Abstract
Fine particulate matter (PM2.5) is one of the major pollutants in metropolitan areas. The current study was conducted to observe the effects of PM2.5 on cardiac autonomic modulation. The participants included 619 men and women aged from 35–75 in a residential area in Shanghai, China. All the participants were divided into four categories according to the distance between their apartments and major road. In addition, individual PM2.5 was measured using SIDEPAKTM AM510 (TSI, USA) from 8:00 am to 6:00 pm. At the end of the individual PM2.5 measurement, the systolic pressure, diastolic pressure, heart rate (HR), low-frequency (LF), high-frequency (HF), and LF/HF were determined. The association between individual PM2.5 level and the above health effects was analyzed using generalized linear regression. The results showed that the average concentration of individual PM2.5 was 95.5 and 87.0 μg/m3 for men and women. Residential distance to major road was negatively correlated with the individual PM2.5. The results indicated that per 1.0 μg/m3 increase of individual PM2.5 was associated with a 2.3 % increase for systolic pressure, 0.3 % increase for diastolic pressure, 0.4 % decrease for LF, and 0.4 % decrease for HF. Nevertheless, there was no statistical association between individual PM2.5 and heart rate and LF/HF in the total model. In addition, the similar results were found in men and women excluding a significant association between PM2.5 and the heart rate in men. The alterations of cardiac autonomic modulation hinted that PM2.5 exposure might be associated with the potential occurrence of cardiovascular disease, such as arrhythmia and ischemic heart diseases.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Numerous studies have consistently shown that exposure to ambient fine particulate matter (PM2.5) increases daily deaths (Schwartz et al. 2002), cardiopulmonary mortality, and morbidity (Brook et al. 2004; Dockery et al. 1993; Peters et al. 2001a, b; Pope et al. 2002). The adverse effects have been associated with both short- and long-term PM2.5 exposure (Brook and Rajagopalan 2007; Mills et al. 2009; Pope 2007). However, little is known about the mechanisms linking PM2.5 and the increased risk of cardiovascular disease. The potential mechanisms such as the increase in oxidative stress (Sorensen et al. 2003; Xu et al. 2011), inflammatory response (Peters et al. 2001a, b), autonomic modulation impairment (Hampel et al. 2014; Luttmann-Gibson et al. 2006), and blood coagulation (Ghio et al. 2000; Schwartz 2001) have been reported. In our previous animal experimental study, ambient PM2.5 caused significant changes of cardiovascular injury-related indicators (Zhao et al. 2010), such as inflammation, endothelial dysfunction, and coagulation disorder. Recently, it has been reported that impaired cardiac autonomic modulation induced by particulate matter might be a risk factor of incidence of arrhythmia events (Bartell et al. 2013) and sudden cardiac death (Baranchuk et al. 2009). Accordingly, an association has been found between traffic exhaust and the onset of a myocardial infarction within 1 h afterward (Peters et al. 2004). Therefore, the detailed mechanisms linking PM2.5 and cardiac autonomic modulation need to be further elucidated. Nowadays, epidemiologic evidence regarding the alterations of cardiac autonomic modulation at the individual level due to PM2.5 is more limited. Several studies have conducted the relationship between PM2.5 and cardiac autonomic modulation. Most of them obtained the exposure assessment from monitoring sites (Bortkiewicz et al. 2014; Hoffmann et al. 2009a, b) or from land use regression model (Cesaroni et al. 2013). In the current study, we attempted to monitor the personal PM2.5 exposure to assess the adverse effects of air pollution. The personal PM2.5 could represent the actual PM2.5 exposure for individual. One study has measured the individual level of environmental tobacco smoke (ETS) using personal monitor, suggesting that subjects with different inductions of CYP1A1 expression in CYP1A1*2A and CYP1A1*2A/*2B carriers may have increased susceptibility to the genotoxic effects of ETS (Georgiadis et al. 2005). Moreover, another study observed the association between PM2.5 exposure and immediate impairment of cardiac autonomic modulation by estimating 24-h individual-level real-time PM2.5 exposure (He et al. 2011), indicating that the increases in preceding 1–6-h moving averages of PM2.5 were significantly associated with the lowering of high-frequency (HF) and low-frequency (LF).
