Abstract
The A2A adenosine receptor (A2AR) is widely distributed on different cellular types in the brain, where it exerts a broad spectrum of pathophysiological functions, and for which a role in different neurodegenerative diseases has been hypothesized or demonstrated. To investigate the role of neuronal A2ARs in neurodegeneration, we evaluated in vitro and in vivo the effect of the neurotoxin 3-nitropropionic acid (3-NP) in a transgenic rat strain overexpressing A2ARs under the control of the neural-specific enolase promoter (NSEA2A rats). We recorded extracellular field potentials (FP) in corticostriatal slice and found that the synaptotoxic effect of 3-NP was significantly reduced in NSEA2A rats compared with wild-type animals (WT). In addition, after exposing corticostriatal slices to 3-NP 10 mM for 2 h, we found that striatal cell viability was significantly higher in NSEA2A rats compared to control rats. These in vitro results were confirmed by in vivo experiments: daily treatment of female rats with 3-NP 10 mg/kg for 8 days induced a selective bilateral lesion in the striatum, which was significantly reduced in NSEA2A compared to WT rats. These results demonstrate that the overexpression of the A2AR selectively at the neuronal level reduced 3-NP-induced neurodegeneration, and suggest an important function of the neuronal A2AR in the modulation of neurodegeneration.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The adenosine A2A receptor (A2AR) is a G protein-coupled receptor widely distributed throughout the body, with high levels of expression in the striatum, spleen, thymus, leukocytes, and blood platelets, and lower levels in the heart, lung, and blood vessels [1, 2]. A2AR exerts a broad spectrum of pathophysiological functions: it induces immunosuppression; modulates inflammation, vasodilation, and coronary blood flow; and controls angiogenesis and cancer pathogenesis [1, 2]. In the brain, A2AR is also quite ubiquitous although its expression levels vary considerably between different regions, being higher in the dorsal and ventral striatum and lower, but still observable, in other brain areas, such as the hippocampus and cerebral cortex [3]. In the brain, A2ARs are involved in the control of motor activity, learning and memory, and excitotoxicity [4, 5], making these receptors an attractive target for the treatment of neurodegenerative diseases, especially those involving basal ganglia. Accordingly, A2AR antagonists are in clinical trials as agents for the treatment of Parkinson’s disease (PD) and recently, the A2AR antagonist istradefylline has been approved in Japan for use in PD patients to minimize the motor symptoms, on the basis of studies demonstrating an antagonistic interaction between A2A and dopamine D2 receptors in the basal ganglia [6,7,8]. However, a considerable body of data indicates that A2ARs play a significant role also in neurodegeneration [9,10,11], prompting many research groups to investigate the possible exploitation of these receptors as drug targets for the treatment of other neurodegenerative diseases, such as Huntington’s disease (HD). HD is a genetic disorder characterized by choreic movements, psychiatric symptoms, dementia, and early death, for which there is no cure and whose progress cannot be reversed or slowed down [12]. The role of A2ARs in the pathogenesis of HD has long been investigated, starting from the observation that the neurons that early degenerate in HD are those where A2ARs are more abundantly expressed, i.e., the medium-sized spiny neurons forming the striatopallidal GABA pathway [8,9,10,11]. Changes in A2AR expression and signaling have been reported in various experimental models of HD and at different stages of the disease. In general, a downregulation of A2ARs has been reported in the basal ganglia of patients and in animal models, but their ability to increase cAMP signaling does not change in the striatum of a genetic model of HD, the R6/2 mice [4]. Instead, in peripheral blood cells of both patients and pre-symptomatic HD subjects, the A2AR density and function have been reported to be aberrantly increased [13].
Several studies tried to assess the pathogenetic role of A2ARs by evaluating the therapeutic potential of both A2AR agonist and antagonist in models of HD and by taking advantages of transgenic animal models. The results, however, are so far controversial. Even though in most cases the treatment with A2AR antagonists has been proved to ameliorate some neurochemical and behavioral alteration induced by in vivo treatment with quinolinic acid (QA) or 3-nitropropionic acid (3-NP) (two neurotoxins able to induce striatal neurodegeneration similar to those observed in HD) [9], in other cases, the A2AR antagonist or the deletion of the receptor in knockout mice resulted in a detrimental effect [14, 15]. Moreover, the evidence that the use of the A2AR agonist seems to be more effective than that of the antagonist in attenuating the symptoms in R6/2 mice (a widely used transgenic model of HD) [16, 17] and that the removal of A2ARs in the genetic HD model N171-82Q worsens the survival and motor function of mice [18] and adds complexity to the field. The A2AR agonist, in addition, prevented NMDA-induced toxicity in R6/2 mice [19], and the activation of the A2AR is critical for maintaining the proper function of BDNF, a neurotrophin involved in cell survival in HD [20, 21]. The picture is complicated also by the fact that A2ARs are functionally expressed not only on neurons but also on glial cells, endothelium, neutrophils, and platelets, and all could contribute to the modulation of neuronal damage.
The aim of the present study was to evaluate the role of neuronal A2ARs in the 3-NP rat model of HD and, to this end, we used a transgenic rat strain overexpressing A2ARs under the control of the neural-specific enolase promoter (NSEA2A rats) [22, 23]. We studied in corticostriatal slices the effect of 3-NP on synaptic transmission and cell survival, and we found a reduction of the toxic effect of 3-NP in NSEA2A compared to control rats. Then, we evaluated in vivo the striatal damage induced by repeated intraperitoneally (i.p.) injection of 3-NP and found that NSEA2A rats were less prone to striatal degeneration than WT rats. The results demonstrate that the neuronal overexpression of A2ARs confers neuroprotection in a model of striatal degeneration, highlighting the importance of neuronal A2ARs for the development of therapeutic strategies for HD.
