Abstract
Purpose
To propose a simple noninvasive method for ureteral stent retrieval using an extraction string sutured to the skin in children.
Methods
A retrospective chart review was performed to gather relevant data from December 2005 to February 2013. After the surgeries, if indicated, a tethered double-J stent was placed in the ureter. A 5-0 non-absorbable Prolene stitch was used as an extraction string passing through the urethra and was sutured to subcoronal skin in boys or inner surface of labia majora in girls. For stent removal, a small amount of 2 % lidocaine jelly was pushed into the urethra 5 min before the procedure. The string was then pulled by continuous and gentle force until the entire stent was out. The suture was then cut to release the stent. No sedation or anesthesia was needed.
Results
A total of 378 double-J stents with extraction strings were inserted for a total of 325 patients (61.2 % male). Of the 53 patients with bilateral ureteral stents, one male patient (1.88 %) experienced early stent protrusion from urethral meatus. Two of 272 patients (0.73 %) with unilateral ureteral stent (one male and one female) encountered the same problem. All other stents were extracted successfully using the extraction string without any complications. No upward stent migration or suture site reaction was encountered.
Conclusion
This method is a safe, easy-to-use, feasible and noninvasive alternative for cystoscopic stent removal with high success rate and minimal complications. This can lead to considerable saving in time and costs for patients, families and healthcare system.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Ureteral stents are an integral part of urologic practice used to prevent ureteral obstruction and maintain the urine flow. In 1978, Finney introduced the double-J stent in an attempt to reduce the stent migration, and since that time, double-J stents are widely used for different indications in children and adults [1].
Ureteral stents have been changed over the past two decades in order to minimize patients’ discomfort, stent encrustation and urinary tract infection (UTI) [2]. Several studies have reviewed and highlighted the advances in stent technology and use of new biomaterials in order to decrease stent-related complications, but minimally invasive method of choice for stent retrieval is less commonly addressed [3]. Routine endoscopic stent retrieval requires general anesthesia or sedation that imposes more cost to the patients and healthcare system. Specifically in pediatric patients, it will also impose the risk of a second anesthesia and urethral injury.
Several techniques have been proposed to obviate the use of cystoscopy in double-J stent retrieval such as using magnets [4–6], crochet hook [7], urethral sound [8] and snail-headed retriever [9]. Although some of these methods may be less costly and may need less experience or facilities, they all retain two major drawbacks: additional urethral instrumentation and low success rate. Moreover, some of these are only applicable to female patients and some need anesthesia or sedation.
Due to the aforementioned reasons, noninvasive stent removal lacks the expected popularity in the urologic armamentarium. This calls for a simple and effective noninvasive method for stent removal with high rates of success. We have previously introduced external extension of double-J stents during pyeloplasty as an inexpensive and noninvasive technique for stent removal [10]. We hereby revisit the concept of using extraction string in children [11] and propose our simple modification in which the distal end of the double-J stent is tethered with an extraction string and sutured to the skin. This method can be used in both genders and in both the pediatric and adult populations.
Patients and methods
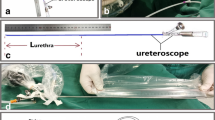
After obtaining ethical approval from institutional review board, a retrospective chart review was performed to gather relevant patients’ data from December 2005 to February 2013. The stent placement and removal technique was the same in all patients. Detailed description of the procedure was given to parents, and informed consent was obtained from them. We used a 5-0 non-absorbable Prolene stitch as extraction string and tied it through one of the distal holes in the bladder coil of the stent; the needle was then removed (Fig. 1). Ureteral stent placement was performed by pushing it up into the renal pelvis using a pusher over the guide wire and developing the distal curl in the bladder. Extraction string remained out of the urethra. A non-absorbable 4-0 stitch was then sutured to the lateral subcoronal skin in boys or inner surface of labia majora in girls. After preparing the appropriate length of extraction string, these two stitches were knotted together without any tension on extraction string (Fig. 2); then, a Foley catheter was inserted into the bladder if indicated.
Double-J stents were left inside for 1–4 weeks postoperatively depending on the type of the surgery. Few days after surgery, the Foley catheter was removed while ureteral stent stayed in place. The surgeon should be careful while removing the Foley catheter in the presence of an extraction string in the urethra; for the prevention of inadvertent removal of the stent, especially in boys, we instilled a small amount of 2 % lidocaine jelly into the urethra using a syringe and then twisted the Foley catheter clockwise and counterclockwise gently before removing the catheter. This maneuver released the probable adhesion between the catheter and the string.
