Abstract
A cross-sectional study was conducted to determine the seroprevalence of bovine brucellosis in communal cattle and wildlife at a wildlife–livestock interface in the southeast lowveld of Zimbabwe, part of the Great Limpopo Transfrontier Conservation Area. RBT and c-Elisa were used in serial for detection of antibodies against Brucella spp. Between July 2007 and October 2009, a total of 1,158 cattle were tested and the overall seroprevalence of brucellosis was 9.9%. A total of 97 wild animals (African buffaloes (n = 47), impala (n = 33), kudu (n = 16), and giraffe (n = 1)) were tested and only one animal (giraffe) was seropositive for brucellosis (1.03%). Brucella seroprevalence showed an increasing trend with age, with adult cattle (>6 years) recording the highest seroprevalence (11.1%), but the differences were not statistically significant. Similarly, female cattle recorded a relatively higher seroprevalence (10.8%) compared to males (7.9%), but the difference was not significant. However, a significant (P < 0.001) association between Brucella seropositivity and abortion history was recorded in female cattle. Similarly, Brucella seropositivity was significantly (P < 0.01) associated with a history of grazing in the park for female cattle. Overall, from the interface area, cattle with a history of grazing in the park recorded a significantly (P < 0.01) higher Brucella seroprevalence (13.5%) compared to those with no history of grazing in the park (4.9%). The significant association between abortion history and seropositivity observed in this study illustrates the potential economic significance of Brucella in cattle in this area. Hence, public awareness and further epidemiological studies of the disease in wildlife, livestock, and humans in the study area are of great importance.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Brucellosis is a global zoonotic disease which causes considerable animal and human health problems as well as huge economic costs (McGiven et al. 2008). The disease is caused by a group of bacteria belonging to the genus Brucella, which are gram-negative coccobacilli that possess surface antigens located on the lipopolysaccharide (Olsen and Tatum 2010; Whatmore 2009). Humans are mainly infected due to the consumption of contaminated non-pastured milk, cheese, or as an occupational exposure to infected animals, carcasses, uterine secretions, or aborted fetuses (Carvalho Neta et al. 2010). Ruminants being major production animals worldwide and prone to brucellosis, this disease has an important economic impact on their production. Its main threat is to cattle, African buffaloes (Syncerus caffer) and swine (Olsen 2010; Carter et al. 1995). Clinical signs of the disease include orchitis in males, abortion in females, and bursitis in both sexes (Olsen and Tatum 2010; OIE 2009). Chronic orchitis and fibrosis of the testicular parenchyma may result in permanent infertility in bulls (Carvalho Neta et al. 2010). As it decreases fertility in females, abortion makes the disease detrimental to production systems (Matope et al. 2010; Bricker and Halling 1994). Transmission of Brucella abortus is mainly by direct and mucosal contact with fluids or tissues associated with the birth or abortion of infected fetuses (Olsen and Tatum 2010). Testing of livestock for brucellosis is done by culture, serology, or by testing milk samples (Muma et al. 2007; McGiven et al. 2008; Nielsen et al. 2002), but isolation and identification of Brucella bacteria offers a definite diagnosis (Abdoel et al. 2008).
Interactions at the wildlife–livestock interface have been shown to influence disease dynamics because of the sharing of grazing land and water between wild and domestic animals (Muma et al. 2007; Bengis et al. 2002). Bovine brucellosis control programs have effectively reduced and eliminated the prevalence of diseases in livestock, but spillover of the disease from domestic livestock to wildlife has complicated regulatory efforts (Olsen and Tatum 2010). In South Africa, several species of wildlife such as African buffalo, hippopotamus (Hippopotamus amphibious), zebra (Equus burchellii), eland (Taurotragus oryx), waterbuck (Kobus elipsiprymnus), and impala (Aerpyceros melampus) have tested serologically positive for brucellosis and surveys revealed up to 23% seropositive African buffaloes from the Kruger National Park (KNP; Herr and Marshall 1981). In Zimbabwe, 48% of African buffalo serum samples were seropositive for Brucella antibodies (Madsen and Anderson 1995). These samples were collected from game areas where contact with domestic cattle, sheep, and goats could be excluded. It was concluded that brucellosis was probably a sustainable infection in African buffalo populations, which consequently should be considered a possible source of re-infection for domestic stock (Madsen and Anderson 1995). Expansion of ecotourism-based industries, changes in land-use practices and an escalating competition for resources have been reported to increase the contact between free-ranging wildlife, domestic animals, and humans (Osofsky et al. 2008; Bengis et al. 2002). The creation of the GLTFCA should increase the contacts between wildlife and livestock between Zimbabwe, South Africa, and Mozambique (Fig. 2). Consumption of raw milk is a tradition practiced by people in cattle-producing areas of Zimbabwe; it is important to understand animal brucellosis. This study was carried out to investigate/explore the presence of bovine brucellosis in communal cattle and wildlife at a wildlife–livestock interface in the southeast lowveld of Zimbabwe in the GLTFCA. Our main concern was to investigate if the presence of the interface has an impact on the prevalence of brucellosis in cattle. As an important animal and human disease, knowledge about brucellosis in such interface areas is important, particularly in the context of the GLTFCA.
