Abstract
Background
Portugal has one of the highest road traffic fatality rates in Europe. A clear association between sleep-disordered breathing (SDB) and traffic accidents has been previously demonstrated. This study aimed to determine prevalence of excessive daytime sleepiness (EDS) and other sleep disorder symptoms among truck drivers and to identify which individual traits and work habits are associated to increased sleepiness and accident risk.
Methods
We evaluated a sample of 714 truck drivers using a questionnaire (244 face-to-face interviews, 470 self-administered) that included sociodemographic data, personal habits, previous accidents, Epworth Sleepiness Scale (ESS), and the Berlin questionnaire (BQ).
Results
Twenty percent of drivers had EDS and 29 % were at high risk for having obstructive sleep apnea syndrome (OSAS). Two hundred sixty-one drivers (36.6 %) reported near-miss accidents (42.5 % sleep related) and 264 (37.0 %), a driving accident (16.3 % sleep related). ESS score ≥11 was a risk factor for both near-miss accidents (odds ratio (OR) = 3.84, p < 0.01) and accidents (OR = 2.25, p < 0.01). Antidepressant use was related to accidents (OR = 3.30, p = 0.03). We found an association between high Mallampati score (III–IV) and near misses (OR = 1.89, p = 0.04).
Conclusion
In this sample of Portuguese truck drivers, we observed a high prevalence of EDS and other sleep disorder symptoms. Accident risk was related to sleepiness and antidepressant use. Identifying drivers at risk for OSAS should be a major priority of medical assessment centers, as a public safety policy.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Traffic accidents are still a serious problem all over the world. Portugal, in particular, keeps a bad reputation for poor driving and a long-time record at the top of the tables for European road fatalities. Indeed, it ranks seventh in Europe, with a number of deaths per million considerably higher than the European average (79 vs. 62) [1].
Truck accidents are a significant public health hazard as far as they are usually associated to severe crashes. It has been estimated that more than half of such crashes involve fatal or incapacitating injuries and the truck driver is found at fault in more than 80 % of the cases [2].
Sleep seems to be related to 15 to 20 % of all accidents. It has been reported that driving skill impairment from sleepiness can even surpass those from alcohol and other drugs, such as antidepressants and antihistamines [3, 4]. Sleep disorders are the most common sources of daytime fatigue and drowsiness. Moreover, a broad variety of factors that characterize truck driving work are also potential contributors to fatigue and crash-related outcomes [5–8]. Thus, a comprehensive multifactorial approach is required to address them successfully.
The most common type of sleep-disordered breathing (SDB) is obstructive sleep apnea syndrome (OSAS). OSAS has been reported to affect approximately 5 % of the general population [9]. However, it appears to be much more common among professional drivers, with an estimated prevalence of 17–28 % [10, 11]. Several studies have shown a clear association between SDB and increased accidents risk [3, 5, 12]. It is estimated that OSAS patients have a two- to sevenfold increased risk of crashes and that these crashes are three to five times more likely to result in personal injuries [13, 14].
One of the major risk factors for OSAS is obesity. This relationship is important, since the body mass index (BMI) may help us to predict the prevalence of sleep apnea in any population of drivers, with an even better reliability than self-reports of sleepiness [10, 15]. The BMI appears not only to be related to an increased risk of crash in patients with OSAS, but also with a higher severity of the disorder. Based on this evidence, the consensus screening criteria published by the American Joint Task Force [16] takes into account the BMI, neck circumference, and blood pressure. Recent studies have shown that these physical measurements associated with the Epworth Sleepiness Scale (ESS) and self-reported history of symptoms and accidents have a high predictive value in detecting drivers with OSAS [2, 17]. However, these screening criteria are still not included in Portuguese and many other countries' medical inspection reports.
This study gives a comprehensive approach of this pathology and addresses lack of related literature in Portugal. Its goals are to determine the prevalence of excessive daytime sleepiness (EDS) and sleep disorder symptoms among commercial truck drivers in north and central Portugal. In addition, it strives to assess individual traits and work habits that are associated to increased sleepiness, near misses, and accidents risk.
Material and methods
We performed a cross-sectional study of commercial truck drivers employed in transportation companies located in the north and center of Portugal.