For ureteral stent removal, a small amount of 2 % lidocaine jelly was pushed into the urethra 5 min before removal. The string was then pulled by continuous and gentle force until the entire stent was out. The suture was then cut to release the stent and was appropriately discarded.
Results
During the study period, 378 double-J stents with extraction strings were inserted for a total of 325 patients of those 199 were male (61.2 %). The mean age (SD) of patients was 3.97 (4.26) years. The characteristics of patients are summarized in Table 1. Indications for ureteral stenting were endoureterotomy, ureteroscopy, ureterocele puncture (when endoscopic ureterocele double-puncture technique was used with double-J placement [12]) and endoscopic antireflux surgery (in cases of unilateral bulking agent injection for single functioning kidney, to prevent possible obstruction and subsequent kidney damage) (Table 2). Upward migration of stent was not encountered among patients. No urine leakage was observed in toilet-trained patients. Of the 53 patients with bilateral ureteral stents, one male patient (1.88 %) experienced early stent protrusion from urethral meatus. Two of 272 patients (0.73 %) with unilateral ureteral stent (one male and one female) encountered the same problem. None of them required stent replacement. All other ureteral stents were removed successfully using extraction strings. No cystoscopic intervention was required for stent removal.
We did not observe any complications attributable to the extraction string sutured to the skin. No suture site infection or scarring was noted in our patients. Urine cultures were taken prior to stent removal. In four patients (1.23 %) who had positive urine cultures, stent removal was postponed for 1 week and antibiotics were given based on the susceptibility results. Double-J stents were removed on the average of 22.3 (5.1) days following surgery.
Discussion
Cystoscopy is most commonly used to extract ureteral stents using endoscopic grasping forceps. In children, this procedure requires a second general anesthesia and additional urethral instrumentation with the risk of related complications. Several experts endeavored to find new minimally invasive methods to obviate the need of cystoscopy for stent removal; use of magnets was one of these attempts. In this method, a magnet is affixed to the distal tip of the ureteral stent and another magnet is used to retrieve the stent using a urethral catheter or specially designed instrument [4, 13, 14]; this method reached 100 % success rate in women but only 76 % success rate in men [14]. Most recently, Wang et al. [6] designed a basket-shaped magnetic stent with hooks on the end of retrieval catheter to increase the success rate. However, this recent technique should be investigated for biocompatibility of the stent, stent-related complications and ureteral dislodgement due to unfolded basket [6]. Crochet hook [7] and snail-headed [9] catheters are also reported for ureteral stent removal with variable success rates but are all confined to female patients. All the aforementioned methods also share the same drawback: the need for additional urethral catheterization. Biodegradable ureteral stents have also been introduced to minimize patients’ discomfort and eliminate the risk of neglected stents, but these stents have not yet got widespread acceptance due to limitations in controlling the degrading time and also stent particles which may lead to ureteral obstruction [15–17].
In 1986, Siegel et al. [11] developed a non-endoscopic method for stent retrieval in children in which a monofilament nylon tether was tied to the distal end of a double-J ureteral stent and could be taped to the penis or abdomen. This string was used for stent removal, and the method was assessed in small studies afterward with acceptable results [18, 19]. Although tethered ureteral stents were manufactured subsequently, this method did not gain widespread popularity mainly due to the concerns about inadvertent displacement of the stent and possible complications. However, a recent randomized controlled trial in adults concluded that tethered ureteral stents might have several advantages without increasing the risk of complications and morbidities [20]. Barnes et al. [20] emphasized that no difference existed in stent-related symptoms between patients with and without extraction string and showed that no specific complications are attributable to the string in the urethra per se. Furthermore, they did not observe any differences in the incidence of postoperative complications including UTI, stent migration and emergency room visit [20]. For tethered stents, a dislodgment rate of 13–15 % is reported in adults and is believed to be higher in females [20, 21]. For example, Althaus et al. [21] recently reported that dislodgment occurred in 13 of 98 cases that had tethered stents fixed with adhesive tapes. However, at least five of these patients intentionally removed the stents and another two accidentally pulled their stent out; most of the dislodgments (9/13) also occurred at the day zero after surgery [21]. It should be noted that these findings might not be applicable to children specifically those at younger ages since adults may more likely remove their stents intentionally and prematurely. In children, dislodgment of the stent by inadvertently pulling the string is the main concern. Our modified technique can be safely used in children by applying a suture to the skin; the risk of inadvertently pulling the string by the child or caregiver is minimized in both males and females with this method, and this may be the main reason that we did not observe a high rate of dislodgment in our experience.
