Abstract
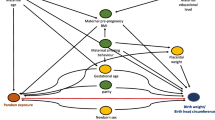
Parabens are a group of antimicrobial preservatives applied in an extensive range of products and are suspected to impair fetal growth because of their disrupting effect on the endocrine system. We aimed to examine maternal urinary paraben concentrations and their neonates’ outcome indexes. Methylparaben (MP), ethylparaben (EP), propylparaben (PP), and butylparaben (BP) concentrations were measured in 105 maternal urine samples collected before delivery. Length, weight, and head circumference at birth were extracted from the mothers’ delivery files. A multivariable linear regression analysis was performed to evaluate the association between paraben levels and neonatal anthropometric indices. The median levels of urinary parabens, especially BP, were higher than those in other countries. Prenatal urinary concentration of MP and BP showed a significantly positive association with birth weight in all neonates (β = 0.79, 95% CI: 0.16, 1.41, and β = 8.56, 95% CI: 3.95, 13.17, respectively), while these chemicals showed a significant negative association with head circumference (β = − 0.002, 95% CI: − 0.004, − 0.000, and β = − 0.016, 95% CI: − 0.030, − 0.002, respectively). A significant positive association between MP and birth length was also found (β = 0.004, 95% CI: 0.00, 0.00) in all the neonates. In sex-stratified adjusted models, MP and BP were found to be associated, respectively, with higher birth length and weight in male neonates (β = 0.008, 95% CI: − 0.001, 0.017, and β = 7.948, 95% CI: 1.045, 14.851). In girls, maternal urinary MP, PP, and BP were associated with increased birth weight (β = 0.831, 95% CI: 0.043, 1.620; β = 4.178, 95% CI: 0.877, 7.480; and β = 10.821, 95% CI: 3.545, 18.097, respectively), and MP and BP were associated with reduced head circumference at birth (β = − 0.003, 95% CI: − 0.005, − 0.001, and β = − 0.035, 95% CI: − 0.055, − 0.016). These results revealed potential impacts between neonatal growth and maternal exposure to parabens. However, these findings should be interpreted while considering the limitations of the present study.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Parabens are a group of alkyl esters of para-hydroxybenzoic acid utilized as antimicrobial preservatives in numerous consumer products such as foodstuffs, personal care products (PCPs), and medications (Andersen 2008; Giulivo et al. 2016). Humans can be exposed to these compounds via different ways, including continuous oral intake, dermal absorption, and inhalation (Soni et al. 2005). Generally, most of the parabens are promptly absorbed, conjugated, and excreted through urine after exposure (Boberg et al. 2010). Biomonitoring can be used as one of the methods to estimate the cumulative exposure of humans to pollutants (Cowan-Ellsberry and Robison 2009). Various studies have been conducted to monitor the urinary concentration of different environmental chemicals like PAHs, BTEX, and parabens, among the population of different countries (Honda et al. 2018; Kiani Feizabadi et al. 2020a; Ma et al. 2013; Moridzadeh et al. 2020; Shahsavani et al. 2017) Therefore, the amount of urinary parabens has been found to be an appropriate and valid biomarker of exposure. In human and animal studies, estrogenic activities have been reported for paraben compounds, and therefore, these compounds have been categorized as endocrine-disrupting chemicals (EDCs) (Koeppe et al. 2013; Oishi 2002; Routledge et al. 1998). Exposure to EDCs has been linked to various adverse health effects, including an increased risk of metabolic syndrome (Giulivo et al. 2016) and breast cancer (Darbre et al. 2004; Harvey and Everett 2012; Pan et al. 2015), changes in various reproductive hormone levels (Meeker et al. 2010; Zhang et al. 2014), and adverse pregnancy outcomes (Aker et al. 2019; Darbre and Harvey 2008; Philippat et al. 2019). Numerous studies have reported the presence of paraben compounds in various human biological samples, including cord blood, urine, breast milk, placental tissues, and amniotic fluid (Giulivo et al. 2016; Hajizadeh et al. 2020b; Smith et al. 2012; Vernet et al. 2018), indicating that parabens could be transmitted to the fetus through the placenta; thus, the fetus is regularly exposed to parabens and their adverse side effects. Therefore, the outcomes of paraben exposure in maternal and their newborns should be evaluated (Zhao et al. 2017). Previous studies in China and the USA revealed an inverse association between maternal urinary levels of parabens and neonatal anthropometric indicators (Geer et al. 2017; Wu et al. 2017). Moreover, the finding of another study demonstrated a negative relationship between exposure to prenatal parabens and neonatal as well as childhood growth (Wu et al. 2018). On the contrary, in a study conducted in France, prenatal urinary levels of parabens indicated a positive association with weight at birth (Philippat et al. 2014). Likewise, a previous study has reported a significant positive correlation between the parabens’ urinary amount in pregnant women and their neonates (Kang et al. 2013). However, some studies have reported a null association (Ferguson et al. 2018; Messerlian et al. 2018).