Participant recruitment and evaluation
Portuguese truck companies operating from the cities of Oporto, Aveiro, Viseu, and Lisbon were selected from the Portuguese Yellow Pages® website. A total of 45 companies were contacted via email. The first approach to the companies took place in July 2011. By September, we had received 11 answers, all of them positive. Later in September, emails were resent to all nonanswering companies. By the end of October 2011, we had received seven more positive answers to this second attempt, completing a final total of 18 companies, which were the core of this investigation. Twenty-seven companies did not give an answer at all and were excluded from the study. No company replied to us in a negative way.
Subsequently, each company's representative was contacted for permission to approach the drivers. The drivers worked either in the transfer (long hauls) or distribution/collection (short hauls) sectors. In each company, all drivers were invited to participate. The companies were visited during the period from August to December 2011.
From the 18 companies that agreed to participate, only six allowed a direct interview with the drivers. Time and logistical issues were the most frequently mentioned reasons for refusal.
In each one of the six companies that allowed a direct approach to the drivers, we arranged one date to visit the company. Interviews took place in the company's office, in one room next to the technical service for employees, where normally the drivers need to go before starting the workday.
Every driver was invited to participate and two researchers performed the interviews individually. Between August and December 2011, 244 drivers (13.1 %) employed in these companies were interviewed by the research team. Neck circumference and Mallampati score were also measured by the researchers.
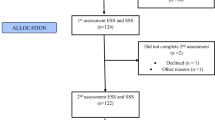
A total of 1,072 questionnaires, the number of employees in the 12 companies where no face-to-face interviews could be conducted, were handed out by the responsible companies to drivers willing to participate, and 470 drivers (43.8 %) completed the questionnaires. No anthropometric measures were taken in this sample. A flow chart describing the selection procedures is presented as Fig. 1.
From the 18 companies that agreed to collaborate in our study, we obtained data on the gender and age distribution of the drivers they employed and found no meaningful differences between respondents and nonrespondents. The proportion of male participants was 100 % against a rate of 99.8 % men in the nonrespondents; the mean age of the participants was 43.1 years and the mean age of nonrespondents was 44.6 years.
Respondents were reassured that the study was strictly anonymous and, therefore, no jobs were at risk by participating. The investigation was approved by both the Ethics Committee of the University of Porto and the transportation companies.
Methods used for data collection
Participants completed a questionnaire evaluating sociodemographic characteristics, work, and sleep habits and accidents' history, including near misses, over the preceding 5 years. In addition, it included questions concerning personal habits like smoking; consumption of alcohol, coffee or caffeinated beverages; and use of hypnotic-sedative drugs and antihistamines. Drivers' past medical history was also assessed, with a special attention given to sleep disorders.
The presence of hypersomnolence was measured by the ESS [18], a validated eight-item self-rating scale. A total score ≥11 was considered indicative of EDS.
The Berlin Questionnaire (BQ) [19, 20], which has been recently validated into the Portuguese language [21], was also included in this investigation. It is a subjective screening tool for OSAS consisting of 10 questions divided into three categories including snoring, sleepiness and fatigue, hypertension, and obesity (defined as a BMI ≥ 30 kg/m2). Drivers who fell into at least two of these categories were classified as being at high risk for having OSAS. To determine the BMI, we used the reported weight (kilograms) and height (meter).
A near-miss driving accident was defined as an unexpected event that had not caused any physical or material damage and, therefore, had limited immediate impact. An accident was defined as a collision of the vehicle to other stationary or moving obstacle, or solely driving off the road.
Statistical analysis
Quantitative variables were described using mean and standard deviations, and qualitative variables were expressed as percentages, unless otherwise stated. The chi-square test was used to assess the relationship between each independent variable and somnolence (self-reported sleepiness while driving [≥3 days/week], EDS [ESS score 11–24], and self-reported falling asleep at the wheel) as well as to assess the relationship between these factors and near-miss accidents and accidents in the past 5 years (bivariate analysis). Subsequently, a multivariate logistic regression analysis was performed including all explanatory variables with p < 0.10 on the bivariate analysis. Statistical significance was accepted for p values ≤0.05 and 95 % confidence intervals (CI) were calculated for results. Odds ratios (ORs) were adjusted for different potential confounders, such as age, BMI, medications causing drowsiness, alcohol intake, sleep schedule, years of licence, and kilometers driven per day (for details, see Tables 4 and 5). Data were analyzed with the use of a statistical analysis software package (StataCorp. 2009, Stata Statistical Software: Release 11, College Station, TX, USA).
