Abstract
Background
Intermittent hypoxia (IH) can damage endothelial cells and lead to apoptosis in obstructive sleep apnea-hypopnea syndrome (OSAHS). Hypoxia induces apoptosis in endothelial cells via upregulation of endothelin-1 (ET-1) and hypoxia inducible factor-1 alpha (HIF-1α) plays a key role in the hypoxic stress response.
Purpose
We investigated an approach to diminish the negative effect of HIF-1α while maintaining its protective effect.
Methods
Human umbilical vein endothelial cells (HUVECs) were subjected to sustained hypoxia (SH) or IH for 24 h, and the responses of HIF-1α, CCAAT/enhancer binding protein beta (C/EBP β), and endothelin-1 (ET-1) were assessed by western blotting. A luciferase reporter system was employed to verify the potential binding site (transcription factor binding site, TFBS) for C/EBP β in the ET-1 promoter. The specificity of regulation of ET-1 by HIF-1α via C/EBP β was evaluated by a lentiviral system. The effects of silencing of C/EBP β on IH-induced apoptosis, vascular endothelial growth factor (VEGF) protein levels, proliferation, and in vitro tube formation were studied.
Results
We found that IH significantly increased HIF-1α, C/EBP β, and ET-1 in HUVECs. Knockdown of HIF-1α or C/EBP β inhibited the upregulation of ET-1 induced by IH. Blocking C/EBP β impaired IH-induced apoptosis but did not affect VEGF expression, proliferation, or in vitro tube formation. C/EBP β was shown to mediate increased ET-1 transcription by HIF-1α through the TFBS, 5′-GTTGCCTGTTG-3′, in ET-1 promoter.
Conclusion
Silencing of C/EBP β can suppress apoptosis but does not affect the protective role of HIF-1α in the hypoxic stress response.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnea-hypopnea syndrome (OSAHS) is a common disease, with an incidence of approximately 2~4% in middle-aged people; this incidence increases by 2.2% per 10 years with increasing age [1]. The main symptoms of OSAHS include snoring and daytime sleepiness, which are characterized by persistent upper airway obstruction and apnea. OSAHS may lead to intermittent hypoxia (IH) due to persistent obstruction of the upper airway and hypopnea, the most important pathophysiological characteristics of OSAHS [2]. The 8-year survival rate of the patients with an Apnea–Hypopnea Index (AHI) score greater than 20 h (AHI > 20) is only 63%, with the main cause of death being cardiovascular events [3]. IH plays an important role in cardiovascular complications, such as hypertension of OSAHS, in which endothelial dysfunction caused by IH may be involved [4].
High endothelin-1(ET-1) expression, often found in the serum of OSAHS patients, is considered to be a critical indicator of endothelial dysfunction [5, 6]. Upregulation of ET-1 induced by hypoxia inducible factor-1 alpha (HIF-1α), the main regulator of hypoxic stress, is among the important factors of various cardiovascular diseases [7]. Although a variety of mitosis signaling pathways and transcription factors can regulate expression of ET-1 [8, 9], during hypoxia HIF-1α dominates the regulation of ET-1 expression [10]. There is a complex relationship between ET-1 and HIF-1α. A recent study shows that knockdown of HIF-1α downregulates ET-1 expression in endothelial cells, and overexpression of HIF-1α upregulates ET-1 expression. Interestingly, HIF-1α depletion not only inhibits hypoxia-induced apoptosis in endothelial cells through suppressing ET-1 expression, but also arrests cell proliferation [11]. Proliferation of endothelial cells is of great importance to the repair of injured vessels during hypoxia conditions. The activity of HIF-1α, an early element responsive to hypoxia, is increased during hypoxia, which promotes the proliferation of endothelial cells by stimulating the transcription of vascular endothelial growth factor (VEGF), a mechanism for self-protection against hypoxic injury in endothelial cells [12, 13]. Therefore, the response of HIF-α during hypoxia conditions plays a dual role in endothelial cells, and to give full play to its positive role and inhibit its negative role, it is necessary to further the study on the relationship between HIF-1α and ET-1.
For this purpose, we first demonstrated how HIF-1α regulates ET-1 expression via CCAAT/enhancer binding protein beta (C/EBP β). On this basis, we blocked hypoxia-induced ET-1 expression by knocking down C/EBP β, a middle link of the HIF-1α/C/EBP β/ET-1 pathway, so the expression of HIF-1α was not affected. By this way, we can make use of the HIF-1α/C/EBP β/ET-1 pathway to inhibit apoptosis, but will not impair the HIF-1α/VEGF pathway to resist hypoxia. We think this will guide the development of new therapies for OSAHS characterized by IH injury.
Materials and methods
Cell culture
HUVECs used in this study were purchased from Invitrogen and maintained in M200 (containing LSGS) supplemented with 10% fetal bovine serum (FBS) and passaged by trypsinization [14]. 293T used for co-transfection in luciferase experiment and production of recombinant virus were purchased from Cell Bank of China Academy of Science (CCAS, Shanghai, China), maintained in Dulbecco’s Modified Eagle Medium (DMEM) supplemented with 10% FBS, passaged by trypsinization, and cultured at 5% CO2 and 37 °C. All reagents for cell culture were purchased from Invitrogen (CA, USA). HUVECs were cultured at 37 °C with 5% CO2 and 95% air for normoxia, and 94% N2, 5% CO2, and 1% air for hypoxia, and at an IH (5 min hypoxia/10 min normoxia).
