Abstract
Objective
We observed serum parameters and urinary findings of IgA nephropathy (IgAN) patients in the short and longer time after tonsillectomy, to provide evidences to clarify the role of tonsils in the pathogenesis of IgAN and the feasibility of tonsillectomy for IgAN patients.
Methods
For the short-term study, 19 patients with both IgAN and chronic tonsillitis (group A) and 19 patients with chronic tonsillitis (group B) were performed bilateral tonsillectomy and 19 healthy people as normal controls (group C). Another 115 patients with IgAN and chronic tonsillitis including 61 patients for tonsillectomy combined with drug therapy and 54 for drug therapy alone followed up for 12 months.
Results
Fourteen patients of group A showed a deterioration of urinary findings, while only 2 patients of group B showed deterioration (P < 0.01). Both serum IgA and IgA1 levels were significantly higher in group A than that in group B or group C (P < 0.05, respectively). Levels of serum IgA and IgA1 of group A increased after tonsillectomy and did not increase instantly, but increased at day 3, then decreased at day 5. Both serum IgA and IgA1 levels were positively related to urinary red blood cell count (P < 0.01, r s = 0.362, r s = 0.347, respectively). For longer-term study, urinary findings of IgAN patients underwent tonsillectomy were improved significantly than that of patients without tonsillectomy (P < 0.05).
Conclusion
Tonsils play an important role in the development of IgAN, and tonsillectomy may be a feasible treatment method for IgAN patients with chronic tonsillitis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Since it was first described by Professor Berger in 1968, IgA nephropathy (IgAN) has become the most common form of primary glomerular disease worldwide [1, 2] and remains a significant cause of end stage renal disease [3]. So far, it is still not very clear about the exact pathogenesis of IgAN, which is characterized by an overrepresentation of poorly galactosylated IgA1 molecules in the serum and mesangial deposition of IgA immune complexes. Mesangial deposition of IgA, especially polymeric IgA1 (pIgA1), suggested to be the initiating event in the pathogenesis of IgAN. Where do the mesangial deposition of IgA come from, however, it remains obscure. Previously, it is generally recognized that in IgAN patients, pathogenic IgA is derived from bone marrow cells [4], while some scholars realized that impaired mucosal immunity plays a significant role in the pathogenesis of IgAN [5–7]. In addition, clinical observations demonstrated that hematuria frequently emerged after tonsillar focal infection [8, 9]. However, tonsillectomy as a kind of therapeutic methods for IgAN patients still remains controversial, and the levels of serum IgA and IgA1 in the short time after tonsillectomy have rarely been reported. So we observed the serum and urinary findings of IgAN patients in short and longer time after tonsillectomy, providing evidence to elucidate the relationship between mucosal immunity and the pathogenesis of IgAN and help for therapy.
Subjects and methods
Subjects
All the patients were admitted to our hospital from October 2005 to September 2011 and satisfied with the following disease definition: (1) IgAN diagnosed by renal biopsy basing on predominant mesangial IgA containing immune complexes detected by immunofluorescence and light microscopy; meanwhile, systemic lupus erythematosus, Henoch–Scho¨nlein purpura and hepatic diseases were excluded by clinical history, physical examination and negative laboratory test results; (2) chronic tonsillitis and tonsils were hypertrophic or atrophic and characterized by a rough surface and pus in the deep crypts, as well as no acute tonsillitis recurrence. The normal controls were selected from individuals checked up at Health Examination Center of our hospital between June 2009 and February 2010. For the short-time observation, the subjects were 19 patients with IgAN and chronic tonsillitis (group A), 19 patients with chronic tonsillitis but without any renal disease (group B) and 19 normal controls (group C). For the longer-time observation, the subjects were 115 patients with IgAN and chronic tonsillitis, including 61 patients underwent both tonsillectomy and drug therapy (group D) and 54 with drug therapy alone (group E). The scientific and ethics committee of our hospital approved the study protocol, and we obtained informed consent from all patients before the study.