Results
Participants' characteristics
The median (percentile 25–75) number of participants at each transportation company was 28 (16–58). Table 1 summarizes the characteristics of the respondents. All responders were male, with a mean age of 43.1 ± 10.0 years, and a mean BMI of 28.5 ± 3.8 kg/m2. Two hundred and forty-seven (34.6 %) drivers were obese. The mean number of hours driven per day was 8.7 (face-to-face interview vs. self-administered questionnaire: 8.6 % vs. 9.0 %, P = 0.02). Three hundred and sixty-three (50.8 %) drivers worked in long-haul trucking (face-to-face interview vs. self-administered questionnaire: 41.0 % vs. 56.0 %, P = 0.01) and 335 (47.0 %) were shift workers (face-to-face interview vs. self-administered questionnaire: 52.9 % s. 43.8 %, P = 0.05). Drivers whose measures were taken (n = 244) had a mean neck circumference of 42.2 ± 3.0 cm and 159 of these (65.0 %) had a Mallampati score of III–IV.
Prevalence of excessive daytime sleepiness and sleep disorder symptoms
Data on reported sleep disorders, symptoms, and drivers' behavior is provided in Table 2. Of the 714 responding drivers, 143 (20.0 %) reported an ESS score ≥11. Two hundred and sixty-one (36.5 %) reported they were habitual snorers, defined as snoring three or more nights per week. Eighty-three (11.6 %) admitted to suffer from witnessed breathing pauses. According to the BQ, 193 (28.8 %) were at high risk for having OSAS.
Sleepiness at the wheel
Six hundred and twelve (85.7 %) drivers reported driving while feeling sleepy and 92 (15.0 %) of these drivers experienced this somnolence three or more times a week. One hundred and ten (15.4 %) drivers admitted to actually having fallen asleep at the wheel in the past 5 years.
Overall, 111 (42.5 %) drivers had a near-miss accident and 43 (16.3 %), a driving accident that they considered to be sleep related. Most drivers considered the period right after lunch as the time of the day associated with a higher somnolence at the wheel. Table 3 presents data about sleepiness at the wheel, near misses, and accidents.
Personal and work factors associated with excessive sleepiness
The information in Table 4 depicts the correlation between personal and work variables and sleepiness, self-reported and measured by the ESS, and falling asleep at the wheel. Most of the associations remained significant after adjustment for potential confounders.
Regarding personal factors, smokers were more likely to report EDS than those who did not smoke. The OR for EDS measured by the ESS in drivers who smoked >20 cigarettes per day was 5.04 (95 % CI 2.45–10.3). Habitual snorers had a 2.47-fold increased risk of falling asleep at the wheel (95 % CI 1.53–4.00). Drivers with a high Mallampati score (III–IV) had a 3.46-fold increased risk of EDS (95 % CI 1.63–7.34). For each centimeter added to the neck circumference, there was a 1.38-fold increased risk of feeling more frequently sleepy while driving (95 % CI 1.15–1.65). Consumption of anxiolytics and antihistamines was associated with a higher risk of falling asleep at the wheel (ORs 2.46, 95 % CI 1.01–6.03 and 2.58, 95 % CI 1.07–6.80, respectively). Drivers with ESS score ≥11 were more likely to report sleepy episodes at the wheel.
Night shifts were associated with higher risk of sleepy driving (OR 2.34, 95 % CI 1.04–5.26). Drivers who averaged less than 8 h of sleep per night were more likely to report excessive somnolence. Moreover, those who averaged less than 6 h of sleep per night had a 3.69-fold increased risk of falling asleep at the wheel (95 % CI 1.89–7.22).
Personal and work factors associated with near-miss accidents and accidents
The association between personal and work factors and near misses and accident rates is shown in Table 5. A BMI ≥35 kg/m2 was associated with a 2.67-fold higher odds (95 % CI, 1.20–5.92) of having had a near miss and with a 2.99-fold increase in the odds (95 % CI, 1.35–6.64) of having had an accident. Consumption of antidepressant drugs was related to an increased accident risk (OR 3.30, 95 % CI 1.15–9.44).