Material and methods
Location and selection of study areas and sites
The study was conducted in the southeast lowveld of Zimbabwe (Fig. 1), a semi-arid area with an annual rainfall below 500–600 mm. Study areas, all located in the Sengwe communal land, were purposively selected to include sites with an interface with wildlife from the Gonarezhou National Park (GNP) and KNP and others without a wildlife–livestock interface area. GNP located in the southeast lowveld is Zimbabwe’s second largest game reserve covering an area of 5,000 km2 of open grasslands and dense woodland. The park forms a direct connection with wildlife populations from the Mozambique’s Limpopo National Park where animals move freely between the two sanctuaries and adjoining South African KNP separated from GNP by the Sengwe communal lands (Fig. 2).
The selected study areas with a wildlife–livestock interface were Malipati and Pesvi communal areas. Malipati lies adjacent to GNP and the selected dip tank lies less than 1 km from the unfenced areas of the Park, allowing direct and indirect contact between domestic and wild animals. Cattle from Malipati share common grazing and watering sources with wild animals (e.g., African buffaloes, zebra, elands, and impalas) particularly during the dry season (August to November) when there is limited pasture and water sources for communal farmers. Pesvi lies adjacent to KNP across the Limpopo River, and the selected dip tank lies less than 3 km from the unfenced northern boundary of the park. During the dry season, when the Limpopo River is dry, wild animals (e.g., African buffaloes) from KNP cross into Pesvi communal areas and cattle from Pesvi communal areas cross into KNP (personal observations, 2008). The comparative study areas without a wildlife–livestock interface were Chomupani and Pfumare communal areas. These areas are situated more than 25 km from GNP boundary and more than 70 km from KNP, and wildlife is either absent or occurs at very low densities. Cattle reared in these areas have no apparent direct contact with wild animals.
Owing to the availability of animal handling facilities and access to large populations of cattle, dip tanks were chosen as the study sites. One dip tank was selected from each study area, giving a total of four dip tanks, two from an interface area (Malipati and Pesvi dip tanks), and two from a non-interface area (Chomupani and Pfumare dip tanks). In these areas, cattle are dipped bi-weekly with acaricides (Amitraz) during the rainy season and monthly during the dry season for the control of ticks. For wildlife, the study sites were GNP and Malilangwe Conservancy (north of GNP).
Sampling of animals and sample collection
For cattle, all herds which were present on the day of sample collection were included for sampling. Systematic random sampling (i.e., 1/10 animals interval) was used to select individual animals. Calves from seropositive dams have been reported to be usually seropositive for up to 4–6 months due to colostral antibodies and later test negative (Blood et al. 2000). Hence, in order to minimize false positive reactors due to maternal antibodies in younger animals, only animals at least 7 months old were included in the present study. Local indigenous cattle used in the study were Tuli, Ngoni, and Sanga type (a stabilized Bos taurus × Bos indicus cross), commonly known as “Mashona.” Blood samples for the detection of antibodies against Brucella spp. were collected from all sampled animals. The survey covered the period from July 2007 to October 2009.
Samples from free-ranging wildlife were collected from various sources. Wildlife samples were collected from those slaughtered for the GNP staff rations, hunter kills, animals captured for translocation, and those captured for the purpose of this study. The survey covered the period from July 2007 to February 2009. An organized boma capture of wildlife (helicopter pushing animals in plastic enclosure for subsequent tele-anesthesia) for the purpose of this study was done during the month of October 2008 where 38 buffaloes, 16 Greater Kudu, and 24 Impalas from four different herds were captured in a boma in GNP (Mabalauta area; Fig. 1). Blood samples were collected for the detection of antibodies against Brucella spp. using the RBT and the c-ELISA.
