Abstract
Objective
The objectives of surgical repair of epispadias include the achievement of urinary continence, cosmetically acceptable genitalia with correction of curvature and normal genital function. To achieve all the aforementioned objectives, patients usually undergo two- or multiple-stage surgeries. Traditionally, the patients undergo epispadias repair in the first stage through modified Cantwell–Ransley or Mitchell–Bagli procedure. Subsequently, in the second stage, bladder neck repair is performed to achieve continence, the most common procedure being modified Young-Dees–Leadbetter. There is no reported single-stage technique of epispadias repair achieving both cosmesis and continence in isolated incontinent epispadias. The objectives of the study were to assess continence and cosmesis with partial penile disassemble and double breasting of bladder neck and posterior urethra in isolated peno-pubic epispadias.
Materials and methods
A retrospective analysis of surgical outcome of seven cases of primary isolated incontinent peno-pubic epispadias repair from July 2008 to July 2012 was carried out. Patients’ age varied from 10 months to 16 years. Penile de-gloving is done with mobilization of urethral plate from ventrum to dorsum, distally till mid-glans and proximally up to pubic symphysis with preservation of blood supply at both ends. Partial mobilization of corporal bodies from its attachment and division of peno-pubic ligament are done to lengthen the penis. A mucosal strip of 5–7 mm is excised to denude the mucosa for double breasting. Tubularization of urethral plate with double breasting from the region of bladder neck to posterior urethra is done to increase the outlet resistance and then tubularization of distal urethral plate. Approximation of mobilized pelvic floor muscles is done to complete sphincteroplasty. Spongioplasty along the entire length and corporoplasty with medial rotation of corporeal bodies is done. Glanuloplasty with meatoplasty is done to bring the meatus ventrally and then skin cover to penis is done with rotation of ventral flaps or z plasty.
Results
Preoperatively, three patients (42.8 %) had moderate and four (58.2 %) had severe chordee. Three (42.8 %) of the seven patients had mild torque toward right. Six patients became fully continent and had excellent cosmesis postoperatively, while one was partially continent with a dry interval of 2 h and required anticholinergics. None of the patients developed fistula, stricture, wound dehiscence or necrosis in a follow-up period of 1–5 years; however, one patient had mild residual chordee but did not require any additional surgery.
Conclusion
Double breasting of bladder neck and posterior urethra with sphincteroplasty and partial penile disassembly produces a reliable tubularized neourethra with complete chordee correction with emphasis on achievement of continence and near-normal-appearing penile morphology through a single-stage surgery. Mobilization of urethral plate and proximal urethra up to bladder neck helps correction of chordee as well as torsion. Partial penile disassembly keeping the urethra attached to glans maintains the dual blood supply, thus preventing stricture and fistula. This small series is a preliminary study, and more studies at different centers may authenticate it by reproducing the results.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Epispadias is a rare congenital anomaly, with a reported incidence of 1 in 117,000 males, and isolated incontinent variant is even rarer. Characteristics of epispadias are a dorsal urethral defect which is replaced by a broad mucosal strip lining the dorsum of the penis extending toward the bladder with or without the potential incompetence of the sphincter mechanism. Epispadias can be divided into glanular, penile and peno-pubic and may occur in isolation or as a part of exstrophy epispadias complex. Peno-pubic epispadias comprises the most common variety (70 %) and is mostly associated with incontinence. In peno-pubic epispadias, the whole urethral plate is wide open with the patulous bladder neck, the external sphincter is incompetent with varying degrees of the pubic diastasis, penis is short with severe dorsal curvature and bladder capacity is small, and the combination of these factors leads to incontinence [1, 2]. The objectives of surgical repair of this entity include the achievement of urinary continence, cosmetically acceptable genitalia with correction of curvature and normal genital function. To achieve all the aforementioned objectives, patients usually undergo two- or multiple-stage surgeries. Traditionally, the patients undergo epispadias repair in the first stage through Cantwell–Ransley [3] or Mitchell–Bagli [4] procedure. Subsequently, in the second stage, bladder neck repair is performed to achieve continence, most common procedure being modified Young-Dees–Leadbetter. There is no technique reported in the literature which gives continence, cosmesis and sexually functional penis in one stage. Aim of the study was to evaluate the functional and cosmetic outcome of double breasting of bladder neck and posterior urethra with partial penile disassembly in one stage in isolated incontinent peno-pubic epispadias.