Materials and methods
Animals
A colony of NSEA2A rats was established at the Istituto Superiore di Sanità. Transgenic rats were generated, as previously described [22], by microinjection of a DNA construct into the male pronucleus of Sprague Dawley rat zygotes with established methods [24]. The construct contained a full-length human A2A cDNA cloned into an expression vector 3′ of the 1.8 kb rat neuron-specific enolase promoter and 5′ of an intron/polyadenylation cassette of SV40 virus. The animals were kept under standardized temperature, humidity, and lighting conditions with free access to water and food. All procedures met the European guidelines for the care and use of laboratory animals (2010/63/UE) and those of the Italian Ministry of Health (Decreto Legislativo 116/92 and Decreto Legislativo 26/2014). Animals of both sexes were used between 3 and 4 months of age.
Genotyping of rats
Transgenic rats were identified by PCR (30 cycles, 54 °C annealing temperature) on their genomic DNA isolated from tail biopsies by the use of the following transgene-specific primers: SV40ipa5: 5_-GAAGGAACC TTACTTCTGTGG-3_ and SV40ipa3: 5-TCTTGTATAGCAGTGCAG C-3_.
Brain slice preparation
Corticostriatal slices were prepared as previously described [25]. Briefly, rats were decapitated under ether anesthesia, and coronal slices (300 μm) were cut with a vibratome and incubated for 1 h in artificial cerebrospinal fluid (ACSF) containing (in mM): 126 NaCl, 3.5 KCl, 1.2 NaH2PO4, 1.2 MgCl2, 2 CaCl2, 25 NaHCO3, and 11 glucose (pH 7.3) saturated with 95% O2 and 5% CO2. Single slices were transferred to a submerged recording chamber and superfused with ACSF at 32–33 °C. Drugs were applied by bath perfusion with ACSF.
Electrophysiology
Extracellular field potentials (FPs) were recorded in the dorsomedial striatum from corticostriatal slices with a glass microelectrode and evoked at the frequency of 0.05 Hz by stimulating the white matter between the cortex and the striatum with a bipolar platinum/iridium concentric electrode (FHC, Bowdoin, ME, USA). Signals were acquired with the DAM-80AC differential amplifier (WPI Instruments, Sarasota, FL, USA) and analyzed with WinLTP software [26].
Ten minutes of stable baseline recording preceded drug application. The effects of the drugs were expressed as percentage variation with respect to basal values, taking as 100% the average of the values obtained over the 5 min immediately before the application of the test compound. The data were expressed as mean ± S.E.M. from n of experiments (one slice tested in each experiment). Slices were obtained always from at least three animals for each set of experiments.
Evaluation of cell viability in corticostriatal slices
After preparation, corticostriatal slices (300 μm) were maintained in oxygenated ACSF for 1 h at room temperature to allow maximal recovery from slicing trauma. Then, slices were exposed to 3-NP 10 mM by placing them in a tube (one slice per tube) at 37 °C in oxygenated ACSF containing the toxin. For cell viability evaluation, after 2 h, slices were moved to a normal ACSF, and striatal area was isolated from the cortex (with the help of a razor blade) and incubated with 0.5 mg/ml of 3,(4,5-dimethylthiazol-2)2,5 difeniltetrazolium bromide (MTT) in gassed ACSF for 30 min at 37 °C [27]. The medium was then withdrawn and precipitated formazan was solubilized by adding DMSO. Striatal cell viability was spectrophotometrically measured at 570 nm. Results were expressed as the percentage of control (untreated slices), which was considered as 100%, and represent the mean ± S.E.M. value of at least nine experiments.
Rat 3-NP administration and analysis of clinical symptoms
3-NP (dissolved in buffered saline, pH 7.4, Sigma Aldrich, St. Louis, MO, USA) was i.p. administered to rats of both genders once a day for 8 days at 10 mg/kg/day. All animals were weighed every day and their general condition assessed by using a behavioral score system with a scale from 0 to 5 (0 = healthy without any symptoms; 1 = general slowness in walking, slight alteration of the hind limbs; 2 = abnormal gait and lack of coordination; 3 = fully developed paralysis of the hind limbs; 4 = fully developed paralysis of fore and hind limbs; 5 = lateral decubitus, animals predominantly lie on the side and/or are not able to straighten up within 30 s after turning them onto their back).
Brain processing
The day after the last injection, rats were anesthetized with i.p. injection of chloral hydrate and transcardially perfused with 100 ml of PBS followed by 4% paraformaldehyde at pH 7.4. Brain samples were then post-fixed overnight in 4% paraformaldehyde in PBS, cryoprotected in 30% sucrose in PBS at 4 °C and then stored at − 80 °C. Coronal brain sections (20 μm thick) from WT and NSEA2A rats were cut on a cryostat microtome, mounted onto a gelatin-coated slide, and stained for Nissl substance by using 1% cresyl violet.
Cresyl violet staining
Coronal sections were stained with cresyl violet for 45 s; differentiated in 70% ethanol; dehydrated by passing twice through 95% ethanol, 100% ethanol, and xylene solutions; and mounted onto microscope slides with Eukitt (Sigma).
Evaluation of striatal lesion
Stained sections were photographed at ×20 magnification using a Zeiss Axioskop 2 microscope and a Canon E06 digital camera. Determination of the lesion area was made on the serial digitized sections by manually delineating the border of the lesion on each section. In each brain, the extension of the lesion was calculated by measuring and averaging the areas of pallor in five serial sections (through the rostrocaudal extent, 100-μm interspace), taken at the level of the maximal extension of the lesion, by using Image J software (NIH, USA).
