Abstract
Antimicrobial resistance (AMR) has become a critical worldwide health crisis. It poses major challenges for healthcare systems across the globe, demanding immediate attention and action. Low and middle-income countries (LMICs), in particular, encounter unique obstacles in addressing AMR due to various factors. This article aims to examine specific challenges and propose effective strategies to combat this issue. Through a comprehensive review of existing literature, this article identifies common barriers and successful interventions in tackling AMR. The research highlights several challenges faced by LMICs in addressing AMR, including limited access to quality healthcare services, socioeconomic disparities, limited awareness, inadequate surveillance systems and data collection, limited regulatory frameworks and quality control, as well as weak healthcare infrastructure and infection prevention practices. The research suggests strategies like improving healthcare access, promoting responsible antimicrobial use, enhancing surveillance, ensuring quality antimicrobial drugs, and fostering global collaboration to address these challenges. By understanding the challenges encountered by LMICs, it is possible to mitigate the impact of AMR and contribute to global efforts in combating this growing threat.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Antimicrobial resistance (AMR) has presented itself an urgent global health crisis (Max et al. 2023) that jeopardizes the effectiveness of antimicrobial drugs and presents significant hurdles to achieve desired patient outcome by the healthcare service delivery systems worldwide (Rehman 2023). Low and middle-income countries (LMICs) face additional barriers to combating AMR due to limited resources, inadequate healthcare infrastructure, and a high incidence of infectious diseases (Ikhimiukor et al. 2022). It is critical to understand these challenges and develop effective strategies to mitigate the impact of this growing public health threat. In LMICs, higher incidences of infectious diseases are commonly observed due to factors like inadequate sanitation, limited access to clean water, overcrowding, and insufficient healthcare resources (Sulis et al. 2022). As a result, the use of antimicrobial drugs, such as antivirals, antibiotics, and antifungals, is widespread (Owoicho et al. 2021; Clement et al. 2020). Inappropriate prescription practices, easy availability of antimicrobials without proper regulation, and limited healthcare accessibility all contribute to the rise and spread of drug-resistant pathogens (Sharma et al. 2022).
Furthermore, various factors also considerably influence the use of antibiotics in LMICs, including poverty, limited education, and a lack of awareness regarding appropriate antimicrobial usage (Charani et al. 2023). These factors lead to self-medication, incomplete treatment courses, and substandard drug quality, contributing to selective pressure that drives the evolution of antimicrobial resistance (Kakkar et al. 2020). Furthermore, LMICs have challenges associated with healthcare infrastructure, such as restricted laboratory capacities, inadequate and fragmented surveillance systems, and an insufficient healthcare workforce (Iskandar et al. 2021; Asghar et al. 2020). However, the need for more reliable data concerning resistance patterns and trends hinders evidence-based decision-making and targeted interventions to effectively combat AMR. Strengthening healthcare systems, enhancing laboratory and surveillance capacities, and improving healthcare delivery are vital components in addressing AMR within these contexts.
This research describes the AMR in LMICs, considered their unique challenges, and identified effective strategies to combat this. Understanding the challenges LMICs face in tackling AMR is crucial for several reasons. Firstly, these countries are highly vulnerable to the effects of AMR and carry a disproportionate share of the global burden of infectious illnesses (Pulingam et al. 2022). Moreover, in LMICs, drug-resistant diseases can upset public health, leading to increased rates of mortality and morbidity and steep increases in healthcare expenses (Kapoor et al. 2023). Secondly, LMICs often need more resources and infrastructure to implement comprehensive AMR control programs (Hein et al. 2022). Therefore, policymakers and healthcare stakeholders would need to devise targeted interventions that are contextually appropriate and resource-sensitive by identifying challenges specific to these contexts. Furthermore, studying about the successful AMR control initiatives in LMICs can offer valuable lessons for other regions facing similar challenges. This would aid in identifying best practices, highlighting areas for improvement, and guiding the development of sustainable and practical strategies to combat AMR.