Materials and methods
A retrospective analysis of surgical outcome of seven cases of peno-pubic epispadias repair from July 2008 to July 2012 at a tertiary care institution was performed. All patients included in the study were having isolated incontinent peno-pubic epispadias, and patients with exstrophy epispadias complex or secondary repair after exstrophy repair were excluded from the study. Patient’s age varied from 10 months to 16 years with a mean age of 10.7 years. Patients were classified on the basis of presence/degree of chordee and torque. Less than 30° of chordee was considered mild, 30°–60° as moderate, while more than 60° was taken as severe chordee. Torque was evaluated for direction toward left or right and classified as less than 45° as mild, 45°–90° as moderate, and more than 90° as severe.
Surgical technique: Incision is given around the coronal sulcus, epispadiac meatus and urethral plate after injection of 1:100,000 adrenaline with lignocaine. Penile de-gloving (Fig. 1b) is done up to the root of penis. Urethral plate is mobilized from ventral to dorsal aspect, proximally up to pubic symphysis (Fig. 1c, d) with division of peno-pubic ligament and distally up to mid-glans, and mobilization is circumferential up to bulbar urethra and only antero-laterally in the region of posterior urethra, thus preserving the prostate. Penis is dissected into three separate compartments, two corpora cavernosa and urethral plate with corpus spongiosum leaving only the distal most attachment at mid-glans taking care to preserve the blood supply at both ends along with laterally situated nerve supply (Fig. 1e, f). Segment of posterior urethra is opened dorsally up to bladder neck (Fig. 1g–i). A mucosal strip of 5–7 mm is excised from posterior urethra up to bladder neck (Figs. 2a–d, 4). Tubularization of urethral plate is done starting proximally from the bladder neck to posterior urethra approximating the denuded urethral mucosa. Double breasting of posterior urethra and bladder neck (vicryl 6-0) is done to increase the outlet resistance and create a continent zone (Figs. 2e–h, 4). Then, rest of urethral plate is tubularized up to the neomeatus after placing a suitable size feeding tube (vicryl 6-0) (Fig. 3a). Spongioplasty is done as an additional covering layer (Fig. 3b). Corporoplasty along with medial rotation of corporeal bodies [5] is done along the entire length (vicryl 6-0) keeping the urethra ventrally as per its normal anatomical location along with transposition of nerve supply dorsally (Fig. 3c). Glanuloplasty along with meatoplasty (Fig. 3) is done to create a conical glans and a wide meatus ventrally (Fig. 3c, d). External sphincter fibers are mobilized bilaterally and approximated in midline to create a neo-sphincter (Fig. 3d). Urethra is brought ventrally with dorsal corporoplasty and is fixed to corporal bodies (Fig. 3e, f). Skin cover is given to the dorsal aspect of penis with rotation of ventral flaps or by doing z plasty (Fig. 3g) at the base if required in selected cases. Preputioplasty is done when adequate prepuce is available to restore the penile configuration as close to normal. Gentle pressure dressing is applied and check dress is usually done on 5th postoperative day. Patients are given anti-inflammatory, anti-erotics and antibiotic drugs in the postoperative period. Per urethral catheter is kept for 10–14 days.