According to the results of two recent systematic reviews, no consensus has been achieved about pregnant mothers’ exposure to parabens and birth outcomes such as head size, birth weight, and body length (Jamal et al. 2019; Zhong et al. 2020). Because of extensive usage of PCPs and the absence of adequate epidemiological research, some researchers are trying to provide epidemiological information regarding the effects of paraben compounds in the human body and their serious outcomes on neonatal anthropometric parameters. Thus, the present study was carried out to determine the relationship between neonatal outcomes and maternal paraben exposure in the Iranian population. The distributions of estrogen receptors may vary by child sex (Gillies and McArthur 2010); thereby, the estrogenic effects may also act in a sex-dependent manner. Similarly, the reproductive and developmental effects of paraben exposures may differ by sex (Dodge et al. 2015). In some of the previous studies, associations have been observed between exposure to parabens and anthropometric measures in sex-stratified models (Fadaei et al. 2020; Philippat et al. 2012); we also performed a sex-stratified analysis.
Material and methods
Study participants and questionnaires
This cross-sectional research was performed on 105 pregnant women aged 18–45 years living in Isfahan Province, Iran. Some parts of the information were collected from people who participated in our previous research (Hajizadeh et al. 2020a), although the present study dataset is considerably different. The aim and methods of the research were explained to all the participants, and assigned consent letter was received from them. This study was conducted upon the approval of the Ethics Committees of Isfahan University of Medical Sciences. The study population was randomly selected from those who attended health centers for pregnancy care in various parts of the city of Isfahan. The inclusion criteria were pregnant women residing in the area for at least 1 year, being in the third trimester of pregnancy, and age > 18 years old. The exclusion criteria were insufficient urine samples, congenital anomalies, stillbirth, twins, any specific medical complications (diabetes, hypertension, etc.), and incomplete information. Information regarding pregnancy, maternal health, demographics, lifestyles, and anthropometric variables had been acquired from medical records and questionnaires previously. Information regarding neonatal anthropometric indices, including head circumference, weight, and length, was extracted from delivery files. After excluding the cases, 105 mother-infant pairs were finally included in this study.
Paraben exposure assessment
In the third trimester, spot urine samples were collected in polypropylene specimen cups and transferred to the laboratory of Isfahan University of Medical Sciences based on the cold chain status, and then frozen at − 80 °C until analysis. The overall concentration of paraben compounds (free and conjugated), including MP, EP, PP, and BP in urine samples, was determined via the dispersion and liquid-liquid microextraction (DLLME) method by gas chromatography–mass spectrometry (GC-MS) (Hajizadeh et al. 2020a,b; Kiani Feizabadi et al. 2020a). In brief, 50 μl of the beta-glucuronidase enzyme was mixed with 1 ml of each urine sample and incubated at 37 °C for 24 h to determine the total concentration of parabens. Afterward, 0.1 g of sodium chloride was added to the obtained mixture and centrifuged for 5 min (sediment settling). The supernatant was decanted and used for the extraction of parabens by the DLLME method. Accordingly, a mixture of 30 μl chlorobenzene and 500 μl of acetone was quickly added to the previously collated supernatants to produce a cloudy state. Next, the obtained cloudy solution was centrifuged at 5000 rpm for 5 min to sediment the finely dispersed droplets. For each sample, the sediment was withdrawn from the tube by a 50-μm micro-syringe, and collected in another vial, and dried under a slow stream of nitrogen gas. Thereafter, 20 μl of MSTFA was added to the sediment and centrifuged to obtain a complete mixture. Finally, 2 μl of the solution was injected into the GC/MS to analyze the parabens. The device calibration curves were drawn for parabens at the concentration of 0.01–1000 ng/ml. The quality assurance and quality control (QA/QC) were applied to ensure the precision and reliability of the obtained results. To ensure the accuracy of the analytical method, quality control (QC) samples along with blank and spiked samples (prepared from pooled human urine) were analyzed. The recovery of the spiked samples was > 89% for all analytes. Moreover, the regression coefficients (R2) with high accuracy (8.4% ≥ RSD) for MP, EP, PP, and BP were 0.994, 0.989, 0.992, and 0.999, respectively. Limit of detection (LOD) and limit of quantification (LOQ) of parabens were determined based on the lowest acceptable point on the calibration curve with a signal-to-noise ratio of 3 and 10, respectively, from the replicate analysis (n = 05) of standard solution at a concentration of 10 ng/ml. LOQs were 0.05 μg/l for MP, EP, and PP and 0.15 μg/l for BP. The LODs for MP, EP, PP, and BP were 0.014, 0.015, 0.016, and 0.046 μg/l, respectively. To adjust the variability of urinary dilution, the amount of urinary creatinine was determined by an automatic chemical analyzer (704auto-analysis, Hitachi, Japan).