Challenges in addressing antimicrobial resistance in low and middle-income countries
Limited access to quality healthcare services
LMICs often face challenges in providing accessible and quality healthcare services to their populations. Inadequate healthcare infrastructure, including a shortage of healthcare facilities and a lack of essential medical equipment, restricts the timely and accurate diagnosis of infectious diseases (Chitungo et al. 2022). Without proper diagnostic tools and technologies, healthcare providers may face challenges in identifying the specific pathogens causing infections and determining the most effective treatment options. In addition, medical personnel such as physicians, nurses, and laboratory technicians are generally in short supply in LMICs (Dhingra et al. 2020). The limited healthcare workforce further compounds the difficulties in delivering quality care to a large population. Overworked healthcare providers may not have sufficient time to devote to each patient, resulting in rushed consultations and potentially inappropriate prescriptions of antimicrobial drugs (Ahmad and Khan 2019). This can contribute to the overuse, underuse, and misuse of these medications, fueling the emergence and spread of drug-resistant pathogens. In addition to infrastructure and workforce challenges, LMICs also face financial corruption and incompetence, making it difficult to invest in the necessary healthcare resources and technologies (Pokharel et al. 2019). Limited funding may restrict the availability and accessibility of essential diagnostic tools, such as microbiology laboratories and rapid diagnostic tests, which are crucial for the accurate and timely identification of drug-resistant infections (Ting et al. 2021).
Socioeconomic disparities and limited awareness
LMICs often face challenges in establishing robust surveillance systems for monitoring antimicrobial resistance. Poverty and limited education levels often result in a lack of understanding about the appropriate use of antimicrobials and the consequences of AMR (Sulis et al. 2022). As a result, individuals may resort to self-medication, obtaining antibiotics without a prescription, or not completing the full course of treatment, leading to inadequate dosing, and promoting the development of resistance.
In LMICs, the availability of substandard or counterfeit drugs is another concern. Due to limited access to regulated pharmacies and regulatory oversight, individuals may purchase medications from informal sources where the quality and authenticity of the drugs cannot be guaranteed (Sakeena et al. 2019; Samreen et al. 2021). Substandard or counterfeit drugs may contain suboptimal doses of active ingredients, leading to ineffective treatment and promoting drug resistance (Orubu et al. 2020).
Inadequate surveillance systems and data collection
LMICs encounter significant obstacles in establishing effective surveillance systems to monitor antimicrobial resistance (AMR). Limited laboratory capacities, inadequate data collection mechanisms, and a lack of standardized protocols contribute to the challenge of collecting and analyzing reliable data on resistance patterns and trends (Gandra et al. 2020). One of the primary challenges is the limited availability of well-equipped laboratories capable of conducting comprehensive AMR testing. LMICs often lack the necessary skilled personnel to perform accurate and timely antimicrobial susceptibility testing (Hoque et al. 2020). This results in a scarcity of data regarding the prevalence and resistance profiles of various pathogens circulating within the population. Insufficient data collection mechanisms further hinder efforts to track and monitor AMR. In many cases, there is a lack of standardized reporting systems, making it difficult to capture and consolidate data from various healthcare facilities and regions (Murray et al. 2022). Inconsistent data collection practices and inadequate integration of data across human, animal, and environmental health sectors limit the understanding of the complex dynamics of AMR transmission (Ukuhor 2021). The absence of standardized protocols for data collection, analysis, and reporting is another significant challenge. Without standardized procedures, comparing data across different regions or over time becomes challenging, hampering the ability to identify emerging trends and implement targeted interventions effectively.
Limited regulatory frameworks and quality control
It may be difficult for LMICs to establish comprehensive regulatory frameworks for manufacturing, distributing, and retailing antimicrobial medications. LMICs may face constraints in establishing regulatory agencies with the capacity to enforce stringent standards for the production, importation, and distribution of antimicrobials (Iwu et al. 2020). Therefore, low-quality medications not only fail to effectively treat infections but also contribute to the development of resistance. In some cases, the improper use of substandard antimicrobials can even worsen patients’ health conditions or result in adverse effects.
Weak healthcare infrastructure and infection prevention practices
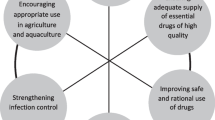
Inadequate supportive healthcare infrastructure is a common problem in LMICs (Fig. 1) (Lucien et al. 2021). Poor sanitation practices, including inadequate sewage systems and waste management, contribute to the dissemination of infectious agents in the community and healthcare settings. Healthcare-associated infections are more likely to occur when water supplies are contaminated, medical waste is not adequately disposed of, and no hygiene measures are in place (Elton et al. 2020). In addition, antimicrobial drug treatment is frequently necessary for these infections, which increases the risk of drug resistance.