Epidemiological data
Information about each animal (cattle) such as sex, age, abortion history, and history of grazing in the Park according to the owner (GNP or KNP) were collected and entered into a data sheet.
Testing for bovine brucellosis
For both cattle and wildlife, antibodies to Brucella spp. were detected by using the RBT and the c-ELISA tests. Testing of serum samples using the RBT was done as described earlier (Alton et al. 1988). Briefly, as outlined earlier (Matope 2008), B. abortus antigen (VLA, UK) was used to screen sera for the presence of antibodies to Brucella spp. The test was performed on round-bottomed welled Pyrex plates where 25 μl of the serum was mixed with equal amounts of stained Rose Bengal antigen (pH 3.65). The samples were mixed on a rocker for 5 min. The degree of agglutination was graded on an ordinal scale from 0 (no agglutination) to 3 (coarse clumping), with RBT scores of 2 and 3 being considered positive.
All RBT seropositive sera were further tested using the SvanovirTM Brucella-Ab c-ELISA test kits (Svanova Biotech, Uppsala, Sweden). The c-ELISA was conducted according to the manufacturer’s instructions. Briefly, as outlined earlier (Matope 2008), the test was carried out in 96-well polystyrene plates (Nalge Nunc, Denmark) that were pre-coated with Brucella spp. lipopolysaccharides (LPS) antigen. Serum diluted 1:10 was added to each well and immediately followed by equal volumes of pre-diluted mouse monoclonal antibodies specific for a common epitope of the O-polysaccharide of the smooth LPS molecule. The reactivity of the mouse monoclonal antibody was detected using goat antibody to mouse IgG that was conjugated to horseradish peroxidase. Hydrogen peroxidase substrate and ABTS chromogen were developed for 10 min. The reaction was stopped using 1 M H2SO4. Optical densities were read at 450 nm using a Titertek Multiscan® PLUS reader (Flow Laboratories, UK). The threshold for determining seropositivity was based upon the manufacturer’s recommendations (≥30%), with antibody titers recorded as percentage inhibition as defined by the ELISA kit supplier. In this study, a serial testing protocol (Matope 2008) was used, and hence, a serum was considered positive for antibodies to Brucella spp. if it was positive for both the RBT and c-ELISA.
Data analysis
The recording and editing of data was performed using Microsoft Excel®. Statistical analyses were performed using Stata SE/9.0 for Windows (Stata Corp., College Station, TX, USA). The overall number of seropositive animals was calculated from the total number of samples tested over the study period and expressed as a percentage. Seropositive cattle were examined in relation to age, sex, location, abortion history, and grazing history. Age, sex, location, abortion, and grazing history categories were generated as follows: four for age (≤2.5, >2.5–4, >4–6, and >6 years), two for sex (male and female), two for location (interface and non-interface), two for abortion history (aborted and not aborted), and two for grazing history (grazing in Park and not grazing in Park). Descriptive statistics for grazing history was restricted to cattle originating from the interface only. The chi-square test was used to measure differences between categories, and values of P < 0.05 were considered as significant.
Logistic regression analyses were conducted in Stata SE/9.0 for Windows to investigate the individual animal risk factors for infection with Brucella spp. Cattle in communal farming areas share common grazing and watering sources, and hence, herd risk factors were not investigated. Logistic regression analysis was used to test the Brucella-seropositive status of cattle (negative = 0, seropositive =1) according to age, sex, and location as predictor variables. The predictor variables were assessed for collinearity by cross tabulations using the two-sided Fisher’s exact test. Abortion history and grazing history were not included in the first model as they had high collinearity with sex and location, respectively. Hence, another model was restricted to females, where the history of abortion and grazing were included as additional predictors of seropositivity.
Results
Cattle
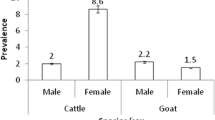
The distribution of sampled cattle and their seroprevalence according to different categories are shown in Table 1. A total of 1,158 cattle were sampled and the overall seroprevalence was 9.9%. The seroprevalence showed an increasing trend with age with adult cattle (>6 years) recording the highest seroprevalence, but the differences were not statistically significant (P > 0.05). Females recorded a relatively higher seroprevalence compared to males, but the difference was not statistically significant (P > 0.05). In females, the seroprevalence was significantly higher (P < 0.001) in those which had a history of abortion. The seroprevalence varied from 9.6% to 11.2% for cattle originating from the interface areas while it varied from 5% to 8.3% for those originating from the non-interface areas. Overall, the seroprevalence was relatively higher for cattle sampled from the interface areas compared to those sampled from the non-interface areas, but the difference was not significant (P > 0.05). From the interface, cattle with a history of grazing in the park recorded a significantly (P < 0.01) higher seroprevalence compared to those with no history of grazing in the park.
