Abstract
Purpose
Significant disturbances of the classical amphetamines on the dopamine (DA) and serotonin (5-HT) systems have been previously reported. However, few studies have been conducted on the effects of new psychoactive phenethylamines on the release of DA and 5-HT. In the present study, the effects of new psychoactive phenethylamines with a variety of aromatic ring substitutions (5-API, 3-FMA, 5-MAPB, and DMMA) on the release of DA and 5-HT were investigated.
Methods
Changes of DA, 5-HT and their metabolites in brain microdialysates from rats following exposure to the drugs were examined using a validated liquid chromatography–tandem mass spectrometry method. Their potencies of DA and 5-HT uptake inhibition as well as dopamine transporter (DAT) and serotonin transporter (SERT) binding were also determined.
Results
With the exception of DMMA, the drugs markedly affected the extracellular concentration of DA, 5-HT and/or their metabolites in rats and acted as potent inhibitors for DAT and/or SERT. Especially, 5-API potently induced the nonselective release of both DA and 5-HT, which was strongly correlated with a high degree of uptake inhibition and binding affinity to DAT and SERT. The 3-FMA, a methamphetamine analog with a halogen-substituted benzene, induced greater 5-HT release than DA.
Conclusions
We found that new psychoactive phenethylamines, with a variety of aromatic ring substitutions, affected the extracellular levels of DA, 5-HT, and/or their metabolites in the nucleus accumbens of rats to varying degrees and in different ways. The current results may assist further research into monoamine neurotransmitter-related mechanisms of new psychoactive phenethylamines.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The dramatic increase and rapid and transient popularity of new psychoactive substances (NPS) represent a burden not only to regulatory authorities, but also to toxicologists and physicians. NPS are considered to produce addictive or psychedelic effects similar to those of traditional drugs, but little is known about their pharmacology and toxicology. Moreover, their unexpected toxic effects, including neuropsychiatric and cardiovascular toxicities, are public health concerns [1,2,3]. These NPS can be divided into six major classes, synthetic cannabinoids, synthetic cathinones, piperazines, phenethylamines, tryptamines, and piperidines. The traditional phenethylamines, such as amphetamine, methamphetamine (METH), and 3,4-methylenedioxymethamphetamine (MDMA), show potent stimulatory properties and are the largest family, consisting of structures with extended side chains, amino group substitutions, or aromatic ring substitution of phenethylamine. These structural modifications may alter the stimulant properties or produce additional psychoactive properties [4].
Dopamine (DA) and serotonin (5-hydroxytryptamine, 5-HT) are the major monoamine neurotransmitters of the central nervous system and play an important role in drug abuse and addiction, which affect the reward circuits [5, 6]. DA and 5-HT are synthesized from tyrosine and tryptophan, respectively, in the nerve terminals and are released by exocytosis. The released DA is bound to the postsynaptic D1 and D2 receptors for signal transmission or to the presynaptic DA transporter (DAT) for reuptake. After uptake, the DA is recycled or metabolized to 3,4-dihydroxyphenylacetic acid (DOPAC) and further to homovanillic acid (HVA) by monoamine oxidase (MAO) and catechol-O-methyltransferase (COMT) in pre- and postsynaptic cells. HVA is the final metabolic product of DA in humans. Similarly, 5-HT is bound to the 5-HT receptors for its effective response or to the 5-HT transporter (SERT) for reuptake. 5-HT is predominantly metabolized to 5-hydroxyindoleacetic acid (5-HIAA) in neurons. Therefore, the reuptake or metabolism of DA or 5-HT is critical to maintain their concentration in the synaptic cleft [6].