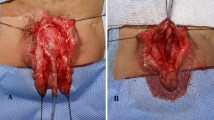
Penile de-gloving, mobilization of urethral plate and partial penile disassembly. a Peno-pubic epispadias with visible verumontanum. b Penile de-gloving. c Mobilization of corporal bodies and division of peno-pubic ligament to lengthen the penis. d Dorsal mobilization of urethra up to bladder neck and partial mobilization of corporal bodies from its attachment. e Ventral mobilization of urethral plate from corpora. f Partial penile disassembly. g–i Dorsal opening of urethra up to bladder neck
Evaluation of postoperative results in the study was done by means of correction of curvature (chordee/torque), patient satisfaction and achievement of continence. Criteria for continence were taken as fully continent when patients void well without any leakage and had a dry interval of 2–4 h. Patients having dry interval of 1–2 h or nocturnal incontinence were labeled as partially continent, while those having continuous dribbling or dry interval of less than 1 h were taken as incontinent. Continence status was analyzed at 3 months postoperatively and reanalyzed at 6 months after which patients were categorized as fully continent, partially continent and incontinent. Cosmesis of the penis was taken as excellent when penis became straight with conical glans having meatus at the tip (Fig. 3d) with projectile straight urinary stream. It was labeled satisfactory when persisting curvature or torque of less than 20° or a non-conical glans not requiring surgical intervention was the end result. Patient having residual curvature more than 30° or poor flow/dribbling of urinary stream was considered as having poor postoperative outcome. Patients were followed up at 1, 3, 6 and 12 months and then annually.
Results
Preoperatively, three patients (42.8 %) had moderate and four (58.2 %) had severe chordee. Three (42.8 %) of the seven patients had torque which was mild and toward right in all the cases. Six (85.7 %) of the seven patients had excellent cosmetic outcome with complete correction of chordee and torque and were pleased with the final appearance (Fig. 5). One patient who had severe chordee preoperatively had mild residual chordee postoperatively; however, he was relatively satisfied with the cosmetic result and did not require any surgical intervention.
All of the seven incontinent patients achieved continence after the surgery. Six patients were fully continent as per the defined criteria 6 months after the surgery. One patient was partially continent with a dry interval of 2 h and required addition of anticholinergics. None of the patients developed fistula, stricture, wound dehiscence or necrosis. Two of the seven patients in the study group were in adolescent age group and had successful ejaculations after the surgery. Semen analysis reported sluggish motility and oligospermia with adequate volume. Patients have been followed up postoperatively for a period ranging from 1 to 5 years.
Discussion
There are many studies in the literature regarding surgical procedures to provide continence for the bladder exstrophy population; however, reports on continence in children with isolated epispadias are not as common. To date, most series have included patients of epispadias with bladder exstrophy [3], making it difficult to draw independent conclusions for isolated primary peno-bubic epispadias. Moreover, of the two most common techniques currently used for epispadias repair, modified Cantwell–Ransley does not address all the goals of epispadias surgery and Mitchell–Bagli, although addresses, is not able to achieve all the goals by means of a single surgery.
Cosmetic correction is an important concern in epispadias repair to deal with, so that the patient has a straight penis of adequate length capable of producing successful intercourse and to prevent psychological complications. Incontinence is the primary concern which is not dealt with in modified Cantwell–Ransley procedure and usually corrected in the second stage through modified Young-Dees–Leadbetter bladder neck reconstruction [6–9]. Mitchell–Bagli procedure provides continence in 4–70 %, but results in a hypospadiac meatus which remains a cosmetic concern and may require surgical correction [10, 11]. Injection of bulking agents at bladder neck to increase the outlet resistance or formal bladder neck reconstruction may be required in incontinent patients. Both the techniques thus expose the patient to two or more surgeries increasing the morbidity, hospital stay and financial burden. Patients undergoing modified Young-Dees–Leadbetter bladder Neck reconstruction to resolve the issue of incontinence may suffer from complications like bladder outlet obstruction (8–10 %) further resulting in formation of bladder stones and epididymitis. Approximately 5–8 % patients have inadequate bladder neck resistance and continue to be incontinent requiring further surgery [12].