Statistical analysis
Statistical analysis of the data was performed with Student’s t test (in the case the D’Agostino-Pearson omnibus normality test demonstrated a Gaussian distribution of the values) or with the Mann–Whitney U test (when the normality test was negative). The GraphPad Prism software (GraphPad Software, San Diego, CA, USA) was used. A p value <0.05 was considered to indicate a significant difference.
Results
3-NP-induced depression of corticostriatal synaptic transmission is attenuated in NSEA2A rats
In corticostriatal slices, we evaluated the synaptic transmission by recording extracellular FP in the dorsomedial striatum after stimulation of the white matter between the cortex and the striatum, and we studied the effect of 3-NP, an irreversible inhibitor of succinate dehydrogenase that causes mitochondrial dysfunctions (and consequently energy impairment, oxidative stress, and excitotoxicity) and, in vivo, reproduces some of the hallmark of HD [28,29,30]. In corticostriatal slices from WT rats, 20 min of slice perfusion with 3-NP 5 mM induced depression of synaptic transmission as shown by the strong reduction of FP amplitude that, however, partially recovered upon washout (Fig. 1a). In slices from NSEA2A rats, 3-NP induced a milder effect, even though the differences are not statistically significant (Fig. 1b). When the concentration of 3-NP was increased up to 10 mM, we observed the complete failure of synaptic transmission in WT rats (Fig. 1c), with a minimal recovery after 3-NP washout (8.65 ± 2.3%, n = 8, Fig. 1d). Interestingly, in NSEA2A rats, we did not observe a complete failure of synaptic transmission but it was possible to record FPs, albeit of small amplitude, all along 3-NP application (Fig. 1c). In addition, 20 min after 3-NP removal, the percentage of recovery of FP was significantly higher than that in WT rats (26.72 ± 7.7% of basal value, n = 8, p < 0.05, Fig. 1d). Importantly, as already described by Chiodi et al. [23], basal synaptic transmission and paired-pulse facilitation were not different between WT and NSEA2A rats. In order to evaluate the role played by A2ARs, the effect of 3-NP was studied in the presence of the A2AR antagonist ZM 241385. In NSEA2A rats, the application of 1 μM ZM 241385 10 min before and then along with 3-NP tended to worsen the effect of 3-NP, abolishing the differences between WT and NSEA2A rats (Fig. 1e). In WT rats, ZM 241385 did not modify the effect of 3-NP (data not shown).
Electrophysiological experiments showing the effect of 3-NP on synaptic transmission in corticostriatal slices. a The concentration of 5 mM 3-NP, applied for 20 min, induced a reduction of synaptic transmission in both WT (n = 9) and NSEA2A (n = 8) rats, that partially recovered 20 min after the washout, with no difference between the two genotypes (b); c slice perfusion with 3-NP 10 mM induced a stronger effect in both WT (n = 8) and NSEA2A (n = 8) and the recovery 20 min after 3-NP washout was significantly higher in NSEA2A than in WT (d); the application of ZM 241385 to corticostriatal slices from NSEA2A rats (1 μM, 10 min before and along with 3-NP, n = 4) worsened 3-NP-induced synaptic depression and, as a result, the effect of 3-NP was comparable to that in WT slices (e). Each point represents the mean of three responses; insets in a show FPs before, during, and after 3-NP application in WT and NSEA2A rats. Horizontal bars indicate the period of drug application. *p ≤ 0.05 vs. WT, Student’s t test
These results demonstrate that the overexpression of A2ARs reduced the synaptotoxic effect of 3-NP.
3-NP-induced cell death is reduced in striatal slices from NSEA2A rats
Having found that the synaptotoxic effect of 3-NP is reduced in corticostriatal slices from NSEA2A rats, we investigated the hypothesis that the overexpression of A2ARs confers neuroprotection against 3-NP-induced cell death. To this end, we treated corticostriatal slices for 2 h with 3-NP 10 mM and evaluated striatal cell viability by using the MTT assay. As shown in Fig. 2, in WT rats, 3-NP treatment produced a significant reduction of cell viability (70.58 ± 3.01% of control values, n = 12, p < 0.05 vs controls). Instead in NSEA2A rats, the same treatment induced only a small, non- significant effect on cell survival (91.52 ± 1.93% of control values, n = 9).
Different effect of 3-NP on striatal cell viability in corticostriatal slices from WT and NSEA2A rats. Corticostriatal slices were incubated for 2 h with 3-NP (10 mM) and then cell viability of the striatal area was evaluated by MTT assay. Bar graphs show the mean ± S.E.M. of cell viability in WT (n = 12) and NSEA2A (n = 9) slices with respect to control values. *p ≤ 0.05 vs. CTR, Student’s t test
In vivo administration of 3-NP to WT and NSEA2A rats: behavioral analysis and histological evaluation of striatal damage
Since the overexpression of A2AR proved to be protective in two different in vitro/ex vivo models, we decided to move to in vivo experiments and to administer 3-NP to WT and NSEA2A rats. Ten WT rats (7 males and 3 females) and 12 NSEA2A rats (7 males and 5 females) were treated with 3-NP (10 mg/kg i.p.) daily for 8 days. Unexpectedly, all the males of both genotypes were found dead 24 h after the first injection, and 1 female overexpressing the A2AR died after the fifth injection. In the remaining female rats, 3-NP administration produced a progressive appearance of motor impairment, which was evaluated with the behavioral score system described in “Materials and methods” section. Even though a trend towards a reduction of the score was seen in NSEA2A rats with respect to WT rats (1.93 ± 0.177 and 2.71 ± 0.72, respectively), the difference was not statistically significant (data not shown). Animals were killed 24 h after the last injection of 3-NP and the brains processed as described [31]. Cresyl violet staining revealed that 3-NP injection resulted in selective bilateral lesions in both WT and NSEA2A female rats, as shown by the area of pallor within the striata (Fig. 3a). To evaluate the severity of the damage, since the extension of the lesion was not identical in the two striata of the same brain, and given the small number of animals, we measured the area of the lesion in each striatum of the brain and counted it as a single value. As shown in Fig. 3b, the extension of the lesion was significantly smaller in NSEA2A rats with respect to WT rats (2.779 ± 0.3 and 4.311 ± 0.4 mm2 respectively, p < 0.05 Mann–Whitney U test).