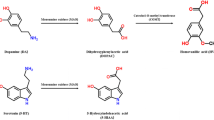
The induction of significant disturbances by classical phenethylamines, such as METH and MDMA, were previously reported on the DA and 5-HT systems. METH and MDMA cause the release of DA and 5-HT, and interact with both DAT and SERT, though MDMA is more serotonergic [7, 8]. However, few studies have been conducted on the effects of new psychoactive phenethylamines on the release of DA and 5-HT [9]. In the present study, the in vivo measurements of DA, 5-HT and their metabolites in rat nucleus accumbens, in addition to in vitro assays for DAT and SERT inhibition and binding, were conducted to investigate the effects of new psychoactive phenethylamines with a variety of aromatic ring substitutions [1-(1H-indol-5-yl)propan-2-amine (5-API or 5-IT), 1-(3-fluorophenyl)-N-methylpropan-2-amine (3-FMA), 1-(benzofuran-5-yl)-N-methylpropan-2-amine (5-MAPB), 2-(3,4-dimethoxyphenyl)-N-methylpropanamine (DMMA); Table 1] on the release of DA and 5-HT.
Materials and methods
Drugs and reagents
The 5-API, 3-FMA, 5-MAPB and DMMA were synthesized as HCl salts and provided by Kyunghee University (Seoul, Republic of Korea). Their purities were not less than 96.5%. METH as an HCl salt, DA, DOPAC, HVA, 5-HT, 5-HIAA, DA-d4, DOPAC-d5, HVA-d5, 5-HIAA-d5, ascorbic acid, GBR12909, and venlafaxine were purchased from Sigma-Aldrich (St. Louis, MO, USA). The 5-HT-d4 was purchased from TLC PharmaChem (Vaughan, Ontario, Canada). 3H-Dopamine, 3H-serotonin, 3H-WIN35,428, and 3H-imipramine were obtained from PerkinElmer (Waltham, MA, USA). Acetonitrile and methanol (HPLC grade) were purchased from Fisher Scientific (Waltham, MA, USA) and Merck (Darmstadt, Germany), respectively. All other chemicals and solvents were of reagent grade.
Animals
Male Sprague–Dawley rats (Daehan Animal, Seoul, Republic of Korea), weighing 270–320 g, were used for in vivo microdialysis experiments. The rats were kept in the laboratory animal facility under a 12 h light/dark cycle. Food and water were freely available for the animals.
In vivo microdialysis experiments
In vivo microdialysis sampling was conducted in accordance with the method described in the previous study with minor modifications [10]. After the rats were intraperitoneally anesthetized by 50 mg/kg sodium pentobarbital, a microdialysis probe guide cannula (CMA 11; CMA Microdialysis AB, Kista, Sweden) was stereotaxically implanted into the brain. The rats were allowed to recover from surgery for 6 days. The microdialysis probe (membrane length, 2 mm; cut-off, 6 kDa; CMA Microdialysis AB) was inserted into the nucleus accumbens shell (AP+ 1.7 mm, ML+ 0.8 mm, from the bregma; DV − 6.0 mm, from the skull) through the guide cannula of unanesthetized rats, and the artificial cerebral spinal fluid (aCSF) was perfused at 1.5 μL/min by using a microinjection pump (CMA 100; CMA Microdialysis AB) for at least 2 h for stabilization. The aCSF (pH 7.4) was prepared as a mixture of 150 mM sodium chloride, 3.0 mM potassium chloride, 1.4 mM calcium chloride, and 0.8 mM magnesium chloride in 10 mM phosphate buffer (pH 7.4). Six baseline samples were collected every 20 min for 2 h. Subsequently, the drugs [METH, 3-FMA, 5-MAPB, and DMMA dissolved in saline, or 5-API dissolved in DMSO/TWEEN 80/saline (5:5:90, v/v/v)] were administered by intraperitoneal injection every hour with a gradually increasing dose (0.3, 1, and 3 mg/kg for METH, 5-API, 3-FMA and DMMA, and 0.1, 0.3 and 1 mg/kg for 5-MAPB), and microdialysate was collected at 20 min intervals. At the termination of experiments, all rats were killed for histological confirmation of microdialysis probe location. Animals were perfused with phosphate-buffered saline and then with 4% paraformaldehyde. Brains were removed, post-fixed in 4% paraformaldehyde and cryoprotected in 30% sucrose. The tissue was then cryosectioned into 30 μm-thick sections and stained with cresyl violet, and the location of microdialysate collections at nucleus accumbens was verified.