Moreover, overcrowded healthcare facilities can impede effective infection control practices. Insufficient space, limited isolation facilities, and a high patient-to-staff ratio make it challenging to implement adequate measures to prevent the transmission of resistant pathogens (Wall 2019). In resource-constrained settings, healthcare providers may face difficulties in adhering to hand hygiene protocols, maintaining cleanliness, and implementing appropriate sterilization and disinfection practices. Limited resources further hinder infection prevention and control efforts (Maillard et al. 2020). LMICs may struggle to allocate funds for necessary infrastructure upgrades, training programs, and the procurement of essential supplies, such as personal protective equipment. Insufficient training and awareness among healthcare professionals about infection prevention practices can also contribute to the spread of resistant infections.
Strategies to address antimicrobial resistance in LMICs
Strengthening healthcare systems
When fighting antimicrobial resistance (AMR), strengthening healthcare systems in LMICs is essential. To begin, the standard and availability of medical care must be enhanced through financial investments in healthcare infrastructure. Upgrading healthcare facilities, expanding medical equipment and diagnostic capabilities, and ensuring a reliable supply of medicines are essential (Anderson et al. 2019). Additionally, healthcare workforce training plays a significant role in addressing AMR. Healthcare professionals must be equipped with the knowledge and skills to diagnose infections accurately, prescribe antibiotics judiciously, and effectively implement infection prevention and control measures (Land et al. 2018). Continuous education and training programs can enhance their capacity and awareness of AMR-related issues.
Equitable access to quality healthcare services is another critical aspect. Healthcare inequalities must be reduced, and universal access to primary medical care should be guaranteed in all areas of the world, including LMICs (Bloom and Cadarette 2019). This may involve improving healthcare infrastructure in underserved areas, implementing telemedicine initiatives, and developing strategies to make essential medicines affordable and accessible. By strengthening healthcare systems, LMICs can enhance their ability to prevent and control AMR effectively. This will contribute to better health outcomes and support global efforts to combat the rising threat of antimicrobial resistance.
Promoting antimicrobial stewardship
Implementing comprehensive antimicrobial stewardship programs can significantly contribute to the responsible use of antimicrobials and mitigate the development of resistance. A critical aspect of antimicrobial stewardship is promoting appropriate prescribing practices. Healthcare professionals must be educated about evidence-based treatment guidelines and encouraged to prescribe antibiotics only when necessary (Majumder et al. 2020). This includes proper diagnosis, selecting the right antibiotic, using the correct dosage and duration, and regularly reassessing the need for continued therapy. In addition, training programs and awareness campaigns can raise awareness about the risks of AMR, the consequences of inappropriate antibiotic use, and the importance of completing full treatment courses. Educating healthcare professionals about alternative treatment options, such as non-antibiotic therapies, can also help reduce unnecessary antibiotic prescriptions.
Establishing guidelines and protocols for treatment and prescription practices is another essential component of antimicrobial stewardship. LMICs should work towards implementing national or local guidelines that provide clear recommendations on antimicrobial use, including specific indications, dosages, and treatment durations (Kpokiri et al. 2020). These guidelines can be a reference for healthcare professionals and promote standardized, evidence-based practices. Public awareness campaigns play a vital role in promoting responsible antimicrobial use. By educating communities about AMR, the importance of proper hygiene practices, and the consequences of self-medication, these campaigns can empower individuals to make informed decisions about their health and reduce the demand for unnecessary antibiotics.
Enhancing surveillance and data collection
LMICs should focus on strengthening their surveillance systems for AMR (Fig. 1). Strengthening surveillance systems allows for the timely detection and monitoring of resistance patterns, enabling effective response strategies. Investing in laboratory capacities is crucial for accurate and reliable data collection. LMICs should prioritize improving laboratory infrastructure, including equipment, personnel training, and quality assurance systems (Hendriksen et al. 2019). Well-equipped laboratories enable identifying and characterizing resistant pathogens, providing essential information for targeted interventions. Standardized data collection, analysis, and reporting protocols are necessary to ensure consistency and comparability of surveillance data. LMICs should establish guidelines outlining methods for collecting and analyzing antimicrobial resistance data. This standardization allows for effective comparisons within the country and across different regions, facilitating the identification of emerging resistance trends (Stewardson et al. 2019).