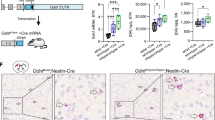
Histological evaluation of 3-NP lesions in WT and NSEA2A rats. a Serial brain sections obtained from WT and NSEA2A rats showing striatal lesions (uncolored areas) induced by i.p. injection of 3-NP. b Bar graphs represent the mean of the lesioned areas (mm2) in WT (n = 6) and NSEA2A (n = 5) rats calculated by Image J software. *p ≤ 0.05 vs. WT, Mann–Whitney U test
These results show that A2AR overexpression in female NSEA2A rats markedly attenuated the striatal lesion induced by systemic 3-NP injection.
Discussion
The main finding of the present study is that the overexpression of A2ARs reduces striatal damage induced by 3-NP, a selective inhibitor of complex II of the mitochondrial respiratory chain which replicates most of the clinical and pathophysiologic hallmarks of HD, such as abnormal movements, cognitive deficits, and progressive degeneration of striatal tissue [32]. Importantly, in this study, we used a validated transgenic model of rat overexpressing the A2ARs selectively in neurons [22, 23, 33,34,35].
The first observation of our study was that in corticostriatal slices, the synaptotoxic effect of 3-NP was significantly attenuated in NSEA2A compared to WT rats. In fact, after slice perfusion with a high concentration of 3-NP, which induced a strong depression of synaptic transmission, FP recovered up to more than 20% of basal values in NSEA2A, while in WT, the FP did not reach the 10% of pre-drug amplitude. To verify whether this difference was in fact due to the higher expression of A2ARs, we treated corticostriatal slices from NSEA2A rats with 3-NP in the presence of an A2AR antagonist, ZM241385, and found that the outcome was not different from that of WT treated with 3-NP alone, thus confirming the causative role of A2ARs in the reduction of synaptotoxicity of 3-NP in NSEA2A rats. The role of A2ARs in striatal neuroprotection was further established by evaluating cell viability in the striatum after exposing corticostriatal slices to 3-NP for 2 h. We found that 3-NP-induced cell death was significantly reduced in the striatum of NSEA2A rats compared to WT rats. These promising results prompted us to verify whether also in vivo NSEA2A rats were protected in the 3-NP models of HD. Peripheral administration of 3-NP is used to generate lesion models of HD [36]: this toxin causes cellular energy depletion by targeting the electron transport chain, and chronic treatment with 3-NP results in the spontaneous formation of bilateral lesions, which involve mainly the medium spiny neurons of the striatum with relative sparing of striatal interneurons [36]. Several different experimental protocols are used for 3-NP-induced striatal lesion, with differences in the dose, duration, and mode of administration [37]. We decided to use a low dose of 3-NP, 10 mg/kg, for 8 days in order to induce a mild effect and to be able to see, in case, even an exacerbation of the lesion in our transgenic animals. Unexpectedly, however, after the first injection of 3-NP, all the males died. It is difficult to explain such a strong effect of 3-NP since higher doses have been safely used in other studies involving male rats [38,39,40]. Furthermore, even though major strain differences in response to chronic systemic administration of 3-NP have been reported in rats, the Sprague Dawley strain used in this study exhibits an intermediate vulnerability to the toxic effect of 3-NP compared to Fisher or Lewis rats [37]. Several studies reported gender differences in the toxic effect of 3-NP and demonstrated a neuroprotective effect of estrogens, while testosterone exacerbated vulnerability to 3-NP [41, 42]. However, no one has described so far such a higher sensitivity of males to 3-NP and the mechanisms underlying this sex specificity remain to be elucidated. Importantly, the necropsy revealed no evident signs of organ toxicity. The difference in the vulnerability to 3-NP was evident only in in vivo experiments since in corticostriatal slices we did not observe gender differences in the response to 3-NP, neither in electrophysiology nor in cell viability evaluation. In the remaining female rats, by analyzing the extension of the lesion, we found a significant reduction of 3-NP-induced striatal degeneration in the rats overexpressing the A2ARs, in agreement with the results obtained in brain slices. The mechanism through which the overexpression of A2ARs produces a reduced sensitivity to the toxic effect of 3-NP may be found in the ability of this receptor to decrease the activation of NMDA receptors [43, 44]. In fact, it is reasonable that after 3-NP administration, membrane depolarization with NMDA receptor activation occurs due to its ability to impair mitochondrial functionality with energetic alterations and reduced ATP production. This is documented by in vivo and in vitro studies demonstrating that NMDA receptor antagonists prevent the effects induced by 3-NP administration [45, 46]. However, an effect of A2ARs on mitochondrial functionality, via direct or indirect actions, cannot be excluded. Indeed, in sympathetic neurons, the selective A2AR agonist CGS 21680 prevented alterations in mitochondrial membrane potential induced by nerve growth factor withdrawal [47]. More recently, in fibroblasts from Niemann-Pick type C patients (a rare disease characterized by cholesterol accumulation, hepatosplenomegaly, and neurodegeneration), the stimulation of A2AR with the agonist CGS 21680 normalized the changes in the mitochondrial membrane potentials typical of the disease [48]. Additionally, in human neuroblastoma (SH-SY5Y) and oligodendroglial precursor (MO3.13) cell lines transiently transfected with NPC1 small interfering RNA (to mimic the alterations of Niemann-Pick disease), the treatment with CGS 21680 rescued mitochondrial abnormalities [49]. Furthermore, the possibility that A2ARs can directly or indirectly influence mitochondrial functionality is also in line with the finding that caffeine, an adenosine receptor antagonist preferentially blocking the A2ARs, improved the impairment of mitochondrial complex activities and the decreased state 3 respiration (NAD+/FAD+-linked) in rats treated with the NMDA activator quinolinic acid in an in vivo model of HD [50]. Even though in this case it is the blockade of the receptor that ameliorates mitochondrial dysfunctions, anyway, the study further suggests that A2ARs may influence mitochondria activity, through a mechanism that still needs to identify.