The overall logistic regression results showed an independent effect of age, sex, and location (Table 2). The model showed a non-significant increase in prevalence with age, in females and for cattle sampled from the interface areas. Logistic regression results restricted to female animals showed an independent effect of age, location, and history of abortion and that of grazing (Table 2). The results showed a non-significant association between antibodies against Brucella spp. and an increasing age of female animals and also a higher prevalence for those sampled from the interface areas. However, the results demonstrated a strong association (P < 0.001) between antibodies against Brucella spp. and a history of abortion (odds ratio (OR) = 35.8; 19.0 < OR < 67.6; χ 2 = 56.8; P < 0.01) and that of grazing in the park (OR = 3.3; 1.8 < OR < 6.1; χ 2 = 4.9; P < 0.01).
Wildlife
A total of 97 wild animals which included 47 buffaloes, 33 impala, 16 kudu, and 1 giraffe were tested for antibodies against Brucella spp. Only one animal, giraffe (Giraffa camelopar dalis) from the north of the park was positive for brucellosis (1.03%), and the rest were negative.
Discussion
This study provides first information on brucellosis infection in cattle and wildlife from the South east Lowveld of Zimbabwe, in the GLTFCA. An overall 9.9% of cattle tested were seropositive, but no Brucella antibodies were detected from buffaloes. Grazing in the adjacent national park seems to be a risk factor increasing brucellosis infection in cattle.
According to the local veterinarian and livestock technicians, none of the cattle from the studied areas had been vaccinated against brucellosis, implying that the antibodies detected were more likely to be due to natural infection with Brucella spp. rather than by B. abortus S19. Furthermore, the c-ELISA test used for confirmation of seropositive animals has been reported to differentiate vaccinal antibodies from those of natural infection (Nielsen et al. 2002). Cross-reactions with Yersinia enterocolitica were unlikely to have an impact on the results since this pathogen is assumed to be rare or absent in the tropics (Godfroid 2002; Nielsen et al. 2004), and the use of specific c-ELISA tests decreases such reactors (McGiven et al. 2008; Nielsen et al. 2004). The RBT screening test used has a high sensitivity (>90%), thus reducing the possibility of false negative reactors (OIE 2009). Despite the use of B. abortus antigens that extensively cross-react with antibodies of Brucella melitensis and Brucella suis (Alvarez et al. 2011; Nielsen et al. 1999), both species have not yet been isolated in cattle in Zimbabwe (Madsen 1989). Therefore, it is unlikely that the classification of tested animals in the present study was biased toward false negative and false positive results due to cross-reactions with other Brucella spp.
In Zimbabwe, brucellosis was reported as early as 1913 in dairy herds when seropositive animals were identified following abortion storms around Harare (Madsen 1989). The disease is endemic in Sub-Saharan African countries, including Zimbabwe with the prevalence rate varying according to agro-ecological regions (McDermott and Arimi 2002; Mohan et al. 1996; Muma et al. 2007; Matope et al. 2010). The source or origin of brucellosis in the present study area could not be accurately ascertained as there have been no previous studies on the disease in the area. However, earlier studies have demonstrated the presence of brucellosis in the commercial and smallholder sectors and other communal areas other than the present study area (Manley 1969; Swanepoel et al. 1975, 1976; Madzima 1987; Madsen 1989; Mohan et al. 1996; Matope et al. 2010). The spread of Brucella spp. from one herd and one area to another is often due to the movement of an infected animal into a non-infected susceptible herd (Matope et al. 2010; Crawford et al. 1990). The purchase of unknown Brucella-status cattle from the commercial to the communal sector for the purpose of restocking herds and genetic improvement and an increased uncontrolled movement of cattle due to agrarian reforms in the country have been attributed as the source of spread of brucellosis into the communal sector (Matope 2008). Unknown Brucella-status cattle purchased from commercial farms and translocated to the communal sector were mixed and cross-bred with the indigenous B. indicus breeds. As pointed out earlier (Matope 2008), these farming practices brought about mixing of naïve cattle between the commercial, communal, and smallholder sectors in the country and could be the source of brucellosis in the latter sectors.