Treatment protocol
At their own decision and our recommendation, patients of group A, group B and group D received bilateral tonsillectomy, which was performed under general anesthesia in the Department of Otorhinolaryngology. Standard indications of tonsillectomy were recurrent tonsillitis three times or more per year, repeated episodes of gross hematuria at the time of tonsillitis or chronic tonsillitis with pus in tonsillar crypt. Patients of group D received both tonsillectomy and drug therapy while group E with drug therapy alone. Drug treatment protocol was as follows: from the time following up patients received oral Tripterygium Glycosides, an extract from a medicinal plant and benefit for IgAN [10–12], (20 mg/tid) therapy for 2 months and gradually withdrawn according to the urinary improvement. At the start of following up, if the urinary protein was greater than 1 g/24 h, the oral prednisone (30 mg/d) was added and lasted for a period of 2–3 months, then gradually withdrawn and to 10 mg/d for a long time (>12 months). Among them, 37 patients of group D and 35 of group E were treated with prednisolone, and there was no difference between numbers of two groups who underwent prednisolone therapy (P > 0.05). Meanwhile, all the patients treated by valsartan (80 mg/qd) or losartan (50 mg/qd) regularly, among them 25 patients of group D and 21 of group E were treated with valsartan and the others with losartan.
Evaluation of laboratory data and clinical data collection
The first morning urine of group A and group B patients was collected at T0 (before tonsillectomy), T2 (1 day after tonsillectomy), T3 (3 days after tonsillectomy), T4 (5 days after tonsillectomy) and for urine sediment test within 2 h. Urine sediment was examined in a centrifuged and concentrated sample of the urine using standardized methodology. At the same time, serum IgA and IgA1 were also evaluated at T0, T1 (immediately after tonsillectomy), T2, T3 and T4. IgA was measured by immunoturbidimetry, while IgA1 was determined by specific enzyme-linked immunosorbent assay (ELISA; R&D Biotechnology, USA). Morning fasting blood of group C was collected once for serum IgA and IgA1 evaluation. According to previous study [13], when urinary protein increased more than 1+ or RBC count in the sediment increased more than 20,000/ml and urinary occult blood test increased more than 1+, it was regarded as a deleterious change. According to the results of the urinary sediment artificial red blood cell (RBC) count, the degree of hematuria was divided into six ranks: <8(0), 8–25(1), 25–50(2), 50–100(3), 100–200(4) and >200 thousand(5). Proteinuria and urine sediment of group D and group E patients were tested at the 0, 1, 2, 3, 6 and 12 months during follow-up. Proteinuria was quantified in a 24-h urine collection at every visit using the routine standard method. Due to decisions of patients themselves, we only evaluated serum creatinine of patients in group D and group E at the starting and the end time point during follow-up. Related characteristics of all subjects were collected and demonstrated in the results.
Statistical analysis
SPSS version 13.0 for Windows (SPSS Inc., Chicago, IL, USA) was used for data analysis. Continuous variables were expressed as mean ± SD and median (IQR) depending on Gaussian distribution of variables. Grouped data were expressed as percentages (N). Comparisons were based on X2-test for categorical data and t test, ANOVA and Kruskal–Wallis T test for quantitative data. Correlations between the different parameters were analyzed by the Spearman’s rank correlation analysis. P values less than 0.05 were considered statistically significant.
Results
Baseline characteristics and clinical outcome
About short-time observation, clinical features of three groups were listed in Table 1. Age, gender, height, weight, blood pressure and course of disease were comparable among groups (P > 0.05). While levels of blood urea nitrogen, serum creatinine and serum uric acid were normal in three groups but were significantly higher in group A than that in group B or group C (P < 0.05, P < 0.01, respectively), and levels of effective glomerular filtration rate (eGFR) were also normal in three groups but were significantly lower in group A than that in group B or group C (P < 0.01).
About the following up study, the baseline clinical and histological characteristics were shown in Table 2. The age, gender, number of patients with episodes of gross hematuria, blood pressure and ratio of global sclerosis, segmental sclerosis, crescent and interstitial fibrosis were comparable between the two groups. All the patients had normal blood pressure. Fifty-eight patients of group D and 50 of group E only presented with hematuria and proteinuria, while 3 patients of group D and 4 of group E presented with renal insufficiency. Urinary protein and RBC count in the urinary sediment were comparable between the two groups at the onset of following up. Furthermore, the other laboratory parameters assessed were not significantly different between the two groups.