Twenty-five microliters of the microdialysates collected from each rat were mixed with 5 μL of the internal standard solution (a mixture solution of deuterated compounds) and analyzed by a fully validated liquid chromatography (LC)–tandem mass spectrometry (MS/MS) as described in our previous study, using a 1260 Infinity LC system and 6460 triple quadrupole MS/MS (Agilent Technologies, Santa Clara, CA, USA) coupled with a 1260 Infinity extra binary pump and degasser (Agilent Technologies) [11]. The XBridge BEH HILIC Sentry Guard Cartridge 130 Å (4.6 × 20 mm, 3.5 μm; Waters, Milford, MA, USA) and the Atlantis T3 column (2.1 × 100 mm, 3 μm; Waters) were employed as sample enrichment and separation columns, respectively. The mobile phases (A, 5 mM ammonium formate/0.1% formic acid in water; B, 0.1% formic acid in acetonitrile) were passed through both the enrichment and separation columns with the following gradient conditions: 0–1.0 min, 5% B; 1.0–6.5 min, 5–90% B; 6.5–7.5 min, 90% B; 7.5–7.6 min, 90–5% B; 7.6–11.5 min, 5% B. The MS/MS system was operated by using electrospray ionization in the polarity-switching mode (DA, 5-HT, and 5-HIAA, positive; DOPAC and HVA, negative). The MS/MS conditions were optimized as follows: drying gas temperature, 350 °C; drying gas flow, 10 L/min; nebulization pressure, 35 psi; capillary voltage, 4.5 kV; temperature of sheath gas, 250 °C; sheath gas flow, 5 L/min. Multiple reaction monitoring (Table 2) was used for quantification. Each analytical stock solution (1 mg/mL) was prepared in 1 mM ascorbic acid in a 1:1 mixture solution of water and methanol to prevent oxidation and stored at − 80 °C before analysis.
DA and 5-HT uptake inhibition assays
The conditions for the DA and 5-HT uptake inhibition assays were adapted from previous studies [12, 13]. Human embryonic kidney 293 (HEK-293) cells were subcultured in fetal bovine serum in 100 × 20 mm polystyrene dish (Corning, Corning, NY, USA) and incubated in a humidified 5% CO2 incubator (Sanyo Electric Biomedical, Osaka, Japan) at 37 °C for 48 h. When the cells reached 60–70% confluence, they were transfected with human DAT or human SERT (cDNA, 3 μg/100 mm dish; polyethyleneimine, 10 μL) and maintained in a humidified 5% CO2 incubator at 37 °C for 24 h. The prepared HEK-293 cells were seeded in 24-well plates (poly-l-lysine coated, clear, flat-bottomed, round well-shaped, volume 3.4 mL; Corning) and incubated for 24 h. The medium was removed and the cells were washed once with 200 μL of uptake buffer/well prior to the addition of 180 μL of uptake buffer (5 mM Tris base, 7.5 mM HEPES, 120 mM NaCl, 5.4 mM KCl, 1.2 mM CaCl2, 1.2 mM MgSO4, 1 mM ascorbic acid, and 5 mM glucose; pH 7.1) to each well, which was followed by the addition of drugs dissolved in 20 μL uptake buffer. The 24-well plates were incubated at 37 °C in a slide warmer (Fisher, Pittsburgh, PA, USA) for 15–20 min. Then, 100 μL of the radiolabeled 60 nM 3H-dopamine or 60 nM 3H-serotonin per well was added to give a final concentration of 20 nM/well and incubated for approximately 5 min at 37 °C by using the slide warmer. The prepared cells were washed three times with ice-cold uptake buffer (200 μL/well). The cells were lysed by the addition of 0.3 mL of 1% sodium dodecyl sulfate per well and agitated in a shaker (KMC-1205S; Vision Scientific, Daejeon, South Korea) for 2 h. Radioactivity was measured by using a Wallac 1450 MicroBeta® TriLux liquid scintillation counter (PerkinElmer). GBR12909 and venlafaxine were used as the standard reuptake inhibitors for DAT and SERT, respectively.