The following variables were also found as predictive factors for near misses and accidents: being a habitual snorer, frequent symptoms of fatigue and headache, history of witnessed apneas, and common medical conditions, such as hypertension and esophageal reflux symptoms. Drivers with a high Mallampati score (III–IV) were more likely to report near-miss accidents.
Drivers at high risk for having OSAS, defined by the BQ, had 2.05-fold higher odds of having had a near-miss accident (95 % CI 1.37–3.05). Drivers with ESS score ≥11 had 3.84-fold higher odds of having had a near-miss accident (95 % CI 2.55–5.76) and 2.25-fold higher odds of having had an accident (95 % CI 1.51–3.35). Supplementary hours working were also associated to accident risk.
Discussion
This study shows a high prevalence of EDS, obesity, and sleep disorder symptoms among commercial truck drivers. Twenty percent of truck drivers had EDS measured by the ESS, compared with the 8.8 % found in a representative sample of Portuguese drivers [22]. In the current report, 30 % of the drivers experienced 6 h of sleep or less per night, which was associated with higher odds of having EDS and falling asleep at the wheel. Sleep loss accumulation leads to chronic somnolence and affects alertness and performance [7, 23–25]. This is particularly important for truck drivers, who spend more time on the road than the average driver. Habitual snoring, a cardinal symptom of OSAS, was reported by 36.5 % of our drivers, with a prevalence varying from 7 to 38 % in other studies [5, 23, 26]. We found a higher prevalence of drivers at high risk for having OSAS, according to the BQ, than reported in a smaller study of 209 commercial truck drivers in Brazil [26] and in a larger study with 931 Persian drivers [27].
The most important predictors of EDS found in our study were the presence of fatigue when waking up, the feeling of not being up to par during daytime, and witnessed apneas. Our study also reports a high and concerning frequency of falling asleep at the wheel and a high proportion of previous near misses and accidents among truck drivers. Fifteen percent of the participants in our study reported having fallen asleep at the wheel, which was a lower prevalence than was found in the Brazilian study [26] (15.4 % vs. 34.5 %), but comparable to others [5, 23]. The prevalence of near misses and accidents was similar to other studies [3] or higher [5, 27], but a greater prevalence of sleep-related accidents and near misses was found. Implication of these results in terms of public health and road safety suggests that policies should be enforced in this respect.
Depression and the use of antidepressants were the most significant risk factors for accidents. This increased prevalence of accidents in drivers using antidepressants and supports the previous evidence on the topic [28]. However, we did not find any relation to accidents in drivers medicated with anxiolytics or antihistamines, in contrast to other studies [3]. Near-miss accident risk was found to be associated with smoking. Prevalence of accidents was higher in drivers who had a regularly alcohol intake (≥4 days/week).
Although previous studies have demonstrated conflicting results regarding the relationship between accident risk and a high score in the ESS [27, 29–31], we found a significant association. Drivers with a high risk of SDB according to the BQ had also a higher rate of car accidents than drivers with low risk BQ. Furthermore, our study indicates that subjective questionnaires used to measure sleepiness can be used to identify drivers with EDS who are at increased accident risk.
Drivers who suffered from obesity, hypertension, or experienced esophageal reflux symptoms were found to have an increased accident risk. Therefore, it is recommended that these drivers be carefully followed by their physician and screened for SDB, which can be achieved by easy and costless measures such as the use of sleep questionnaires. Those drivers suspicious of suffering from sleep apnea should be referred to a sleep specialist.
The present study has limitations that need to be addressed. As every other questionnaire-based study some information may not be absolutely reliable, in particular if we consider that some drivers may be expected to have underreported their symptoms. Therefore, the estimated frequency of sleepy episodes at the wheel and the prevalence of sleep disorders' symptoms in this group might conceivably be lower than reality.
The overall rate of response to the questionnaire was lower than desirable. However, no meaningful differences were observed between the respondents and drivers employed by these companies, and the differences between drivers evaluated by face-to-face interview and those fulfilling a self-administered questionnaire regarding their professional activities are likely to reflect differences between the companies that allowed the personal interviews. Although the internal validity of our findings is not expected to have been compromised by the relatively low participation rate and the associations observed with sleepiness and accidents may apply also in other settings, the findings on sleep disorder symptoms and frequency of the main outcomes may not be easy to generalize. This, however, does not compromise the importance of our results in this specific setting and its usefulness for public health action.