Statistical analysis
For statistical analyses, a half of the limit of detection (LOD) was considered for the paraben concentration values which were below LOD (Hajizadeh et al. 2020b; Kiani Feizabadi et al. 2020a). Furthermore, because of the skewed distribution of the urinary paraben concentrations, the natural logarithm (ln) transformation of paraben concentrations was used to achieve a normal distribution. Descriptive statistics were utilized for the participants’ characteristics, the urinary paraben concentrations, and the birth outcomes. Pearson’s correlation analysis was applied to examine the correlations among urinary levels of parabens. Multivariable linear regression models were also utilized to evaluate the association between maternal prenatal paraben concentrations and anthropometric measures (birth length, weight, and head circumference). Besides the crude model, a confounder adjusted model was also fitted. The potential variables as confounders such as maternal age (continuous), maternal pre-pregnancy body mass index (BMI; continuous), maternal education (≤ high school diploma, high school diploma, > high school diploma), gestational age (days), parity, maternal passive smoking status (ever/never), income level, and infant sex (male and female) were entered in the adjusted model (Model 2) as some previous studies had suggested (Jamal et al. 2019). Due to birth weight variations with regard to the season, and due to the potential for seasonal variation in the consumption of PCPs along with the change of seasons and, therefore, changes in urinary parabens, we adjusted the season of birth in the models of birth weight (Messerlian et al. 2018). Moreover, the head circumference model was adjusted by the type of delivery, and the birth length model by mothers’ height (vaginal/cesarean section). Some prenatal parameters (e.g., smoking) are significant in early delivery, but the relationship between paraben exposure and gestational age is still unknown. Thus, gestational age was not considered as an intermediate variable. According to the literature, gestational age is an effective variable on birth outcomes (MacKenzie et al. 2019) and, therefore, it was adjusted in Model 2. Additionally, as a sensitivity analysis, Model 3 was adjusted for all the mentioned confounder variables except for gestational age. For each of the parabens, separate models were performed. In some earlier research, associations were found between EDC exposure and birth length, weight, and head circumference in sex-stratified models (Philippat et al. 2012; Wolff et al. 2008); given the hormonally active nature of parabens, we further evaluated the associations between urinary levels of parabens and anthropometric measures stratified by infant sex. Data analyses were performed in SPSS 20 software (SPSS Inc., Chicago, IL). All the tests were two-tailed, and a p value < 0.05 was considered statistically significant.
Results
Table 1 presents the sociodemographic characteristics of the participants (mothers and infants). The mean maternal age was 33.9 ± 8.4 (ranging from 18 to 45). Among the pregnant women, 43.8% were primiparous, and around 80% completed education at high school or higher. Approximately two thirds (68.5%) of the females were included in the overweight pre-pregnancy BMI group, and 78.1% of the participants were passive smokers during pregnancy. Of the 105 single live births, 56 (53.3%) were girls. The mean (± SD) gestational age was 38.8 ± 1.5 weeks, the mean birth weight was 3176 ± 516 g, the mean birth length was 50.1 ± 3.7 cm, and the mean head circumference was 34.5 ± 1.5 cm.
The creatinine-adjusted and unadjusted maternal urinary paraben concentrations are summarized in Table 2. As expected, exposure to paraben compounds was prevalent. The detection range of parabens in urinary samples of females was 86%–100%. The creatinine-adjusted means of MP, EP, PP, and BP were 163, 27.6, 32.9, and 15.4 ng/ml, respectively. According to the estimated correlation coefficient, a weak-to-medium correlation was found among the paraben compounds. A medium correlation existed between MP, PP, and BP (r = 0.63–0.35, p < 0.05), while PP and EP were slightly correlated (r = 0.202, p < 0.05) (data not shown).
The relationship between urinary parabens and anthropometric measures (birth length, weight, and head circumference) was evaluated using linear regression. The regression coefficients (95% CI for regression coefficients) in three models are demonstrated in Tables 3, 4, and 5.
In the unadjusted and adjusted linear regression models, a positive significant relationship was observed between MP and BP concentrations and birth weight (adjusted regression coefficient for MP and BP, β = 0.79, 95% CI: 0.169, 1.41; p = 0.014; β = 8.56, 95% CI: 3.95, 13.17; p = 0.001, respectively). Also, PP concentrations were positively associated with birth weight in all the neonates (β = 1.4, 95% CI: 0.04, 2.8) in the crude model. However, after adjusting the confounders’ effect, the association was not statistically significant anymore (p value > 0.05) (Table 3). In sex-stratified analyses, positive significant associations were found between MP and PP and birth weight in covariate-adjusted models (Model 2), only observed in girls (regression coefficient for MP and PP, β = 0.831, 95% CI: 0.043, 1.620; p = 0.039; β = 4.178, 95% CI: 0.877, 7.480; p = 0.014, respectively], but not in boys. Furthermore, the concentration of BP was positively associated with birth weight in both girls (β = 10.821, 95% CI: 3.545, 18.097) and boys (β = 7.948, 95% CI: 1.045, 14.851) in covariate-adjusted models (Table 6). In all the neonates, urinary levels of MP were found to be positively associated with birth length, both in crude (β = 0.005, 95% CI: 0.002, 0.009) and adjusted models (β = 0.004, 95% CI: 0.00, 0.009). However, regarding the adjusted model in subgroup analysis by sex, positive associations were found between the urinary levels of MP and the length of male neonates (β = 0.008, 95% CI: − 0.001, 0.017). Other analyzed parabens did not indicate any significant association with birth length in the two sexes.