Effects of (sustained hypoxia) SH and IH on HIF-1α, C/EBP β, and ET-1 proteins in HUVECs
The suspension of HUVECs in logarithmic phase were prepared in M200 supplemented with 10% FBS and the number of viable cells was counted with a hemocytometer by trypan blue staining. Cells were seeded to six-well plates at a concentration of 2 × 106 cells per well and maintained in normoxia for 24 h. Then, cells were exposed to SH or IH for 1 h, 3 h, 6 h, 12 h, and 24 h and collected for detection of HIF-1α, C/EBP β, and ET-1 by western blotting.
Lentiviral mediated RNA interference of HIF-1α or C/EBP β in HUVECs
Construction of siRNA plasmids
siRNA sequences were designed to target HIF-1α (NM_001530.3) and C/EBP β (NM_005194): siRNA-HIF-1α, 5′-GAATTACCGAATTGATGGG-3′; siRNA-C/EBP β, 5′-GTGGCCAACTTCTACTACG-3′, respectively. A siRNA-scramble sequence, 5′-CTGTAAAGATGAGTGATGC-3′, was used as a negative control (NC). The complementary double chains were designed and chemically synthesized and cloned into the pSIH1-shRNA vector (System Biosciences, CA, USA); the resulting vectors were named pSIH1-HIF-1α, pSIH1-C/EBP β, and pSIH1-NC.
Construction of recombinant lentivirus
Following the manufacturer’s instructions, the expression vectors and Lentivirus Package plasmid mix (System Biosciences) were co-transfected into 293T producer cells using Lipofectamine™ 2000 (Invitrogen). Forty-eight hours later, the supernatants were collected and cleared by centrifugation and filtering through 0.45-μm polyvinylidene fluoride (PVDF) membranes (Millipore, WI, USA). Viral titer was evaluated by gradient dilution. The packaged lentiviruses were named Lv-shRNA-HIF-1α, Lv-shRNA-C/EBP β, and Lv-NC.
Lentiviral infection of HUVECs
Suspensions of HUVECs in logarithmic phase were prepared in M200 supplemented with 10% of FBS, and the number of viable cells was counted by a hemocytometer via trypan blue staining. Cells were seeded on to six-well plates at a concentration of 2 × 106 cells per well and maintained in normoxia for 24 h. The cells were divided into five groups: (1) control (not infected); (2) NC control (cells infected with Lv-NC); (3) HIF-1α silencing group (cells infected with Lv-shRNA-HIF-1α); (4) C/EBP β silencing group (cells infected with Lv-shRNA-C/EBP β); and (5) HIF-1α and C/EBP β silencing group (cells infected with Lv-shRNA-HIF-1α and Lv-shRNA-C/EBP β). After overnight culture, cells were treated with the corresponding lentivirus at a multiplicity of infection (MOI) of 20 and cultured for 72 h. Cells were collected, and western blotting was used to measure HIF-1α, C/EBP β and ET-1 levels to determine the efficiency of the genetic intervention.
Validation of binding site of C/EBP β in ET-1 promoter by luciferase assay
Prediction by bioinformatics
We retrieved the sequence of human ET-1 gene and found its location in human genome from NCBI (National Center for Biotechnology Information), selected the 2500-bp DNA sequence upstream to the transcription start site, and predicted and obtained the core promoter (a 950-bp sequence) using Promoter 2.0. Then, a theoretic binding site (5′-GCCACC-3′) was identified by using TRANSFAC to predict all binding sites of C/EBP β on ET-1’s promoter.
Construction of vectors
HUVECs in logarithmic phase (approximately 5 × 106 cells) were collected, total RNA was extracted using Trizol (Invitrogen), and cDNA was prepared by reverse transcription. The PCR primers 5′-CGGAATTCGCCACCATGCAACGCCTGGTGGC-3′ and 5′-CGGGATCCCTAGCAGTGGCCGGAGGA-3′, which contain an EcoR I cutting site, kozak sequence(5′-GCCACC-3′), and a BamH I cutting site, respectively, were used to amplify the CD sequence of the C/EBP β gene. The PCR product was digested and cloned into the pcDH vector (System Biosciences), and the resultant vector was named pcDH-C/EBP β. HUVECs (approximately 5 × 106 cells) were collected, and genomic DNA was extracted for amplification of the ET-1 promoter. The PCR primers 5′-CCGCTCGAGATAGATGCAAAGAACTTCAGCAA-3′ and 5′-CCCAAGCTTTTCAAACTGAACCCAAAG-3′, which contain an Xho I site and a Hind III site, respectively, were used to amplify a 950-bp sequence containing the predicted binding site for C/EBP β, 5′-GTTGCCTGTTG-3′. The PCR product was digested and cloned into pGL3-basic vector (Promega, MI, USA), and the result vector was named pGL3-WT-ET-1. Meanwhile, a reporter vector containing mutant binding site was prepared by point mutation which mutated 5′-GTTGCCTGTTG-3′ to 5′-TGTGGTCGCTT-3′; the result vector being named pGL3-MT-ET-1. The products of all cloning and mutagenesis reactions were confirmed by DNA sequencing and endotoxin free DNA was prepared in all cases.