In a limited set of experiments, we evaluated whether the overexpression of A2ARs provided similar protection also against other neurotoxin agents. To this end, in electrophysiological experiments in corticostriatal slices, we investigated the effect of the quinolinic acid (QA), an excitotoxin able to induce a marked striatal degeneration accompanied by HD-like neurochemical and functional alterations [51]. We found in WT rats that slice perfusion with QA, 1.2 mM, for 10 min induced a strong reduction of the FP amplitude that partially recovered after washout, an effect which was significantly reduced in NSEA2A rats (unpublished results). This finding suggests that the protection afforded by A2AR overexpression is not specific to 3-NP but may represent a more general strategy against striatal neurodegeneration.
The role of A2ARs in the modulation of neurodegeneration has been long investigated, with several studies demonstrating a beneficial effect of the antagonists in different models of neuronal damage, and many others suggesting positive results with the use of A2AR agonists (see [52] for a comprehensive and updated review). Our results are in line with studies demonstrating a beneficial effect of A2AR stimulation on symptoms and disease progression in rodent models of HD. In particular, one of the first studies describing a positive effect of the A2AR agonist CGS 21680 in HD came from the group of Chern, who demonstrated that CGS 21680 attenuated symptoms of Huntington’s disease in a transgenic mouse model [16]. The same authors demonstrated that chronic CGS 21680 treatment improved the urea cycle deficiency in the R6/2 mice [53]. Positive effects were obtained also with T1-11, an A2AR agonist isolated from a Chinese medicinal herb in rodent models of HD [54, 55],
Contrasting results have been described also with A2AR knockout animals, which in some cases proved to be protected towards a neurodegenerative stimulus, and in other cases, the removal of the receptor resulted in a detrimental effect [15, 18, 56]. As for HD, Fink and colleagues [56] found that the knockout or the pharmacological inactivation of A2ARs attenuates 3-NP-induced striatal damage, in contrast with our results showing that the overexpression of the receptor is neuroprotective towards the same toxin. In addition, while Mieves and collaborators showed that the deletion of A2AR worsened survival and motor behavior in a transgenic mouse model of Huntington’s disease [18], a more recent paper demonstrated that inactivation of adenosine A2AR reverses working memory deficits in the R6/2 transgenic model of HD [57]. However, several reasons can explain such results: in fact, many cell types that are involved in the evolution of brain damage (neurons, astrocytes, microglial cells as well as peripheral inflammatory cells) express the A2AR, and the stimulation of the receptor can produce different effects depending on which cell it is located [4, 9, 52]. Importantly, in the present study, we were able to dissect out the contribution of A2ARs selectively increased in neurons in the modulation of brain damage induced by 3-NP, since the A2AR overexpression occurs exclusively in neuronal cells.
In a previous paper, we evaluated spontaneous and K+-evoked glutamate efflux in striatal synaptosomes prepared from WT and NSEA2A rats, and we found that under condition of depolarization, such as with high K+, a higher degree of presynaptic A2AR stimulation occurs in NSEA2A [23], suggesting that endogenous adenosine more effectively activates transgenic receptors than lower levels of endogenous receptors. It is reasonable to think that also at the post synaptic level, endogenous adenosine will more effectively activate the A2ARs in NSEA2A than in WT rats. As discussed above, the stimulation of the postsynaptic A2ARs decreases NMDA-mediated currents, and this could explain the reduced 3-NP-induced toxicity in NSEA2A rats. On the contrary, it has been demonstrated in synaptosome preparations that the stimulation of presynaptic A2ARs, while it does not modify glutamate release per se, increases high K+-induced presynaptic glutamate release, with a potential detrimental effects in condition of excitotoxicity [23, 58, 59]. Since in the present study we found a reduced 3-NP-induced neurotoxicity in NSEA2A rats, it is reasonable to think that the post synaptic receptors play a prominent role in the toxicity induced by 3-NP, overcoming the harmful effect of the presynaptic receptors (also considering that 3-NP is unable, per se, to evoke glutamate release in the striatum [60, 61], and probably, for this reason, A2AR-mediated facilitation of glutamate release does not play a critical role).
Even though a neuronal-selective knock down of the endogenous receptor is necessary to definitively assess the role of the neuronal receptor in neurodegeneration, the present results point to an important role of neuronal A2AR in the modulation of neurodegeneration.
Overall, the current study gives evidence for a neuroprotective role of neuronal A2ARs in a rat model of HD, adding new clues to the comprehension of the complex role exerted by A2AR in the modulation of striatal degeneration.