The prevalence rate reported in this study was lower than previous reports for commercial dairy farms in Zimbabwe (Manley 1969; Swanepoel et al. 1975; 1976) but higher than that reported from smallholder farms (Madzima 1987; Madsen 1989; Mohan et al. 1996; Matope et al. 2010). The most important spread of brucellosis takes place from cow to cow, with infected cows contaminating the pasture and uninfected animals becoming infected by ingestion when grazing (Madsen 1989). However, the final prevalence rate is determined by the intensity of cattle contacts within and between herds and with infected pasture and water (Madsen 1989). Hence, brucellosis risk increases with change from a purely extensive, nomadic to a more-intensive form of cattle management (Thim and Wundt 1976). This probably explains the higher prevalence reported in commercial dairy farmers compared to the lower prevalence reported in traditional purely extensive form of cattle management in the study area. Carvalho Neta et al. (2010) described other factors associated with outcome of infection in cattle as dependent on age, reproductive and immunological status, natural resistance, route of infection, infectious challenge, and virulence of the strain.
As abortion is one of the main signs of brucellosis infection in cattle, the significant association between Brucella seropositivity and abortion history observed during the present study is consistent with earlier reports (Kubuafor et al. 2000; England et al. 2004; Muma et al. 2006; Matope et al. 2010). The presence of erythritol which is a growth stimulant for B. abortus increases the cows’ susceptible to Brucella infection particularly during early pregnancy (Moreno and Moriyon 2006; Quinn et al. 1999), and such infections can result in late term abortion (Carvalho Neta et al. 2010; Cunningham 1977). However, the association between history of abortion and seropositivity in infected herds could be distorted because a certain proportion of infected cows may not abort (Abernethy et al. 2011; Brinley Morgan 1977).
In support of earlier observations (McDermott et al. 1987), our findings suggest that the risk of infection with Brucella spp. is independent of cattle sex, but the sex and brucellosis risk association can vary with different cattle populations (Kadohira et al. 1997; Kubuafor et al. 2000; Omer et al. 2000). As reported earlier (Omer et al. 2000; Muma et al. 2006; Matope et al. 2010), older animals had increased chances of testing Brucella positive. The onset of sexual maturity is associated with a significant increase in the risk of infection with Brucella spp. (Walker 1999), and such animals are likely to seroconvert. However, cattle breeds’ variation of the age at which sexual maturity is attained is likely to influence the observed relationship between age and positive reactors in different sub-populations.
Brucellosis has been reported to be prevalent in areas of livestock–wildlife interactions (Nicoletti 1980; Jiwa et al. 1996; Muma et al. 2006, 2007). Although not statistically significant, the results of the present study showed that cattle at the interface and having a history of grazing in the park had increased chances of testing Brucella positive. At the interface, cattle share grazing pastures and watering points with African buffalos, greater kudus, and impalas. Although not detected in this study (except one giraffe), earlier studies in Zimbabwe showed the presence of brucellosis in wild animals such as the African buffalo, eland antelope, giraffe, impala, hippopotamus, black rhinoceros (Diceros bicornis), Burchell’s zebra, and waterbuck (Condy and Vickers 1969, 1972; Madsen and Anderson 1995). The absence of Brucella spp. seropositive wildlife during the present study could be attributed to the small sample size or that the sampled herds/animals were free from Brucella infection. However (Madsen and Anderson 1995), working in the same study area reported a seroprevalence of 8.2% (4 of 49) and 8.8% (3 of 34) in African buffaloes sampled from the GNP and surrounding hunting areas, respectively, and a seroprevalence of 3.7% (2 of 54) in giraffes, 3.7% (8 of 218) in eland, and 1.9% (1 of 53) in impala sampled from two mixed cattle and game ranches in the southeast lowveld. According to (Madsen and Anderson 1995), contact with livestock was likely in the cases of seropositive eland antelope, impala, and giraffe. However, about half of the positive samples from buffalo were obtained from animals that had no contact with cattle or other livestock. This probably demonstrates an independent Brucella infection cycle in the African buffalo, which consequently should be considered as a possible source of infection to domestic stock (Madsen and Anderson 1995). Hence, considering the contagious nature of Brucella spp. sharing grazing land and watering points between cattle and wildlife at the studied interface is likely to facilitate transmission of the disease in both directions. Despite a bias in the sample size, we do not have any explanation on the almost complete absence of seropositives in wildlife species, particularly in buffaloes. The fact that cattle grazing in the national park had an increased risk ratio (1.8) of contracting brucellosis may support the hypothesis of wildlife being a reservoir for the pathogen. Follow-up studies will be necessary to confirm the absence/presence of brucellosis in these wildlife populations. Olsen and Tatum (2010) described how difficult it is to eradicate brucellosis in cattle without resolution of the disease in wildlife. If the absence/presence is confirmed, this may indirectly inform about the degree of present contacts between buffalo populations from GNP and KNP, both belonging to the GLTFCA but separated by the Sengwe communal land.
