Abstract
Rural communities face tremendous challenges in accessing mental health and substance abuse treatment services. Some of the most promising advancements in the delivery of rural health care services have been in the area of telecommunication technology. These applications have the potential to reduce the disparities in the delivery of substance abuse and mental health services between urban and rural communities. The purpose of this inquiry was to explore the advances and uses of telecommunications technology, and related issues, in the delivery of mental health and substance abuse treatment services within rural areas. A review of the academic literature and other relevant works was conducted and the content was organized into four major themes: (a) advantages of telehealth and applications to rural practice, (b) barriers to implementation in rural practice, (c) utilization in rural areas, and (d) areas for further research.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The prevalence of substance abuse and mental illness varies greatly based on race, gender, age, and life experiences. Moreover, literature establishes that additional disparities exist between social classes, geographic locations, and cultural variations.1 In many rural areas, the provision of adequate mental health and substance abuse services is compounded by geographic isolation, low socioeconomic status of the population, and a high incidence of unique cultural groups that face language and cultural barriers to treatment. Rural treatment programs face ever increasing difficulty in recruiting and retaining qualified professionals and staff due to the economic climate. The ongoing shortage of service providers further inhibits the provision of adequate services, and as the population ages, demand continues to increase. One of the most promising advancements in rural health care has been the proliferation of telecommunication technology. The use of video conferencing, telerobotics, picture phones, interactive video, and virtual reality has provided a new way to increase access to specialty services that might not otherwise be available to the rural population.
The passage of the Telecommunication Act of 1996 helped pave the way for the use of technology as a treatment modality by removing certain economic and legal barriers to its use. The federal government currently commits millions of taxpayer dollars each year to promote the use of telecommunications in healthcare. In support of these efforts, the Rural Health Care Program of the Universal Service Fund has also aided these communities by allowing rural areas to receive the technology needed for telecommunication at a rate comparable to urban areas. As a result, the use of telecommunication technology to provide care in rural areas is on the rise. Telehealth is being successfully implemented in numerous geographic locations to treat a variety of illnesses and addictions.2–11 The purpose of this paper is to explore the advances made and current uses of telecommunication technology in the provision of mental health and substance abuse services within rural settings. It reflects a review of academic literature and relevant unpublished works. Additionally, a summary of terminology noted in the literature is included as a guide for the reader.
Terminology
Telehealth is used to provide health care, health information, and health education across a distance through the use of telecommunication technology and specially adapted equipment. It allows physicians, nurses, and other healthcare personnel to assess, diagnose, and treat patients without requiring that both individuals be physically located in the same place. This capacity is particularly advantageous to rural communities as access to specialty healthcare can be difficult but readily improved through the use of telecommunication.
The terms telehealth, telemedicine, telemental health, telepsychiatry, and telecommunication technology are sometimes used interchangeably. In this document, the word telehealth will be used to refer to health technology in general. More specific terms, such as telepsychiatry or telemental health, will be used referring to these specialty services available via telecommunication devices.
Telecommunication technology currently includes a range of devices, including but not limited to: voice modalities, such as telephone and radio, picture phones and teleconferencing, fax and emails, data imaging computers, interactive video and virtual reality, and telerobotic methods.
Methods
A review of literature spanning the years 1996 through 2012 was conducted to identify relevant studies and central works examining or exploring the use of telehealth in a variety of rural health settings, in particular, those pertaining to the treatment of mental health and substance abuse. The year 1996 was selected as the starting point since legislation surrounding reimbursement for telehealth services emerged during this time period. PubMed and Google Scholar were the bibliographic databases queried. PubMed was elected as one of the databases to be queried as it houses one of the most comprehensive bodies of literature on a wide array of health concerns. Google Scholar was chosen as the second database to examine because its content is more expansive than most other bibliographic databases.
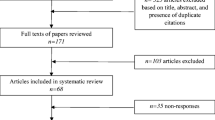
The theoretical framework employed was inductive in nature. Themes were inductively identified based on the literature collected during the review. Selection criteria for literature included the following parameters: publication in English; immediately available online; emphasis on telemental health, telepsychiatry, or telehealth to provide services for substance abuse disorders; application to rural practice either nationally or internationally; and date of publication (between 1996 and 2012). Key words employed in the search were telehealth, telemedicine, telepsychiatry, telemental health, telecommunications technology, rural health, rural health services, rural mental health services, rural substance abuse treatment, and rural health clinicians. Medical Subject Headings (MeSH) and string searches were used to retrieve the most relevant articles. Approximately 240 non-duplicated abstracts were identified.
