Abstract
As China experiences a rapidly aging population, the prevalence of Chinese older adults suffering from mental health issues also increases. Because cigarette smoking and alcohol consumption are two major public health concerns in China, we examined smoking and alcohol consumption status with loneliness, depression, and loss of interest among Chinese older adults. Panel data were extracted from the Chinese Longitudinal Healthy Longevity Survey, and older adults were selected as the final study sample (age ≥ 65) from two different time points (the 2011–2012 and 2014 waves). We analyzed Chinese older men and women with the adoption of panel logistic regression models to study mental health measurements of loneliness, depression, and loss of interest. Among males, compared with non-alcohol users, former alcohol users had higher odds of reporting depression (adjusted odds ratio [AOR] = 1.39, 95% CI: 1.01, 1.91; p < 0.05), while current alcohol users did not. Current and former smoking statuses were positively associated with depression (all p < 0.05). However, only current smoking status was positively associated with loss of interest (p < 0.05). Among females, former alcohol consumption was positively associated with loneliness, and current alcohol consumption was positively associated with depression. Health practitioners should evaluate the roles of smoking and alcohol consumption on Chinese older adults’ mental health measurements in the long term.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Background of Smoking and Alcohol Consumption in China
Cigarette smoking and alcohol consumption are two major public health issues around the world, including in China. The top three behavioral risk factors creating disease burden in China are poor diet, smoking, and alcohol consumption (Li et al., 2015). In 2010, an estimated 1740 billion cigarettes were smoked by 318 million Chinese smokers (Liu et al., 2017). Social influences appear to be a significant factor to smoking in China, such as shown by a study by Ma and colleagues (2013), which found that having friends and grandparents who smoked was associated with current smoking status (Ma et al., 2013). On the other hand, alcohol consumption is an especially major problem among Chinese men, who have been found to have 13 times the consumption rate of Chinese women (Gu & Ming, 2020).
Both smoking and alcohol consumption, not unexpectedly, have had negative effects on the Chinese population. A study of Chinese men between the ages of 40 and 79 found strong associations between alcohol drinking with mortality from stroke, cirrhosis, esophageal cancer, and accidents (Yang et al, 2012). Furthermore, cigarette use primarily manifests its negative impact in the form of lung cancer, attributing to over 20% of total cancer mortality in China in 2015 (Parascandola & Xiao, 2019). Unfortunately, limited resources (such as treatment centers and programs) are in place for the management of alcohol-related disorders (Tang et al., 2012). There seems to be somewhat of a stronger effort by the Chinese government in terms of smoking cessation resources.
In addition, both smoking and alcohol consumption have been normalized for generations in China. It is very common to observe alcohol use as a way to strengthen social relationships with others, especially during business and social activities (Lee et al., 2020). Alcohol consumption is a way to preserve “face” and “status” among friends and colleagues (Mou & Lin, 2020). This is also a popular cultural behavior in many Chinese-speaking territories and nations such as Taiwan, Hong-Kong, Singapore, Malaysia, and others. In fact, the Chinese tend to frequently use cigarette and alcohol-related products as gifts (Wang et al., 2014; Xu et al., 2016). Under such circumstance, the tradition of smoking and alcohol consumption may be considered a normalized behavior in the Chinese society.
Initiation age of smoking and alcohol consumption is another factor to consider in China. The legal age for smoking and alcohol consumption is 18 years old in China, but it is widely believed that many people used these two substances long before the legal age. For example, the average age of smoking initiation is about 21 years old among Chinese smokers, but many smokers may have started smoking before this age (Li et al., 2016; Zhang et al., 2013). The laissez-faire policy for cigarette and alcohol sales in the last few decades, in addition of the normalized culture of smoking and alcohol consumption, may have led to early smoking and alcohol consumption initiation in China.
Smoking, Alcohol Consumption, and Mental Health
It has been found that among individuals with alcohol use disorder, depressive disorders are the most common psychiatric disorders (Grant et al., 2004). This co-occurrence is of significance to society; for example, lower remission likelihood has been observed in people with current substance-induced major depressive disorder (MDD) than those without baseline MDD (Hasin et al., 2002). Similarly, much has been done in the past to examine the relationship between smoking and depression as well. Mood problems have been found as both a trigger and a barrier to smoking cessation (Clancy et al., 2013).