Observation of short term after tonsillectomy
The urinary findings of IgAN patients at different time before and after tonsillectomy were shown in Fig. 1. After tonsillectomy, 14 of 19 patients of group A (73.68 %) showed a deterioration of urinary findings and 5 did not, while only 2 of 19 patients of group B (10.52 %) showed deterioration. The deterioration was significantly more frequent in group A than in group B (P < 0.0 1) (Fig. 2a). Deterioration of urinary findings of 2 cases of group A occurred at T2 and became most significant at T3, while the remaining 12 cases occurred at T3. Previous of gross hematuria following upper respiratory tract infections existed in 10 of 14 patients (group A1) who showed a deterioration of urinary findings after tonsillectomy (71.42 %) as against in zero of 5 (group A2) without the deterioration (0 %). There was significant difference between group A1 than group A2 (P < 0.05; Fig. 2b).
The urinary findings of IgAN patients at different time before and short time after tonsillectomy. a Urinary protein qualitative test of sediment at different time points of short observation; plus symbol means positive result. b Urinary RBC count of sediment at different time points of short observation. The horizontal line means the median level of data
The urinary findings condition of subjects for short-time observation after tonsillectomy and previous upper respiratory tract infections. a Deterioration of urinary findings of patients in group A and group B after tonsillectomy; **P < 0.01 versus group B; b previous gross hematuria following upper respiratory tract infections of patients in group A; *P < 0.05 versus group A2. Yes = patients had history of gross hematuria after upper respiratory tract infections and No = patients without history of gross hematuria after upper respiratory tract infections
Before tonsillectomy, the levels of serum IgA and IgA1 in all the subjects were shown in Fig. 3. The levels of serum IgA in groups A, B and C were 2.56 ± 0.77 g/L, 2.04 ± 0.53 g/L and 1.94 ± 0.68 g/L, respectively, while serum IgA1 were 2.27 ± 0.85 g/L, 1.68 ± 0.46 g/L and 1.56 ± 0.62 g/L, respectively. Both the serum IgA and IgA1 levels were significantly higher in group A than that in group B or group C, respectively (P < 0.05, respectively). But there was no significant difference between group B and group C (P > 0.05). After tonsillectomy, the change tendency of serum IgA and IgA1 in group A and group B was shown in Fig. 4. In group A, levels of serum IgA and IgA1 had the same change tendency, which decreased at T1, at T2 began to increase, reached highest at T3 and at T4 decreased again. There had significant difference between T0 and T3, T3 and T4 (P < 0.05, respectively), while no significant difference at T1, T2, T4 compared with T0, respectively (P > 0.05, respectively). In group B, levels of serum IgA and IgA1 had no significant difference between different time points (P > 0.05).
The change tendency of serum IgA and IgA1 levels at different time points after tonsillectomy. a Levels of serum IgA and IgA1 in group A at different time points and their change tendency; *P < 0.05, versus T0; # P < 0.05, versus T4; b levels of serum IgA and IgA1 in group B at different time points and their change tendency; T0 = before tonsillectomy, T2 = 1 day after tonsillectomy, T3 = 3 days after tonsillectomy, T4 = 5 days after tonsillectomy
There existed significantly positive correlation between level of serum IgA and IgA1 and RBC count in the urinary sediment (P < 0.01, r s = 0.362, r s = 0.34, respectively) (Fig 5).