Findings
Of the approximate 240 articles identified, 38 met the selection criteria. These items were reviewed for content and applicability. Additional literature has been included to brief the reader on findings and developments not specific to rural areas but of importance to the field of telehealth. Numerous broad topics emerged, and after re-organization and further analysis of the information, content was organized into four major themes: (a) advantages of telehealth and applications to rural practice, (b) barriers to implementation in rural practice, (c) utilization in rural areas, and (d) areas for further research.
Theme no. 1: advantages of telehealth and application to rural practice
The shortage of care providers is one of the primary barriers to adequate mental health and substance abuse services for many rural communities. In a 2007 position statement, the American Telemedicine Association (ATA) described several ways in which telehealth technology could potentially relieve this shortage by bringing the patient and the provider together with a virtual visit via video conferencing.12 The technology could further alleviate the problem by enabling providers to store and forward digital images and clinical data, afford a way to monitor a patient’s condition in the home setting, enhancing staff training, supplying on-the-spot interactive technical assistance during surgeries and other medical procedures (including inaccessible locations such as ships and remote locations), and serving individuals who are incarcerated or institutionalized. Literature establishes that telehealth can successfully be implemented for overcoming barriers to adequate services in rural and geographically isolated locations. The benefits of telehealth to the client include reduced travel time and cost, reduced separation of families, and a reduced number of missed appointments.13,14 Moreover, the literature supports that rurally located patients express satisfaction with services and a willingness to reuse services.15,16 The benefits of telehealth for the rurally located provider include enhanced training, a reduction in isolation, and increased opportunities for collaboration.15,17,18
Theme no. 2: barriers to implementation in rural practice
While the rapid evolution of technology has increased the capacity to offer mental health and substance abuse services in rural areas, funding and reimbursement mechanisms have not been as swift in their development. As a result, financial sustainability has been one of the primary barriers to expansion of telehealth services in rural areas.19,20 This challenge is often compounded by startup costs for purchasing equipment and ongoing costs to maintain it.19,20
The Balanced Budget Act of 1997 presented the first authorization for using Medicare funds for Telemedicine.21 The act allowed for fee splitting, limited CPT code (current procedural terminology) reimbursement, and limited eligible providers. Additional allowances came through the Benefits Improvement and Protection Act of 2000.22 Reimbursement was initially allowed only in primary care Health Professional Shortage Areas and not in Metropolitan Statistical Areas. However, the Medicare Patient and Physician Improvement Act of 2008 expanded coverage to include sites such as skilled nursing facilities, hospital-based dialysis centers, and community mental health centers.23 In addition, Medicare eligible practitioners were able to receive reimbursement. Services covered include consultations, inpatient and outpatient visits, individual psychotherapy, and pharmacologic management.
The Medicare Telehealth Enhancement Act of 2008 expanded services again by eliminating geographic restrictions based on rural designation, including underserved urban and suburban areas, and adding home health and other treatment providers.24 The federal government does not mandate reimbursement for telehealth under Medicaid; however, it does allow for reimbursement if certain parameters are met.25 The public health insurance program is state-administered, thus reimbursement for telehealth services is optional. Currently, as many as 35 states provide some form of reimbursement for such services and 13 of these have expanded this benefit to care rendered by psychologists. In some areas, the practitioner providing the service must be licensed in the state where the patient is located.26 Notably, a few states have established laws for private insurance companies prohibiting the exclusion and allowing for the reimbursement of telehealth services. While reimbursement for telehealth services has been implemented through Medicaid, Medicare, and some private insurance companies, reimbursement is less than that of services provided in face-to-face encounters.6,27 Literature indicates that although clinics face financial barriers, clients often save money through use of telehealth services due to a reduction in travel.6,28
Reimbursement problems are also a key impediment to rural communities looking to expand mental health and substance abuse services through telehealth.6,27,29 In order for funding to increase, insurers, policymakers, local champions, key stake holders, and funding agencies alike need to be convinced that telehealth is not only a valid alternative to face-to-face encounters, but that it also yields equitable results. More randomized controlled studies have been conducted to demonstrate the validity and equality of services.30
Other barriers to implementation include the space needed to house technological equipment on both the provider and client end, as well as startup and purchasing costs of equipment.19,20 Providers frequently feel undertrained to provide the service and use the equipment. Training on optimizing audio and video quality, the technical aspects of using equipment, and clear clinical policies regarding specific procedures and services are necessary for successful use.31 While the above obstacles are often present initially, over time providers demonstrate increasing satisfaction and comfort using telehealth to provide services. In addition to the aforementioned issues, variability in technology, licensure requirements and time zone differences, can also be prohibitive to use.10