Loss of interest, or anhedonia, is one of the criteria commonly used in the USA for depression screening and is in fact a criterion used for the diagnosis of MDD. In addition, Beutel et al. (2017) has reported an association between loneliness and depression, and lonely study participants smoked more. It is evident that many of the aforementioned issues seem to have some relationship between one another.
China, plagued by a low fertility rate, is experiencing a rapidly aging population and anticipated to have an increase in median age by 8.47 years between 2019 and 2044 (Chen et al., 2019). In China, a study of primary care clinic patients found that while prevalent, depressive disorders are not well recognized in Chinese older adults (Zhong et al., 2020). Nonetheless, self-reported loneliness has been associated with, over the subsequent 3-year period, increasing dying risk (Luo & Waite, 2014). In addition, loneliness or social isolation is a primary risk factor for physical and mental health issues among older adults (Ong et al., 2016).
As the population continues to age in the upcoming years, there is concern that mental health problems will continue to put increasing burden on the elderly Chinese population, and in a society where history and social factors play a role in smoking and drinking behaviors (Lee et al., 2020). We intend to examine such behaviors with mental health, in particular loneliness, loss of interest, and depression, to contribute to any ongoing and future efforts and policy decisions aimed at improving the well-being of Chinese older adults. We believe that mental health lies on a spectrum, and frequent fluctuations can occur. Therefore, it is important to not look solely at depression, but also loneliness and loss of interest, which are likely precursors to or factors that interact with depressive symptoms. Examining how smoking and alcohol use relate to such qualities could potentially help prevent negative downstream effects on mental health.
Materials and Methods
Study Sample
Two waves of longitudinal data from the Chinese Longitudinal Healthy Longevity Survey (CLHLS; 2011–2012 and 2014) were extracted for this present research. CLHLS is an internationally collaborative dataset and a currently ongoing open cohort, established by researchers and investigators from the Duke University, Peking University, and others. The CLHLS dataset, aiming to study the health and longevity of Chinese older adults, happens to be the first longitudinal dataset targeting the oldest-old in a developing country. Study participants of CLHLS are mostly centenarians, nonagenarians, octogenarians, and younger older adults (between 65 and 79 years of age). The dataset also includes some middle-aged adults. To study Chinese older adults’ health and longevity, the CLHLS dataset covers a wide array of topics, such as family relationship, social welfare, healthcare utilization, mental health, cognitive function, chronic disease, and other lifestyle-related measurements. The CLHLS investigators conducted face-to-face interviews for data collection and obtained informed consent from all study participants. The random cluster sampling includes participants from 23 mega cities and provinces in China. Other information about this dataset can be found elsewhere (Zeng, 2012). Because we only relied on a publicly available and de-identified secondary dataset, this research effort did not fall into the category of human subject research. The research ethics committees of the Peking and Duke Universities approved the CLHLS study and design (IRB00001052-13,074).
Measurements
The outcomes included a total of three self-reported and dichotomous variables: loneliness (no/yes), depression (no/yes), and loss of interest (no/yes).
The major predictors in the analyses were smoking and alcohol consumption. In each variable, the categories included three types of consumption status: none, former, and current. Older adults were asked if they currently use alcohol or smoke, or had used alcohol or smoked in the past, separately. Those who had never used alcohol or smoked were grouped as none. The categories were reclassified by the authors of this present research.
We selected a set of sociodemographic variables as covariates in our regression models: age (65–80, 81–95, above 95; measured in years), formal education (none, 1–5, 6–10, 11 and above; measured in years), marital status (not married (including those who were never married, divorced, or widowed), married), living arrangement (with household members, others (alone or in an institution)), types of residence (rural, urban), and income (less than 6000, 6001–20,000, 20,001–40,000, above 40,000; measured in Renminbi (RMB), the Chinese currency).
Furthermore, in order to examine the possible correlates with mental health outcomes, we also selected a set of health and wellbeing measurements: exercise status (no, yes), quality of sleep (others (including those who reported bad and neutral), good), life satisfaction (others (including those who reported bad and neutral), good), and chronic conditions requiring inpatient treatments in the past two years (none, yes).