Luciferase assay
Suspensions of 293T cells at passage 3 were prepared in DMEM supplemented with 10% FBS, and the number of viable cells was counted with a hemocytometer by trypan blue staining. Cells were seeded to six-well plates at a concentration of 2 × 105 cells per well and maintained at 37 °C and 5% CO2 for 24 h. Transfection was conducted using Lipofectamine2000 according to the manufacturer’s instructions, with 100 ng pGL-TK (Promega) used as a reference of luciferase activity detection. Luciferase activities were measured by the dual luciferase reporter assay system (Promega) 48 h after transfection. Cells were divided into nine groups: a control group (not transfected), cells transfected with pGL3-WT-ET1, pGL3-WT-ET1 + pSIH-shRNA-NC, pGL3-WT-ET1 + pcDH-C/EBP β, pGL3-WT-ET1 + pSIH-shRNA-C/EBP β, pGL3-MT-ET1, pGL3-MT-ET1 + pSIH-shRNA-NC, pGL3-MT-ET1 + pcDH-C/EBP β, or pGL3-MT-ET1 + pSIH-shRNA-C/EBP β.
Detection of effects of blocking C/EBP β on ET-1 or VEGF expression in HUVECs exposed to IH
Suspensions of HUVECs were prepared by trypsin digestion in M200 supplemented with 10% FBS 72 h after being infected with the lentivirus. The cells were plated into six-well plates at a concentration of 2 × 106 cells per well and maintained in IH for 12 h. The cells were collected, and total protein was extracted for detection of ET-1 and VEGF by western blotting. The cells were divided into five groups: a normoxia control group, IH group, LV-NC + IH group, Lv-shRNA-HIF-1α + IH group, and Lv-shRNA-C/EBP β + IH group.
Effects of C/EBP β silencing on apoptosis, cellular proliferation, and ability of tube formation in HUVECs exposed to IH
The cells were divided into four groups: a normoxia control group, IH group, LV-NC + IH group, and Lv-shRNA-C/EBP β + IH group. HUVECs, in which C/EBP β expression was knocked down by lentivirus, were exposed to IH for 12 h, and apoptosis was detected using the Annexin V:FITC Apoptosis Detection Kit II (BD Biosciences, NJ, USA). The cells were washed with Dulbecco’s Phosphate-Buffered Saline (dPBS, pH = 7.4) twice (2000×g, 5 min), resuspended in 500-μL binding buffer with 5 μL Annexin V-FITC in the dark for 10 min and, then, stained with 5 μL propidium iodide (PI) for 5 min. Apoptosis was analyzed at an excitation wavelength of 488 nm using the FL1 channel for Annexin V-FITC and the FL2 channel for PI.
HUVECs in logarithmic phase, seeded to six-well plates at 2 × 105 cells/well, were infected with Lv-NC or Lv-shRNA-HIF-1α or Lv-shRNA-C/EBP β for 72 h. The cells were then exposed to IH for 12 h and used for proliferation analysis. Suspensions of HUVECs that had undergone gene intervention and IH were prepared, and the number of viable cells was counted with a hemocytometer by trypan blue staining. Cells were plated into 96-well plates at a concentration of 1 × 104 cells per well and incubated under normal conditions. Viabilities were examined via Cell Counting Kit-8 (CCK-8, Dojindo, Japan). At 12, 24, and 48 h of incubation, cells were treated with CCK-8 (10 μL/well) solution and then incubated at 37 °C and 5% CO2 for 4 h before the absorbency was measured (optic density, OD) at 450 nm.
The tube formation assay was conducted in IH. The cells were divided into four groups: an IH group, LV-NC + IH group, Lv-shRNA-HIF-1α + IH group, and Lv-shRNA-C/EBP β + IH group. Ten microliters of Matrigel (BD Biosciences) at 4 °C was added to each well of precooled 96-well plates using precooled tips and dispensed evenly by shaking the plate. The plate was cooled on ice for 2 min and then incubated in a cell culture incubator for 30 min. The concentration of trypsinized cell suspension (1 × 105 cells/mL) was measured by live cell counting. The HUVECs 72 h after being infected with the lentivirus were seeded into the pre-incubated plate at 100 μL/well and incubated under IH. Photos were acquired on an inverted fluorescence microscopic 6 h later.