High-frequency and LF are two key indicators which reflect the heart rate variability (HRV), and the latter is a measure of beat-to-beat temporal changes in heart rate and could provide indirect insight into autonomic nervous system tone. Reduction of the HRV has been associated with an increased risk of mortality in middle-aged and elderly subjects (Dekker et al. 1997), in patients with diabetes mellitus, and in survivors of myocardial infarction (Tapanainen et al. 2002). High-frequency is a representative of respiration-linked parasympathetic cardiac modulation, and LF is considered to be an indicative of both parasympathetic and sympathetic modulation (Cavalcanti et al. 1997; Latalova et al. 2010). The individual PM2.5-induced alterations of cardiac autonomic function have been investigated in cardiac patients and hypertensive patients (Chuang et al. 2005). In the current study, we attempt to further explore the effects of individual PM2.5 on cardiac autonomic nervous function in general population whose apartments with different distances to a major road. The individual PM2.5, blood pressure, and HRV-related index are measured to explore the potential mechanisms linking individual PM2.5 and cardiac autonomic function.
Materials and methods
Study population and design
The participants included 619 men and women aged from 35–75 in Shanghai, China. The study was performed from September to December 2013. All participants live in a big community which is close to the major road. The total population is around 20,000 residents in the community. The community consists of a residential district and several small business districts. All the participants live or work in the community from 8:00 am to 6:00 pm every day. The residential areas were categorized as ≤50, 51–100, 101–200, and >200 m according to the distance to major road. The study was approved by the relevant institutional ethics committees and followed strict internal and external quality assurance protocols. The participants gave informed consent before the experiment. The research included a self-administered questionnaire and the further cardiac autonomic nervous function detection. At the end of the individual PM2.5 measurement, the participants answered a self-administered questionnaire including a personal interview regarding age, address, highest education level, sociodemographic characteristics, lifestyle factors, and physician-diagnosed chronic disease history. The chronic disease histories such as CVD, hypertension, and diabetes were confirmed as a self-reported history. The education condition was classified according to the International Standard Classification of Education as total years of formal education, combining primary schooling and vocational or professional education. Three categories were defined with the highest category of ≥18 years of education (equivalent to a university degree) and the lowest category of ≤10 years (equivalent to a basic school degree and no vocational training). Smoking status was divided into current smoking, cessation of smoking within last year, cessation of smoking more than 1 year, and non-smoking. Body mass index (BMI) was calculated according to standardized protocols.
Individual PM2.5 exposure monitoring
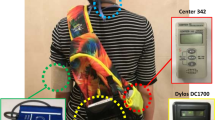
Individual PM2.5 exposure was measured using SIDEPAKTM AM510 (TSI, USA). Every participant carries one AM510. The machine attached a sampling plastic tube that was connected to an inlet port. The plastic tube was placed at the height that was at the same height of breathing, so that it would represent the individual’s actual exposure. The machine was set to record PM2.5 data every 5 min. The measurement duration was from 8:00 am to 6:00 pm, which represented the work hour for 1 day.
Cardiac autonomic modulation determination
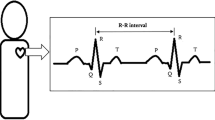
At the end of the individual PM2.5 measurement, the participants returned the AM510 at 6:00 pm. The participants quietly seated in a chair for determining the HRV. The Model SKY-A4 Bioelectric Signals Processing System (Shanghai Sky-Tech Co., Ltd, China) was used to determine the HRV. The major equipment connects with an electrode that is fixed with an arm. The electrode is put on the position of pulse wave. The signaling of pulse wave can be transmitted to a connecting computer. After record of more than 256 continuous heartbeats, the output signaling can be transmitted to a computer. Then, the computer can give the HRV-related data, such as HF, LF, and HF/LF. If there are any artifacts or missing beats, the software can automatically adjust them. The systolic blood pressure (SBP), diastolic blood pressure (DBP), and heart rate (HR) were detected using Omron arm blood pressure monitor. The averages of the three times measures of seated systolic and diastolic blood pressures were used to represent a participant’s blood pressure.