In our study, we did not observe any string breakage during stent removal and stent retrieval was totally successful in all patients. Using a non-absorbable monofilament suture is mandatory to avoid both string breakage and bacterial colonization. Neglected ureteral stent is a major concern in urologic practice and may lead to bothersome symptoms like hematuria, stone formation, recurrent UTI, septicemia and even death [22, 23]. In our technique, external extension and fixation of the string prevent forgetting the stent due to its visibility [20]. Extraction string attached to the skin also prevents proximal stent migration that is reported in 0.6–4.2 % of patients without extraction string [24, 25]. Although involuntary urine leakage or incontinency attributed to the extraction string may be a concern, we did not observe this complication in toilet-trained children. In younger children, urine leakage could not be investigated; however, this would not be troublesome since the child is in diaper. Urine leakage may be the result of stent displacement beyond the urethral sphincter [18]. By applying the skin suture, the risk of inadvertently pulling the string is greatly reduced and this may explain lack of this complication in our patients.
Removing ureteral stent using extraction string is an outpatient procedure and reduces the costs to both patients’ families and healthcare system. This method is also timesaving by eliminating the need for secondary cystoscopy, general anesthesia and hospitalization specifically in busy healthcare settings that scheduling a cystoscopy is time-consuming [26]. Surgeons should educate patient’s family about handling the extraction string and how they can avoid pulling the string during diaper changing. Stent extraction can be easily done at home by well-informed parents; however, we performed the procedure for all patients during a follow-up visit at our clinic by a physician.
We are aware that our study has some limitations. Firstly, we did not compare our results with a control group that underwent cystoscopic stent removal and we ought to rely on previous studies in this regard that mostly address the adult population. We also were not able to objectively assess patients’ symptoms because of the retrospective design of our study; however, previous randomized controlled studies suggest that no additional discomfort is associated with tethered stents [20]. Accordingly, further studies and randomized trials are required prior to suggesting our method as a routine technique in pediatric urology practice. Future studies may also investigate this method in adult patients.
In conclusion, ureteral stent removal using an extraction string sutured to the skin is a noninvasive and easy-to-use technique without inflicting any major complications to the patient. It also results in significant cost savings for patients and healthcare system. This technique of non-cystoscopic ureteral stent retrieval has the potential to be used routinely in patients requiring ureteral stents considering its great benefits.
References
Finney RP (1978) Experience with new double J ureteral catheter stent. J Urol 120(6):678–681
Al-Aown A, Kyriazis I, Kallidonis P, Kraniotis P, Rigopoulos C, Karnabatidis D, Petsas T, Liatsikos E (2010) Ureteral stents: new ideas, new designs. Ther Adv Urol 2(2):85–92. doi:10.1177/1756287210370699
Denstedt JD, Reid G, Sofer M (2000) Advances in ureteral stent technology. World J Urol 18(4):237–242. doi:10.1007/s003450000180237.345
Mykulak DJ, Herskowitz M, Glassberg KI (1994) Use of magnetic internal ureteral stents in pediatric urology: retrieval without routine requirement for cystoscopy and general anesthesia. J Urol 152(3):976–977
Taylor WN, McDougall IT (2002) Minimally invasive ureteral stent retrieval. J Urol 168(5):2020–2023. doi:10.1097/01.ju.0000033964.15384.e2
Wang J, Feng J, Hu W, Song Y, Xu X, Fan M, Huang C (2014) Preclinical evaluation of a newly designed ureteral stent and magnetic retrieval catheter for minimally invasive stent removal. Urology 84(4):960–966. doi:10.1016/j.urology.2014.06.024