Statistical Analysis
For statistical analysis, we employed panel logistic regression models to examine older adults’ loneliness, depression, and loss of interest, given that our outcomes were all dichotomous. Compared with the cross-sectional study design, which only provides a snapshot of the associations, the major advantage of adopting a panel analysis is that the approach enables the researchers to examine the potential variances in mental health measurements in different time points by considering intra-individual variability (Hsiao, 2007). In addition, panel analysis may help strengthen the capacity to consider the complexity of human behavior (Hsiao, 2007) and other chronic conditions like mental health issues. Because of the potential gender disparities of woman being more likely to have mental health problems than man (Riecher-Rössler, 2017; Yu, 2018), we performed gender-stratified models to examine the potential gender differences between older men and women. In each sex, model 1 examined loneliness, model 2 examined depression, and model 3 examined loss of interest.
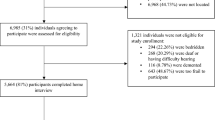
To conduct panel analysis, we selected older adults who fully answered all questions of interest in two waves. We removed missing information or participants who only responded to only one of the surveys. Next, we merged the two waves together with complete responses from study participants. In the final study sample, there were a total of 3098 and 2776 observations from male and female participants, respectively (total n = 5874). Each older adult provided two sets of complete responses, with 1549 males and 1388 females participating in the survey. For regressions, we reported adjusted odds ratio (AOR = 1.00 is the reference level) and 95% confidence interval (95% CI) as main results. Our statistical tests were two-tailed with a level of significance of 0.05 (p < 0.05). We used the publicly available statistical package R (version 3.6.1) for all statistical analyses. Package “GLMMadaptive” was used for panel data analysis (Rizopoulos, 2022).
Results
Sample Characteristics
Table 1 shows the sample characteristics of observations from male participants. In the overall sample, approximately 39.1%, 24.7%, and 36.2% were non-smokers, former smokers, and current smokers, respectively. For alcohol use status, around 50.1% were non-users, 19.5% were former users, and 30.4% were current users. Among male study participants, more than 90% of them were under 95 years of age. Most older males received some level of formal education (1 years or above), were married, lived with household members, resided in urban communities, and had lower level of income (lower than 20,000 RMB per year). In terms of health-related measurements among older males, approximately 42.7% exercised, 68.4% reported good sleep quality, 65.9% had good life satisfaction, and 78.2% did not have any chronic conditions that required inpatient treatments in the past 2 years.
Table 2 shows the sample characteristics of observations from female participants. In the overall sample, approximately 89.3%, 4.9%, and 5.8% were non-smokers, former smokers, and current smokers, respectively. For alcohol consumption, nearly 87.2% were non-users, 5.0% were former users, and 7.8% were current users. Among female study participants, about 13.2% were above 95 years of age, which was higher than the male participants. Most older females received no formal education, were not married, lived with household members, resided in rural communities, and had lower level of income (lower than 20,000 RMB per year). In terms of health-related measurements among older females, approximately 35.3% exercised, 59.7% reported good sleep quality, 66.7% had good life satisfaction, and 77.7% did not have any chronic conditions that required inpatient treatments in the past 2 years.
Tables 1 and 2 also provided comprehensive descriptive statistics categorized by loneliness, depression, and loss of interest among older males and females, respectively.
Associations of Smoking and Alcohol Consumption with Loneliness, Depression, and Loss of Interest Among Chinese Older Males and Females
Table 3 shows the associations of smoking and alcohol use behaviors with loneliness, depression, and loss of interest among male and female participants. First, we discussed the study results from male participants. In the first model, neither smoking nor alcohol consumption was associated with loneliness. In the second model regarding depression, former and current smokers had higher odds of reporting depression (all p < 0.05), compared with older adults who did not smoke at all. Former alcohol consumption also was positively associated with depression. For loss of interest, current smoking status was positively associated with loss of interest (AOR = 1.51, 95% CI: 1.09, 2.09; p < 0.05).
Next, we showed the study results from female participants. Among females, we only observed that participants who reported current alcohol consumption had higher odds of reporting depression (AOR = 1.87, 95% CI: 1.23, 2.83; p < 0.01), compared with female participants who did not consume alcohol at all. Former alcohol consumption was positively associated with loneliness (p < 0.05). No smoking-related category was associated with mental health measurements among female participants.