Statistical analysis
The entire study population consisted of 619 participants. There were 12 participants whose measurements for cardiac autonomic modulation were incomplete, and six participants have not finished the questionnaire, thus leaving 601 participants for the final analyses. For each participant, the average PM2.5 was calculated according to the monitoring data from 8:00 am to 6:00 pm. The mean, median, and interquartile range for personal PM2.5 were assessed for total, men, and women, respectively. The distribution was divided into seven categories according to a progressive increase as 35 μg/m3 of individual PM2.5. The number of participants for every category was calculated. The data of LF and HF were expressed as Log-LF and Log-HF using a logarithm transformation.
One-way ANOVA was used to analyze the difference of individual PM2.5 for the participants who were divided into four categories on the basis of the residential distance to major road (≤50, 51–100, 101–200, >200 m). To assess the association between the individual PM2.5 exposure and cardiac autonomic modulation, generalized linear regression was performed. The SBP, DBP, HR, LF, HF, or LF/HF were separately used as dependent variables, and the individual PM2.5 was used as the independent variable. The factors such as BMI, educational level, smoking status, history diseases, and home decoration status were adjusted in the model. The statistical package was the SPSS16.0 for Windows. The level of 5 % is considered as significant.
Results and discussion
Individual PM2.5 exposure and distribution of participants
The results showed that the average individual PM2.5 for total, men, and women was 90.2, 95.5, and 87.0 μg/m3, respectively (Table 1). The personal PM2.5 concentration in most of the participants (n = 338) was between 35 and 105 μg/m3 (Fig. 1a). Figure 1b displayed the individual PM2.5 concentration for participants in different category. The results indicated that the individual PM2.5 concentration decreased with the increase of residential proximity to major road. The average individual PM2.5 concentration exceeded 120 μg/m3 in those participants whose apartments were within 50 m of a major road. For the subjects living within 200 m of a major road, the reduction of the individual PM2.5 exposure was associated with the residential distance to major road. The participants living within 50 m of a major road compared with those living more than 200 m away had 51 % higher of the individual PM2.5.
Distribution of individual fine particulate matter (PM2.5) exposure and residents distance to major roads for 601 participants. The distribution was divided into seven categories according to a progressive increase as 35 μg/m3 of individual PM2.5 every category (a). The individual PM2.5 exposure for participants according to the residential distance to major road (b)
Traffic was one of the major sources of environmental pollution in metropolitan areas, emitting pollutants such as particulate matter and noise. Because of the growing traffic-related air pollution and rising population in most metropolitans in China, most of the population live closely to the heavy traffic road and are exposed to high concentration of traffic-related air pollution. Recently, the ambient PM2.5 exposure has become the main air pollutant in China. The Chinese government has paid more attention in controlling the PM2.5 air pollution. In 2012, the government established the air quality standard for PM2.5 (the 24-h average, 75 μg/m3). Previous study indicated that the risk of developing deep vein thrombosis was increased in subjects living near a major traffic road when compared with those living away from the major road (Baccarelli et al. 2009). Another study indicated that long-term residential exposure to high level of PM2.5 was associated with systemic inflammatory markers (Hoffmann et al. 2009a, b). In the current study, one of the key findings was that most of participants were exposed to high concentration of PM2.5, which was significantly higher than the Chinese national ambient Air Quality Standard for PM2.5. Importantly, for subjects living within 200 m of a major road, the reduction of the individual PM2.5 exposure was associated with the residence distance to major road. The current results indicated that traffic-related PM2.5 pollution has been the main source of individual PM2.5 exposure.
Descriptive statistics of the study population
Table 2 describes the statistics of the study population. The total participants were 619, and 18 participants with incomplete data were excluded. There are 226 men and 375 women in the final analysis. BMI was expressed as mean ± SD. The number and rate of CVD, hypertension, and diabetes were calculated. Educational level, smoking status, and home decoration status in the last 6 months were obtained to control the confounding factor. The SBP, DBP, HR, LF, HF, and LF/HF in total, men, and women were analyzed.