Correlations between rank of RBC count in the urinary sediment and the levels of serum IgA and IgA1. a Correlations between rank of RBC count in the urinary sediment and the level of serum IgA (P < 0.01, r s = 0.362); b correlations between rank of RBC count in the urinary sediment and the level of serum IgA1 (P < 0.01, r s = 0.347); Spearman’s rank correlation analysis was applied to determine the correlation
Outcome of longer-time observation
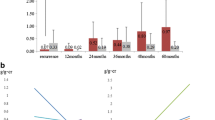
During follow-up, the levels and change tendency of urinary protein and urinary RBC count of different groups were shown in Fig 6. The urinary protein levels of group D at the 0, 1, 2, 3, 6 and 12 months during follow-up were 1.172 ± 0.845 g/24 h, 0.824 ± 0.512 g/24 h, 0.663 ± 0.341 g/24 h, 0.414 ± 0.304 g/24 h, 0.246 ± 0.164 g/24 h and 0.124 ± 0.122 g/24 h, respectively, while group E were 1.205 ± 0.78 g/24 h, 1.109 ± 0.621 g/24 h, 0.853 ± 0.426 g/24 h, 0.746 ± 0.442 g/24 h, 0.583 ± 0.353 g/24 h and 0.526 ± 0.332 g/24 h, respectively. The urinary RBC count of group D at the 0, 1, 2, 3, 6 and 12 months during follow-up were 13.44 ± 9.35 × 104/ml, 6.14 ± 4.41 × 104/ml, 4.27 ± 2.87 × 104/ml, 2.16 ± 1.03 × 104/ml, 1.02 ± 0.83 × 104/ml and 0.98 ± 0.67 × 104/ml, respectively, when group E were 13.21 ± 9.61 × 104/ml, 9.84 ± 7.23 × 104/ml, 6.57 ± 4.33 × 104/ml, 5.62 ± 3.11 × 104/ml, 2.94 ± 1.34 × 104/ml and 3.46 ± 2.07 × 104/ml, respectively. Urinary protein and urinary RBC count of group D at one month after tonsillectomy decreased significantly compared with before tonsillectomy (P < 0.01). There existed significant difference between the 2 and 1, the 3 and 2, the 3 and 6 months of urinary protein and urinary RBC count of group D (P < 0.05, respectively). Though urinary protein and RBC count of group E decreased significantly during follow-up, there existed significant difference compared with group D at different time points (P < 0.05, respectively).
The urinary protein and RBC count change condition of subjects for longer-time observation at different time points after different treatment. a Change tendency of urinary protein in different groups; Pa < 0.05 versus group E; Pb < 0.01, Pc < 0.05 versus the prior time point, respectively; b change tendency of urinary RBC count in different groups; Pa < 0.05 versus group E; Pb < 0.01, Pc < 0.05 versus the prior time point, respectively
Discussion
So far it is not very clear about the pathogenesis of IgAN; however, high level of aberrant IgA, especially pIgA1, suggested to be the initiating event in the pathogenesis of IgAN. In our study, both the levels of serum IgA and IgA1 were significantly higher in group A compared with group B or group C, respectively (P < 0.05, respectively), but there was no significant difference between group B and group C (P > 0.05), which is consistent with previous studies. In human, there are two subclasses of human IgA, IgA1 and IgA2, both of which are produced in mucosal and systemic immune compartments and can exist in monomeric or polymeric [14, 15]. Compared with IgA2, the major difference of IgA1 is the presence of an 18 amino acid hinge region. The hinge region is rich in serine, proline and threonine and having a variable number of O-linked oligosaccharides [16, 17], which play a significant role in the pathogenesis of IgAN.
However, what is the origin of pathogenic IgA? It is generally recognized that in IgAN pathogenic IgA1 is derived from bone marrow cells [4]. However, clinical observations demonstrated that hematuria frequently emerged after upper respiratory infection, especially tonsillar focal infection. In addition, high levels of pIgA are present in serum and tonsillar tissues of patients with IgAN. Then, it is suggested that tonsil may play a possible pathogenetic role of IgA in IgAN. Our study revealed that 14 of 19 patients of group A (73.68 %) showed a deterioration of urinary findings and 5 did not, while only 2 of 19 patients of group B (10.52 %) showed deterioration (P < 0.01, group A vs. group B). Previous gross hematuria following upper respiratory tract infections existed in 10 of 14 patients (group A1) who showed a deterioration of urinary findings after tonsillectomy (71.42 %) as against in zero of 5 (group A2) without the deterioration (0 %) (P < 0.05, group A1 vs. group A2). Therefore, we suggested that there existed intimate relationship between lgAN, tonsil and deterioration of urinary findings.