Detection of protein contents
The concentration of the protein sample was measured by BCA protein assay (Pierce, IL, USA) according to the manufacturer’s instructions. Protein samples (10 μg/lane) were separated by 11% Sodium dodecyl sulfate-polyacrylamide gel electrophoresis (SDS-PAGE) at 110 V for 90 min, and the gel was stained with Ponceau S. The proteins were transferred to PVDF membranes using wet transfer (400 mA, 90 min). The membranes were blocked in tris-buffered saline with Tween 20 (TBST) containing 5% non-fat milk at room temperature for 2 h and incubated with primary antibodies (Santacruz, CA, USA) (β-actin, 1:300; HIF-1α, 1:200; C/EBP β, 1:400; ET-1, 1:600; VEGF, 1:350) at 4 °C overnight. The blots were then rinsed with TBST three times and incubated with a secondary antibody (Santacruz) (rabbit anti-mouse IgG, 1:3000) for 2 h. ECL chemiluminescence substrates (Pierce) and X-ray film were used to detect the bands, and relative optical densities were analyzed with the image processing software “Totallab V1.10”; relative contents of proteins were calculated by dividing the optical density of the target band with the optical density of the β-actin band.
Statistical method
Statistical analysis was performed with a Statistical Package for Social Science (SPSS) software version 13.0 (SPSS Inc., USA). Protein expression difference analysis was conducted on the basis of the control group. All results were expressed as mean ± S.D. The differences between two groups were determined by t test for parametric data. A p value < 0.05 was considered statistically significant for all analysis.
Results
Effects of SH and IH on HIF-1α, C/EBP β, and ET-1 proteins in HUVECs
HUVECs were exposed to two different hypoxia modes for 0–24 h, and the expression of protein HIF-1α, C/EBP β, and ET-1 were significantly increased, but the pattern of changes varied widely from each of the three proteins. HIF-1α increased first with the highest appearing at 3 h and then decreased to the 24 h for the SH group (t = 4.213, P = 0.003 at 3 h; t = 4.161, P = 0.004 at 6 h; t = 2.971, P = 0.021 at 12 h; vs the group at 0 h). For the IH group the HIF-1α expression increased with time passing (t = 2.515, P = 0.042 at 6 h; t = 3.756, P = 0.007 at 12 h; t = 4.441, P = 0.002 at 24 h; vs the group at 0 h). C/EBP β increased continuously over the 24 h in HUVECs exposed to SH (the highest point at 24 h; t = 2.624, P = 0.031 at 12 h; t = 3.501, P = 0.008 at 24 h; vs the group at 0 h) but increased and then decreased in cells exposed to IH (the highest point at 3 h to 6 h; t = 2.432, P = 0.027 at 3 h; t = 2.896, P = 0.024 at 6 h; t = 2.107, P = 0.035 at 12 h; vs the group at 0 h). ET-1 increased continuously over the 24 h in HUVECs exposed to SH (the highest point at 24 h; t = 2.423, P = 0.033 at 12 h; t = 3.866, P = 0.007 at 24 h; vs the group at 0 h) but increased and then decreased in cells exposed to IH (the highest appearing at 6 h; t = 2.624, P = 0.031 at 6 h; t = 2.702, P = 0.043 at 24 h; vs the group at 0 h). IH has its peak impact more rapidly than SH, but that the overall size of the impact of each are similar if you compare time points 24 h (SH) with 6 h (IH). Based on the data ET-1 protein, we draw a conclusion that the expression of ET-1 induced by IH is more intense than SH in light of the protein level change with time (t = 4.374, P = 0.004, at 6 h; t = 2.128, P = 0.039 at 24 h; vs the group exposed to SH) (Fig. 1).
Effects of SH and IH on HIF-1α, C/EBP β, and ET-1 proteins in HUVECs. HUVECs were subjected to SH or IH for 24 h and western blotted for HIF-1α (124 kDa), C/EBP β (30 kDa), and ET-1 (28 kDa). Upper panels represent the optical density of the target band divided by the optical density of the β-actin (43 kDa) band. Lower panels show representative blots. Data are expressed as the mean ± SD of at least three independent experiments. *p < 0.05; **p < 0.01, relative to the group at 0 h
Lentiviral mediated RNA interference to HIF-1α or C/EBP β in HUVECs
Recombinant lentiviruses were constructed and used to infect HUVECs at an MOI of 20, and GFP marker was observed by fluorescence microscopy 72 h later. The difference between cells expressing GFP (right) and the total number of cells (left) indicated a delivery efficiency close to 100% (Fig. 2a). The results of western blotting showed that the expression of HIF-1α, C/EBP β, and ET-1 in HIF-1α gene silencing group significantly decreased (t = 3.681, P = 0.007 vs uninfected control group and t = 3.894, P = 0.006 vs NC control group for HIF-1α; t = 4.135, P = 0.005 vs uninfected control group and t = 4.004, P = 0.005 vs NC control group for C/EBP β; t = 2.551, P = 0.035 vs uninfected control group and t = 2.331, P = 0.041 vs NC control group for ET-1). There was no significant change in the expression of HIF-1α protein in the C/EBP β silencing group while the expression of C/EBP β and ET-1 protein decreased significantly (t = 4.512, P = 0.002, vs uninfected control group and t = 4.324, P = 0.003, vs NC control group for C/EBP β; t = 4.102 P = 0.004, vs uninfected control group and t = 4.219, P = 0.003, vs NC control group for ET-1). The expression of HIF-1α, C/EBP β, and ET-1 protein in HIF-1α and C/EBP β silencing groups decreased significantly (t = 3.916, P = 0.007, vs uninfected control group and t = 4.006, P = 0.004, vs the NC control group for HIF-1α; t = 3.753, P = 0.008, vs uninfected control group and t = 4.321, P = 0.003, vs the NC control group for C/EBP β; t = 4.266, P = 0.003, vs uninfected control group and t = 3.715, P = 0.006, vs the NC control group for ET-1. Fig. 2b). In addition to displaying efficiency of the HIF-1α and C/EBP β gene silencing mediated by lentivirus pathway, it is more important to demonstrate the upstream and downstream relations between HIF-1α, C/EBP β, and ET-1, namely, HIF-1α and ET-1 locating at the upper and lower, and C/EBP β at the middle of the pathway HIF-1α/C/EBP β/ET-1.