In this study, the morbidity of CVD, hypertension, and diabetes in participants was roughly 10 %, respectively. Prior study reported that chronic cardiovascular disease acted as a significant effect modifier in the relationship between PM air pollution and decreased HRV (Holguin et al. 2003; Park et al. 2005). It has been reported that the PM2.5 was associated with reduced HF and increased LF/HF in elderly subjects with stable coronary artery disease (Timonen et al. 2006). In this study, the history disease was adjusted in the model, which may contribute to find the real association between exposure and effects.
Multiple linear regression analyses
Table 3 shows the total and sex-stratified results. In the multiple linear regression analysis, the factors such as BMI, disease history, educational level, smoking status, and home decoration status were adjusted. In total model, per 1.0 μg/m3 increase in individual PM2.5 was associated with an increase in systolic pressure of 2.3 % [95 % confidence interval (CI), 2.1 to 2.4 %] and diastolic pressure of 0.3 % (95 % CI, 0.2 to 0.4 %). On the contrary, per 1.0 μg/m3 increase of PM2.5 induced 0.4 % (95 % CI, −0.6 to −0.3 %) decrease in HF and 0.4 % (95 % CI, −0.5 to −0.3 %) decrease in LF. Meanwhile, there was no statistical association between individual PM2.5 and LF/HF and heart rate.
It has been reported that lung lesion following exposure to ambient particles may impact cardiac functions indirectly (Cozzi et al. 2007; Gilmour et al. 2006). The possible mechanisms involved in these events include disturbances in cardiac autonomic control (Shields et al. 2013), reduction in cardiac vagal control (He et al. 2011), and an imbalance in cardiac autonomic control (Min et al. 2008). Previous study suggested that there were elevations in PM2.5-predicted risk for exercise-induced ST segment depression in subjects with coronary artery disease (Pekkanen et al. 2002). Several other studies have demonstrated a link between changes in heart rate variability and PM2.5 in mice (Chen and Hwang 2005), rats (Farraj et al. 2011) and elderly humans (He et al. 2011). However, to our knowledge, few studies utilize the personal PM2.5 to assess the short-term effect of PM2.5 exposure on cardiac autonomic function. The current study measured the personal PM2.5 exposure for 601 participants, which may represent the actual exposures that the participants experienced. Our individual PM2.5 determination was suggestive of an acute adverse effect of PM2.5 on cardiac autonomic function impairment. Such an acute effect on cardiac autonomic modulation suggested an acute triggering effect of PM2.5 in terms of its mechanistic impact on the onset of cardiac events, such as arrhythmia and sudden cardiac death. In most studies, acute short-term PM increases that might trigger an acute cardiovascular event have been investigated (Delfino et al. 2008; Dubowsky et al. 2006; Ruckerl et al. 2007; Yue et al. 2007). In the adjusted model, the results indicated that elevated individual PM2.5 induced the decrease of LF and HF. The reduced LF and HF value induced by PM2.5 reflects the activity of both the sympathetic and parasympathetic nervous systems (Cavalcanti et al. 1997; Latalova et al. 2010).
Recently, the link between environmental factors such as air pollution and propensity to hypertension has gained attention (Dong et al. 2013). Imbalanced activation of the autonomic nervous system has been postulated to play a role in the pathogenesis of acute increases in blood pressure in response to PM2.5 exposure, primarily on account of the alterations of sympathetic activation-related heart rate variability (Brook et al. 2009; Cosselman et al. 2012). Our results showed an association between PM2.5 and the increase of blood pressure, verifying the possible changes of the sympathetic activation-related autonomic nervous system. Although the mechanisms linking the autonomic nervous modulation and short- or long-term PM2.5 exposure might be different, our short-term results were consistent with the previous study which suggested that long-term concentrated ambient PM2.5 exposure increased blood pressure through sympathetic nervous system activation (Ying et al. 2014).