Kawahara T, Ito H, Terao H, Yamagishi T, Ogawa T, Uemura H, Kubota Y, Matsuzaki J (2012) Ureteral stent retrieval using the crochet hook technique in females. PLoS One 7(1):e29292. doi:10.1371/journal.pone.0029292
Corrales J, Meza M, Quiche J, Zorrilla J (2008) A technique for the removal of ureteral catheters in infants and children using a urethral sound. J Urol 180(1):295–296. doi:10.1016/j.juro.2008.03.079
Yu DS, Yang TH, Ma CP (1995) Snail-headed catheter retriever: a simple way to remove catheters from female patients. J Urol 154(1):167–168
Kajbafzadeh AM, Zeinoddini A, Ebadi M, Heidari R, Tajalli A (2014) External extension of double-J ureteral stent during pyeloplasty: inexpensive stent and non-cystoscopic removal. Int Urol Nephrol 46(4):671–676. doi:10.1007/s11255-013-0594-9
Siegel A, Altadonna V, Ellis D, Hulbert W, Elder J, Duckett J (1986) Simplified method of indwelling ureteral stent removal. Urology 28(5):429
Kajbafzadeh A, Salmasi AH, Payabvash S, Arshadi H, Akbari HR, Moosavi S (2007) Evolution of endoscopic management of ectopic ureterocele: a new approach. J Urol 177(3):1118–1123. doi:10.1016/j.juro.2006.11.001
Altarac S, Vrazic M (2012) A new type of ureteral stent will facilitate stent removal. Eur Urol 61(1):225–226. doi:10.1016/j.eururo.2011.08.075
Macaluso JN Jr, Deutsch JS, Goodman JR, Appell RA, Prats LJ Jr, Wahl P (1989) The use of the Magnetip double-J ureteral stent in urological practice. J Urol 142(3):701–703
Chew BH, Paterson RF, Clinkscales KW, Levine BS, Shalaby SW, Lange D (2013) In vivo evaluation of the third generation biodegradable stent: a novel approach to avoiding the forgotten stent syndrome. J Urol 189(2):719–725. doi:10.1016/j.juro.2012.08.202
Kotsar A, Nieminen R, Isotalo T, Mikkonen J, Uurto I, Kellomaki M, Talja M, Moilanen E, Tammela TL (2012) Preclinical evaluation of new indomethacin-eluting biodegradable urethral stent. J Endourol 26(4):387–392. doi:10.1089/end.2011.0327
Olweny EO, Landman J, Andreoni C, Collyer W, Kerbl K, Onciu M, Valimaa T, Clayman RV (2002) Evaluation of the use of a biodegradable ureteral stent after retrograde endopyelotomy in a porcine model. J Urol 167(5):2198–2202
Birch BR, Das G, Wickham JE (1988) Tethered ureteric stents—a clinical assessment. Br J Urol 62(5):409–411
Bregg K, Riehle RA Jr (1989) Morbidity associated with indwelling internal ureteral stents after shock wave lithotripsy. J Urol 141(3):510–512
Barnes KT, Bing MT, Tracy CR (2014) Do ureteric stent extraction strings affect stent-related quality of life or complications after ureteroscopy for urolithiasis: a prospective randomised control trial. BJU Int 113(4):605–609. doi:10.1111/bju.12541
Althaus A, Li K, Pattison E, Eisner B, Pais V, Steinberg P (2014) Rate of dislodgement of ureteral stents when utilizing an extraction string after endoscopic urologic surgery. J Urol. doi:10.1016/j.juro.2014.12.087
Sancaktutar AA, Adanur S, Resorlu B, Tepeler A, Ziypak T, Soylemez H, Atar M, Bozkurt Y, Penbegul N, Tufek A, Yavuz S (2013) The forgotten ureteral stent in children: from diagnosis to treatment. J Urol 189(3):1054–1060. doi:10.1016/j.juro.2012.09.089
Singh V, Srinivastava A, Kapoor R, Kumar A (2005) Can the complicated forgotten indwelling ureteric stents be lethal? Int Urol Nephrol 37(3):541–546. doi:10.1007/s11255-004-4704-6
Breau RH, Norman RW (2001) Optimal prevention and management of proximal ureteral stent migration and remigration. J Urol 166(3):890–893
Slaton JW, Kropp KA (1996) Proximal ureteral stent migration: an avoidable complication? J Urol 155(1):58–61
Fernando A, Bultitude M (2014) Tether your stents! BJU Int 113(4):517–518. doi:10.1111/bju.12635
Conflict of interest
No conflict of interest exists in relation to the material of the manuscript to none of the authors, and there was no source of extra-institutional commercial funding.
Ethical standard
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional review board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kajbafzadeh, AM., Nabavizadeh, B., Keihani, S. et al. Revisiting the tethered ureteral stents in children: a novel modification. Int Urol Nephrol 47, 881–885 (2015). https://doi.org/10.1007/s11255-015-0963-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-0963-7