DAT and SERT binding assays
The DAT binding assay was performed using 20 nM 3H-WIN35,428 by the protocol provided by the membrane manufacturer (PerkinElmer) with minor modifications [14, 15]. Briefly, cloned human DAT membranes (12 μg/well; PerkinElmer) were incubated at 4 °C for 120 min in a final volume of 0.25 mL reaction mixture containing 3H-WIN35,428 and various concentrations of the drug in 50 mM Tris–HCl (pH 7.4) buffer containing 100 mM NaCl. Then, the incubation was terminated by rapid filtration using a cell harvester (Inotech Biosystems, Dietikon, Switzerland) through the Filtermat A glass fiber filter (PerkinElmer) presoaked in 0.5% polyethyleneimmine (PEI). The filter was covered with the MeltiLex sheet (PerkinElmer), sealed in a sample bag, dried in a microwave oven, and analyzed by liquid scintillation counting (PerkinElmer). Nonspecific binding was determined in the presence of 10 μM GBR-12909. The binding affinity of the compound was calculated by computerized nonlinear regression analysis (GraphPad Prism Program; GraphPad Software, La Jolla, CA, USA).
The SERT binding assay was also performed using 2 nM 3H-imipramine, as previously described [15, 16]. Cloned human serotonin transporter membranes (9 μg/well, PerkinElmer) and 2 nM 3H-imipramine were incubated in buffer containing 50 mM Tris-HCl (pH 7.4), 120 mM NaCl and 5 mM KCl. After incubation for 30 min at 27 °C, the reaction was terminated by rapid filtration through a Filtermat A glass fiber filter (PerkinElmer) presoaked in 0.5% PEI. The filter was covered with the MeltiLex sheet (PerkinElmer), sealed in a sample bag, dried in a microwave oven, and analyzed by liquid scintillation counting (PerkinElmer). Nonspecific binding was determined in the presence of 10 μM fluoxetine. The binding affinity of the compound was calculated in the same method as that of the DAT binding assay.
Data processing and statistical analysis
The LC–MS/MS data for the measurements of DA, 5-HT, and metabolites in the nucleus accumbens after the exposure of METH, 5-API, 3-FMA, 5-MAPB or DMMA to rats was processed using the Mass Hunter software (B. 04. 00, Agilent Technologies). The baseline value was determined from three consecutive microdialysates with less than 20% fluctuation in the concentrations of DA, 5-HT, and their metabolites before drug or vehicle administration. The quantification of DA, 5-HT, and their metabolites were divided by the selected baseline value and expressed as percentages. Their concentrations were then adjusted with those of vehicles at the same time points. Statistical analysis was conducted by one-way analysis of variance (ANOVA) for repeated measures followed by a Bonferroni post hoc test. The binding affinity of the compound was calculated by computerized nonlinear regression analysis (GraphPad Software).
Results
Measurement of DA, 5-HT, and their metabolites in the rat nucleus accumbens
The changes in the concentrations of DA, 5-HT, and their metabolites in the microdialysates collected from the rat nucleus accumbens after exposure to 5-API, 3-FMA, 5-MAPB or DMMA are shown in Fig. 1. The treatment of METH was applied as a positive control (Fig. 1a).