As reported in Table 5, MP and BP urinary concentrations were statically significant with a higher head circumference in all three models. The regression coefficients in covariate-adjusted models were − 0.002 (95% CI: − 0.004, − 0.000; p = 0.035) for MP and − 0.016 (95% CI: − 0.030, − 0.002; p = 0.026) for BP. The urinary PP concentration was found to be positively associated with the head circumference in all the neonates (β = − 0.009, 95% CI: − 0.015, − 0.002) in the unadjusted model; however, after adjusting the confounder variables, no significant association was found between PP exposure and the head circumference. The sex stratification analysis in covariate-adjusted models showed a significant negative association between urinary MP and BP levels and head circumference in girls (regression coefficient for MP and BP, β = − 0.003, 95% CI: − 0.005, − 0.001; p = 0.011; β = − 0.035, 95% CI: − 0.055, − 0.016; p = 0.001, respectively). There was no significant association between birth length in boys and urinary parabens.
We adjusted Model 3 by all the confounders adjusted in Model 2 except for gestational age. The significant associations found between the urinary paraben and anthropometric measures (birth length, weight, and head circumference) in Model 3 were approximately the same as the results observed in Model 2.
Discussion
The present study examined the association between maternal urinary paraben exposure and some birth outcomes such as length, weight, and head circumference. We found obvious associations between paraben exposure in Iranian pregnant women and their infant weight, length, and head circumference at birth. The application of parabens in numerous consumer products led to MP and PP detection in 90 urinary samples of pregnant women in prior studies (Jamal et al. 2020; Shirai et al. 2013; Wu et al. 2017), similar to the present research. In agreement with the other sources (Casas et al. 2011; Kang et al. 2013; Shirai et al. 2013), the detection frequency of EP in the present study was > 80%, while in two other studies conducted in Puerto Rico (Aker et al. 2019) and USA (Aung et al. 2019), the percentage of EP detection was 57.6% and 59.5%, respectively. Nevertheless, the detection rate of BP in this research was higher than that presented by other researchers (Jamal et al. 2020; Sakhi et al. 2018; Wu et al. 2017). In line with other reports, MP and PP had the maximum urinary concentration of parabens (Chang et al. 2019; Hajizadeh et al. 2020a; Wu et al. 2018). The levels of MP and PP in this research were lower than those of reports conducted on Spanish (Casas et al. 2011) and Japanese populations (Shirai et al. 2013). On the other hand, EP and BP were higher. Moreover, the urinary concentrations of MP, EP, PP, and BP detected in mothers in China (Wu et al. 2017), Denmark (de Renzy-Martin et al. 2014), and Norway (Sakhi et al. 2018) were lower than those of the Iranian women in the present study. The difference in reported concentrations could be due to various socioeconomic characteristics and some variances in lifestyle (Hajizadeh et al. 2020a). In accordance with previous studies (Asimakopoulos et al. 2014; Kiani Feizabadi et al. 2020b; Larsson et al. 2014), we observed a significant positive association between MP and PP (correlation coefficient = 0.636), which indicates that these compounds are applied in combination, which is the common exposure source.
Based on two systematic reviews, epidemiologic investigations on associations between maternal paraben and anthropometric measures (length, weight, and head circumference at birth) are limited (Jamal et al. 2019; Zhong et al. 2020). In this research, a significant relationship was found between MP and BP and birth weight in covariate-adjusted models. Although, in the sex-stratified model, a significant positive correlation was found between MP, PP, and BP levels and the birth weight of girls, only a significant positive association was found between the boys’ weight and BP concentration. Equally, the results of previous studies in China and France showed that maternal paraben exposure had a positive association with birth weight (Philippat et al. 2014; Wu et al. 2017). In accordance with our results, Aker et al.’s study in the USA revealed that the maternal urinary BP concentration was related to weight increase in both male and female neonates (Aker et al. 2019). In another study, only in the sex-stratified model, a significant positive relationship was found between maternal BP concentration and the birth weight of boys (Jamal et al. 2020). However, the results of other studies indicated a negative relationship between birth weight and maternal paraben exposure (Geer et al. 2017; Philippat et al. 2012). The exact mechanisms of gaining birth weight due to paraben exposure are not clearly understood. It has been reported that exposure to EDC, such as parabens compounds, can directly affect weight gain by changing lipid homeostasis toward lipid accumulation and adipogenesis. Furthermore, the increase in weight by paraben exposure can be attributed to the increase in adipocytes’ number and size, and also a change in endocrine pathways responsible for adipose tissue metabolism control (Newbold et al. 2008). Accordingly, maternal perinatal paraben exposures raised neonatal weight gain, resulting in higher birth weight. It has been shown that the distribution pattern of estrogen receptors can differ by neonate sex (Gillies and McArthur 2010); therefore, the effects of estrogen can vary and be specific depending on the sex. Likewise, the reproductive outcomes and developmental effects of maternal exposure to parabens may vary by sex (Dodge et al. 2015). Although our findings demonstrated a sexually dimorphic pattern between prenatal exposure to parabens and fetus birth weight, these associations must be verified on larger sample size.