Like some other European countries, Portugal still lacks a strict policy towards regulating commercial truck drivers concerning sleep disorders. Identifying drivers at risk for SDB has not only benefits for the driver itself as it is should be a major priority of medical assessment centers, as a public safety policy. Making rapid referral of suspected OSAS cases, diagnosing them, and initiating an adequate treatment is of essential scale [32, 33]. In the future, this data could provide the key to present discrepancies in the criteria to grant access to a driving license among the different European Union members, promoting the creation of a global system of commercial driver screening. From our data, we strongly suggest that this screening should be urgently implemented as an occupational requirement for professional drivers, not only for new drivers but also for those renewing their license.
References
Road safety PIN report: 2010 road safety target outcome: 100,000 fewer deaths since 2001.http://www.etsc.eu/documents/pin/report.pdf. Date last updated: June 1 2011. Date last accessed: January 4 2012.
Talmage JB, Hudson TB, Hegmann KT, Thiese MS (2008) Consensus criteria for screening commercial drivers for obstructive sleep apnea: evidence of efficacy. J Occup Environ Med 53:324–329
Howard ME, Desai AV, Grunstein RR, Hukins C, Armstrong JG, Joffe D, Swann P, Campbell DA, Pierce RJ (2004) Sleepiness, sleep-disordered breathing, and accident risk factors in commercial vehicle drivers. Am J Respir Crit Care Med 170:1014–1021
Akerstedt T (2000) Consensus statement: fatigue and accidents in transport operations. J Sleep Res 9:395
Vennelle M, Engleman HM, Douglas NJ (2010) Sleepiness and sleep-related accidents in commercial bus drivers. Sleep Breath 14:39–42
Åkerstedt T (2003) Shift work and disturbed sleep/wakefulness. Occup Med 53(2):89–94
Morrow PC, Crum MR (2004) Antecedents of fatigue, close calls, and crashes among commercial motor-vehicle drivers. J Saf Res 35(1):59–69
Harneet K, Walia AL, Hayes KA, Przepyszny PK, Sanjay RP (2012) Clinical presentation of shift workers to a sleep clinic. Sleep Breath 16(2):543–547
Young T, Peppard PE, Gottlieb DJ (2002) Epidemiology of obstructive sleep apnea: a population health perspective. Am J Respir Crit Care Med 165(9):1217
Pack, AI, Dinges, D, Maislin, G (2002) A study of prevalence of sleep apnea among commercial truck drivers. Federal Motor Carrier Safety Administration, Publication No. DOT-RT-02-030, Washington, DC.
Tregear S, Reston J, Schoelles K, Phillips B (2009) Obstructive sleep apnea and risk of motor vehicle crash: systematic review and meta-analysis. J Clin Sleep Med 5(6):573–581
Stoohs RA, Guilleminault C, Itoi A, Dement WC (1994) Traffic accidents in commercial long-haul truck drivers: the influence of sleep-disordered breathing and obesity. Sleep 17(7):619–623
Mulgrew A, Nasvadi G, Butt A, Cheema R, Fox N, Fleetham J, Ryan C, Cooper P, Ayas N (2008) Risk and severity of motor vehicle crashes in patients with obstructive sleep apnoea/hypopnoea. Thorax 63(6):536–541
Kingshott RN, Cowan JO, Jones DR, Flannery EM, Smith AD, Herbison GP, Taylor DR (2004) The role of sleep-disordered breathing, daytime sleepiness, and impaired performance in motor vehicle crashes—a case control study. Sleep Breath 8:61–72
Parks PD, Durand G, Tsismenakis AJ, Vela-Bueno A, Kales SN (2009) Screening for obstructive sleep apnea during commercial driver medical examinations. J Occup Environ Med 51(3):275
Hartenbaum N, Collop N, Rosen I, Phillips B, George C, Rowley J, Freedman N, Weaver T, Gurubhagavatula I, Strohl K (2006) Sleep apnea and commercial motor vehicle operators: statement from the joint task force of the American College of Chest Physicians, the American College of Occupational and Environmental Medicine, and the National Sleep Foundation. Chest 130:902–905
Simpson L, Hillman DR, Cooper MN, Ward KL, Hunter M, Cullen S, James A, Palmer LJ, Mukherjee S, Eastwood P (2012) High prevalence of undiagnosed obstructive sleep apnoea in the general population and methods for screening for representative controls. Sleep Breath; PMID: 23161476 (in press).