Changes in the concentrations of dopamine (DA) and serotonin (5-HT) and their metabolites [3,4-dihydroxyphenylacetic acid (DOPAC), homovanillic acid (HVA) and 5-hydroxyindoleacetic acid (5-HIAA)] in microdialysates collected from rats after exposure to each aromatic ring-substituted phenethylamine. Each arrow, in order, represents the time of the administration of 0.3, 1, and 3 mg/kg intraperitoneally (i.p.), respectively, for methamphetamine (METH), 5-API, 3-FMA, and DMMA, and 0.1, 0.3, and 1 mg/kg (i.p.) for 5-MAPB [mean ± standard error of the mean (SEM); n = 4–6; DA, aP < 0.05 or aaP < 0.01; 5-HT, bP < 0.05 or bbP < 0.01; DOPAC, cP < 0.05 or ccP < 0.01; HVA, dP < 0.05 or ddP < 0.01; 5-HIAA, eP < 0.05 or eeP < 0.01 vs. vehicle treated group]
The exposure to 5-API induced a significant increase in both the DA and the 5-HT concentrations after injection of 3 mg/kg (at 140 and 160 min) and 1 mg/kg (after 80 min), respectively. The concentration of DOPAC was below the limit of quantification 60 min after the injection of 1 mg/kg (Fig. 1b).
The administration of 3-FMA induced significant alterations in the concentration of 5-HT, but not in the concentrations of DA. The level of 5-HT markedly increased after the injection of 3 mg/kg (at 140 and 160 min) and that of 5-HIAA significantly (P < 0.05) increased in a dose-dependent manner. Although the concentration of HVA, a metabolite of DA, significantly increased, those of DA and DOPAC, another metabolite, did not change significantly (Fig. 1c).
In case of 5-MAPB, the level of 5-HT significantly increased after the administration of 1 mg/kg and that of DOPAC decreased after the injection of lower doses (0.1 and 0.3 mg/kg) (Fig. 1d). The administration of 3 mg/kg 5-MAPB was not performed owing to severe toxicity or death. DMMA caused the increased extracellular levels of only HVA (Fig. 1e).
The areas under the curves for DA, 5-HT, and their metabolites vs. time (AUC, 0–180 min) after exposure to 5-API, 3-FMA, 5-MAPB or DMMA, which were derived from the data in Fig. 1, are shown in Fig. 2. The 5-API induced the release of DA, similar to METH. The 5-API, 3-FMA and 5-MAPB caused an increase in extracellular 5-HT levels, whereas METH did not significantly increase them.
DA and 5-HT reuptake inhibition
The median inhibition concentration (IC50) values of 5-API, 3-FMA, 5-MAPB and DMMA for DAT and SERT are shown in Table 3, and the corresponding uptake inhibition curves are presented in Fig. 3. With the exception of DMMA, the other drugs mainly inhibited DAT, with IC50 values of from 0.33 to 3.1 µM. Among them, 5-API was a highly potent inhibitor of both DAT and SERT.
DAT and SERT binding affinities
The DAT and SERT binding affinities of 5-API, 3-FMA, 5-MAPB, and DMMA are shown in Table 4. Among the drugs, only 5-API had submicromolar affinities for both DAT and SERT. 5-MAPB had a higher binding affinity for DAT than for SERT.
Discussion
New psychoactive phenethylamines have been rapidly introduced, and the knowledge of their effects on the central nervous system is promptly required for their control as scheduled drugs. However, only limited in vitro studies have been conducted owing to the lack of reference standard drugs and the difficulties of brain sampling and analytical techniques in animal studies. In the present study, the in vivo measurements of DA, 5-HT, and their metabolites, as well as the in vitro assays of the DART and SERT were simultaneously performed and provided an important insight into the effects of the drugs on the DA and 5-HT systems. It is well known that METH, the positive control in the present study, potently induces DA release by blocking DAT [7]. Our results also confirmed that METH induced DAT-mediated DA release.