According to the findings of covariate-adjusted models, a positive association was found between urinary MP concentrations and neonatal length (β = 0.005, 95% CI: 0.002, 0.009). Also, after subgroup analysis by sex, a significant positive relationship was found between urinary MP and boys’ birth length. Additionally, no significant association was observed between parabens and the girls’ birth length, although the relationship was positive. Previous studies presenting the association between maternal urinary paraben concentration and birth length have demonstrated no consistent findings. In accordance with our results, Aker et al. in the USA and Philippat in France found a significant correlation between the concentrations of MP in mothers and boys’ birth length (Philippat et al. 2014, Wu et al. 2017). However, the results of other studies showed negative associations between maternal paraben exposures and birth length (Chang et al. 2019; Wu et al. 2018). In the study conducted by Jamal et al., the correlation between parabens and birth length was positive but non-significant for boys, while for girls, the association was negative but non-significant. The differences observed in the results of these studies might be due to the heterogeneity in the exposure pathways and the application of only one spot urine measurement for prenatal paraben exposure or variances in adjustment for confounding factors.
Head circumference is one of the most significant and accessible clinical indicators for assessing brain growth during infancy and childhood (Esmaeili and Esmaeili 2015; Treit et al. 2016). In the present research, significant associations were found between urinary MP and BP concentration and neonates’ head circumference in unadjusted and adjusted models, while in the case of PP concentration, the association was positive just in the unadjusted model. Besides, a significant positive association between MP and BP concentrations and head circumference was observed just for girls. Previous studies investigating the association between maternal urinary paraben concentration and head circumference have demonstrated a non-significant relationship (Chang et al. 2019; Geer et al. 2017). Inconsistent with our findings, in Jamal et al.’s study, MP and BP concentrations in mothers were significantly correlated with the neonatal head circumference. Moreover, a significant association was observed between BP and increased head circumference in girls (Jamal et al. 2020). In agreement with our results, Messerlian et al.’s study in the USA indicated that MP in maternal urine was related to neonatal head circumference reduction (Messerlian et al. 2018). In Iran, Fadaei et al. (2020) reported a negative association between maternal urinary BP and girls’ head circumference and a positive association between BP and PP and the mentioned index in male infants. Although the neonates’ head circumference reduction’s link to maternal urinary parabens is negligible in our research and prior studies, its impact could be significant in the population, and future clinical research should increase the sample size in order to confirm the previously mentioned results, discover the exact mechanism of the sex-specific association of parabens, and investigate the other unknown toxicological effects of these compounds.
This study had some limitations. The sample size in such epidemiological studies, especially in research related to subgroup analyses, should be increased. The sex-stratified models were limited by very small subgroups, and thus, the results must be used with caution. In this study, the urine samples were collected as spot and cross-sectional. Assessing prenatal paraben exposure by using spot sampling may result in exposure misclassifications. The maximum rate of paraben exposure in pregnant women was achieved through the dermal absorption and ingestion of consumer products. Since the consumption habits of individuals do not change easily, the analysis of parabens in single spot urine could be representative. Moreover, despite the short half-life of parabens, their levels in a spot urine sample reasonably represent an individual’s exposure over several months (Smith et al. 2012). In addition, some earlier studies have demonstrated that spot sampling is a suitable predictor of long-term exposure and provides adequate sensitivity to categorize individuals’ exposure in epidemiologic investigations (Dewalque et al. 2015; Mahalingaiah et al. 2008). However, further studies are warranted to evaluate the association between maternal paraben exposure during pregnancy and birth outcomes in multiple urine samples. One more limitation was that we could not separate the isotherms by our detection method, and then we analyzed the sum of the isomers (nPrP vs. iso-PrP, n-BuP vs. iso-BuP). According to the results of Błędzka’ study, the toxicological effects of n-PrP vs. iso-PrP and n-BuP vs. iso-BuP were alike (Błędzka et al. 2014). Nevertheless, as a strength of this study, the association between urinary levels of paraben and anthropometric measures (birth length, weight, and head circumference) was evaluated in three models, and numerous potential confounder variables were considered, including socioeconomic factors, gestational age, physical activity, prepregnancy BMI, parity, and mode of delivery. However, an obvious limit of the present study is that the other typical environmental phenolic compounds were not adjusted to verify the robustness of the results. High levels of parabens, especially BP, in the present study compared to previous studies provide an opportunity to investigate the potential effects of parabens in a paired mother-infant population. Findings confirm the probability of parabens’ exposure effect on the offspring size at birth. Still, more extensive investigations are required to better understand how they influence infant growth. In the meantime, pregnant women should be advised on simple ways to decrease paraben exposure.
Conclusion
A significant amount of urinary paraben was detected in the majority of individuals; in particular, the mean urinary BP concentration was higher than in other countries. Findings indicated that exposure to parabens during pregnancy can increase weight and length at birth, while conversely, exposure to MP and PP is related to a decreased head circumference. Moreover, findings showed a sex-dependent association between prenatal exposure to parabens and fetus growth indicators. In boys, maternal urinary MP and BP were associated with increased birth length and weight, respectively. In girls, maternal urinary MP, PP, and BP were associated with increased birth weight, and MP and BP with a reduced head circumference at birth. Although these results might be interpreted with caution in light of innate investigation limitations, they highlight the possible relevance of maternal perinatal paraben exposure to birth outcomes. With the extensive usage of parabens and their possible endocrine-disrupting effects, further studies are needed to replicate the findings of the present study, as well as to simplify the mechanism of the sex-specific relationship of parabens on a larger sample size.