The results of the present study established the presence of brucellosis in cattle in communal lands in the southeast lowveld of Zimbabwe with some degree of positive associations between its presence and the interface. If confirmed, these observations would mean that human communities living at the edge of the GLTFCA pay a sanitary price for being at the interface. This price is paid in terms of economic loss and also potentially in terms of public health as brucellosis could be a serious zoonosis. Although no human brucellosis information was available when this study was conducted, we strongly suggest further studies to investigate the impact of this zoonosis on human populations. Its cost to these communities is not isolated and should be added to other disease burdens such as tick-borne pathogens and bovine tuberculosis recently detected in the buffalo population of GNP (de Garine-Wichatitsky et al. 2010) and nearby KNP buffalo. Therefore, tackling the sanitary issue in the periphery of the GLTFCA is of primordial importance for the success of this TFCA initiative (Osofsky et al. 2008).
References
Abdoel, T, Dias I, T., Cardoso R and Smits H, L., 2008. Simple and rapid field tests for brucellosis in livestock, Veterinary Microbiology 130, 312–319
Abernethy, D.A., Moscard-Costello, J., Dickson, E., Harwood, R., Burns, K., McKillop, E., McDowell, S., Pfeiffer, D.U., (2011). Epidemiology and management of a bovine brucellosis cluster in Northern Ireland, Preventive Veterinary Medicine, 98, 223–229
Alton, G., Jones, L.M., Angus, R.D., Verger, J.M., 1988. Techniques for the brucellosis laboratory, (Institute National de la Recherche Agronomique, Paris)
Álvarez, J., Luis Sáez, J., García, N., Serrat, C., Pérez-Sancho, M., González, S., Jesús Ortega, M., Gou, J., Carbajo, L., Garrido, F., Goyache, J. and Domínguez, L., 2011. Management of an outbreak of brucellosis due to B. melitensis in dairy cattle in Spain, Research in Veterinary Science, 90, 208–211
Bengis, R.G., Kock, R.A. and Fischer, J., 2002. Infectious animal diseases: the wildlife/livestock interface. Office International Des Epizooties 21: 53–65
Blood, D.C., Henderson. J.A. and Radostitis, M.O., 2000. Veterinary medicine, a text book of diseases of cattle, sheep, goats and horses, (Baillire Tindall, London)
Bricker, B.J. and Halling, S.M., 1994. Differentiation of Brucella abortus bv. 1, 2, and 4, Brucella melitensis, Brucella ovis and Brucella suis bv. 1 by PCR. Journal of Clinical Microbiology, 32, 2660
Brinley Morgan, W.J., 1977. The diagnosis of Brucella abortus infection in Britain. In: R.P. Crawford and R.J. Hidalgo (eds), Bovine brucellosis, an international symposium, (Texas A&M University Press, College Station), 21–39
Carter, G.R., Chengappa, M.M. and Roberts, A.W., 1995. Essential of veterinary microbiology, (Williams & Wilkins, Lippincott)
Carvalho Neta, A.V., Juliana, C., Mol, P.S., Xavier, M. N., Paixão, T. A., Lage, A. P. and Santos, R. L., 2010. Pathogenesis of bovine brucellosis, The Veterinary Journal, 184,146–155
Condy J.B. and Vickers D.B., 1969. The isolation of Brucella abortus from a waterbuck, The Veterinary Record, 85, 200
Condy J.B. and Vickers D.B., 1972. Brucellosis in Rhodesian Wildlife, Journal of the South African Veterinary Association, 43, 175–179
Crawford, R.P., Huber, J.D. and Adams, B.C. 1990: Epidemiology and surveillance. In: K.E. Nelson and J.R. Ducan (eds), Animal brucellosis, (CRC, Boca Raton), 131–151
Cunningham, B., 1977. A difficult disease called brucellosis. In: R.P. Crawford and R.J. Hidalgo (eds), Bovine brucellosis: an international symposium, (Texas A&M University Press, College Station), 11–20
de Garine-Wichatitsky, M., A. Caron, A. Gomo, C. Foggin, K. Dutlow, D. Pfukenyi, E. Lane, S. Le Bel, M. Hofmeyr, T. Hlokwe, and A. Michel., 2010. Bovine tuberculosis in buffaloes, Southern Africa. Emerging Infectious Diseases, 16, 884–885