Integration of surveillance efforts across human, animal, and environmental health sectors is also essential. Like many other diseases, AMR can be spread between people, animals, and the environment. LMICs should strive for a One Health approach, fostering collaboration and data sharing among sectors (Frost et al. 2019). This integrated approach enables a comprehensive understanding of the drivers of AMR and supports the development of holistic interventions. Timely and accurate data are critical for evidence-based decision-making. Surveillance data provide crucial information for policymakers, healthcare providers, and researchers to assess the magnitude of the AMR problem, identify high-risk areas, and design targeted interventions (Fadare et al. 2019). Strengthening surveillance systems empowers countries to take proactive measures to combat AMR effectively.
Improving access to quality-assured antimicrobial drugs
In the fight against AMR, people in LMICs must have access to antimicrobial medications that are both inexpensive and of high enough quality to prevent unnecessary suffering. However, LMICs must first establish effective regulatory frameworks to regulate antimicrobial drug production, distribution, and sale. Strengthening regulatory agencies and implementing stringent standards can help prevent the availability of substandard or counterfeit medications in the market (Kamere et al. 2022). In addition, quality control measures play a crucial role in maintaining the efficacy of antimicrobial drugs. Therefore, LMICs should prioritize establishing quality control systems to ensure all medications meet the necessary standards. This includes rigorous testing of active ingredients, adherence to proper manufacturing processes, and regular inspections of production facilities. By improving quality control mechanisms, LMICs can enhance the availability of effective antimicrobial drugs and reduce the risk of promoting drug resistance through substandard or counterfeit medications (Charani et al. 2023).
Collaboration with international organizations and manufacturers is vital in improving drug affordability and availability. LMICs can work closely with pharmaceutical companies and international bodies to negotiate fair pricing agreements and access affordable generic versions of essential antimicrobial drugs. Joint efforts can also be made to improve the supply chain and distribution networks, ensuring a steady and reliable availability of quality-assured drugs in remote and underserved areas (Iriti et al. 2020). Furthermore, capacity-building initiatives can be established to enhance local manufacturing capabilities and promote the production of high-quality antimicrobial drugs within LMICs. By investing in research and development, knowledge transfer, and technology transfer, LMICs can reduce their reliance on imported medications and build self-sufficiency in meeting their healthcare needs (Kakooza et al. 2023).
Fostering international collaboration and support
Addressing AMR challenges requires the collective efforts of international organizations, governments, and stakeholders to provide the necessary resources and expertise. Financial assistance is essential for LMICs to strengthen their healthcare systems, invest in laboratory infrastructure, and implement comprehensive AMR programs (Blaskovich 2020). International organizations and donor countries should allocate resources specifically for AMR-related initiatives in LMICs, enabling them to enhance their capacities and implement effective strategies. Technical expertise and capacity-building initiatives are also critical.
Moreover, LMICs can benefit from partnerships with more advanced healthcare systems and international organizations that can provide training, mentorship, and guidance on best practices in AMR prevention and control (Khalifa et al. 2019). These initiatives can empower LMICs’ healthcare professionals, researchers, and policymakers to develop and implement evidence-based interventions. By learning from each other’s experiences, LMICs can avoid duplicating efforts, optimize resources, and accelerate progress in addressing AMR (Krockow and Tarrant 2019).
Conclusion
This research emphasizes the critical need to recognize and address the unique obstacles LMICs face in the fight against antimicrobial resistance (AMR). LMICs can effectively address AMR and safeguard public health by strengthening the identified strategies and minimizing contributing factors. Moreover, policymakers, healthcare providers, researchers, and international organizations must prioritize and allocate resources toward sustainable interventions. By doing so, it is achievable to collectively mitigate the impact of AMR, protect vulnerable populations, and ensure the long-term effectiveness of antimicrobial drugs.