Availability of data and materials
The data that support the findings of this study are available from the corresponding author (Ghasem kiani Feizabadi) upon reasonable request.
References
Aker AM, Ferguson KK, Rosario ZY, Mukherjee B, Alshawabkeh AN, Cordero JF, Meeker JD (2019) The associations between prenatal exposure to triclocarban, phenols and parabens with gestational age and birth weight in northern Puerto Rico. Environ Res 169:41–51
Andersen FA (2008) Final amended report on the safety assessment of methylparaben, ethylparaben, propylparaben, isopropylparaben, butylparaben, isobutylparaben, and benzylparaben as used in cosmetic products. Int J Toxicol 27:1–82
Asimakopoulos AG, Thomaidis NS, Kannan K (2014) Widespread occurrence of bisphenol A diglycidyl ethers, p-hydroxybenzoic acid esters (parabens), benzophenone type-UV filters, triclosan, and triclocarban in human urine from Athens, Greece. Sci Total Environ 470:1243–1249
Aung MT, Ferguson KK, Cantonwine DE, McElrath TF, Meeker JD (2019) Preterm birth in relation to the bisphenol A replacement, bisphenol S, and other phenols and parabens. Environ Res 169:131–138
Błędzka D, Gromadzińska J, Wąsowicz W (2014) Parabens. From environmental studies to human health. Environ Int 67:27–42
Boberg J, Taxvig C, Christiansen S, Hass U (2010) Possible endocrine disrupting effects of parabens and their metabolites. Reproductive Toxicology 30:301–312
Casas L, Fernández MF, Llop S, Guxens M, Ballester F, Olea N, Irurzun MB, Rodríguez LSM, Riaño I, Tardón A (2011) Urinary concentrations of phthalates and phenols in a population of Spanish pregnant women and children. Environ Int 37:858–866
Chang C-H, Wang P-W, Liang H-W, Huang Y-F, Huang L-W, Chen H-C, Pan W-C, Lin M-H, Yang W, Mao I-F (2019) The sex-specific association between maternal paraben exposure and size at birth. Int J Hyg Environ Health 222:955–964
Cowan-Ellsberry CE, Robison SH (2009) Refining aggregate exposure: example using parabens. Regul Toxicol Pharmacol 55:321–329
Darbre PD, Harvey PW (2008) Paraben esters: review of recent studies of endocrine toxicity, absorption, esterase and human exposure, and discussion of potential human health risks. J Appl Toxicol 28:561–578
Darbre P, Aljarrah A, Miller W, Coldham N, Sauer M, Pope G (2004) Concentrations of parabens in human breast tumours. J Appl Toxicol 24:5–13
de Renzy-Martin KT, Frederiksen H, Christensen JS, Kyhl HB, Andersson A-M, Husby S, Barington T, Main KM, Jensen TK (2014) Current exposure of 200 pregnant Danish women to phthalates, parabens and phenols. Reproduction 147:443–453
Dewalque L, Pirard C, Vandepaer S, Charlier C (2015) Temporal variability of urinary concentrations of phthalate metabolites, parabens and benzophenone-3 in a Belgian adult population. Environ Res 142:414–423
Dodge LE, Williams PL, Williams MA, Missmer SA, Toth TL, Calafat AM, Hauser R (2015) Paternal urinary concentrations of parabens and other phenols in relation to reproductive outcomes among couples from a fertility clinic. Environ Health Perspect 123:665–671
Esmaeili M, Esmaeili M (2015) Head circumference in Iranian infants. Iran J Neonatol 6:28–32
Fadaei S, Pourzamani H, Ebrahimpour K, Feizi A, Daniali SS, Kelishadi R (2020) Association of maternal urinary concentration of parabens and neonatal anthropometric indices. J Environ Health Sci Eng 18(2):617–628
Ferguson KK, Meeker JD, Cantonwine DE, Mukherjee B, Pace GG, Weller D, McElrath TF (2018) Environmental phenol associations with ultrasound and delivery measures of fetal growth. Environ Int 112:243–250
Geer LA, Pycke BF, Waxenbaum J, Sherer DM, Abulafia O, Halden RU (2017) Association of birth outcomes with fetal exposure to parabens, triclosan and triclocarban in an immigrant population in Brooklyn, New York. J Hazard Mater 323:177–183
Gillies GE, McArthur S (2010) Estrogen actions in the brain and the basis for differential action in men and women: a case for sex-specific medicines. Pharmacol Rev 62:155–198
Giulivo M, de Alda ML, Capri E, Barceló D (2016) Human exposure to endocrine disrupting compounds: their role in reproductive systems, metabolic syndrome and breast cancer. A review. Environ Res 151:251–264
Hajizadeh Y, Kiani Feizabadi G, Ebrahimpour K, Shoshtari-Yeganeh B, Fadaei S, Darvishmotevalli M, Karimi H (2020a) Urinary paraben concentrations and their implications for human exposure in Iranian pregnant women. Environ Sci Pollut Res 27:14723–14734
Hajizadeh Y, Kiani Feizabadi G, Feizi A, Ebrahimpour K (2020b) The association of personal care products uses and dietary habits with the urinary concentration of parabens in Iranian adults. Int J Environ Health Res. https://doi.org/10.1080/09603123.2020.1798362
