Abstract
Ischemia, reperfusion, and subsequent free radical damage have been implicated in many voiding disorders. Our goal was to investigate further the mechanisms of these disorders, with particular emphasis on nerve and mitochondrial function and on detrusor smooth-muscle cells. The effects on contractile responses to various stimulations, citrate synthase, choline acetyltransferase activities, and vesicular acetylcholine transporter were evaluated after ischemia alone and ischemia/reperfusion 2 h, 7 days, and 14 days. Nerve density and detrusor cell apoptosis were also measured. The contractile responses were significantly decreased at both 7 and 14 days reperfusion, although at 14 days some recovery was observed. Similar patterns were seen for the intramural nerves, both nerve cell cytoskeletal structures and cholinergic neurotransmitters. Citrate synthase activity was also depressed by ischemia and 2 h reperfusion, but the activity recovered by 7 days. Detrusor cell apoptosis was not significantly affected by ischemia and 2 h reperfusion; but showed an approximately 14-fold increase at both 7 and 14 days reperfusion. Reperfusion following ischemia resulted in worsening intramural bladder nerve dysfunction, nerve fiber injury, mitochondrial injury, and damaged detrusor muscle cells. However, at 14 days reperfusion, nerve and mitochondrial regeneration occurred and resulted in partial recovery of contractile function.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The urinary bladder regularly experiences ischemia and reperfusion. During the normal micturition cycle, there is a brief period of ischemia and hypoxia during bladder contraction and immediate reperfusion following voiding. In the rat bladder, Saito et al. observed that acute urinary retention decreased blood flow and there was a subsequent increase in blood flow following catheterization [1]. Similarly, in normal humans, there is a significant decrease in blood flow at maximum bladder capacity and rebound immediately following drainage [2]. Further, it is thought that several pathological situations that induce bladder dysfunction, such as partial bladder outlet obstruction, bladder hyperactivity, arterial atherosclerosis and/or diabetes may be mainly or partially caused by ischemia and reperfusion (I/R) injury [3–5]. Previous studies have shown that reperfusion causes more severe damage than ischemia alone [6]. During the reperfusion period, the formation of reactive oxygen species (ROS) and reactive nitrogen species (RNS) causes an alteration of cellular ionic homeostasis, promoting intracellular Ca2+ build up, and resulting in cellular and subcellular membrane peroxidation [7].
Studies have shown ROS and RNS are the leading cause of neuronal dysfunction in ischemic overactive bladder [5, 8]. Inhibition of nitric oxide (NO) synthesis has been shown to diminish the dysfunction caused by bladder outlet obstruction [9]. These oxidative and nitrosative stresses are well known neurotoxic agents. They are involved in bladder intramural nerve damage and are likely to result in nerve degeneration.
It is known that nerve fibers can regenerate after injury, however, there is considerable uncertainty about when nerve terminals and endplates will re-develop and at what time neuromuscular transmission re-occurs. There is a lack of information about the bladder nerve and detrusor cell recovery process following I/R. We therefore carried out this study by immunohistological techniques, biochemical study, and Western blotting to evaluate the possibility that nerve endings of the bladder may be injured during I/R and that there may be regeneration following reperfusion. In addition, we also assess the subsequent damage to detrusor smooth-muscle cells.
Materials and methods
These studies were approved by the Institutional Animal Care and Use Committee of the Stratton Affairs Medical Center, Albany, NY.
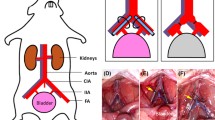
Five groups of four male New Zealand White rabbits (3–5 kg) each were studied. All rabbits were initially sedated with ketamine–xylazine (25 mg/kg ketamine/5 mg/kg xylazine, i.m.) and anesthesia was maintained with isoflorane (1–3%) inhalation. In group 1, (ischemia alone groups), vesical arteries were dissected free of the surrounding connective tissue and were then clamped bilaterally with microvascular clamps for 2 h and the animals were euthanized immediately on the same day. In groups 2, 3, and 4, bilateral ischemia was induced for 2 h, after which the microvascular clamps were removed and the rabbits were allowed to recover for 2 h, 7 days, or 14 days, respectively. In group 5, sham surgery was performed and the animals were euthanized 14 days after surgery. Sham surgery consisted of dissecting the vessels entering the bladder base and then closing the incision. Gentamicin (1 mg/kg) and buprenorphine hydrochloride (0.3 mg/kg) were given intramuscularly to all rabbits on the first and second days after surgery.