Abbreviations
- AMR:
-
antimicrobial resistance
- LMICs:
-
low and middle-income countries
References
Ahmad M, Khan AU (2019) Global economic impact of antibiotic resistance: a review. J Glob Antimicrob Resist 19:313–316. https://doi.org/10.1016/j.jgar.2019.05.024
Anderson M, Schulze K, Cassini A, Plachouras D, Mossialos E (2019) A governance framework for development and assessment of national action plans on antimicrobial resistance. Lancet Infect Dis 19(11):e371–e384. https://doi.org/10.1016/S1473-3099(19)30415-3
Asghar S, Atif M, Mushtaq I, Malik I, Hayat K, Babar Z-U-D (2020) Factors associated with inappropriate dispensing of antibiotics among non-pharmacist pharmacy workers. Res Soc Adm Pharm 16(6):805–811. https://doi.org/10.1016/j.sapharm.2019.09.003
Blaskovich MAT (2020) Antibiotics special issue: challenges and opportunities in antibiotic discovery and development. ACS Infect Dis 6(6):1286–1288. https://doi.org/10.1021/acsinfecdis.0c00331
Bloom DE, Cadarette D (2019) Infectious disease threats in the twenty-first century: strengthening the global response. Front Immunol 10:549. https://doi.org/10.3389/fimmu.2019.00549
Charani E, Mendelson M, Pallett SJC, Ahmad R, Mpundu M, Mbamalu O, Bonaconsa C, Nampoothiri V, Singh S, Peiffer-Smadja N, Anton-Vazquez V, Moore LSP, Schouten J, Kostyanev T, Vlahović-Palčevski V, Kofteridis D, Corrêa JS, Holmes AH (2023) An analysis of existing national action plans for antimicrobial resistance—Gaps and opportunities in strategies optimising antibiotic use in human populations. Lancet Global Health 11(3):e466–e474. https://doi.org/10.1016/S2214-109X(23)00019-0
Chitungo I, Dzinamarira T, Nyazika TK, Herrera H, Musuka G, Murewanhema G (2022) Inappropriate antibiotic use in Zimbabwe in the COVID-19 era: a perfect recipe for antimicrobial resistance. Antibiotics 11(2):244. https://doi.org/10.3390/antibiotics11020244
Clement M, Olabisi M, David E, Issa M (2020) Veterinary pharmaceuticals and antimicrobial resistance in developing countries. In: Oppong Bekoe S, Saravanan M, Kwame Adosraku R, Ramkumar PK (eds) Veterinary Medicine and Pharmaceuticals. IntechOpen. https://doi.org/10.5772/intechopen.84888
Dhingra S, Rahman NAA, Peile E, Rahman M, Sartelli M, Hassali MA, Islam T, Islam S, Haque M (2020) Microbial resistance movements: an overview of global public health threats posed by antimicrobial resistance, and how best to counter. Front Public Health 8:535668. https://doi.org/10.3389/fpubh.2020.535668
Elton L, Thomason MJ, Tembo J, Velavan TP, Pallerla SR, Arruda LB, Vairo F, Montaldo C, Ntoumi F, Abdel Hamid MM, Haider N, Kock R, Ippolito G, Zumla A, McHugh TD, the PANDORA-ID-NET consortium (2020) Antimicrobial resistance preparedness in sub-Saharan African countries. Antimicrob Resist Infect Control 9(1):145. https://doi.org/10.1186/s13756-020-00800-y
Fadare JO, Ogunleye O, Iliyasu G, Adeoti A, Schellack N, Engler D, Massele A, Godman B (2019) Status of antimicrobial stewardship programmes in Nigerian tertiary healthcare facilities: findings and implications. J Glob Antimicrob Resist 17:132–136. https://doi.org/10.1016/j.jgar.2018.11.025
Frost I, Van Boeckel TP, Pires J, Craig J, Laxminarayan R (2019) Global geographic trends in antimicrobial resistance: the role of international travel. J Travel Med 26(8):taz036. https://doi.org/10.1093/jtm/taz036
Gandra S, Alvarez-Uria G, Turner P, Joshi J, Limmathurotsakul D, Van Doorn HR (2020) Antimicrobial resistance surveillance in low- and middle-income countries: progress and challenges in eight south Asian and Southeast Asian countries. Clin Microbiol Rev 33(3):e00048. https://doi.org/10.1128/CMR.00048-19