Our technique, similar to Mitchell–Bagli procedure, does complete proximal dissection which facilitates exposure, allowing easier tubularization of the bladder neck in a proximal extension of the urethroplasty and anatomical placement of bladder neck and posterior urethra in pelvis. In addition, caliber of the patulous bladder neck is reduced with elongation of the posterior urethra and reinforcing a second layer through double breasting in the region of bladder neck and posterior urethra. Mobilization of external urethral sphincter fibers and approximation in midline create a neo-sphincter which further helps in increasing the resistance in the sphincter zone, thus adding another factor for continence. Bladder capacity in these incontinent patients is usually small which increases with time due to increases in the outlet resistance. Prostatic growth at the time of puberty as thought earlier may not help in attainment of continence in these patients [13]. Thus, combination of double breasting of bladder neck and posterior urethra, normalization of the caliber of patulous bladder neck, elongation of the posterior urethra, sphincteroplasty and successive increase in the bladder capacity aids to achieve continence with continence rates increasing to 100 % as compared to 70 % in the Mitchell’s procedure. At the same time, by avoiding complete penile disassembly by keeping the distal most attachment intact, it reduces the risk of ischemic complications and eliminates the risk of creating a hypospadiac meatus. Others have described partial penile disassembly as keeping urethral plate attached to one of the corpora which does not allow the lengthening of urethra and limits complete correction of dorsal curvature [14, 15]. Complete mobilization of urethral plate right up to bladder neck helps to increase urethral length, and spongioplasty maintains the pliability of urethra which also serves to increase the continence rates. Mobilization of urethral plate from corpora up to bulb corrects the curvature as well as torque. In case of persistence of dorsal curvature after urethral plate mobilization which is likely due to dorsoventral disproportion of corporeal bodies, a superficial dorsal corporotomy with or without graft can be done, though we did not require it in any of our patients.
Similarly, torque in epispadias may be due to attachment of urethral plate to corpora or its attachment with corporal bodies or differential corporal growth. Mobilization of the urethral plate and partial mobilization from its attachment to crura may correct the torque, but if it still persists then plication of tunica or corporotomy with or without graft is usually required. Division of peno-pubic ligament and partial mobilization of crura from its bony attachments help lengthen the penis.
Urethro-cutaneous fistulas and urethral strictures represent the most common complications following the modified Cantwell–Ransley procedure; however, we did not come across this complication in our series. Pippi Salle et al. [16] and Surer et al. [17] evaluated their patients 3 months postoperatively and found that fistula and stricture rate was 19 and 10 %, respectively, using the Cantwell–Ransley technique. Ransley and Duffy [3] reported a fistula rate of 4 % and urethral stricture rate of 5.3 %, while others had peno-pubic fistula up to 44 % [18]. Possible explanations of not having the dorsal fistula in our series are meticulous mobilization of urethra with spongiosum preserving the blood supply at both ends, keeping distal urethra attached to glans, tubularization with spongioplasty and corporoplasty after adequate mobilization covering the dorsal aspect of urethra which is potential site for urethral fistula. Double breasting urethral plate closure also helps in reducing the risk of peno-pubic fistula. Strictures were prevented by adequate mobilization of wide urethral plate, avoiding any tension during tubularization and preserving dual blood supply to the urethra. In Mitchell series, hypospadiac meatus occurred in 30–70 % patients, but we did not come across any such situation in our series by keeping the distal most attachment of the urethra beyond the mid-glans intact.
Adequate narrowing of bladder neck and posterior urethra also helps in prevention of retrograde ejaculation. Two of the adolescent patients had successful ejaculations after the surgery. Semen analysis reported oligospermia with adequate volume and sluggish motility.
The present series provides preliminary evidence that single-stage epispadias reconstruction using partial penile disassembly with double breasting at bladder neck and posterior urethra can achieve urinary continence along with cosmetic parameters of curvature correction avoiding morbidity of multiple procedures. Although our study group was small during a follow-up ranging from 1 to 5 years, none of the patients developed any significant complications and all achieved sustained continence after surgery.
This is the first study to achieve all the objectives for isolated peno-pubic epispadias surgery through a single stage. The limitations of the study had been small number of cases, retrospective in nature and lack of objective documentation like urethral pressure profile and uroflowmetry.