Bladder strip preparation and isometric contractile responses
After the bladders were removed and weighed, three 0.2 × 1 cm longitudinal strips were obtained. The bladder strips included muscle and mucosa layers. The rest of the bladder tissue was separated by blunt dissection into muscle and mucosa layers and immediately frozen in liquid nitrogen and stored at −80°C for further biochemical and Western blotting studies.
Each strip was mounted in a separate 12-ml bath containing Tyrode’s solution (124.9 mM NaCl, 2.6 mM KCl, 23.8 mM NaHCO3, 0.5 mM MgCl2, 0.4 mM NaH2PO4, 1.8 mM CaCl2, and 5.5 mM dextrose) maintained at 37°C and equilibrated with a mixture of 95% oxygen and 5% carbon dioxide. The contractile responses were recorded on a Grass model D polygraph and digitized using a Polyview digital recorder connected to the polygraph. In brief, an initial resting tension of 2 g was applied for 30 min, and the responses were recorded isometrically using a force–displacement transducer. Electrical field stimulation (FS) was achieved by use of supramaximal voltages (80 V) at 2, 8, and 32 Hz. After FS, the maximal responses were determined sequentially for adenosine triphosphate (ATP) (2 mM), carbachol (20 μM), and KCl (120 mM). A series of three washes, at 15-min intervals, with Tyrode’s solution followed each of the pharmacological stimulations.
Protein isolation and Western blotting
Frozen muscle tissue samples of bladder muscle wall were homogenized on ice in buffer (50 mM Tris, pH 7.5, 5% Triton) containing the Halt protease inhibitor cocktail (Pierce, Rockford, IL, USA) at 100 mg/ml. After addition of SDS (final concentration, 1%), the sample was boiled for 5 min and centrifuged at 10,000 rpm for 15 min. Protein concentration of the supernatant was determined using the BCA protein assay (Pierce) against a BSA protein standard in a SpectraMAX Plus microplate reader (Molecular Devices, Sunnyvale, CA, USA). Equal amounts of total protein (30 μg) from control and ischemic rabbit bladders were loaded on 10% SDS-PAGE gels and transferred to Immobilon-P membranes in buffer (25 mM Tris, 192 mM glycine, and 20% (v/v) methanol). Membranes were blocked with 5% nonfat milk. The membranes were then washed and probed with primary antibody, which was goat anti-vesicular acetylcholine transporter (VAChT) (Santa Cruz Biotechnology, Santa Cruz, CA, USA) at 1:50 dilution, followed by incubation with bovine anti-goat secondary antibody (1:5,000 dilution; Santa Cruz Biotechnology). Substrates were visualized using ECL plus (Amersham Pharmacia Biotech, Buckinghamshire, UK) substrate. Band intensities were scanned and analyzed with a Kodak Image Station 440CF and Kodak 1D image-analysis software (Scientific Image System, Rochester, NY, USA)
Choline acetyl transferase (ChAT) activity
Frozen muscle tissue samples are homogenized in ice-cold phosphate buffer (50 mM, pH 7.4) containing 10 mM EDTA and centrifuged at 20,000g for 30 min to remove the cell membranes, mitochondria, and nuclei. Aliquots are incubated at 37°C for 10 and 20 min with 200 μl reaction mixture consisting of 0.2–10 mM acetyl-coenzyme A (acetyl-CoA) (substrate), 0.2 mM 3H-acetyl-CoA (200 mCi/mmol), 8 mM choline, 50 mM sodium phosphate, 0.3 M NaCl, 20 mM EDTA, and 96 nM physostigmine. After incubation, each solution is diluted with 5 ml 0.01 M sodium phosphate and the reaction stopped with 2 ml acetonitrile containing 5 mg/ml tetraphenylboron. The contents of each reaction tube are then transferred to a 20-ml scintillation vial and 10 ml Betamax scintillation fluid is added slowly to each vial. The vials are shaken gently and the samples are left to stand for 1 h while the phases separate, extracting acetylcholine (3H-Ach) into the Betamax phase while 3H-acetyl-CoA stays in the aqueous phase. The aqueous phase is removed and 3H-ACh is measured using scintillation spectroscopy.