Hein W, Aglanu LM, Mensah-Sekyere M, Harant A, Brinkel J, Lamshöft M, Lorenz E, Eibach D, Amuasi J (2022) Fighting antimicrobial resistance: development and implementation of the Ghanaian National Action Plan (2017–2021). Antibiotics 11(5):613. https://doi.org/10.3390/antibiotics11050613
Hendriksen RS, Munk P, Njage P, Van Bunnik B, McNally L, Lukjancenko O, Röder T, Nieuwenhuijse D, Pedersen SK, Kjeldgaard J, Kaas RS, Clausen PTLC, Vogt JK, Leekitcharoenphon P, Van De Schans MGM, Zuidema T, De Roda Husman AM, Rasmussen S, Petersen B, Aarestrup FM (2019) Global monitoring of antimicrobial resistance based on metagenomics analyses of urban sewage. Nature Commun 10(1):1124. https://doi.org/10.1038/s41467-019-08853-3
Hoque R, Ahmed SM, Naher N, Islam MA, Rousham EK, Islam BZ, Hassan S (2020) Tackling antimicrobial resistance in Bangladesh: a scoping review of policy and practice in human, animal and environment sectors. PLoS One 15(1):e0227947. https://doi.org/10.1371/journal.pone.0227947
Ikhimiukor OO, Odih EE, Donado-Godoy P, Okeke IN (2022) A bottom-up view of antimicrobial resistance transmission in developing countries. Nat Microbiol 7(6):757–765. https://doi.org/10.1038/s41564-022-01124-w
Iriti M, Vitalini S, Varoni EM (2020) Humans, animals, food and environment: one health approach against global antimicrobial resistance. Antibiotics 9(6):346. https://doi.org/10.3390/antibiotics9060346
Iskandar K, Molinier L, Hallit S, Sartelli M, Hardcastle TC, Haque M, Lugova H, Dhingra S, Sharma P, Islam S, Mohammed I, Naina Mohamed I, Hanna PA, Hajj SE, Jamaluddin NAH, Salameh P, Roques C (2021) Surveillance of antimicrobial resistance in low- and middle-income countries: a scattered picture. Antimicrob Resist Infect Control 10(1):63. https://doi.org/10.1186/s13756-021-00931-w
Iwu CD, Korsten L, Okoh AI (2020) The incidence of antibiotic resistance within and beyond the agricultural ecosystem: a concern for public health. MicrobiologyOpen 9(9). https://doi.org/10.1002/mbo3.1035
Kakkar AK, Shafiq N, Singh G, Ray P, Gautam V, Agarwal R, Muralidharan J, Arora P (2020) Antimicrobial stewardship programs in resource constrained environments: understanding and addressing the need of the systems. Front Public Health 8:140. https://doi.org/10.3389/fpubh.2020.00140
Kakooza F, Kiggundu R, Mboowa G, Kateete PD, Nsangi OT, Kabahita JM, Ssentalo Bagaya B, Golparian D, Unemo M (2023) Antimicrobial susceptibility surveillance and antimicrobial resistance in Neisseria gonorrhoeae in Africa from 2001 to 2020: a mini-review. Front Microbiol 14:1148817. https://doi.org/10.3389/fmicb.2023.1148817
Kamere N, Garwe ST, Akinwotu OO, Tuck C, Krockow EM, Yadav S, Olawale AG, Diyaolu AH, Munkombwe D, Muringu E, Muro EP, Kaminyoghe F, Ayotunde HT, Omoniyei L, Lawal MO, Barlatt SHA, Makole TJ, Nambatya W, Esseku Y, Ashiru-Oredope D (2022) Scoping review of national antimicrobial stewardship activities in eight African countries and adaptable recommendations. Antibiotics 11(9):1149. https://doi.org/10.3390/antibiotics11091149
Kapoor D, Garg D, Beriwal N, Sidharth, Kumar A, Mukherjee SB, Pemde HK, Sharma S (2023) Clinico-etiologic profile of children and adolescents with drug-resistant epilepsy in a low-resource setting: 10 years’ experience. J Child Neurol 088307382311744. https://doi.org/10.1177/08830738231174493