Tonsil as one of the mucosa-associated lymphoid tissues (MALT), its most important function is to produce B cells in follicle germinal center, which can synthesize hydrophilic secretory dimers IgA to protect the body from the invasion of exogenous material (bacteria and/or virus). Previous studies revealed that a deterioration of urinary findings happened tonsillar stimulated by an ultra short wave, which suggested that tonsil stimulation created a condition similar to that induced by an upper respiratory tract infection [8]. Our studies observed that in a short time after tonsillectomy, there occurred a deterioration of urinary findings and elevated levels of serum IgA and IgA1, while in a longer time after tonsillectomy, it occurred decreased urinary protein and RBC count in the urinary sediment. For correlation analysis, the serum IgA and IgA1 levels were correlated significantly with the RBC count in the urinary sediment in short-time study. All these suggested that tonsils play an important role in the development of IgAN. What are tonsils specific role in the development of IgAN, it is still controversial. Based on a great of studies, some scholars believed that at least a part of mesangial deposition of pIgA may directly originate from tonsil [18–20]. Meanwhile, some scholars put forward the ‘mucosa-bone-marrow axis’ and hypothesized that there existed an impaired IgA immune response in the ‘mucosa-bone-marrow axis’ of IgAN patients [4, 21–24]. Furthermore, clinical and experimental studies demonstrated that continued traffic happens between the mucosa and bone marrow in humans, mediated by antigen-specific lymphocytes and antigen-presenting cells [25, 26]. In our study, we observed levels of serum IgA and IgA1 at different time points after tonsillectomy, revealed that levels of serum IgA and IgA1 deceased at T1, began to increase at T2, reached highest at T3 and decreased at T4. There existed significant difference between T0 and T3, T3 and T4 (P < 0.05, respectively), while no difference between T0 and T1, T0 and T4 (P > 0.05, respectively). If serum IgA directly come from tonsils, level of serum IgA should decreased instantly after tonsillectomy or increased instantly because of tonsillar IgA quickly released after tissue injury, which is inconsistent with our results that tonsillectomy has no immediate effect on the levels of serum IgA and IgA1. So we may confirm that impaired mucosal immunity of tonsils contribute to the development of IgAN and speculate tonsillectomy may be a helpful therapy.
Clinically, IgAN may be asymptomatic and is detected by the presence of microscopic hematuria or proteinuria at screening or check-up visits. So abnormality of urinary findings may be the main characteristic of IgAN patients. Studies suggested that proteinuria was one of the risks for dialysis or death [27], and hematuria was the risk for end stage renal disease in IgAN [28]. Our longer-term study observed significantly decreased urinary protein and RBC count in the urinary sediment at every time points during follow-up compared with the onset time and controls(P < 0.01 and P < 0.05, respectively). From the above data, we concluded that tonsillectomy can improve urinary findings of patients with both IgAN and tonsillitis. Then, we speculated that tonsillectomy may be a feasible treatment method for IgAN patients with chronic tonsillitis, though tonsillectomy still controversial for IgAN patients [29].
Conclusion
Our study showed that tonsils play an important role in the development of IgAN, and tonsillectomy may be a feasible treatment method for IgAN patients with chronic tonsillitis, though further investigations need to do.