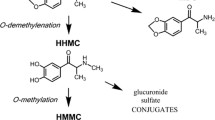
A previous study reported that 5-API, which is often used as an MDMA replacement, acted as a potent inhibitor for both DAT and SERT in rat brain synaptosomes, but induced more potent inhibition of DAT than SERT [17]. In addition, in other previous in vitro studies, 5-API showed DAT and SERT-mediated releasing properties [18, 19]. The present animal study also demonstrated that 5-API induced the nonselective potent release of both DA and 5-HT (Fig. 2a, d), which was strongly correlated with high degrees of uptake inhibition (Table 3) and binding affinity (Table 4) to DAT and SERT. Interestingly, it was reported as a potent in vitro inhibitor of human monoamine oxidase A, for the transformation of DA to DOPAC [20], which was consistent with the current in vivo results. Our results clearly showed that although the concentration of DA significantly increased (Fig. 2a), DOPAC and HVA decreased in rats (Fig. 2b, c). From our AUC results, the total change in DOPAC and HVA concentration was decreased (Fig. 2b, c) as compared with that of DA (Fig. 2a).
Few studies on the effects of 3-FMA on neurotransmitter release have been conducted. Previously, para-halogenated amphetamines, including 4-FMA, were reported to induce the release of both DA and 5-HT and to block both DAT and SERT, but were more effective to 5-HT [21]. A recent study on the neurotoxicity of 3-FMA concluded that the D1 receptor played an important role in 3-FMA. Moreover, the concentration of DA significantly declined, but the DA turnover rate, (DOPAC + HVA)/DA, was increased in the mice striatum collected 1 day after the intraperitoneal administration of 40 mg/kg 3-FMA [22]. In our study, the administration of 3-FMA induced a significant increase in the concentrations of 5-HT and its metabolite (Fig. 2d, e), instead of DA and its metabolites. However, it had high binding affinities for both DAT and SERT (Table 4); thus, the release of 5-HT in the synaptic cleft might be attributable to exocytosis. The doses of 3-FMA in the present study (0.3, 1, and 3 mg/kg) seem too low to affect the DAT, because, in the previous study [22], 40–80 mg/kg doses of 3-FMA were administered to mice.
A previous study on the effects of 5-MAPB on extracellular monoamine levels in the mouse striatum by using microdialysis reported that it significantly increased the DA and 5-HT concentrations in a dose-dependent manner (0.4 × 10−4, 0.8 × 10−4, and 1.6 × 10−4 mol/kg) and showed a larger increase in the 5-HT level than the level of DA [23]. These results were consistent with ours, in which 5-MAPB considerably affected both DAT and SERT inhibition (Table 3) and effected a noticeable increase in the concentration of 5-HT at a high dose (Fig. 1d).
DMMA is considered as an MDMA analog. MDMA is a popular recreational drug, which exerted a greater influence on 5-HT release and SERT inhibition [8]. However, DMMA was significantly less potent than MDMA on SERT in a previous study [24]. Our results also showed that DMMA induced weak inhibition (Fig. 3e) and binding affinity at SERT, and almost no increase in the 5-HT concentration (Fig. 2d).
Conclusions
We found that new psychoactive phenethylamines, with a variety of aromatic ring substitutions, affected the extracellular levels of DA, 5-HT, and/or their metabolites in the nucleus accumbens of rats to varying degrees and in different ways. These drugs acted as potent inhibitors for DAT and/or SERT. The current results may be helpful for further research into monoamine neurotransmitter-related mechanisms of new psychoactive phenethylamines. Although it is difficult to postulate the effects of new psychoactive phenethylamines on the release of DA and 5-HT from their chemical structure, further studies on the chemical structure could provide insight into the mechanism of action and predict the liability of NPS abuse.