References
Fredholm BB, IJzerman AP, Jacobson KA, Klotz KN, Linden J (2001) International Union of Pharmacology. XXV. Nomenclature and classification of adenosine receptors. Pharmacol Rev 53:527–552
Fredholm BB, IJzerman AP, Jacobson KA, Linden J, Müller CE (2011) International Union of Basic and Clinical Pharmacology. LXXXI. Nomenclature and classification of adenosine receptors—an update. Pharmacol Rev 63:1–34
Svenningsson P, Hall H, Sedvall G, Fredholm BB (1997) Distribution of adenosine receptors in the postmortem human brain: an extended autoradiographic study. Synapse 27:322–335
Chen JF, Sonsalla PK, Pedata F, Melani A, Domenici MR, Popoli P, Geiger J, Lopes LV, de Mendonca A (2007) Adenosine A2A receptors and brain injury: broad spectrum of neuroprotection, multifaceted actions and “fine tuning” modulation. Prog Neurobiol 83:310–331
Gomes CV, Kaster MP, Tome AR, Agostinho PM, Cunha RA (2011) Adenosine receptors and brain diseases: neuroprotection and neurodegeneration. Biochim Biophys Acta 1808:1380–1399
Kondo T, Mizuno Y, Japanese Istradefylline Study Group (2015) A long-term study of istradefylline safety and efficacy in patients with Parkinson disease. Clin Neuropharmacol 38:41–46
Vorovenci RJ, Antonini A (2015) The efficacy of oral adenosine A(2A) antagonist istradefylline for the treatment of moderate to severe Parkinson’s disease. Expert Rev Neurother 15:1383–1390
Fuxe K, Guidolin D, Agnati LF, Borroto-Escuela DO (2015) Dopamine heteroreceptor complexes as therapeutic targets in Parkinson’s disease. Expert Opin Ther Targets 19:377–398
Popoli P, Blum D, Martire A, Ledent C, Ceruti S, Abbracchio MP (2007) Functions, dysfunctions and possible therapeutic relevance of adenosine A2A receptors in Huntington’s disease. Prog Neurobiol 81:331–348
Popoli P, Blum D, Domenici MR, Burnouf S, Chern Y (2008) A critical evaluation of adenosine A2A receptors as potentially “druggable” targets in Huntington’s disease. Curr Pharm Des 14:1500–1511
Lee CF, Chern Y (2014) Adenosine receptors and Huntington’s disease. Int Rev Neurobiol 119:195–232
Ross CA, Aylward EH, Wild EJ, Langbehn DR, Long JD, Warner JH, Scahill RI, Leavitt BR, Stout JC, Paulsen JS, Reilmann R, Unschuld PG, Wexler A, Margolis RL, Tabrizi SJ (2014) Huntington disease: natural history, biomarkers and prospects for therapeutics. Nat Rev Neurol 10:204–216
Varani K, Abbracchio MP, Cannella M, Cislaghi G, Giallonardo P, Mariotti C, Cattabriga E, Cattabeni F, Borea PA, Squitieri F, Cattaneo E (2003) Aberrant A2A receptor function in peripheral blood cells in Huntington’s disease. FASEB J 17:2148–2150
Blum D, Galas MC, Pintor A, Brouillet E, Ledent C, Muller CE, Bantubungi K, Galluzzo M, Gall D, Cuvelier L, Rolland AS, Popoli P, Schiffmann SN (2003) A dual role of adenosine A2A receptors in 3-nitropropionic acid-induced striatal lesions: implications for the neuroprotective potential of A2A antagonists. J Neurosci 23:5361–5369
Huang QY, Wei C, Yu L, Coelho JE, Shen HY, Kalda A, Linden J, Chen JF (2006) Adenosine A2A receptors in bone marrow-derived cells but not in forebrain neurons are important contributors to 3-nitropropionic acid-induced striatal damage as revealed by cell-type-selective inactivation. J Neurosci 26:11371–11378
Chou SY, Lee YC, Chen HM, Chiang MC, Lai HL, Chang HH, Wu YC, Sun CN, Chien CL, Lin YS, Wang SC, Tung YY, Chang C, Chern Y (2005) CGS21680 attenuates symptoms of Huntington’s disease in a transgenic mouse model. J Neurochem 93:310–320
Domenici MR, Scattoni ML, Martire A, Lastoria G, Potenza RL, Borioni A, Venerosi A, Calamandrei G, Popoli P (2007) Behavioral and electrophysiological effects of the adenosine A2A receptor antagonist SCH 58261 in R6/2 Huntington’s disease mice. Neurobiol Dis 28:197–205
Mievis S, Blum D, Ledent C (2011) A2A receptor knockout worsens survival and motor behaviour in a transgenic mouse model of Huntington’s disease. Neurobiol Dis 41:570–576
Martire A, Calamandrei G, Felici F, Scattoni ML, Lastoria G, Domenici MR, Tebano MT, Popoli P (2007) Opposite effects of the A2A receptor agonist CGS21680 in the striatum of Huntington’s disease versus wild-type mice. Neurosci Lett 417:78–83
Tebano MT, Martire A, Chiodi V, Ferrante A, Popoli P (2010) Role of adenosine A(2A) receptors in modulating synaptic functions and brain levels of BDNF: a possible key mechanism in the pathophysiology of Huntington’s disease. ScientificWorldJournal 10:1768–1782
Zuccato C, Cattaneo E (2007) Role of brain-derived neurotrophic factor in Huntington’s disease. Prog Neurobiol 81:294–330
Gimenez-Llort L, Schiffmann SN, Shmidt T, Canela L, Camon L, Wassholm M, Canals M, Terasmaa A, Fernandez-Teruel A, Tobena A, Popova E, Ferre S, Agnati L, Ciruela F, Martinez E, Scheel-Kruger J, Lluis C, Franco R, Fuxe K, Bader M (2007) Working memory deficits in transgenic rats overexpressing human adenosine A2A receptors in the brain. Neurobiol Learn Mem 87:42–56