References
Li LS, Liu ZH (2004) Epidemiologic data of renal diseases from a single unit in China: analysis based on 13,519 renal biopsies. Kidney Int 66:920–923
D’Amico G (1987) The commonest glomerulonephritis in the world: igA nephropathy. Q J Med 64:709–727
Sanders JT, Wyatt RJ (2008) IgA nephropathy and Henoch-Schonlein purpura nephritis. Curr Opin Pediatr 20:163–170
van den Wall BA, Daha MR, Evers-Schouten J et al (1988) Serum IgA and the production of IgA by peripheral blood and bone marrow lymphocytes in patients with primary IgA nephropathy: evidence for the bone marrow as the source of mesangial IgA. Am J Kidney Dis 12:410–414
Lai KN (2012) Pathogenesis of IgA nephropathy. Nat Rev Nephrol 8:275–283
Floege J (2011) The pathogenesis of IgA nephropathy: what is new and how does it change therapeutic approaches? Am J Kidney Dis 58:992–1004
Barratt J, Feehally J (2011) Primary IgA nephropathy: new insights into pathogenesis. Semin Nephrol 31:349–360
Yamabe H, Sugawara T, Nakamura M et al (2004) Involvement of tonsils in IgA nephropathy. Acta Otolaryngol Suppl 555:54–57
Masuda Y, Terazawa K, Kawakami S et al (1988) Clinical and immunological study of IgA nephropathy before and after tonsillectomy. Acta Otolaryngol Suppl 454:248–255
Qian SZ, Xu Y, Zhang JW (1995) Recent progress in research on Tripterygium: a male antifertility plant. Contraception 51:121–129
Rong S, Hu WX, Liu ZH, Tang Z, Li LS (1998) A new regime of Tripterygium wilfordii Hook f. in treating primary mesangial proliferative glomerulonephritis (in Chinese). J Nephrol Dial Transplant 7:409–414
Chen YZ, Gao Q, Zhao XZ (2010) etal (2010) Meta-analysis of Tripterygium wilfordii Hook F in the immunosuppressive treatment of IgA nephropathy. Intern Med 49(19):2049–2055
Yamabe H, Sugawara T, Nakamura M, Shimada M (2004) Involvement of tonsils in IgA nephropathy. Acta Otolaryngol Suppl 555:54–57
Kerr MA (1990) The structure and function of human IgA. Biochem J 271:285–296
Woof JM, Russell MW (2011) Structure and function relationships in IgA. Mucosal Immunol 4:590–597
Lai KN (2009) Recent advances in IgA nephropathy. World Scientific, Hackensack NJ, p 419
Tomino Y (2007) IgA nephropathy today in Contributions to nephrology. Basel, Karger, p 255
Tomino Y, Sakai H, Endoh M et al (1983) Cross-reactivity of IgA antibodies between renal mesangial areas and nuclei of tonsillar cells in patients with IgA nephropathy. Clin Exp Immunol 51:605–610
Xie Y, Chen X, Nishi S et al (2004) Relationship between tonsils and IgA nephropathy as well as indications of tonsillectomy. Kidney Int 65:1135–1144
Meng H, Ohtake H, Ishida A et al (2012) IgA production and tonsillar focal infection in IgA nephropathy. J Clin Exp Hematop 52:161–170
van den Wall BA, Beyer WE, Evers-Schouten JH et al (1989) Humoral immune response to influenza vaccination in patients with primary immunoglobulin A nephropathy. J Clin Invest 84:1070–1075
van den Wall BA, Daha MR, van Es LA (1989) Immunopathogenetic aspects of IgA nephropathy. Nephrologie 10:141–145
van Es LA, van den Wall BA, Stad RK et al (1995) Enigmas in the pathogenesis of IgA nephropathy. Contrib Nephrol 111:169–175
Suzuki Y, Tomino Y (2007) The mucosa-bone-marrow axis in IgA nephropathy. Contrib Nephrol 157:70–79
Kunkel EJ, Butcher EC (2003) Plasma-cell homing. Nat Rev Immunol 3:822–829
Wiedle G, Dunon D, Imhof BA (2001) Current concepts in lymphocyte homing and recirculation. Crit Rev Clin Lab Sci 38:1–31
Berthoux F, Mohey H, Laurent B et al (2011) Predicting the risk for dialysis or death in IgA nephropathy. J Am Soc Nephrol 22:752–761
Vivante A, Calderon-Margalit R, Skorecki K Hematuria and risk for end-stage kidney disease. Curr Opin Nephrol Hypertens. doi:10.1097/MNH.0b013e32835f7241
Ponticelli C (2012) Tonsillectomy and IgA nephritis. Nephrol Dial Transplant 27:2610–2613
Acknowledgments
This study was supported by grants from the Key Program (81170663) of the National Natural Science Foundation of China and Program (12JJ6094) of the Natural Science Foundation of Hunan province.
Conflict of interest
The authors have no conflicts of interest to disclose.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Liu, Y., Liu, H., Tu, X. et al. Study of tonsillectomy for IgA nephropathy patients: short- and longer-term observation. Int Urol Nephrol 46, 1153–1159 (2014). https://doi.org/10.1007/s11255-013-0606-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-013-0606-9