References
Kersten BP, McLaughlin ME (2015) Toxicology and management of novel psychoactive drugs. J Pharm Pract 28:50–65. https://doi.org/10.1177/0897190014544814
Nelson ME, Bryant SM, Aks SE (2014) Emerging drugs of abuse. Dis Mon 60:110–132. https://doi.org/10.1016/j.disamonth.2014.01.001
Rivera JV, Vance EG, Rushton WF, Arnold JK (2017) Novel psychoactive substances and trends of abuse. Crit Care Nurs Q 40:374–382. https://doi.org/10.1097/CNQ.0000000000000174
Hill SL, Thomas SH (2011) Clinical toxicology of newer recreational drugs. Clin Toxicol 49:705–719. https://doi.org/10.3109/15563650.2011.615318
Gingrich JA, Hen R (2001) Dissecting the role of the serotonin system in neuropsychiatric disorders using knockout mice. Psychopharmacology 155:1–10 (PMID: 11374326)
Sanders-Bush E, Hazelwood L (2011) 5-Hydroxytryptamine (serotonin) and dopamine. In: Brunton LL, Chabner BA, Knollmann BC (eds) Goodman & Gilman’s pharmacological basis of therapeutics, 12th edn. McGraw-Hill, New York, pp 335–361
Courtney KE, Ray LA (2014) Methamphetamine: an update on epidemiology, pharmacology, clinical phenomenology, and treatment literature. Drug Alcohol Depend 143:11–21. https://doi.org/10.1016/j.drugalcdep.2014.08.003
Lyles J, Cadet JL (2003) Methylenedioxymethamphetamine (MDMA, Ecstasy) neurotoxicity: cellular and molecular mechanisms. Brain Res Rev 42:155–168 (PMID: 12738056)
Kim M, Kim DH, Lee YS, Jang C-G, Yang CH, Lee S (2017) Changes in dopamine, serotonin and their metabolites in brain microdialysates from rats following exposure to new psychoactive drugs. Forensic Toxicol 35:66–76. https://doi.org/10.1007/s11419-016-0335-8
Zhao RJ, Yoon SS, Lee BH, Kwon YK, Kim KJ, Shim I, Choi K-H, Kim MR, Golden GT, Yang CH (2006) Acupuncture normalizes the release of accumbal dopamine during the withdrawal period and after the ethanol challenge in chronic ethanol-treated rats. Neurosci Lett 395:28–32. https://doi.org/10.1016/j.neulet.2005.10.043
Kim M, Lee JG, Yang CH, Lee S (2016) Silica stationary phase-based on-line sample enrichment coupled with LC–MS/MS for the quantification of dopamine, serotonin and their metabolites in rat brain microdialysates. Anal Chim Acta 923:55–65. https://doi.org/10.1016/j.aca.2016.03.021
Paudel S, Cao Y, Guo S, An B, Kim KM, Cheon SH (2015) Design and synthesis of 4-benzylpiperidine carboxamides as dual serotonin and norepinephrine reuptake inhibitors. Bioorg Med Chem 23:6418–6426. https://doi.org/10.1016/j.bmc.2015.08.022
Torres GE, Yao WD, Mohn AR, Quan H, Kim KM, Levey AI, Staudinger J, Caron MG (2001) Functional interaction between monoamine plasma membrane transporters and the synaptic PDZ domain-containing protein PICK1. Neuron 30:121–134 (PMID: 11343649)
Wigestrand MB, Stenberg M, Walaas SI, Fonnum F, Andersson PL (2013) Non-dioxin-like PCBs inhibit [3H]WIN-35,428 binding to the dopamine transporter: a structure-activity relationship study. Neurotoxicology 39:18–24. https://doi.org/10.1016/j.neuro.2013.07.005
Kim Y, Tae J, Lee K, Rhim H, Choo IH, Cho H, Park W-K, Keum G, Choo H (2014) Novel N-biphenyl-2-ylmethyl 2-methoxyphenylpiperazinylalkanamides as 5-HT7R antagonists for the treatment of depression. Bioorg Med Chem 22:4587–4596. https://doi.org/10.1016/j.bmc.2014.07.026