Despite the financial barriers and with support of the Patient Protection and Affordable Care Act of 2010 and an unlimited growing market, expansion in telehealth is occurring and companies, with a vested interest, such as Verizon®, are taking note.14,32
Theme no. 3: utilization in rural areas
Utility
Telehealth is gaining mainstream status among practitioners in rural areas, and literature indicates that both patients and practitioners view it as an acceptable substitution for in-person treatment.15,33,34 The driving forces behind the rapid proliferation of telehealth include new innovations in technology, a growing evidence base, increasing levels of consumer acceptance, vendor interest, and the emerging regulatory framework promoting its use. As early as 1998, the use of telemental health in rural and remote areas had expanded to include pre-admission and discharge planning, case management, evaluations, family visits, psychotherapy, court commitment hearings, and family support groups and to enhance provider training, clinical supervision, and provision of medical services to deployed personnel.18,35 Larger-scale telemental health initiatives have been initiated to provide services in rural areas such as Hawaii, Texas, Maryland, Alabama, India, and Australia.4,8–11 The University of Hawaii Rural Health Collaboration (UHRHC) is one such example, and initial evidence suggests that it is a promising development to increase access to health services and reduce disparities.8
Provider use and provider training
Telehealth has also demonstrated promising results as a mode of training primary care providers. It has been shown to increase access to peer consultation, enhance provider skills and knowledge, reduce isolation from academic input, and increase practitioners confidence and competence in managing psychiatric patients.15,17 Studies have indicated that the use of telemental health modalities by rural practitioners evolves through recurrent use. Over time, rural practitioners become significantly more likely to consult peers and to seek help with new and current treatment plans. Collaboration increases as relationships with other practitioners are established via telecommunication.17 Overall, the literature establishes that staff response to telehealth training and services is positive.15,18
Adult psychiatric care
The delivery of psychiatric services through telecommunication routes is also on the rise in both urban and rural areas. Telepsychiatry, in particular video teleconferencing (VTC), is used to treat a variety of disorders and is capable of allowing providers to reliably assess, diagnose, and treat many mental health and substance abuse concerns from a distance.12,33,36 It is important to note that while several studies have shown psychiatry via VTC to be comparable to face-to-face interventions, other modes of telepsychiatry have not been proven.37 For rural communities, the benefits of telepsychiatry are multifactoral and include improved functioning, a reduction in hospital referrals, improved convenience, decreased number of missed appointments, a reduction in travel time as well as time spent waiting for specialty services, reduced level of stigma, and enhanced access to treatment.9,38–40
Though a more novel application, emergency telepsychiatry in rural practice is also demonstrating promising results. The Burke Mental Health Emergency Center (MHEC) is the first freestanding rural comprehensive psychiatric emergency program in which services are performed entirely by telepsychiatrists. Analysis of admissions to the Burke Center’s locked unit demonstrated a 70% reduction in hospital referrals, as well as reduced hospital stays to an average of 3.9 hours.9
Pediatric telemental health and psychiatric care
The use of telepsychiatry and telemental health for children is not as widespread as in adults, but it is growing. In general, telehealth is gaining popularity in pediatric and adolescent services and has been implemented in various areas including treatment of depression, anxiety, substance abuse, ADHD, eating disorders, and general mental health promotion with high parent, provider, and patient satisfaction.20,41–44 Studies specific to rural areas have concluded that the use of telepsychiatry can improve rural health care for pediatric clients and that the quality of clinical interactions appears comparable to face-to face meetings.5,42,45,46 Moreover, telehealth modalities minimize family disruption, provide a shorter waiting time for treatment, are favored by families over traveling long distances to receive care, and may be the preferred treatment over face-to-face interviews.5,41 Determinants of satisfaction with services include an established physician–client relationship and high quality audio and video transmission.47,48 Overall, the quality of care of rurally located pediatric patients needing mental health services is improved through telehealth, reduces the burden on families, and may be preferred by some children over face-to-face interviews.5,49 The primary barrier to using telepsychiatry for children in rural areas is the absence of reimbursement for such services.5 Other problems in the use of this technology for rurally located children include the cost of implementation, complexity of hardware, difficulty assessing non-verbal communication, and that it may take longer to establish rapport with some children.50–53
Substance abuse treatment