ChAT activity is reported as fmoles Acetyl-Co-A generated per min per mg protein/30 min.
Citrate synthase (CS) assay
Frozen muscle and mucosa tissue samples are homogenized in ice-cold Tris buffer (50 mM, pH 7.6) at 50 mg/ml and centrifuged at 2500g for 10 min to remove the cell membranes and nuclei. A sample aliquot (100 μl) of supernatant is added to a 0.5-cm cuvette, with 1.0 ml 0.05 M Tris buffer (pH 7.6), 50 μl 0.2–10 mM oxaloacetate (substrate), 30 μl 12.3 mM acetyl-coenzyme A, 100 μl 1 mM 5,5′-dithiobis-2-nitrobenzoic acid (DTNB), and 100 μl 10% Triton X-100. The free coenzyme-A generated by CS activity reacts with DTNB to form a colored compound that is quantified at 412 nm. Absorbance is recorded every 30 s for 6 min (reaching steady state), using a Hitachi spectrophotometer. Protein concentration is determined using the Lowry method. Citrate synthase activity is given as nmol Coenzyme A generated per min per mg protein.
Immunohistological study
Neurofilament immunofluorescence staining
A section of full thickness bladder tissue from each specimen was immediately fixed in 10% neutral buffered formalin, routinely processed and embedded in a paraffin block. Five-micron thick sections were cut from each block and mounted on positively charged slides, deparaffinized in xylene, and hydrated through graded ethanol. Sections were then stained with the mouse monoclonal anti-neurofilament clone 2f11 (Neomarkers, Freemont, CA, USA) on the Ventana ES automated immunostainer. Detection was achieved using an Alex Fluor-488 conjugated secondary antibody, goat polyclonal to Mouse IgG (Jackson, West Grove, PA, USA; dilution 1:1,000). The transverse section of each specimen was captured in five frames at 200× magnification. The nerves in each image were highlighted using the Image Pro Plus software by manually selecting the pixel value within the stained nerves. The quantitative nerve density data was thus acquired from the stained cross-sections and the averages were then calculated for each group.
Apoptosis staining
To detect the cells undergoing apoptosis, an ApopTag detection kit (Millipore, Billerica, MA, USA) was used. Kit instructions for the formalin-fixed, paraffin-embedded tissue method was followed. Pretreatment was with proteinase K for 15 min at room temperature. Slides were incubated in equilibration buffer for 20 min followed by incubation in terminal deoxynucleotidyl transferase (TdT) enzyme at 37°C for 1 h. This step was followed by the stop wash buffer and incubated with anti-digoxigenin peroxidase according to the kit instructions. Diaminobenzidine development was done and counterstained with methyl green. Apoptotic cells appeared as dark-brown-stained cells. The transverse section of each specimen was captured in five frames at 200× magnification. The terminal deoxynucleotidyl transferase biotin-dUTP nick end labeling (TUNEL) positive detrusor cells were acquired from the stained cross-sections and the averages were then calculated for each group.
Data analysis
The contractile responses were normalized to a 100-mg tissue mass. All the data are presented as the mean value ± standard error of the mean. Analysis of variance followed by Bonferroni’s test for individual comparisons was used. Statistical significance was judged by a P value of <0.05.
Results
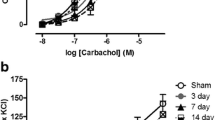
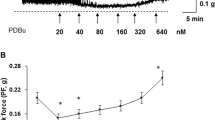
The contractility response to field stimulation is presented in Fig. 1a. The contractile responses to field stimulation were significantly decreased by 30–50 in the ischemia and I/R groups whereas at 7 and 14 days reperfusion the responses were significantly decreased by approximately 65%. For the rate of tension generation (Fig. 1b), the contractile velocity was little affected by ischemia alone, but was decreased significantly by approximately 60% at 7 and 14 days reperfusion. The responses to ATP, carbachol, and KCl showed little response to ischemia alone, but were significantly decreased by 40–60% after 7 and 14 days reperfusion. (Fig. 1c).