Khalifa HO, Soliman AM, Ahmed AM, Shimamoto T, Nariya H, Matsumoto T, Shimamoto T (2019) High prevalence of antimicrobial resistance in gram-negative bacteria isolated from clinical settings in Egypt: recalling for judicious use of conventional antimicrobials in developing nations. Microb Drug Resist 25(3):371–385. https://doi.org/10.1089/mdr.2018.0380
Kpokiri EE, Taylor DG, Smith FJ (2020) Development of antimicrobial stewardship programmes in low and middle-income countries: a mixed-methods study in Nigerian hospitals. Antibiotics 9(4):204. https://doi.org/10.3390/antibiotics9040204
Krockow EM, Tarrant C (2019) The international dimensions of antimicrobial resistance: contextual factors shape distinct ethical challenges in South Africa, Sri Lanka and the United Kingdom. Bioethics 33(7):756–765. https://doi.org/10.1111/bioe.12604
Land KJ, Boeras DI, Chen X-S, Ramsay AR, Peeling RW (2018) Reassured diagnostics to inform disease control strategies, strengthen health systems and improve patient outcomes. Nat Microbiol 4(1):46–54. https://doi.org/10.1038/s41564-018-0295-3
Lucien MAB, Canarie MF, Kilgore PE, Jean-Denis G, Fénélon N, Pierre M, Cerpa M, Joseph GA, Maki G, Zervos MJ, Dely P, Boncy J, Sati H, Rio AD, Ramon-Pardo P (2021) Antibiotics and antimicrobial resistance in the COVID-19 era: perspective from resource-limited settings. Int J Infect Dis 104:250–254. https://doi.org/10.1016/j.ijid.2020.12.087
Maillard J-Y, Bloomfield SF, Courvalin P, Essack SY, Gandra S, Gerba CP, Rubino JR, Scott EA (2020) Reducing antibiotic prescribing and addressing the global problem of antibiotic resistance by targeted hygiene in the home and everyday life settings: a position paper. Am J Infect Control 48(9):1090–1099. https://doi.org/10.1016/j.ajic.2020.04.011
Majumder MAA, Singh K, Hilaire MG-S, Rahman S, Sa B, Haque M (2020) Tackling antimicrobial resistance by promoting antimicrobial stewardship in medical and allied health professional curricula. Expert Rev Anti-Infect Ther 18(12):1245–1258. https://doi.org/10.1080/14787210.2020.1796638
Max BL, Angolile CM, Raymond VG, Mashauri HL (2023) The dawn of repurposing vitamins as potential novel antimicrobial agents: a call for global emergency response amidst AMR crisis. Health Sci Rep 6(5):e1276. https://doi.org/10.1002/hsr2.1276
Murray CJL, Ikuta KS, Sharara F, Swetschinski L, Robles Aguilar G, Gray A, Han C, Bisignano C, Rao P, Wool E, Johnson SC, Browne AJ, Chipeta MG, Fell F, Hackett S, Haines-Woodhouse G, Kashef Hamadani BH, Kumaran EAP, McManigal B, Naghavi M (2022) Global burden of bacterial antimicrobial resistance in 2019: a systematic analysis. The Lancet 399(10325):629–655. https://doi.org/10.1016/S0140-6736(21)02724-0
Orubu ESF, Zaman MH, Rahman MT, Wirtz VJ (2020) Veterinary antimicrobial resistance containment in Bangladesh: evaluating the national action plan and scoping the evidence on implementation. J Glob Antimicrob Resist 21:105–115. https://doi.org/10.1016/j.jgar.2019.09.020
Owoicho O, Tapela K, Djomkam Zune AL, Nghochuzie NN, Isawumi A, Mosi L (2021) Suboptimal antimicrobial stewardship in the COVID-19 era: is humanity staring at a postantibiotic future? Future Microbiol 16(12):919–925. https://doi.org/10.2217/fmb-2021-0008
Pokharel S, Raut S, Adhikari B (2019) Tackling antimicrobial resistance in low-income and middle-income countries. BMJ Glob Health 4(6):e002104. https://doi.org/10.1136/bmjgh-2019-002104
Pulingam T, Parumasivam T, Gazzali AM, Sulaiman AM, Chee JY, Lakshmanan M, Chin CF, Sudesh K (2022) Antimicrobial resistance: prevalence, economic burden, mechanisms of resistance and strategies to overcome. Eur J Pharm Sci 170:106103. https://doi.org/10.1016/j.ejps.2021.106103