Knockdown of HIF-1α and C/EBP β via lentivirus. a HUVECs were infected with the Lv-shRNA-HIF-1α and Lv-shRNA-C/EBPβ for 72 h. GFP was detected, and the proportion of GFP-expressing cells suggested that the gene delivery efficiency was higher than 90% in all cases. b HUVECs were infected with the lentiviruses for 72 h and subjected to western blotting detection for HIF-1α, C/EBP β, and ET-1 proteins. Upper panels: the optical density of the target band divided by the optical density of the β-actin band. Lower panels: representative blots. Data are expressed as the mean ± SD of at least three independent experiments. *p < 0.05; **p < 0.01, relative to the group uninfected or infected with the Lv-NC
Effect of E/CBP β gene knockdown on expression of ET-1 and VEGF protein in HUVEC cells under IH exposure
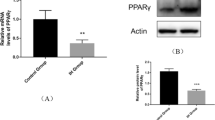
The results of ET-1 and VEGF protein showed that (Fig. 3), when exposed HUVECs to IH for 12 h, the expression of ET-1 and VEGF protein in HUVECs increased significantly (t = 4.882, P = 0.002 vs normal oxygen level control group for ET-1; t = 4.762, P = 0.002 vs normal oxygen level control group for VEGF). The expression of ET-1 and VEGF protein in HIF-1α gene silencing combined IH group significantly declined (t = 3.703, P = 0.007 vs IH exposure; t = 3.913, P = 0.005 vs Lv-NC infection combined IH exposure group for ET-1; t = 4.511, P = 0.002 vs IH exposure; t = 3.798, P = 0.008 vs Lv-NC infection combined IH exposure group for VEGF), C/EBP β silencing and overexpression significantly reduced and upregulated ET-1 expression (t = 3.802, P = 0.006 vs Lv-shRNA-HIF-1α infection combined IH exposure group; t = 3.961,P = 0.006 vs IH exposure group), and C/EBP β silence had no significant effect on the expression of VEGF protein (t = 1.021, P = 0.081, vs IH exposure group), which was consistent with results of Fig. 5a showing the apoptosis, proliferation, and cell tube formation.
Effect of intervention of C/EBP β on the ET-1 and VEGF protein in HUVEC with IH. HUVECs were infected with the indicated lentiviruses for 72 h and then subjected to western blotting to detect ET-1 (a) and VEGF protein (b). Upper panel: the optical density of the target band divided by the optical density of the beta-actin band; lower panel: representative blots. Data are expressed as the mean ± SD of at least three independent experiments. **p < 0.01
Validation of binding site of C/EBP β in the ET-1 promoter by luciferase assay
According to bioinformatics analysis, there is a predicted binding site for C/EBP β, 5′-GTTGCCTGTTG-3′ in the ET-1 promoter. Luciferase reporter vectors were constructed to verify the binding site. In cells transfected with the reporter vectors containing the wild-type C/EBP β binding site, overexpression of C/EBP β further increased luciferase activity from 26.31 ± 3.55 to 60.08 ± 8.91 (t = 2.262, P = 0.025), and silencing C/EBP β decreased luciferase activity from 26.31 ± 3.55 to 5.12 ± 0.72 (t = 2.072, P = 0.048). In the group transfected with the luciferase reporter vector carrying the mutant C/EBP β binding site, the luciferase activity did not respond to C/EBP β interventions (t = 1.021, P = 0.137). NC co-transfection had no observable effect on luciferase activity (t = 0.987, P = 0.155) (Fig. 4). These results suggest that C/EBP β regulates the ET-1 gene through the TFBS.
Validation of binding site of C/EBP β in ET-1 promoter. 293T cells were transfected with the indicated vectors and subjected to luciferase activity assay 48 h later. Data are expressed as the mean ± SD of at least three independent experiments. **p < 0.01, relative to the group transfected with the same vector but without the pcDH-CEBP β or pSIH-CEBP β
Effects of C/EBP β silencing on apoptosis, proliferation, and tube formation in HUVECs exposed to IH
Exposure of IH for 12 h increased apoptosis by 7.12-fold (t = 4.031, P = 0.005, vs normoxia group), and C/EBP β silencing effectively inhibited apoptosis induced by IH (t = 2.511, P = 0.030, vs IH group) (Fig. 5a). Cell proliferation activity test showed that the proliferation activity in normal or C/EBP β silencing + IH group were significantly higher than that in IH or NC + IH or HIF-α silencing + IH groups (t = 4.673, P = 0.003, vs IH or NC + IH or HIF-α silencing + IH group, 48 h); there was no significant difference between normal and IH groups(t = 1.114, P = 0.092), and there was no significant difference among the three groups of IH and NC + IH and HIF-α silencing + IH groups (t = 1.742, P = 0.059) (Fig. 5b). In vitro tube formation experiment showed the tube formation activity of HIF-1α gene silencing group declined under IH exposure (t = 4.451, P = 0.004, vs IH exposure or Lv-NC infection and IH exposure group); the tube formation cell viability of C/EBP β gene silencing group did not changed significantly (t = 1.528, P = 0.062, vs IH exposure group or Lv-NC infection and IH exposure group). These results suggest HIF-1α silencing, but not C/EBP β, inhibited tube formation by endothelial cells in IH for 6 h (Fig. 5c).