Effects of ischemia/reperfusion on maximal contractile responses (a) and rate of tension generation (b) to field stimulations. (c) The isometric contractile responses to ATP, carbachol, and KCl. Each bar indicates mean ± SEM for four individual rabbits; crosses denote significantly different from control group; asterisks denote significantly different from ischemia/reperfusion 7 days group; P < 0.05
Representative pictures of neurofilament immunofluorescence staining and the nerve density are shown in Figs. 2 and 3. There was a 20% decrease in nerve count by ischemia alone. By 7 days reperfusion the count decreased significantly by 60%; but returned to 40% of control count at 14 days reperfusion; which was significantly increased compared with 7 days reperfusion but still significantly lower than control.
Representative photo-micrographs of control (a), ischemia/reperfusion for 2 h (b), ischemia/reperfusion for 1 week (c), and ischemia/reperfusion for 2 weeks (d), showing neurofilament (arrow) within detrusor muscle bundles using anti-neurofilament immunofluorescence. All figures are in 400× magnification; scale bar represents 100 μm
Cholinergic nerve indicator, ChAT activities are shown in Fig. 4. ChAT activity did not change after ischemia alone. The activity decreased significantly to 70% of control activity after 2 h reperfusion; 30% of control at 7 days reperfusion; and then significantly increased to 60% of control at 14 days reperfusion. The other cholinergic nerve marker, VAChT expression, had almost the same pattern except no decrease was observed after 2 h reperfusion (Fig. 5).
Effects of ischemia/reperfusion on choline acetyltransferase (ChAT) activities in rabbit bladder wall. Each bar indicates mean ± SEM for four individual rabbits; crosses denote significantly different from control group; asterisks denote significantly different from ischemia/reperfusion 7 days group; P < 0.05
Representative Western blots of rabbit bladder homogenate probed for vesicular acetylcholine transporter (VAChT) expression (a) and average expression of VAChT in different samples (b). Y-axis numbers represent values compared with the control group, control is 100%. Equal amounts of total extractable proteins (40 μg) from rabbit bladder smooth muscle were separated by electrophoresis, transferred to membranes, and probed with specific antibody specific to VAChT, as described above. Lane 1 represents control group; lane 2, ischemia alone; lane 3, ischemia and reperfusion for 2 h; lane 4, ischemia and reperfusion for 1 week; lane 5, ischemia and reperfusion for 2 weeks. b Average expression of VAChT in different samples. Each bar indicates mean ± SEM for four individual rabbits; crosses denote significantly different from control group; asterisks denote significantly different from ischemia/reperfusion 7 days group; P < 0.05
Figure 6 displays the mitochondria marker enzyme citrate synthase activity in both bladder smooth muscle and mucosa. As demonstrated previously, CS activity is significantly higher in the mucosa than in the muscle layer. In the muscle layer, the CS activity decreased significantly to 70% of control activity by ischemia alone; remained at this activity for 2 h and 7 days reperfusion, and returned to control levels at 14 days reperfusion. For the mucosa, the CS activity decreased significantly to 70% of control activity for both the ischemia alone and the 2 h reperfusion period. At 7 days, the CS activity returned to control values, and increased to 35% above control values at 14 days reperfusion.
Effects of ischemia/reperfusion on citrate synthase (CS) activities in rabbit bladder wall and mucosa. Each bar indicates mean ± SEM for four individual rabbits; crosses denote significantly different from control group; asterisks denote significantly different from ischemia/reperfusion 7 days group; P < 0.05
TUNEL staining for detection of apoptotic detrusor cells following I/R are shown in Figs. 7 and 8. There were no significant differences between control, ischemia alone, and ischemia then reperfusion 2 h. However, at 7 days reperfusion, the apoptotic rate increased 13-fold, and by 14 days the rate had increased 15-fold.