Rehman S (2023) A parallel and silent emerging pandemic: antimicrobial resistance (AMR) amid COVID-19 pandemic. J Infect Public Health 16(4):611–617. https://doi.org/10.1016/j.jiph.2023.02.021
Sakeena MHF, Bennett AA, Carter SJ, McLachlan AJ (2019) A comparative study regarding antibiotic consumption and knowledge of antimicrobial resistance among pharmacy students in Australia and Sri Lanka. PLoS One 14(3):e0213520. https://doi.org/10.1371/journal.pone.0213520
Samreen Ahmad I, Malak HA, Abulreesh HH (2021) Environmental antimicrobial resistance and its drivers: a potential threat to public health. J Glob Antimicrob Resist 27:101–111. https://doi.org/10.1016/j.jgar.2021.08.001
Sharma A, Singh A, Dar MA, Kaur RJ, Charan J, Iskandar K, Haque M, Murti K, Ravichandiran V, Dhingra S (2022) Menace of antimicrobial resistance in LMICs: current surveillance practices and control measures to tackle hostility. J Infect Public Health 15(2):172–181. https://doi.org/10.1016/j.jiph.2021.12.008
Stewardson AJ, Marimuthu K, Sengupta S, Allignol A, El-Bouseary M, Carvalho MJ, Hassan B, Delgado-Ramirez MA, Arora A, Bagga R, Owusu-Ofori AK, Ovosi JO, Aliyu S, Saad H, Kanj SS, Khanal B, Bhattarai B, Saha SK, Uddin J, Harbarth S (2019) Effect of carbapenem resistance on outcomes of bloodstream infection caused by Enterobacteriaceae in low-income and middle-income countries (PANORAMA): a multinational prospective cohort study. Lancet Infect Dis 19(6):601–610. https://doi.org/10.1016/S1473-3099(18)30792-8
Sulis G, Sayood S, Gandra S (2022) Antimicrobial resistance in low- and middle-income countries: current status and future directions. Expert Rev Anti-Infect Ther 20(2):147–160. https://doi.org/10.1080/14787210.2021.1951705
Ting DSJ, Ho CS, Deshmukh R, Said DG, Dua HS (2021) Infectious keratitis: an update on epidemiology, causative microorganisms, risk factors, and antimicrobial resistance. Eye 35(4):1084–1101. https://doi.org/10.1038/s41433-020-01339-3
Ukuhor HO (2021) The interrelationships between antimicrobial resistance, COVID-19, past, and future pandemics. J Infect Public Health 14(1):53–60. https://doi.org/10.1016/j.jiph.2020.10.018
Wall S (2019) Prevention of antibiotic resistance – an epidemiological scoping review to identify research categories and knowledge gaps. Glob Health Action 12(sup1):1756191. https://doi.org/10.1080/16549716.2020.1756191
Author information
Authors and Affiliations
Contributions
Moustaq Karim Khan Rony was involved in the conception and design of the study. Moustaq Karim Khan Rony and Priyanka Das Sharmi were involved in drafting the manuscript or revising it critically for important intellectual content. Moustaq Karim Khan Rony, Priyanka Das Sharmi, Hasnat M. Alamgir were involved in the final approval of the version to be published, and each author participated sufficiently in the work to take public responsibility for appropriate portions of the content. Moustaq Karim Khan Rony and Hasnat M. Alamgir are accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Ethics declarations
Consent for publication
We give full consideration for publication and participate.
Conflict of interest
The authors declare no competing interests.
Additional information
Responsible Editor: Diane Purchase
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Rony, M.K.K., Sharmi, P.D. & Alamgir, H.M. Addressing antimicrobial resistance in low and middle-income countries: overcoming challenges and implementing effective strategies. Environ Sci Pollut Res 30, 101896–101902 (2023). https://doi.org/10.1007/s11356-023-29434-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-023-29434-4