Telehealth is playing a larger role in the provision of substance abuse treatment.54–58 Research supports that the use of telehealth in the delivery of substance abuse services is effective, produces higher completion rates to traditional services, and that clients may prefer telehealth sessions because of its convenience and perceived increase in confidentiality.54–56,59,60 Although the literature specific to rural areas is notably sparse, the limited extant research suggests that telephone and web-based interventions are being used to enhance programs and may in some instances enhance abstinence and self-awareness in addicted individuals.4,27
Post traumatic stress disorder
Although preliminary research clearly established that a variety of telemental health modalities were feasible, reliable, and satisfactory for general clinical assessments and care, less is known about the clinical application and effectiveness of this approach in the assessment or treatment of PTSD.61,62 The application of telemental health in PTSD assessment and treatment remains a controversial issue.28,36 Yet, over the past 10 years the body of literature related to PTSD and telemental health has yielded positive results.63–65 It has been applied successfully in psycho-education, screening, and clinical therapy groups.63–65 The Veterans Administration (VA) has implemented telehealth modalities and reports that PTSD treatment is comparable to services provided face-to-face. In addition, veterans, clinic staff, and remote clinicians all viewed VTC treatment as helpful.63,64 Literature specific to rural areas is aligned with these findings and supports that the approach has also successfully been used to treat culturally unique groups such as Native American Indian Veterans with PTSD.7,66
Cross-cultural applications
Literature over the past 15 years indicates that therapies for mental health and substance abuse, offered via telehealth, are acceptable across cultural lines. The approach is a viable method to increase culturally competent services in rural areas for specialty populations such as Native American Indian Veterans, Chinese Americans, and Latin Americans.3,67–69 These modalities have proven themselves in terms of client and provider acceptance, reliability of assessment data, and feasibility.3,67–69 Nonetheless, more research is needed in order to develop culturally aligned evidence-based practices and mental health promotion interventions for individual populations. Studies have indicated that the success of a program is often influenced by utilizing individuals from the specialty population to assist in running the clinic and acting as liaisons with staff located elsewhere.66 The incorporation of culturally aligned teachings and perceptions into sessions conducted via telehealth increases viability and consumer acceptance. One example of this is the facilitation of Native American talking circles using telehealth modalities.70
Areas for further research
The body of knowledge related to telehealth is undoubtedly expanding, but there are major areas that remain under-examined. For instance, a limited number of randomized controlled research studies are represented in the literature, in spite of the growth in telemental health services within rural and non-rural communities.63,71,72 Furthermore, there are few published works on the use of telehealth to provide or enhance substance abuse services in rural areas.
The ATA report has also identified deficits in research, among them the effectiveness of assessment of patients in acute psychiatric units, consultative psychiatry, and the provision of services to geriatric patients in nursing facilities.73 In 2011, researchers stressed the lack of data showing the efficacy of child and adolescent telemental health services and the importance of generating good process and outcome data, as these are critical to the development of evidence-based practice standards.74
Implications for Behavioral Health
A combination of geographic isolation, disparities between social classes, unique cultural groups, lack of funding, and low socioeconomic status makes adequate provision of mental health and substance abuse services a significant challenge in rural communities. The body of literature examined in this review illustrates that telemedicine has been successfully used to enhance a variety of clinical services and educational initiatives in rural communities, and serves as a viable mode to increase access to specialty professional services in remote areas in a convenient and economical way. Nonetheless, more research is warranted to determine the quality and clinical effectiveness of the services provided using this technology.
Preliminary research and the limited number of controlled studies identified demonstrate promise in providing training, technical assistance, evaluation, and treatment using distance technology. The military, in particular, is using telemental health and telepsychiatry in a variety of ways. Yet, significant barriers to fully realizing telemental health services in rural communities persist. Several states have yet to resolve credentialing and licensure issues. Requiring that practitioners be licensed in the same state as patients being served is an added financial burden that inhibits the use of telecommunication services in many areas.
Furthermore, technology requirements raise additional financial and infrastructure problems. The equipment is often expensive and on-going transmission costs and professional services are prohibitive to some rural communities. For many rural areas, phones remain a primary method of transmission. The quality and type of phone system vary and are frequently not compatible with the technology needs of high speed computers and videoconferencing. Additionally, the funding and reimbursement of services are inconsistent among states. Although federal legislation has aided in the promotion of technology, private insurance and Medicare or Medicaid disallow or limit reimbursement for many of the telecommunication services rendered.