Harvey PW, Everett DJ (2012) Parabens detection in different zones of the human breast: consideration of source and implications of findings. J Appl Toxicol 32:305–309
Honda M, Robinson M, Kannan K (2018) Parabens in human urine from several Asian countries, Greece, and the United States. Chemosphere 201:13–19
Jamal A, Rastkari N, Dehghaniathar R, Aghaei M, Nodehi RN, Nasseri S, Kashani H, Yunesian M (2019) Prenatal exposure to parabens and anthropometric birth outcomes: a systematic review. Environ Res 173:419–431
Jamal A, Rastkari N, Dehghaniathar R, Nodehi RN, Nasseri S, Kashani H, Shamsipour M, Yunesian M (2020) Prenatal urinary concentrations of environmental phenols and birth outcomes in the mother-infant pairs of Tehran Environment and Neurodevelopmental Disorders (TEND) cohort study. Environ Res 184:109331
Kang S, Kim S, Park J, Kim HJ, Lee J, Choi G, Choi S, Kim S, Kim SY, Moon HB, Kim S, Kho YL, Choi K (2013) Urinary paraben concentrations among pregnant women and their matching newborn infants of Korea, and the association with oxidative stress biomarkers. Sci Total Environ 461:214–221
Kiani Feizabadi G, Hajizadeh Y, Feizi A, Ebrahimpour K (2020a) Urinary concentrations of parabens in a population of Iranian adolescent and their association with sociodemographic indicators. Arch Environ Contam Toxicol 79:195–207
Kiani Feizabadi G, Hajizadeh Y, Feizi A, Ebrahimpour K (2020b) Urinary concentrations of parabens amongst Iranian adults and their associations with socio-demographic factors. J Environ Health Sci Eng 18(2):1227–1238
Koeppe ES, Ferguson KK, Colacino JA, Meeker JD (2013) Relationship between urinary triclosan and paraben concentrations and serum thyroid measures in NHANES 2007–2008. Sci Total Environ 445:299–305
Larsson K, Björklund KL, Palm B, Wennberg M, Kaj L, Lindh CH, Jönsson BA, Berglund M (2014) Exposure determinants of phthalates, parabens, bisphenol A and triclosan in Swedish mothers and their children. Environ Int 73:323–333
Ma W-L, Wang L, Guo Y, Liu L-Y, Qi H, Zhu N-Z, Gao C-J, Li Y-F, Kannan K (2013) Urinary concentrations of parabens in Chinese young adults: implications for human exposure. Arch Environ Contam Toxicol 65:611–618
MacKenzie AP, Stephenson CD, Funai EF (2019) Prenatal assessment of gestational age, date of delivery, and fetal weight. Up ToDate. D. Levine. https://www.uptodate.com/contents/prenatal-assessment-of-gestational-age-date-of-delivery-andfetal-weight
Mahalingaiah S, Meeker JD, Pearson KR, Calafat AM, Ye X, Petrozza J, Hauser R (2008) Temporal variability and predictors of urinary bisphenol A concentrations in men and women. Environ Health Perspect 116:173–178
Meeker JD, Yang T, Ye X, Calafat AM, Hauser R (2010) Urinary concentrations of parabens and serum hormone levels, semen quality parameters, and sperm DNA damage. Environ Health Perspect 119:252–257
Messerlian C, Mustieles V, Minguez-Alarcon L, Ford JB, Calafat AM, Souter I, Williams PL, Hauser R (2018) Preconception and prenatal urinary concentrations of phenols and birth size of singleton infants born to mothers and fathers from the Environment and Reproductive Health (EARTH) study. Environ Int 114:60–68
Moridzadeh M, Dehghani S, Rafiee A, Hassanvand MS, Dehghani M, Hoseini M (2020) Assessing BTEX exposure among workers of the second largest natural gas reserve in the world: a biomonitoring approach. Environ Sci Pollut Res 27:44519–44527
Newbold RR, Padilla-Banks E, Jefferson WN, Heindel JJ (2008) Effects of endocrine disruptors on obesity. Int J Androl 31:201–208
Oishi S (2002) Effects of propyl paraben on the male reproductive system. Food Chem Toxicol 40:1807–1813
Pan S, Yuan C, Tagmount A, Rudel RA, Ackerman JM, Yaswen P, Vulpe CD, Leitman DC (2015) Parabens and human epidermal growth factor receptor ligand cross-talk in breast cancer cells. Environ Health Perspect 124:563–569
Philippat C, Mortamais M, Chevrier C, Petit C, Calafat AM, Ye X, Silva MJ, Brambilla C, Pin I, Charles M-A (2012) Exposure to phthalates and phenols during pregnancy and offspring size at birth. Environ Health Perspect 120:464–470
Philippat C, Botton J, Calafat AM, Ye X, Charles M-A, Slama R, Group ES (2014) Prenatal exposure to phenols and growth in boys. Epidemiology 25:625
Philippat C, Heude B, Botton J, Alfaidy N, Calafat AM, Slama R, Group EMCCS (2019) Prenatal exposure to select phthalates and phenols and associations with fetal and placental weight among male births in the EDEN cohort (France). Environ Health Perspect 127:017002