In the current study, the effect estimates were analyzed in men and women, respectively. The results showed that per 1.0 μg/m3 increase of PM2.5 is associated with the 3.2 % increase in SPB, 0.7 % increase in DBP, 0.4 % decrease in LF, and 0.4 % decrease HF in men. Similarly, very similar results were observed in women. The only difference was that there was a 1.4 % increase in heart rate in men but not in women. Although there is no significant relationship between PM2.5 concentration and heart rate in the total model and women. One potential explanation might be the different sympathetic modulation in various organs in response to diverse stimuli (Do et al. 2011). Besides, the obvious reaction of heart rate in men in our study might associate with the higher individual PM2.5 exposure in men. Similarly, prior study observed the association between high levels of PM2.5 and new-grade systemic inflammatory state in men but not in women (Hoffmann et al. 2009b).
In this study, short-term PM2.5 exposure induced the decrease of LF and HF and the increase of systolic pressure and diastolic pressure both in men and women. Such an acute effect on cardiac autonomic nervous suggested an acute triggering effect of PM2.5, which hinted its mechanistic impact on the onset of cardiac events, such as arrhythmia and sudden cardiac death.
Conclusion
The key finding of our study was that elevated PM2.5 was associated with the alterations of cardiac autonomic modulation in participants. The similar results were observed in men and women. The results indicated that short-term exposure to ambient PM2.5 might induce the alteration of sympathetic modulation-related autonomic nervous function. Our findings provided a possible explanation for prior results about the association between air pollution and autonomic nervous system, suggesting that the alterations of autonomic nervous function might be a potential mechanism linking PM2.5 and cardiovascular disease.
References
Baccarelli A, Martinelli I, Pegoraro V, Melly S, Grillo P, Zanobetti A, Hou L, Bertazzi PA, Mannucci PM, Schwartz J (2009) Living near major traffic roads and risk of deep vein thrombosis. Circulation 119:3118–3124
Baranchuk A, Nault MA, Morillo CA (2009) The central nervous system and sudden cardiac death: what should we know? Cardiol J 16:105–112
Bartell SM, Longhurst J, Tjoa T, Sioutas C, Delfino RJ (2013) Particulate air pollution, ambulatory heart rate variability, and cardiac arrhythmia in retirement community residents with coronary artery disease. Environ Health Perspect 121:1135–1141
Bortkiewicz A, Gadzicka E, Stroszejn-Mrowca G, Szyjkowska A, Szymczak W, Koszada-Wlodarczyk W, Szadkowska-Stanczyk I (2014) Cardiovascular changes in workers exposed to fine particulate dust. Int J Occup Med Environ Health 27:78–92
Brook RD, Rajagopalan S (2007) Air pollution and cardiovascular events. N Engl J Med 356:2104–2105, 2105–2106
Brook RD, Franklin B, Cascio W, Hong Y, Howard G, Lipsett M, Luepker R, Mittleman M, Samet J, Smith SJ, Tager I (2004) Air pollution and cardiovascular disease: a statement for healthcare professionals from the expert panel on population and prevention science of the American Heart Association. Circulation 109:2655–2671
Brook RD, Urch B, Dvonch JT, Bard RL, Speck M, Keeler G, Morishita M, Marsik FJ, Kamal AS, Kaciroti N, Harkema J, Corey P, Silverman F, Gold DR, Wellenius G, Mittleman MA, Rajagopalan S, Brook JR (2009) Insights into the mechanisms and mediators of the effects of air pollution exposure on blood pressure and vascular function in healthy humans. Hypertension 54:659–667
