging. J Magn Reson Imaging 13:496–520
Aronen HJ, Gazit I, Louis D et al (1994) Cerebral blood volume maps of gliomas: comparison with tumor grade and histologic findings. Radiology 191:41–51
Sugahara T, Korogi Y, Kochi M et al (1998) Correlation of MR imagingdetermined cerebral blood volume maps with histologic and angiographic determination of vascularity of gliomas. AJR Am J Roentgenol 171:1479–1486
Knopp EA, Cha S, Johnson G et al (1999) Glial neoplasms: dynamic contrast-enhanced T2*-weighted MR imaging. Radiology 211:791–798
Aprile I, Muti M, Principi M et al (2002) Magnetic Resonance comparative study between enhancement, rCBV and ACD in brain glioblastomas. Radiol Med (Torino) 104:87–91
Preul C, Kühn B, Lang EW et al (2003) Differentiation of cerebral tumors using multi-section echo planar MR perfusion imaging. Eur J Radiol 48:244–251
Principi M, Italiani M, Guiducci A et al (2003) Perfusion MRI in the evaluation of the relationship between tumour growth, necrosis and angiogenesis in glioblastomas and grade 1 meningiomas. Neuroradiology 45:205–211
Schmainda KM, Rand SD, Joseph AM et al (2004) Characterization of a first-pass gradient-echo spin-echo method to predict brain tumor grade and angiogenesis. AJNR Am J Neuroradiol 25:1524–1532
Law M, Yang S, Babb JS et al (2004) Comparison of cerebral blood volume and vascular permeability from dynamic susceptibility contrast-enhanced perfusion MR imaging with glioma grade. AJNR Am J Neuroradiol 25:746–755
Bulakbasi N, Kocaoglu M, Farzaliyev A et al (2005) Assessment of diagnostic accuracy of perfusion MR imaging in primary and metastatic solitary malignant brain tumors. AJNR Am J Neuroradiol 26:2187–2199
Boxerman JL, Schmainda KM, Weisskoff RM (2006) Relative cerebral blood volume maps corrected for contrast agent extravasation significantly correlate with glioma tumor grade, whereas uncorrected maps do not. AJNR Am J Neuroradiol 27:859–867
Hakyemez B, Erdogan C, Bolca N et al (2006) Evaluation of different cerebral mass lesions by perfusion-weighted MR imaging. J Magn Reson Imaging 24:817–824
Leon SP, Folkerth RD, Black PM (1996) Microvessel density is a prognostic indicator for patients with astroglial brain tumors. Cancer 77: 362–372
Lev MH, Ozsunar Y, Henson JW et al (2004) Glial tumor grading and outcome prediction using dynamic spin-echo MR susceptibility mapping compared with conventional contrast-enhanced MR: confounding effect of elevated rCBV of oligodendrogliomas. AJNR Am J Neuroradiol 25:214–221
Scarabino T, Giannatempo GM, Nemore F et al (2003) 3.0 Tesla Magnetic Resonance. Part 2: morphological and functional brain. Radiol Med (Torino) 105:150–161
DeLano MC, Fisher C (2006) 3T MR imaging of the brain. Magn Reson Imaging Clin N Am 14:77–88
Scarabino T, Giannatempo GM, Popolizio T et al (2007) 3.0 T functional brain imaging: a five-year experience. Radiol Med (Torino) (in press)
Frayne R, Goodyear BG, Dickhoff P et al (2003) Magnetic resonance imaging at 3.0 Tesla: challenges and advantages in clinical neurological imaging. Invest Radiol 38:385–402
Scarabino T, Maiorana A, Nemore F et al (2003) 3.0 Tesla Magnetic Resonance. Part I: safety problems related to installation and use. Radiol Med (Torino) 105:141–149
Uematsu H, Maeda M (2006) Doubleecho perfusion-weighted MR imaging: basic concepts and application in brain tumors for the assessment of tumor blood volume and vascular permeability. Eur Radiol 16:180–186
Keston P, Murray AD, Jackson A (2003) Cerebral perfusion imaging using contrast-enhanced MRI. Clin Radiol 58:505–513
Sorensen AG, Reimer P (2000) Cerebral MR perfusion imaging: principles and current applications. Georg Thieme Verlag, Stuttgart, Germany
Manka C, Träber F, Gieseke J et al (2005) Three-dimensional dynamic susceptibility-weighted perfusion MR imaging at 3.0 T: feasibility and contrast agent dose. Radiology 234:869–877
Strugar JG, Criscuolo GR, Rothbart D, Harrington WN (1995) Vascular endothelial growth/permeability factor expression in human glioma specimens: correlation with vasogenic brain edema and tumor-associated cysts. J Neurosurg 83:682–689
Chiang IC, Kuo Y-T, Lu C-Y et al (2004) Distinction between high-grade gliomas and solitary metastases using peritumoral 3-T magnetic resonance spectroscopy, diffusion, and perfusion imagings. Neuroradiology 46:619–627
Law M, Cha S, Knopp EA et al (2002) High-grade gliomas and solitary metastases: differentiation by using perfusion and proton spectroscopic MR imaging. Radiology 222:715–721
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Di Costanzo, A., Pollice, S., Trojsi, F. et al. Role of perfusion-weighted imaging at 3 Tesla in the assessment of malignancy of cerebral gliomas. Radiol med 113, 134–143 (2008). https://doi.org/10.1007/s11547-008-0232-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11547-008-0232-2