Routledge EJ, Parker J, Odum J, Ashby J, Sumpter JP (1998) Some alkyl hydroxy benzoate preservatives (parabens) are estrogenic. Toxicol Appl Pharmacol 153:12–19
Sakhi AK, Sabaredzovic A, Papadopoulou E, Cequier E, Thomsen C (2018) Levels, variability and determinants of environmental phenols in pairs of Norwegian mothers and children. Environ Int 114:242–251
Shahsavani S, Dehghani M, Hoseini M, Fararouei M (2017) Biological monitoring of urinary 1-hydroxypyrene by PAHs exposure among primary school students in Shiraz, Iran. Int Arch Occup Environ Health 90:179–187
Shirai S, Suzuki Y, Yoshinaga J, Shiraishi H, Mizumoto Y (2013) Urinary excretion of parabens in pregnant Japanese women. Reprod Toxicol 35:96–101
Smith KW, Braun JM, Williams PL, Ehrlich S, Correia KF, Calafat AM, Ye XY, Ford J, Keller M, Meeker JD, Hauser R (2012) Predictors and variability of urinary paraben concentrations in men and women, including before and during pregnancy. Environ Health Perspect 120:1538–1543
Soni M, Carabin I, Burdock G (2005) Safety assessment of esters of p-hydroxybenzoic acid (parabens). Food Chem Toxicol 43:985–1015
Treit S, Zhou D, Chudley AE, Andrew G, Rasmussen C, Nikkel SM, Samdup D, Hanlon-Dearman A, Loock C, Beaulieu C (2016) Relationships between head circumference, brain volume and cognition in children with prenatal alcohol exposure. PLoS One 11:e0150370
Vernet C, Philippat C, Calafat AM, Ye X, Lyon-Caen S, Siroux V, Schisterman EF, Slama R (2018) Within-day, between-day, and between-week variability of urinary concentrations of phenol biomarkers in pregnant women. Environ Health Perspect 126:037005
Wolff MS, Engel SM, Berkowitz GS, Ye X, Silva MJ, Zhu C, Wetmur J, Calafat AM (2008) Prenatal phenol and phthalate exposures and birth outcomes. Environ Health Perspect 116:1092–1097
Wu C, Huo W, Li Y, Zhang B, Wan Y, Zheng T, Zhou A, Chen Z, Qian M, Zhu Y (2017) Maternal urinary paraben levels and offspring size at birth from a Chinese birth cohort. Chemosphere 172:29–36
Wu C, Xia W, Li Y, Li J, Zhang B, Zheng T, Zhou A, Zhao H, Huo W, Hu J (2018) Repeated measurements of paraben exposure during pregnancy in relation to fetal and early childhood growth. Environ Sci Technol 53:422–433
Zhang L, Dong L, Ding S, Qiao P, Wang C, Zhang M, Zhang L, Du Q, Li Y, Tang N (2014) Effects of n-butylparaben on steroidogenesis and spermatogenesis through changed E2 levels in male rat offspring. Environ Toxicol Pharmacol 37:705–717
Zhao H, Huo W, Li J, Ma X, Xia W, Pang Z, Xie M, Xu S, Cai Z (2017) Exposure to benzophenones, parabens and triclosan among pregnant women in different trimesters. Sci Total Environ 607:578–585
Zhong Q, Peng M, He J, Yang W, Huang F (2020) Association of prenatal exposure to phenols and parabens with birth size: a systematic review and meta-analysis. Sci Total Environ 703:134720
Acknowledgements
The authors acknowledge the financial assistance received from the Vice-Chancellor of Research of Isfahan University of Medical Sciences (IUMS), Iran.
Funding
This work was supported by the Isfahan University of Medical Science (grant number: 198001).
Author information
Authors and Affiliations
Contributions
The authors confirm contribution to the paper as follows: study conception and design: Yaghoub Hajizadeh, Ghasem Kiani Feizabadi; material preparation: Ghasem Kiani Feizabadi, Nasim Rafiei, Maryam Moradnia; data collection: Maryam Moradnia, Masoumeh Tahmasbizadeh, Mohammad Darvishmotevalli, Saeid Fadaei, Hossein Karimi; analysis and interpretation of results: Ghasem Kiani Feizabadi, Saeid Fadaei; draft manuscript preparation: Yaghoub Hajizadeh, Ghasem Kiani Feizabadi, Maryam Moradnia. All authors reviewed the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Ethical approval
This study was approved by the Ethics Committee, Isfahan University of Medical Sciences (code: IR.MUI.RESEARCH.REC.1398.092). The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Consent to participate
All the participants were informed about the voluntary nature, purpose, and methods of the study, and provided a signed consent letter.
Consent to publish
Not applicable.
Conflicts of interest
The authors declare that they have no competing interests.
Additional information
Responsible Editor: Lotfi Aleya
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hajizadeh, Y., Moradnia, M., Kiani Feizabadi, G. et al. The sex-specific association between maternal urinary paraben levels and offspring size at birth. Environ Sci Pollut Res 28, 36029–36038 (2021). https://doi.org/10.1007/s11356-021-13175-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-021-13175-3