Cavalcanti S, Severi S, Chiari L, Avanzolini G, Enzmann G, Bianco G, Panzetta G (1997) Autonomic nervous function during haemodialysis assessed by spectral analysis of heart-rate variability. Clin Sci (Lond) 92:351–359
Cesaroni G, Badaloni C, Gariazzo C, Stafoggia M, Sozzi R, Davoli M, Forastiere F (2013) Long-term exposure to urban air pollution and mortality in a cohort of more than a million adults in Rome. Environ Health Perspect 121:324–331
Chen LC, Hwang JS (2005) Effects of subchronic exposures to concentrated ambient particles (CAPs) in mice. IV. Characterization of acute and chronic effects of ambient air fine particulate matter exposures on heart-rate variability. Inhal Toxicol 17:209–216
Chuang KJ, Chan CC, Chen NT, Su TC, Lin LY (2005) Effects of particle size fractions on reducing heart rate variability in cardiac and hypertensive patients. Environ Health Perspect 113:1693–1697
Cosselman KE, Krishnan RM, Oron AP, Jansen K, Peretz A, Sullivan JH, Larson TV, Kaufman JD (2012) Blood pressure response to controlled diesel exhaust exposure in human subjects. Hypertension 59:943–948
Cozzi E, Wingard CJ, Cascio WE, Devlin RB, Miles JJ, Bofferding AR, Lust RM, Van Scott MR, Henriksen RA (2007) Effect of ambient particulate matter exposure on hemostasis. Transl Res 149:324–332
Dekker JM, Schouten EG, Klootwijk P, Pool J, Swenne CA, Kromhout D (1997) Heart rate variability from short electrocardiographic recordings predicts mortality from all causes in middle-aged and elderly men. The Zutphen Study. Am J Epidemiol 145:899–908
Delfino RJ, Staimer N, Tjoa T, Polidori A, Arhami M, Gillen DL, Kleinman MT, Vaziri ND, Longhurst J, Zaldivar F, Sioutas C (2008) Circulating biomarkers of inflammation, antioxidant activity, and platelet activation are associated with primary combustion aerosols in subjects with coronary artery disease. Environ Health Perspect 116:898–906
Do CJ, Da SA, Cai Z, Lin S, Dubinion JH, Hall JE (2011) Control of blood pressure, appetite, and glucose by leptin in mice lacking leptin receptors in proopiomelanocortin neurons. Hypertension 57:918–926
Dockery DW, Pope CR, Xu X, Spengler JD, Ware JH, Fay ME, Ferris BJ, Speizer FE (1993) An association between air pollution and mortality in six US cities. N Engl J Med 329:1753–1759
Dong GH, Qian ZM, Xaverius PK, Trevathan E, Maalouf S, Parker J, Yang L, Liu MM, Wang D, Ren WH, Ma W, Wang J, Zelicoff A, Fu Q, Simckes M (2013) Association between long-term air pollution and increased blood pressure and hypertension in China. Hypertension 61:578–584
Dubowsky SD, Suh H, Schwartz J, Coull BA, Gold DR (2006) Diabetes, obesity, and hypertension may enhance associations between air pollution and markers of systemic inflammation. Environ Health Perspect 114:992–998
Farraj AK, Hazari MS, Haykal-Coates N, Lamb C, Winsett DW, Ge Y, Ledbetter AD, Carll AP, Bruno M, Ghio A, Costa DL (2011) ST depression, arrhythmia, vagal dominance, and reduced cardiac micro-RNA in particulate-exposed rats. Am J Respir Cell Mol Biol 44:185–196
Georgiadis P, Topinka J, Vlachodimitropoulos D, Stoikidou M, Gioka M, Stephanou G, Autrup H, Demopoulos NA, Katsouyanni K, Sram R, Kyrtopoulos SA (2005) Interactions between CYP1A1 polymorphisms and exposure to environmental tobacco smoke in the modulation of lymphocyte bulky DNA adducts and chromosomal aberrations. Carcinogenesis 26:93–101
Ghio AJ, Kim C, Devlin RB (2000) Concentrated ambient air particles induce mild pulmonary inflammation in healthy human volunteers. Am J Respir Crit Care Med 162:981–988
Gilmour PS, Nyska A, Schladweiler MC, McGee JK, Wallenborn JG, Richards JH, Kodavanti UP (2006) Cardiovascular and blood coagulative effects of pulmonary zinc exposure. Toxicol Appl Pharmacol 211:41–52