Discussion
We used panel logistic regression models, controlled for sociodemographic and health related variables, to examine the associations of smoking and alcohol consumption status with loneliness, depression, and loss of interest among Chinese older males and females. With the adoption of panel data, the capacity for accounting the complexity of human behavior and intra-individual variability may be strengthened in two difference time points (Hsiao, 2007). The use of a large study sample, such as CLHLS, was able to increase the generalizability of our study findings.
It was found that in older Chinese males, being a current smoker was positively associated with loss of interest between the two survey waves, but not loneliness. We suspected that such an association exists due to the sense of control from choosing to smoke voluntarily, meaning that when someone begins experiencing loss of interest, they start engaging in activities to feel rewarding and take control again, such as smoking behavior.
A study by Fidler and West (Fidler & West, 2009) found that among a general population of smokers, nicotine has the perceived ability to manage mood, such as through stress relief. Such perception by smokers could at least partly explain why individuals who reported loss of interest were current smokers. This also may imply to our findings in depression, given that we observed that current smoking status was associated with higher odds of depression. This is different from current alcohol consumption, given that alcohol is a type of depressant, which can break the balance in human body and, eventually, can alter an individual’s neuropsychological functioning (Hilliard, 2021). But smoking a cigarette does not usually reveal such effects immediately.
However, our study did not demonstrate an association between loneliness and alcohol consumption among older males. It might be possible that male study participants were reluctant to admit the feeling of loneliness, again due to the rich social transitions of the Chinese society, and admitting to loneliness potentially being perceived a sign of weakness or inferiority. In fact, alcohol consumption is often considered one of the methods to show courage and strength among friends and colleagues in China (Mou & Lin, 2020). This context is especially common among males; men could lose “face” among his peers if he refuses a drink. This social phenomenon may help interpret the insignificant finding between loneliness and alcohol consumption among Chinese males. Nevertheless, it also has been observed that loneliness was associated with decreased alcohol consumption frequency among middle-aged and older adult drinkers in the USA (Canham et al., 2016). This may indicate a cultural gap between the east and the west. Therefore, further research efforts are warranted to address these knowledge gaps, and potential cultural disparities between the eastern and western culture also need to be examined.
Among older females, participants who reported current alcohol consumption had higher odds of reporting depression, compared with those who did not use alcohol at all. The Chinese culture has a deep history of social drinking, and a study of individuals in Wuhan City, China, found that having friends and colleagues with deviant alcohol consumption was a risk factor for alcohol abuse (Zhang et al., 2004). It has been found previously that weak connectedness with friends was associated with depressive symptoms (Ge et al., 2017). This may indicate the association between current alcohol consumption and depression that we observed in this present research. Unfortunately, these discussions were only based on previous research findings and speculations because we did not have information regarding social drinking from the CLHLS dataset. Interestingly, such association between current alcohol consumption and depression was not observed among older males. Further research efforts should continue to examine the potential gender disparities on alcohol consumption and depression.
There are several policy implications for our findings. First of all, policymakers can place more emphasis on helping elderly Chinese people engage in healthy and enriching hobbies such as sports and reading, maybe via community-based centers/events, since it is possible that having hobbies may help them feel less of a need to continue smoking cigarettes, especially Chinese males. In regard to former alcohol consumption and development of depression among the men, we suggest that alcohol cessation programs incorporate mental health and wellness into the programs, so those who may seek help via these programs can hopefully recognize and prevent the symptoms of depression and seek help for such issues if necessary. Among the Chinese elderly women, a potential policy implication for the observation that current alcohol drinkers had higher odds of reporting depression would be education on healthy activities and gatherings that do not involve the use of alcohol; moreover, training peer educators who can ultimately educate people in their social circle about the harmful effects of alcohol on mental health may also be beneficial.
Adjusting cultural norms may be another approach. Because of the normalized culture, previous studies have observed some counterintuitive study results related to sleep. In Gu et al. (2010) and Lee et al. (2021), despite two very different analytical approaches in both studies, they all observed that smoking and alcohol consumption were associated with better sleep quality. In particular, Lee et al. (2021) also mentioned that the cultural norms of smoking and alcohol consumption may be a factor to affect older adults’ well-being and sleep. Therefore, providing educational protocols for adjusting the culture of smoking and alcohol consumption might be a key for the next generation and, eventually, reduce the potential negative consequences related to mental health. More research should follow up the role of cultural norms and perception of smoking and alcohol consumption.