England, T., Kelly, L., Jones, R.D., MacMillan, A. and Wooldridge, M., 2004. A simulation model of brucellosis spread in British cattle under several testing regimes. Preventive Veterinary Medicine, 63, 63–73
Godfroid, J., 2002. Brucellosis in wildlife. Revue Scientifique Et Technique D’Office International Des Epizooties, 21, 277–286
Herr, S. and Marshall, C., 1981. Brucellosis in free-living African buffalo (Syncerus caffer): a serological survey, Onderstepoort Journal Veterinary Research, 48, 133–134
Jiwa, S.F.H., Kazwala, R.R., Tungaraza, R., Kimera, S.I. and Kalaye, W.J. 1996: Bovine brucellosis serum agglutination test prevalence and breed disposition according to prevalent management systems in the Lake Victoria zone of Tanzania. Preventive Veterinary Medicine, 26, 341–346
Kadohira, M., McDermott, J.J., Shoukri, M.M. and Kyule, M.N., 1997. Variations in the prevalence of antibody to Brucella infection in cattle by farm, area and district in Kenya. Epidemiology and Infections, 118: 35–41
Kubuafor, D.K., Awumbila, B. and Akanmori, B.D., 2000. Seroprevalence of brucellosis in cattle and humans in Akwapim-South district of Ghana: public health implications. Acta Tropica, 76, 45–48
Madsen, M., 1989. The current state of brucellosis in Zimbabwe. Zimbabwe Veterinary Journal, 20, 133–149
Madsen, M. and Anderson, E .C., 1995. Serological survey of Zimbabwe wildlife for brucellosis. Journal of Zoo and Wildlife Medicine, 26, 240–245
Madzima, W.M., 1987. Zimbabwe. In: Bovine brucellosis and brucellosis of small ruminants: Diagnosis, control and vaccination, (Technical series, Office International des Epizooties (OIE), Paris), 80–82
Manley, F.H., 1969. Brucellosis in Rhodesia. (unpublished report, Director of Veterinary Services, Salisbury)
Matope, G., 2008. The impact of restocking communal cattle on the spread of brucellosis in Zimbabwe, (unpublished DPhil thesis, University of Zimbabwe, Harare, Zimbabwe)
Matope, G., Bhebhe, E., Muma, J.B., Lund, A. and Skjerve, E., 2010. Herd-level factors for Brucella seropositivity in cattle reared in smallholder dairy farms of Zimbabwe. Preventive Veterinary Medicine, 94,213–221
McDermott, J.J. and Arimi, S.M., 2002. Brucellosis in sub-Saharan Africa:epidemiology, control and impact,Veterinary Microbiology 90,111–134
McDermott, J.J., Deng, K.A., Jayatileka, T.N. and El Jack, M.A., 1987. A cross-sectional cattle disease study in Kongor rural council, southern Sudan. I. Prevalence estimates and age sex and breed associations for brucellosis and contagious bovine pleuropneumonia. Preventive Veterinary Medicine, 5, 111–123
McGiven J. A., Sawyer J., Perrett L.L., Brew S. D., Commander N. J, Fisher A., McLarnon S., Harper K. and Stack J. A., 2008. A new homogeneous assay for high throughput serological diagnosis of brucellosis in ruminants, Journal of Immunological Methods, 337 (1), 7–15
Mohan, K., Makaya, P.V., Muvavarirwa, P., Matope, G., Mahembe, E. and Pawandiwa, A., 1996. Brucellosis surveillance and control in Zimbabwe: bacteriological and serological investigation in dairy herds. Onderstepoort Journal of Veterinary Research, 63, 47–51
Moreno, E., and Moriyon, 1. 2006. The genus Brucella. In: Dworking, M., S. Falkow, E. Rosenberg, K-H Scheifer and E. Stackebrant. (eds). Vol. 5 part1. section 3.1. The Prokaryotes: Springer-Verlag, New York, 315–456
Muma, J.B., Samui, K.L., Siamudaala, V.M., Oloya, J., Matope, G., Omer, M.K., Munyeme, M., Mubita, C. and Skjerve, E., 2006. Prevalence of antibodies to Brucella spp. and individual risk factors of infection in traditional cattle, goats and sheep reared in livestock–wildlife interface areas of Zambia. Tropical Animal Health and Production, 38, 195–206