Hampel R, Ruckerl R, Yli-Tuomi T, Breitner S, Lanki T, Kraus U, Cyrys J, Belcredi P, Bruske I, Laitinen TM, Timonen K, Wichmann HE, Peters A, Schneider A (2014) Impact of personally measured pollutants on cardiac function. Int J Hyg Environ Health 217:460–464
He F, Shaffer ML, Li X, Rodriguez-Colon S, Wolbrette DL, Williams R, Cascio WE, Liao D (2011) Individual-level PM(2). (5) exposure and the time course of impaired heart rate variability: the APACR Study. J Expo Sci Environ Epidemiol 21:65–73
Hoffmann B, Moebus S, Dragano N, Mohlenkamp S, Memmesheimer M, Erbel R, Jockel KH (2009a) Residential traffic exposure and coronary heart disease: results from the Heinz Nixdorf Recall Study. Biomarkers 14(Suppl 1):74–78
Hoffmann B, Moebus S, Dragano N, Stang A, Mohlenkamp S, Schmermund A, Memmesheimer M, Brocker-Preuss M, Mann K, Erbel R, Jockel KH (2009b) Chronic residential exposure to particulate matter air pollution and systemic inflammatory markers. Environ Health Perspect 117:1302–1308
Holguin F, Tellez-Rojo MM, Hernandez M, Cortez M, Chow JC, Watson JG, Mannino D, Romieu I (2003) Air pollution and heart rate variability among the elderly in Mexico City. Epidemiology 14:521–527
Latalova K, Prasko J, Diveky T, Grambal A, Kamaradova D, Velartova H, Salinger J, Opavsky J (2010) Autonomic nervous system in euthymic patients with bipolar affective disorder. Neuro Endocrinol Lett 31:829–836
Luttmann-Gibson H, Suh HH, Coull BA, Dockery DW, Sarnat SE, Schwartz J, Stone PH, Gold DR (2006) Short-term effects of air pollution on heart rate variability in senior adults in Steubenville, Ohio. J Occup Environ Med 48:780–788
Mills NL, Donaldson K, Hadoke PW, Boon NA, MacNee W, Cassee FR, Sandstrom T, Blomberg A, Newby DE (2009) Adverse cardiovascular effects of air pollution. Nat Clin Pract Cardiovasc Med 6:36–44
Min KB, Min JY, Cho SI, Paek D (2008) The relationship between air pollutants and heart-rate variability among community residents in Korea. Inhal Toxicol 20:435–444
Park SK, O’Neill MS, Vokonas PS, Sparrow D, Schwartz J (2005) Effects of air pollution on heart rate variability: the VA normative aging study. Environ Health Perspect 113:304–309
Pekkanen J, Peters A, Hoek G, Tiittanen P, Brunekreef B, de Hartog J, Heinrich J, Ibald-Mulli A, Kreyling WG, Lanki T, Timonen KL, Vanninen E (2002) Particulate air pollution and risk of ST-segment depression during repeated submaximal exercise tests among subjects with coronary heart disease: the Exposure and Risk Assessment for Fine and Ultrafine Particles in Ambient Air (ULTRA) study. Circulation 106:933–938
Peters A, Dockery DW, Muller JE, Mittleman MA (2001a) Increased particulate air pollution and the triggering of myocardial infarction. Circulation 103:2810–2815
Peters A, Frohlich M, Doring A, Immervoll T, Wichmann HE, Hutchinson WL, Pepys MB, Koenig W (2001b) Particulate air pollution is associated with an acute phase response in men; results from the MONICA-Augsburg Study. Eur Heart J 22:1198–1204
Peters A, von Klot S, Heier M, Trentinaglia I, Hormann A, Wichmann HE, Lowel H (2004) Exposure to traffic and the onset of myocardial infarction. N Engl J Med 351:1721–1730
Pope CR (2007) Mortality effects of longer term exposures to fine particulate air pollution: review of recent epidemiological evidence. Inhal Toxicol 19(Suppl 1):33–38
Pope CR, Burnett RT, Thun MJ, Calle EE, Krewski D, Ito K, Thurston GD (2002) Lung cancer, cardiopulmonary mortality, and long-term exposure to fine particulate air pollution. JAMA 287:1132–1141