The discord between federal and state expectations goes beyond funding; there are also ethical elements at play. The Health Insurance Portability and Accountability Act (HIPAA) and confidentiality concerns are not completely resolved. More work is required to ensure that care provided via distance is conducted in a manner that protects client information.
Several key ingredients to the success of a telemental health or substance abuse program were identified. Strong leadership; flexibility to adapt to the evolving needs of the community; adequate coordination with multidisciplinary teams; adequate and ongoing training for providers, champions, and key stakeholders who buy into the solution and dedicate themselves to political advocacy; and continuous assessment of community needs are critical to ensuring success.9,10
Telehealth can play a considerable role in reducing health disparities for those residing in rural communities. The technology allows for increased access to specialized mental health services, technical information, and training that may not be locally available. If funding and reimbursement issues can be properly addressed, telehealth holds great promise for the future of rural communities.
References
Primm AB, Vasquez MJT, Mays RA, Sammons-Posey D, McKnight-Eily LR, Presley-Cantrell LR, et al. The role of public health in addressing racial and ethnic disparities in mental health and mental illness. Preventing Chronic Disease 2010; 7(1): A20. http://www.cdc.gov/pcd/issues/2010/jan/09_0125.htm. Accessed June 11, 2012.
National Association of State Alcohol and Drug Abuse Directors, Inc. Tele-health in Sate Substance Use Disorder (SUD) Services, 2009. Supported by: The Substance Abuse and Mental Health Services Administration’s (SAMHSA) Center for Substance Abuse Treatment (CSAT), under the NOMS Collaborative Support Initiative, Grant # 5H79TI019551, June.
Chong, J, Moreno, F. Feasibility and acceptability of clinic-based telepsychiatry for low-income Hispanic primary care patients. Telemedicine Journal and E-Health 2012; 18(4): 297–304
Thara, R. Using mobile telepsychiatry to close the mental health gap. Current Psychiatry Reports 2012; 14(3): 167–8.
Sulzbacher, S, Vallen, T, Waetzig, EG. Telepsychiatry improves pediatric behavioral health care in rural communities. Journal of Telemedicine and Telecare 2006, 12(6): 285–8
Campbell, NC, Meile, GM, Nunes, EV, et al. Web-based, psychosocial treatment for substance use disorders in community treatment settings. Psychological Services 2012; 9(2): 212–214. doi:10.1037/a0025968
Teleservices improve access to PTSD treatment. Telemedicine Journal and E-Health 2010 Jul-Aug; 16(6): 654–8, doi:10.1089/tmj.2010.9958
Chung-Do J, Helm, S, Fukuda, M, et al. Rural mental health implications for telepsychiatry in clinical service, workforce development, and organizational capacity. Telemedicine Journal and E-Health 2012; 18(3): 244–6.
2011 APA Gold Award: A telepsychiatry solution for rural eastern Texas. Psychiatric Services 2011; 62 (11): 1384–1386. doi:10.1176/appi.ps.62.11.1384
Ulzen, T, Williamson, L, Foster, PP, et al. The evolution of a community based telepsychiatry program in rural Alabama- A brief report. Community Mental Health Journal 2012; doi:10.1007/s10597-012-9493-2.
Edward, K. The VA Maryland health care system’s telemental health program. Psychological Services 2012; 9(2): 203–205.
American Tele-medicine Association (ATA). Tele-health and health care provider shortages, position statement and recommendations. Available online at http://www.americantelemed.org/files/public/policy/Telehealth_and_the_Provider_Shortage.pdf. Accessed December 5, 2011.
Center for Telehealth and E-Law. While a telehealth program can provide many benefits, attention must be paid to state and federal laws that determine what is considered a legal interaction. Available online at http://healthcare-executive-insight.advanceweb.com/Features/Articles/Telehealth-Can-Save-Time-Money.aspx. Accessed December 5, 2011.
Sarasohn-Kahn, J. Tele-health beginning to go mainstream, but long road lies ahead. IHealth Newsletter 2010 June 7.
Hilty, DM, Luo, JS, Morache, C, et al. Tele-psychiatry: An overview for psychiatrists. CNS Drugs 2002; 16: 527–548.