Muma, J.B., Munyeme, M., Samui, K.L, Skejerve, E. and Oloya, B.C., 2007. Risk factors for brucellosis in indigenous cattle reared in livestock–wildlife interface areas of Zambia. Preventive Veterinary Medicine, 80, 306–317
Nicoletti, P., 1980. The epidemiology of bovine brucellosis. Advances in Veterinary Science and Comparative Medicine, 24, 69–98
Nielsen, K., Gall, D., Smith, P., Vigliocco, A., Perez, B., Samartino, L., Nicoletti, P., Dajer, A., Elzer, P. and Enright, F., 1999. Validation of the fluorescence polarization assay as a serological test for the presumptive diagnosis of porcine brucellosis. Veterinary Microbiology, 68, 245–253
Nielsen, K., Gall, D., Bermudez, R., Renteria, T., Moreno, F., Corral, A., Monroy, O., Monge, F., Smith, P., Widdison, J., Mardrueno, M., Calderon, N., Guerrero, R., Tinoco, R., Osuna, J. and Kelly, W., 2002. Field trial of the brucellosis fluorescence polarization assay. Journal of Immunochemistry, 23, 307–316
Nielsen, K., Smith, P., Widdison, J., Gall, D., Kelly, L., Kelly, W. and Nicoletti, P., 2004. Serological relationship between cattle exposed to Brucella abortus, Yersinia enterocolitica O: 9 and Escherichia coli O157: H7. Veterinary Microbiology, 100, 25–30
OIE, 2009. Manual of the diagnostic tests and vaccines for terrestrial animals, (Office International Des Epizooties, Paris)
Olsen, S. C., 2010. Brucellosis in the United States: role and significance of wildlife reservoirs, Vaccine, 28S, 73–76
Olsen, S. and Tatum, F., 2010. Bovine brucellosis, Veterinary Clinics of North America: Food Animal Practice, 26, 15–27
Omer, M.K., Skjerve, E., Woldehiwet, Z. and Holstad, G., 2000. Risk factors for Brucella spp. infection in dairy cattle farms in Asmara, State of Eritrea. Preventive Veterinary Medicine, 46, 257–265
Osofsky, S. A., H. M. Cumming, and M. D. Kock., 2008. Transboundary management of natural resources and the importance of a “one health” approach. In E. Fearn (ed), State of the wild: a global portrait of wildlife, wildlands, and oceans, (Island Press, Washington, D.C.)
Quinn, P.J., Carter, M.E., Markey, B. and Carter, G.R., 1999. Clinical veterinary microbiology, (Mosby International Limited, Edinburgh)
Swanepoel, R., Blackburn, N.K. and Lander, K., 1975. Investigation of infectious infertility and abortion of cattle. Rhodesia (Zimbabwe) Veterinary Journal, 6, 42–55
Swanepoel, R., Blackburn, N.K. and Lander, K., 1976. The occurrence, diagnosis and control of brucellosis in cattle in Rhodesia. Rhodesia Veterinary Journal, 7, 24–31
Thim, B. and Wundt, W., 1976. The epidemiological situation of brucellosis in Africa. In: International symposium on brucellosis (II), Rabat, 1975, (Development of Biological Standards 31), 201–217
Walker, R.L., 1999. Veterinary microbiology, (Blackwell Science, Cambridge)
Whatmore A.M., 2009. Current understanding of the genetic diversity of Brucella, an expanding genus of zoonotic pathogens, Infection Genetics and Evolution, 9, 1168–1184
Acknowledgments
This work was conducted within the framework of the Research Platform “production and Conservation in partnership” RP-PCP. We thank the Ministère Francais de Affaires Etrangères for supporting this project through the French Embassy in Zimbabwe (RP-PCP grant/project AHE#1 2007 to 2009). Thanks are extended to the Veterinary services in the Chiredzi district, the Central Veterinary Laboratory and the Park and Wildlife Management Authority for field support and permit to work in areas under their jurisdiction.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Gomo, C., de Garine-Wichatitsky, M., Caron, A. et al. Survey of brucellosis at the wildlife–livestock interface on the Zimbabwean side of the Great Limpopo Transfrontier Conservation Area. Trop Anim Health Prod 44, 77–85 (2012). https://doi.org/10.1007/s11250-011-9890-5
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11250-011-9890-5