Effects of C/EBP β silencing on apoptosis, cell proliferation, and in vitro tube formation in HUVECs exposed to IH. a HUVECs were infected with the indicated lentiviruses, exposed to IH for 12 h and, then, subjected to apoptosis analysis. Left: the apoptosis rate (early + later) of the indicated group, right: representative plots. b HUVECs were infected with the indicated lentiviruses and exposed to IH for 12 h and then seeded to 96-well plates and subjected to cell vitality assays at the indicated time (12–48 h). c HUVECs were infected with the indicated lentiviruses and subjected to in vitro tube formation assays while exposed to IH for 6 h. Left: representative images; right: tube counting data. Data are expressed as the mean ± SD of at least three independent experiments. *p < 0.05; **p < 0.01, relative to the group uninfected or infected by Lv-NC
Discussion
Hypoxia inducible factor-1 (HIF-1) was first found by Semenza et al. in 1991 and is a protein that could specifically bind to the oligonucleotide sequence of the erythropoietin gene enhancer [15]. ET-1, an important cytokine first reported in 1988, plays crucial roles in hypertension and other cardiovascular diseases due to its potent function to contract vessels [16]. As an independent risk factor in cardiovascular diseases, ET-1 has become a target in the study of sleep apnea studies. ET-1 levels in the hypertensive patients complicated with OSAHS were higher than in those patients without OSAHS [17]. As a nuclear transcription factor, HIF-1α can upregulate ET-1 expression in hypoxia [18, 19]. In the OSA mouse model, activation of ET-1 by HIF-1α is associated with vascular remodeling [20], which was exactly consistent with our confirmed data (Fig. 1). According to the current researches, the high expression of ET-1 is beneficial for endothelial cell injury healing caused by hypoxia while HIF-1α shows a dual effect of resisting damage and promoting damage. On the one hand, as the start of hypoxia response, the expression of HIF-1α can promote the proliferation of endothelial cells in the hypoxic environment by upregulating the expression of downstream gene VEGF, which promotes angiogenesis allowing a strong hypoxic damage tolerance [21, 22]. On the other hand, the high expression of HIF-1α may induce endothelial cell apoptosis by upregulating the ET-1expression [23, 24]. Therefore, we are very interested in the upstream and downstream relations between HIF-1 alpha and ET-1 and their specific actions. If we can fully understand the regulation mechanism between HIF-1α and ET-1, it is possible to start with the intermediate link of the pathway, inhibiting the expression of ET-1 and retaining the hypoxia tolerance activity of HIF-1α, thus getting a significant hypoxia tolerance solution.
At the beginning of the study, we predict the promoter region of human ET-1 through the bioinformatics software Promoter2.0 followed by predicting the ET-1 promoter nuclear transcription factor which may have theoretical binding sites on it through the transcription factor analysis and prediction software TRANSFAC, and the data showed that there was no binding site for HIF-1α. At this point, we thought that HIF-1α might regulate ET-1 transcription in an indirect way, that is to say, between HIF-1α and ET-1, there exists a key intermediate link. We continued to detect the expression of the nuclear transcription factors theoretically binding to the ET-1 promoter in the endothelial cells under IH exposure and found that the protein expression of the nuclear factor C/EBP β and the content of ET-1 are entirely positive correlated in HUVECs under the condition of normal oxygen and IH exposure.
C/EBPs, a family of transcription factors, including six members-C/EBPα, β, γ, δ, ε, and ζ, are involved in multiple cellular functions [25]. Although research has shown that C/EBPs play an important role in high glucose-induced increased expression of ET-1 in human endothelial cells [26], it is unclear whether C/EBPs play a similar role in the regulation of ET-1 in hypoxia. Research has shown that C/EBP family members play an important role in the regulation of HIF-1α in extreme hypoxia [27]. TATA and CAAT boxes are two highly conservative mammalian promoter elements that exist at about – 150 bp away from the ET-1 gene. Both are necessary for transcriptional activity, and the latter is a common cis-acting element recognized by C/EBP family members [28]. This indicates that C/EBP β is highly likely to be the link we are searching for between HIF-1α and ET-1. In fact, we first demonstrated that C/EBP β does have TFBS 5′-GTTGCCTGTTG-3′ on the ET-1 gene promoter by a luciferase reporter gene experiment, and we also determined the relationship between the three by knocking down each of HIF-1α, C/EBP β, and ET-1 protein and detecting the other two proteins, that is, HIF-1α/C/EBP β/ET-1. We even demonstrated the specificity of the HIF-1α/C/EBP β /ET-1 pathway by blocking the link between HIF-1α and ET-1 through the C/EBP β gene.