Hilty, DM, Nesbitt, TS, Kuenneth, CA, et al. Rural versus suburban primary care needs, utilization and satisfaction with telepsychiatric consultation. The Journal of Rural Health 2007; 23(2): 163–165: doi:10.1111/j.1748-0361.2007.00084.x
Hilty, D, Yellowlees, P, Nesbitt, T. Evolution of telepsychiatry to rural sites: changes over time in types of referral and in primary care providers knowledge, skills and satisfaction. General Hospital Psychiatry 2006; 28(5): 367–373.
D’Souza, RA. A pilot study of an educational services for rural mental health practitioners in South Australia using telemedicine. Journal of Telemedicine and Telecare 2000; 6: 187–189.
Hilty, DM, Cobb, HC, Neufeld, JD, et al. Telepsychiatry reduces geographic physician disparity in rural settings, but is it financially feasible because of reimbursement. Psychiatric Clinics of North America 2008 Mar; 31(1): 85–94.
Larson, JC, Jacob, MK, Craighead, WE. Establishing a telepsychiatry consultation practice in rural Georgia for primary care physicians: A feasibility report. Clinical Pediatrics 2012; doi:10.1177/0009922812441671
Center for Medicaid and Medicare Services (CMA). The Balanced Budget Act of 1997: Pub 100–02 Medicare Benefit Policy. U.S. Department of Health &Human Services (DHHS), 1997. Available online at https://www.cms.gov/demoprojectsevalrpts/downloads/cc_section4016_bba_1997.pdf. Accessed on November 2, 2011.
Center for Medicaid and Medicare Services (CMA). Benefits Improvement Act of 2000. Medicare Carriers Manual, Part 3 - Claims Process Transmittal 1798 U.S. Department of Health &Human Services (DHHS), MAY 16, 2003. Available online at https://www.cms.gov/Transmittals/Downloads/R1798B3.pdf. Accessed November 3, 2011.
Centers for Medicare &Medicaid Services (CMS). The Medicare Patient and Physician Improvement Act of 2008. Pub 100–02 Medicare Benefit Policy Department of Health &Human Services (DHHS), 2008. Available online at https://www.cms.gov/transmittals/downloads/R140BP.pdf. Accessed November 10, 2011.
Participatory Politics Foundation. H.R. 6163 - Medicare Telehealth Enhancement Act of 2008. Available online at http://www.opencongress.org/bill/110-h6163/show
Telemedicine. Medicaid.gov website. Available online at http://www.medicaid.gov/Medicaid-CHIP-Program-Information/By-Topics/Delivery-Systems/Telemedicine.html. Accessed July 11, 2012.
Center for Substance Abuse Treatment (CSAT). Considerations for the Provision of E-Therapy. HHS Publication No. (SMA) 09–4450. Rockville, MD: Center for Substance Abuse Treatment, Substance Abuse and Mental Health Services Administration, 2009.
Rose, GL, Skelly, JM, Badger, GJ. Interactive voice response for relapse prevention following cognitive behavioral therapy for alcohol use disorders: A pilot study. Psychological Services May 2012; 9(2): 174–184. doi:10.1037/a0027606
Telemedicine Information Exchange. Available at: http://tie.telemed.org/default.asp. Accessed December 12, 2011.
Smith, HA, Allison, RA. Telemental health: Delivering mental health care at a distance. Unpublished summary report, U.S. Department of Health and Human Services, Office for the Advancement of Telehealth, Rockville, MD, 1998.
Rabinowitz, T, Brennan, DM, Chumbler, NR, et al. Telemedicine and e-Health. Psychiatric Services 2008; 14(9): 972–976. doi:10.1089/tmj.2008.0119.
Kennedy, C, Yellowlees, P. A community based approach to evaluation of health outcomes and costs for telepsychiatry in a rural population: preliminary results. Journal of Telemedicine and Telecare 2000; 6 Suppl 1:S155-7.
Horowitz, BT. Verizon Previews remote monitoring, telehealth platforms at mhealth summit. eWeek.com 2011Dec. 7.
Miller, W, Baca, C, Compton, W, et al. Addressing Substance Abuse in Health Care Settings. Alcoholism: Clinical and Experimental Research 2006; 30(2): 292–302.
Christopher P, Siemer BS, Fogel, J, et al. Telemental Health and Web-based Applications in Children and Adolescents Child and Adolescent Psychiatric Clinics of North America 2011 Jan; 20(1): 135–153.