Chiodi V, Ferrante A, Ferraro L, Potenza RL, Armida M, Beggiato S, Pezzola A, Bader M, Fuxe K, Popoli P, Domenici MR (2016) Striatal adenosine-cannabinoid receptor interactions in rats over-expressing adenosine A2A receptors. J Neurochem 136:907–917
Popova E, Krivokharchenko A, Ganten D, Bader M (2002) Comparison between PMSG- and FSH-induced superovulation for the generation of transgenic rats. Mol Reprod Dev 63:177–182
Chiodi V, Mallozzi C, Ferrante A, Chen JF, Lombroso PJ, Di Stasi AM, Popoli P, Domenici MR (2014) Cocaine-induced changes of synaptic transmission in the striatum are modulated by adenosine A2A receptors and involve the tyrosine phosphatase STEP. Neuropsychopharmacology 39:569–578
Anderson WW, Collingridge GL (2007) Capabilities of the WinLTP data acquisition program extending beyond basic LTP experimental functions. J Neurosci Methods 162:346–356
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65:55–63
Brouillet E, Guyot MC, Mittoux V, Altairac S, Condé F, Palfi S, Hantraye P (1998) Partial inhibition of brain succinate dehydrogenase by 3-nitropropionic acid is sufficient to initiate striatal degeneration in rat. J Neurochem 70:794–805
Brouillet E, Conde F, Beal MF, Hantraye P (1999) Replicating Huntington’s disease phenotype in experimental animals. Prog Neurobiol 59:427–468
Damiano M, Galvan L, Deglon N, Brouillet E (2010) Mitochondria in Huntington’s disease. Biochim Biophys Acta 1802:52–61
Apolloni S, Amadio S, Parisi C, Matteucci A, Potenza RL, Armida M, Popoli P, D'Ambrosi N, Volonte C (2014) Spinal cord pathology is ameliorated by P2X7 antagonism in a SOD1-mutant mouse model of amyotrophic lateral sclerosis. Dis Model Mech 7:1101–1109
Borlongan CV, Koutouzis TK, Sanberg PR (1997) 3-Nitropropionic acid animal model and Huntington’s disease. Neurosci Biobehav Rev 21:289–293
Coelho JE, Alves P, Canas PM, Valadas JS, Shmidt T, Batalha VL, Ferreira DG, Ribeiro JA, Bader M, Cunha RA, do Couto FS, Lopes LV (2014) Overexpression of adenosine A2A receptors in rats: effects on depression, locomotion, and anxiety. Front Psychiatry 5:67. https://doi.org/10.3389/fpsyt.2014.00067
Jastrzębska J, Nowak E, Smaga I, Bystrowska B, Frankowska M, Bader M, Filip M, Fuxe K (2014) Adenosine (A)(2A)receptor modulation of nicotine-induced locomotor sensitization. A pharmacological and transgenic approach. Neuropharmacology 81:318–326
Batalha VL, Ferreira DG, Coelho JE, Valadas JS, Gomes R, Temido-Ferreira M, Shmidt T, Baqi Y, Buée L, Müller CE, Hamdane M, Outeiro TF, Bader M, Meijsing SH, Sadri-Vakili G, Blum D, Lopes LV (2016) The caffeine-binding adenosine A2A receptor induces age-like HPA-axis dysfunction by targeting glucocorticoid receptor function. Sci Rep 6:31493. https://doi.org/10.1038/srep31493
Brouillet E, Jenkins BG, Hyman BT, Ferrante RJ, Kowall NW, Srivastava R, Roy DS, Rosen BR, Beal MF (1993) Age-dependent vulnerability of the striatum to the mitochondrial toxin 3-nitropropionic acid. J Neurochem 60:356–359
Ouary S, Bizat N, Altairac S, Menetrat H, Mittoux V, Conde F, Hantraye P, Brouillet E (2000) Major strain differences in response to chronic systemic administration of the mitochondrial toxin 3-nitropropionic acid in rats: implications for neuroprotection studies. Neuroscience 97:521–530
Mu S, OuYang L, Liu B, Zhu Y, Li K, Zhan M, Liu Z, Jia Y, Lei W, Reiner A (2011) Preferential interneuron survival in the transition zone of 3-NP-induced striatal injury in rats. J Neurosci Res 89:744–754
Colle D, Santos DB, Moreira EL, Hartwig JM, dos Santos AA, Zimmermann LT, Hort MA, Farina M (2013) Probucol increases striatal glutathione peroxidase activity and protects against 3-nitropropionic acid-induced pro-oxidative damage in rats. PLoS One 8:e67658. https://doi.org/10.1371/journal.pone.0067658
Tasset I, Perez-Herrera A, Medina FJ, Arias-Carrion O, Drucker-Colin R, Tunez I (2013) Extremely low-frequency electromagnetic fields activate the antioxidant pathway Nrf2 in a Huntington’s disease-like rat model. Brain Stimul 6:84–86
Mogami M, Hida H, Hayashi Y, Kohri K, Kodama Y, Gyun Jung C, Nishino H (2002) Estrogen blocks 3-nitropropionic acid-induced Ca2+i increase and cell damage in cultured rat cerebral endothelial cells. Brain Res 956:116–125
Nishino H, Nakajima K, Kumazaki M, Fukuda A, Muramatsu K, Deshpande SB, Inubushi T, Morikawa S, Borlongan CV, Sanberg PR (1998) Estrogen protects against while testosterone exacerbates vulnerability of the lateral striatal artery to chemical hypoxia by 3-nitropropionic acid. Neurosci Res 30:303–312
Tebano MT, Pintor A, Frank C, Domenici MR, Martire A, Pepponi R, Potenza RL, Grieco R, Popoli P (2004) Adenosine A2A receptor blockade differentially influences excitotoxic mechanisms at pre- and postsynaptic sites in the rat striatum. J Neurosci Res 77:100–107