Based on comparing the correlation of the expression of HIF-1α, C/EBP β, and ET-1 in HUVECs under IH exposure, this study demonstrated and expanded the knowledge of the HIF-1α /C/EBP β /ET-1 pathway of endothelial cell hypoxia injury and finally confirmed the existence of this pathway. Based on this, we blocked the expression of the downstream function gene ET-1 through silencing target intermediate link C/EBP β, but did not affect the function of hypoxia tolerance of the upstream gene HIF-1α. The functional experiment showed that C/EBP β silencing could effectively inhibit the apoptosis of HUVECs induced by IH and had no obvious effect on the proliferation activity and tube formation of endothelial cells under the HIF-Iα-VEGF dominated IH condition. As can be clearly seen from our data, VEGF, the classic downstream gene of HIF-1α, is not interfered with by silencing C/EBP β. The finding that knockdown of C/EBP β in HUVECs to inhibit ET-1 without affecting the upstream HIF-1α is important. In terms of protecting cells from hypoxia-induced injury, silencing C/EBP β suppressed apoptosis, while the beneficial effects of HIF-1α could directly regulate factors downstream, such as VEGF [29, 30], to help protect cells against injury.
Conclusion
In IH environment, the pathway of HIF-1α /C/EBP β /ET-1 dominates the pathological process of endothelial cell injury. Targeted knockout of C/EBP β can effectively inhibit the apoptosis of endothelial cells induced by IH through inhibiting the expression of ET-1. At the same time, it does not affect the hypoxia damage tolerance pathway and function of HIF-1α. Generally, C/EBP β is a promising target against intermittent hypoxia-induced damage of endothelial cells and a target for the gene therapy of OSAHS.
Abbreviations
- SH:
-
Sustained hypoxia
- IH:
-
Intermittent hypoxia
- OSAHS:
-
Obstructive sleep apnea-hypopnea syndrome
- HIF-1α:
-
Hypoxia-inducible factor 1-alpha
- C/EBP β:
-
CCAAT/enhancer binding protein beta
- HUVECs:
-
Human umbilical vein endothelial cells
- ET-1:
-
Endothelin-1
- VEGF:
-
Vascular endothelial growth factor
- TFBS:
-
Transcription factor binding site
- FBS:
-
Fetal bovine serum
- MOI:
-
Multiplicity of infection
- TBST:
-
Tris-buffered saline with Tween 20
- PVDF:
-
Polyvinylidene fluoride
- SDS-PAGE:
-
Sodium dodecyl sulfate-polyacrylamide gel electrophoresis
References
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence ofsleep-disordered breathing among middle-aged adults. N Engl J Med 328:1230–1235
Ma L, Zhang J, Liu Y (2016) Roles and mechanisms of obstructive sleep apnea-hypopnea syndrome and chronic intermittent hypoxia in atherosclerosis: evidence and prospective. Oxidative Med Cell Longev 2016:8215082
He J, Kryger MH, Zorick FJ, Conway W, Roth T (1998) Mortality and apnea index in obstructive sleep apnea. Experience in 385 male patients. Chest 94:9–14
McNicholas WT, Bonsignore MR (2007) Sleep apnoea as an independent risk factor for cardiovascular disease: current evidence, basic mechanisms and research priorities. Eur Respir J 29:156–178
Zamarron-Sanz C, Ricoy-Galbaldon J, Gude-Sampedro F, Riveiro-Riveiro A (2006) Plasma levels of vascular endothelial markers in obstructive sleep apnea. Arch Med Res 37:552–555
Gjorup PH, Wessels J, Pedersen EB (2008) Abnormally increased nitric oxide synthesis and increased endothelin-1 in plasma in patients with obstructive sleep apnoea. Scand J Clin Lab Invest 68:375–385
Pernow J, Shemyakin A, Böhm F (2012) New perspectives on endothelin-1 in atherosclerosis and diabetes mellitus. Life Sci 91:507–516
Quehenberger P, Bierhaus A, Fasching P, Muellner C, Klevesath M, Hong M, Stier G, Sattler M, Schleicher E, Speiser W, Nawroth PP (2000) Endothelin-1 transcription is controlled by nuclear factor-kappa B in AGE-stimulated cultured endothelial cells. Diabetes 49:1561–1570
Manea SA, Manea A, Heltianu C (2010) Inhibition of the JAK/STAT signaling pathway prevents high glucose-induced increase in endothelin-1 synthesis in human endothelial cells. Cell Tissue Res 340:71–79
Stow LR, Jacobs ME, Wingo CS, Cain BD (2011) Endothelin-1 gene regulation. FASEB J25:16–28
YunCheng Tai (2016) The regulation and mechanism of the permeability of rat vascular endothelial. Anhui Medical University
Jeon M, Shin Y, Jung J, Jung UW, Lee JH, Moon JS, Kim I, Shin JS, Lee SK, Song JS (2018) HIF1A overexpression using cell-penetrating DNA-binding protein induces angiogenesis in vitro and in vivo. Mol Cell Biochem 437(1–2):99–107