James, LC, and Folen, RA. Behavioral Tele-health: Using Tele-medicine to Expand Behavioral Medicine Services. Journal of Healthcare Information Management 1999 Winter; 13(4): 15–23.
Doze S, Simpson J, Hailey D, Jacobs P. Evaluation of a telepsychiatry pilot project. Journal of Telemedicine and Telecare 1999; 5: 38–46.
García-Lizana, F, Muñoz-Mayorga, I. What about telepsychiatry? A systematic review. Primary Care Companion Journal of Clinical Psychiatry 2010; 12(2): e1-e5. doi:10.4088/PCC.09m00831whi
Saeed, A, Diamond, J, Bloch, R. Use of telepsychiatry to improve care for people with mental illness in rural North Carolina. North Carolina Medical Journal 2011; 72(3): 219–222.
Krupinski E, Nypaver M, Poropatich R, et al. Telemedicine/telehealth: an international perspective. Clinical applications in telemedicine/telehealth. Telemedicine Journal and E-Health 2002); 8(1): 13–34.
Farrell, SP, McKinnon CR. Technology and rural mental health. Archives Psychiatric of Nursing 2003; 17(1): 20–26.
Elford DR, White H, St John K, et al. A prospective satisfaction study and cost analysis of a pilot child telepsychiatry service in Newfoundland. Journal of Telemedicine and Telecare 2001; 7: 73–81.
Ermer DJ. Experience with a rural telepsychiatry clinic for children and adolescents Psychiatric Services 1999 Feb; 50(2): 260–1.
Myers KM, Valentine JM, Melzer SM. Child and adolescent telepsychiatry: utilization and satisfaction. Telemedicine and e-Health 2008 March; 14(2):131–7.
Palmer NB, Myers KM, Vander Stoep A, et al. Attention deficit/hyperactivity disorder and telemental health. Current Psychiatry Reports 2010 Oct; 12(5): 409–17.
Savin D, Garry MT, Zuccaro P, et al. Telepsychiatry for treating rural American Indian youth Journal of American Academy of Child and Adolescent Psychiatry 2006 Apr; 45(4): 484–8.
Greenberg, N, Boydell, KM, Volpe, T. Pediatric telepsychiatry in Ontario: caregiver and service provider perspectives. Journal of Behavioral Health Services 2006; 33: 105–111.
Elford R, White H, Bowering R, et al. A randomized, controlled trial of child psychiatric assessments conducted using videoconferencing. Journal of Telemedicine and Telecare 2000; 6: 73–82.
Kopel H, Nunn K, Dossetor D. Evaluating satisfaction with a child and adolescent psychological telemedicine outreach service. Journal of Telemedicine and Telecare 2001; 7: 35–40.
Pignateillo, A, Teshima, J, Boydell, KM, et al. Child telepsychiatry in rural and remote primary care. Child Adolescent Psychiatric Clinics of North America 2011; 20(1): 13–38.
Miller TW, Clark J, Veltkamp LJ, et al.: Teleconferencing model for forensic consultation, court testimony, and continuing education. Behavioral Sciences and the Law 2008; 26: 301–313.
Gelber, H: The experience in Victoria with telepsychiatry for the child and adolescent mental health service. Journal of Telemedicine and Telecare 2001; 7(Suppl 2): 32–34.
Gelber H, Alexander, M: An evaluation of an Australian videoconferencing project for child and adolescent telepsychiatry. Journal of Telemedicine and Telecare 1999, 5(Suppl 1): S21–S23.
Myers KM, Valentine JM, Melzer SM. Feasibility, acceptability, and sustainability of telepsychiatry for children and adolescents. Psychiatric Services 2007; 58: 1493–1496.
Telehealth in State Substance Use Disorder (SUD) Services. The National Association of State Alcohol and Drug Abuse Directors, Inc. (NASADAD), 2009. Available online at: http://www.tnpcaeducation.org/resourcelibrary/clinical/Telehealth%20in%20Substance%20Use%20Disorder%20Services%20Report%2009.pdf
King, VL, Stoller, KB, Kidorf, M, et al. Assessing the effectiveness of an internet-based videoconferencing platform for delivering intensified substance abuse counseling. Journal of Substance Abuse Treatment 2009 Apr; 36(3): 331–8.
Rohde, P, Lewinsohn, PM, Seeley, JR. Comparability of telephone and face-to-face interviews in assessing axis I and II disorders. American Journal of Psychiatry 1997; 154: 1593–1598.