Wirkner K, Gerevich Z, Krause T, Gunther A, Koles L, Schneider D, Norenberg W, Illes P (2004) Adenosine A2A receptor-induced inhibition of NMDA and GABAA receptor-mediated synaptic currents in a subpopulation of rat striatal neurons. Neuropharmacology 46:994–1007
Kim GW, Copin JC, Kawase M, Chen SF, Sato S, Gobbel GT, Chan PH (2000) Excitotoxicity is required for induction of oxidative stress and apoptosis in mouse striatum by the mitochondrial toxin, 3-nitropropionic acid. J Cereb Blood Flow Metab 20:119–129
Centonze D, Prosperetti C, Barone I, Rossi S, Picconi B, Tscherter A, De Chiara V, Bernardi G, Calabresi P (2006) NR2B-containing NMDA receptors promote the neurotoxic effects of 3-nitropropionic acid but not of rotenone in the striatum. Exp Neurol 202:470–479
Ramirez SH, Fan S, Maguire CA, Perry S, Hardiek K, Ramkumar V, Gelbard HA, Dewhurst S, Maggirwar SB (2004) Activation of adenosine A2A receptor protects sympathetic neurons against nerve growth factor withdrawal. J Neurosci Res 77:258–269
Visentin S, De Nuccio C, Bernardo A, Pepponi R, Ferrante A, Minghetti L, Popoli P (2013) The stimulation of adenosine A2A receptors ameliorates the pathological phenotype of fibroblasts from Niemann-Pick type C patients. J Neurosci 33:15388–15393
Ferrante A, De Nuccio C, Pepponi R, Visentin S, Martire A, Bernardo A, Minghetti L, Popoli P (2016) Stimulation of adenosine A2A receptors reduces intracellular cholesterol accumulation and rescues mitochondrial abnormalities in human neural cell models of Niemann-Pick C1. Neuropharmacology 103:155–162
Mishra J, Kumar A (2014) Improvement of mitochondrial NAD(+)/FAD(+)-linked state-3 respiration by caffeine attenuates quinolinic acid induced motor impairment in rats: implications in Huntington’s disease. Pharmacol Rep 66:1148–1155
Beal MF, Kowall NW, Ellison DW, Mazurek MF, Swartz KJ, Martin JB (1986) Replication of the neurochemical characteristics of Huntington’s disease by quinolinic acid. Nature 321:168–171
Cunha RA (2016) How does adenosine control neuronal dysfunction and neurodegeneration? J Neurochem 139:1019–1055
Chiang MC, Chen HM, Lai HL, Chen HW, Chou SY, Chen CM, Tsai FJ, Chern Y (2009) The A2A adenosine receptor rescues the urea cycle deficiency of Huntington’s disease by enhancing the activity of the ubiquitin-proteasome system. Hum Mol Genet 18:2929–2942
Huang NK, Lin JH, Lin JT, Lin CI, Liu EM, Lin CJ, Chen WP, Shen YC, Chen HM, Chen JB, Lai HL, Yang CW, Chiang MC, Wu YS, Chang C, Chen JF, Fang JM, Lin YL, Chern Y (2011) A new drug design targeting the adenosinergic system for Huntington’s disease. PLoS One 6(6):e20934
Chou AH, Chen YL, Chiu CC, Yuan SJ, Weng YH, Yeh TH, Lin YL, Fang JM, Wang HL (2015) T1-11 and JMF1907 ameliorate polyglutamine-expanded ataxin-3-induced neurodegeneration, transcriptional dysregulation and ataxic symptom in the SCA3 transgenic mouse. Neuropharmacology 99:308–317
Fink JS, Kalda A, Ryu H, Stack EC, Schwarzschild MA, Chen JF, Ferrante RJ (2004) Genetic and pharmacological inactivation of the adenosine A2A receptor attenuates 3-nitropropionic acid-induced striatal damage. J Neurochem 88:538–544
Li W, Silva HB, Real J, Wang YM, Rial D, Li P, Payen MP, Zhou Y, Muller CE, Tomé AR, Cunha RA, Chen JF (2015) Inactivation of adenosine A2A receptors reverses working memory deficits at early stages of Huntington’s disease models. Neurobiol Dis 79:70–80
Marchi M, Raiteri L, Risso F, Vallarino A, Bonfanti A, Monopoli A, Ongini E, Raiteri M (2002) Effects of adenosine A1 and A2A receptor activation on the evoked release of glutamate from rat cerebrocortical synaptosomes. Br J Pharmacol 136:434–440
Vaz SH, Lérias SR, Parreira S, Diógenes MJ, Sebastião AM (2015) Adenosine A2A receptor activation is determinant for BDNF actions upon GABA and glutamate release from rat hippocampal synaptosomes. Purinergic Signal 11:607–612
Beal MF, Brouillet E, Jenkins BG, Ferrante RJ, Kowall NW, Miller JM, Storey E, Srivastava R, Rosen BR, Hyman BT (1993) Neurochemical and histologic characterization of striatal excitotoxic lesions produced by the mitochondrial toxin 3-nitropropionic acid. J Neurosci 13:4181–4192
Sánchez-Carbente MR, Massieu L (1999) Transient inhibition of glutamate uptake in vivo induces neurodegeneration when energy metabolism is impaired. J Neurochem 72:129–138
Acknowledgments
We thank Adriano Urcioli and Alessio Gugliotta for the assistance with animal work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflicts of interest.
Ethical approval
All applicable international, national, and/or institutional guidelines for the care and use of animals were followed.
Rights and permissions
About this article
Cite this article
Domenici, M.R., Chiodi, V., Averna, M. et al. Neuronal adenosine A2A receptor overexpression is neuroprotective towards 3-nitropropionic acid-induced striatal toxicity: a rat model of Huntington’s disease. Purinergic Signalling 14, 235–243 (2018). https://doi.org/10.1007/s11302-018-9609-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11302-018-9609-4