A few study limitations exist. First, because we only used the 2011–2012 and 2014 waves of CLHLS for this research, we were unable to examine smoking and alcohol consumption since the outbreak of coronavirus disease (COVID-19). The situation of substance use behavior and mental health and/or wellbeing among Chinese older adults may have changed after the outbreak. Second, we only applied two waves of longitudinal data from CLHLS for this research. This is mainly because some questions regarding mental health measurements were inconsistent, or some questions have been redefined. Therefore, we chose to adopt only the 2011–2012 and the 2014 waves in order to capture three important mental health-related measurements in a single research effort: loneliness, depression, and loss of interest. Third, we only looked into smoking and alcohol consumption statuses in this present research. Responses regarding the amount of consumption for each substance had many inconsistencies and missing values in between the study periods. With the inclusion of the amount of consumption, we might need to excessively impute data, making the study estimates less accurate.
Next, we should note that the proportion of older women smoking or using alcohol was smaller than for older men. For example, among older women, only 5.3% smoked. With smaller sample sizes among older women, the statistical power may not be as strong. We should be careful about making a conclusive claim for Chinese older women. Further research efforts should continue to investigate this topic of interest with larger sample, in which case the statistical power and generalizability may increase. Last but not least, as we relied on a secondary dataset, self-reported bias might occur. However, this is a common study limitation in most survey-based research. A previous population-based study already has shown that self-reported health measurements were consistent to reflect individuals’ objective health conditions (Wu et al., 2013). The self-reported mental health measurements in this research may provide sufficient information to describe Chinese older adults' objective mental health. Therefore, this limitation should not be a primary concern for this research.
Conclusion
Despite these limitations, this present study adds to the body of literature to examine the associations of smoking and alcohol consumption with mental health issues among Chinese older adults such as loneliness, depression, and loss of interest, with the adoption of the panel logistic regression models. We carried out a secondary data analysis to examine this topic of interest by using a secondary dataset, CLHLS. Some gender disparities were observed between older men and women. The general findings indicated that older men who were current smokers had higher odds of reporting depression and loss of interest. Older women who were current alcohol users had higher odds of reporting depression, compared with those who did not use alcohol at all, but this association was not observed in older men. Smoking-related categories were not associated with mental health outcomes among older females in this research. We suggest that, with available clinical data, more research should continue to examine this topic of interest. The long-term effects of smoking and alcohol consumption on developing mental health issues among Chinese older adults should be investigated further.
References
Canham, S. L., Mauro, P. M., Kaufmann, C. N., & Sixsmith, A. (2016). Association of alcohol use and loneliness frequency among middle-aged and older adult drinkers. Journal of Aging and Health, 28(2), 267–284. https://doi.org/10.1177/0898264315589579
Chen, R., Xu, P., Song, P., Wang, M., & He, J. (2019). China has faster pace than Japan in population aging in next 25 years. Bioscience Trends, 13(4), 287–291. https://doi.org/10.5582/bst.2019.01213
Clancy, N., Zwar, N., & Richmond, R. (2013). Depression, smoking and smoking cessation: A qualitative study. Family Practice, 30(5), 587–592. https://doi.org/10.1093/fampra/cmt032
Beutel, M. E., Klein, E. M., Brähler, E., Reiner, I., Jünger, C., Michal, M., Wiltink, J., Wild, P. S., Münzel, T., Lackner, K. J., & Tibubos, A. N. (2017). Loneliness in the general population: Prevalence, determinants and relations to mental health. BMC Psychiatry, 17(1), 97. https://doi.org/10.1186/s12888-017-1262-x
Fidler, J. A., & West, R. (2009). Self-perceived smoking motives and their correlates in a general population sample. Nicotine & Tobacco Research, 11(10), 1182–1188. https://doi.org/10.1093/ntr/ntp120
Ge, L., Yap, C. W., Ong, R., & Heng, B. H. (2017). Social isolation, loneliness and their relationships with depressive symptoms: A population-based study. PLoS ONE, 12(8), e0182145. https://doi.org/10.1371/journal.pone.0182145
Grant, B. F., Stinson, F. S., Dawson, D. A., Chou, S. P., Dufour, M. C., Compton, W., Pickering, R. P., & Kaplan, K. (2004). Prevalence and co-occurrence of substance use disorders and independent mood and anxiety disorders: Results from the National Epidemiologic Survey on Alcohol and Related Conditions. Archives of General Psychiatry, 61(8), 807–816. https://doi.org/10.1001/archpsyc.61.8.807
Gu, D., Sautter, J., Pipkin, R., & Zeng, Y. (2010). Sociodemographic and health correlates of sleep quality and duration among very old Chinese. Sleep, 33(5), 601–610. https://doi.org/10.1093/sleep/33.5.601
Gu, J., & Ming, X. (2020). Perceived social discrimination, socioeconomic status, and alcohol consumption among Chinese adults: A nationally representative study. International Journal of Environmental Research and Public Health, 17(17), 6043. https://doi.org/10.3390/ijerph17176043
Hasin, D., Liu, X., Nunes, E., McCloud, S., Samet, S., & Endicott, J. (2002). Effects of major depression on remission and relapse of substance dependence. Archives of General Psychiatry, 59(4), 375–380. https://doi.org/10.1001/archpsyc.59.4.375
Hilliard, J. (2021). Is alcohol a depressant? Retrieved from https://www.addictioncenter.com/alcohol/is-alcohol-a-depressant/. Accessed 30 Aug 2021
Hsiao, C. (2007). Panel data analysis—Advantages and challenges. TEST, 16(1), 1–22.