Brinkø A, Larsen MT, Koldsø H, Besenbacher L, Kolind A, Schiøtt B, Sinning S, Jensen HH (2016) Synthesis and inhibitory evaluation of 3-linked imipramines for the exploration of the S2 site of the human serotonin transporter. Bioorg Med Chem 24:2725–2738. https://doi.org/10.1016/j.bmc.2016.04.039
Marusich JA, Antonazzo KR, Blough BE, Brandt SD, Kavanagh PV, Partilla JS, Baumann MH (2016) The new psychoactive substances 5-(2-aminopropyl)indole (5-IT) and 6-(2-aminopropyl)indole (6-IT) interact with monoamine transporters in brain tissue. Neuropharmacology 101:68–75. https://doi.org/10.1016/j.neuropharm.2015.09.004
Luethi D, Kolaczynska KE, Docci L, Krahenbuhl S, Hoener MC, Liechti ME (2017) Pharmacological profile of mephedrone analogs and related new psychoactive substances. Neuropharmacology 134:4–12. https://doi.org/10.1016/j.neuropharm.2017.07.026
Shimshoni JA, Winkler I, Golan E, Nutt D (2017) Neurochemical binding profiles of novel indole and benzofuran MDMA analogues. Naunyn Schmiedebergs Arch Pharmacol 390:15–24. https://doi.org/10.1007/s00210-016-1297-4
Herraiz T, Brandt SD (2014) 5-(2-Aminopropyl)indole (5-IT): a psychoactive substance used for recreational purposes is an inhibitor of human monoamine oxidase (MAO). Drug Test Anal 6:607–613. https://doi.org/10.1002/dta.1530
Rickli A, Hoener MC, Liechti ME (2015) Monoamine transporter and receptor interaction profiles of novel psychoactive substances: para-halogenated amphetamines and pyrovalerone cathinones. Eur Neuropsychopharmacol 25:365–376. https://doi.org/10.1016/j.euroneuro.2014.12.012
Nguyen P-T, Shin E-J, Dang D-K, Tran H-Q, Jang C-G, Jeong JH, Lee YJ, Lee HJ, Lee YS, Yamada K, Nabeshima T, Kim H-C (2018) Role of dopamine D1 receptor in 3-fluoromethamphetamine-induced neurotoxicity in mice. Neurochem Int 113:69–84. https://doi.org/10.1016/j.neuint.2017.11.017
Fuwa T, Suzuki J, Tanaka T, Inomata A, Honda Y, Kodama T (2016) Novel psychoactive benzofurans strongly increase extracellular serotonin level in mouse corpus striatum. J Toxicol Sci 41:329–337. https://doi.org/10.2131/jts.41.329
Montgomery T, Buon C, Eibauer S, Guiry PJ, Keenan AK, McBean GJ (2007) Comparative potencies of 3,4-methylenedioxymethamphetamine (MDMA) analogues as inhibitors of [3H]noradrenaline and [3H]5-HT transport in mammalian cell lines. Br J Pharmacol 152:1121–1130. https://doi.org/10.1038/sj.bjp.0707473
Acknowledgements
This research was supported by grants from the Ministry of Food and Drug Safety (14182MFDS979 and 16182MFDS417) and by the Basic Science Research Program through the National Research Foundation of Korea (NRF) funded by the Ministry of Education (NRF-2016R1A6A1A03011325).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Ethical approval
This article does not contain any studies with human participants performed by any of the authors. All animal experiments were approved of the Institutional Animal Care and Use Committee at Daegu Haany University.
Rights and permissions
About this article
Cite this article
Kim, M., Yang, C.H., Lee, Y.S. et al. Effects of aromatic ring-substituted phenethylamines on the release of dopamine and serotonin. Forensic Toxicol 37, 104–112 (2019). https://doi.org/10.1007/s11419-018-0440-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11419-018-0440-y