Ruckerl R, Greven S, Ljungman P, Aalto P, Antoniades C, Bellander T, Berglind N, Chrysohoou C, Forastiere F, Jacquemin B, von Klot S, Koenig W, Kuchenhoff H, Lanki T, Pekkanen J, Perucci CA, Schneider A, Sunyer J, Peters A (2007) Air pollution and inflammation (interleukin-6, C-reactive protein, fibrinogen) in myocardial infarction survivors. Environ Health Perspect 115:1072–1080
Schwartz J (2001) Air pollution and blood markers of cardiovascular risk. Environ Health Perspect 109(Suppl 3):405–409
Schwartz J, Laden F, Zanobetti A (2002) The concentration-response relation between PM (2.5) and daily deaths. Environ Health Perspect 110:1025–1029
Shields KN, Cavallari JM, Hunt MJ, Lazo M, Molina M, Molina L, Holguin F (2013) Traffic-related air pollution exposures and changes in heart rate variability in Mexico City: a panel study. Environ Health 12:7
Sorensen M, Daneshvar B, Hansen M, Dragsted LO, Hertel O, Knudsen L, Loft S (2003) Personal PM2.5 exposure and markers of oxidative stress in blood. Environ Health Perspect 111:161–166
Tapanainen JM, Thomsen PE, Kober L, Torp-Pedersen C, Makikallio TH, Still AM, Lindgren KS, Huikuri HV (2002) Fractal analysis of heart rate variability and mortality after an acute myocardial infarction. Am J Cardiol 90:347–52
Timonen KL, Vanninen E, de Hartog J, Ibald-Mulli A, Brunekreef B, Gold DR, Heinrich J, Hoek G, Lanki T, Peters A, Tarkiainen T, Tiittanen P, Kreyling W, Pekkanen J (2006) Effects of ultrafine and fine particulate and gaseous air pollution on cardiac autonomic control in subjects with coronary artery disease: the ULTRA study. J Expo Sci Environ Epidemiol 16:332–341
Xu Z, Xu X, Zhong M, Hotchkiss IP, Lewandowski RP, Wagner JG, Bramble LA, Yang Y, Wang A, Harkema JR, Lippmann M, Rajagopalan S, Chen LC, Sun Q (2011) Ambient particulate air pollution induces oxidative stress and alterations of mitochondria and gene expression in brown and white adipose tissues. Part Fibre Toxicol 8:20
Ying Z, Xu X, Bai Y, Zhong J, Chen M, Liang Y, Zhao J, Liu D, Morishita M, Sun Q, Spino C, Brook RD, Harkema JR, Rajagopalan S (2014) Long-term exposure to concentrated ambient PM2.5 increases mouse blood pressure through abnormal activation of the sympathetic nervous system: a role for hypothalamic inflammation. Environ Health Perspect 122:79–86
Yue W, Schneider A, Stolzel M, Ruckerl R, Cyrys J, Pan X, Zareba W, Koenig W, Wichmann HE, Peters A (2007) Ambient source-specific particles are associated with prolonged repolarization and increased levels of inflammation in male coronary artery disease patients. Mutat Res 621:50–60
Zhao J, Xie Y, Qian X, Jiang R, Song W (2010) Acute effects of fine particles on cardiovascular system: differences between the spontaneously hypertensive rats and wistar kyoto rats. Toxicol Lett 193:50–60
Acknowledgments
This work was supported by the grants from the National Natural Science Foundation of China (Nos.:91543119, 81001229)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The study was approved by the relevant institutional ethics committees and followed strict internal and external quality assurance protocols. The participants gave informed consent before the experiment.
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Responsible editor: Philippe Garrigues
Rights and permissions
About this article
Cite this article
Xie, Y., Bo, L., Jiang, S. et al. Individual PM2.5 exposure is associated with the impairment of cardiac autonomic modulation in general residents. Environ Sci Pollut Res 23, 10255–10261 (2016). https://doi.org/10.1007/s11356-015-5933-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-015-5933-1