Lee, Y. H., Chang, Y. C., Liu, C. T., & Shelley, M. (2020). Correlates of alcohol consumption and alcohol dependence among older adults in contemporary China: Results from the Chinese Longitudinal Healthy Longevity Survey. Journal of Ethnicity in Substance Abuse, 19(1), 70–85. https://doi.org/10.1080/15332640.2018.1456388
Lee, Y. H., Wu, Y. H., Shelley, M., Arndt, S., & Chang, Y. C. (2021). The effects of cigarette smoking, alcohol consumption, and use of both cigarettes and alcohol on Chinese older adults’ sleep: Results from a longitudinal study. International Journal of Mental Health and Addiction (online First). https://doi.org/10.1007/s11469-021-00697-7
Li, S., Meng, L., Chiolero, A., Ma, C., & Xi, B. (2016). Trends in smoking prevalence and attributable mortality in China, 1991–2011. Preventive Medicine, 93, 82–87. https://doi.org/10.1016/j.ypmed.2016.09.027
Li, Y., Liu, S., Wang, L., & Zhou, M. (2015). Burden of disease attributable to main behavioral risk factor of chronic disease inactivity in China, 1990 and 2010. Zhonghua Yu Fang Yi Xue Za Zhi [chinese Journal of Preventive Medicine], 49(4), 303–308.
Liu, S., Zhang, M., Yang, L., Li, Y., Wang, L., Huang, Z., Wang, L., Chen, Z., & Zhou, M. (2017). Prevalence and patterns of tobacco smoking among Chinese adult men and women: Findings of the 2010 national smoking survey. Journal of Epidemiology and Community Health, 71(2), 154–161. https://doi.org/10.1136/jech-2016-207805
Luo, Y., & Waite, L. J. (2014). Loneliness and mortality among older adults in China. The Journals of Gerontology. Series B, Psychological Sciences and Social Sciences, 69(4), 633–645. https://doi.org/10.1093/geronb/gbu007
Ma, G. X., Shive, S. E., Ma, X. S., Toubbeh, J. I., Tan, Y., Lan, Y. J., Zhai, C. K., & Pei, X. (2013). Social influences on cigarette smoking among Mainland Chinese and Chinese Americans: A comparative study. American Journal of Health Studies, 28(1), 12–20.