Yang C, Xu Y, Zhou H, Yang L, Yu S, Gao Y, Huang Y, Lu L, Liang X (2016) Tetramethylpyrazine protects CoCl2-induced apoptosis in human umbilical vein endothelial cells by regulating the PHD2/HIF/1α-VEGF pathway. Mol Med Rep 13(2):1287–1296
Li X, Gao Y, Li J, Zhang K, Han J, Li W, Hao Q, Zhang W, Wang S, Zeng C, Zhang W, Zhang Y, Li M, Zhang C (2018) FOXP3 inhibits angiogenesis by downregulating VEGF in breast cancer. Cell Death Dis 9(7):744
Semenza GL, Nejfelt MK, Chi SM, Antonarakis SE (1991) Hypoxia-inducible nuclear factors bind to an enhancer element located 3′ to the human erythropoietin gene. Proc Natl Acad Sci U S A 88:5680–5684
Bourque SL, Davidge ST, Adams MA (2011) The interaction between endothelin-1 and nitric oxide in the vasculature: new perspectives. Am J Physiol Regul Integr Comp Physiol 300:R1288–R1295
Yanagisawa M, Kurihara H, Kimura S, Tomobe Y, Kobayashi M, Mitsui Y, Yazaki Y, Goto K, Masaki T (1988) A novel potent vasoconstrictor peptide produced by vascular endothelial cells. Nature 332:411–415
Hu J, Discher DJ, Bishopric NH, Webster KA (1998) Hypoxia regulates expression of theendothelin-1 gene through a proximal hypoxia-inducible factor-1 binding site on the antisense strand. Biochem Biophys Res Commun 245:894–899
Minchenko A, Caro J (2000) Regulation of endothelin-1 gene expression in human microvascular endothelial cells by hypoxia and cobalt: role of hypoxia responsive element. Mol Cell Biochem 208:53–62
Castro-Grattoni AL (2016) Intermittent hypoxia-induced cardiovascular remodeling is reversed by normoxia in a mouse model of sleep apnea. Chest 149:1400–1408
Sarada SK, Himadri P, Ruma D, Sharma SK, Pauline T, Mrinalini (2008) Selenium protects the hypoxia induced apoptosis in neuroblastoma cells through upregulation of Bcl-2. Brain Res 209:29–39
Kim HG, Hwang YP, Jeong HG (2008) Metallothionein-III induces HIF-1-mediated VEGF expression in brain endothelial cells. Biochem Biophy Res Comm 369:666–671
Salceda S, Caro J (1997) Hypoxia-inducible factor 1(HIF-1) protein is rapidly degraded by the ubiquitin-proteasome system under normoxic conditions. Its stabilization by hypoxia depends on redox-induced changes. J Biol Chem 272:22642–22647
Hamrick SE, McQuillen PS, Jiang X, Mu D, Madan A, Ferriero DM (2005) A role for hypoxia-inducible factor-1a in desferoxamine neuroprotection. Neurosci Lett 379:96–100
Poli V (1998) The role of C/EBP isoforms in the control of inflammatory and native immunity functions. J Biol Chem 273:29279–29282
Manea SA, Todirita A, Manea A (2013) High glucose-induced increased expression of endothelin-1in human endothelial cells is mediated by activated CCAAT/enhancer-binding proteins. PLoSOne 8:e84170
Jiang C, Sun J, Dai Y, Cao P, Zhang L, Peng S, Zhou Y, Li G, Tang J, Xiang J (2015) HIF-1A and C/EBPs transcriptionally regulate adipogenic differentiation of bone marrow-derived MSCs in hypoxia. Stem Cell Res Ther 6:21
Lee ME, Bloch KD, Clifford JA, Quertermous T (1990) Functional analysis of theendothelin-1 gene promoter. Evidence for an endothelial cell-specific cis-acting sequence. J Biol Chem 265:10446–10450
Surazynski A, Donald SP, Cooper SK, Whiteside MA, Salnikow K, Liu Y, Phang JM (2008) Extracellular matrix and HIF-1 signaling: the role of prolidase. Int J Cancer 122(6):1435–1440
Fang J, Zhou Q, Liu LZ, Xia C, Hu X, Shi X, Jiang BH (2007) Apigenin inhibits tumor angiogenesis through decreasing HIF-1alpha and VEGF expression. Carcinogenesis 28(4):858–864
Funding
The National Natural Science Foundation of China provided financial support in the form of national natural science funding (No. 81372529), the Natural Science Fund Project of Shanghai (13ZR1414400); the Innovation Fund Project of Education Commission in Shanghai (14ZZ079); and the Special issue of the Military Medical of Second Military Medical University (2012JS21). The sponsor had no role in the design or conduct of this research.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Additional information
Yu Feng and Qingchu Li contributed equally to this work.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Feng, Y., Li, Q., Wu, Y. et al. Blocking C/EBP β protects vascular endothelial cells from injury induced by intermittent hypoxia. Sleep Breath 23, 953–962 (2019). https://doi.org/10.1007/s11325-018-1759-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-018-1759-7