Johns MW (1991) A new method for measuring daytime sleepiness: the Epworth sleepiness scale. Sleep 14(6):540–545
Netzer NC, Stoohs RA, Netzer CM, Clark K, Strohl KP (1999) Using the Berlin Questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 131(7):485–491
Kang K, Park KS, Kim JE, Kim SW, Kim YT, Kim JS, Lee HW (2012) Usefulness of the Berlin Questionnaire to identify patients at high risk for obstructive sleep apnea: a population-based door-to-door study. Sleep Breath; PMID: 23054593 (in press).
Vaz A, Drummond M, Mota PC, Severo M, Almeida J, Winck JC (2011) Tradução do Questionário de Berlim para língua Portuguesa e sua aplicação na identificação da SAOS numa consulta de patologia respiratória do sono. Rev Port Pneumol 17(2):59–65
Gonçalves M, AR. P, Ferreira J: Conduzir com sono pode matar. www.apsono.com/documentos/4f26d30c7a720APC_brochura_sono_net2pdf 2011, Portuguese Sleep Association. Date last updated: March 1 2011. Date last accessed: February 2 2012.
Hui D, Chan J, Ko F, Choy D, Li T, Chan A, Wong K, Lai C (2002) Prevalence of snoring and sleep-disordered breathing in a group of commercial bus drivers in Hong Kong. Intern Med J 32(4):149–157
Krieger J (2007) Sleep apnoea and driving: how can this be dealt with? Eur Respir Rev 16(106):189–195
Hoekema A, Stegenga B, Bakker M, Brouwer WH, de Bont LG, Wijkstra PJ, van der Hoeven JH (2007) Simulated driving in obstructive sleep apnoeahypopnoea; effects of oral appliances and continuous positive airway pressure. Sleep Breath 11:129–138
Lemos LC, Marqueze EC, Sachi F, Lorenzi-Filho G, Moreno CRC (2009) Obstructive sleep apnea syndrome in truck drivers. J Bras Pneumol 35(6):500–506
Amra B, Dorali R, Mortazavi S, Golshan M, Farajzadegan Z, Fietze I, Penzel T (2011) Sleep apnea symptoms and accident risk factors in Persian commercial vehicle drivers. Sleep Breath 16(1):187–191
Christensen LQ, Nielsen LM, Nielsen SL (1990) Traffic accidents and drivers suspected for drug influence. Forensic Sci Int 45(3):273–280
Masa JF, Rubio M, Findley LJ (2000) Habitually sleepy drivers have a high frequency of automobile crashes associated with respiratory disorders during sleep. Am J Respir Crit Care Med 162(4):1407
Young T, Palta M, Dempsey J, Skatrud J, Weber S, Badr S (1993) The occurrence of sleep-disordered breathing among middle-aged adults. N Engl J Med 328(17):1230–1235
Teran-Santos J, Jimenez-Gomez A, Cordero-Guevara J (1999) The association between sleep apnea and the risk of traffic accidents. N Engl J Med 340(11):847–851
Hoekema A, Stegenga B, Bakker M, Brouwer WH, de Bont LG, Wijkstra PJ, van der Hoeven JH (2007) Simulated driving in obstructive sleep apnoea–hypopnoea: effects of oral appliances and continuous positive airway pressure. Sleep Breath 11(3):129–138
Stoohs RA, Barger K, Dement WC (1997) Sleep disordered breathing in primary care medicine. Sleep Breath 2(1):11–22
Acknowledgments
The authors would like to thank all drivers and managers of the transport companies, who generously provided us with the necessary information.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Catarino, R., Spratley, J., Catarino, I. et al. Sleepiness and sleep-disordered breathing in truck drivers. Sleep Breath 18, 59–68 (2014). https://doi.org/10.1007/s11325-013-0848-x
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-013-0848-x