Representative microphotographs reveals in-situ TUNEL staining for apoptosis cells in control (a), ischemia/reperfusion for 2 h (b), ischemia/reperfusion for 1 week (c) and ischemia/reperfusion for 2 weeks (d), showing detrusor smooth-muscle cell apoptosis (arrow) using TUNEL assay kit. All figures are 200× magnification. Scale bar represents 100 μm
Discussion
Our experiment provides an excellent animal preparation to evaluate bladder function after acute ischemia, such as acute bladder distention, and subsequent reperfusion, for example after bladder decompression. Our data confirm that reperfusion causes more injury than ischemia itself and that the bladder is able to recover over time. The bladder nerves progressively regenerated and mitochondrial function recovered by 2 weeks of reperfusion, especially in the bladder mucosa layer.
Our preparation of ischemia and later reperfusion has significant clinical correlates. It is well known that reperfusion after ischemia occurs with normal voiding. Under pathological conditions, such as bladder outlet obstruction or chronic arterial atherosclerosis in the elderly, I/R injury is more prominent and is considered the direct etiology of these specific urinary tract dysfunctions [7]. Our data clearly demonstrated that both ischemia alone and I/R resulted in a decrease in contractile responses to field stimulation (FS) and contractile agonists, resulting in bladder denervation, decreased ChAT activity, and promoted detrusor cell apoptosis. Previous studies have provided evidence that chronic bladder outlet obstruction, diabetic cystopathy, and atherosclerosis in the elderly all increased bladder neurogenic overcontraction and led to smooth muscle instability at resting tension [8, 10]. It was suggested that the super-sensitivity of detrusor cells after bladder outlet obstruction was because of partial denervation of the bladder [11]. In a previous study using an ischemia 4 hours model, the contractile responses to FS, carbachol, and KCl were significantly decreased after 1 day and 1 week reperfusion but significantly increased after 4 weeks reperfusion compared with responses after 1 week reperfusion [6]. Our results provided biochemical and histological evidence that bladder recovery began at 2 weeks reperfusion.
We provide good evidence that the bladder is able to recover from I/R injuries. ChAT, the biosynthetic enzyme of acetylcholine, and VAChT are both required for cholinergic neurotransmission. Both ChAT and VAChT are synthesized only in cholinergic neurons, thus ChAT and VAChT are complementary markers of cholinergic nerves. Neurofilaments are the major cytoskeletal components in neuronal cells [12]. In ischemic nerve degeneration, myelin appears to be particularly vulnerable to free radicals, activated neutrophils, and cytokine formation [13]. In our study, ChAT and VAChT both decreased up to 7 days of reperfusion and then increased. Similarly, neurofilament staining decreased up to 7 days of reperfusion and then increased. Previous studies have shown that the I/R injury is primarily related to free radical damage The current study shows that maximal damage is observed at 7 days following the start of reperfusion, and the bladder shows some recovery by 2 weeks. The mechanisms may relate to catalase and superoxide dismutase (SOD). In a previous study in the rabbit bladder subjected to I/R, the natural antioxidant mechanism, SOD, significantly decreased at 7 days of reperfusion but recovered by 14 days [14]. Similar findings are seen in other preparations; for example, in a preparation looking at myocardial I/R injury, it was also shown that catalase and SOD protect the myocardium from I/R injury [15, 16].
Our data also show significant abnormalities of activity of citrate synthase, a mitochondrial marker, after I/R. Mitochondria play a predominant role in cellular energy production. In the absence of oxygen (hypoxia or ischemia), the mitochondrial respiration chain is disturbed and ATP synthesis decreases. Mitochondria are highly vulnerable to ischemic changes. Disruption of the mitochondrial respiratory chain after I/R results in overproduction of mitochondrial reactive oxygen species (ROS), activation and leakage of pro-apoptosis mediators from mitochondria into the cytosol, opening of the mitochondrial permeability transition pore, and activation of downstream events eventually leading to cell apoptosis [17]. Hence our finding of progressive muscle cell apoptosis is not surprising. ROS may also stimulate secondary the messenger calcium. Calcium can upregulate several protein kinases, phosphatases, and proteases and is an important positive modulator of the mitochondria transition pore [18, 19]. Opening the mitochondrial pore causes swelling, collapses membrane potential, and finally results in total inhibition of mitochondrial function [20, 21].