Conclusion
Double breasting of bladder neck and posterior urethra with sphincteroplasty and partial penile disassembly produces a reliable neourethra, complete chordee correction with emphasis on achievement of continence and near-normal-appearing penile morphology through a single-stage surgery. Mobilization of urethral plate and proximal urethra up to bladder neck helps correction of chordee as well as torsion. Partial penile disassembly keeping the urethra attached to glans distally maintains the dual blood supply of urethra and helps in preventing stricture and fistula. Double breasting of bladder neck and urethra prevents retrograde ejaculation. This small series is a preliminary study and more studies at different centers may authenticate it by reproducing the results.
References
Lascaratos J, Poulakou-Rembelakou E, Rembelakos A, Marketos S (1995) The first case of epispadias: an unknown disease of the Byzantine Emperor Heraclius (610–641 AD). Br J Urol 76:380–383
Gearhart JP, Mathews RI (2007) Exstrophy-epispadias complex. In: Wein AJ (ed) Campbell-Walsh urology, 10th edn. Saunders Elsevier, Philadelphia, p 3325
Ransley PG, Duffy PG (1995) Bladder exstrophy closure and epispadias repair. In: Spitz L, Coran AG (eds) Rob & Smith operative surgery (pediatric surgery). Chapman & Hall, London, pp 745–759
Mitchell ME, Bagli DJ (1996) Complete penile disassembly for epispadias repair: the Mitchell technique. J Urol 155:303–304
Koff SA, Eakins M (1984) The treatment of penile chordee using corporeal rotation. J Urol 131:931
Dees JE (1949) Congenital epispadias with incontinence. J Urol 62:513
Kramer SA, Kelalis PP (1982) Assessment of urinary continence in epispadias: review of 94 patients. J Urol 128:290
Mollard P, Basset T, Mure PY (1998) Male epispadias: experience with 45 cases. J Urol 160:55
Mouriquand PD, Bubanj T, Feyaerts M, Jandric M, Timsit M, Mollard P et al (2003) Long-term results of bladder neck reconstruction for incontinence in children with classical bladder exstrophy or incontinent epispadias. Br J Urol Int 92:997
Hafez AT, Helmy T (2011) Complete penile disassembly for epispadias repair in postpubertal patients. Urology 78:1407–1410
Hammouda HM (2003) Results of complete penile disassembly for epispadias repair in 42 patients. J Urol 170:1963–1965
Surer Ilhami, Baker LA, Jeffs RD, Gearhart JP (2001) Modified Young-Dees–Leadbetter bladder neck reconstruction in patients with successful primary bladder closure elsewhere. J Urol 165:2438–2440
Gearhart JP, Yang A, Leonard MP, Jeffs RD, Zerhouni EA (1993) Prostate size and configuration in adults with bladder exstrophy. J Urol 149(2):308–310
Perovic SA, Vukadinovic V, Djordjevic ML, Djakovic NG (1999) Penile disassembly technique for epispadias repair: variants of technique. J Urol 162:1181–1184
Mokhless I, Youssif M, Ismail HR, Higazy H (2008) Partial penile disassembly for isolated epispadias repair. Urology 71:235–238
Pippi Salle JL, Jednak R, Capolicchio JP, França IMP, Labbie A, Gosalbez R (2002) A ventral rotational skin flap to improve cosmesis and avoid chordee recurrence in epispadias repair. Br J Urol Int 90:918–923
Surer I, Baker LA, Jeffs RD, Gearhart JP (2000) The modified Cantwell–Ransley repair for exstrophy and epispadias: 10 year experience. J Urol 164:1040–1043
Sarin YK, Manchanda V (2006) Mitchell’s technique for epispadias repair: our preliminary experience. J Indian Assoc Pediatr Surg 11:31–34
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Bhat, A., Upadhayay, R., Bhat, M. et al. Double breasting of bladder neck and posterior urethra for continence in isolated peno-pubic epispadias. Int Urol Nephrol 47, 789–795 (2015). https://doi.org/10.1007/s11255-015-0947-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-0947-7