Carlson LE, Lounsberry JJ, Maciejewski O, et al. Telehealth-delivered group smoking cessation for rural and urban participants: Feasibility and cessation rates. Addictive Behaviors 2012; 37(1): 108–114.
SAMHSA (Substance Abuse and Mental Health Services Administration). From the 2005 Drug and Alcohol Services Information System Report. Available online at http://wwwdasis.samhsa.gov/teds05/TEDSD2k5Chp3.htm. Accessed on May 17, 2011.
Copeland, J, Martin, G. Web‐based interventions for substance use disorders: A qualitative review. Journal of Substance Abuse Treatment 2004; 26(2): 109–116.
Washington State Provider Agencies Add Online Element to Services. Alcoholism and Drug Abuse Weekly. Available online at http://www.weinerpublic.com/page131.html. Accessed June 25, 2009.
Frueh, BC, Deitsch, SE, Santos, AB, et al. Procedural and methodological issues in telepsychiatry research and program development. Psychiatric Services 2000; 51: 1522–1527.
Hilty, DM, Marks, SL, Urness, D, et al. Clinical and educational telepsychiatry applications: A review. Canadian Journal of Psychiatry 2004; 49: 12–23.
Porcari, CE, Amdur, RL, Koch, EI, et al. Assessment of post-traumatic stress disorder in veterans by videoconferencing and by face-to-face methods. Journal of Telemedicine and Telecare 2009; 15: 89–94.
Morland, LA, Pierce, K, Wong, M. (in press). Telehealth and PSTD psychoeducation groups in the Pacific Islands: A feasibility study. Telehealth and Telecare.
Lange, A, Rietdijk, D, Hudcovicova, M, et al. Interapy: A controlled randomized trial of the standardized treatment of posttraumatic stress through the Internet. Journal of Consulting and Clinical Psychology 2003; 71(5): 901–909.
Brooks, E, Manson, S, Bair, B, et al. The diffusion of telehealth in rural American Indian Communities: A retrospective survey of key stakeholders. Telemedicine and E-Health 2012; 18(1): 60–66 doi:10.1089/tmj.2011.0076.
Brooks, E, Grinsby, J, Manson, SM, et al. Acceptability of telepsychiatry in American Indians. Telemedicine Journal of E-Health 2008; 14(5): 461–6.
Bair, B, Brooks, E, Dailey, N, et al. Review of American Indian veteran telemental health. Telemedicine Journal of E-Health 2012; 18(2): 87–94.
Yeung A, Hails K, Chang T, et al. A study of the effectiveness of telepsychiatry-based culturally sensitive collaborative treatment of depressed Chinese Americans. BMC Psychiatry 2011; 11: 154.
Gibson, K, O’Donnell, SD, Coulson, H, et al. Mental health professionals’ perspectives of telemental health with remote and rural First Nations communities. Journal of Telemedicine and Telecare 2011; (17): 263–267.
Wallace PG, Haines A, Harrison R, et al. Design and performance of a multicentre, randomized controlled trial of teleconsulting. Journal of Telemedicine and Telecare 2002; 8(Suppl 2): 94–5.
Dongier M, Tempier R, Lalinec-Michaud M, et al. Telepsychiatry: psychiatric consultation through two-way television. A controlled study. Canadian Journal of Psychiatry 1986; 31: 32–4.
American Tele-medicine Association. Evidence based practice for telemental health. Available online at http://www.americantelemed.org/files/public/standards/EvidenceBasedTelementalHealth_WithCover.pdf Accessed December 5, 2011.
Myers, K, Palmer, N, Geyer, J, Research in Child and Adolescent Telemental Health, Child and Adolescent Clinics of North America Volume 2011; 20(1): 155–171.
Acknowledgments
This study was made possible with funding from: Life Sciences Discovery Fund Authority, of the State of Washington; OGRD#109212, Roll, J. (PI)
Conflict of Interest
The authors of this work attest to having no conflicts of interest in the subject matter of this manuscript. Further, this work has not been previously published and is not currently being reviewed for publication elsewhere.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Benavides-Vaello, S., Strode, A. & Sheeran, B.C. Using Technology in the Delivery of Mental Health and Substance Abuse Treatment in Rural Communities: A Review. J Behav Health Serv Res 40, 111–120 (2013). https://doi.org/10.1007/s11414-012-9299-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11414-012-9299-6