We also found that there was considerable and progressive muscle cell apoptosis after I/R. Several studies in I/R and diabetes have shown that oxidative stress is associated with an increase in detrusor apoptotic cells [3, 22]. Our results are very similar to this. Interestingly, although most other measures we used had recovered by 14 days of reperfusion, we still found an increase in muscle apoptosis at 14 days. In a rat bladder I/R study, peak apoptosis was observed 3 days after ischemia induction and then decrease at 7 days reperfusion [22]. The differences of apoptosis time course may be associated with different species (rat vs. rabbit) and different ischemia duration (30 min vs. 2 h).
Another interesting finding of this study is that the mitochondrial marker citrate synthase recovered by 7 days in the mucosa but not until 14 days in the muscle. This somewhat quicker improvement in the mucosa is suggested by a previous study of SOD in the muscle and mucosa in which SOD levels were higher in the mucosa [14]. In a partial bladder outlet obstruction study, protein nitration and carbonylation increased significantly in mucosa at 8 weeks obstruction, much more than in the wall layer at the same period [4]. The bladder mucosa has a high metabolic rate and greater blood flow than the detrusor muscle layer, so is more vulnerable to ischemic damage [23]. However, higher metabolic rate and blood supply may also account for quick recovery in I/R injury.
Our results confirm that reperfusion results in greater injury than 2 h of ischemia in the rabbit bladder; and that the mechanisms of this injury involve mitochondrial and neuronal damage.
Abbreviations
- I/R:
-
Ischemia and reperfusion
- ROS:
-
Reactive oxygen species
- RNS:
-
Reactive nitrogen species
- NO:
-
Nitric oxide
- ATP:
-
Adenosine triphosphate
- VAChT:
-
Vesicular acetylcholine transporter
- ChAT:
-
Choline acetyltransferase
- CS:
-
Citrate synthase
- FS:
-
Field stimulation
- SOD:
-
Superoxide dismutase
- DTNB:
-
5,5′-Dithiobis-2-nitrobenzoic acid
- TdT:
-
Terminal deoxynucleotidyl transferase
- TUNEL:
-
Terminal deoxynucleotidyl transferase biotin-dUTP nick end labeling
References
Saito M, Miyagawa I (2001) Bladder dysfunction after acute urinary retention in rats. J Urol 165:1745–1747. doi:10.1016/S0022-5347(05)66406-3
Kershen RT, Azadzoi KM, Siroky MB (2002) Blood flow, pressure and compliance in the male human bladder. J Urol 168:121–125. doi:10.1016/S0022-5347(05)64843-4
Beshay E, Carrier S (2004) Oxidative stress plays a role in diabetes-induced bladder dysfunction in a rat model. Urology 64:1062–1067. doi:10.1016/j.urology.2004.06.021
Juan YS, Lin WY, Kalorin C, Kogan BA, Levin RM, Mannikarottu A (2007) The effect of partial bladder outlet obstruction on carbonyl and nitrotyrosine distribution in rabbit bladder. Urology 70:1249–1253. doi:10.1016/j.urology.2007.09.047
Azadzoi KM, Yalla SV, Siroky MB (2007) Oxidative stress and neurodegeneration in the ischemic overactive bladder. J Urol 178:710–715. doi:10.1016/j.juro.2007.03.096
Bratslavsky G, Kogan BA, Matsumoto S, Aslan AR, Levin RM (2003) Reperfusion injury of the rat bladder is worse than ischemia. J Urol 170:2086–2090. doi:10.1097/01.ju.0000092144.48045.13
Zhao Y, Levin SS, Wein AJ, Levin RM (1997) Correlation of ischemia/reperfusion or partial outlet obstruction-induced spectrin proteolysis by calpain with contractile dysfunction in rabbit bladder. Urology 49:293–300. doi:10.1016/S0090-4295(96)00452-9
Azadzoi KM, Tarcan T, Kozlowski R, Krane RJ, Siroky MB (1999) Overactivity and structural changes in the chronically ischemic bladder. J Urol 162:1768–1778. doi:10.1016/S0022-5347(05)68236-5