Mou, Y., & Lin, C. A. (2020). Consuming alcohol to prepare for adulthood: An event history analysis of the onset of alcohol use among Chinese college students. SAGE Open, 10(3), 1–11. https://doi.org/10.1177/2158244020939911
Ong, A. D., Uchino, B. N., & Wethington, E. (2016). Loneliness and health in older adults: A mini-review and synthesis. Gerontology, 62(4), 443–449. https://doi.org/10.1159/000441651
Parascandola, M., & Xiao, L. (2019). Tobacco and the lung cancer epidemic in China. Translational Lung Cancer Research, 8(Suppl 1), S21–S30. https://doi.org/10.21037/tlcr.2019.03.12
Riecher-Rössler, A. (2017). Sex and gender differences in mental disorders. The Lancet, Psychiatry, 4(1), 8–9. https://doi.org/10.1016/S2215-0366(16)30348-0
Rizopoulos, D. (2022). Package “GLMMadaptive.” Retrieved from https://cran.r-project.org/web/packages/GLMMadaptive/GLMMadaptive.pdf. Accessed June 2022
Tang, Y. L., Hao, W., & Leggio, L. (2012). Treatments for alcohol-related disorders in China: A developing story. Alcohol and Alcoholism (oxford, Oxfordshire), 47(5), 563–570. https://doi.org/10.1093/alcalc/ags066
Wang, J., Li, C., Jia, C., Liu, Y., Liu, J., Yan, X., & Fang, Y. (2014). Smoking, smoking cessation and tobacco control in rural China: A qualitative study in Shandong Province. BMC Public Health, 14, 916.
Wu, S., Wang, R., Zhao, Y., Ma, X., Wu, M., Yan, X., & He, J. (2013). The relationship between self-rated health and objective health status: A population-based study. BMC Public Health, 13, 320. https://doi.org/10.1186/1471-2458-13-320
Xu, Y., Xu, S., Wu, Q., & Guo, Y. (2016). Association between secondhand smoke exposure at home and cigarette gifting and sharing in Zhejiang, China: A repeat cross-sectional study. British Medical Journal Open, 6, e010058.
Yang, L., Zhou, M., Sherliker, P., Cai, Y., Peto, R., Wang, L., Millwood, I., Smith, M., Hu, Y., Yang, G., & Chen, Z. (2012). Alcohol drinking and overall and cause-specific mortality in China: Nationally representative prospective study of 220,000 men with 15 years of follow-up. International Journal of Epidemiology, 41(4), 1101–1113. https://doi.org/10.1093/ije/dys075
Yu, S. (2018). Uncovering the hidden impacts of inequality on mental health: A global study. Translational Psychiatry, 8(1), 98. https://doi.org/10.1038/s41398-018-0148-0
Zeng, Y. (2012). Towards deeper research and better policy for healthy aging –Using the unique data of Chinese Longitudinal Healthy Longevity Survey. China Economic Journal, 5(2–3), 131–149. https://doi.org/10.1080/17538963.2013.764677
Zhang, J., Wang, J., Lu, Y., Qiu, X., & Fang, Y. (2004). Alcohol abuse in a metropolitan city in China: A study of the prevalence and risk factors. Addiction (abingdon, England), 99(9), 1103–1110. https://doi.org/10.1111/j.1360-0443.2004.00799.x
Zhang, L., Cui, Y., Wang, C., Jiang, Y., & Yang, L. (2013). Survey on status of smoking, passive smoking and quitting smoking in rural areas of the midwestern provinces in China. Zhonghua Liu Xing Bing Xue Za Zhi, 34(2), 137–139.
Zhong, B. L., Ruan, Y. F., Xu, Y. M., Chen, W. C., & Liu, L. F. (2020). Prevalence and recognition of depressive disorders among Chinese older adults receiving primary care: A multi-center cross-sectional study. Journal of Affective Disorders, 260, 26–31. https://doi.org/10.1016/j.jad.2019.09.011
Acknowledgements
We sincerely thank Ms. Ya-Rou Chen with her help for literature review. Data used for this research were provided by the “Chinese Longitudinal Healthy Longevity Survey” (CLHLS) managed by the Center for Healthy Aging and Development Studies, Peking University. CLHLS is supported by funds from the US National Institutes on Aging (NIA), China Natural Science Foundation, China Social Science Foundation, and United Nations Population Fund. We thank research participants and researchers for their efforts in collecting the CLHLS data.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical Approval
The research ethics committees of the Duke University and Peking University approved the CLHLS study and design (IRB00001052-13074). All participants provided informed consent to the data investigators. Because this study relied on a secondary data analysis, this research did not fall into the category of human subjects research. No experimental interventions were conducted.
Competing Interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Chang, YC., Lee, YH., Chiang, T. et al. Associations of Smoking and Alcohol Consumption with Loneliness, Depression, and Loss of Interest Among Chinese Older Males and Females. Int J Ment Health Addiction 22, 1047–1062 (2024). https://doi.org/10.1007/s11469-022-00912-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11469-022-00912-z