Conners W, Whitebeck C, Chicester P, Legget R, Lin AD, Johnson A et al (2006) L-NAME, a nitric oxide synthase inhibitor, diminishes oxidative damage in urinary bladder partial outlet obstruction. Am J Physiol Renal Physiol 290:F357–F363. doi:10.1152/ajprenal.00261.2005
Pandita RK, Fujiwara M, Alm P, Andersson KE (2000) Cystometric evaluation of bladder function in non-anesthetized mice with and without bladder outlet obstruction. J Urol 164:1385–1389. doi:10.1016/S0022-5347(05)67204-7
Sibley GN (1987) The physiological response of the detrusor muscle to experimental bladder outflow obstruction in the pig. Br J Urol 60:332–336
Vannucchi MG, Midrio P, Zardo C, Faussone-Pellegrini MS (2004) Neurofilament formation and synaptic activity are delayed in the myenteric neurons of the rat fetus with gastroschisis. Neurosci Lett 364:81–85. doi:10.1016/j.neulet.2004.03.095
Coban YK, Ciralik H, Kurutas EB (2006) Ischemic preconditioning reduces the severity of ischemia–reperfusion injury of peripheral nerve in rats. J Brachial Plex Peripher Nerve Inj 1:2. doi:10.1186/1749-7221-1-2
Erdem E, Leggett R, Dicks B, Kogan BA, Levin RM (2005) Effect of bladder ischaemia/reperfusion on superoxide dismutase activity and contraction. BJU Int 96:169–174. doi:10.1111/j.1464-410X.2005.05589.x
Chen Z, Siu B, Ho YS, Vincent R, Chua CC, Hamdy RC et al (1998) Overexpression of MnSOD protects against myocardial ischemia/reperfusion injury in transgenic mice. J Mol Cell Cardiol 30:2281–2289. doi:10.1006/jmcc.1998.0789
Woo YJ, Zhang JC, Vijayasarathy C, Zwacka RM, Englehardt JF, Gardner TJ, Sweeney HL (1998) Recombinant adenovirus-mediated cardiac gene transfer of superoxide dismutase and catalase attenuates postischemic contractile dysfunction. Circulation 98:II255–260; discussion II260–251
DiMauro S, Hirano M, Schon EA (2006) Approaches to the treatment of mitochondrial diseases. Muscle Nerve 34:265–283. doi:10.1002/mus.20598
Marchetti P, Castedo M, Susin SA, Zamzami N, Hirsch T, Macho A et al (1996) Mitochondrial permeability transition is a central coordinating event of apoptosis. J Exp Med 184:1155–1160. doi:10.1084/jem.184.3.1155
Marchetti P, Susin SA, Decaudin D, Gamen S, Castedo M, Hirsch T et al (1996) Apoptosis-associated derangement of mitochondrial function in cells lacking mitochondrial DNA. Cancer Res 56:2033–2038
Crompton M (1999) The mitochondrial permeability transition pore and its role in cell death. Biochem J 341(Pt 2):233–249. doi:10.1042/0264-6021:3410233
Morin D, Hauet T, Spedding M, Tillement J (2001) Mitochondria as target for antiischemic drugs. Adv Drug Deliv Rev 49:151–174. doi:10.1016/S0169-409X(01)00132-6
Saito M, Miyagawa IN (2002) (G)-Nitro-L-arginine methylester, a nitric oxide synthase inhibitor, diminishes apoptosis induced by ischemia–reperfusion in the rat bladder. Neurourol Urodyn 21:566–571. doi:10.1002/nau.10012
Badger WJ, Whitbeck C, Kogan B, Chichester P, Levin RM (2006) The immediate effect of castration on female rabbit bladder blood flow and tissue oxygenation. Urol Int 76:264–268. doi:10.1159/000091631
Acknowledgements
This material is based upon work supported in part by the Office of Research and Development Medical Research Service, Department of Veteran’s Affairs. And in part by NIH grant RO-1-DK 067114 and the Capital Region Medical Research Foundation.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Juan, YS., Chuang, S.M., Kogan, B.A. et al. Effect of ischemia/reperfusion on bladder nerve and detrusor cell damage. Int Urol Nephrol 41, 513–521 (2009). https://doi.org/10.1007/s11255-008-9492-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-008-9492-y